Abstract
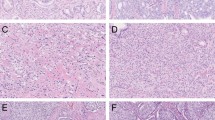
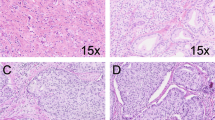
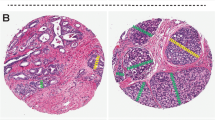
The Gleason scoring system is widely used for the grading and prognostication of prostate cancer. A Gleason pattern 4 subtype known as cribriform morphology has now been recognized as an aggressive and often lethal pattern of prostate cancer. The vast majority of published and ongoing prostate cancer studies still do not acknowledge the prognostic differences between various Gleason pattern 4 morphologies. As a result, current treatment recommendations are likely to be imprecise and not tailored towards patients who are most likely to die from the disease. Use of active surveillance for patients with Gleason score 3 + 4 prostate cancer has been suggested. However, the success of such paradigms would require cribriform morphology to be reported at the time of prostate biopsy, as patients harbouring such a pattern are poor candidates for surveillance. To date, only a limited number of studies have described the molecular alterations that occur in the cribriform morphological pattern. Further refinement of prostate cancer grading paradigms to distinguish cribriform from noncribriform Gleason pattern 4 is essential.
Key points
-
Optimizing the detection and treatment of lethal prostate cancer is critical.
-
The Gleason scoring system is the most widely used pathological grading system for characterizing prostate cancer aggressiveness.
-
Gleason pattern 4 consists of four distinct morphological subtypes — fused, poorly formed, cribriform, and glomeruloid.
-
Cribriform morphology is now recognized as the most aggressive Gleason pattern 4 subtype.
-
Molecular alterations in cribriform tumours have been observed and might explain the aggressiveness of this subtype.
-
Although not yet mandatory, the routine reporting of cribriform morphology on pathological biopsy reports should be highly encouraged.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Gleason, D. F. Classification of prostatic carcinomas. Cancer Chemother. Rep. 50, 125–128 (1966).
National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology: Prostate Cancer Version 2.2018. National Comprehensive Cancer Network https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf (2018).
Gleason, D. F. & Mellinger, G. T. Prediction of prognosis for prostatic adenocarcinoma by combined histological grading and clinical staging. J. Urol. 111, 58–64 (1974).
Kryvenko, O. N. & Epstein, J. I. Changes in prostate cancer grading: Including a new patient-centric grading system. Prostate 76, 427–433 (2016).
McNeal, J. E., Reese, J. H., Redwine, E. A., Freiha, F. S. & Stamey, T. A. Cribriform adenocarcinoma of the prostate. Cancer 58, 1714–1719 (1986).
McNeal, J. E., Villers, A. A., Redwine, E. A., Freiha, F. S. & Stamey, T. A. Histologic differentiation, cancer volume, and pelvic lymph node metastasis in adenocarcinoma of the prostate. Cancer 66, 1225–1233 (1990).
Epstein, J. I., Allsbrook, W. C., Amin, M. B., Egevad, L. L. & ISUP Grading Committee. The 2005 International Society of Urological Pathology (ISUP) Consensus Conference on Gleason grading of prostatic carcinoma. Am. J. Surg. Pathol. 29, 1228–1242 (2005).
Latour, M. et al. Grading of invasive cribriform carcinoma on prostate needle biopsy: an interobserver study among experts in genitourinary pathology. Am. J. Surg. Pathol. 32, 1532–1539 (2008).
Iczkowski, K. A. et al. Digital quantification of five high-grade prostate cancer patterns, including the cribriform pattern, and their association with adverse outcome. Am. J. Clin. Pathol. 136, 98–107 (2011).
Miyamoto, H., Hernandez, D. J. & Epstein, J. I. A pathological reassessment of organ-confined, Gleason score 6 prostatic adenocarcinomas that progress after radical prostatectomy. Hum. Pathol. 40, 1693–1698 (2009).
Alberts, A. R. et al. Biopsy undergrading in men with Gleason score 6 and fatal prostate cancer in the European Randomized study of Screening for Prostate Cancer Rotterdam. Int. J. Urol. 24, 281–286 (2017).
Ross, H. M. et al. Do adenocarcinomas of the prostate with Gleason score (GS) ≤6 have the potential to metastasize to lymph nodes? Am. J. Surg. Pathol. 36, 1346–1352 (2012).
Epstein, J. I. et al. The 2014 International Society of Urological Pathology (ISUP) Consensus Conference on Gleason grading of prostatic carcinoma: definition of grading patterns and proposal for a new grading system. Am. J. Surg. Pathol. 40, 244–252 (2016).
Humphrey, P. A., Moch, H., Cubilla, A. L., Ulbright, T. M. & Reuter, V. E. The 2016 WHO classification of tumours of the urinary system and male genital organs — part B: prostate and bladder tumours. Eur. Urol. 70, 106–119 (2016).
Flood, T. A. et al. Utility of Gleason pattern 4 morphologies detected on transrectal ultrasound (TRUS)-guided biopsies for prediction of upgrading or upstaging in Gleason score 3 + 4 = 7 prostate cancer. Virchows Arch. 469, 313–319 (2016).
Kweldam, C. F. et al. Gleason grade 4 prostate adenocarcinoma patterns: an interobserver agreement study among genitourinary pathologists. Histopathology 69, 441–449 (2016).
Lotan, T. L. & Epstein, J. I. Gleason grading of prostatic adenocarcinoma with glomeruloid features on needle biopsy. Hum. Pathol. 40, 471–477 (2009).
Robinson, B. D. & Epstein, J. I. Intraductal carcinoma of the prostate without invasive carcinoma on needle biopsy: emphasis on radical prostatectomy findings. J. Urol. 184, 1328–1333 (2010).
Van der Kwast, T. et al. Biopsy diagnosis of intraductal carcinoma is prognostic in intermediate and high risk prostate cancer patients treated by radiotherapy. Eur. J. Cancer 48, 1318–1325 (2012).
Kimura, K. et al. Prognostic value of intraductal carcinoma of the prostate in radical prostatectomy specimens. Prostate 74, 680–687 (2014).
Roobol, M. J. et al. Improving the Rotterdam European Randomized Study of Screening for Prostate Cancer Risk Calculator for initial prostate biopsy by incorporating the 2014 International Society of Urological Pathology Gleason Grading and cribriform growth. Eur. Urol. 72, 45–51 (2017).
Chua, M. L. K. et al. A prostate cancer “nimbosus”: genomic instability and SChLAP1 dysregulation underpin aggression of intraductal and cribriform subpathologies. Eur. Urol. 72, 665–674 (2017).
Sarbay, B. C., Kir, G., Topal, C. S. & Gumus, E. Significance of the cribriform pattern in prostatic adenocarcinomas. Pathol. Res. Pract. 210, 554–557 (2014).
Dong, F. et al. Architectural heterogeneity and cribriform pattern predict adverse clinical outcome for Gleason grade 4 prostatic adenocarcinoma. Am. J. Surg. Pathol. 37, 1855–1861 (2013).
Trudel, D. et al. Prognostic impact of intraductal carcinoma and large cribriform carcinoma architecture after prostatectomy in a contemporary cohort. Eur. J. Cancer 50, 1610–1616 (2014).
Kir, G., Sarbay, B. C., Gumus, E. & Topal, C. S. The association of the cribriform pattern with outcome for prostatic adenocarcinomas. Pathol. Res. Pract. 210, 640–644 (2014).
Kryvenko, O. N. et al. Gleason score 7 adenocarcinoma of the prostate with lymph node metastases: analysis of 184 radical prostatectomy specimens. Arch. Pathol. Lab Med. 137, 610–617 (2013).
Flood, T. A. et al. Perineural invasion on biopsy is associated with upstaging at radical prostatectomy in Gleason score 3 + 4 = 7 prostate cancer. Pathol. Int. 66, 629–632 (2016).
Harding-Jackson, N. et al. Outcome of Gleason 3 + 5 = 8 prostate cancer diagnosed on needle biopsy: prognostic comparison with Gleason 4 + 4 = 8. J. Urol. 196, 1076–1081 (2016).
McKenney, J. K. et al. Histologic grading of prostatic adenocarcinoma can be further optimized: analysis of the relative prognostic strength of individual architectural patterns in 1275 patients from the Canary retrospective cohort. Am. J. Surg. Pathol. 40, 1439–1456 (2016).
Kweldam, C. F. et al. Disease-specific survival of patients with invasive cribriform and intraductal prostate cancer at diagnostic biopsy. Mod. Pathol. 29, 630–636 (2016).
Siadat, F. et al. Not all gleason pattern 4 prostate cancers are created equal: A study of latent prostatic carcinomas in a cystoprostatectomy and autopsy series. Prostate 75, 1277–1284 (2015).
Truong, M. et al. A comprehensive analysis of cribriform morphology on MR/US fusion biopsy correlated with radical prostatectomy specimens. J. Urol. 199, 106–113 (2018).
Qian, J., Jenkins, R. B. & Bostwick, D. G. Detection of chromosomal anomalies and c-myc gene amplification in the cribriform pattern of prostatic intraepithelial neoplasia and carcinoma by fluorescence in situ hybridization. Mod. Pathol. 10, 1113–1119 (1997).
Ronen, S. et al. PTEN loss and p27 loss differ among morphologic patterns of prostate cancer, including cribriform. Hum. Pathol. 65, 85–91 (2017).
Hubbard, G. K. et al. MYC overexpression combined with Pten loss generates genomic instability and rapid metastasis in a new mouse model of lethal prostate adenocarcinoma [abstract]. Cancer Res. 73 (Suppl.), 1086 (2013).
Downes, M. R., Satturwar, S., Trudel, D. & van der Kwast, T. H. Evaluation of ERG and PTEN protein expression in cribriform architecture prostate carcinomas. Pathol. Res. Pract. 213, 34–38 (2017).
Mosquera, J. M. et al. Prevalence of TMPRSS2-ERG fusion prostate cancer among men undergoing prostate biopsy in the United States. Clin. Cancer Res. 15, 4706–4711 (2009).
Fine, S. W. et al. TMPRSS2-ERG gene fusion is associated with low Gleason scores and not with high-grade morphological features. Mod. Pathol. 23, 1325–1333 (2010).
Chen, H. H. et al. NRIP/DCAF6 stabilizes the androgen receptor protein by displacing DDB2 from the CUL4A-DDB1 E3 ligase complex in prostate cancer. Oncotarget 8, 21501–21515 (2017).
Mukai, S. et al. Expression of human kallikrein 1-related peptidase 4 (KLK4) and MET phosphorylation in prostate cancer tissue: immunohistochemical analysis. Hum. Cell 28, 133–142 (2015).
Pierconti, F. et al. Epigenetic silencing of SOCS3 identifies a subset of prostate cancer with an aggressive behavior. Prostate 71, 318–325 (2011).
Pierconti, F. et al. SOCS3 immunohistochemical expression seems to support the 2005 and 2014 International Society of Urological Pathology (ISUP) modified Gleason grading system. Prostate 77, 597–603 (2017).
Olkhov-Mitsel, E. et al. Distinct DNA methylation alterations are associated with cribriform architecture and intraductal carcinoma in Gleason pattern 4 prostate tumors. Oncol. Lett. 14, 390–396 (2017).
Sowalsky, A. G. et al. Gleason score 7 prostate cancers emerge through branched evolution of clonal Gleason pattern 3 and 4. Clin. Cancer Res. 23, 3823–3833 (2017).
Herawi, M. & Epstein, J. I. Immunohistochemical antibody cocktail staining (p63/HMWCK/AMACR) of ductal adenocarcinoma and Gleason pattern 4 cribriform and noncribriform acinar adenocarcinomas of the prostate. Am. J. Surg. Pathol. 31, 889–894 (2007).
Epstein, J. I., Amin, M. B., Reuter, V. E. & Humphrey, P. A. Contemporary Gleason grading of prostatic carcinoma: an update with discussion on practical issues to implement the 2014 International Society of Urological Pathology (ISUP) consensus conference on Gleason grading of prostatic carcinoma. Am. J. Surg. Pathol. 41, e1–e7 (2017).
Downes, M. R. et al. Determination of the association between T2-weighted MRI and Gleason sub-pattern: a proof of principle study. Acad. Radiol 23, 1412–1421 (2016).
Truong, M. et al. Impact of Gleason subtype on prostate cancer detection using multiparametric MRI: correlation with final histopathology. J. Urol. 198, 316–321 (2017).
Keefe, D. T. et al. Cribriform morphology predicts upstaging after radical prostatectomy in patients with Gleason score 3 + 4 = 7 prostate cancer at transrectal ultrasound (TRUS)-guided needle biopsy. Virchows Arch. 467, 437–442 (2015).
Morlacco, A., Cheville, J. C., Rangel, L. J., Gearman, D. J. & Karnes, R. J. Adverse disease features in Gleason score 3 + 4 “favorable intermediate-risk” prostate cancer: implications for active surveillance. Eur. Urol. 72, 442–447 (2016).
Cole, A. I. et al. Prognostic value of percent Gleason grade 4 at prostate biopsy in predicting prostatectomy pathology and recurrence. J. Urol. 196, 405–411 (2016).
Huang, C. C. et al. Gleason score 3 + 4 = 7 prostate cancer with minimal quantity of gleason pattern 4 on needle biopsy is associated with low-risk tumor in radical prostatectomy specimen. Am. J. Surg. Pathol. 38, 1096–1101 (2014).
Choy, B. et al. Prognostic Significance of percentage and architectural types of contemporary Gleason pattern 4 prostate cancer in radical prostatectomy. Am. J. Surg. Pathol. 40, 1400–1406 (2016).
Kweldam, C. F. et al. Presence of invasive cribriform or intraductal growth at biopsy outperforms percentage grade 4 in predicting outcome of Gleason score 3 + 4 = 7 prostate cancer. Mod. Pathol. 30, 1126–1132 (2017).
Sadimin, E. T., Khani, F., Diolombi, M., Meliti, A. & Epstein, J. I. Interobserver reproducibility of percent Gleason pattern 4 in prostatic adenocarcinoma on prostate biopsies. Am. J. Surg. Pathol. 40, 1686–1692 (2016).
Patel, H. D., Tosoian, J. J., Carter, H. B. & Epstein, J. I. Adverse pathologic findings for men electing immediate radical prostatectomy: defining a favorable intermediate-risk group. JAMA Oncol. 4, 89–92 (2017).
Valerio, M. et al. New and established technology in focal ablation of the prostate: a systematic review. Eur. Urol. 71, 17–34 (2017).
Gordetsky, J., Rais-Bahrami, S. & Epstein, J. I. Pathological findings in multiparametric MRI/ultrasound fusion guided biopsy: relation to prostate cancer focal therapy. Urology 105, 18–23 (2017).
Nassiri, N. et al. Focal therapy eligibility determined by magnetic resonance imaging/ultrasound fusion biopsy. J. Urol. 199, 453–458 (2018).
Kweldam, C. F. et al. Cribriform growth is highly predictive for postoperative metastasis and disease-specific death in Gleason score 7 prostate cancer. Mod. Pathol. 28, 457–464 (2015).
Kweldam, C. F. et al. Prostate cancer outcomes of men with biopsy Gleason score 6 and 7 without cribriform or intraductal carcinoma. Eur. J. Cancer 66, 26–33 (2016).
Iczkowski, K. A., Paner, G. P. & Van der Kwast, T. The new realization about cribriform prostate cancer. Adv. Anat. Pathol. 25, 31–37 (2018).
Reviewer information
Nature Reviews Urology thanks R. Montironi, G. Netto, and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
All authors contributed to researching data for the article, discussion of content, writing the article, and review and editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Review criteria
PubMed and Embase searches were conducted using the following search terms: “prostate cancer” and “cribriform”; and “cribriform” and “Gleason.” A total of 401 unique results were identified. Abstracts were reviewed, and appropriate English-language peer-reviewed full-text articles were extracted for more comprehensive review. Initially, selected articles involved histological evaluation of prostate cancer for cribriform morphology, prostate cancer prognostication based on cribriform morphology, treatment of prostate cancer containing cribriform morphology, or biomolecular studies involving prostate tumours containing cribriform morphology. The final articles selected for inclusion were those considered to have a good quality of evidence and high relevance according to mutual agreement by the authors.
Rights and permissions
About this article
Cite this article
Truong, M., Frye, T., Messing, E. et al. Historical and contemporary perspectives on cribriform morphology in prostate cancer. Nat Rev Urol 15, 475–482 (2018). https://doi.org/10.1038/s41585-018-0013-1
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41585-018-0013-1
This article is cited by
-
Active surveillance should be considered for select men with Grade Group 2 prostate cancer
BMC Urology (2023)
-
Integrated analysis of single-cell and bulk RNA sequencing identifies a signature based on macrophage marker genes involved in prostate cancer prognosis and treatment responsiveness
Functional & Integrative Genomics (2023)
-
A systematic review and meta-analysis of artificial intelligence diagnostic accuracy in prostate cancer histology identification and grading
Prostate Cancer and Prostatic Diseases (2023)
-
Identification of ISG15 and ZFP36 as novel hypoxia- and immune-related gene signatures contributing to a new perspective for the treatment of prostate cancer by bioinformatics and experimental verification
Journal of Translational Medicine (2022)
-
The influence of BRCA2 mutation on localized prostate cancer
Nature Reviews Urology (2019)