Abstract
Intra-articular drug delivery has a number of advantages over systemic administration; however, for the past 20 years, intra-articular treatment options for the management of knee osteoarthritis (OA) have been limited to analgesics, glucocorticoids, hyaluronic acid (HA) and a small number of unproven alternative therapies. Although HA and glucocorticoids can provide clinically meaningful benefits to an appreciable number of patients, emerging evidence indicates that the apparent effectiveness of these treatments is largely a result of other factors, including the placebo effect. Biologic drugs that target inflammatory processes are used to manage rheumatoid arthritis, but have not translated well into use in OA. A lack of high-level evidence and methodological limitations hinder our understanding of so-called ‘stem’ cell therapies and, although the off-label administration of intra-articular cell therapies (such as platelet-rich plasma and bone marrow aspirate concentrate) is common, high-quality clinical data are needed before these treatments can be recommended. A number of promising intra-articular treatments are currently in clinical development in the United States, including small-molecule and biologic therapies, devices and gene therapies. Although the prospect of new, non-surgical treatments for OA is exciting, the benefits of new treatments must be carefully weighed against their costs and potential risks.
Key points
-
The cost and unclear effectiveness of hyaluronic acid and glucocorticoids have raised concerns over their broad use for osteoarthritis (OA)-related knee pain.
-
Self-reported parameters such as pain and stiffness are particularly responsive to intra-articular placebo, which poses challenges when attempting to ascribe clinical meaning to therapeutic interventions.
-
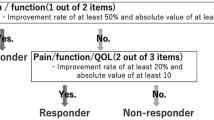
Estimates of the minimal (clinically) important difference for patient-reported outcomes can provide useful pretext when appraising the effectiveness of intra-articular therapies.
-
Lack of data, study heterogeneity and methodological limitations hinder our understanding of point-of-care injectable cell therapies such as platelet-rich plasma, bone marrow aspirate concentrate and adipose tissue-derived treatments.
-
The generally positive efficacy conclusions concerning mesenchymal ‘stem’ cell therapy for knee cartilage pathology might be overstated owing to selective outcome reporting.
-
A number of intra-articular therapeutic candidates for OA are currently in clinical development, including small-molecule therapies, biologic therapies, gene therapies and novel devices.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Sinusas, K. Osteoarthritis: diagnosis and treatment. Am. Fam. Physician 85, 49–56 (2012).
Liu-Bryan, R. Synovium and the innate inflammatory network in osteoarthritis progression. Curr. Rheumatol Rep. 15, 323 (2013).
Haseeb, A. & Haqqi, T. M. Immunopathogenesis of osteoarthritis. Clin. Immunol. 146, 185–196 (2013).
Aigner, T., Söder, S., Gebhard, P. M., McAlinden, A. & Haag, J. Mechanisms of disease: role of chondrocytes in the pathogenesis of osteoarthritis — structure, chaos and senescence. Nat. Clin. Pract. Rheumatol. 3, 391–399 (2007).
Chevalier, X., Eymard, F. & Richette, P. Biologic agents in osteoarthritis: hopes and disappointments. Nat. Rev. Rheumatol. 9, 400–410 (2013).
Lories, R. J. & Luyten, F. P. The bone–cartilage unit in osteoarthritis. Nat. Rev. Rheumatol. 7, 43–49 (2011).
Emami, A. et al. Toxicology evaluation of drugs administered via uncommon routes: intranasal, intraocular, intrathecal/intraspinal, and intra-articular. Int. J. Toxicol. 37, 4–27 (2018).
Evans, C. H., Kraus, V. B. & Setton, L. A. Progress in intra-articular therapy. Nat. Rev. Rheumatol. 10, 11–22 (2014).
Rousseau, J.-C. & Delmas, P. D. Biological markers in osteoarthritis. Nat. Clin. Pract. Rheumatol. 3, 346–356 (2007).
Robinson, W. H. et al. Low-grade inflammation as a key mediator of the pathogenesis of osteoarthritis. Nat. Rev. Rheumatol. 12, 580–592 (2016).
Sellam, J. & Berenbaum, F. The role of synovitis in pathophysiology and clinical symptoms of osteoarthritis. Nat. Rev. Rheumatol. 6, 625–635 (2010).
Maudens, P., Jordan, O. & Allémann, E. Recent advances in intra-articular drug delivery systems for osteoarthritis therapy. Drug Discov. Today 23, 1761–1775 (2018).
Miller, R. E., Block, J. A. & Malfait, A.-M. What is new in pain modification in osteoarthritis? Rheumatology 58, 26 (2018).
Nelson, A. E., Allen, K. D., Golightly, Y. M., Goode, A. P. & Jordan, J. M. A systematic review of recommendations and guidelines for the management of osteoarthritis: the chronic osteoarthritis management initiative of the U.S. bone and joint initiative. Semin. Arthritis Rheum. 43, 701–712 (2014).
Nguyen, C., Lefèvre-Colau, M.-M., Poiraudeau, S. & Rannou, F. Evidence and recommendations for use of intra-articular injections for knee osteoarthritis. Ann. Phys. Rehabil. Med. 59, 184–189 (2016).
Gerwin, N., Hops, C. & Lucke, A. Intraarticular drug delivery in osteoarthritis. Adv. Drug Deliv. Rev. 58, 226–242 (2006).
Habib, G. S. Systemic effects of intra-articular corticosteroids. Clin. Rheumatol. 28, 749–756 (2009).
Jackson, D. W., Evans, N. A. & Thomas, B. M. Accuracy of needle placement into the intra-articular space of the knee. J. Bone Joint Surg. Am. 84, 1522–1527 (2002).
Larsen, C. et al. Intra-articular depot formulation principles: role in the management of postoperative pain and arthritic disorders. J. Pharm. Sci. 97, 4622–4654 (2008).
Bannuru, R. R., Natov, N. S., Dasi, U. R., Schmid, C. H. & McAlindon, T. E. Therapeutic trajectory following intra-articular hyaluronic acid injection in knee osteoarthritis — meta-analysis. Osteoarthr. Cartil. 19, 611–619 (2011).
Rosseland, L. A., Helgesen, K. G., Breivik, H. & Stubhaug, A. Moderate-to-severe pain after knee arthroscopy is relieved by intraarticular saline: a randomized controlled trial. Anesth. Analg. 98, 1546–1551 (2004).
Abhishek, A. & Doherty, M. Mechanisms of the placebo response in pain in osteoarthritis. Osteoarthr. Cartil. 21, 1229–1235 (2013).
Bannuru, R. R. et al. Effectiveness and implications of alternative placebo treatments: a systematic review and network meta-analysis of osteoarthritis trials. Ann. Intern. Med. 163, 365–372 (2015).
Kirwan, J. R. & Rankin, E. Intra-articular therapy in osteoarthritis. Baillieres Clin. Rheumatol 11, 769–794 (1997).
Hameed, F. & Ihm, J. Injectable medications for osteoarthritis. PM R. 4, S75–S81 (2012).
Saltzman, B. M. et al. The therapeutic effect of intra-articular normal saline injections for knee osteoarthritis: a meta-analysis of evidence level 1 studies. Am. J. Sports Med. 45, 2647–2653 (2017).
Sullivan, G. M. & Feinn, R. Using effect size — or why the P value is not enough. J. Grad. Med. Educ. 4, 279–282 (2012).
Jaeschke, R., Singer, J. & Guyatt, G. H. Measurement of health status: ascertaining the minimal clinically important difference. Control. Clin. Trials 10, 407–415 (1989).
Redelmeier, D. A. & Lorig, K. Assessing the clinical importance of symptomatic improvements. An illustration in rheumatology. Arch. Intern. Med. 153, 1337–1342 (1993).
Angst, F., Aeschlimann, A. & Angst, J. The minimal clinically important difference raised the significance of outcome effects above the statistical level, with methodological implications for future studies. J. Clin. Epidemiol. 82, 128–136 (2017).
McGlothlin, A. E. & Lewis, R. J. Minimal clinically important difference: defining what really matters to patients. JAMA 312, 1342–1343 (2014).
Devji, T. et al. Application of minimal important differences in degenerative knee disease outcomes: a systematic review and case study to inform BMJ Rapid Recommendations. BMJ Open 7, e015587 (2017).
Dworkin, R. H. et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J. Pain 9, 105–121 (2008).
Copay, A. G., Subach, B. R., Glassman, S. D., Polly, D. W. & Schuler, T. C. Understanding the minimum clinically important difference: a review of concepts and methods. Spine J. 7, 541–546 (2007).
King, M. T. A point of minimal important difference (MID): a critique of terminology and methods. Expert Rev. Pharmacoecon Outcomes Res. 11, 171–184 (2011).
Wright, A., Hannon, J., Hegedus, E. J. & Kavchak, A. E. Clinimetrics corner: a closer look at the minimal clinically important difference (MCID). J. Man. Manip. Ther. 20, 160–166 (2012).
Cook, C. E. Clinimetrics corner: the minimal clinically important change score (MCID): a necessary pretense. J. Man. Manip. Ther. 16, E82–E83 (2008).
Revicki, D., Hays, R. D., Cella, D. & Sloan, J. Recommended methods for determining responsiveness and minimally important differences for patient-reported outcomes. J. Clin. Epidemiol. 61, 102–109 (2008).
Bedard, N. A. et al. Impact of clinical practice guidelines on use of intra-articular hyaluronic acid and corticosteroid injections for knee osteoarthritis. J. Bone Joint Surg. Am. 100, 827–834 (2018).
Migliore, A. et al. The discrepancy between recommendations and clinical practice for viscosupplementation in osteoarthritis: mind the gap! Eur. Rev. Med. Pharmacol. Sci. 19, 1124–1129 (2015).
Jevsevar, D. S. et al. The American Academy of Orthopaedic Surgeons evidence-based guideline on: treatment of osteoarthritis of the knee, 2nd edition. J. Bone Joint Surg. Am. 95, 1885–1886 (2013).
Chao, J. et al. Inflammatory characteristics on ultrasound predict poorer longterm response to intraarticular corticosteroid injections in knee osteoarthritis. J. Rheumatol. 37, 650–655 (2010).
Gaffney, K., Ledingham, J. & Perry, J. D. Intra-articular triamcinolone hexacetonide in knee osteoarthritis: factors influencing the clinical response. Ann. Rheum. Dis. 54, 379–381 (1995).
Raynauld, J.-P. et al. Safety and efficacy of long-term intraarticular steroid injections in osteoarthritis of the knee: a randomized, double-blind, placebo-controlled trial. Arthritis Rheum. 48, 370–377 (2003).
Jones, A. & Doherty, M. Intra-articular corticosteroids are effective in osteoarthritis but there are no clinical predictors of response. Ann. Rheum. Dis. 55, 829–832 (1996).
Caborn, D. et al. A randomized, single-blind comparison of the efficacy and tolerability of hylan G-F 20 and triamcinolone hexacetonide in patients with osteoarthritis of the knee. J. Rheumatol. 31, 333–343 (2004).
Arden, N. K. et al. A randomised controlled trial of tidal irrigation versus corticosteroid injection in knee osteoarthritis: the KIVIS Study. Osteoarthr. Cartil. 16, 733–739 (2008).
McAlindon, T. E. et al. OARSI guidelines for the non-surgical management of knee osteoarthritis. Osteoarthr. Cartil. 22, 363–388 (2014).
Bannuru, R. R. et al. Therapeutic trajectory of hyaluronic acid versus corticosteroids in the treatment of knee osteoarthritis: a systematic review and meta-analysis. Arthritis Rheum. 61, 1704–1711 (2009).
Bellamy, N. et al. Intraarticular corticosteroid for treatment of osteoarthritis of the knee. Cochrane Database Syst. Rev. 2, CD005328 (2006).
Jüni, P. et al. Intra-articular corticosteroid for knee osteoarthritis. Cochrane Database Syst. Rev. 10, CD005328 (2015).
National Institute for Health and Care Excellence. Osteoarthritis: Care and Management in Adults (NICE, 2014).
Hochberg, M. C. et al. American College of Rheumatology 2012 recommendations for the use of nonpharmacologic and pharmacologic therapies in osteoarthritis of the hand, hip, and knee. Arthritis Care Res. 64, 465–474 (2012).
Wernecke, C., Braun, H. J. & Dragoo, J. L. The effect of intra-articular corticosteroids on articular cartilage: a systematic review. Orthop. J. Sports Med. 3, 2325967115581163 (2015).
Bedard, N. A. et al. The John N. Insall Award: do intraarticular injections increase the risk of infection after TKA? Clin. Orthop. Relat. Res. 475, 45–52 (2017).
McAlindon, T. E. et al. Effect of intra-articular triamcinolone versus saline on knee cartilage volume and pain in patients with knee osteoarthritis: a randomized clinical trial. JAMA 317, 1967–1975 (2017).
Cicuttini, F. M., Jones, G., Forbes, A. & Wluka, A. E. Rate of cartilage loss at two years predicts subsequent total knee arthroplasty: a prospective study. Ann. Rheum. Dis. 63, 1124–1127 (2004).
Hitzl, W. et al. Greater lateral femorotibial cartilage loss in osteoarthritis initiative participants with incident total knee arthroplasty: a prospective cohort study. Arthritis Care Res. 67, 1481–1486 (2015).
Bannuru, R. R., Vaysbrot, E. E. & McIntyre, L. F. Did the American Academy of Orthopaedic Surgeons osteoarthritis guidelines miss the mark? Arthroscopy 30, 86–89 (2014).
Carlson, V. R. et al. Compliance with the AAOS guidelines for treatment of osteoarthritis of the knee: a survey of the American Association of Hip and Knee Surgeons. J. Am. Acad. Orthop. Surg. 26, 103–107 (2018).
Rutjes, A. W. S. et al. Viscosupplementation for osteoarthritis of the knee: a systematic review and meta-analysis. Ann. Intern. Med. 157, 180–191 (2012).
Bellamy, N. et al. Viscosupplementation for the treatment of osteoarthritis of the knee. Cochrane Database Syst. Rev. 3, CD005321 (2006).
Jevsevar, D., Donnelly, P., Brown, G. A. & Cummins, D. S. Viscosupplementation for osteoarthritis of the knee: a systematic review of the evidence. J. Bone Joint Surg. Am. 97, 2047–2060 (2015).
Vannabouathong, C. et al. Nonoperative treatments for knee osteoarthritis: an evaluation of treatment characteristics and the intra-articular placebo effect: a systematic review. JBJS Rev. 6, e5 (2018).
Kapoor, M., Martel-Pelletier, J., Lajeunesse, D., Pelletier, J.-P. & Fahmi, H. Role of proinflammatory cytokines in the pathophysiology of osteoarthritis. Nat. Rev. Rheumatol. 7, 33–42 (2011).
Martel-Pelletier, J. Pathophysiology of osteoarthritis. Osteoarthr. Cartil. 6, 374–376 (1998).
Ashraf, S. et al. Regulation of senescence associated signaling mechanisms in chondrocytes for cartilage tissue regeneration. Osteoarthr. Cartil. 24, 196–205 (2016).
Pettipher, E. R., Higgs, G. A. & Henderson, B. Interleukin 1 induces leukocyte infiltration and cartilage proteoglycan degradation in the synovial joint. Proc. Natl Acad. Sci. USA 83, 8749–8753 (1986).
Kato, T. et al. Exosomes from IL-1β stimulated synovial fibroblasts induce osteoarthritic changes in articular chondrocytes. Arthritis Res. Ther. 16, R163 (2014).
Jacques, C., Gosset, M., Berenbaum, F. & Gabay, C. The role of IL-1 and IL-1Ra in joint inflammation and cartilage degradation. Vitam. Horm. 74, 371–403 (2006).
Chevalier, X. et al. Intraarticular injection of anakinra in osteoarthritis of the knee: a multicenter, randomized, double-blind, placebo-controlled study. Arthritis Rheum. 61, 344–352 (2009).
Kraus, V. B. et al. Effects of intraarticular IL1-Ra for acute anterior cruciate ligament knee injury: a randomized controlled pilot trial (NCT00332254). Osteoarthr. Cartil. 20, 271–278 (2012).
Goldring, S. R. & Goldring, M. B. The role of cytokines in cartilage matrix degeneration in osteoarthritis. Clin. Orthop. Relat. Res. 427, S27–S36 (2004).
Stannus, O. et al. Circulating levels of IL-6 and TNF-α are associated with knee radiographic osteoarthritis and knee cartilage loss in older adults. Osteoarthr. Cartil. 18, 1441–1447 (2010).
Malfait, A. M. et al. Intra-articular injection of tumor necrosis factor-α in the rat: an acute and reversible in vivo model of cartilage proteoglycan degradation. Osteoarthr. Cartil. 17, 627–635 (2009).
Lindsley, H. B. et al. Treatment of knee osteoarthritis with intra-articular infliximab improves total WOMAC score. High baseline levels of synovial cellularity predict improvement [abstract FRI0304]. Ann. Rheum. Dis. 71 (Suppl. 3), 417 (2014).
Ohtori, S. et al. Efficacy of direct injection of etanercept into knee joints for pain in moderate and severe knee osteoarthritis. Yonsei Med. J. 56, 1379 (2015).
Wang, J. Efficacy and safety of adalimumab by intra-articular injection for moderate to severe knee osteoarthritis: an open-label randomized controlled trial. J. Int. Med. Res. 46, 326–334 (2018).
Hunter, D. J. et al. Phase 1 safety and tolerability study of BMP-7 in symptomatic knee osteoarthritis. BMC Musculoskelet. Disord. 11, 232 (2010).
Lohmander, L. S. et al. Intraarticular sprifermin (recombinant human fibroblast growth factor 18) in knee osteoarthritis: a randomized, double-blind, placebo-controlled trial. Arthritis Rheumatol. 66, 1820–1831 (2014).
Hall, M. P., Band, P. A., Meislin, R. J., Jazrawi, L. M. & Cardone, D. A. Platelet-rich plasma: current concepts and application in sports medicine. J. Am. Acad. Orthop. Surg. 17, 602–608 (2009).
Hsu, W. K. et al. Platelet-rich plasma in orthopaedic applications: evidence-based recommendations for treatment. J. Am. Acad. Orthop. Surg. 21, 739–471 (2013).
Andia, I. & Maffulli, N. Platelet-rich plasma for managing pain and inflammation in osteoarthritis. Nat. Rev. Rheumatol. 9, 721–730 (2013).
Gutman, S. I. 510(k) summary: 3i CelSep centrifuge system. FDA https://www.accessdata.fda.gov/cdrh_docs/pdf/K994148.pdf (2000).
Melkerson, M. N. 510(k) summary. FDA https://www.accessdata.fda.gov/cdrh_docs/pdf8/K082333.pdf (2009).
Vaught, M. S. & Cole, B. J. Coding and reimbursement issues for platelet-rich plasma. Oper. Tech. Sports Med. 19, 185–189 (2011).
Jones, I. A., Togashi, R. C. & Vangsness, C. T. The economics and regulation of PRP in the evolving field of orthopedic biologics. Curr. Rev. Musculoskelet. Med. 17, 602–608 (2018).
Dhillon, R. S., Schwarz, E. M. & Maloney, M. D. Platelet-rich plasma therapy - future or trend? Arthritis Res. Ther. 14, 219 (2012).
Beitzel, K. et al. US definitions, current use, and FDA stance on use of platelet-rich plasma in sports medicine. J. Knee Surg. 28, 29–34 (2015).
Chahla, J. et al. A call for standardization in platelet-rich plasma preparation protocols and composition reporting: a systematic review of the clinical orthopaedic literature. J. Bone Joint Surg. Am. 99, 1769–1779 (2017).
Chen, X., Jones, I. A., Park, C. & Vangsness, C. T. The efficacy of platelet-rich plasma on tendon and ligament healing: a systematic review and meta-analysis with bias assessment. Am. J. Sports Med. 2016, 363546517743746 (2017).
Khoshbin, A. et al. The efficacy of platelet-rich plasma in the treatment of symptomatic knee osteoarthritis: a systematic review with quantitative synthesis. Arthroscopy 29, 2037–2048 (2013).
Kanchanatawan, W. et al. Short-term outcomes of platelet-rich plasma injection for treatment of osteoarthritis of the knee. Knee Surg. Sports Traumatol. Arthrosc. 24, 1665–1677 (2016).
Tubach, F. et al. Evaluation of clinically relevant changes in patient reported outcomes in knee and hip osteoarthritis: the minimal clinically important improvement. Ann. Rheum. Dis. 64, 29–33 (2005).
Escobar, A. et al. Responsiveness and clinically important differences for the WOMAC and SF-36 after total knee replacement. Osteoarthr. Cartil. 15, 273–280 (2007).
Angst, F., Aeschlimann, A., Michel, B. A. & Stucki, G. Minimal clinically important rehabilitation effects in patients with osteoarthritis of the lower extremities. J. Rheumatol. 29, 131–138 (2002).
Chahla, J. et al. Concentrated bone marrow aspirate for the treatment of chondral injuries and osteoarthritis of the knee: a systematic review of outcomes. Orthop. J. Sports Med. 4, 2325967115625481 (2016).
Bowen, J. E. Technical issues in harvesting and concentrating stem cells (bone marrow and adipose). PM R. 7, S8–S18 (2015).
McCarrel, T. & Fortier, L. Temporal growth factor release from platelet-rich plasma, trehalose lyophilized platelets, and bone marrow aspirate and their effect on tendon and ligament gene expression. J. Orthop. Res. 27, 1033–1042 (2009).
Turner, L. & Knoepfler, P. Selling stem cells in the USA: assessing the direct-to-consumer industry. Cell Stem Cell 19, 154–157 (2016).
Pittenger, M. F. et al. Multilineage potential of adult human mesenchymal stem cells. Science 284, 143–147 (1999).
Aronowitz, J. A., Lockhart, R. A. & Hakakian, C. S. Mechanical versus enzymatic isolation of stromal vascular fraction cells from adipose tissue. Springerplus 4, 713 (2015).
Chirba, M. A., Sweetapple, B., Hannon, C. P. & Anderson, J. A. FDA regulation of adult stem cell therapies as used in sports medicine. J. Knee Surg. 28, 55–62 (2015).
Food and Drug Administration. Regulatory considerations for human cells, tissues, and cellular and tissue-based products: minimal manipulation and homologous use. FDA https://www.fda.gov/downloads/biologicsbloodvaccines/guidancecomplianceregulatoryinformation/guidances/cellularandgenetherapy/ucm585403.pdf (2017).
Marks, P. & Gottlieb, S. Balancing safety and innovation for cell-based regenerative medicine. N. Engl. J. Med. 378, 954–959 (2018).
Kokai, L. E., Marra, K. & Rubin, J. P. Adipose stem cells: biology and clinical applications for tissue repair and regeneration. Transl Res. 163, 399–408 (2014).
Oberbauer, E. et al. Enzymatic and non-enzymatic isolation systems for adipose tissue-derived cells: current state of the art. Cell Regen (Lond.) 4, 7 (2015).
Bourin, P. et al. Stromal cells from the adipose tissue-derived stromal vascular fraction and culture expanded adipose tissue-derived stromal/stem cells: a joint statement of the International Federation for Adipose Therapeutics and Science (IFATS) and the International Society for Cellular Therapy (ISCT). Cytotherapy 15, 641–648 (2013).
Koh, Y.-G., Choi, Y.-J., Kwon, O.-R. & Kim, Y.-S. Second-look arthroscopic evaluation of cartilage lesions after mesenchymal stem cell implantation in osteoarthritic knees. Am. J. Sports Med. 42, 1628–1637 (2014).
Koh, Y.-G., Kwon, O.-R., Kim, Y. S., Choi, Y.-J. & Tak, D.-H. Adipose-derived mesenchymal stem cells with microfracture versus microfracture alone: 2-year follow-up of a prospective randomized trial. Arthroscopy 32, 97–109 (2016).
Pak, J. et al. Current use of autologous adipose tissue-derived stromal vascular fraction cells for orthopedic applications. J. Biomed. Sci. 24, 9 (2017).
Pers, Y.-M. et al. Adipose mesenchymal stromal cell-based therapy for severe osteoarthritis of the knee: a phase I dose-escalation trial. Stem Cells Transl Med. 5, 847–856 (2016).
Fodor, P. B. & Paulseth, S. G. Adipose derived stromal cell (ADSC) injections for pain management of osteoarthritis in the human knee joint. Aesthet. Surg. J. 36, 229–236 (2016).
Mendicino, M., Bailey, A. M., Wonnacott, K., Puri, R. K. & Bauer, S. R. MSC-based product characterization for clinical trials: an FDA perspective. Cell Stem Cell 14, 141–145 (2014).
Freitag, J. et al. Mesenchymal stem cell therapy in the treatment of osteoarthritis: reparative pathways, safety and efficacy - a review. BMC Musculoskelet. Disord. 17, 230 (2016).
Pas, H. I. et al. Stem cell injections in knee osteoarthritis: a systematic review of the literature. Br. J. Sports Med. 51, 1125–1133 (2017).
McIntyre, J. A., Jones, I. A., Han, B. & Vangsness, C. T. Intra-articular mesenchymal stem cell therapy for the human joint: a systematic review. Am. J. Sports Med. 11, 036354651773584 (2017).
Chahla, J. et al. Intra-articular cellular therapy for osteoarthritis and focal cartilage defects of the knee: a systematic review of the literature and study quality analysis. J. Bone Joint Surg. Am. 98, 1511–1521 (2016).
Pak, J., Lee, J. H., Park, K. S., Jeon, J. H. & Lee, S. H. Potential use of mesenchymal stem cells in human meniscal repair: current insights. Open Access J. Sports Med. 8, 33–38 (2017).
Caplan, A. I. Mesenchymal stem cells. J. Orthop. Res. 9, 641–650 (1991).
Caplan, A. I. Mesenchymal stem cells: time to change the name! Stem Cells Transl Med. 6, 1445–1451 (2017).
Dominici, M. et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8, 315–317 (2006).
Horwitz, E. M. et al. Clarification of the nomenclature for MSC: The International Society for Cellular Therapy position statement. Cytotherapy 7, 393–395 (2005).
Bianco, P., Robey, P. G. & Simmons, P. J. Mesenchymal stem cells: revisiting history, concepts, and assays. Cell Stem Cell 2, 313–319 (2008).
Stappenbeck, T. S. & Miyoshi, H. The role of stromal stem cells in tissue regeneration and wound repair. Science 324, 1666–1669 (2009).
Galipeau, J. & Krampera, M. The challenge of defining mesenchymal stromal cell potency assays and their potential use as release criteria. Cytotherapy 17, 125–127 (2015).
Marks, P. W., Witten, C. M. & Califf, R. M. Clarifying stem-cell therapy’s benefits and risks. N. Engl. J. Med. 376, 1007–1009 (2017).
Prockop, D. J. et al. Defining the risks of mesenchymal stromal cell therapy. Cytotherapy 12, 576–578 (2010).
Toyserkani, N. M. et al. Concise review: a safety assessment of adipose-derived cell therapy in clinical trials: a systematic review of reported adverse events. Stem Cells Transl Med. 6, 1786–1794 (2017).
Vega, A. et al. Treatment of knee osteoarthritis with allogeneic bone marrow mesenchymal stem cells: a randomized controlled trial. Transplantation 99, 1681–1690 (2015).
Vangsness, C. T. J. et al. Adult human mesenchymal stem cells delivered via intra-articular injection to the knee following partial medial meniscectomy: a randomized, double-blind, controlled study. J. Bone Joint Surg. Am. 96, 90–98 (2014).
Trounson, A. & McDonald, C. Stem cell therapies in clinical trials: progress and challenges. Cell Stem Cell 17, 11–22 (2015).
McIntyre, J. A., Jones, I. A., Danilkovich, A. & Vangsness, C. T. The placenta: applications in orthopaedic sports medicine. Am. J. Sports Med. 122, 363546517697682 (2017).
Goldberg, A., Mitchell, K., Soans, J., Kim, L. & Zaidi, R. The use of mesenchymal stem cells for cartilage repair and regeneration: a systematic review. J. Orthop. Surg. Res. 12, 39 (2017).
Jones, I. A., Chen, X., Evseenko, D. & Vangsness, C. T. Nomenclature inconsistency and selective outcome reporting hinders our understanding of stem cell therapy for the knee. J. Bone Joint Surg. Am. (in the press).
Shkhyan, R. et al. Drug-induced modulation of gp130 signalling prevents articular cartilage degeneration and promotes repair. Ann. Rheum. Dis. 77, 760–769 (2018).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03513016 (2018).
Jeon, O. H. et al. Local clearance of senescent cells attenuates the development of post-traumatic osteoarthritis and creates a pro-regenerative environment. Nat. Med. 23, 775–781 (2017).
Lozada, C. J. et al. A double-blind, randomized, saline-controlled study of the efficacy and safety of co-administered intra-articular injections of Tr14 and Ze14 for treatment of painful osteoarthritis of the knee: the MOZArT trial. Eur. J. Integ. Med. 13, 54–63 (2017).
Lei, J., Priddy, L. B., Lim, J. J. & Koob, T. J. Dehydrated human amnion/chorion membrane (dHACM) allografts as a therapy for orthopedic tissue repair. Tech. Orthop. 32, 149–157 (2017).
Lei, J., Priddy, L. B., Lim, J. J., Massee, M. & Koob, T. J. Identification of extracellular matrix components and biological factors in micronized dehydrated human amnion/chorion membrane. Adv. Wound Care (New Rochelle) 6, 43–53 (2017).
Malarkey, M. A. Surgical biologics - untitled letter. FDA https://www.fda.gov/biologicsbloodvaccines/guidancecomplianceregulatoryinformation/complianceactivities/enforcement/untitledletters/ucm367184 (2013).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03485157 (2018).
Willett, N. J. et al. Intra-articular injection of micronized dehydrated human amnion/chorion membrane attenuates osteoarthritis development. Arthritis Res. Ther. 16, R47 (2014).
Shimonkevitz, R. et al. A diketopiperazine fragment of human serum albumin modulates T-lymphocyte cytokine production through RAP1. J. Trauma 64, 35–41 (2008).
Bar-Or, D. et al. A randomized clinical trial to evaluate two doses of an intra-articular injection of LMWF-5A in adults with pain due to osteoarthritis of the knee. PLoS ONE 9, e87910 (2014).
Schwappach, J., Dryden, S. M. & Salottolo, K. M. Preliminary trial of intra-articular LMWF-5A for osteoarthritis of the knee. Orthopedics 40, e49–e53 (2017).
Cole, B., McGrath, B., Salottolo, K. & Bar-Or, D. LMWF-5A for the treatment of severe osteoarthritis of the knee: integrated analysis of safety and efficacy. Orthopedics 41, e77–e83 (2018).
Ampio Pharmaceuticals. Ampio pharmaceuticals reports positive results for both primary and secondary endpoints of pivotal phase 3 trial of Ampion™ in severe osteoarthritis-of-the knee (OAK). Ampiopharma https://ampiopharma.com/news/ampio-pharmaceuticals-reports-positive-results-primary-secondary-endpoints-pivotal-phase-3-trial-ampion-severe-osteoarthritis-knee-oak/ (2017).
Bar-Or, D. et al. Low molecular weight fraction of commercial human serum albumin induces morphologic and transcriptional changes of bone marrow-derived mesenchymal stem cells. Stem Cells Transl Med. 4, 945–955 (2015).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03349645 (2017).
Hangody, L. et al. Intraarticular injection of a cross-linked sodium hyaluronate combined with triamcinolone hexacetonide (Cingal) to provide symptomatic relief of osteoarthritis of the knee: a randomized, double-blind, placebo-controlled multicenter clinical trial. Cartilage 89, 1947603517703732 (2017).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02381652 (2015).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03390036 (2018).
O’Shaughnessey, K. et al. Autologous protein solution prepared from the blood of osteoarthritic patients contains an enhanced profile of anti-inflammatory cytokines and anabolic growth factors. J. Orthopaed. Res. 32, 1349–1355 (2014).
Hix, J. et al. An autologous anti-inflammatory protein solution yielded a favorable safety profile and significant pain relief in an open-label pilot study of patients with osteoarthritis. Biores Open Access 6, 151–158 (2017).
King, W., Bendele, A., Marohl, T. & Woodell-May, J. Human blood-based anti-inflammatory solution inhibits osteoarthritis progression in a meniscal-tear rat study. J. Orthopaed. Res. 35, 2260–2268 (2017).
Wanstrath, A. W. et al. Evaluation of a single intra-articular injection of autologous protein solution for treatment of osteoarthritis in a canine population. Vet. Surg. 45, 764–774 (2016).
van Drumpt, R. A. M., van der Weegen, W., King, W., Toler, K. & Macenski, M. M. Safety and treatment effectiveness of a single autologous protein solution injection in patients with knee osteoarthritis. Biores Open Access 5, 261–268 (2016).
Kon, E., Engebretsen, L., Verdonk, P., Nehrer, S. & Filardo, G. Clinical outcomes of knee osteoarthritis treated with an autologous protein solution injection: a 1-year pilot double-blinded randomized controlled trial. Am. J. Sports Med. 46, 171–180 (2018).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02138890 (2016).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02905240 (2018).
Dell’accio, F. & Cailotto, F. Pharmacological blockade of the WNT-beta-catenin signaling: a possible first-in-kind DMOAD. Osteoarthr. Cartil. 26, 4–6 (2018).
Usami, Y., Gunawardena, A. T., Iwamoto, M. & Enomoto-Iwamoto, M. Wnt signaling in cartilage development and diseases: lessons from animal studies. Lab. Invest. 96, 186–196 (2016).
Deshmukh, V. et al. A small-molecule inhibitor of the Wnt pathway (SM04690) as a potential disease modifying agent for the treatment of osteoarthritis of the knee. Osteoarthr. Cartil. 26, 18–27 (2018).
Yasuhara, R. et al. Roles of β-catenin signaling in phenotypic expression and proliferation of articular cartilage superficial zone cells. Lab. Invest. 91, 1739–1752 (2011).
Zhu, M. et al. Inhibition of β-catenin signaling in articular chondrocytes results in articular cartilage destruction. Arthritis Rheum. 58, 2053–2064 (2008).
Yazici, Y. et al. A novel Wnt pathway inhibitor, SM04690, for the treatment of moderate to severe osteoarthritis of the knee: results of a 24-week, randomized, controlled, phase 1 study. Osteoarthr. Cartil. 25, 1598–1606 (2017).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03122860 (2018).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT02536833 (2018).
Jeyanesh, R. S. et al. Results from a 52-week, phase 2a study of an intra-articular, Wnt pathway inhibitor, SM04690, for knee osteoarthritis. Samumed https://www.samumed.com/medium/image/the-orthobiologic-institute-tobi-annual-symposium-06072018_318/view.aspx (2018).
Roemer, F. W. et al. Structural effects of sprifermin in knee osteoarthritis: a post-hoc analysis on cartilage and non-cartilaginous tissue alterations in a randomized controlled trial. BMC Musculoskelet. Disord. 17, 267 (2016).
Eckstein, F., Wirth, W., Guermazi, A., Maschek, S. & Aydemir, A. Brief report: intraarticular sprifermin not only increases cartilage thickness, but also reduces cartilage loss: location-independent post hoc analysis using magnetic resonance imaging. Arthritis Rheumatol. 67, 2916–2922 (2015).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT01919164 (2018).
Hochberg, M. et al. Efficacy and safety of intra-articular sprifermin in symptomatic radiographic knee osteoarthritis: results of the 2-year primary analysis from a 5-year randomised, placebo-controlled, phase II study [abstract]. Arthritis Rheumatol. 69 (Suppl. 10), 1L (2017).
Caterina, M. J. & Julius, D. The vanilloid receptor: a molecular gateway to the pain pathway. Annu. Rev. Neurosci. 24, 487–517 (2001).
Simone, D. A., Nolano, M., Johnson, T., Wendelschafer-Crabb, G. & Kennedy, W. R. Intradermal injection of capsaicin in humans produces degeneration and subsequent reinnervation of epidermal nerve fibers: correlation with sensory function. J. Neurosci. 18, 8947–8959 (1998).
Anand, P. & Bley, K. Topical capsaicin for pain management: therapeutic potential and mechanisms of action of the new high-concentration capsaicin 8% patch. Br. J. Anaesth. 107, 490–502 (2011).
Remadevi, R. & Szallisi, A. Adlea (ALGRX-4975), an injectable capsaicin (TRPV1 receptor agonist) formulation for longlasting pain relief. IDrugs 11, 120–132 (2008).
Stevens, R. et al. Efficacy and safety of CNTX-4975 in subjects with moderate to severe osteoarthritis knee pain: 24-week, randomized, double-blind, placebo-controlled, dose-ranging study. Ann. Rheum. Dis. 76 (Suppl. 2), 121–121 (2017).
Hanson, P. D. CNTX-4975 administration in subjects with knee pain associated with osteoarthritis: results of the randomized, double-blind, placebo-controlled, phase 2b TRIUMPH study. availclinical https://www.availclinical.com/wp-content/uploads/2012/02/OA-Double-Blind-Study-Results.pdf (2017).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03429049 (2018).
Lee, D. K. et al. Continuous transforming growth factor beta1 secretion by cell-mediated gene therapy maintains chondrocyte redifferentiation. Tissue Eng. 11, 310–318 (2005).
Ha, C.-W., Noh, M. J., Choi, K. B. & Lee, K. H. Initial phase I safety of retrovirally transduced human chondrocytes expressing transforming growth factor-beta-1 in degenerative arthritis patients. Cytotherapy 14, 247–256 (2012).
Cherian, J. J. et al. Preliminary results of a phase II randomized study to determine the efficacy and safety of genetically engineered allogeneic human chondrocytes expressing TGF-β1 in patients with grade 3 chronic degenerative joint disease of the knee. Osteoarthr. Cartil. 23, 2109–2118 (2015).
Guermazi, A. et al. Structural effects of intra-articular TGF-β1 in moderate to advanced knee osteoarthritis: MRI-based assessment in a randomized controlled trial. BMC Musculoskelet. Disord. 18, 461 (2017).
Kim, M.-K. et al. A multicenter, double-blind, phase III clinical trial to evaluate the efficacy and safety of a cell and gene therapy in knee osteoarthritis patients. Hum. Gene Ther. Clin. Dev. 29, 48–59 (2018).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03203330 (2018).
Food and Drug Administration. Drug approval package: ZILRETTA (triamcinolone acetonide). FDA https://www.accessdata.fda.gov/drugsatfda_docs/nda/2017/208845Orig1s000TOC.cfm (2017).
Kraus, V. B. et al. Synovial and systemic pharmacokinetics (PK) of triamcinolone acetonide (TA) following intra-articular (IA) injection of an extended-release microsphere-based formulation (FX006) or standard crystalline suspension in patients with knee osteoarthritis (OA). Osteoarthr. Cartil. 26, 34–42 (2018).
Bodick, N. et al. An intra-articular, extended-release formulation of triamcinolone acetonide prolongs and amplifies analgesic effect in patients with osteoarthritis of the knee: a randomized clinical trial. J. Bone Joint Surg. Am. 97, 877–888 (2015).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT01487161 (2018).
Conaghan, P. G. et al. Brief report: a phase IIb trial of a novel extended-release microsphere formulation of triamcinolone acetonide for intraarticular injection in knee osteoarthritis. Arthritis Rheumatol. 70, 204–211 (2018).
Conaghan, P. G. et al. Effects of a single intra-articular injection of a microsphere formulation of triamcinolone acetonide on knee osteoarthritis pain: a double-blinded, randomized, placebo-controlled, multinational study. J. Bone Joint Surg. Am. 100, 666–677 (2018).
Bianco, P. et al. The meaning, the sense and the significance: translating the science of mesenchymal stem cells into medicine. Nat. Med. 19, 35–42 (2013).
Prockop, D. J. Repair of tissues by adult stem/progenitor cells (MSCs): controversies, myths, and changing paradigms. Mol. Ther. 17, 939–946 (2009).
Bravery, C. A. et al. Potency assay development for cellular therapy products: an ISCT review of the requirements and experiences in the industry. Cytotherapy 15, 9–19 (2013).
Acknowledgements
The work of the authors was supported by grants UL1TR001855 and UL1TR000130 from the National Center for Advancing Translational Science (NCATS) of the US National Institutes of Health. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Reviewer information
Nature Reviews Rheumatology thanks C. Evans, D. Hunter and A. Migliore for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
All authors researched data for the article, made a substantial contribution to discussions of content, wrote the article and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
C.T.V.Jr. declares that he holds shares in CarthroniX Inc. and in Parcus Medical. The other authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jones, I.A., Togashi, R., Wilson, M.L. et al. Intra-articular treatment options for knee osteoarthritis. Nat Rev Rheumatol 15, 77–90 (2019). https://doi.org/10.1038/s41584-018-0123-4
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41584-018-0123-4
This article is cited by
-
M2 macrophage-derived exosomal miR-26b-5p regulates macrophage polarization and chondrocyte hypertrophy by targeting TLR3 and COL10A1 to alleviate osteoarthritis
Journal of Nanobiotechnology (2024)
-
Zhuifeng Tougu capsules in the treatment of knee osteoarthritis (cold dampness obstruction syndrome): a randomized, double blind, multicenter clinical study
Chinese Medicine (2024)
-
H3K36 methyltransferase NSD1 protects against osteoarthritis through regulating chondrocyte differentiation and cartilage homeostasis
Cell Death & Differentiation (2024)
-
Atorvastatin loaded lecithin-coated zein nanoparticles based thermogel for the intra-articular management of osteoarthritis: in-silico, in-vitro, and in-vivo studies
Journal of Pharmaceutical Investigation (2024)
-
Tribological behavior of shape-specific microplate-enriched synovial fluids on a linear two-axis tribometer
Friction (2024)