Abstract
Social determinants of health are the conditions in which people are born, grow, live, work and age. These circumstances are the non-medical factors that influence health outcomes. Evidence indicates that health behaviours, comorbidities and disease-modifying therapies all contribute to multiple sclerosis (MS) outcomes; however, our knowledge of the effects of social determinants — that is, the ‘risks of risks’ — on health has not yet changed our approach to MS. Assessing and addressing social determinants of health could fundamentally improve health and health care in MS; this approach has already been successful in improving outcomes in other chronic diseases. In this narrative Review, we identify and discuss the body of evidence supporting an effect of many social determinants of health, including racial background, employment and social support, on MS outcomes. It must be noted that many of the published studies were subject to bias, and screening tools and/or practical interventions that address these social determinants are, for the most part, lacking. The existing work does not fully explore the potential bidirectional and complex relationships between social determinants of health and MS, and the interpretation of findings is complicated by the interactions and intersections among many of the identified determinants. On the basis of the reviewed literature, we consider that, if effective interventions targeting social determinants of health were available, they could have substantial effects on MS outcomes. Therefore, funding for and focused design of studies to evaluate and address social determinants of health are urgently needed.
Key points
-
Addressing an individual’s social determinants of health — that is, the conditions under which they are born, grow, live, work and age — could provide opportunities to reduce the burden of living with multiple sclerosis (MS).
-
Individual factors that may influence MS-related outcomes include sex, gender and sexuality, race and ethnicity, education and employment, socioeconomic status, and domestic abuse.
-
Societal infrastructures, including access to food, health care and social support, can also affect MS-related outcomes.
-
Awareness of the specific circumstances of a patient with MS might help neurologists deliver better care.
-
Social determinants of health are not static and can change according to wider sociopolitical contexts, as highlighted by the COVID-19 pandemic.
-
Rigorous studies of interventions to ameliorate the effects of poor social determinants on people with MS are urgently needed.
Similar content being viewed by others
Introduction
As defined by the WHO, social determinants of health are the conditions under which people are born, grow, live, work, and age (Fig. 1). These conditions are shaped by the distribution of economy, governance and resources at the global, national and local levels. They are also responsible for health inequities and avoidable differences in health status. Social determinants can be more important than health care or lifestyle choices in influencing health, and it has been suggested that social determinants of health account for 30–55% of health outcomes.
Social determinants of health are the conditions in which people are born, grow, live, work and age. They are non-medical factors that influence health outcomes through a wide-reaching influence on all aspects of life. Social determinants of health can be divided into two categories: individual factors and structural determinants. Individual factors (for example, gender, race and ethnicity) have an effect via societal inequalities and structural determinants (such as health-care access and social support), which in turn affect health through their influence on the individual.
Multiple sclerosis (MS) affects over 2.8 million people worldwide and is widely acknowledged to be highly heterogeneous1. The disease is thought to develop as a result of environmental exposures in genetically susceptible people2. Over the past 20 years, the number of disease-modifying therapies available for the treatment of MS has rapidly increased and the emphasis on multidisciplinary health-care management has grown; however, a cure remains elusive. Disease-modifying therapies have had a considerable effect on long-term disease outcomes, with the natural history of MS changing substantially over the past 20 years3. Most neurologists use physical signs and symptoms, and (visible) MRI brain lesions to estimate a person’s risk of ongoing disease activity, to direct treatment (including disease-modifying therapies) and to measure outcomes. However, addressing an individual’s social determinants of health has the potential to provide additional opportunities to reduce the burden of living with MS.
Despite the growing recognition of the importance of social determinants of health, little progress has been made towards addressing these determinants in people living with MS. Emerging data suggest that the cumulative effects of exposure to social and environmental stressors can manifest in later adulthood and have a negative effect on general and brain health4. A holistic approach that includes consideration of social determinants of health, which can be considered the ‘risks of risks’, offers the potential for opportunities to fundamentally improve health and health care in MS and other neurological diseases.
Although some social determinants of health, such as employment status, have already been investigated in the context of MS, the MS-specific evidence regarding other social determinants of health is of variable quality and quantity, limiting the interpretation of some findings. Nevertheless, we can learn a lot from looking at the wider public health environment — strategies that have been shown to improve general health status by modifying social determinants of health can also be applied to the management of MS. In this Review, we aim to provide an overview of the current literature about the effect of social determinants of health on MS outcomes to increase awareness and encourage high quality research on this topic. We also highlight potential bidirectional relationships between MS outcomes and social determinants of health. We conclude by providing recommendations on how neurologists and the wider clinical team might assess and address social determinants of health in practice, as the first step in managing the influence of these factors on MS care.
Social determinants of health
Social determinants of health can be classified in several ways but for the purposes of this Review we divide them into two categories: individual factors and structural determinants. Individual factors include characteristics such as gender, race and ethnicity that have an effect on health via an interaction with structural or societal inequalities. Structural determinants are societal infrastructures that influence health; for example, health-care access and social support. Importantly, these two categories are not always clearly divided and bidirectional influences exist between individual factors and structural determinants. For example, a person’s individual circumstances (such as racial background) can influence their place in society and potentially their access to services such as health care. Furthermore, a person’s access to services and infrastructure such as health care or social support can influence how much adverse personal circumstances such as employment status might affect their health.
For the purposes of this Review, we focus on individual-level MS-related outcomes, including clinical (relapses, disability, cognition), radiological (MRI) and patient-reported (quality of life and effect of disease) outcomes. To maintain a clear focus on the person with MS, we do not discuss societal outcomes, such as health economic findings. We review the literature on a range of social determinants of health including gender, race, education, employment, domestic abuse, socioeconomic status, health-care access, food disparities, neighbourhood environment and pollution, social support, and COVID-19 in relation to MS diagnosis, disease progression and disability.
Individual factors
Sex, gender and sexuality
MS is more common in women than in men and the sex ratio seems to be widening5. The characteristics of the disease also seem to differ between men and women6; however, a detailed description of these epidemiological observations and their potential biological underpinnings is outside the scope of this Review.
The effect of MS on quality of life seems to vary between men and women. Among people with MS, evidence suggests that women report worse fatigue and anxiety than men, whereas men report greater limitations in walking, dexterity and emotional roles than women7,8. In one study, the relationship between Expanded Disability Status Scale (EDSS) scores and the patient-reported Multiple Sclerosis Quality of Life-54 (MSQOL-54) instrument differed between men and women, suggesting that the relationship between the physical aspects of MS and quality of life is weaker in women than in men8. That societal influences have a role in this gender difference seems highly likely; however, unpicking such relationships is complex and studies have not yet fully addressed this question. It should be noted that the social construct of gender is more complex than a binary biological variable. In the studies described above, researchers focused on cisgender men and women, and a wider scope of study is required to represent all people living with MS.
Sexual and gender minority (SGM) people face unique obstacles in accessing quality health care, which subsequently affects disease-related outcomes9. The effect of intersectionality between chronic neurological disease and sexual and/or gender minoritization has been poorly studied. One relatively small study performed in San Francisco, which examined people who were at risk of sexual and/or gender minoritization, found that the majority of SGM people living with MS reported that their gender identity or sexual orientation did not affect their health care9. Although most of the participants felt comfortable discussing their sexuality or gender identity with their physician, a few reported homophobia or gender discrimination from health-care professionals, limiting their engagement with care and hence their potential access to disease-modifying therapy. Very few participants reported taking part in either SGM or MS support groups9. In a second small study, compared with cisgender participants, transgender participants reported that they were less comfortable discussing sexual health with their doctor, which could affect their quality of life10. From the studies performed to date, there do seem to be differences between gender groups in terms of how MS affects people and how it might influence their interactions with health-care providers. Further work is required to ensure that the effect of gender on MS is better understood, and that services are able to provide equitable and effective care for all people living with MS.
Race and ethnicity
Interest in the relationship between racial and ethnic background and MS outcomes is increasing, particularly in the USA. Several studies have identified worse clinical outcomes in Black, Hispanic and Latinx people with MS than in white people with MS; these observed differences are unlikely to be solely genetic in origin and are far more likely to result from systemic racism across health and other services11. The magnitude of racial and ethnic influences on social determinants of health are likely to differ across countries and regions; these geographic discrepancies must be considered when attempting to draw population-level conclusions12.
Although MS was historically thought to be most common in white people, evidence now indicates that it occurs at higher frequency in minoritized racial or ethnic populations than previously thought13. In the USA, strong correlations exist between race, health-care access and socioeconomic status. Also in the USA, systemic differences in health-care access, socioeconomic inequalities, cognitive biases and racism within health care have been shown to have a role in poorer disease-related outcomes in people from minoritized racial and ethnic groups across multiple diseases14. A multicentre, retrospective study published in 2004, was one of the first to extensively characterize MS in Black Americans15. Compared with white Americans, Black Americans in this study had a slightly older age at onset and a higher prevalence of opticospinal disease, with more rapid disease progression and shorter time to an EDSS score of 6.0. In support of these clinical observations, a longitudinal study in people with MS identified more rapid brain and retinal atrophy in Americans from African ancestral backgrounds than Americans from European ancestral backgrounds16.
A more recent study compared MS mortality rates among five groups that the authors defined by ethnicity and race: non-Hispanic white, non-Hispanic Black, non-Hispanic Asian or Pacific Islander, non-Hispanic American Indian or Alaska Native, and Hispanic17. Among individuals aged under 55 years, non-Hispanic Black Americans had the highest MS mortality rate of all these groups. In another single-centre study, decreased cortical thickness, decreased subcortical volume and decreased cognitive scores were observed in Black Americans with MS compared with white Americans with MS18. Some of these disparities in outcome might be partially explained by disparities in age at disease onset — later disease onset is a known indicator of poor prognosis. Furthermore, compared with white people, Hispanic people were less likely to present with late-onset MS, but more likely to present with motor symptoms at onset, another poor prognostic indicator19. Confounding factors including diagnostic delay, selection bias and other socioeconomic factors, which were not fully addressed in the studies discussed above, are likely to contribute to racial disparities in MS outcome15.
Despite progress in understanding MS in diverse populations, substantial gaps in our knowledge remain. Barriers to filling these gaps include low enrolment of minoritized populations in clinical trials and substantial limitations to many of the current datasets. For example, much of the existing data is retrospective and focuses on measures of physical disability. Research examining other measures such as cognitive dysfunction and brain changes on MRI often have small sample sizes and do not control for socioeconomic status and other social determinants of health, which are inextricably linked to race and might affect outcomes. Furthermore, reference scores and norms used in tests such as detailed cognitive assessments are often based on white control populations. For example, a study examining early cognitive dysfunction in MS used healthy control groups consisting of Black and Hispanic people and found no significant difference in oral Symbol Digit Modalities Test (SDMT) scores between participants with early MS and healthy participants with the same racial background20. Importantly, overall scores were lower in Black and Hispanic people than white people (both healthy controls and participants with MS), possibly a result of the influence of race on other social determinants of health such as educational attainment and socioeconomic status.
In a number of US-based military studies, data on service-connected disability were used to identify people with MS — MS is considered a service-connected disability when it manifests during or within 7 years of military service21. However, receiving a service-connected MS diagnosis is likely to be more difficult for Black people owing to delays caused by racism and inequality within the health-care system. This means that within US military cohorts — often the most complete in terms of data, and used to understand the influence of race22 — biases unrelated to MS could influence findings including those related to MS incidence and prevalence, and age and disability at diagnosis. Existing studies focus on countries without universal health-care systems and with majority white populations. This narrow focus leaves considerable gaps in our knowledge when it comes to non-white-majority countries and those with universal health-care systems, which are still vulnerable to racial biases23.
Education
Evidence suggests that level of education has an influence on clinical outcomes related to MS, but few MS-specific studies have examined the effect of education on patient-reported or health economic outcomes, as discussed in more detail below. Education precedes and influences occupation, income and often wealth; in some studies it is considered a proxy measure of socioeconomic status. Measures of educational level, commonly completion of high school (12 years of schooling in most countries), have been widely used in MS research, and the results of these studies suggest that higher levels of education are protective against disability progression in people with relapsing MS. For example, in a study of 1,372 Belgian people with relapse-onset MS, participants with <12 years of formal education had a higher risk of reaching an EDSS score of 6.0 than participants with >12 years of formal education in a Cox proportional hazards model adjusted for gender, age, age at onset and disease-modifying therapy, although this relationship was not observed in participants with progressive-onset MS24. Similarly, in another study, a lower level of education in Brazilian people with MS was associated with higher EDSS scores, longer disease duration and a higher T2 lesion load25.
However, all of the studies examining links between education and MS outcomes are limited by their design; as with all case–control studies they are subject to ascertainment bias and involve analysis of selected retrospective data. First, reverse causation might explain some of the observed differences, so prospective longitudinal studies are needed to investigate this possibility. Second, low levels of education are associated with exposure to a range of factors that increase the risk of MS and of worse disease outcomes. Such factors include smoking, low levels of health literacy, lack of employment and low socioeconomic status, and the studies performed so far have not been designed in a way that enables researchers to dissect out the contribution of these different relationships. Third, the studies performed to date focused on years of education, whereas quality of education has not been studied in any meaningful way. Last, it is possible that prodromal MS influences educational achievement26 and thus limits access to higher levels of education, which would place people with earlier MS onset at an educational disadvantage.
Employment
Employment is crucially important when considering population health and health inequalities; however, the relationship between employment status and health or chronic disease is complex and bidirectional. Exclusion from the workplace results in material deprivation, and can adversely affect social status and identity27. As we discuss in this section, few studies have examined the effect of unemployment on health outcomes in MS; however, greater disability, as measured by EDSS, has been consistently associated with lower rates of employment28,29. The strength of this relationship varies between and within countries, and more recent data suggest a narrowing in the difference in employment rates between people with and without MS30. Evidence indicates that higher EDSS scores, fatigue31 and cognitive impairment32 are independently associated with a greater likelihood of unemployment in people with MS33, whereas clinical stability is associated with a reduced risk of leaving employment34,35. Progressive MS is associated with a higher risk of leaving employment than relapsing MS29,36,37. Unemployed people with MS seem to have a higher number of physical comorbidities than employed people with MS38; however, the results of one study suggest that this difference is substantially reduced after adjustment for MS symptom severity, suggesting that the comorbidities and MS symptoms do not act independently37. Furthermore, most studies performed to date compared sociodemographic, clinical and psychosocial variables between employed and unemployed people with MS, using employment status as the outcome variable, which means they did not examine the true complexity of any relationship.
In one study, people with MS who were not working at 10 years after diagnosis had a significant reduction in functioning (in terms of bodily function, as well as activities and participation in activities of daily life), an increased self-reported effect of MS and decreased fine hand function compared with people with MS who were working at this time point39. Another cross-sectional study identified increased perceived stress, reduced self-reported physical and mental health related quality of life, and decreased life satisfaction in unemployed people with MS compared with employed people with MS40. The results of another study indicate that employment status is the most important variable for predicting mental health status in people with MS under 45 years of age41. Similar to education, we note that employment status is associated with a number of risk factors for MS development and subsequent disability such as smoking and low health-care literacy; however, the studies performed to date have not addressed this relationship.
Evidence indicates that other social determinants of health interact with the relationship between employment and MS. For example, younger age and higher education level are consistently associated with a higher employment rate in people living with MS29,36, and in one study a high frequency of social or lifestyle activities at baseline was associated with a greater likelihood of being employed 10 years later31. Studies that investigated sex differences in the likelihood of leaving employment as a result of MS reported a range of results, including no difference, greater likelihood in men and greater likelihood in women29,34,42. In a study of people with MS in the USA, non-Hispanic white people had higher employment rates (48%) than Hispanic people (45%) and non-Hispanic Black people (36%)43, highlighting the potential role of other sociodemographic factors in determining employment status.
Socioeconomic status
Socioeconomic status refers to relative position within the social hierarchy and is measured by indicators such as income, occupation and place of residence. Therefore, socioeconomic status draws on multiple social determinants of health, but it also exerts an independent effect. Evidence has shown that socioeconomic status has an effect on health across a wide range of indicators, settings and populations44. Although reducing socioeconomic inequalities in health is an international policy priority, large disparities persist in both countries with and countries without universal health-care systems45.
To date, studies investigating the relationship between socioeconomic status and MS have mainly focused on the risk of developing MS. Overall, findings are conflicting, with some studies finding an association between high socioeconomic status and risk of MS, some finding an association between low socioeconomic status and risk of MS, and others finding no association46,47. In a meta-analysis published in 2015, all the studies that identified a link between high socioeconomic status and MS risk were from countries that were considered to have more inequality; a potential explanation for this relationship could be differences in the skills that are required to navigate complex health-care systems or differences in insurance status in payer-based systems.
Available data regarding the effect of socioeconomic status on MS disability outcomes indicate a relationship between greater deprivation at disease onset and greater disability even in countries with a universal health-care system, including a higher risk of reaching EDSS scores of 4.0 and 6.0 in Cox proportional hazards models46,48, faster retinal neurodegeneration49 and onset of secondary progression46. Evidence also indicates that higher socioeconomic status in people with MS is associated with a lower burden of psychiatric symptoms and a higher likelihood of symptom recovery following mental health treatment50,51.
In regions without universal health care, lower socioeconomic status is associated with reduced access to highly effective disease-modifying therapy for MS52. People living in poverty are less likely than other people to be able to access insurance systems that cover comprehensive disease-modifying therapy, and large studies have shown a direct effect of this disparity on cancer outcomes53. Therefore, the relationship between socioeconomic status and disability in MS could be mediated by access to disease-modifying therapy. However, this hypothesis is still a matter of debate and the mechanisms underlying the relationship are likely to vary substantially within and between geographical regions. The results of some studies indicate that, in countries with a universal health-care system, people with MS with higher socioeconomic status are more likely to be prescribed disease-modifying therapy and less likely to experience delays in disease-modifying therapy escalation than people with lower socioeconomic status54,55,56; however, other studies have found no evidence to support this conclusion57,58. These contrasting results are likely to be related to the specific scope and limitations of individual studies, along with differences in local prescribing ‘cultures’. Evidence also suggests that socioeconomic status-related disparities in disease severity, health-care access and literacy can affect prescribing decisions in MS54,57,58; however, research into ways to overcome barriers and/or enact local change is lacking.
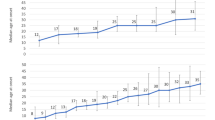
Substantial associations exist between socioeconomic status and MS disability risk factors, such as smoking, obesity and comorbid disease, which might influence any observed relationship between socioeconomic status and disability outcomes. Most studies that examine the relationship between socioeconomic status and MS diagnosis or disability outcomes do not control for these risk factors59. As mentioned above, comorbidities have been associated with poorer long term outcomes in MS60; actively addressing these, especially in more deprived populations, is a potential means through which MS outcomes could be improved. The relationship between socioeconomic status and MS diagnosis and disability is not unidirectional; evidence from the UK MS Register indicates that MS restricts social and economic opportunities, even several years before diagnosis61 (Fig. 2). Critical study of the timing and mechanism(s) through which socioeconomic factors might exert their influence on MS outcomes, along with means by which neurology teams can intervene to ameliorate these, thus has the potential to markedly change outcomes for many people living with MS.
Many social determinants of health interact and intersect with each other, leading to poorer outcomes, in either an additive or even a multiplicative manner. There are potential further interactions between living with chronic multiple sclerosis symptoms such as cognitive impairment and bladder or bowel impairment, and social determinants of health. Multiple sclerosis and its symptoms might reduce an individual’s social determinants of health, particularly those related to employment and social isolation, which might then amplify the effect of multiple sclerosis. Studying this vicious cycle is complex owing to the multiple and varying influences that exist at both the individual and group level.
Domestic abuse
Domestic abuse is defined as “a pattern of behaviour in any relationship that is used to gain or maintain power and control over an intimate partner”, which can be “physical, sexual, emotional, economic or psychological actions or threats of actions that influence another person”62. This abuse has a serious effect on the individual, the family and the health-care system; however, no data on domestic abuse and disease-related outcomes in MS have been published to date.
According to data from Public Health England, people with disabilities experience disproportionately higher rates of domestic abuse over a longer period of time, with greater severity and frequency, than non-disabled people63. In addition to practices such as gaslighting and physical abuse, less widely recognized forms of abuse, such as ridiculing or physical neglect, have been reported64. Domestic abuse can involve a range of people including intimate partners, family members and carers, and disabled women are much more likely to experience abuse than disabled men63. In a survey of US adults with advanced MS, more than half of the respondents reported abuse from their caregivers65, and the WHO has identified substantial barriers to disabled people seeking support after abuse66. Further research is needed to understand the best and most sensitive means of applying this knowledge across clinical practice in MS; although this is a challenging area, given the potential risk that people living with MS are at, it is clearly important.
Intermediate determinants
Health-care access
Health care for people living with MS includes not only care associated with MS management, but also care of any comorbidities, health screening and preventive care, and access to services for transient acute health issues. Studies of health-care access that consider the progression of MS as an outcome of interest have investigated access and the use of neurologists67, investigation and treatment of MS-related bladder symptoms68, and the use of disease-modifying therapy58,69. Other studies have investigated access to cancer screening, management of hypertension and osteoporosis in women with severe MS70, general health needs71 and social support72; studies addressing health care are discussed in more detail below.
In a US-based study, participants with lower levels of MS-related disability were more likely to receive their usual care directly from a neurologist, and those with higher disability were less likely to receive medical care67. In another study, women with an EDSS score of ≥7 had an uptake of breast, ovarian and colorectal cancer screening tests that was far below the general population average in the USA70. Although this study did not include people with mild or moderate MS-related disability, this finding highlights an area of potential concern in comprehensive MS care. An important limitation of studies performed in the USA is that they primarily include participants who receive health care through a private health-care insurance system, meaning that those without health-care insurance are not studied. Studies of health-care needs in countries with a public or universal health-care system have identified health-care needs of people with MS outside MS-related specialists, tests or treatments. One such study found that overall health needs are not met as MS disability increases71; individuals with greater disability had greater unmet physiotherapy, occupational therapy and social needs.
Food access
Food poverty refers to the inability to acquire or consume an adequate quantity of nutritious food. In 2021, 8% of UK households were food insecure, and of this 4% were living in food poverty73. To date, no publications have described the effect of food poverty on MS disease activity or outcomes. However, the effect of dietary interventions on MS outcomes has been studied, with the overwhelming majority of studies examining food supplements rather than overall diet quality. An observational study identified an association between a healthier diet and higher mental and physical health quality of life scores; a dose–response relationship was observed between diet habits questionnaire score and quality of life score74. In a second study, healthier dietary intake on subscales for fibre, fruit and vegetables, and fat was associated with better quality of life scores75. However, this study identified no association between diet scores and disability. With all of these studies, participant bias, potential reverse causation and confounding are major concerns, and in 2020, a systematic review concluded that many of the studies investigating dietary interventions for MS had major problems with design or implementation that substantially limit their interpretation76.
Air pollution
Exposure to particulate matter via air pollution has been associated with poor brain health77; additionally it might lie on the MS causative pathway and/or trigger relapses due to pro-inflammatory influences78. Studies of the relationship between air pollution and MS outcomes have generally focused on ecological-level assessments and have reported modest but statistically significant negative effects. Outcomes that have been studied so far include relapses, EDSS score and new MRI lesions. Specific findings are discussed in more detail below.
Associations between air pollutants and MS outcomes have been identified in France79,80, Iran81, Israel82 and Italy83,84. These studies all studied particulate matter <10 µm (PM10) and were performed in locations that were generally less polluted with low levels of deprivation. In Lombardy, Italy, admissions to hospital for MS relapse increased by 42% when PM10 was in the highest quartile, with a maximal effect observed 0–7 days after exposure83. A study in France of 1,783 MS relapses in 424 participants with MS assessed the effects of PM10, NO2, and O3 (ozone) in a multi-pollutant model, but found a significant association between only MS relapses and O3 (ref.79). Another study in France with a case–crossover design in 536 people with MS found that PM10 concentrations were significantly increased in the days prior to clinical relapse onset compared with other time points80. In 287 Israeli people with MS, exposure to PM2.5 was independently associated with MS relapses in those who did not smoke; an inverse relationship was found between O3 exposure and relapses in participants <40 years old82. In Isfahan, Iran, increases in the air quality index — a measure of six air pollutants — were modestly associated with higher EDSS scores among people with MS81. Only one study examined the effect of pollution at the level of individual participants, finding that higher PM10 exposure was associated with gadolinium-enhancing lesions independent of smoking status, disease-modifying therapy and season84.
Overall, the relatively small number of studies, inconsistent inclusion of smoking status, different MS disease outcomes, and the older nature of several studies in locations with limited air pollution, make it difficult to draw any definitive conclusions on the effect of neighbourhood air pollution on MS outcomes. The complex association between poor air quality and deprivation85 adds to its strength as a social determinant of health; however, this specific relationship has not been studied in MS.
Social support
Social support can be tangible (for example, financial assistance) or intangible (for example, emotional support or companionship) and can come from many potential sources, including health-care providers, government-funded social support schemes, charitable organizations, family, friends, pets, neighbours and coworkers. MS is a disabling and stigmatizing disease that can lead to social isolation and exclusion86. People with MS report reduced social participation compared with before their diagnosis, owing to disability, physical barriers and often reduced financial resources87,88. Two studies found that people with MS who have cognitive impairment and reduced mobility have reduced social contacts, higher unemployment rates and lower standards of living than those without disability in these domains89,90. Other evidence indicates that MS symptoms, including bladder dysfunction, poor sleep, pain, spasticity and fatigue, negatively affect social interactions and quality of life91,92. People with MS also report changes in family relationships and friendships; for example, divorce, or needing support from family members to assist with activities of daily living90. One study found that even relatively mild MS-related disability has a negative effect on social activities, as measured by the Environmental Status Scale (ESS)93.
Evidence indicates that the social isolation and exclusion caused by MS can result in poor mental health, worse quality of life, and poor engagement with care94. In a study in 140 participants with MS, social isolation was associated with suicidal intent95, and in another study, higher social capital, which refers to the many resources derived from the social interaction between individuals and groups, was associated with lower self-reported physical and psychological effects of the disease96. The often intangible nature of social support can make it complex to study and develop interventions for; however, there seems to be an opportunity for further work in this area, with the potential to substantially improve quality of life for people with MS.
COVID-19
The effect of the COVID-19 pandemic on every facet of life cannot be underestimated. People with chronic diseases, including MS, experienced the pandemic differently from those without chronic diseases; health inequity between these two groups has been highlighted and exacerbated by the crisis. In the USA, evidence indicates that people with MS with poorer social determinants of health (that is, lower predicted health status) reported more depressive symptoms and worse general mental health in the midst of the pandemic97. In a US-based study, 69 people with MS were surveyed in mid-2020 and 20% of participants reported losing their job as a result of the pandemic98. Black participants, Hispanic and Latinx participants, and participants with lower levels of education seemed to have a greater risk of job loss than other participants. Studies performed in Spain and Australia found that lockdown and isolation precautions, including inability to go outside, led to reclusion and lack of outdoor walks, resulting in worse mental health among people with MS99,100. In Italy, a web-based survey performed during the pandemic found that people with MS reported significantly less social support, higher perceived stress and more depression than a control group of people without MS101. In one study, 52 of 324 participants with MS reported a positive effect of the COVID-19 pandemic on their quality of life, with strategies such as working from home allowing greater time and flexibility to overcome MS symptoms102.
Acting on the evidence
Addressing social determinants of health in MS is complex in clinical practice. Not only are there difficulties related to the variable quality of and biases within the literature, variation within different health-care systems and national contexts require careful consideration. Effecting change will require a multidisciplinary effort, including primary care providers and allied health-care professionals. Many of the steps required to assess and improve social determinants of health might seem to be outside the scope of individual neurologists, and this, together with time and service pressures, can mean that many of these determinants remain unidentified in clinical practice, and potentially modifiable risk factors are left unaddressed.
As neurologists, we increasingly understand that non-medical factors related to the individual and societal social context can have an effect on health. For example, findings from the wider public health literature have identified effects of structural and societal changes on population health103, and being aware of a patient’s specific circumstances might help the neurologist to deliver better care. However, population-level metrics do not directly translate to individual needs — living in a deprived area is not the same as being deprived — so identifying those at greatest need requires clinicians to actively enquire104. The Core-5 screening tool105 was developed to identify individuals with poor social determinants of health in health-care settings, and is way to identify those at greatest need of input. The tool was independently tested within both inpatient and outpatient settings; staff survey data indicated high acceptance and usability106. In Box 1, we suggest a short screening questionnaire, based on the Core-5 screening tool, that can be used to assess social determinants of health in people living with MS. Although not all of the questions are applicable across all health-care and welfare systems, they provide a framework for systematic inquiry to identify individuals with the greatest need of support.
Individual determinants
Sex, gender, sexuality, race, ethnicity
As discussed above, sex, gender, sexuality and race affect all aspects of health care. Addressing the effect of these factors within our individual clinical practices requires reflection and thought. There remains a belief among some clinicians that people from minoritized racial and ethnic populations are at lower risk of MS than those of white European ancestries; however, this is not necessarily the case14,107. We suggest that neurologists ensure that they consider MS in all individuals in whom the clinical history and investigations support the diagnosis, and consider auditing the time to diagnosis among different racial and ethnic groups. Algorithms for the treatment of MS exist in a number of public health-care systems108, have been recommended within mixed health-care systems109, and are recognized as an aspiration in private health-care systems52. Auditing practice against these algorithms might provide a practical benchmark for neurologists.
People from under-represented ethnic groups and genders might struggle to access and navigate health-care services equitably, and neurologists should ensure that their practice is inclusive and mindful of the difficulties that these individuals might encounter. Patient mistrust related to prior negative health-care experiences should also be recognized and addressed110. MS teams should advocate for, and support, all of their patients to have equal access to diagnostic and monitoring investigations through tailored support where necessary. We suggest that where neurologists are involved in recruitment to research studies, they should ensure that recruitment patterns from their centre match the demographic characteristics of their local population in terms of age, gender and race.
Risk of abuse
Given that individuals with MS are at higher risk of domestic and carer abuse than the general population, safety should routinely be enquired about, ideally as part of routine reviews. By embedding this inquiry within routine care, with appropriate training and education for those carrying out such reviews, biases leading to people at risk of abuse being either missed or singled out can be reduced. This approach has been successfully deployed in other areas of medical care111. Neurologists should be mindful of who accompanies people to their appointments, and ensure that they have the time and ability to ask and address this issue during the appointment. They should also be aware of how to raise safeguarding concerns.
Education
Most people with MS seen in adult services have completed their education at the time of diagnosis; however, some might still be in, or wish to return to, either full or part time education, and MS teams have an important role in supporting patients in this. MS teams also need to ascertain the educational level of individuals with MS to provide appropriate information and support for complex decision-making.
Employment
In contrast to many other social determinants of health, validated scales, such as the Multiple Sclerosis Work Instability Scale (MS-WIS)112 and the Buffalo Vocational Monitoring Survey (BVMS)113,114, can be used to identify individuals living with MS who are at higher risk of job loss. Early use of disease-modifying therapies in order to minimize the risk of cognitive impairment and disability is key in enabling people with MS to remain in employment.
The MS team should discuss with their patients the pros and cons of disclosing a diagnosis of MS to employers. A work instability review might be useful for some people with MS; those at high risk of unemployment should have targeted interventions to support job retention. Such interventions include effective symptom management115, optimal treatment of comorbidities37 and assessment of cognition, mood and self-efficacy32,116. Employment support including vocational services, flexibility in the workplace28,36 and balance between working and private life31 is important to enable individuals with MS to achieve a sustainable working life over time.
Intermediate determinants
Socioeconomic status
According to a systematic review published in 2021, socioeconomic inequalities in health-care access seem to be more prevalent for specialist visits than for primary care, and in non-universal health-care systems than in universal health-care systems117. Across Europe, people with a higher socioeconomic status are more likely to use health-care specialists; education and occupation are also important contributing factors118. Improving access to health care is a structural task beyond the remit of neurologists; however, neurologists working in private or mixed health-care systems might be able to help by exploring how financial considerations might limit health-care choices, and ensuring that where possible steps are taken to mitigate this limitation. Working with communities and charitable groups that support individuals facing challenges in navigating local health-care services can also help improve health outcomes119.
Neurologists and the wider MS team should be aware of local services that aim to support individuals at risk of food insecurity and food poverty. We suggest that raising awareness of these services within patient groups in a non-judgemental manner could be a practical step to address food poverty. Identifying individuals who might benefit from this type of support is not always straightforward, and simple interventions such as publicity or posters might substantially increase awareness among those in need.
Social prescribing
The aim of social prescribing is to connect patients to non-clinical services and support, and to give individuals the knowledge, skills, motivation and confidence to manage their own health and well-being120. Social prescribing has a limited but increasing evidence base. Professional society and patient advocacy resources could be provided to remind people with MS of their rights as employees, citizens and patients. However, as highlighted by some minoritized groups with MS, the response to such resources varies across individuals; people do not always want to be defined by their need for support9. Systems that have a broad approach to social prescribing121 are being studied to identify strategies to address some of these concerns; where available, MS teams are encouraged to take part in such studies.
Conclusions
Social determinants of health are not static, and change according to wider sociopolitical contexts — as highlighted by the COVID-19 pandemic. Some have argued that digital literacy could be an increasingly important social determinant of health122. The rapid move to online communication — both for health-care and wider purposes — that was caused by the COVID-19 pandemic has created substantial inequities with direct relevance to people living with chronic neurological conditions.
We do not address income directly as part of this Review. As with other social determinants, the relationship between income and MS is bidirectional that is, diagnosis of MS is associated with lower income123, and lower income is associated with worse health outcomes. This relationship is mediated via social determinants of health. In non-universal health-care systems, where people with MS might need to meet the cost of disease-modifying therapy, the high cost of these medications will adversely affect those on lower incomes. This means that these individuals will accrue the risk of worse disease outcomes owing to lack of treatment access as well as low income and often poor social determinants of health. Intersectionality, that is, the interactions among multiple social determinants of health, has been shown to be important in dictating outcomes in cancer53, and the same is likely to be true for MS. Other previously unidentified social determinants of health undoubtedly exist, but require rigorous research to investigate.
In our view, the existing evidence supports a potentially major effect of social determinants of health on outcomes in people with MS. However, the evidence is limited, and the potential bidirectional and complex relationships, which involve multiple confounding factors have not been adequately addressed. Rigorous studies of interventions to ameliorate the effect of poor social determinants of health are almost completely lacking, and this Review highlights an important and urgent need for these. The importance of minimizing the effect of MS through early effective treatment with disease-modifying therapies, and the subsequent downstream implications of such disability prevention should not be underestimated. In our opinion, it is possible to change poor MS disease outcomes via a holistic approach, targeting either in isolation might mean that opportunities to comprehensively modify disease outcomes are missed.
Although addressing many social determinants of health is outside the role of neurologists, it is increasingly clear that ignoring the societal context of someone living with MS would be to neglect a potentially substantial effect on disease outcomes. Treating inflammatory neurological disease without holistically considering the person means that we are only addressing one factor that affects MS disability, thus unintentionally putting people with MS at risk of poorer outcomes.
References
Multiple Sclerosis International Federation. Atlas of MS, 3rd edn. MS International Federation https://www.msif.org/wp-content/uploads/2020/12/Atlas-3rd-Edition-Epidemiology-report-EN-updated-30-9-20.pdf (2020).
Dobson, R. & Giovannoni, G. Multiple sclerosis–a review. Eur. J. Neurol. 26, 27–40 (2019).
Beiki, O., Frumento, P., Bottai, M., Manouchehrinia, A. & Hillert, J. Changes in the risk of reaching multiple sclerosis disability milestones in recent decades: A nationwide population-based cohort study in Sweden. JAMA Neurol. 76, 665–671 (2019).
Marshall, C. R., Noyce, A. J., Neligan, A. & Dobson, R. Brain health: the hidden casualty of a humanitarian crisis. Lancet Reg. Health Eur. 15, 100374 (2022).
Krysko, K. M. et al. Sex effects across the lifespan in women with multiple sclerosis. Ther. Adv. Neurol. Disord. 13, 1756286420936166 (2020).
Simmons, S. B., Schippling, S., Giovannoni, G. & Ontaneda, D. Predicting disability worsening in relapsing and progressive multiple sclerosis. Curr. Opin. Neurol. 34, 312–321 (2021).
Kister, I., Bacon, T. & Cutter, G. R. How multiple sclerosis symptoms vary by age, sex, and race/ethnicity. Neurol. Clin. Pract. 11, 335–341 (2021).
Miller, A. & Dishon, S. Health-related quality of life in multiple sclerosis: the impact of disability, gender and employment status. Qual. Life Res. 15, 259–271 (2006).
Anderson, A. et al. Experiences of sexual and gender minority people living with multiple sclerosis in Northern California: an exploratory study. Mult. Scler. Relat. Disord. 55, 103214 (2021).
Khayambashi, S. et al. Gender identity and sexual orientation affect health care satisfaction, but not utilization, in persons with multiple sclerosis. Mult. Scler. Relat. Disord. 37, 101440 (2020).
Jacobs, B. M. et al. Towards a global view of multiple sclerosis genetics. Nat. Rev. Neurol. https://doi.org/10.1038/s41582-022-00704-y (2022).
Lebrun, L. A. & LaVeist, T. A. Black/white racial disparities in health: a cross-country comparison of Canada and the United States. Arch. Intern. Med. 171, 1591–1593 (2011).
Langer-Gould, A. M., Gonzales, E. G., Smith, J. B., Li, B. H. & Nelson, L. M. Racial and ethnic disparities in multiple sclerosis prevalence. Neurology https://doi.org/10.1212/WNL.0000000000200151 (2022).
Amezcua, L., Rivera, V. M., Vazquez, T. C., Baezconde-Garbanati, L. & Langer-Gould, A. Health disparities, inequities, and social determinants of health in multiple sclerosis and related disorders in the US: a review. JAMA Neurol. 78, 1515–1524 (2021).
Cree, B. A. C. et al. Clinical characteristics of African Americans vs Caucasian Americans with multiple sclerosis. Neurology 63, 2039–2045 (2004).
Caldito, N. G. et al. Brain and retinal atrophy in African-Americans versus Caucasian-Americans with multiple sclerosis: a longitudinal study. Brain 141, 3115–3129 (2018).
Amezcua, L., Rivas, E., Joseph, S., Zhang, J. & Liu, L. Multiple sclerosis mortality by race/ethnicity, age, sex, and time period in the United States, 1999-2015. Neuroepidemiology 50, 35–40 (2018).
Bross, M. et al. Cortical surface thickness, subcortical volumes and disability between races in relapsing-remitting multiple sclerosis. Mult. Scler. Relat. Disord. 53, 103025 (2021).
Amezcua, L. & McCauley, J. L. Race and ethnicity on MS presentation and disease course. Mult. Scler. 26, 561–567 (2020).
Amezcua, L., Smith, J. B., Gonzales, E. G., Haraszti, S. & Langer-Gould, A. Race, ethnicity, and cognition in persons newly diagnosed with multiple sclerosis. Neurology 94, e1548–e1556 (2020).
US Department of Veterans Affairs. Multiple sclerosis centers of excellence. VA https://www.va.gov/MS/veterans/benefits/index.asp (2022).
Wallin, M. T. et al. The Gulf War era multiple sclerosis cohort: age and incidence rates by race, sex and service. Brain 135, 1778–1785 (2012).
Fernandez Turienzo, C. et al. Addressing inequities in maternal health among women living in communities of social disadvantage and ethnic diversity. BMC Public Health 21, 176 (2021).
D’hooghe, M. B., Haentjens, P., Van Remoortel, A., De Keyser, J. & Nagels, G. Self-reported levels of education and disability progression in multiple sclerosis. Acta Neurol. Scand. 134, 414–419 (2016).
Rimkus, C. et al. The protective effects of high-education levels on cognition in different stages of multiple sclerosis. Mult. Scler. Relat. Disord. 22, 41–48 (2018).
Marrie, R. A. et al. From the prodromal stage of multiple sclerosis to disease prevention. Nat. Rev. Neurol. https://doi.org/10.1038/s41582-022-00686-x (2022).
Bacci, S., Pigini, C., Seracini, M. & Minelli, L. Employment condition, economic deprivation and self-evaluated health in Europe: evidence from EU-SILC 2009–2012. Int. J. Environ. Res. Public Health 14, 143 (2017).
Moore, P. et al. Demographic and clinical factors associated with changes in employment in multiple sclerosis. Mult. Scler. 19, 1647–1654 (2013).
Pearson, J. F. et al. Multiple sclerosis impact on employment and income in New Zealand. Acta Neurol. Scand. 136, 223–232 (2017).
Van Dijk, P. A., Kirk-Brown, A. K., Taylor, B. & van der Mei, I. Closing the gap: longitudinal changes in employment for Australians with multiple sclerosis. Mult. Scler. 23, 1415–1423 (2017).
Forslin, M., Fink, K., Hammar, U., von Koch, L. & Johansson, S. Predictors for employment status in people with multiple sclerosis: a 10-year longitudinal observational study. Arch. Phys. Med. Rehabil. 99, 1483–1490 (2018).
D’hooghe, M. B. et al. Perceived neuropsychological impairment inversely related to self-reported health and employment in multiple sclerosis. Eur. J. Neurol. 26, 1447–1454 (2019).
van Gorp, D. A. M. et al. Cognitive functioning as a predictor of employment status in relapsing-remitting multiple sclerosis: a 2-year longitudinal study. Neurol. Sci. 40, 2555–2564 (2019).
Chen, J. et al. Risk factors for leaving employment due to multiple sclerosis and changes in risk over the past decades: using competing risk survival analysis. Mult. Scler. 27, 1250–1261 (2021).
Chalmer, T. A. et al. Clinically stable disease is associated with a lower risk of both income loss and disability pension for patients with multiple sclerosis. J. Neurol. Neurosurg. Psychiatry 91, 67–74 (2020).
Marck, C. H. et al. Predictors of change in employment status and associations with quality of life: a prospective international study of people with multiple sclerosis. J. Occup. Rehabil. 30, 105–114 (2020).
Chen, J. et al. Comorbidities are prevalent and detrimental for employment outcomes in people of working age with multiple sclerosis. Mult. Scler. 26, 1550–1559 (2020).
Renner, A., Baetge, S. J., Filser, M. & Penner, I.-K. Working ability in individuals with different disease courses of multiple sclerosis: factors beyond physical impairment. Mult. Scler. Relat. Disord. 46, 102559 (2020).
Conradsson, D. M. et al. Employment status of people with multiple sclerosis in relation to 10-year changes in functioning and perceived impact of the disease. Mult. Scler. Relat. Disord. 46, 102519 (2020).
Beier, M. et al. Relationship of perceived stress and employment status in individuals with multiple sclerosis. Work 62, 243–249 (2019).
Krokavcova, M. et al. Employment status and perceived health status in younger and older people with multiple sclerosis. Int. J. Rehabil. Res. 35, 40–47 (2012).
Lehmann, A. I. et al. Factors associated with employment and expected work retention among persons with multiple sclerosis: findings of a cross-sectional citizen science study. J. Neurol. 267, 3069–3082 (2020).
Krause, J. S., Rumrill, P., Dismuke-Greer, C. E. & Jarnecke, M. Quality employment outcomes after multiple sclerosis: a comparison of participants from a specialty hospital and the National MS Society. J. Vocat. Rehabil. 48, 177–186 (2018).
Frieden, T. R. The future of public health. N. Engl. J. Med. 373, 1748–1754 (2015).
Cookson, R. et al. Health equity indicators for the English NHS: a longitudinal whole-population study at the small-area level. Health Serv. Deliv. Res. 4, 1–224 (2016).
Harding, K. E. et al. Socioeconomic status and disability progression in multiple sclerosis: a multinational study. Neurology 92, e1497–e1506 (2019).
Goulden, R., Ibrahim, T. & Wolfson, C. Is high socioeconomic status a risk factor for multiple sclerosis? A systematic review. Eur. J. Neurol. 22, 899–911 (2015).
Calocer, F. et al. Socioeconomic deprivation increases the risk of disability in multiple sclerosis patients. Mult. Scler. Relat. Disord. 40, 101930 (2020).
Vasileiou, E. S. et al. Socioeconomic disparity is associated with faster retinal neurodegeneration in multiple sclerosis. Brain 144, 3664–3673 (2021).
Maldonado, D. A. P. et al. The impact of socioeconomic status on mental health and health-seeking behavior across race and ethnicity in a large multiple sclerosis cohort. Mult. Scler. Relat. Disord. 58, 103451 (2022).
Wang, Y. et al. Socioeconomic status and race are correlated with affective symptoms in multiple sclerosis. Mult. Scler. Relat. Disord. 41, 102010 (2020).
National Multiple Sclerosis Society. Access to high quality MS healthcare principles. National Multiple Sclerosis Society https://www.nationalmssociety.org/Get-Involved/Advocate-for-Change/Take-Action/Access-to-High-Quality-Healthcare/Access-to-High-Quality-MS-Healthcare-Principles (2022).
Leech, M. M., Weiss, J. E., Markey, C. & Loehrer, A. P. Influence of race, insurance, rurality, and socioeconomic status on equity of lung and colorectal cancer care. Ann. Surg. Oncol. 29, 3630–3639 (2022).
Calocer, F., Dejardin, O., Droulon, K., Launoy, G. & Defer, G. Socio-economic status influences access to second-line disease modifying treatment in relapsing remitting multiple sclerosis patients. PLoS ONE 13, e0191646 (2018).
Das, J. et al. The association between deprivation and the access to disease modifying therapies for multiple sclerosis: an England wide community-based study in the UK MS Register. Mult. Scler. Relat. Disord. 57, 103474 (2022).
Gómez-Figueroa, E. et al. Socioeconomic status and access to multiple sclerosis treatment in Mexico. Mult. Scler. Relat. Disord. 52, 102967 (2021).
Reyes, S. et al. Socioeconomic status and disease-modifying therapy prescribing patterns in people with multiple sclerosis. Mult. Scler. Relat. Disord. 41, 102024 (2020).
Flemmen, H. Ø. et al. The influence of socioeconomic factors on access to disease modifying treatment in a Norwegian multiple sclerosis cohort. Mult. Scler. Relat. Disord. 61, 103759 (2022).
Kivimäki, M. et al. Association between socioeconomic status and the development of mental and physical health conditions in adulthood: a multi-cohort study. Lancet Public Health 5, e140–e149 (2020).
Salter, A., Kowalec, K., Fitzgerald, K. C., Cutter, G. & Marrie, R. A. Comorbidity is associated with disease activity in MS: findings from the CombiRx trial. Neurology 95, e446–e456 (2020).
Jennum, P., Wanscher, B., Frederiksen, J. & Kjellberg, J. The socioeconomic consequences of multiple sclerosis: a controlled national study. Eur. Neuropsychopharmacol. 22, 36–43 (2012).
United Nations. What is domestic abuse? United Nations https://www.un.org/en/coronavirus/what-is-domestic-abuse (2022).
Public Health England. Disability and domestic abuse: risk, impacts and response. Public Health England https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/480942/Disability_and_domestic_abuse_topic_overview_FINAL.pdf (2015).
Cohen, M., Forte, T., Dumont, J., Hyman, I. & Romans, S. Adding insult to injury: intimate partner violence among women and men reporting activity limitations. Ann. Epidemiol. 16, 644–651 (2006).
Morrison, E. H., Sorkin, D., Mosqueda, L. & Ayutyanont, N. Abuse and neglect of people with multiple sclerosis: a survey with the North American Research Committee on Multiple Sclerosis (NARCOMS). Mult. Scler. Relat. Disord. 46, 102530 (2020).
World Health Organization. World report on disability. WHO https://www.who.int/teams/noncommunicable-diseases/sensory-functions-disability-and-rehabilitation/world-report-on-disability (2011).
Minden, S. L. et al. Access to and utilization of neurologists by people with multiple sclerosis. Neurology 70, 1141–1149 (2008).
Marrie, R. A., Cutter, G., Tyry, T., Vollmer, T. & Campagnolo, D. Disparities in the management of multiple sclerosis-related bladder symptoms. Neurology 68, 1971–1978 (2007).
Li, P. et al. Disease-modifying therapy adherence and associated factors in a national sample of Medicare patients with multiple sclerosis. Value Health 23, 328–334 (2020).
Dobos, K., Healy, B. & Houtchens, M. Access to preventive health care in severely disabled women with multiple sclerosis. Int. J. MS Care 17, 200–205 (2015).
Lonergan, R. et al. Unmet needs of multiple sclerosis patients in the community. Mult. Scler. Relat. Disord. 4, 144–150 (2015).
Bo, M. et al. Access to social security benefits among multiple sclerosis patients in Italy: a cross-sectional study. Mult. Scler. Relat. Disord. 24, 107–112 (2018).
Department for Environment Food & Rural Affairs. United Kingdom Food Security Report 2021: Theme 4: Food security at household level. GOV.UK https://www.gov.uk/government/statistics/united-kingdom-food-security-report-2021/united-kingdom-food-security-report-2021-theme-4-food-security-at-household-level (2021).
Simpson-Yap, S., Nag, N., Probst, Y., Jelinek, G. & Neate, S. Higher-quality diet and non-consumption of meat are associated with less self-determined disability progression in people with multiple sclerosis: a longitudinal cohort study. Eur. J. Neurol. 29, 225–236 (2022).
Marck, C. H., Probst, Y., Chen, J., Taylor, B. & van der Mei, I. Dietary patterns and associations with health outcomes in Australian people with multiple sclerosis. Eur. J. Clin. Nutr. 75, 1506–1514 (2021).
Parks, N. E., Jackson-Tarlton, C. S., Vacchi, L., Merdad, R. & Johnston, B. C. Dietary interventions for multiple sclerosis-related outcomes. Cochrane Database Syst. Rev. 5, CD004192 (2020).
Erickson, L. D., Gale, S. D., Anderson, J. E., Brown, B. L. & Hedges, D. W. Association between exposure to air pollution and total gray matter and total white matter volumes in adults: a cross-sectional study. Brain Sci. 10, 164 (2020).
Ziaei, A. et al. Gene-environment interactions increase the risk of pediatric-onset multiple sclerosis associated with ozone pollution. Mult. Scler. 28, 1330–1339 (2022).
Jeanjean, M. et al. Ozone, NO and PM are associated with the occurrence of multiple sclerosis relapses. Evidence from seasonal multi-pollutant analyses. Environ. Res. 163, 43–52 (2018).
Roux, J. et al. Air pollution by particulate matter PM10 may trigger multiple sclerosis relapses. Environ. Res. 156, 404–410 (2017).
Ashtari, F. et al. An 8-year study of people with multiple sclerosis in Isfahan, Iran: association between environmental air pollutants and severity of disease. J. Neuroimmunol. 319, 106–111 (2018).
Elgabsi, M. et al. An impact of air pollution on moderate to severe relapses among multiple sclerosis patients. Mult. Scler. Relat. Disord. 53, 103043 (2021).
Angelici, L. et al. Effects of particulate matter exposure on multiple sclerosis hospital admission in Lombardy region, Italy. Environ. Res. 145, 68–73 (2016).
Bergamaschi, R. et al. Air pollution is associated to the multiple sclerosis inflammatory activity as measured by brain MRI. Mult. Scler. J. 24, 1578–1584 (2018).
Tonne, C. et al. Socioeconomic and ethnic inequalities in exposure to air and noise pollution in London. Environ. Int. 115, 170–179 (2018).
Freeman, J., Gorst, T., Gunn, H. & Robens, S. “A non-person to the rest of the world”: experiences of social isolation amongst severely impaired people with multiple sclerosis. Disabil. Rehabil. 42, 2295–2303 (2020).
Gallagher, P. & Mulvany, F. Levels of ability and functioning: using the WHODAS II in an Irish context. Disabil. Rehabil. 26, 506–517 (2004).
Yorkston, K. M. et al. Measuring participation in people living with multiple sclerosis: a comparison of self-reported frequency, importance and self-efficacy. Disabil. Rehabil. 30, 88–97 (2008).
Tyszka, A. C. & Farber, R. S. Exploring the relation of health-promoting behaviors to role participation and health-related quality of life in women with multiple sclerosis: a pilot study. Am. J. Occup. Ther. 64, 650–659 (2010).
Tabuteau-Harrison, S. L., Haslam, C. & Mewse, A. J. Adjusting to living with multiple sclerosis: the role of social groups. Neuropsychol. Rehabil. 26, 36–59 (2016).
Moriya, R. & Kutsumi, M. Fatigue in Japanese people with multiple sclerosis. Nurs. Health Sci. 12, 421–428 (2010).
Irvine, H., Davidson, C., Hoy, K. & Lowe-Strong, A. Psychosocial adjustment to multiple sclerosis: exploration of identity redefinition. Disabil. Rehabil. 31, 599–606 (2009).
Patti, F. et al. Longitudinal changes in social functioning in mildly disabled patients with relapsing-remitting multiple sclerosis receiving subcutaneous interferon β-1a: results from the COGIMUS (COGnitive Impairment in MUltiple Sclerosis) study (II). Qual. Life Res. 21, 1111–1121 (2012).
Koutsogeorgou, E., Chiesi, A. M. & Leonardi, M. Social capital components and social support of persons with multiple sclerosis: a systematic review of the literature from 2000 to 2018. Disabil. Rehabil. 42, 3437–3449 (2020).
Feinstein, A. An examination of suicidal intent in patients with multiple sclerosis. Neurology 59, 674–678 (2002).
Reyes, S., Suarez, S., Allen-Philbey, K., Thomson, A. & Giovannoni, G. The impact of social capital on patients with multiple sclerosis. Acta Neurol. Scand. 142, 58–65 (2020).
Uhr, L., Rice, D. R. & Mateen, F. J. Sociodemographic and clinical factors associated with depression, anxiety, and general mental health in people with multiple sclerosis during the COVID-19 pandemic. Mult. Scler. Relat. Disord. 56, 103327 (2021).
Bishop, M. & Rumrill, S. P. The employment impact of the COVID-19 pandemic on Americans with MS: preliminary analysis. J. Vocat. Rehabil. 54, 81–87 (2021).
Giménez-Llort, L., Martín-González, J. J. & Maurel, S. Secondary impacts of COVID-19 pandemic in fatigue, self-compassion, physical and mental health of people with multiple sclerosis and caregivers: the Teruel Study. Brain Sci. 11, 1233 (2021).
Learmonth, Y. C. et al. The impact of the Australian Black Summer Bushfires and the COVID-19 pandemic on wellbeing in persons with multiple sclerosis; preparation for future and ongoing crises. Disabil. Rehabil. https://doi.org/10.1080/09638288.2022.2037756 (2022).
Bonavita, S., Sparaco, M., Russo, A., Borriello, G. & Lavorgna, L. Perceived stress and social support in a large population of people with multiple sclerosis recruited online through the COVID‐19 pandemic. Eur. J. Neurol. 28, 3396–3402 (2021).
Morris-Bankole, H. & Ho, A. K. The COVID-19 pandemic experience in multiple sclerosis: the good, the bad and the neutral. Neurol. Ther. 10, 279–291 (2021).
Marmot, M., Allen, J., Boyce, T., Goldblatt, P. & Morrison, J. Marmot Review 10 years on. Institute of Health Equity https://www.instituteofhealthequity.org/resources-reports/marmot-review-10-years-on (2020).
Moscrop, A., Ziebland, S., Bloch, G. & Iraola, J. R. If social determinants of health are so important, shouldn’t we ask patients about them? BMJ 371, m4150 (2020).
Bechtel, N., Jones, A., Kue, J. & Ford, J. L. Evaluation of the core 5 social determinants of health screening tool. Public. Health Nurs. 39, 438–445 (2022).
Bradywood, A., Leming-Lee, T. S., Watters, R. & Blackmore, C. Implementing screening for social determinants of health using the Core 5 screening tool. BMJ Open Qual. 10, e001362 (2021).
Dobson, R. et al. Ethnic and socioeconomic associations with multiple sclerosis risk. Ann. Neurol. 87, 599–608 (2020).
NHS England. Treatment algorithm for multiple sclerosis disease-modifying therapies. NHS England https://www.england.nhs.uk/commissioning/wp-content/uploads/sites/12/2019/03/Treatment-Algorithm-for-Multiple-Sclerosis-Disease-Modifying-Therapies-08-03-2019-1.pdf (2019).
Wiendl, H. et al. Multiple Sclerosis Therapy Consensus Group (MSTCG): position statement on disease-modifying therapies for multiple sclerosis (white paper). Ther. Adv. Neurol. Disord. 14, 17562864211039648 (2021).
Hoffman, K. M., Trawalter, S., Axt, J. R. & Oliver, M. N. Racial bias in pain assessment and treatment recommendations, and false beliefs about biological differences between blacks and whites. Proc. Natl Acad. Sci. USA 113, 4296–4301 (2016).
Kirk, L. & Bezzant, K. What barriers prevent health professionals screening women for domestic abuse? A literature review. Br. J. Nurs. 29, 754–760 (2020).
McFadden, E. et al. Screening for the risk of job loss in multiple sclerosis (MS): development of an MS-specific Work Instability Scale (MS-WIS). Mult. Scler. 18, 862–870 (2012).
Kordovski, V. M. et al. Identifying employed multiple sclerosis patients at-risk for job loss: when do negative work events pose a threat? Mult. Scler. Relat. Disord. 4, 409–413 (2015).
Vanotti, S. et al. Employment status monitoring in an Argentinian population of patients with multiple sclerosis: particularities of a developing country. Work 68, 1121–1131 (2021).
Simmons, R. D., Tribe, K. L. & McDonald, E. A. Living with multiple sclerosis: longitudinal changes in employment and the importance of symptom management. J. Neurol. 257, 926–936 (2010).
Honan, C. A., Brown, R. F. & Batchelor, J. Perceived cognitive difficulties and cognitive test performance as predictors of employment outcomes in people with multiple sclerosis. J. Int. Neuropsychol. Soc. 21, 156–168 (2015).
Lueckmann, S. L. et al. Socioeconomic inequalities in primary-care and specialist physician visits: a systematic review. Int. J. Equity Health 20, 58 (2021).
Fjær, E. L. et al. Exploring the differences in general practitioner and health care specialist utilization according to education, occupation, income and social networks across Europe: findings from the European Social Survey (2014) special module on the social determinants of health. Eur. J. Public Health 27, 73–81 (2017).
Crawshaw, A. F. et al. Defining the determinants of vaccine uptake and undervaccination in migrant populations in Europe to improve routine and COVID-19 vaccine uptake: a systematic review. Lancet Infect. Dis. https://doi.org/10.1016/S1473-3099(22)00066-4 (2022).
Morse, D. F. et al. Global developments in social prescribing. BMJ Glob. Health 7, e008524 (2022).
Hoffmeister, L. V. et al. Evaluation of the impact and implementation of social prescribing in primary healthcare units in Lisbon: a mixed-methods study protocol. Int. J. Integr. Care 21, 26 (2021).
Rodriguez, J. A., Shachar, C. & Bates, D. W. Digital inclusion as health care — supporting health care equity with digital-infrastructure initiatives. N. Engl. J. Med. 386, 1101–1103 (2022).
Kavaliunas, A., Danylaitė Karrenbauer, V., Binzer, S. & Hillert, J. Systematic review of the socioeconomic consequences in patients with multiple sclerosis with different levels of disability and cognitive function. Front. Neurol. 12, 737211 (2021).
Acknowledgements
This work received no specific funding. R.D. works within the Preventive Neurology Unit, which is part funded by Barts Charity. Y.L. and C.H.M. are funded by MS Australia fellowships.
Author information
Authors and Affiliations
Contributions
R.D., D.R.R., M.D., R.H., Y.L., F.J.M., S.R., M.J.W., G.G. and H.L.F. researched data for the article. All authors contributed substantially to discussion of the content. R.D., D.R.R., M.D., R.H., Y.L., F.J.M., S.R., M.J.W., G.G. and H.L.F wrote the article. All authors reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Neurology thanks A. He, who co-reviewed with J. Hillert; E. Vasileiou, who co-reviewed with K. Fitzgerald; and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Review criteria To ensure an inclusive overview, we searched PubMed, Scopus, CINAHL through EBSCOhost, MEDLINE through OVID, all other Web of Science (BCI OR SciELO OR WoS OR CABI OR RSCI OR CCC) core collection, PsychINFO and Emcare (OVID) using a search strategy based on the WHO social and immediate determinants of health and a wide range of MS terms on 17 January 2022. We considered any original studies examining social determinants of health and MS outcomes from 2004 onwards, and did not restrict based on language, given the wide-reaching effects of social determinants of health. Out of 2,453 papers screened, a total of 194 papers were considered for inclusion, and the final decision was based on relevance to social determinants of health and MS, along with novelty and current relevance.
Related links
Social determinants of health: https://www.who.int/health-topics/social-determinants-of-health#tab=tab_1
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dobson, R., Rice, D.R., D’hooghe, M. et al. Social determinants of health in multiple sclerosis. Nat Rev Neurol 18, 723–734 (2022). https://doi.org/10.1038/s41582-022-00735-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41582-022-00735-5
This article is cited by
-
Real-World Safety and Effectiveness After 5 Years of Dimethyl Fumarate Treatment in Black and Hispanic Patients with Multiple Sclerosis in ESTEEM
Neurology and Therapy (2023)
-
Multiple Sclerosis Pathogenesis and Updates in Targeted Therapeutic Approaches
Current Allergy and Asthma Reports (2023)