Abstract
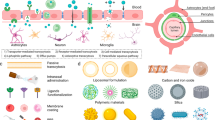
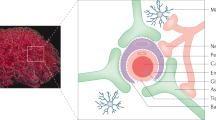
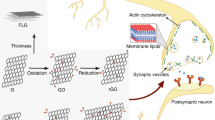
Despite the rising global incidence of central nervous system (CNS) disorders, CNS drug development remains challenging, with high costs, long pathways to clinical use and high failure rates. The CNS is highly protected by physiological barriers, in particular, the blood–brain barrier and the blood–cerebrospinal fluid barrier, which limit access of most drugs. Biomaterials can be designed to bypass or traverse these barriers, enabling the controlled delivery of drugs into the CNS. In this Review, we first examine the effects of normal and diseased CNS physiology on drug delivery to the brain and spinal cord. We then discuss CNS drug delivery designs and materials that are administered systemically, directly to the CNS, intranasally or peripherally through intramuscular injections. Finally, we highlight important challenges and opportunities for materials design for drug delivery to the CNS and the anticipated clinical impact of CNS drug delivery.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Wittchen, H.-U. et al. The size and burden of mental disorders and other disorders of the brain in Europe 2010. Eur. Neuropsychopharmacol. 21, 655–679 (2011).
Lindsley, C. W. 2013 Statistics for global prescription medications: CNS therapeutics maintain a leading position among small molecule therapeutics. ACS Chem. Neurosci. 5, 250–251 (2014).
Helmbrecht, H., Joseph, A., McKenna, M., Zhang, M. & Nance, E. Governing transport principles for nanotherapeutic application in the brain. Curr. Opin. Chem. Eng. 30, 112–119 (2020).
GBD 2016 Stroke Collaborators. Global, regional, and national burden of stroke, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 18, 439–458 (2019).
Zlokovic, B. V. Neurovascular mechanisms of Alzheimer’s neurodegeneration. Trends Neurosci. 28, 202–208 (2005).
Armulik, A. et al. Pericytes regulate the blood–brain barrier. Nature 468, 557–561 (2010).
Bell, R. D. et al. Pericytes control key neurovascular functions and neuronal phenotype in the adult brain and during brain aging. Neuron 68, 409–427 (2010).
Sweeney, M. D., Ayyadurai, S. & Zlokovic, B. V. Pericytes of the neurovascular unit: key functions and signaling pathways. Nat. Neurosci. 19, 771–783 (2016).
Abbott, N. J., Patabendige, A. A., Dolman, D. E., Yusof, S. R. & Begley, D. J. Structure and function of the blood–brain barrier. Neurobiol. Dis. 37, 13–25 (2010).
Vanlandewijck, M. et al. A molecular atlas of cell types and zonation in the brain vasculature. Nature 554, 475–480 (2018).
Pardridge, W. M. Drug transport across the blood–brain barrier. J. Cereb. Blood Flow Metab. 32, 1959–1972 (2012).
Groothuis, D. R. The blood-brain and blood-tumor barriers: a review of strategies for increasing drug delivery. Neuro-Oncology 2, 45–59 (2000).
Oldendorf, W. H. Brain uptake of radiolabeled amino acids, amines, and hexoses after arterial injection. Am. J. Physiol. 221, 1629–1639 (1971).
Banks, W. A. Brain meets body: the blood-brain barrier as an endocrine interface. Endocrinology 153, 4111–4119 (2012).
Pardridge, W. M. CSF, blood-brain barrier, and brain drug delivery. Expert Opin. Drug Deliv. 13, 963–975 (2016).
Pardridge, W. M. Drug transport in brain via the cerebrospinal fluid. Fluids Barriers CNS 8, 7 (2011).
Yamada, K. et al. Basic fibroblast growth factor prevents thalamic degeneration after cortical infarction. J. Cereb. Blood Flow Metab. 11, 472–478 (1991).
Day-Lollini, P. A., Stewart, G. R., Taylor, M. J., Johnson, R. M. & Chellman, G. J. Hyperplastic changes within the leptomeninges of the rat and monkey in response to chronic intracerebroventricular infusion of nerve growth factor. Exp. Neurol. 145, 24–37 (1997).
Cserr, H. F., Cooper, D. N., Suri, P. K. & Patlak, C. S. Efflux of radiolabeled polyethylene glycols and albumin from rat brain. Am. J. Physiol. 240, F319–F328 (1981).
Szentistvanyi, I., Patlak, C. S., Ellis, R. A. & Cserr, H. F. Drainage of interstitial fluid from different regions of rat brain. Am. J. Physiol. 246, F835–F844 (1984).
Henrich-Noack, P. et al. The blood–brain barrier and beyond: Nano-based neuropharmacology and the role of extracellular matrix. Nanomedicine 17, 359–379 (2019).
Wolak, D. J. & Thorne, R. G. Diffusion of macromolecules in the brain: implications for drug delivery. Mol. Pharm. 10, 1492–1504 (2013).
Sykova, E. & Nicholson, C. Diffusion in brain extracellular space. Physiol. Rev. 88, 1277–1340 (2008).
Nance, E. A. et al. A dense poly(ethylene glycol) coating improves penetration of large polymeric nanoparticles within brain tissue. Sci. Transl. Med. 4, 149ra119 (2012).
Patel, T., Zhou, J., Piepmeier, J. M. & Saltzman, W. M. Polymeric nanoparticles for drug delivery to the central nervous system. Adv. Drug Deliv. Rev. 64, 701–705 (2012).
Curtis, C., Toghani, D., Wong, B. & Nance, E. Colloidal stability as a determinant of nanoparticle behavior in the brain. Colloids Surf. B Biointerfaces 170, 673–682 (2018).
Morrison, P. F. & Dedrick, R. L. Transport of cisplatin in rat brain following microinfusion: an analysis. J. Pharm. Sci. 75, 120–128 (1986).
Wen, P. Y. & Kesari, S. Malignant gliomas in adults. N. Engl. J. Med. 359, 492–507 (2008).
Nduom, E. K., Yang, C., Merrill, M. J., Zhuang, Z. & Lonser, R. R. Characterization of the blood-brain barrier of metastatic and primary malignant neoplasms. J. Neurosurg. 119, 427–433 (2013).
Jain, R. K. Normalizing tumor microenvironment to treat cancer: bench to bedside to biomarkers. J. Clin. Oncol. 31, 2205–2218 (2013).
Wiranowska, M. & Rojiani, M. V. in Glioma – Exploring Its Biology and Practical Relevance Ch. 12 (ed. Ghosh, A.) (IntechOpen, 2011).
Yao, Q., Kou, L., Tu, Y. & Zhu, L. MMP-responsive ‘smart’ drug delivery and tumor targeting. Trends Pharmacol. Sci. 39, 766–781 (2018).
National Spinal Cord Injury Statistical Center (NSCISC). Spinal Cord Injury: Facts and Figures at a Glance (University of Alabama at Birmingham, 2021).
Lee, S. et al. A novel antagonist of p75NTR reduces peripheral expansion and CNS trafficking of pro-inflammatory monocytes and spares function after traumatic brain injury. J. Neuroinflammation 13, 88 (2016).
Centers for Disease Control and Prevention (CDC). Report to Congress on Traumatic Brain Injury in the United States: Epidemiology and Rehabilitation (National Center for Injury Prevention and Control; Division of Unintentional Injury Prevention, 2015).
Hulsebosch, C. E. Recent advances in pathophysiology and treatment of spinal cord injury. Adv. Physiol. Educ. 26, 238–255 (2002).
Beattie, M. S. Inflammation and apoptosis: linked therapeutic targets in spinal cord injury. Trends Mol. Med. 10, 580–583 (2004).
Wang, C. X., Nuttin, B., Heremans, H., Dom, R. & Gybels, J. Production of tumor necrosis factor in spinal cord following traumatic injury in rats. J. Neuroimmunol. 69, 151–156 (1996).
Ramlackhansingh, A. F. et al. Inflammation after trauma: microglial activation and traumatic brain injury. Ann. Neurol. 70, 374–383 (2011).
Kandell, R. M., Waggoner, L. E. & Kwon,E. J. Nanomedicine for acute brain injuries: insight from decades of cancer nanomedicine. Mol. Pharmaceutics https://doi.org/10.1021/acs.molpharmaceut.0c00287 (2020).
Kudryashev, J. A. et al. An activity-based nanosensor for traumatic brain injury. ACS Sens. 5, 686–692 (2020).
Delbary-Gossart, S. et al. A novel inhibitor of p75-neurotrophin receptor improves functional outcomes in two models of traumatic brain injury. Brain 139, 1762–1782 (2016).
Hurlbert, R. J. et al. Pharmacological therapy for acute spinal cord injury. Neurosurgery 72, 93–105 (2013).
Bowers, C. A., Kundu, B., Rosenbluth, J. & Hawryluk, G. W. Patients with spinal cord injuries favor administration of methylprednisolone. PLoS ONE 11, e0145991 (2016).
Fehlings, M. G. et al. A clinical practice guideline for the management of patients with acute spinal cord injury: recommendations on the use of methylprednisolone sodium succinate. Glob. Spine J. 7, 203S–211S (2017).
Hurlbert, R. J. & Hamilton, M. G. Methylprednisolone for acute spinal cord injury: 5-year practice reversal. Can. J. Neurol. Sci. 35, 41–45 (2008).
Angeli, C. A. et al. Recovery of over-ground walking after chronic motor complete spinal cord injury. N. Engl. J. Med. 379, 1244–1250 (2018).
Gill, M. L. et al. Neuromodulation of lumbosacral spinal networks enables independent stepping after complete paraplegia. Nat. Med. 24, 1677–1682 (2018).
Profaci, C. P., Munji, R. N., Pulido, R. S. & Daneman, R. The blood–brain barrier in health and disease: Important unanswered questions. J. Exp. Med. 217, e20190062 (2020).
Yang, A. C. et al. Physiological blood–brain transport is impaired with age by a shift in transcytosis. Nature 583, 425–430 (2020).
Montagne, A. et al. Blood-brain barrier breakdown in the aging human hippocampus. Neuron 85, 296–302 (2015).
Khandaker, G. M. et al. Inflammation and immunity in schizophrenia: implications for pathophysiology and treatment. Lancet Psychiatry 2, 258–270 (2015).
Iturria-Medina, Y. et al. Early role of vascular dysregulation on late-onset Alzheimer’s disease based on multifactorial data-driven analysis. Nat. Commun. 7, 11934 (2016).
Winkler, E. A. et al. Blood–spinal cord barrier disruption contributes to early motor-neuron degeneration in ALS-model mice. Proc. Natl Acad. Sci. USA 111, E1035–E1042 (2014).
Yamazaki, Y. et al. Selective loss of cortical endothelial tight junction proteins during Alzheimer’s disease progression. Brain 142, 1077–1092 (2019).
Yamada, M. & Hamaguchi, T. The sulfation code for propagation of neurodegeneration. J. Biol. Chem. 293, 10841–10842 (2018).
Blanchard, J. W. et al. Reconstruction of the human blood–brain barrier in vitro reveals a pathogenic mechanism of APOE4 in pericytes. Nat. Med. 26, 952–963 (2020).
Kisler, K. et al. Pericyte degeneration leads to neurovascular uncoupling and limits oxygen supply to brain. Nat. Neurosci. 20, 406–416 (2017).
Sweeney, M. D., Sagare, A. P. & Zlokovic, B. V. Blood–brain barrier breakdown in Alzheimer disease and other neurodegenerative disorders. Nat. Rev. Neurol. 14, 133–150 (2018).
Zlokovic, B. V. Neurovascular pathways to neurodegeneration in Alzheimer’s disease and other disorders. Nat. Rev. Neurosci. 12, 723–738 (2011).
Winkler, E. A., Sengillo, J. D., Bell, R. D., Wang, J. & Zlokovic, B. V. Blood–spinal cord barrier pericyte reductions contribute to increased capillary permeability. J. Cereb. Blood Flow Metab. 32, 1841–1852 (2012).
Nikolakopoulou, A. M. et al. Pericyte loss leads to circulatory failure and pleiotrophin depletion causing neuron loss. Nat. Neurosci. 22, 1089–1098 (2019).
Campbell, B. C. V. & Khatri, P. Stroke. Lancet 396, 129–142 (2020).
Wardlaw, J. M. et al. Recombinant tissue plasminogen activator for acute ischaemic stroke: an updated systematic review and meta-analysis. Lancet 379, 2364–2372 (2012).
Davis, S. M. & Donnan, G. A. 4.5 hours: the new time window for tissue plasminogen activator in stroke. Stroke 40, 2266–2267 (2009).
Berkhemer, O. A. et al. A randomized trial of intraarterial treatment for acute ischemic stroke. N. Engl. J. Med. 372, 11–20 (2015).
Campbell, B. C. et al. Endovascular therapy for ischemic stroke with perfusion-imaging selection. N. Engl. J. Med. 372, 1009–1018 (2015).
Goyal, M. et al. Randomized assessment of rapid endovascular treatment of ischemic stroke. N. Engl. J. Med. 372, 1019–1030 (2015).
Saver, J. L. et al. Stent-retriever thrombectomy after intravenous t-PA vs. t-PA alone in stroke. N. Engl. J. Med. 372, 2285–2295 (2015).
Bracard, S. et al. Mechanical thrombectomy after intravenous alteplase versus alteplase alone after stroke (THRACE): a randomised controlled trial. Lancet Neurol. 15, 1138–1147 (2016).
Nogueira, R. G. et al. Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N. Engl. J. Med. 378, 11–21 (2018).
Hettiaratchi, M. H. et al. Local delivery of stabilized chondroitinase ABC degrades chondroitin sulfate proteoglycans in stroke-injured rat brains. J. Control. Release 297, 14–25 (2019).
George, P. M. et al. Engineered stem cell mimics to enhance stroke recovery. Biomaterials 178, 63–72 (2018).
Bolan, F., Louca, I., Heal, C. & Cunningham, C. J. The potential of biomaterial-based approaches as therapies for ischemic stroke: a systematic review and meta-analysis of pre-clinical studies. Front. Neurol. 10, 924 (2019).
Saraiva, C. et al. MicroRNA-124-loaded nanoparticles increase survival and neuronal differentiation of neural stem cells in vitro but do not contribute to stroke outcome in vivo. PLoS ONE 13, e0193609 (2018).
Chamorro, A., Dirnagl, U., Urra, X. & Planas, A. M. Neuroprotection in acute stroke: targeting excitotoxicity, oxidative and nitrosative stress, and inflammation. Lancet Neurol. 15, 869–881 (2016).
Pardridge, W. M. Why is the global CNS pharmaceutical market so under-penetrated? Drug Discov. Today 7, 5–7 (2002).
Furtado, D. et al. Overcoming the blood–brain barrier: the role of nanomaterials in treating neurological diseases. Adv. Mater. 30, 1801362 (2018).
Tang, W. et al. Emerging blood–brain-barrier-crossing nanotechnology for brain cancer theranostics. Chem. Soc. Rev. 48, 2967–3014 (2019).
Johnsen, K. B., Burkhart, A., Thomsen, L. B., Andresen, T. L. & Moos, T. Targeting the transferrin receptor for brain drug delivery. Prog. Neurobiol. 181, 101665 (2019).
van Rooy, I., Mastrobattista, E., Storm, G., Hennink, W. E. & Schiffelers, R. M. Comparison of five different targeting ligands to enhance accumulation of liposomes into the brain. J. Control. Release 150, 30–36 (2011).
Israel, L. L. et al. A combination of tri-leucine and angiopep-2 drives a polyanionic polymalic acid nanodrug platform across the blood–brain barrier. ACS Nano 13, 1253–1271 (2019).
Yu, Y. J. et al. Boosting brain uptake of a therapeutic antibody by reducing its affinity for a transcytosis target. Sci. Transl. Med. 3, 84ra44 (2011).
Couch, J. A. et al. Addressing safety liabilities of TfR bispecific antibodies that cross the blood-brain barrier. Sci. Transl. Med. 5, 183ra157 (2013).
Bien-Ly, N. et al. Transferrin receptor (TfR) trafficking determines brain uptake of TfR antibody affinity variants. J. Exp. Med. 211, 233–244 (2014).
Lesley, J., Schulte, R. & Woods, J. Modulation of transferrin receptor expression and function by anti-transferrin receptor antibodies and antibody fragments. Exp. Cell Res. 182, 215–233 (1989).
Wiley, D. T., Webster, P., Gale, A. & Davis, M. E. Transcytosis and brain uptake of transferrin-containing nanoparticles by tuning avidity to transferrin receptor. Proc. Natl Acad. Sci. USA 110, 8662–8667 (2013).
Johnsen, K. B. et al. Antibody affinity and valency impact brain uptake of transferrin receptor-targeted gold nanoparticles. Theranostics 8, 3416–3436 (2018).
Clark, A. J. & Davis, M. E. Increased brain uptake of targeted nanoparticles by adding an acid-cleavable linkage between transferrin and the nanoparticle core. Proc. Natl Acad. Sci. USA 112, 12486–12491 (2015).
Wyatt, E. A. & Davis, M. E. Method of establishing breast cancer brain metastases affects brain uptake and efficacy of targeted, therapeutic nanoparticles. Bioeng. Transl. Med. 4, 30–37 (2019).
Cai, L. et al. Endo/lysosome-escapable delivery depot for improving BBB transcytosis and neuron targeted therapy of Alzheimer’s disease. Adv. Funct. Mater. 30, 1909999 (2020).
Li, S.-D. & Huang, L. Pharmacokinetics and biodistribution of nanoparticles. Mol. Pharm. 5, 496–504 (2008).
Betzer, O. et al. The effect of nanoparticle size on the ability to cross the blood–brain barrier: an in vivo study. Nanomedicine 12, 1533–1546 (2017).
Nowak, M., Brown, T. D., Graham, A., Helgeson, M. E. & Mitragotri, S. Size, shape, and flexibility influence nanoparticle transport across brain endothelium under flow. Bioeng. Transl. Med. 5, e10153 (2020).
Moos, T. & Morgan, E. H. Restricted transport of anti-transferrin receptor antibody (OX26) through the blood–brain barrier in the rat. J. Neurochem. 79, 119–129 (2001).
Johnsen, K. B. et al. Targeting transferrin receptors at the blood-brain barrier improves the uptake of immunoliposomes and subsequent cargo transport into the brain parenchyma. Sci. Rep. 7, 10396 (2017).
Marcos-Contreras, O. A. et al. Selective targeting of nanomedicine to inflamed cerebral vasculature to enhance the blood–brain barrier. Proc. Natl Acad. Sci. USA 117, 3405–3414 (2020).
Marcos-Contreras, O. A. et al. Combining vascular targeting and the local first pass provides 100-fold higher uptake of ICAM-1-targeted vs untargeted nanocarriers in the inflamed brain. J. Control. Release 301, 54–61 (2019).
Gonzalez-Carter, D. et al. Targeting nanoparticles to the brain by exploiting the blood–brain barrier impermeability to selectively label the brain endothelium. Proc. Natl Acad. Sci. USA 117, 19141–19150 (2020).
Stein, S. C. et al. Erythrocyte-bound tissue plasminogen activator is neuroprotective in experimental traumatic brain injury. J. Neurotrauma 26, 1585–1592 (2009).
Brenner, J. S. et al. Red blood cell-hitchhiking boosts delivery of nanocarriers to chosen organs by orders of magnitude. Nat. Commun. 9, 2684 (2018).
Klyachko, N. L. et al. Macrophages with cellular backpacks for targeted drug delivery to the brain. Biomaterials 140, 79–87 (2017).
Hou, J. et al. Accessing neuroinflammation sites: Monocyte/neutrophil-mediated drug delivery for cerebral ischemia. Sci. Adv. 5, eaau8301 (2019).
Zheng, M., Huang, M., Ma, X., Chen, H. & Gao, X. Harnessing exosomes for the development of brain drug delivery systems. Bioconjug. Chem. 30, 994–1005 (2019).
Yuan, D. et al. Macrophage exosomes as natural nanocarriers for protein delivery to inflamed brain. Biomaterials 142, 1–12 (2017).
Alvarez-Erviti, L. et al. Delivery of siRNA to the mouse brain by systemic injection of targeted exosomes. Nat. Biotechnol. 29, 341–345 (2011).
Tian, T. et al. Surface functionalized exosomes as targeted drug delivery vehicles for cerebral ischemia therapy. Biomaterials 150, 137–149 (2018).
Haney, M. J. et al. TPP1 delivery to lysosomes with extracellular vesicles and their enhanced brain distribution in the animal model of batten disease. Adv. Healthc. Mater. 8, 1801271 (2019).
Rapoport, S. I., Hori, M. & Klatzo, I. Testing of a hypothesis for osmotic opening of the blood-brain barrier. Am. J. Physiol. 223, 323–331 (1972).
Chian, R. J. et al. IGF-1:tetanus toxin fragment C fusion protein improves delivery of IGF-1 to spinal cord but fails to prolong survival of ALS mice. Brain Res. 1287, 1–19 (2009).
Chu, C. et al. Optimization of osmotic blood-brain barrier opening to enable intravital microscopy studies on drug delivery in mouse cortex. J. Control. Release 317, 312–321 (2020).
Karakatsani, M. E. et al. Amelioration of the nigrostriatal pathway facilitated by ultrasound-mediated neurotrophic delivery in early Parkinson’s disease. J. Control. Release 303, 289–301 (2019).
Rich, M. C. et al. Focused ultrasound blood brain barrier opening mediated delivery of MRI-visible albumin nanoclusters to the rat brain for localized drug delivery with temporal control. J. Control. Release 324, 172–180 (2020).
Thévenot, E. et al. Targeted delivery of self-complementary adeno-associated virus serotype 9 to the brain, using magnetic resonance imaging-guided focused ultrasound. Hum. Gene Ther. 23, 1144–1155 (2012).
Zhou, Y., Yang, K., Cui, J., Ye, J. & Deng, C. Controlled permeation of cell membrane by single bubble acoustic cavitation. J. Control. Release 157, 103–111 (2012).
Lipsman, N. et al. Blood–brain barrier opening in Alzheimer’s disease using MR-guided focused ultrasound. Nat. Commun. 9, 2336 (2018).
Carpentier, A. et al. Clinical trial of blood-brain barrier disruption by pulsed ultrasound. Sci. Transl. Med. 8, 343re2 (2016).
Langer, R. & Folkman, J. Polymers for the sustained release of proteins and other macromolecules. Nature 263, 797–800 (1976).
Wang, P. P., Frazier, J. & Brem, H. Local drug delivery to the brain. Adv. Drug Deliv. Rev. 54, 987–1013 (2002).
Walter, K. A. et al. Interstitial taxol delivered from a biodegradable polymer implant against experimental malignant glioma. Cancer Res. 54, 2207–2212 (1994).
Sampath, P. et al. Camptothecin analogs in malignant gliomas: comparative analysis and characterization. J. Neurosurg. 98, 570–577 (2003).
Brem, S. et al. Local delivery of temozolomide by biodegradable polymers is superior to oral administration in a rodent glioma model. Cancer Chemother. Pharmacol. 60, 643–650 (2007).
Grossman, S. A. et al. The intracerebral distribution of BCNU delivered by surgically implanted biodegradable polymers. J. Neurosurg. 76, 640–647 (1992).
Perry, J., Chambers, A., Spithoff, K. & Laperriere, N. Gliadel wafers in the treatment of malignant glioma: a systematic review. Curr. Oncol. 14, 189–194 (2007).
Fung, L. K., Shin, M., Tyler, B., Brem, H. & Saltzman, W. M. Chemotherapeutic drugs released from polymers: distribution of 1,3-bis(2-chloroethyl)-l-nitrosourea in the rat brain. Pharm. Res. 13, 671–682 (1996).
Wait, S. D., Prabhu, R. S., Burri, S. H., Atkins, T. G. & Asher, A. L. Polymeric drug delivery for the treatment of glioblastoma. Neuro-Oncology 17, ii9–ii23 (2015).
Ramachandran, R. et al. Theranostic 3-dimensional nano brain-implant for prolonged and localized treatment of recurrent glioma. Sci. Rep. 7, 43271 (2017).
Lee, J. H. et al. Collagen gel three-dimensional matrices combined with adhesive proteins stimulate neuronal differentiation of mesenchymal stem cells. J. R. Soc. Interface 8, 998–1010 (2011).
Jeong, D. U. et al. Hydrogel-mediated local delivery of dexamethasone reduces neuroinflammation after traumatic brain injury. Biomed. Mater. 16, 035002 (2021).
Tsintou, M. et al. The use of hydrogel-delivered extracellular vesicles in recovery of motor function in stroke: a testable experimental hypothesis for clinical translation including behavioral and neuroimaging assessment approaches. Neural Regen. Res. 16, 605–613 (2021).
Alvarado-Velez, M. et al. Immuno-suppressive hydrogels enhance allogeneic MSC survival after transplantation in the injured brain. Biomaterials 266, 120419 (2021).
Piantino, J., Burdick, J. A., Goldberg, D., Langer, R. & Benowitz, L. I. An injectable, biodegradable hydrogel for trophic factor delivery enhances axonal rewiring and improves performance after spinal cord injury. Exp. Neurol. 201, 359–367 (2006).
Sellers, D. L., Kim, T. H., Mount, C. W., Pun, S. H. & Horner, P. J. Poly(lactic-co-glycolic) acid microspheres encapsulated in Pluronic F-127 prolong hirudin delivery and improve functional recovery from a demyelination lesion. Biomaterials 35, 8895–8902 (2014).
Chu, D. S. et al. MMP9-sensitive polymers mediate environmentally-responsive bivalirudin release and thrombin inhibition. Biomater. Sci. 3, 41–45 (2015).
He, W., Reaume, M., Hennenfent, M., Lee, B. P. & Rajachar, R. Biomimetic hydrogels with spatial- and temporal-controlled chemical cues for tissue engineering. Biomater. Sci. 8, 3248–3269 (2020).
Taylor, S. J., McDonald, J. W. III & Sakiyama-Elbert, S. E. Controlled release of neurotrophin-3 from fibrin gels for spinal cord injury. J. Control. Release 98, 281–294 (2004).
Nguyen, L. H. et al. Three-dimensional aligned nanofibers-hydrogel scaffold for controlled non-viral drug/gene delivery to direct axon regeneration in spinal cord injury treatment. Sci. Rep. 7, 42212 (2017).
George, P. M. et al. Electrical preconditioning of stem cells with a conductive polymer scaffold enhances stroke recovery. Biomaterials 142, 31–40 (2017).
Leprince, L., Dogimont, A., Magnin, D. & Demoustier-Champagne, S. Dexamethasone electrically controlled release from polypyrrole-coated nanostructured electrodes. J. Mater. Sci. Mater. Med. 21, 925–930 (2010).
Gao, W. & Borgens, R. B. Remote-controlled eradication of astrogliosis in spinal cord injury via electromagnetically-induced dexamethasone release from “smart” nanowires. J. Control. Release 211, 22–27 (2015).
Du, Z. J., Bi, G.-Q. & Cui, X. T. Electrically controlled neurochemical release from dual-layer conducting polymer films for precise modulation of neural network activity in rat barrel cortex. Adv. Funct. Mater. 28, 1703988 (2018).
Koch, B., Rubino, I., Quan, F. S., Yoo, B. & Choi, H. J. Microfabrication for drug delivery. Materials 9, 646 (2016).
Tian, X. et al. Injectable PLGA-coated ropivacaine produces a long-lasting analgesic effect on incisional pain and neuropathic pain. J. Pain 22, 180–195 (2021).
Menei, P., Montero-Menei, C., Venier, M. C. & Benoit, J. P. Drug delivery into the brain using poly(lactide-co-glycolide) microspheres. Expert Opin. Drug Deliv. 2, 363–376 (2005).
Menei, P. et al. Local and sustained delivery of 5-fluorouracil from biodegradable microspheres for the radiosensitization of malignant glioma: a randomized phase II trial. Neurosurgery 56, 242–248 (2005). discussion 242–248.
Bege, N. et al. In situ forming nimodipine depot system based on microparticles for the treatment of posthemorrhagic cerebral vasospasm. Eur. J. Pharm. Biopharm. 84, 99–105 (2013).
Hanggi, D. et al. Dose-related efficacy of a continuous intracisternal nimodipine treatment on cerebral vasospasm in the rat double subarachnoid hemorrhage model. Neurosurgery 64, 1155–1159 (2009). discussion 1159–1161.
Hanggi, D. et al. Local delivery of nimodipine by prolonged-release microparticles — feasibility, effectiveness and dose-finding in experimental subarachnoid hemorrhage. PLoS ONE 7, e42597 (2012).
Nance, E. Brain-penetrating nanoparticles for analysis of the brain microenvironment. Methods Mol. Biol. 1570, 91–104 (2017).
Nance, E. et al. Brain-penetrating nanoparticles improve paclitaxel efficacy in malignant glioma following local administration. ACS Nano 8, 10655–10664 (2014).
Ranganath, S. H. et al. The use of submicron/nanoscale PLGA implants to deliver paclitaxel with enhanced pharmacokinetics and therapeutic efficacy in intracranial glioblastoma in mice. Biomaterials 31, 5199–5207 (2010).
El Demerdash, N., Kedda, J., Ram, N., Brem, H. & Tyler, B. Novel therapeutics for brain tumors: current practice and future prospects. Expert Opin. Drug Deliv. 17, 9–21 (2020).
During, M. J. et al. Biochemical and behavioral recovery in a rodent model of Parkinson’s disease following stereotactic implantation of dopamine-containing liposomes. Exp. Neurol. 115, 193–199 (1992).
Zhigaltsev, I. V. et al. Liposomes containing dopamine entrapped in response to transmembrane ammonium sulfate gradient as carrier system for dopamine delivery into the brain of parkinsonian mice. J. Liposome Res. 11, 55–71 (2001).
Zhang, C. et al. Convection enhanced delivery of cisplatin-loaded brain penetrating nanoparticles cures malignant glioma in rats. J. Control. Release 263, 112–119 (2017).
Saucier-Sawyer, J. K. et al. Distribution of polymer nanoparticles by convection-enhanced delivery to brain tumors. J. Control. Release 232, 103–112 (2016).
Kunwar, S. et al. Phase III randomized trial of CED of IL13-PE38QQR vs Gliadel wafers for recurrent glioblastoma. Neuro-Oncology 12, 871–881 (2010).
Allard, E., Passirani, C. & Benoit, J. P. Convection-enhanced delivery of nanocarriers for the treatment of brain tumors. Biomaterials 30, 2302–2318 (2009).
Chen, M. Y. et al. Surface properties, more than size, limiting convective distribution of virus-sized particles and viruses in the central nervous system. J. Neurosurg. 103, 311–319 (2005).
Zhang, C. et al. Strategies to enhance the distribution of nanotherapeutics in the brain. J. Control. Release 267, 232–239 (2017).
Lonser, R. R., Akhter, A. S., Zabek, M., Elder, J. B. & Bankiewicz, K. S. Direct convective delivery of adeno-associated virus gene therapy for treatment of neurological disorders. J. Neurosurg. 134, 1751–1763 (2020).
Johnston, L. C. et al. Clinically relevant effects of convection-enhanced delivery of AAV2-GDNF on the dopaminergic nigrostriatal pathway in aged rhesus monkeys. Hum. Gene Ther. 20, 497–510 (2009).
Papisov, M. I., Belov, V. V. & Gannon, K. S. Physiology of the intrathecal bolus: the leptomeningeal route for macromolecule and particle delivery to CNS. Mol. Pharm. 10, 1522–1532 (2013).
Iliff, J. J. et al. A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid beta. Sci. Transl. Med. 4, 147ra111 (2012).
Fowler, M. J. et al. Intrathecal drug delivery in the era of nanomedicine. Adv. Drug Deliv. Rev. 165, 77–95 (2020).
Tan, J. Y., Sellers, D. L., Pham, B., Pun, S. H. & Horner, P. J. Non-viral nucleic acid delivery strategies to the central nervous system. Front. Mol. Neurosci. 9, 108 (2016).
Wei, H. et al. Dual responsive, stabilized nanoparticles for efficient in vivo plasmid delivery. Angew. Chem. Int. Ed. Engl. 52, 5377–5381 (2013).
Schellinger, J. G. et al. Melittin-grafted HPMA-oligolysine based copolymers for gene delivery. Biomaterials 34, 2318–2326 (2013).
Cheng, Y., Yumul, R. C. & Pun, S. H. Virus-inspired polymer for efficient in vitro and in vivo gene delivery. Angew. Chem. Int. Ed. Engl. 55, 12013–12017 (2016).
Varkouhi, A. K., Scholte, M., Storm, G. & Haisma, H. J. Endosomal escape pathways for delivery of biologicals. J. Control. Release 151, 220–228 (2011).
Householder, K. T., Dharmaraj, S., Sandberg, D. I., Wechsler-Reya, R. J. & Sirianni, R. W. Fate of nanoparticles in the central nervous system after intrathecal injection in healthy mice. Sci. Rep. 9, 12587 (2019).
Calias, P., Banks, W. A., Begley, D., Scarpa, M. & Dickson, P. Intrathecal delivery of protein therapeutics to the brain: A critical reassessment. Pharmacol. Ther. 144, 114–122 (2014).
Khan, A. R., Liu, M., Khan, M. W. & Zhai, G. Progress in brain targeting drug delivery system by nasal route. J. Control. Release 268, 364–389 (2017).
Sellers, D. L. et al. Targeting ligands deliver model drug cargo into the central nervous system along autonomic neurons. ACS Nano 13, 10961–10971 (2019).
Poovaiah, N. et al. Treatment of neurodegenerative disorders through the blood–brain barrier using nanocarriers. Nanoscale 10, 16962–16983 (2018).
Yamamoto, A. et al. Absorption of water-soluble compounds with different molecular weights and [Asu1.7]-eel calcitonin from various mucosal administration sites. J. Control. Release 76, 363–374 (2001).
Thorne, R. G., Pronk, G. J., Padmanabhan, V. & Frey, W. H. Delivery of insulin-like growth factor-I to the rat brain and spinal cord along olfactory and trigeminal pathways following intranasal administration. Neuroscience 127, 481–496 (2004).
Miyake, M. M. & Bleier, B. S. The blood-brain barrier and nasal drug delivery to the central nervous system. Am. J. Rhinol. Allergy 29, 124–127 (2015).
Shrewsbury, S. B. et al. The SNAP 101 double-blind, placebo/active-controlled, safety, pharmacokinetic, and pharmacodynamic study of INP105 (nasal olanzapine) in healthy adults. J. Clin. Psychiatry 81, 19m13086 (2020).
Van de Bittner, G. C. et al. Positron emission tomography assessment of the intranasal delivery route for orexin A. ACS Chem. Neurosci. 9, 358–368 (2018).
Lochhead, J. J. & Thorne, R. G. Intranasal delivery of biologics to the central nervous system. Adv. Drug Deliv. Rev. 64, 614–628 (2012).
Song, Q. et al. Biomimetic ApoE-reconstituted high density lipoprotein nanocarrier for blood–brain barrier penetration and amyloid beta-targeting drug delivery. Mol. Pharm. 13, 3976–3987 (2016).
Bourganis, V., Kammona, O., Alexopoulos, A. & Kiparissides, C. Recent advances in carrier mediated nose-to-brain delivery of pharmaceutics. Eur. J. Pharm. Biopharm. 128, 337–362 (2018).
Haque, S., Md, S., Sahni, J. K., Ali, J. & Baboota, S. Development and evaluation of brain targeted intranasal alginate nanoparticles for treatment of depression. J. Psychiatr. Res. 48, 1–12 (2014).
Zada, M. H., Kubek, M., Khan, W., Kumar, A. & Domb, A. Dispersible hydrolytically sensitive nanoparticles for nasal delivery of thyrotropin releasing hormone (TRH). J. Control. Release 295, 278–289 (2019).
Ahmad, E. et al. Evidence of nose-to-brain delivery of nanoemulsions: cargoes but not vehicles. Nanoscale 9, 1174–1183 (2017).
Rinaldi, F. et al. inPentasomes: An innovative nose-to-brain pentamidine delivery blunts MPTP parkinsonism in mice. J. Control. Release 294, 17–26 (2019).
Mistry, A., Stolnik, S. & Illum, L. Nose-to-brain delivery: investigation of the transport of nanoparticles with different surface characteristics and sizes in excised porcine olfactory epithelium. Mol. Pharm. 12, 2755–2766 (2015).
Sonvico, F. et al. Surface-modified nanocarriers for nose-to-brain delivery: from bioadhesion to targeting. Pharmaceutics 10, 34 (2018).
Kamei, N. et al. Effective nose-to-brain delivery of exendin-4 via coadministration with cell-penetrating peptides for improving progressive cognitive dysfunction. Sci. Rep. 8, 17641 (2018).
Tosolini, A. P. & Sleigh, J. N. Intramuscular delivery of gene therapy for targeting the nervous system. Front. Mol. Neurosci. 13, 1047–1016 (2020).
Chen, Z., Fan, G., Li, A., Yuan, J. & Xu, T. rAAV2-retro enables extensive and high-efficient transduction of lower motor neurons following intramuscular injection. Mol. Ther. Methods Clin. Dev. 17, 21–33 (2020).
Xu, X. et al. Viral vectors for neural circuit mapping and recent advances in trans-synaptic anterograde tracers. Neuron 107, 1029–1047 (2020).
Towne, C., Schneider, B. L., Kieran, D., Redmond, D. E. Jr. & Aebischer, P. Efficient transduction of non-human primate motor neurons after intramuscular delivery of recombinant AAV serotype 6. Gene Ther. 17, 141–146 (2010).
Davidson, B. L. & Breakefield, X. O. Viral vectors for gene delivery to the nervous system. Nat. Rev. Neurosci. 4, 353–364 (2003).
Tosolini, A. P. & Morris, R. Targeting motor end plates for delivery of adenoviruses: an approach to maximize uptake and transduction of spinal cord motor neurons. Sci. Rep. 6, 33058 (2016).
Francis, J. W. et al. Tetanus toxin fragment C as a vector to enhance delivery of proteins to the CNS. Brain Res. 1011, 7–13 (2004).
Stoeckel, K., Schwab, M. & Thoenen, H. Role of gangliosides in the uptake and retrograde axonal transport of cholera and tetanus toxin as compared to nerve growth factor and wheat germ agglutinin. Brain Res. 132, 273–285 (1977).
Li, J. et al. Identification of peptide sequences that target to the brain using in vivo phage display. Amino Acids 42, 2373–2381 (2011).
Sellers, D. L. et al. Targeted axonal import (TAxI) peptide delivers functional proteins into spinal cord motor neurons after peripheral administration. Proc. Natl Acad. Sci. USA 113, 2514–2519 (2016).
Kerman, I. A., Enquist, L. W., Watson, S. J. & Yates, B. J. Brainstem substrates of sympatho-motor circuitry identified using trans-synaptic tracing with pseudorabies virus recombinants. J. Neurosci. 23, 4657–4666 (2003).
Card, J. P. et al. Neurotropic properties of pseudorabies virus: uptake and transneuronal passage in the rat central nervous system. J. Neurosci. 10, 1974–1994 (1990).
Thorne, R. G. & Frey, W. H. II Delivery of neurotrophic factors to the central nervous system: pharmacokinetic considerations. Clin. Pharmacokinet. 40, 907–946 (2001).
Lee, D. C., Sellers, D. L., Liu, F., Boydston, A. J. & Pun, S. H. Synthesis and characterization of anionic poly(cyclopentadienylene vinylene) and its use in conductive hydrogels. Angew. Chem. Int. Ed. 59, 13430–13436 (2020).
Guo, B. & Ma, P. X. Conducting polymers for tissue engineering. Biomacromolecules 19, 1764–1782 (2018).
Mazzini, L. et al. Results from phase I clinical trial with intraspinal injection of neural stem cells in amyotrophic lateral sclerosis: a long-term outcome. Stem Cells Transl. Med. 8, 887–897 (2019).
Zhao, Y. et al. Dual targeted nanocarrier for brain ischemic stroke treatment. J. Control. Release 233, 64–71 (2016).
Xia, H., Anderson, B., Mao, Q. & Davidson, B. L. Recombinant human adenovirus: targeting to the human transferrin receptor improves gene transfer to brain microcapillary endothelium. J. Virol. 74, 11359–11366 (2000).
Maier, K. E. et al. A new transferrin receptor aptamer inhibits new world hemorrhagic fever mammarenavirus entry. Mol. Ther. Nucleic Acids 5, e321 (2016).
Wu, X. et al. Elucidation and structural modeling of CD71 as a molecular target for cell-specific aptamer binding. J. Am. Chem. Soc. 141, 10760–10769 (2019).
Fan, K. et al. Ferritin nanocarrier traverses the blood brain barrier and kills glioma. ACS Nano 12, 4105–4115 (2018).
Kariolis, M. S. et al. Brain delivery of therapeutic proteins using an Fc fragment blood-brain barrier transport vehicle in mice and monkeys. Sci. Transl. Med. 12, eaay1359 (2020).
Li, X. et al. Enhanced in vivo blood–brain barrier penetration by circular Tau–transferrin receptor bifunctional aptamer for tauopathy therapy. J. Am. Chem. Soc. 142, 3862–3872 (2020).
Demeule, M. et al. Identification and design of peptides as a new drug delivery system for the brain. J. Pharmacol. Exp. Ther. 324, 1064–1072 (2008).
Dal Magro, R. et al. ApoE-modified solid lipid nanoparticles: A feasible strategy to cross the blood-brain barrier. J. Control. Release 249, 103–110 (2017).
He, C. et al. Two-step targeted hybrid nanoconstructs increase brain penetration and efficacy of the therapeutic antibody trastuzumab against brain metastasis of HER2-positive breast cancer. Adv. Funct. Mater. 28, 1705668 (2018).
Li, J. et al. A multifunctional polymeric nanotheranostic system delivers doxorubicin and imaging agents across the blood–brain barrier targeting brain metastases of breast cancer. ACS Nano 8, 9925–9940 (2014).
Jiang, Y., Yang, W., Zhang, J., Meng, F. & Zhong, Z. Protein toxin chaperoned by LRP-1-targeted virus-mimicking vesicles induces high-efficiency glioblastoma therapy in vivo. Adv. Mater. 30, 1800316 (2018).
Shi, X.-X. et al. Angiopep-2 conjugated nanoparticles loaded with doxorubicin for the treatment of primary central nervous system lymphoma. Biomater. Sci. 8, 1290–1297 (2020).
Tao, J. et al. Angiopep-2-conjugated “core–shell” hybrid nanovehicles for targeted and pH-triggered delivery of arsenic trioxide into glioma. Mol. Pharm. 16, 786–797 (2019).
Han, L. et al. Systemic delivery of monoclonal antibodies to the central nervous system for brain tumor therapy. Adv. Mater. 31, e1805697 (2019).
Meng, X. et al. Dual functionalized brain-targeting nanoinhibitors restrain temozolomide-resistant glioma via attenuating EGFR and MET signaling pathways. Nat. Commun. 11, 594 (2020).
Wen, J. et al. Sustained delivery and molecular targeting of a therapeutic monoclonal antibody to metastases in the central nervous system of mice. Nat. Biomed. Eng. 3, 706–716 (2019).
Xie, J. et al. Dual-sensitive nanomicelles enhancing systemic delivery of therapeutically active antibodies specifically into the brain. ACS Nano 14, 6729–6742 (2020).
You, L. et al. Targeted brain delivery of rabies virus glycoprotein 29-modified deferoxamine-loaded nanoparticles reverses functional deficits in parkinsonian mice. ACS Nano 12, 4123–4139 (2018).
Guo, Q. et al. A dual-ligand fusion peptide improves the brain-neuron targeting of nanocarriers in Alzheimer’s disease mice. J. Control. Release 320, 347–362 (2020).
Wang, P. et al. Systemic delivery of BACE1 siRNA through neuron-targeted nanocomplexes for treatment of Alzheimer’s disease. J. Control. Release 279, 220–233 (2018).
Burtea, C. et al. Magnetic resonance molecular imaging of vascular cell adhesion molecule-1 expression in inflammatory lesions using a peptide-vectorized paramagnetic imaging probe. J. Med. Chem. 52, 4725–4742 (2009).
Lutton, E. M. et al. Acute administration of catalase targeted to ICAM-1 attenuates neuropathology in experimental traumatic brain injury. Sci. Rep. 7, 3846 (2017).
Fehlings, M. G. et al. Rho inhibitor VX-210 in acute traumatic subaxial cervical spinal cord injury: design of the SPinal Cord Injury Rho INhibition InvestiGation (SPRING) Clinical Trial. J. Neurotrauma 35, 1049–1056 (2018).
Dautry-Varsat, A., Ciechanover, A. & Lodish, H. F. pH and the recycling of transferrin during receptor-mediated endocytosis. Proc. Natl Acad. Sci. USA 80, 2258–2262 (1983).
Young, S. P., Bomford, A. & Williams, R. The effect of the iron saturation of transferrin on its binding and uptake by rabbit reticulocytes. Biochem. J. 219, 505–510 (1984).
Acknowledgements
The authors are grateful for support from NIH 2R01NS064404 (S.H.P.), U54CA199090 (S.H.P.), R01AG063845 (S.H.P. and D.L.S.), 1R21HD100639 (E.N.), 5R35GM124677 (E.N.), R21NS099654 (D.L.S.), 1R01NS118247 (D.L.S.) and DOD SC130249 (S.H.P.).
Author information
Authors and Affiliations
Contributions
E.N., S.H.P., R.S. and D.L.S. contributed equally to the literature search, figure preparation, writing and editing of the article.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information
Nature Reviews Materials thanks Ravi Bellamkonda and the other, anonymous, reviewer(s) for their contribution to the peer review of this work
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nance, E., Pun, S.H., Saigal, R. et al. Drug delivery to the central nervous system. Nat Rev Mater 7, 314–331 (2022). https://doi.org/10.1038/s41578-021-00394-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41578-021-00394-w
This article is cited by
-
Multifaceted applications of micro/nanorobots in pharmaceutical drug delivery systems: a comprehensive review
Future Journal of Pharmaceutical Sciences (2024)
-
Intracerebral fate of engineered nanoparticles
Nature Nanotechnology (2024)
-
Nanoparticle delivery for central nervous system diseases and its clinical application
Nano Research (2024)
-
The protein corona from nanomedicine to environmental science
Nature Reviews Materials (2023)
-
Pathogenesis-adaptive polydopamine nanosystem for sequential therapy of ischemic stroke
Nature Communications (2023)