Abstract
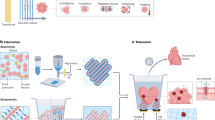
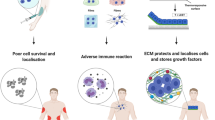
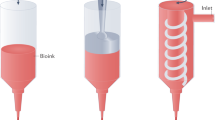
Organs are complex systems composed of different cells, proteins and signalling molecules that are arranged in a highly ordered structure to orchestrate a myriad of functions in our body. Biofabrication strategies can be applied to engineer 3D tissue models in vitro by mimicking the structure and function of native tissue through the precise deposition and assembly of materials and cells. This approach allows the spatiotemporal control over cell–cell and cell–extracellular matrix communication and thus the recreation of tissue-like structures. In this Review, we examine biofabrication strategies for the construction of functional tissue replacements and organ models, focusing on the development of biomaterials, such as supramolecular and photosensitive materials, that can be processed using biofabrication techniques. We highlight bioprinted and bioassembled tissue models and survey biofabrication techniques for their potential to recreate complex tissue properties, such as shape, vasculature and specific functionalities. Finally, we discuss challenges, such as scalability and the foreign body response, and opportunities in the field and provide an outlook to the future of biofabrication in regenerative medicine.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Change history
03 May 2018
This article was originally published with incorrect affiliations for Sang Jin Lee, Yuya Morimoto, Shoji Takeuchi and James J. Yoo. Please see below the correct affiliations.
References
Gomes, M. E., Rodrigues, M. T., Domingues, R. M. A. & Reis, R. L. Tissue engineering and regenerative medicine: new trends and directions-a year in review. Tissue Eng. Part B Rev. 23, 211–224 (2017).
Tschugg, A. et al. A prospective randomized multicenter phase I/II clinical trial to evaluate safety and efficacy of NOVOCART disk plus autologous disk chondrocyte transplantation in the treatment of nucleotomized and degenerative lumbar disks to avoid secondary disease: safety results of Phase I-a short report. Neurosurg. Rev. 40, 155–162 (2017).
Martin, I. et al. The survey on cellular and engineered tissue therapies in Europe in 2013. Tissue Eng. A 22, 5–16 (2016).
Groll, J. et al. Biofabrication: reappraising the definition of an evolving field. Biofabrication 8, 013001 (2016).
Lind, J. U. et al. Instrumented cardiac microphysiological devices via multimaterial three-dimensional printing. Nat. Mater. 16, 303–308 (2017).
Dai, X. et al. Coaxial 3D bioprinting of self-assembled multicellular heterogeneous tumor fibers. Sci. Rep. 7, 1457 (2017).
Faulkner-Jones, A. et al. Bioprinting of human pluripotent stem cells and their directed differentiation into hepatocyte-like cells for the generation of mini-livers in 3D. Biofabrication 7, 044102 (2015).
Homan, K. A. et al. Bioprinting of 3D convoluted renal proximal tubules on perfusable chips. Sci. Rep. 6, 34845 (2016).
Jeon, H. et al. Generation of multilayered 3D structures of HepG2 cells using a bio-printing technique. Gut Liver 11, 121–128 (2017).
Burdick, J. A. & Murphy, W. L. Moving from static to dynamic complexity in hydrogel design. Nat. Commun. 3, 1269 (2012).
Gobaa, S. et al. Artificial niche microarrays for probing single stem cell fate in high throughput. Nat. Methods 8, 949–955 (2011).
Lutolf, M. P. & Hubbell, J. A. Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat. Biotechnol. 23, 47 (2005).
Tibbitt, M. W. & Anseth, K. S. Hydrogels as extracellular matrix mimics for 3D cell culture. Biotechnol. Bioeng. 103, 655–663 (2009).
Khetan, S. & Burdick, J. A. Patterning hydrogels in three dimensions towards controlling cellular interactions. Soft Matter 7, 830–838 (2011).
Moroni, L. et al. Biofabrication: a guide to technology and terminology. Trends Biotechnol. 36, 384–402 (2018).
Jungst, T., Smolan, W., Schacht, K., Scheibel, T. & Groll, J. Strategies and molecular design criteria for 3D printable hydrogels. Chem. Rev. 116, 1496–1539 (2016).
Guvendiren, M., Molde, J., Soares, R. M. & Kohn, J. Designing biomaterials for 3D printing. ACS Biomater. Sci. Eng. 2, 1679–1693 (2016).
Ligon, S. C., Liska, R., Stampfl, J., Gurr, M. & Mulhaupt, R. Polymers for 3D printing and customized additive manufacturing. Chem. Rev. 117, 10212–10290 (2017).
Shi, W. et al. Structurally and functionally optimized silk-fibroin-gelatin scaffold using 3D printing to repair cartilage injury in vitro and in vivo. Adv. Mater. 29, 1701089 (2017).
Levato, R. et al. The bio in the ink: cartilage regeneration with bioprintable hydrogels and articular cartilage-derived progenitor cells. Acta Biomater. 61, 41–53 (2017).
Compaan, A. M., Christensen, K. & Huang, Y. Inkjet bioprinting of 3D silk fibroin cellular constructs using sacrificial alginate. ACS Biomater. Sci. Eng. (2016).
Colosi, C. et al. Microfluidic bioprinting of heterogeneous 3D tissue constructs using low-viscosity bioink. Adv. Mater. 28, 677–684 (2016).
Ouyang, L., Highley, C. B., Sun, W. & Burdick, J. A. A. Generalizable strategy for the 3D bioprinting of hydrogels from nonviscous photo-crosslinkable inks. Adv. Mater. 29, 1604983 (2017).
Liu, W. et al. Rapid continuous multimaterial extrusion bioprinting. Adv. Mater. 29, 1604630 (2017).
Schacht, K. et al. Biofabrication of cell-loaded 3D spider silk constructs. Angew. Chem. Int. Ed. 54, 2816–2820 (2015).
Ouyang, L. L., Highley, C. B., Rodell, C. B., Sun, W. & Burdick, J. A. 3D printing of shear-thinning hyaluronic acid hydrogels with secondary cross-linking. ACS Biomater. Sci. Eng. 2, 1743–1751 (2016).
Li, C. et al. Rapid formation of a supramolecular polypeptide–dna hydrogel for in situ three-dimensional multilayer bioprinting. Angew. Chem. Int. Ed. 54, 3957–3961 (2015).
Dubbin, K., Hori, Y., Lewis, K. K. & Heilshorn, S. C. Dual-stage crosslinking of a gel-phase bioink improves cell viability and homogeneity for 3D bioprinting. Adv. Healthc. Mater. 5, 2488–2492 (2016).
Loo, Y. & Hauser, C. A. E. Bioprinting synthetic self-assembling peptide hydrogels for biomedical applications. Biomed. Mater. 11, 014103 (2015).
Landers, R., Hübner, U., Schmelzeisen, R. & Mülhaupt, R. Rapid prototyping of scaffolds derived from thermoreversible hydrogels and tailored for applications in tissue engineering. Biomaterials 23, 4437–4447 (2002).
Wu, W., DeConinck, A. & Lewis, J. A. Omnidirectional printing of 3D microvascular networks. Adv. Mater. 23, H178–H183 (2011).
Hinton, T. J. et al. Three-dimensional printing of complex biological structures by freeform reversible embedding of suspended hydrogels. Sci. Adv. 1, e1500758 (2015).
Bhattacharjee, T. et al. Writing in the granular gel medium. Sci. Adv. 1, e1500655 (2015).
Highley, C. B., Rodell, C. B. & Burdick, J. A. Direct 3D printing of shear-thinning hydrogels into self-healing hydrogels. Adv. Mater. 27, 5075–5079 (2015).
Shi, L. et al. Dynamic coordination chemistry enables free directional printing of biopolymer hydrogel. Chem. Mater. 29, 5816–5823 (2017).
Miller, J. S. et al. Rapid casting of patterned vascular networks for perfusable engineered 3D tissues. Nat. Mater. 11, 768 (2012).
Kolesky, D. B., Homan, K. A., Skylar-Scott, M. A. & Lewis, J. A. Three-dimensional bioprinting of thick vascularized tissues. Proc. Natl Acad. Sci. USA 113, 3179–3184 (2016).
Bhattacharjee, T. et al. Liquid-like solids support cells in 3D. ACS Biomater. Sci. Eng. 2, 1787–1795 (2016).
Mironov, V. et al. Organ printing: tissue spheroids as building blocks. Biomaterials 30, 2164–2174 (2009).
Sego, T. J., Kasacheuski, U., Hauersperger, D., Tovar, A. & Moldovan, N. I. A heuristic computational model of basic cellular processes and oxygenation during spheroid-dependent biofabrication. Biofabrication 9, 024104 (2017).
Bakirci, E., Toprakhisar, B., Zeybek, M., Ozaydin, I. G. & Koc, B. Cell sheet based bionk for 3D bioprinting applications. Biofabrication 9, 024105 (2017).
Owaki, T., Shimizu, T., Yamato, M. & Okano, T. Cell sheet engineering for regenerative medicine: current challenges and strategies. Biotechnol. J. 9, 904–914 (2014).
Roh, S., Parekh, D. P., Bharti, B., Stoyanov, S. D. & Velev, O. D. 3D printing by multiphase silicone/water capillary inks. Adv. Mater. 29, 1701554 (2017).
Rutz, A. L., Hyland, K. E., Jakus, A. E., Burghardt, W. R. & Shah, R. N. A multimaterial bioink method for 3D printing tunable, cell-compatible hydrogels. Adv. Mater. 27, 1607–1614 (2015).
Rosales, A. M. & Anseth, K. S. The design of reversible hydrogels to capture extracellular matrix dynamics. Nat. Rev. Mater. 1, 15012 (2016).
Fairbanks, B. D. et al. A versatile synthetic extracellular matrix mimic via thiol-norbornene photopolymerization. Adv. Mater. 21, 5005–5010 (2009).
Stichler, S. et al. Thiol-ene clickable poly(glycidol) hydrogels for biofabrication. Ann. Biomed. Eng. 45, 273–285 (2017).
Stichler, S., Bertlein, S., Tessmar, J., Jungst, T. & Groll, J. Thiol-ene cross-linkable hydrogels as bioinks for biofabrication. Macromol. Symp. 372, 102–107 (2017).
Bertlein, S. et al. Thiol-ene clickable gelatin: a platform bioink for multiple 3D biofabrication technologies. Adv. Mater. 29, 1703404 (2017).
Yeh, Y.-C., Ouyang, L., Highley, C. B. & Burdick, J. A. Norbornene-modified poly (glycerol sebacate) as a photocurable and biodegradable elastomer. Polym. Chem. 8, 5091–5099 (2017).
Mondschein, R. J., Kanitkar, A., Williams, C. B., Verbridge, S. S. & Long, T. E. Polymer structure-property requirements for stereolithographic 3D printing of soft tissue engineering scaffolds. Biomaterials 140, 170–188 (2017).
Vitale, A. et al. Oxygen-inhibition lithography for the fabrication of multipolymeric structures. Adv. Mater. 27, 4560–4565 (2015).
Zhang, A. P. et al. Rapid fabrication of complex 3D extracellular microenvironments by dynamic optical projection stereolithography. Adv. Mater. 24, 4266–4270 (2012).
Zhu, W. et al. Direct 3D bioprinting of prevascularized tissue constructs with complex microarchitecture. Biomaterials 124, 106–115 (2017).
Brandenberg, N. & Lutolf, M. P. In situ patterning of microfluidic networks in 3D cell-laden hydrogels. Adv. Mater. 28, 7450–7456 (2016).
Arakawa, C. K., Badeau, B. A., Zheng, Y. & DeForest, C. A. Multicellular vascularized engineered tissues through user-programmable biomaterial photodegradation. Adv. Mater. 29, 1703156 (2017).
Mouser, V. H. et al. Development of a thermosensitive HAMA-containing bio-ink for the fabrication of composite cartilage repair constructs. Biofabrication 9, 015026 (2017).
Rhee, S., Puetzer, J. L., Mason, B. N., Reinhart-King, C. A. & Bonassar, L. J. 3D bioprinting of spatially heterogeneous collagen constructs for cartilage tissue engineering. ACS Biomater. Sci. Eng. 2, 1800–1805 (2016).
Diamantides, N. et al. Correlating rheological properties and printability of collagen bioinks: the effects of riboflavin photocrosslinking and pH. Biofabrication 9, 034102 (2017).
Bolaños, R. A. V. et al. The use of a cartilage decellularized matrix scaffold for the repair of osteochondral defects: the importance of long-term studies in a large animal model. Osteoarthritis Cartilage 25, 413–420 (2017).
Pati, F. et al. Printing three-dimensional tissue analogues with decellularized extracellular matrix bioink. Nat. Commun. 5, 3935 (2014).
Kim, B. S., Kim, H., Gao, G., Jang, J. & Cho, D. W. Decellularized extracellular matrix: a step towards the next generation source for bioink manufacturing. Biofabrication 9, 034104 (2017).
Levato, R. et al. The bio in the ink: cartilage regeneration with bioprintable hydrogels and articular cartilage-derived progenitor cells. Acta Biomaterialia (2017).
Shi, W. et al. Structurally and functionally optimized silk-fibroin–gelatin scaffold using 3D printing to repair cartilage injury in vitro and in vivo. Adv. Mater. 29, 1701089 (2017).
Klotz, B. J., Gawlitta, D., Rosenberg, A. J. W. P., Malda, J. & Melchels, F. P. W. Gelatin-methacryloyl hydrogels: towards biofabrication-based tissue repair. Trends Biotechnol. 34, 394–407 (2016).
Khalil, S. & Sun, W. Bioprinting endothelial cells with alginate for 3D tissue constructs. J. Biomech. Eng. 131, 111002 (2009).
Duan, B., Hockaday, L. A., Kang, K. H. & Butcher, J. T. 3D bioprinting of heterogeneous aortic valve conduits with alginate/gelatin hydrogels. J. Biomed. Mater. Res. A 101, 1255–1264 (2013).
Jose, R. R., Brown, J. E., Polido, K. E., Omenetto, F. G. & Kaplan, D. L. Polyol-silk bioink formulations as two-part room-temperature curable materials for 3D printing. ACS Biomater. Sci. Eng. 1, 780–788 (2015).
Sommer, M. R., Schaffner, M., Carnelli, D. & Studart, A. R. 3D printing of hierarchical silk fibroin structures. ACS Appl. Mater. Inter 8, 34677–34685 (2016).
Badylak, S. F., Taylor, D. & Uygun, K. Whole-organ tissue engineering: decellularization and recellularization of three-dimensional matrix scaffolds. Annu. Rev. Biomed. Eng. 13, 27–53 (2011).
Cheng, J. et al. Rheological properties of cell-hydrogel composites extruding through small-diameter tips. J. Manuf. Sci. Eng. 130, 021014 (2008).
Xu, C. X. et al. Study of droplet formation process during drop-on-demand inkjetting of living cell-laden bioink. Langmuir 30, 9130–9138 (2014).
Zhang, Z. Y., Xu, C. X., Xiong, R. T., Chrisey, D. B. & Huang, Y. Effects of living cells on the bioink printability during laser printing. Biomicrofluidics 11, (2017).
Nussinovitch, A. Resemblance of immobilized trichoderma-viride fungal spores in an alginate matrix to a composite-material. Biotechnol. Progr. 10, 551–554 (1994).
Zhang, X. Z. & Chu, C. C. Fabrication and characterization of microgel-impregnated, thermosensitive PNIPAAm hydrogels. Polymer 46, 9664–9673 (2005).
Lim, C. T., Zhou, E. H. & Quek, S. T. Mechanical models for living cells — a review. J. Biomech. 39, 195–216 (2006).
Mekhileri, N. V. et al. Automated 3D bioassembly of micro-tissues for biofabrication of hybrid tissue engineered constructs. Biofabrication 10, (2018).
Yeo, M., Lee, J. S., Chun, W. & Kim, G. H. An innovative collagen-based cell-printing method for obtaining human adipose stem cell-laden structures consisting of core sheath structures for tissue engineering. Biomacromolecules 17, 1365–1375 (2016).
Levato, R. et al. Biofabrication of tissue constructs by 3D bioprinting of cell-laden microcarriers. Biofabrication 6, (2014).
Kamperman, T. et al. Single cell microgel based modular bioinks for uncoupled cellular micro- and macroenvironments. Adv. Healthc. Mater. 6, (2017).
Bhatia, S. N. & Ingber, D. E. Microfluidic organs-on-chips. Nat. Biotechnol. 32, 760–772 (2014).
Cohen, D. L., Malone, E., Lipson, H. & Bonassar, L. J. Direct freeform fabrication of seeded hydrogels in arbitrary geometries. Tissue Eng. 12, 1325–1335 (2006).
Pati, F., Gantelius, J. & Svahn, H. A. 3D bioprinting of tissue/organ models. Angew. Chem. Int. Ed. 55, 4650–4665 (2016).
Min, D. et al. Bioprinting of biomimetic skin containing melanocytes. Exp. Dermatol. https://doi.org/10.1111/exd.13376 (2017).
Lee, V. et al. Design and fabrication of human skin by three-dimensional bioprinting. Tissue Eng. C 20, 473–484 (2014).
Lee, W. et al. Multi-layered culture of human skin fibroblasts and keratinocytes through three-dimensional freeform fabrication. Biomaterials 30, 1587–1595 (2009).
Mandrycky, C., Wang, Z., Kim, K. & Kim, D. H. 3D bioprinting for engineering complex tissues. Biotechnol. Adv. 34, 422–434 (2016).
Ozbolat, I. T., Peng, W. & Ozbolat, V. Application areas of 3D bioprinting. Drug Discov. Today 21, 1257–1271 (2016).
Arslan-Yildiz, A. et al. Towards artificial tissue models: past, present, and future of 3D bioprinting. Biofabrication 8, 014103 (2016).
Vyas, D. et al. Self-assembled liver organoids recapitulate hepatobiliary organogenesis in vitro. Hepatology 67, 750–761 (2017).
Bhise, N. S. et al. A liver-on-a-chip platform with bioprinted hepatic spheroids. Biofabrication 8, 014101 (2016).
Knowlton, S. & Tasoglu, S. A. Bioprinted liver-on-a-chip for drug screening applications. Trends Biotechnol. 34, 681–682 (2016).
Konar, D., Devarasetty, M., Yildiz, D. V., Atala, A. & Murphy, S. V. Lung-on-a-chip technologies for disease modeling and drug development. Biomed. Eng. Comput. Biol. 7, 17–27 (2016).
Doryab, A., Amoabediny, G. & Salehi-Najafabadi, A. Advances in pulmonary therapy and drug development: lung tissue engineering to lung-on-a-chip. Biotechnol. Adv. 34, 588–596 (2016).
Horvath, L. et al. Engineering an in vitro air-blood barrier by 3D bioprinting. Sci. Rep. 5, 7974 (2015).
Huh, D. et al. Reconstituting organ-level lung functions on a chip. Science 328, 1662–1668 (2010).
Wang, Z., Lee, S. J., Cheng, H. J., Yoo, J. J. & Atala, A. 3D bioprinted functional and contractile cardiac tissue constructs. Acta Biomater. https://doi.org/10.1016/j.actbio.2018.02.007 (2018).
Zhang, Y. S. et al. Bioprinting 3D microfibrous scaffolds for engineering endothelialized myocardium and heart-on-a-chip. Biomaterials 110, 45–59 (2016).
King, S. M. et al. 3D proximal tubule tissues recapitulate key aspects of renal physiology to enable nephrotoxicity testing. Front. Physiol. 8, 123 (2017).
Abaci, H. E. & Shuler, M. L. Human-on-a-chip design strategies and principles for physiologically based pharmacokinetics/pharmacodynamics modeling. Integr. Biol. 7, 383–391 (2015).
Skardal, A. et al. Multi-tissue interactions in an integrated three-tissue organ-on-a-chip platform. Sci. Rep. 7, 8837 (2017).
Weiswald, L. B., Bellet, D. & Dangles-Marie, V. Spherical cancer models in tumor biology. Neoplasia 17, 1–15 (2015).
Skardal, A., Devarasetty, M., Rodman, C., Atala, A. & Soker, S. Liver-tumor hybrid organoids for modeling tumor growth and drug response in vitro. Ann. Biomed. Eng. 43, 2361–2373 (2015).
Friedrich, J., Ebner, R. & Kunz-Schughart, L. A. Experimental anti-tumor therapy in 3D: spheroids — old hat or new challenge? Int. J. Radiat. Biol. 83, 849–871 (2007).
Xu, F. et al. A three-dimensional in vitro ovarian cancer coculture model using a high-throughput cell patterning platform. Biotechnol. J. 6, 204–212 (2011).
King, S. M., Presnell, S. C. & Nguyen, D. G. Development of 3D bioprinted human breast cancer for in vitro drug screening. Cancer Res. 74 (Suppl), 2034 (2014).
Morimoto, Y., Hsiao, A. Y. & Takeuchi, S. Point-, line-, and plane-shaped cellular constructs for 3D tissue assembly. Adv. Drug Deliv. Rev. 95, 29–39 (2015).
Morimoto, Y., Onuki, M. & Takeuchi, S. Mass production of cell-laden calcium alginate particles with centrifugal force. Adv. Healthc. Mater. 6, 1601375 (2017).
Tan, W. H. & Takeuchi, S. Monodisperse alginate hydrogel microbeads for cell encapsulation. Adv. Mater. 19, 2696–2701 (2007).
Headen, D. M., Aubry, G., Lu, H. & Garcia, A. J. Microfluidic-based generation of size-controlled, biofunctionalized synthetic polymer microgels for cell encapsulation. Adv. Mater. 26, 3003–3008 (2014).
Griffin, D. R., Weaver, W. M., Scumpia, P. O., Di Carlo, D. & Segura, T. Accelerated wound healing by injectable microporous gel scaffolds assembled from annealed building blocks. Nat. Mater. 14, 737–744 (2015).
Matsunaga, Y. T., Morimoto, Y. & Takeuchi, S. Molding cell beads for rapid construction of macroscopic 3D tissue architecture. Adv. Mater. 23, H90–H94 (2011).
Hong, S. M., Hsu, H. J., Kaunas, R. & Kameoka, J. Collagen microsphere production on a chip. Lab. Chip 12, 3277–3280 (2012).
Kato-Negishi, M., Morimoto, Y., Onoe, H. & Takeuchi, S. Millimeter-sized neural building blocks for 3D heterogeneous neural network assembly. Adv. Healthc. Mater. 2, 1564–1570 (2013).
Luo, H. Y. et al. Fabrication of viable centimeter-sized 3D tissue constructs with microchannel conduits for improved tissue properties through assembly of cell-laden microbeads. J. Tissue Eng. Regen. Med. 8, 493–504 (2014).
Dutta, D., Heo, I. & Clevers, H. Disease modeling in stem cell-derived 3D organoid systems. Trends Mol. Med. 23, 393–410 (2017).
Chung, S. E., Park, W., Shin, S., Lee, S. A. & Kwon, S. Guided and fluidic self-assembly of microstructures using railed microfluidic channels. Nat. Mater. 7, 581–587 (2008).
Yang, W., Yu, H., Li, G., Wang, Y. & Liu, L. High-throughput fabrication and modular assembly of 3D heterogeneous microscale tissues. Small 13, 1602769 (2017).
Kang, E. et al. Digitally tunable physicochemical coding of material composition and topography in continuous microfibres. Nat. Mater. 10, 877–883 (2011).
Wei, D. et al. Continuous fabrication and assembly of spatial cell-laden fibers for a tissue-like construct via a photolithographic-based microfluidic chip. ACS Appl. Mater. Inter 9, 14606–14617 (2017).
Onoe, H. et al. Metre-long cell-laden microfibres exhibit tissue morphologies and functions. Nat. Mater. 12, 584–590 (2013).
Jun, Y. et al. Microfluidics-generated pancreatic islet microfibers for enhanced immunoprotection. Biomaterials 34, 8122–8130 (2013).
Sakai, S., Yamaguchi, S., Takei, T. & Kawakami, K. Oxidized alginate-cross-linked alginate/gelatin hydrogel fibers for fabricating tubular constructs with layered smooth muscle cells and endothelial cells in collagen gels. Biomacromolecules 9, 2036–2041 (2008).
Lee, K. H., Shin, S. J., Park, Y. & Lee, S. H. Synthesis of cell-laden alginate hollow fibers using microfluidic chips and microvascularized tissue-engineering applications. Small 5, 1264–1268 (2009).
Yang, J. et al. Cell sheet engineering: recreating tissues without biodegradable scaffolds. Biomaterials 26, 6415–6422 (2005).
Leng, L., McAllister, A., Zhang, B. Y., Radisic, M. & Gunther, A. Mosaic hydrogels: one-step formation of multiscale soft materials. Adv. Mater. 24, 3650–3658 (2012).
Yan, J., Chen, F. & Amsden, B. G. Cell sheets prepared via gel-sol transition of calcium RGD-alginate. Acta Biomaterialia 30, 277–284 (2016).
Kim, K., Utoh, R., Ohashi, K., Kikuchi, T. & Okano, T. Fabrication of functional 3D hepatic tissues with polarized hepatocytes by stacking endothelial cell sheets in vitro. J. Tissue Eng. Regen. Med. 11, 2071–2080 (2017).
Cheng, S. et al. Self-adjusting, polymeric multilayered roll that can keep the shapes of the blood vessel scaffolds during biodegradation. Adv. Mater. 29, 1700171 (2017).
Ito, A. et al. Novel methodology for fabrication of tissue-engineered tubular constructs using magnetite nanoparticles and magnetic force. Tissue Eng. 11, 1553–1561 (2005).
Hsu, A. R. & Ellington, J. K. Patient-specific 3-dimensional printed titanium truss cage with tibiotalocalcaneal arthrodesis for salvage of persistent distal tibia nonunion. Foot Ankle Spec. 8, 483–489 (2015).
Jeong, C. G. & Atala, A. 3D printing and biofabrication for load bearing tissue engineering. Adv. Exp. Med. Biol. 881, 3–14 (2015).
Bose, S., Vahabzadeh, S. & Bandyopadhyay, A. Bone tissue engineering using 3D printing. Mater. Today 16, 496–504 (2013).
McBeth, C. et al. 3D bioprinting of GelMA scaffolds triggers mineral deposition by primary human osteoblasts. Biofabrication 9, 015009 (2017).
Yao, Q. et al. Design, construction and mechanical testing of digital 3D anatomical data-based PCL-HA bone tissue engineering scaffold. J. Mater. Sci. Mater. Med. 26, 5360 (2015).
Wang, M. O., Piard, C. M., Melchiorri, A., Dreher, M. L. & Fisher, J. P. Evaluating changes in structure and cytotoxicity during in vitro degradation of three-dimensional printed scaffolds. Tissue Eng. A 21, 1642–1653 (2015).
Pati, F. et al. Ornamenting 3D printed scaffolds with cell-laid extracellular matrix for bone tissue regeneration. Biomaterials 37, 230–241 (2015).
Kang, H. W. et al. A 3D bioprinting system to produce human-scale tissue constructs with structural integrity. Nat. Biotechnol. 34, 312–319 (2016).
Ballyns, J. J. et al. Image-guided tissue engineering of anatomically shaped implants via MRI and micro-CT using injection molding. Tissue Eng. A 14, 1195–1202 (2008).
Hockaday, L. A. et al. Rapid 3D printing of anatomically accurate and mechanically heterogeneous aortic valve hydrogel scaffolds. Biofabrication 4, 035005 (2012).
Bowles, R. D., Gebhard, H. H., Hartl, R. & Bonassar, L. J. Tissue-engineered intervertebral discs produce new matrix, maintain disc height, and restore biomechanical function to the rodent spine. Proc. Natl Acad. Sci. USA 108, 13106–13111 (2011).
Makris, E. A., Gomoll, A. H., Malizos, K. N., Hu, J. C. & Athanasiou, K. A. Repair and tissue engineering techniques for articular cartilage. Nat. Rev. Rheumatol. 11, 21–34 (2015).
Tatman, P. D. et al. Multiscale biofabrication of articular cartilage: bioinspired and biomimetic approaches. Tissue Eng. B 21, 543–559 (2015).
Di Bella, C., Fosang, A., Donati, D. M., Wallace, G. G. & Choong, P. F. 3D bioprinting of cartilage for orthopedic surgeons: reading between the lines. Front. Surg. 2, 39 (2015).
Gruene, M. et al. Laser printing of stem cells for biofabrication of scaffold-free autologous grafts. Tissue Eng. C 17, 79–87 (2011).
Cui, X., Breitenkamp, K., Finn, M. G., Lotz, M. & D’Lima, D. D. Direct human cartilage repair using three-dimensional bioprinting technology. Tissue Eng. A 18, 1304–1312 (2012).
Cui, X., Breitenkamp, K., Lotz, M. & D’Lima, D. Synergistic action of fibroblast growth factor-2 and transforming growth factor-beta1 enhances bioprinted human neocartilage formation. Biotechnol. Bioeng. 109, 2357–2368 (2012).
Xu, T. et al. Hybrid printing of mechanically and biologically improved constructs for cartilage tissue engineering applications. Biofabrication 5, 015001 (2013).
Mannoor, M. S. et al. 3D printed bionic ears. Nano Lett. 13, 2634–2639 (2013).
Almqvist, K. F. et al. Treatment of cartilage defects in the knee using alginate beads containing human mature allogenic chondrocytes. Am. J. Sport Med. 37, 1920–1929 (2009).
Dhollander, A. A. M. et al. Midterm results of the treatment of cartilage defects in the knee using alginate beads containing human mature allogenic chondrocytes. Am. J. Sport Med. 40, 75–82 (2012).
Skardal, A. et al. Bioprinted amniotic fluid-derived stem cells accelerate healing of large skin wounds. Stem Cells Transl Med. 1, 792–802 (2012).
Yang, J. et al. Cell delivery in regenerative medicine: the cell sheet engineering approach. J. Control. Release 116, 193–203 (2006).
Iwata, T. et al. Cell sheet engineering and its application for periodontal regeneration. J. Tissue Eng. Regen. Med. 9, 343–356 (2015).
Frontera, W. R. & Ochala, J. Skeletal muscle: a brief review of structure and function. Calcified Tissue Int. 96, 183–195 (2015).
Ostrovidov, S. et al. Skeletal muscle tissue engineering: methods to form skeletal myotubes and their applications. Tissue Eng. Part B Rev. 20, 403–436 (2014).
Gaebel, R. et al. Patterning human stem cells and endothelial cells with laser printing for cardiac regeneration. Biomaterials 32, 9218–9230 (2011).
Xu, T., Baicu, C., Aho, M., Zile, M. & Boland, T. Fabrication and characterization of bio-engineered cardiac pseudo tissues. Biofabrication 1, 035001 (2009).
Gaetani, R. et al. Cardiac tissue engineering using tissue printing technology and human cardiac progenitor cells. Biomaterials 33, 1782–1790 (2012).
Gao, L. et al. Myocardial tissue engineering with cells derived from human-induced pluripotent stem cells and a native-like, high-resolution, 3-dimensionally printed scaffold. Circ. Res. 120, 1318–1325 (2017).
Atala, A., Kasper, F. K. & Mikos, A. G. Engineering complex tissues. Sci. Transl Med. 4, 160rv12 (2012).
Lee, C. H. et al. Regeneration of the articular surface of the rabbit synovial joint by cell homing: a proof of concept study. Lancet 376, 440–448 (2010).
Merceron, T. K. et al. A 3D bioprinted complex structure for engineering the muscle-tendon unit. Biofabrication 7, 035003 (2015).
Novosel, E. C., Kleinhans, C. & Kluger, P. J. Vascularization is the key challenge in tissue engineering. Adv. Drug Deliv. Rev. 63, 300–311 (2011).
Jain, R. K., Au, P., Tam, J., Duda, D. G. & Fukumura, D. Engineering vascularized tissue. Nat. Biotechnol. 23, 821–823 (2005).
Gross, B. C., Erkal, J. L., Lockwood, S. Y., Chen, C. & Spence, D. M. Evaluation of 3D printing and its potential impact on biotechnology and the chemical sciences. Anal. Chem. 86, 3240–3253 (2014).
Ozbolat, I. T. & Yu, Y. Bioprinting toward organ fabrication: challenges and future trends. IEEE Trans. Biomed. Eng. 60, 691–699 (2013).
Zheng, Y. et al. Microstructured templates for directed growth and vascularization of soft tissue in vivo. Biomaterials 32, 5391–5401 (2011).
Choi, N. W. et al. Microfluidic scaffolds for tissue engineering. Nat. Mater. 6, 908–915 (2007).
Kolesky, D. B. et al. 3D bioprinting of vascularized, heterogeneous cell-laden tissue constructs. Adv. Mater. 26, 3124–3130 (2014).
Attalla, R., Ling, C. & Selvaganapathy, P. Fabrication and characterization of gels with integrated channels using 3D printing with microfluidic nozzle for tissue engineering applications. Biomed. Microdevices 18, 17 (2016).
L’Heureux, N. et al. Human tissue-engineered blood vessels for adult arterial revascularization. Nat. Med. 12, 361–365 (2006).
Schubert, C., van Langeveld, M. C. & Donoso, L. A. Innovations in 3D printing: a 3D overview from optics to organs. Br. J. Ophthalmol. 98, 159–161 (2014).
Kato-Negishi, M., Onoe, H., Ito, A. & Takeuchi, S. Rod-shaped neural units for aligned 3D neural network connection. Adv. Healthc. Mater. 6, 1700143 (2017).
de Vos, P., Faas, M. M., Strand, B. & Calafiore, R. Alginate-based microcapsules for immunoisolation of pancreatic islets. Biomaterials 27, 5603–5617 (2006).
Vegas, A. J. et al. Combinatorial hydrogel library enables identification of materials that mitigate the foreign body response in primates. Nat. Biotechnol. 34, 345–352 (2016).
Rengifo, H. R., Giraldo, J. A., Labrada, I. & Stabler, C. L. Long-term survival of allograft murine islets coated via covalently stabilized polymers. Adv. Healthc. Mater. 3, 1061–1070 (2014).
Veiseh, O. et al. Size- and shape-dependent foreign body immune response to materials implanted in rodents and non-human primates. Nat. Mater. 14, 643–651 (2015).
Vegas, A. J. et al. Long-term glycemic control using polymer-encapsulated human stem cell-derived beta cells in immune-competent mice. Nat. Med. 22, 306–311 (2016).
Dufrane, D., Goebbels, R. M., Saliez, A., Guiot, Y. & Gianello, P. Six-month survival of microencapsulated pig islets and alginate biocompatibility in primates: proof of concept. Transplantation 81, 1345–1353 (2006).
Elliott, R. B. et al. Live encapsulated porcine islets from a type 1 diabetic patient 9.5 yr after xenotransplantation. Xenotransplantation 14, 157–161 (2007).
Capone, S. H. et al. Impact of alginate composition: from bead mechanical properties to encapsulated HepG2/C3A cell activities for in vivo implantation. PLOS ONE 8, e62032 (2013).
Song, W. et al. Engraftment of human induced pluripotent stem cell-derived hepatocytes in immunocompetent mice via 3D co-aggregation and encapsulation. Sci. Rep. 5, 16884 (2015).
Qi, M. et al. PVA hydrogel sheet macroencapsulation for the bioartificial pancreas. Biomaterials 25, 5885–5892 (2004).
Veriter, S. et al. The impact of hyperglycemia and the presence of encapsulated islets on oxygenation within a bioartificial pancreas in the presence of mesenchymal stem cells in a diabetic Wistar rat model. Biomaterials 32, 5945–5956 (2011).
Fozdar, D. Y., Soman, P., Lee, J. W., Han, L. H. & Chen, S. Three-dimensional polymer constructs exhibiting a tunable negative poisson’s ratio. Adv. Funct. Mater. 21, 2712–2720 (2011).
Lee, H. & Cho, D. W. One-step fabrication of an organ-on-a-chip with spatial heterogeneity using a 3D bioprinting technology. Lab. Chip 16, 2618–2625 (2016).
Clausen, A., Wang, F., Jensen, J. S., Sigmund, O. & Lewis, J. A. Topology optimized architectures with programmable Poisson’s ratio over large deformations. Adv. Mater. 27, 5523–5527 (2015).
Shan, S. et al. Multistable architected materials for trapping elastic strain energy. Adv. Mater. 27, 4296–4301 (2015).
Martin, J. J., Fiore, B. E. & Erb, R. M. Designing bioinspired composite reinforcement architectures via 3D magnetic printing. Nat. Commun. 6, 8641 (2015).
Han, X., Bibb, R. & Harris, R. Engineering design of artificial vascular junctions for 3D printing. Biofabrication 8, 025018 (2016).
Sun, Y., Yang, X. & Wang, Q. In-silico analysis on biofabricating vascular networks using kinetic Monte Carlo simulations. Biofabrication 6, 015008 (2014).
Yang, X., Mironov, V. & Wang, Q. Modeling fusion of cellular aggregates in biofabrication using phase field theories. J. Theor. Biol. 303, 110–118 (2012).
McCune, M., Shafiee, A., Forgacs, G. & Kosztin, I. Predictive modeling of post bioprinting structure formation. Soft Matter 10, 1790–1800 (2014).
Zhu, W. et al. 3D printing of functional biomaterials for tissue engineering. Curr. Opin. Biotechnol. 40, 103–112 (2016).
Tumbleston, J. R. et al. Additive manufacturing. Continuous liquid interface production of 3D objects. Science 347, 1349–1352 (2015).
Janusziewicz, R., Tumbleston, J. R., Quintanilla, A. L., Mecham, S. J. & DeSimone, J. M. Layerless fabrication with continuous liquid interface production. Proc. Natl Acad. Sci. USA 113, 11703–11708 (2016).
Shanjani, Y., Pan, C. C., Elomaa, L. & Yang, Y. A novel bioprinting method and system for forming hybrid tissue engineering constructs. Biofabrication 7, 045008 (2015).
Hoffmann, A. et al. New stereolithographic resin providing functional surfaces for biocompatible three-dimensional printing. J. Tissue Eng. 8, 2041731417744485 (2017).
Morris, V. B., Nimbalkar, S., Younesi, M., McClellan, P. & Akkus, O. Mechanical properties, cytocompatibility and manufacturability of chitosan:PEGDA hybrid-gel scaffolds by stereolithography. Ann. Biomed. Eng. 45, 286–296 (2017).
Serpooshan, V. et al. Bioacoustic-enabled patterning of human iPSC-derived cardiomyocytes into 3D cardiac tissue. Biomaterials 131, 47–57 (2017).
Bouyer, C. et al. A bio-acoustic levitational (BAL) assembly method for engineering of multilayered, 3D brain-like constructs, using human embryonic stem cell derived neuro-progenitors. Adv. Mater. 28, 161–167 (2016).
Durmus, N. G. et al. Magnetic levitation of single cells. Proc. Natl Acad. Sci. USA 112, E3661–E3668 (2015).
Li, Y. et al. Rapid assembly of heterogeneous 3D cell microenvironments in a microgel array. Adv. Mater. 28, 3543–3548 (2016).
O’Bryan, C. S. et al. Self-assembled micro-organogels for 3D printing silicone structures. Sci. Adv. 3, e1602800 (2017).
Vrij, E. et al. Directed Assembly and Development of Material-Free Tissues with Complex Architectures. Adv. Mater. 28, 4032–4039 (2016).
Fernandez, J. G. & Khademhosseini, A. Micro-masonry: construction of 3D structures by microscale self-assembly. Adv. Mater. 22, 2538–2541 (2010).
Qi, H. et al. DNA-directed self-assembly of shape-controlled hydrogels. Nature Commun. 4, 2275 (2013).
Todhunter, M. E. et al. Programmed synthesis of three-dimensional tissues. Nat. Methods 12, 975–981 (2015).
Tasoglu, S., Diller, E., Guven, S., Sitti, M. & Demirci, U. Untethered micro-robotic coding of three-dimensional material composition. Nat. Commun. 5, 3124 (2014).
Dondossola, E. et al. Examination of the foreign body response to biomaterials by nonlinear intravital microscopy. Nat. Biomed. Eng. 1, 0007 (2016).
Doloff, J. C. et al. Colony stimulating factor-1 receptor is a central component of the foreign body response to biomaterial implants in rodents and non-human primates. Nat. Mater. 16, 671–680 (2017).
Gullo, M. R., Takeuchi, S. & Paul, O. Multicellular biohybrid materials: probing the interplay of cells of different types precisely positioned and constrained on 3D wireframe-like microstructures. Adv. Healthc. Mater. 6, 1601053 (2017).
Nava, M. M., Zandrini, T., Cerullo, G., Osellame, R. & Raimondi, M. T. 3D stem cell niche engineering via two-photon laser polymerization. Methods Mol. Biol. 1612, 253–266 (2017).
Richter, B. et al. Guiding cell attachment in 3D microscaffolds selectively functionalized with two distinct adhesion proteins. Adv. Mater. 29, 1604342 (2017).
Villar, G., Graham, A. D. & Bayley, H. A tissue-like printed material. Science 340, 48–52 (2013).
Chiang, M. Y., Hsu, Y. W., Hsieh, H. Y., Chen, S. Y. & Fan, S. K. Constructing 3D heterogeneous hydrogels from electrically manipulated prepolymer droplets and crosslinked microgels. Sci. Adv. 2, e1600964 (2016).
Inostroza-Brito, K. E. et al. Cross-linking of a biopolymer-peptide co-assembling system. Acta Biomaterialia 50, 80–89 (2017).
Hardin, J. O., Ober, T. J., Valentine, A. D. & Lewis, J. A. Microfluidic printheads for multimaterial 3D printing of viscoelastic inks. Adv. Mater. 27, 3279–3284 (2015).
Snyder, J., Son, A. R., Hamid, Q., Wu, H. & Sun, W. Hetero-cellular prototyping by synchronized multi-material bioprinting for rotary cell culture system. Biofabrication 8, 015002 (2016).
Duchi, S. et al. Handheld co-axial bioprinting: application to in situ surgical cartilage repair. Sci. Rep. 7, 5837 (2017).
Mogas-Soldevila, L., Duro-Royo, J. & Oxman, N. Water-based robotic fabrication: large-scale additive manufacturing of functionally graded hydrogel composites via multichamber extrusion. 3D Print. Addit. Manuf. 1, 141–151 (2014).
Schuurman, W. et al. Bioprinting of hybrid tissue constructs with tailorable mechanical properties. Biofabrication 3, 021001 (2011).
Graham, A. D. et al. High-resolution patterned cellular constructs by droplet-based 3D printing. Sci. Rep. 7, 7004 (2017).
Gu, Q., Tomaskovic-Crook, E., Wallace, G. G. & Crook, J. M. 3D bioprinting human induced pluripotent stem cell constructs for in situ cell proliferation and successive multilineage differentiation. Adv. Healthc. Mater. 6, 1700175 (2017).
Zujur, D. et al. Three-dimensional system enabling the maintenance and directed differentiation of pluripotent stem cells under defined conditions. Sci. Adv. 3, e1602875 (2017).
Whulanza, Y., Ucciferri, N., Domenici, C., Vozzi, G. & Ahluwalia, A. Sensing scaffolds to monitor cellular activity using impedance measurements. Biosens. Bioelectron. 26, 3303–3308 (2011).
Orsi, G. et al. Combining inkjet printing and sol-gel chemistry for making pH-sensitive surfaces. Curr. Top. Med. Chem. 15, 271–278 (2015).
Muskovich, M. & Bettinger, C. J. Biomaterials-based electronics: polymers and interfaces for biology and medicine. Adv. Healthc. Mater. 1, 248–266 (2012).
Minev, I. R. et al. Biomaterials. Electronic dura mater for long-term multimodal neural interfaces. Science 347, 159–163 (2015).
Tatara, A. M. et al. Reconstruction of large mandibular defects using autologous tissues generated from in vivo bioreactors. Acta Biomater. 45, 72–84 (2016).
Emans, P. J. et al. Autologous engineering of cartilage. Proc. Natl Acad. Sci. USA 107, 3418–3423 (2010).
Kluin, J. et al. In situ heart valve tissue engineering using a bioresorbable elastomeric implant — from material design to 12 months follow-up in sheep. Biomaterials 125, 101–117 (2017).
Rothuizen, T. C. et al. Development and evaluation of in vivo tissue engineered blood vessels in a porcine model. Biomaterials 75, 82–90 (2016).
Di Bella, C. et al. In-situ handheld 3D Bioprinting for cartilage regeneration. J. Tissue Eng. Regen. Med. 12, 611–621 (2017).
Gladman, A. S., Matsumoto, E. A., Nuzzo, R. G., Mahadevan, L. & Lewis, J. A. Biomimetic 4D printing. Nat. Mater. 15, 413–418 (2016).
Hendrikson, W. J. et al. Towards 4D printed scaffolds for tissue engineering: exploiting 3D shape memory polymers to deliver time-controlled stimulus on cultured cells. Biofabrication 9, 031001 (2017).
Peltola, S. M. et al. A review of rapid prototyping techniques for tissue engineering purposes. Ann. Med. 40, 268–280 (2008).
Malda, J. et al. 25th anniversary article: Engineering hydrogels for biofabrication. Adv. Mater. 25, 5011–5028 (2013).
Acknowledgements
L.M. acknowledges the Dutch Province of Limburg and the European Research Council (grant #637308) for funding. J.A.B. thanks the AO foundation for funding. S.J.L. and J.J.Y. were supported by the US National Institutes of Health (1P41EB023833-01). S.T. and Y.M. thank A. Shima, S. Nagata and F. Ozawa for valuable discussion.
Author information
Authors and Affiliations
Contributions
All authors contributed equally to the preparation of this manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
Taylor & Francis Ltd: http://www.tandfonline.com
Rights and permissions
About this article
Cite this article
Moroni, L., Burdick, J.A., Highley, C. et al. Biofabrication strategies for 3D in vitro models and regenerative medicine. Nat Rev Mater 3, 21–37 (2018). https://doi.org/10.1038/s41578-018-0006-y
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41578-018-0006-y
This article is cited by
-
Nano-biomaterials and advanced fabrication techniques for engineering skeletal muscle tissue constructs in regenerative medicine
Nano Convergence (2023)
-
Nature-inspired micropatterns
Nature Reviews Methods Primers (2023)
-
Biomaterial-based platforms for tumour tissue engineering
Nature Reviews Materials (2023)
-
Volumetric additive manufacturing of pristine silk-based (bio)inks
Nature Communications (2023)
-
Light-based vat-polymerization bioprinting
Nature Reviews Methods Primers (2023)