Abstract
Over the past decade, traumatic brain injury (TBI) has emerged as a major public health concern, attracting considerable interest from the scientific community, clinical and behavioural services and policymakers, owing to its rising prevalence, wide-ranging risk factors and substantial lifelong familial and societal impact. This increased attention to TBI has resulted in increased funding and advances in legislation. However, many questions surrounding TBI remain unanswered, including questions on sex and gender trends with respect to vulnerability to injury, presentation of injury, response to treatment, and outcomes. Here, we review recent research efforts aimed at advancing knowledge on the constructs of sex and gender and their respective influences in the context of TBI, and discuss methodological challenges in disentangling the differential impacts of these two constructs, particularly in marginalized populations.
Key points
-
The effects of biological sex, as well as gender, which represents an amalgamation of social, biological, cultural and behavioural elements, are underappreciated in traumatic brain injury (TBI) research and practice.
-
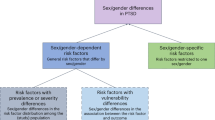
Differential environmental exposures, biological vulnerabilities to injury, and gender disparities in norms and role expectations affect the reported prevalence and incidence of TBI.
-
Preclinical studies of TBI provide inconsistent results on the neuroprotective effects of sex hormones.
-
Certain groups of men and women are more vulnerable to TBI than others, owing to the unique interactions between their biological, behavioural, social and cultural conditions preceding injury and at the time of injury.
-
The transition from an injury event to disability in TBI is affected by a plethora of factors, including attitudes at local, family and societal levels, economic deprivation, and endorsement of civil rights legislation.
-
Explicit and consistent consideration of the interrelated constructs of sex and gender in TBI research will produce a better understanding of the different mechanisms that shape the health status trajectory and outcomes of TBI.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Menon, D. K. et al. Position statement: definition of traumatic brain injury. Arch. Phys. Med. Rehabil. 91, 1637–1640 (2010).
Maas, A. I. et al. Traumatic brain injury: integrated approaches to improve prevention, clinical care, and research. Lancet Neurol. 16, 987–1048 (2017).
Quaglio, G., Gallucci, M., Brand, H., Dawood, A. & Cobello, F. Traumatic brain injury: a priority for public health policy. Lancet Neurol. 16, 951–952 (2017). This commentary highlights the global burden of TBI and presents the challenges associated with its prevention, treatment and related research. The authors note that clinical protocols currently do not consider between-patient differences in post-injury trajectories and outcomes.
Kindig, D. Population health equity: rate and burden, race and class. JAMA 317, 467–468 (2017).
Asaria, M., Doran, T. & Cookson, R. The costs of inequality: whole-population modelling study of lifetime inpatient hospital costs in the English National Health Service by level of neighbourhood deprivation. J. Epidemiol. Community Health 70, 990–996 (2016).
Masel, B. E. & DeWitt, D. S. Traumatic brain injury: a disease process, not an event. J. Neurotrauma 27, 1529–1540 (2010).
Chan, V., Mollayeva, T., Ottenbacher, K. J. & Colantonio, A. Clinical profile and comorbidity of traumatic brain injury among younger and older men and women: a brief research notes. BMC Res. Notes 10, 371 (2017).
De Loof, A. Only two sex forms but multiple gender variants: how to explain? Commun. Integr. Biol. 11, e1427399 (2018).
Nguyen, R. et al. The international incidence of traumatic brain injury: a systematic review and meta-analysis. Can. J. Neurol. Sci. 43, 774–785 (2016).
Chen, A. Y. & Colantonio, A. Defining neurotrauma in administrative data using the International Classification of Diseases Tenth Revision. Emerg. Themes Epidemiol. 8, 4 (2011).
Bazarian, J. J., Veazie, P., Mookerjee, S. & Lerner, E. B. Accuracy of mild traumatic brain injury case ascertainment using ICD-9 codes. Acad. Emerg. Med. 13, 31–38 (2006).
Kroshus, E., Baugh, C. M., Stein, C. J., Austin, S. B. & Calzo, J. P. Concussion reporting, sex, and conformity to traditional gender norms in young adults. J. Adolesc. 54, 110–119 (2017).
Miyashita, T. L., Diakogeorgiou, E. & VanderVegt, C. Gender differences in concussion reporting among high school athletes. Sports Health 8, 359–363 (2016). This work found that female athletes were significantly more likely to report a concussion than were their male counterparts. These results raise the issue of potential underreporting by men, either due to different norms and expectations in their sports, or in general related to their gender identity.
Demakis, G. J. & Rimland, C. Untreated mild traumatic brain injury in a young adult population. Arch. Clin. Neuropsychol. 25, 191–196 (2010).
Stergiou-Kita, M., Mansfield, E., Sokoloff, S. & Colantonio, A. Gender influences on return to work after mild traumatic brain injury. Arch. Phys. Med. Rehabil. 97, S40–S45 (2016).
Wright, D. W. et al. Gender differences in neurological emergencies part II: a consensus summary and research agenda on traumatic brain injury. Acad. Emerg. Med. 21, 1414–1420 (2014).
Tierney, R. T. et al. Gender differences in head-neck segment dynamic stabilization during head acceleration. Med. Sci. Sports Exerc. 37, 272–279 (2005).
Chang, V. C., Guerriero, E. N. & Colantonio, A. Epidemiology of work-related traumatic brain injury: a systematic review. Am. J. Ind. Med. 58, 353–377 (2015).
US Department of Health & Human Services. TBI: get the facts. Centers for Disease Control and Prevention http://www.cdc.gov/traumaticbraininjury/get_the_facts.html (2017).
Lagbas, C., Bazargan-Hejazi, S., Shaheen, M., Kermah, D. & Pan, D. Traumatic brain injury related hospitalization and mortality in California. Biomed Res. Int. 2013, 143092 (2013).
Colantonio, A., Croxford, R., Farooq, S., Laporte, A. & Coyte, P. C. Trends in hospitalization associated with traumatic brain injury in a publicly insured population, 1992–2002. J. Trauma 66, 179–183 (2009).
Suzuki, S., Brown, C. M. & Wise, P. M. Mechanisms of neuroprotection by estrogen. Endocrine 29, 209–215 (2006).
Green, P. S. & Simpkins, J. W. Neuroprotective effects of estrogens: potential mechanisms of action. Int. J. Dev. Neurosci. 18, 347–358 (2000).
Arevalo, M.-A., Azcoitia, I. & Garcia-Segura, L. M. The neuroprotective actions of oestradiol and oestrogen receptors. Nat. Rev. Neurosci. 16, 17–29 (2014).
Raghava, N., Das, B. C. & Ray, S. K. Neuroprotective effects of estrogen in CNS injuries: insights from animal models. Neurosci. Neuroecon. 6, 15–29 (2017).
Roof, R. L., Duvdevani, R. & Stein, D. G. Gender influences outcome of brain injury: progesterone plays a protective role. Brain Res. 607, 333–336 (1993).
Roof, R. L. & Hall, E. D. Estrogen-related gender difference in survival rate and cortical blood flow after impact-acceleration head injury in rats. J. Neurotrauma 17, 1155–1169 (2000).
O’Connor, C. A., Cernak, I. & Vink, R. Interaction between anesthesia, gender, and functional outcome task following diffuse traumatic brain injury in rats. J. Neurotrauma. 20, 533–541 (2003).
Emerson, C. S., Headrick, J. P. & Vink, R. Estrogen improves biochemical and neurologic outcome following traumatic brain injury in male rats, but not in females. Brain Res. 608, 95–100 (1993).
Hall, E. D., Gibson, T. R. & Pavel, K. M. Lack of a gender difference in post-traumatic neurodegeneration in the mouse controlled cortical impact injury model. J. Neurotrauma 22, 669–679 (2005).
Baran, S. E., Armstrong, C. E., Niren, D. C. & Conrad, C. D. Prefrontal cortex lesions and sex differences in fear extinction and perseveration. Learn. Mem. 17, 267–278 (2010).
Bruce-Keller, A. J. et al. Gender and estrogen manipulation do not affect traumatic brain injury in mice. J. Neurotrauma 24, 203–215 (2007).
Robertson, C. L. & Saraswati, M. Progesterone protects mitochondrial function in a rat model of pediatric traumatic brain injury. J. Bioenerg. Biomembr. 47, 43–51 (2014).
Sacco, S., Ricci, S., Degan, D. & Carolei, A. Migraine in women: the role of hormones and their impact on vascular diseases. J. Headache Pain 13, 177–189 (2012).
Armstead, W. M., Kiessling, J. W., Bdeir, K., Kofke, W. A. & Vavilala, M. S. Adrenomedullin prevents sex-dependent impairment of autoregulation during hypotension after piglet brain injury through inhibition of ERK MAPK upregulation. J. Neurotrauma 27, 391–402 (2010).
Armstead, W. M., Kiessling, J. W., Kofke, W. A. & Vavilala, M. S. Impaired cerebral blood flow autoregulation during posttraumatic arterial hypotension after fluid percussion brain injury is prevented by phenylephrine in female but exacerbated in male piglets by ERK MAPK upregulation. Crit. Care Med. 38, 1868–1874 (2010).
Stein, D. M. et al. Brief episodes of intracranial hypertension and cerebral hypoperfusion are associated with poor functional outcome after severe traumatic brain injury. J. Trauma 71, 364–373 (2011).
Sorge, R. E. et al. Olfactory exposure to males, including men, causes stress and related analgesia in rodents. Nat. Methods 11, 629–632 (2014).
Junges, R., Zitzmann, N. U., Walter, C. & Rösing, C. K. Dental care providers’ decision making regarding maintenance of compromised teeth and implant therapy indication: an analysis of gender and enrollment in teaching positions. Clin. Oral Implants Res. 25, 1027–1033 (2014).
Mansuy, I. M. & Mohanna, S. Epigenetics and the human brain: where nurture meets nature. Cerebrum 2011, 8 (2011).
Wasserman, E. B., Kerr, Z. Y., Zuckerman, S. L. & Covassin, T. Epidemiology of sports-related concussions in National Collegiate Athletic Association athletes from 2009–2010 to 2013–2014. Am. J. Sports Med. 44, 226–233 (2016).
Covassin, T., Schatz, P. & Swanik, C. B. Sex differences in neuropsychological function and post-concussion symptoms of concussed collegiate athletes. Neurosurgery 61, 345–350 (2007).
Arellano-Orden, V. et al. Gender influences cerebral oxygenation after red blood cell transfusion in patients with severe traumatic brain injury. Neurocrit. Care 14, 18–23 (2011).
Kim, H., Colantonio, A., Bayley, M. & Dawson, D. Discharge against medical advice after traumatic brain injury: is intentional injury a predictor? J. Trauma 71, 1219–1225 (2011).
Marcoux, J. et al. Discharge against medical advice in traumatic brain injury: follow-up and readmission rate. Can. J. Neurol. Sci. 44, 311–317 (2017).
Czosnyka, M. et al. Gender-related differences in intracranial hypertension and outcome after traumatic brain injury. Acta Neurochir. Suppl. 102, 25–28 (2008).
Gilthorpe, M. S., Wilson, R. C., Moles, D. R. & Bedi, R. Variations in admissions to hospital for head injury and assault to the head — part 1: age and gender. Br. J. Oral Maxillofac. Surg. 37, 294–300 (1999).
Ottochian, M. et al. Severe traumatic brain injury: is there a gender difference in mortality? Am. J. Surg. 197, 155–158 (2009).
Adeloye, A., Kattan, K. R. & Silverman, F. N. Thickness of the normal skull in the American blacks and whites. Am. J. Phys. Anthropol. 43, 23–30 (1975).
De Boer, H. H., Van der Merwe, A. E. & Soerdjbalie-Maikoe, V. V. Human cranial vault thickness in a contemporary sample of 1097 autopsy cases: relation to body weight, stature, age, sex and ancestry. Int. J. Legal Med. 130, 1371–1377 (2016).
McCarthy, M. M., Pickett, L. A., VanRyzin, J. W. & Kight, K. E. Surprising origins of sex differences in the brain. Horm. Behav. 76, 3–10 (2015).
Ritchie, S. J. et al. Sex differences in the adult human brain: evidence from 5216 UK Biobank participants. Cereb. Cortex 28, 2959–2975 (2018).
Kurth, F., Thompson, P. M. & Luders, E. Investigating the differential contributions of sex and brain size to gray matter asymmetry. Cortex 99, 235–242 (2018).
Ono, K. E. et al. Sex-based differences as a predictor of recovery trajectories in young athletes after a sports-related concussion. Am. J. Sports Med. 44, 748–752 (2016).
Ferguson, P. L., Pickelsimer, E. E., Corrigan, J. D., Bogner, J. A. & Wald, M. Prevalence of traumatic brain injury among prisoners in South Carolina. J. Head Trauma Rehabil. 27, E11–E20 (2012).
Kaba, F., Diamond, P., Haque, A., MacDonald, R. & Venters, H. Traumatic brain injury among newly admitted adolescents in the New York city jail system. J. Adolesc. Health 54, 615–617 (2014).
Bay, E., Sikorskii, A. & Saint-Arnault, D. Sex differences in depressive symptoms and their correlates after mild-to-moderate traumatic brain injury. J. Neurosci. Nurs. 41, 298–309 (2009).
Ponsford, J. et al. Predictors of postconcussive symptoms 3 months after mild traumatic brain injury. Neuropsychology 26, 304–313 (2012).
Wäljas, M. et al. A prospective biopsychosocial study of the persistent post-concussion symptoms following mild traumatic brain injury. J. Neurotrauma 32, 534–547 (2015).
Mollayeva, T., Cassidy, J. D., Shapiro, C. M., Mollayeva, S. & Colantonio, A. Concussion/mild traumatic brain injury-related chronic pain in males and females: a diagnostic modelling study. Medicine 96, e5917 (2017).
Mollayeva, T., Mollayeva, S., Shapiro, C. M., Cassidy, J. D. & Colantonio, A. Insomnia in workers with delayed recovery from mild traumatic brain injury. Sleep Med. 19, 153–161 (2016).
Mollayeva, T. et al. Sleep stage distribution in persons with mild traumatic brain injury: a polysomnographic study according to American Academy of Sleep Medicine standards. Sleep Med. 34, 179–192 (2017).
Hill, C. A. et al. A causal account of the brain network computations underlying strategic social behavior. Nat. Neurosci. 20, 1142–1149 (2017).
Haddon, W. Jr. On the escape of tigers: an ecologic note. Am. J. Public Health Nations Health 60, 2229–2234 (1970).
Engström, K. G., Angrén, J., Björnstig, U. & Saveman, B. I. Mass casualty incidents in the underground mining industry: applying the Haddon matrix on an integrative literature review. Disaster Med. Public Health Prep. 12, 138–146 (2018).
Department of Economic and Social Affairs Population Division. World Population Ageing: 1950–2050. United Nations http://www.un.org/esa/population/publications/worldageing19502050 (2001).
Ramanathan, D. M., McWilliams, N., Schatz, P. & Hillary, F. G. Epidemiological shifts in elderly traumatic brain injury: 18-year trends in Pennsylvania. J. Neurotrauma 29, 1371–1378 (2012).
McGuire, C., Kristman, V. L., Martin, L. & Bédard, M. Characteristics and incidence of traumatic brain injury in older adults using home care in Ontario from 2003–2013. Can. Geriatr. J. 20, 2–9 (2017).
Marquez de la Plata, C. D. et al. Impact of age on long-term recovery from traumatic brain injury. Arch. Phys. Med. Rehabil. 89, 896–903 (2008).
Mak, C. H. et al. Traumatic brain injury in the elderly: is it as bad as we think? Curr. Transl Geriatr. Exp. Gerontol. Rep. 1, 171–178 (2012).
Mathias, J. L. & Wheaton, P. Contribution of brain or biological reserve and cognitive or neural reserve to outcome after TBI: a meta-analysis. Neurosci. Biobehav. Rev. 55, 573–593 (2015).
Gillespie, L. D. et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst. Rev. 9, CD007146 (2012).
Fu, W. W., Fu, T. S., Jing, R., McFaull, S. R. & Cusimano, M. D. Predictors of falls and mortality among elderly adults with traumatic brain injury: a nationwide, population-based study. PLOS ONE 12, e0175868 (2017).
Institute of Medicine of the National Academies. Gulf War and Health Volume 7: Long-Term Consequences of Traumatic Brain Injury. 1–388 (The National Academies Press, 2009).
US Department of Health & Human Services. Alzheimer’s disease. Centers for Disease Control and Prevention https://www.cdc.gov/aging/aginginfo/alzheimers.htm (2018).
Mazure, C. M. & Swendsen, J. Sex differences in Alzheimer’s disease and other dementias. Lancet Neurol. 15, 451–452 (2016).
Klose, M. et al. Acute and long-term pituitary insufficiency in traumatic brain injury: a prospective single-centre study. Clin. Endocrinol. 67, 598–606 (2007).
Davis, D. P. et al. Traumatic brain injury outcomes in pre- and post- menopausal females versus age-matched males. J. Neurotrauma 23, 140–148 (2006).
Xu, W. et al. Meta-analysis of modifiable risk factors for Alzheimer’s disease. J. Neurol. Neurosurg. Psychiatry 86, 1299–1306 (2015).
Chen, R. et al. Incident dementia in a defined older Chinese population. PLOS ONE 6, e24817 (2011).
Seidler, A. et al. Occupational exposure to low frequency magnetic fields and dementia: a case-control study. Occup. Environ. Med. 64, 108–114 (2007).
Moon, J. H. Endocrine risk factors for cognitive impairment. Endocrinol. Metab. 31, 185–192 (2016).
Takahashi, M., Oda, Y., Sato, K. & Shirayama, Y. Vascular risk factors and the relationships between cognitive impairment and hypoperfusion in late-onset Alzheimer’s disease. Acta Neuropsychiatr. https://doi.org/10.1017/neu.2018.17 (2018).
World Health Organization. Understanding and addressing violence against women. WHO http://apps.who.int/iris/bitstream/10665/77433/1/WHO_RHR_12.35_eng.pdf (2012).
Tjaden, P. & Thoennes, N. Full report of the prevalence, incidence, and consequences of violence against women (National Institute of Justice, 2000).
Ivany, A. S. & Schminkey, D. Intimate partner violence and traumatic brain injury: state of the science and next steps. Fam. Community Health 39, 129–137 (2016).
Faugno, D., Waszak, D., Strack, G. B., Brooks, M. A. & Gwinn, C. G. Strangulation forensic examination: best practice for health care providers. Adv. Emerg. Nurs. J. 35, 314–327 (2013).
Goldin, Y., Haag, H. L. & Trott, C. T. Screening for history of traumatic brain injury among women exposed to intimate partner violence. PM R. 8, 1104–1110 (2016).
Reichard, A. A., Langlois, J. A., Sample, P. L., Wald, M. M. & Pickelsimer, E. E. Violence, abuse, and neglect among people with traumatic brain injuries. J. Head Trauma Rehabil. 22, 390–402 (2007).
Hoopes, M. J. et al. Uncovering a missing demographic in trauma registries: epidemiology of trauma among American Indians and Alaska Natives in Washington state. Inj. Prevent. 21, 335–343 (2015).
Strayer, H. & Lucas, M. P. Whose head hurts in Alaska? TBI trends and disparities. Brain Inj. 28, 566 (2014).
Zeiler, K. J. & Zeiler, F. A. Social determinants of traumatic brain injury in the North American indigenous population: a review. Can. J. Neurol. Sci. 44, 525–531 (2017).
Farrer, T. J., Frost, R. B. & Hedges, D. W. Prevalence of traumatic brain injury in intimate partner violence offenders compared to the general population: a meta-analysis. Trauma Violence Abuse 13, 77–82 (2012).
Dyer, K. F., Bell, R., McCann, J. & Rauch, R. Aggression after traumatic brain injury: analysing socially desirable responses and the nature of aggressive traits. Brain Inj. 20, 1163–1173 (2006).
Hall, K. M. et al. Family stressors in traumatic brain injury: a two-year follow-up. Arch. Phys. Med. Rehabil. 75, 876–884 (1994).
Fazel, S., Geddes, J. R. & Kushel, M. The health of homeless people in high-income countries: descriptive epidemiology, health consequences, and clinical and policy recommendations. Lancet 384, 1529–1540 (2014).
Topolovec-Vranic, J. et al. Traumatic brain injury among people who are homeless: a systematic review. BMC Public Health 12, 1059 (2012).
Hwang, S. W. et al. The effect of traumatic brain injury on the health of homeless people. CMAJ 179, 779–784 (2008).
Oddy, M., Moir, J. F., Fortescue, D. & Chadwick, S. The prevalence of traumatic brain injury in the homeless community in a UK city. Brain Inj. 26, 1058–1064 (2012).
To, M. J. et al. Healthcare utilization, legal incidents, and victimization following traumatic brain injury in homeless and vulnerably housed individuals: a prospective cohort study. J. Head Trauma Rehabil. 30, 270–276 (2015).
Nikoo, M. et al. Incidence and associated risk factors of traumatic brain injury in a cohort of homeless and vulnerably housed adults in 3 Canadian cities. J. Head Trauma Rehabil. 32, E19–E26 (2017).
Hux, K., Schneider, T. & Bennett, K. Screening for traumatic brain injury. Brain Inj. 23, 8–14 (2009).
Beijer, U. & Andréasson, S. Physical diseases among homeless people: gender differences and comparisons with the general population. Scand. J. Public Health 37, 93–100 (2009).
Chang, V. C., Ruseckaite, R., Collie, A. & Colantonio, A. Examining the epidemiology of work-related traumatic brain injury through a sex/gender lens: analysis of workers’ compensation claims in Victoria, Australia. Occup. Environ. Med. 71, 695–703 (2014).
Kim, H., Colantonio, A. & Chipman, M. Traumatic brain injury occurring at work. NeuroRehabilitation 21, 269–278 (2006).
Slavova, S. & Bunn, T. L. Work-related concussion surveillance. Am. J. Ind. Med. 58, 40–45 (2015).
Konda, S., Tiesman, H. M. & Reichard, A. A. Fatal traumatic brain injuries in the construction industry, 2003–2010. Am. J. Ind. Med. 59, 212–220 (2016).
Tricco, A. C., Colantonio, A., Chipman, M., Liss, G. & McLellan, B. Work-related deaths and traumatic brain injury. Brain Inj. 20, 719–724 (2006).
Kristman, V. L. et al. Prevalence of lost-time claims for mild traumatic brain injury in the working population: improving estimates using workers compensation databases. Brain Inj. 22, 51–59 (2008).
Mollayeva, T., Mollayeva, S., Lewko, J. & Colantonio, A. Sex differences in work-related traumatic brain injury due to assault. Work 54, 415–423 (2016).
Amodio, V., Bruch, H., Mollayeva, T. & Colantonio, A. Using the narratives of Ontarians with a work-related traumatic brain injury to inform injury prevention: a mixed methods approach. Work 56, 563–570 (2017).
Corrigan, J. D. et al. Employment after traumatic brain injury: differences between men and women. Arch. Phys. Med. Rehabil. 88, 1400–1409 (2007).
Devitt, R. et al. Prediction of long-term occupational performance outcomes for adults after moderate to severe traumatic brain injury. Disabil. Rehabil. 28, 547–559 (2006).
Hayes, J. P., Bigler, E. D. & Verfaellie, M. Traumatic brain injury as a disorder of brain connectivity. J. Int. Neuropsychol. Soc. 22, 120–137 (2016).
Bushman, B. J. & O’Brien, E. H. in Encyclopedia of Human Behavior (ed. Ramachandran, V. S.) 37–43 (Academic Press, 2012).
Spencer, D. et al. Prenatal androgen exposure and children’s aggressive behavior and activity level. Horm. Behav. 96, 156–165 (2017).
Mhillaj, E. et al. Effects of anabolic-androgens on brain reward function. Front. Neurosci. 9, 295 (2015).
Fishbein, D., Dariotis, J. K., Ferguson, P. L. & Pickelsimer, E. E. Relationships between traumatic brain injury and illicit drug use and their association with aggression in inmates. Int. J. Offender Ther. Comp. Criminol. 60, 575–597 (2016).
McGlade, E., Rogowska, J. & Yurgelun-Todd, D. Sex differences in orbitofrontal connectivity in male and female veterans with TBI. Brain Imaging Behav. 9, 535–549 (2015).
Scott, C. et al. A comparison of adult outcomes for males compared to females following pediatric traumatic brain injury. Neuropsychology 29, 501–508 (2015).
McIsaac, K. E. et al. Association between traumatic brain injury and incarceration: a population-based cohort study. CMAJ Open 4, E746–E753 (2016).
Elbogen, E. B., Wolfe, J. R., Cueva, M., Sullivan, C. & Johnson, J. Longitudinal predictors of criminal arrest after traumatic brain injury: results from the Traumatic Brain Injury Model System National Database. J. Head Trauma Rehabil. 30, E3–E13 (2015).
Colantonio, A. et al. Traumatic brain injury and early life experiences among men and women in a prison population. J. Correct. Health Care 20, 271–279 (2014). This study reports a high prevalence of TBI in the prison population, with women more often sustaining their injuries before their first crime. The paper also highlights a high prevalence of early-life adversity among women with a history of TBI.
Durand, E. et al. History of traumatic brain injury in prison populations: a systematic review. Ann. Phys. Rehabil. Med. 60, 95–101 (2017).
Walmsley, R. World Female Imprisonment List 3rd edn (Institute for Criminal Policy Research, 2015).
Heerkens, Y. F. et al. Reconsideration of the scheme of the International Classification of Functioning, Disability and Health: incentives from the Netherlands for a global debate. Disabil. Rehabil. 40, 603–611 (2017).
World Health Organization. International Classification of Functioning, Disability and Health (ICF) (WHO, Geneva, 2001).
Xiong, C., Martin, T., Sravanapudi, A., Colantonio, A. & Mollayeva, T. Factors associated with return to work in men and women with work-related traumatic brain injury. Disabil. Health J. 9, 439–448 (2016).
Mollayeva, T., Shapiro, C. M., Mollayeva, S., Cassidy, J. D. & Colantonio, A. Modeling community integration in workers with delayed recovery from mild traumatic brain injury. BMC Neurol. 15, 194 (2015).
Hackman, J., Maupin, J. & Brewis, A. A. Weight-related stigma is a significant psychosocial stressor in developing countries: evidence from Guatemala. Soc. Sci. Med. 161, 55–60 (2016).
Daibes, M. A., Safadi, R. R., Athamneh, T., Anees, I. F. & Constantino, R. E. ‘Half a woman, half a man; that is how they make me feel’: a qualitative study of rural Jordanian women’s experience of infertility. Cult. Health Sex. 20, 516–530 (2017).
Oyesanya, T. O. & Ward, E. C. Mental health in women with traumatic brain injury: a systematic review on depression and hope. Health Care Women Int. 37, 45–74 (2016).
Toor, G. K. et al. Long-term health service outcomes among women with traumatic brain injury. Arch. Phys. Med. Rehabil. 97, S54–S63 (2016).
Niemeier, J. P., Marwitz, J. H., Lesher, K., Walker, W. C. & Bushnik, T. Gender differences in executive functions following traumatic brain injury. Neuropsychol. Rehabil. 17, 293–313 (2007).
Forslund, M. V. et al. The trajectories of overall disability in the first 5 years after moderate and severe traumatic brain injury. Brain Inj. 31, 329–335 (2017).
De Hoyos, A. Issues on luck egalitarianism, responsibility, and intercultural healthcare policies. Camb. Q. Healthc. Ethics 25, 186–196 (2016).
Nunes, R. & Rego, G. Priority setting in health care: a complementary approach. Health Care Anal. 22, 292–303 (2014).
Gao, S., Kumar, R. G., Wisniewski, S. R. & Fabio, A. Disparities in health care utilization of adults with traumatic brain injuries are related to insurance, race, and ethnicity: a systematic review. J. Head Trauma Rehabil. 33, E40–E50 (2018).
World Health Organization. World Health Assembly 2012: gender, equity and human rights at the core of the health response. WHO http://www.who.int/pmnch/media/news/2012/20120519_wha_side_events/en (2012).
Sridharan, S., Maplazi, J., Shirodkar, A., Richardson, E. & Nakaima, A. Incorporating gender, equity, and human rights into the action planning process: moving from rhetoric to action. Glob. Health Action 9, 30870 (2016). This research explores how a theory-driven perspective of gender, equity and human rights can move into the action planning process. Nine specific recommendations are proposed for the WHO and other organizations to consider.
Clayton, J. A. & Collins, F. S. Policy: NIH to balance sex in cell and animal studies. Nature 509, 282–283 (2014). This article provides an overview of NIH plans to address the issue of sex and gender inclusion multi-dimensionally across biomedical research.
US Department of Health & Human Services. Consideration of sex as a biological variable in NIH-funded research. NIH https://grants.nih.gov/grants/guide/notice-files/NOT-OD-15-102.html (2015).
Government of Canada. Constitution Act, 1982, Schedule B to the Canada Act 1982 (UK), 1982, c 11 — Part I. Justice Laws Website http://laws-lois.justice.gc.ca/eng/Const/page-15.html (updated 7 Sep 2018).
Canadian Health Care. Canadian Health Act. CHC http://www.canadian-healthcare.org/page2.html (1984).
McCullough, L. D., McCarthy, M. M. & de Vries, G. J. NIH policy: status quo is also costly. Nature 510, 340 (2014).
Heidari, S., Babor, T. F., De Castro, P., Tort, S. & Curno, M. Sex and gender equity in research: rationale for the SAGER guidelines and recommended use. Res. Integr. Peer Rev. 1, 2 (2016).
Government of Canada. Sex and gender champions. Canadian Institutes of Health Research http://www.cihr-irsc.gc.ca/e/50652.html (2018).
Colantonio, A. Sex, gender, and traumatic brain injury: a commentary. Arch. Phys. Med. Rehabil. 97, S1–S4 (2016). Featured in a special sex, gender and traumatic brain injury issue of the journal, this article acknowledges the paucity of sex-stratified data in TBI research and its potential to hinder advancements in prevention, management and treatment.
Mollayeva, T. & Colantonio, A. Gender, sex and traumatic brain injury: transformative science to optimize patient outcomes. Healthc. Q. 20, 6–9 (2017).
Soares, J. M., Marques, P., Magalhïes, R., Santos, N. C. & Sousa, N. Brain structure across the lifespan: the influence of stress and mood. Front. Aging Neurosci. 6, 330 (2014).
May, A. Experience-dependent structural plasticity in the adult human brain. Trends Cogn. Sci. 15, 475–482 (2011).
Xiao, H., Yang, Y., Xi, J. & Chen, Z. Structural and functional connectivity in traumatic brain injury. Neural Regen. Res. 10, 2062 (2015).
Dall’Acqua, P. et al. Functional and structural network recovery after mild traumatic brain injury: a 1-year longitudinal study. Front. Hum. Neurosci. 11, 280 (2017).
Kwako, L. E. et al. Traumatic brain injury in intimate partner violence: a critical review of outcomes and mechanisms. Trauma Violence Abuse 12, 115–126 (2011).
Shiroma, E. J., Ferguson, P. L. & Pickelsimer, E. E. Prevalence of traumatic brain injury in an offender population: a meta-analysis. J. Correct. Health Care 16, 147–159 (2010).
Heyer, N. J. & Franklin, G. M. Work-related traumatic brain injury in Washington State, 1988 through 1990. Am. J. Public Health 84, 1106–1109 (1994).
Kristman, V. L. et al. The burden of work disability associated with mild traumatic brain injury in Ontario compensated workers: a prospective cohort study. Open Occup. Health Saf. J. 2, 1–8 (2010).
Acknowledgements
This work was supported by the Alzheimer’s Association under award AARF-16442937, by the Eunice Kennedy Shriver National Institute of Child Health & Human Development of the NIH under award R21HD089106 and the Canadian Institutes of Health Research (CIHR) Institute for Gender and Health grant #CGW-126580. The content is solely the responsibility of the authors and does not necessarily represent the official views of the Alzheimer’s Association, NIH or CIHR. We gratefully acknowledge the involvement of J. Babineau, information specialist at the Toronto Rehabilitation Institute–University Health Network for her help with the comprehensive literature search in MEDLINE and Web of Science.
Review criteria
The search strategy was developed in collaboration with a medical information specialist at a large rehabilitation teaching hospital. MEDLINE and Web of Science electronic databases were searched from inception until July 2017 (Supplementary Box 1). All searches were limited to studies in the English language. A repeat search was performed in all databases in May 2018 to identify the most recent publications. The following medical subject headings (MeSH) were used to identify publications of interest: “brain injuries, traumatic”, “gender identity”, “sex characteristics” and “social determinants of health”. “Intimate partner violence”, “homeless persons”, “prisoners” and “accidents, occupational” were also explored. The search was supplemented with citations from identified articles.
Author information
Authors and Affiliations
Contributions
T.M. and S.M researched data for the article. All authors made substantial contributions to discussions of the content, wrote the article and reviewed and edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Mollayeva, T., Mollayeva, S. & Colantonio, A. Traumatic brain injury: sex, gender and intersecting vulnerabilities. Nat Rev Neurol 14, 711–722 (2018). https://doi.org/10.1038/s41582-018-0091-y
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41582-018-0091-y
This article is cited by
-
Preso enhances mGluR1-mediated excitotoxicity by modulating the phosphorylation of mGluR1-Homer1 complex and facilitating an ER stress after traumatic brain injury
Cell Death Discovery (2024)
-
Overexpress miR-132 in the Brain Parenchyma by a Non-invasive Way Improves Tissue Repairment and Releases Memory Impairment After Traumatic Brain Injury
Cellular and Molecular Neurobiology (2024)
-
Effectiveness of brandt-daroff exercises in the treatment of benign paroxysmal positional vertigo: a systematic review of randomized controlled trials
European Archives of Oto-Rhino-Laryngology (2024)
-
Dynamic Changes and Effects of H2S, IGF-1, and GH in the Traumatic Brain Injury
Biochemical Genetics (2024)
-
Non-Invasive Brain Stimulation Combined with Neuromuscular Electrical Stimulation for Upper Limb Rehabilitation in Stroke Survivors: A Systematic Review
Current Physical Medicine and Rehabilitation Reports (2024)