Abstract
The idea that infectious agents in the brain have a role in the pathogenesis of Alzheimer disease (AD) was proposed nearly 30 years ago. However, this theory failed to gain substantial traction and was largely disregarded by the AD research community for many years. Several recent discoveries have reignited interest in the infectious theory of AD, culminating in a debate on the topic at the Alzheimer’s Association International Conference (AAIC) in July 2019. In this Viewpoint article, experts who participated in the AAIC debate weigh up the evidence for and against the infectious theory of AD and suggest avenues for future research and drug development.
The contributors
Ruth F. Itzhaki has a BSc in physics and an MSc and a PhD in biophysics from the University of London, UK. She worked as a postdoctoral researcher at the University of Cambridge, UK, where she held a Beit Memorial Fellowship in the Radiotherapeutics Department and the Wheldale Onslow Fellowship at Newnham College. She then moved to the Paterson Laboratories, Manchester, UK, and later to Manchester University. Her research topics have been diverse, and she is currently studying viruses in Alzheimer disease (AD) and the role of apolipoprotein E in infection. She is now an Emeritus Professor at Manchester University and a Visiting Professor at Oxford University, UK.
Todd E. Golde is a Professor of Neuroscience and Director of the Evelyn F. and William L. McKnight Brain Institute at the University of Florida, Gainesville, FL, USA. He also directs the NIH-funded Florida Alzheimer’s Disease Research Center. With over 30 years of research experience in AD, Dr Golde has made substantial contributions to the field. His early studies helped establish the underpinnings of the amyloid hypothesis and provided insight into the therapeutic targeting of amyloid deposition. More recently, he has focused on the role of the immune system and stress pathways in AD.
Michael T. Heneka studied medicine in Tübingen (Germany), Lausanne (Switzerland) and London (UK) and thereafter specialized in clinical neurology and neurosciences. He is currently serving as the Director of the Department of Neurodegenerative Disease and Geriatric Psychiatry at the University of Bonn Medical Center, Bonn, Germany. His research focuses on the interaction between immunological and neurodegenerative processes.
Ben Readhead is an Australian-born medical practitioner. He is passionate about innovation in the life sciences, with a focus on the application of biomedical informatics to enable precision medicine and improve patient care. His research is focused on developing and applying integrative genomics approaches to high-dimensional biomedical data with the goal of improving therapeutic options for patients with neurodegenerative diseases, particularly AD. He is especially interested in understanding the complex web of interactions between the brain microbiome and host biology in the context of neurodegenerative disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Jamieson, G. A., Maitland, N. J., Wilcock, G. K., Craske, J. & Itzhaki, R. F. Latent herpes simplex virus type 1 in normal and Alzheimer’s disease brains. J. Med. Virol. 33, 224–227 (1991).
Itzhaki, R. F. et al. Herpes simplex virus type 1 in brain and risk of Alzheimer’s disease. Lancet 349, 241–244 (1997).
Miklossy, J. Bacterial amyloid and DNA are important constituents of senile plaques: further evidence of the spirochetal and biofilm nature of senile plaques. J. Alzheimers Dis. 53, 1459–1473 (2016).
Balin, B. J. et al. Chlamydia pneumoniae: an etiologic agent for late-onset dementia. Front. Aging Neurosci. 10, 302 (2018).
Dominy, S. S. et al. Porphyromonas gingivalis in Alzheimer’s disease brains: evidence for disease causation and treatment with small-molecule inhibitors. Sci. Adv. 5, eaau3333 (2019).
Itzhaki, R. F. Corroboration of a major role for herpes simplex virus type 1 in Alzheimer’s disease. Front. Aging Neurosci. 10, 324 (2018).
Abbott, A. Gut feeling secures medical Nobel for Australian doctors. Nature 437, 801 (2005).
Itzhaki, R. F., Dobson, C. B., Shipley, S. J. & Wozniak, M. A. The role of viruses and of APOE in dementia. Ann. NY Acad. Sci. 1019, 15–18 (2004).
Eimer, W. A. et al. Alzheimer’s disease-associated β-amyloid is rapidly seeded by Herpesviridae to protect against brain infection. Neuron 99, 56–63.e3 (2018).
Kumar, D. K. et al. Amyloid-β peptide protects against microbial infection in mouse and worm models of Alzheimer’s disease. Sci. Transl. Med. 8, 340ra72 (2016).
Readhead, B. et al. Multiscale analysis of independent Alzheimer’s cohorts finds disruption of molecular, genetic, and clinical networks by human herpesvirus. Neuron 99, 64–82 (2018).
Tzeng, N. S. et al. Anti-herpetic medications and reduced risk of dementia in patients with herpes simplex virus infections — a nationwide, population-based cohort study in Taiwan. Neurotherapeutics 15, 417–429 (2018).
Golde, T. E. Harnessing immunoproteostasis to treat neurodegenerative disorders. Neuron 101, 1003–1015 (2019).
Haeberlein, S. B. et al. EMERGE and ENGAGE topline results: two phase 3 studies to evaluate aducanumab in patients with early Alzheimer’s disease. Clinical Trials on Alzheimer's Disease (CTAD) https://investors.biogen.com/static-files/ddd45672-9c7e-4c99-8a06-3b557697c06f (2019).
Belluck, P. A common virus may play role in Alzheimer’s disease, study finds. The New York Times (New York) 17 (21 Jun 2018).
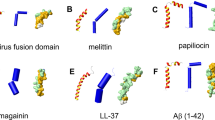
Soscia, S. J. et al. The Alzheimer’s disease-associated amyloid β-protein is an antimicrobial peptide. PLoS One 5, e9505 (2010).
Bourgade, K. et al. β-Amyloid peptides display protective activity against the human Alzheimer’s disease-associated herpes simplex virus-1. Biogerontology 16, 85–98 (2015).
Tsai, M. C. et al. Increased risk of dementia following herpes zoster ophthalmicus. PLoS One 12, e0188490 (2017).
Mori, I. et al. Reactivation of HSV-1 in the brain of patients with familial Alzheimer’s disease. J. Med. Virol. 73, 605–611 (2004).
Gérard, H. C. et al. Chlamydophila (Chlamydia) pneumoniae in the Alzheimer’s brain. FEMS Immunol. Med. Microbiol. 48, 355–366 (2006).
Alonso, R., Pisa, D., Férnandez-Férnandez, A. M. & Carrasco, L. Infection of fungi and bacteria in brain tissue from elderly persons and patients with Alzheimer’s disease. Front. Aging Neurosci. 10, 159 (2018).
Hammond, C. J. et al. Immunohistological detection of Chlamydia pneumoniae in the Alzheimer’s disease brain. BMC Neurosci. 11, 121 (2010).
Pisa, D., Alonso, R., Rábano, A., Rodal, I. & Carrasco, L. Different brain regions are infected with fungi in Alzheimer’s disease. Sci. Rep. 5, 15015 (2015).
Klapper, P. E., Cleator, G. M. & Longson, M. Mild forms of herpes encephalitis. J. Neurol. Neurosurg. Psychiatry 47, 1247–1250 (1984).
Itzhaki, R. F. et al. Microbes and Alzheimer’s disease. J. Alzheimers Dis. 51, 979–984 (2016).
Lövheim, H. et al. Herpes simplex virus, APOEε4, and cognitive decline in old age: results from the Betula Cohort Study. J. Alzheimers Dis. 67, 211–220 (2019).
Miklossy, J. Historic evidence to support a causal relationship between spirochetal infections and Alzheimer’s disease. Front. Aging Neurosci. 7, 46 (2015).
Balin, B. J. et al. Identification and localization of Chlamydia pneumoniae in the Alzheimer’s brain. Med. Microbiol. Immunol. 187, 23–42 (1998).
Alonso, R. et al. Fungal infection in patients with Alzheimer’s disease. J. Alzheimers Dis. 41, 301–311 (2014).
Iwashyna, T. J., Ely, E. W., Smith, D. M. & Langa, K. M. Long-term cognitive impairment and functional disability among survivors of severe sepsis. JAMA 301, 489–499 (2009).
Widmann, C. N. & Heneka, M. T. Long-term cerebral consequences of sepsis. Lancet Neurol. 13, 630–636 (2014).
Warren-Gash, C. et al. Human herpesvirus infections and dementia or mild cognitive impairment: a systematic review and meta-analysis. Sci. Rep. 9, 4743 (2019).
Golde, T. E., DeKosky, S. T. & Galasko, D. Alzheimer’s disease: the right drug, the right time. Science 362, 1250–1251 (2018).
Tejera, D. et al. Systemic inflammation impairs microglial Aβ clearance through NLRP3 inflammasome. EMBO J. 38, e101064 (2019).
Venegas, C. et al. Microglia-derived ASC specks cross-seed amyloid-β in Alzheimer’s disease. Nature 552, 355–361 (2017).
Ising, C. et al. NLRP3 inflammasome activation drives tau pathology. Nature 575, 669–673 (2019).
Itzhaki, R. F. & Lathe, R. Herpes viruses and senile dementia: first population evidence for a causal link. J. Alzheimers Dis. 64, 363–366 (2018).
Wozniak, M., Bell, T., Dénes, Á. & Itzhaki, R. Anti-HSV1 activity of brown algal polysaccharides and possible relevance to the treatment of Alzheimer’s disease. Int. J. Biol. Macromol. 74, 530–540 (2015).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
T.E.G. is a co-founder and is on the scientific advisory board (SAB) of Lacerta Therapeutics. He is an SAB member for Promis Therapeutics and has served on SABs for Abbvie, Pfizer, Novartis, Roche/Genetic, Bristol Myers Squibb, Eli Lilly and Biogen. He is an inventor on a number of patents relating to Alzheimer disease therapeutics. He receives funding from the NIH, the Facial Pain Research Foundation and the State of Florida. M.T.H. serves as an advisory board member for IFM Therapeutics, Alector and Tiaki. The other authors declare no competing interests.
Additional information
Dr Robert Moir (1961–2019) was the fifth participant of the AAIC debate, but sadly passed away as this manuscript was being prepared. The authors dedicate this Viewpoint to him as a tribute to an indomitable and original thinker, brilliant and unorthodox scientist, and true forerunner of research into the role of microorganisms in Alzheimer disease.
Rights and permissions
About this article
Cite this article
Itzhaki, R.F., Golde, T.E., Heneka, M.T. et al. Do infections have a role in the pathogenesis of Alzheimer disease?. Nat Rev Neurol 16, 193–197 (2020). https://doi.org/10.1038/s41582-020-0323-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41582-020-0323-9
This article is cited by
-
The interaction between ageing and Alzheimer's disease: insights from the hallmarks of ageing
Translational Neurodegeneration (2024)
-
Integrative Multi-omics Analysis to Characterize Herpes Virus Infection Increases the Risk of Alzheimer’s Disease
Molecular Neurobiology (2024)
-
Clinical evidence of human pathogens implicated in Alzheimer’s disease pathology and the therapeutic efficacy of antimicrobials: an overview
Translational Neurodegeneration (2023)
-
Human-derived air–liquid interface cultures decipher Alzheimer’s disease–SARS-CoV-2 crosstalk in the olfactory mucosa
Journal of Neuroinflammation (2023)
-
Effects and mechanism of Aβ1−42 on EV-A71 replication
Virology Journal (2022)