Abstract
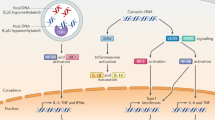
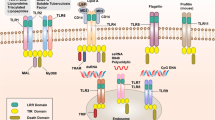
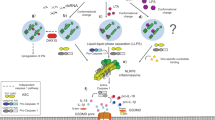
The innate immune system has the capacity to detect ‘non-self’ molecules derived from pathogens, known as pathogen-associated molecular patterns, via pattern recognition receptors. In addition, an increasing number of endogenous host-derived molecules, termed damage-associated molecular patterns (DAMPs), have been found to be sensed by various innate immune receptors. The recognition of DAMPs, which are produced or released by damaged and dying cells, promotes sterile inflammation, which is important for tissue repair and regeneration, but can also lead to the development of numerous inflammatory diseases, such as metabolic disorders, neurodegenerative diseases, autoimmune diseases and cancer. Here we examine recent discoveries concerning the roles of DAMP-sensing receptors in sterile inflammation and in diseases resulting from dysregulated sterile inflammation, and then discuss insights into the cross-regulation of these receptors and their ligands.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Burnet, F. M. S. The Clonal Selection Theory of Acquired Immunity (Vanderbilt University Press, 1959).
Janeway, C. A. Jr. Approaching the asymptote? Evolution and revolution in immunology. Cold Spring Harb. Symp. Quant. Biol. 54(Pt 1), 1–13 (1989).
Poltorak, A. et al. Defective LPS signaling in C3H/HeJ and C57BL/10ScCr mice: mutations in Tlr4 gene. Science 282, 2085–2088 (1998).
Matzinger, P. Tolerance, danger, and the extended family. Annu. Rev. Immunol. 12, 991–1045 (1994).
Land, W. Allograft injury mediated by reactive oxygen species: from conserved proteins of Drosophila to acute and chronic rejection of human transplants. Part III: interaction of (oxidative) stress-induced heat shock proteins with Toll-like receptor-bearing cells of innate immunity and its consequences for the development of acute and chronic allograft rejection. Transplant. Rev. 17, 67–86 (2003).
Cao, X. Self-regulation and cross-regulation of pattern-recognition receptor signalling in health and disease. Nat. Rev. Immunol. 16, 35–50 (2016).
Hudson, B. I. & Lippman, M. E. Targeting RAGE signaling in inflammatory disease. Annu. Rev. Med. 69, 349–364 (2018).
Ford, J. W. & McVicar, D. W. TREM and TREM-like receptors in inflammation and disease. Curr. Opin. Immunol. 21, 38–46 (2009).
Heng, B. C., Aubel, D. & Fussenegger, M. G protein-coupled receptors revisited: therapeutic applications inspired by synthetic biology. Annu. Rev. Pharmacol. Toxicol. 54, 227–249 (2014).
Weiss, E. & Kretschmer, D. Formyl-peptide receptors in infection, inflammation, and cancer. Trends Immunol. 39, 815–829 (2018).
Eisenhut, M. & Wallace, H. Ion channels in inflammation. Pflug. Arch. 461, 401–421 (2011).
Chen, G. Y. & Nunez, G. Sterile inflammation: sensing and reacting to damage. Nat. Rev. Immunol. 10, 826–837 (2010).
Lau, C. M. et al. RNA-associated autoantigens activate B cells by combined B cell antigen receptor/Toll-like receptor 7 engagement. J. Exp. Med. 202, 1171–1177 (2005).
Qin, C. et al. Critical role of P2Y12 receptor in regulation of TH17 differentiation and experimental autoimmune encephalomyelitis pathogenesis. J. Immunol. 199, 72–81 (2017).
Roh, J. S. & Sohn, D. H. Damage-associated molecular patterns in inflammatory diseases. Immune Netw. 18, e27 (2018).
Roers, A., Hiller, B. & Hornung, V. Recognition of endogenous nucleic acids by the innate immune system. Immunity 44, 739–754 (2016).
Mangan, M. S. J. et al. Targeting the NLRP3 inflammasome in inflammatory diseases. Nat. Rev. Drug Discov. 17, 588–606 (2018).
Li, T. & Chen, Z. J. The cGAS–cGAMP–STING pathway connects DNA damage to inflammation, senescence, and cancer. J. Exp. Med. 215, 1287–1299 (2018).
Kawasaki, T. & Kawai, T. Toll-like receptor signaling pathways. Front. Immunol. 5, 461 (2014).
Yu, L., Wang, L. & Chen, S. Endogenous Toll-like receptor ligands and their biological significance. J. Cell Mol. Med. 14, 2592–2603 (2010).
Erridge, C. Endogenous ligands of TLR2 and TLR4: agonists or assistants? J. Leukoc. Biol. 87, 989–999 (2010).
Yang, H. et al. MD-2 is required for disulfide HMGB1-dependent TLR4 signaling. J. Exp. Med. 212, 5–14 (2015).
Lee, K. M. & Seong, S. Y. Partial role of TLR4 as a receptor responding to damage-associated molecular pattern. Immunol. Lett. 125, 31–39 (2009).
Lin, Q., Li, M., Fang, D., Fang, J. & Su, S. B. The essential roles of Toll-like receptor signaling pathways in sterile inflammatory diseases. Int. Immunopharmacol. 11, 1422–1432 (2011).
Wu, H. et al. TLR4 activation mediates kidney ischemia/reperfusion injury. J. Clin. Invest. 117, 2847–2859 (2007).
Bell, M. T. et al. Toll-like receptor 4-dependent microglial activation mediates spinal cord ischemia–reperfusion injury. Circulation 128, S152–S156 (2013).
Wu, H. et al. HMGB1 contributes to kidney ischemia reperfusion injury. J. Am. Soc. Nephrol. 21, 1878–1890 (2010).
Tsung, A. et al. The nuclear factor HMGB1 mediates hepatic injury after murine liver ischemia–reperfusion. J. Exp. Med. 201, 1135–1143 (2005).
Leemans, J. C. et al. Renal-associated TLR2 mediates ischemia/reperfusion injury in the kidney. J. Clin. Invest. 115, 2894–2903 (2005).
Bamboat, Z. M. et al. Toll-like receptor 9 inhibition confers protection from liver ischemia–reperfusion injury. Hepatology 51, 621–632 (2010).
Pope, M. R. & Fleming, S. D. TLR2 modulates antibodies required for intestinal ischemia/reperfusion-induced damage and inflammation. J. Immunol. 194, 1190–1198 (2015).
Cavassani, K. A. et al. TLR3 is an endogenous sensor of tissue necrosis during acute inflammatory events. J. Exp. Med. 205, 2609–2621 (2008).
Barrat, F. J. et al. Nucleic acids of mammalian origin can act as endogenous ligands for Toll-like receptors and may promote systemic lupus erythematosus. J. Exp. Med. 202, 1131–1139 (2005).
Viglianti, G. A. et al. Activation of autoreactive B cells by CpG dsDNA. Immunity 19, 837–847 (2003).
Christensen, S. R. et al. Toll-like receptor 7 and TLR9 dictate autoantibody specificity and have opposing inflammatory and regulatory roles in a murine model of lupus. Immunity 25, 417–428 (2006).
Wu, X. & Peng, S. L. Toll-like receptor 9 signaling protects against murine lupus. Arthritis Rheum. 54, 336–342 (2006).
Bekeredjian-Ding, I. B. et al. Plasmacytoid dendritic cells control TLR7 sensitivity of naive B cells via type I IFN. J. Immunol. 174, 4043–4050 (2005).
Midwood, K. et al. Tenascin-C is an endogenous activator of Toll-like receptor 4 that is essential for maintaining inflammation in arthritic joint disease. Nat. Med. 15, 774–780 (2009).
Shi, B. et al. SNAPIN: an endogenous Toll-like receptor ligand in rheumatoid arthritis. Ann. Rheum. Dis. 71, 1411–1417 (2012).
Roelofs, M. F. et al. Identification of small heat shock protein B8 (HSP22) as a novel TLR4 ligand and potential involvement in the pathogenesis of rheumatoid arthritis. J. Immunol. 176, 7021–7027 (2006).
Kim, S. J. et al. Identification of a novel Toll-like receptor 7 endogenous ligand in rheumatoid arthritis synovial fluid that can provoke arthritic joint inflammation. Arthritis Rheumatol. 68, 1099–1110 (2016).
Patidar, A. et al. DAMP-TLR-cytokine axis dictates the fate of tumor. Cytokine 104, 114–123 (2018).
Hardison, S. E. & Brown, G. D. C-type lectin receptors orchestrate antifungal immunity. Nat. Immunol. 13, 817–822 (2012).
Ahrens, S. et al. F-actin is an evolutionarily conserved damage-associated molecular pattern recognized by DNGR-1, a receptor for dead cells. Immunity 36, 635–645 (2012).
Sancho, D. et al. Identification of a dendritic cell receptor that couples sensing of necrosis to immunity. Nature 458, 899–903 (2009).
Tullett, K. M. et al. Targeting CLEC9A delivers antigen to human CD141(+) DC for CD4(+) and CD8(+)T cell recognition. JCI Insight 1, e87102 (2016).
Haddad, Y. et al. The dendritic cell receptor DNGR-1 promotes the development of atherosclerosis in mice. Circ. Res. 121, 234–243 (2017).
Del Fresno, C. & Saz-Leal, P. DNGR-1 in dendritic cells limits tissue damage by dampening neutrophil recruitment. Science 362, 351–356 (2018).
Suzuki, Y. et al. Involvement of Mincle and Syk in the changes to innate immunity after ischemic stroke. Sci. Rep. 3, 3177 (2013).
De Rivero Vaccari, J. C. et al. Mincle signaling in the innate immune response after traumatic brain injury. J. Neurotrauma 32, 228–236 (2015).
Nagata, M. et al. Intracellular metabolite beta-glucosylceramide is an endogenous Mincle ligand possessing immunostimulatory activity. Proc. Natl Acad. Sci. USA 114, E3285–e3294 (2017).
Chiba, S. et al. Recognition of tumor cells by Dectin-1 orchestrates innate immune cells for anti-tumor responses. eLife 3, e04177 (2014).
Gong, T., Jiang, W. & Zhou, R. Control of inflammasome activation by phosphorylation. Trends Biochem. Sci. 43, 685–699 (2018).
Halle, A. et al. The NALP3 inflammasome is involved in the innate immune response to amyloid-beta. Nat. Immunol. 9, 857–865 (2008).
Duewell, P. et al. NLRP3 inflammasomes are required for atherogenesis and activated by cholesterol crystals. Nature 464, 1357–1361 (2010).
Zhong, Z. et al. New mitochondrial DNA synthesis enables NLRP3 inflammasome activation. Nature 560, 198–203 (2018).
Zhou, R., Yazdi, A. S., Menu, P. & Tschopp, J. A role for mitochondria in NLRP3 inflammasome activation. Nature 469, 221–225 (2011). Zhou et al. provide the first study to show the crucial role of mitochondria in NLRP3 inflammasome activation.
Iyer, S. S. et al. Mitochondrial cardiolipin is required for Nlrp3 inflammasome activation. Immunity 39, 311–323 (2013).
Chen, J. & Chen, Z. J. PtdIns4P on dispersed trans-Golgi network mediates NLRP3 inflammasome activation. Nature 564, 71–76 (2018). This study suggests that Golgi dispersion acts as an upstream event to initiate NLRP3 inflammasome assembly.
Gong, T., Yang, Y., Jin, T., Jiang, W. & Zhou, R. Orchestration of NLRP3 inflammasome activation by ion fluxes. Trends Immunol. 39, 393–406 (2018).
Youm, Y. H. et al. Canonical Nlrp3 inflammasome links systemic low-grade inflammation to functional decline in aging. Cell Metab. 18, 519–532 (2013).
Zanoni, I. et al. An endogenous caspase-11 ligand elicits interleukin-1 release from living dendritic cells. Science 352, 1232–1236 (2016).
Kerur, N. et al. cGAS drives noncanonical-inflammasome activation in age-related macular degeneration. Nat. Med. 24, 50–61 (2018).
Schuberth-Wagner, C. et al. A conserved histidine in the RNA Sensor RIG-I controls immune tolerance to N1-2’O-methylated self RNA. Immunity 43, 41–51 (2015).
Devarkar, S. C. et al. Structural basis for m7G recognition and 2′-O-methyl discrimination in capped RNAs by the innate immune receptor RIG-I. Proc. Natl Acad. Sci. USA 113, 596–601 (2016).
Boelens, M. C. et al. Exosome transfer from stromal to breast cancer cells regulates therapy resistance pathways. Cell 159, 499–513 (2014).
Nabet, B. Y. et al. Exosome RNA unshielding couples stromal activation to pattern recognition receptor signaling in cancer. Cell 170, 352–366.e13 (2017). Boelens et al. and Nabet et al. demonstrate that endogenous 5′ppp RNA promotes breast cancer cells growth and therapy resistance via RIG-I signalling.
Liddicoat, B. J. et al. RNA editing by ADAR1 prevents MDA5 sensing of endogenous dsRNA as nonself. Science 349, 1115–1120 (2015).
Eckard, S. C. et al. The SKIV2L RNA exosome limits activation of the RIG-I-like receptors. Nat. Immunol. 15, 839–845 (2014).
Roulois, D. et al. DNA-demethylating agents target colorectal cancer cells by inducing viral mimicry by endogenous transcripts. Cell 162, 961–973 (2015).
Chiappinelli, K. B. et al. Inhibiting DNA methylation causes an interferon response in cancer via dsRNA including endogenous retroviruses. Cell 162, 974–986 (2015). Roulois et al. and Chiappinelli et al. suggest that endogenous retroviral RNA activates MDA5-signalling in tumour cells to reduce cancer cell proliferation and facilitate tumour immunotherapy.
Ishizuka, J. J. et al. Loss of ADAR1 in tumours overcomes resistance to immune checkpoint blockade. Nature 565, 43–48 (2019).
Li, X. D. et al. Pivotal roles of cGAS–cGAMP signaling in antiviral defense and immune adjuvant effects. Science 341, 1390–1394 (2013).
Rathinam, V. A. et al. The AIM2 inflammasome is essential for host defense against cytosolic bacteria and DNA viruses. Nat. Immunol. 11, 395–402 (2010).
Komada, T. et al. Macrophage uptake of necrotic cell DNA activates The Aim2 inflammasome to regulate a proinflammatory phenotype in CKD. J. Am. Soc. Nephrol. 29, 1165–1181 (2018). This study shows that self-DNA released from necrotic cells activates the AIM2 inflammasome, contributing to chronic kidney injury.
Pokatayev, V. et al. RNase H2 catalytic core Aicardi–Goutieres syndrome-related mutant invokes cGAS–STING innate immune-sensing pathway in mice. J. Exp. Med. 213, 329–336 (2016).
Mackenzie, K. J. et al. Ribonuclease H2 mutations induce a cGAS/STING-dependent innate immune response. EMBO J. 35, 831–844 (2016).
Gao, D. et al. Activation of cyclic GMP–AMP synthase by self-DNA causes autoimmune diseases. Proc. Natl Acad. Sci. USA 112, E5699–E5705 (2015).
Maelfait, J., Bridgeman, A., Benlahrech, A., Cursi, C. & Rehwinkel, J. Restriction by SAMHD1 limits cGAS/STING-dependent innate and adaptive immune responses to HIV-1. Cell Rep. 16, 1492–1501 (2016).
Hartlova, A. et al. DNA damage primes the type I interferon system via the cytosolic DNA sensor STING to promote anti-microbial innate immunity. Immunity 42, 332–343 (2015). Pokatayev et al., Mackenzie et al., Gao et al., Maelfait et al. and Hartlova et al. demonstrate that aberrant activation of the cGAS–STING pathway can lead to the development of autoimmune diseases in mouse models, such as AGS and AT.
Rodero, M. P., Tesser, A. & Bartok, E. Type I interferon-mediated autoinflammation due to DNase II deficiency. Nat. Commun. 8, 2176 (2017).
Woo, S. R. et al. STING-dependent cytosolic DNA sensing mediates innate immune recognition of immunogenic tumors. Immunity 41, 830–842 (2014).
Xu, M. M. et al. Dendritic cells but not macrophages sense tumor mitochondrial dna for cross-priming through signal regulatory protein alpha signaling. Immunity 47, 363–373.e5 (2017).
Cunha, L. D. et al. LC3-associated phagocytosis in myeloid cells promotes tumor immune tolerance. Cell 175, 429–441.e16 (2018).
Harding, S. M. et al. Mitotic progression following DNA damage enables pattern recognition within micronuclei. Nature 548, 466–470 (2017).
Li, T. et al. Antitumor activity of cGAMP via stimulation of cGAS–cGAMP–STING–IRF3 mediated innate immune response. Sci. Rep. 6, 19049 (2016).
Ahn, J. et al. Inflammation-driven carcinogenesis is mediated through STING. Nat. Commun. 5, 5166 (2014).
Bakhoum, S. F. et al. Chromosomal instability drives metastasis through a cytosolic DNA response. Nature 553, 467–472 (2018).
Larkin, B. et al. Cutting edge: activation of STING in T cells induces type I IFN responses and cell death. J. Immunology 199, 397–402 (2017).
Gulen, M. F. et al. Signalling strength determines proapoptotic functions of STING. Nat. Commun. 8, 427 (2017).
d’Adda di Fagagna, F. Living on a break: cellular senescence as a DNA-damage response. Nat. Rev. Cancer 8, 512–522 (2008).
Dou, Z. et al. Cytoplasmic chromatin triggers inflammation in senescence and cancer. Nature 550, 402–406 (2017).
Gluck, S. et al. Innate immune sensing of cytosolic chromatin fragments through cGAS promotes senescence. Nat. Cell Biol. 19, 1061–1070 (2017).
Yang, H., Wang, H., Ren, J., Chen, Q. & Chen, Z. J. cGAS is essential for cellular senescence. Proc. Natl Acad. Sci. USA 114, E4612–e4620 (2017). Dou et al., Gluck et al. and Yang et al. demonstrate that cGAS is essential for cellular senescence.
Hu, B. et al. The DNA-sensing AIM2 inflammasome controls radiation-induced cell death and tissue injury. Science 354, 765–768 (2016).
Lian, Q. et al. Chemotherapy-induced intestinal inflammatory responses are mediated by exosome secretion of double-strand DNA via AIM2 inflammasome activation. Cell Res. 27, 784–800 (2017).
Feng, L. et al. Chronic vascular inflammation in patients with type 2 diabetes: endothelial biopsy and RT-PCR analysis. Diabetes Care 28, 379–384 (2005).
Tanaka, N. et al. The receptor for advanced glycation end products is induced by the glycation products themselves and tumor necrosis factor-alpha through nuclear factor-kappa B, and by 17beta-estradiol through Sp-1 in human vascular endothelial cells. J. Biol. Chem. 275, 25781–25790 (2000).
Chen, Y. et al. HMGB1 contributes to the expression of p-glycoprotein in mouse epileptic brain through toll-like receptor 4 and receptor for advanced glycation end products. PLOS ONE 10, e0140918 (2015).
Wautier, J. L. et al. Receptor-mediated endothelial cell dysfunction in diabetic vasculopathy: soluble receptor for advanced glycation end products blocks hyperpermeability in diabetic rats. J. Clin. Invest. 97, 238–243 (1996).
Manigrasso, M. B., Juranek, J., Ramasamy, R. & Schmidt, A. M. Unlocking the biology of RAGE in diabetic microvascular complications. Trends Endocrinol. Metab. 25, 15–22 (2014).
Nagareddy, P. R. et al. Hyperglycemia promotes myelopoiesis and impairs the resolution of atherosclerosis. Cell Metab. 17, 695–708 (2013).
Kraakman, M. J. et al. Neutrophil-derived S100 calcium-binding proteins A8/A9 promote reticulated thrombocytosis and atherogenesis in diabetes. J. Clin. Invest. 127, 2133–2147 (2017). Nagareddy et al. and Kraakman et al. demonstrate that S100A8/A9 bind to RAGE on common myeloid progenitor cells and Kupfer cells to facilitate myelopoiesis and thrombopoietin production, respectively, which promotes inflammatory cell recruitment and atherogenesis.
Roth, S. & Singh, V. Brain-released alarmins and stress response synergize in accelerating atherosclerosis progression after stroke. Sci. Transl Med. 10, eaao1313 (2018).
Pickering, R. J. et al. Transactivation of RAGE mediates angiotensin-induced inflammation and atherogenesis. J. Clin. Invest. 129, 406–421 (2019).
Kwak, T. et al. Targeting of RAGE-ligand signaling impairs breast cancer cell invasion and metastasis. Oncogene 36, 1559–1572 (2017).
Mendez, O. & Peg, V. Extracellular HMGA1 promotes tumor invasion and metastasis in triple-negative breast cancer. Clin. Cancer Res. 24, 6367–6382 (2018).
Nasser, M. W. et al. RAGE mediates S100A7-induced breast cancer growth and metastasis by modulating the tumor microenvironment. Cancer Res. 75, 974–985 (2015).
Wang, W. et al. Upregulation of PD-L1 via HMGB1-activated IRF3 and NF-κB contributes to UV radiation-induced immune suppression. Cancer Res. 79, 2909–2922 (2019).
He, S. et al. HMGB1 released by irradiated tumor cells promotes living tumor cell proliferation via paracrine effect. Cell Death Dis. 9, 648 (2018).
Sinha, P. et al. Proinflammatory S100 proteins regulate the accumulation of myeloid-derived suppressor cells. J. Immunol. 181, 4666–4675 (2008).
Wild, C. A. et al. HMGB1 conveys immunosuppressive characteristics on regulatory and conventional T cells. Int. Immunol. 24, 485–494 (2012).
Liu, Z., Falo, L. D. Jr. & You, Z. Knockdown of HMGB1 in tumor cells attenuates their ability to induce regulatory T cells and uncovers naturally acquired CD8 T cell-dependent antitumor immunity. J. Immunol. 187, 118–125 (2011).
Cheng, P. et al. Inhibition of dendritic cell differentiation and accumulation of myeloid-derived suppressor cells in cancer is regulated by S100A9 protein. J. Exp. Med. 205, 2235–2249 (2008).
Deane, R. et al. RAGE mediates amyloid-beta peptide transport across the blood-brain barrier and accumulation in brain. Nat. Med. 9, 907–913 (2003).
Takuma, K. et al. RAGE-mediated signaling contributes to intraneuronal transport of amyloid-beta and neuronal dysfunction. Proc. Natl Acad. Sci. USA 106, 20021–20026 (2009).
Lue, L. F. et al. Involvement of microglial receptor for advanced glycation endproducts (RAGE) in Alzheimer’s disease: identification of a cellular activation mechanism. Exp. Neurol. 171, 29–45 (2001).
Chuah, Y. K., Basir, R., Talib, H., Tie, T. H. & Nordin, N. Receptor for advanced glycation end products and its involvement in inflammatory diseases. Int. J. Inflam. 2013, 403460 (2013).
Tammaro, A. et al. TREM-1 and its potential ligands in non-infectious diseases: from biology to clinical perspectives. Pharmacol. Ther. 177, 81–95 (2017).
Jay, T. R., von Saucken, V. E. & Landreth, G. E. TREM2 in neurodegenerative diseases. Mol. Neurodegener. 12, 56 (2017).
Bouchon, A., Dietrich, J. & Colonna, M. Inflammatory responses can be triggered by TREM-1, a novel receptor expressed on neutrophils and monocytes. J. Immunol. 164, 4991–4995 (2000).
Bouchon, A., Facchetti, F., Weigand, M. A. & Colonna, M. TREM-1 amplifies inflammation and is a crucial mediator of septic shock. Nature 410, 1103–1107 (2001).
Wu, J. et al. The proinflammatory myeloid cell receptor TREM-1 controls Kupffer cell activation and development of hepatocellular carcinoma. Cancer Res. 72, 3977–3986 (2012).
El Mezayen, R. et al. Endogenous signals released from necrotic cells augment inflammatory responses to bacterial endotoxin. Immunol. Lett. 111, 36–44 (2007).
Read, C. B. et al. Identification of neutrophil PGLYRP1 as a ligand for TREM-1. J. Immunol. 194, 1417–1421 (2015).
Fu, L. et al. Identification of extracellular actin as a ligand for triggering receptor expressed on myeloid cells-1 signaling. Front. Immunol. 8, 917 (2017).
Nguyen-Lefebvre, A. T. et al. The innate immune receptor TREM-1 promotes liver injury and fibrosis. J. Clin. Invest. 128, 4870–4883 (2018).
Ho, C. C. et al. TREM-1 expression in tumor-associated macrophages and clinical outcome in lung cancer. Am. J. Respir. Crit. Care Med. 177, 763–770 (2008).
Bailey, C. C., DeVaux, L. B. & Farzan, M. The triggering receptor expressed on myeloid cells 2 binds apolipoprotein E. J. Biol. Chem. 290, 26033–26042 (2015).
Wang, Y. et al. TREM2 lipid sensing sustains the microglial response in an Alzheimer’s disease model. Cell 160, 1061–1071 (2015). This study demonstrates that TREM2 acts as a lipid-sensing receptor to sustain microglial response to Aβ accumulation in a mouse model of AD.
Poliani, P. L. et al. TREM2 sustains microglial expansion during aging and response to demyelination. J. Clin. Invest. 125, 2161–2170 (2015).
Cannon, J. P., O’Driscoll, M. & Litman, G. W. Specific lipid recognition is a general feature of CD300 and TREM molecules. Immunogenetics 64, 39–47 (2012).
Yeh, F. L., Wang, Y., Tom, I., Gonzalez, L. C. & Sheng, M. TREM2 binds to apolipoproteins, including APOE and CLU/APOJ, and thereby facilitates uptake of amyloid-beta by microglia. Neuron 91, 328–340 (2016).
Yuan, P. et al. TREM2 haplodeficiency in mice and humans impairs the microglia barrier function leading to decreased amyloid compaction and severe axonal dystrophy. Neuron 90, 724–739 (2016).
Wang, Y. et al. TREM2-mediated early microglial response limits diffusion and toxicity of amyloid plaques. J. Exp. Med. 213, 667–675 (2016).
Paloneva, J. et al. Mutations in two genes encoding different subunits of a receptor signaling complex result in an identical disease phenotype. Am. J. Hum. Genet. 71, 656–662 (2002).
Paloneva, J. et al. DAP12/TREM2 deficiency results in impaired osteoclast differentiation and osteoporotic features. J. Exp. Med. 198, 669–675 (2003).
Cantoni, C. et al. TREM2 regulates microglial cell activation in response to demyelination in vivo. Acta Neuropathol. 129, 429–447 (2015).
Stefano, L. et al. The surface-exposed chaperone, Hsp60, is an agonist of the microglial TREM2 receptor. J. Neurochem. 110, 284–294 (2009).
Rayaprolu, S. et al. TREM2 in neurodegeneration: evidence for association of the p.R47H variant with frontotemporal dementia and Parkinson’s disease. Mol. Neurodegener. 8, 19 (2013).
Cady, J. et al. TREM2 variant p.R47H as a risk factor for sporadic amyotrophic lateral sclerosis. JAMA Neurol. 71, 449–453 (2014).
Idzko, M., Ferrari, D. & Eltzschig, H. K. Nucleotide signalling during inflammation. Nature 509, 310–317 (2014).
Rossol, M. et al. Extracellular Ca2+ is a danger signal activating the NLRP3 inflammasome through G protein-coupled calcium sensing receptors. Nat. Commun. 3, 1329 (2012).
Zhang, Q. et al. Circulating mitochondrial DAMPs cause inflammatory responses to injury. Nature 464, 104–107 (2010).
Marques, P. E. et al. Chemokines and mitochondrial products activate neutrophils to amplify organ injury during mouse acute liver failure. Hepatology 56, 1971–1982 (2012).
Dorward, D. A. et al. Novel role for endogenous mitochondrial formylated peptide-driven formyl peptide receptor 1 signalling in acute respiratory distress syndrome. Thorax 72, 928–936 (2017).
Cardini, S. et al. Genetic ablation of the Fpr1 gene confers protection from smoking-induced lung emphysema in mice. Am. J. Respir. Cell Mol. Biol. 47, 332–339 (2012).
Su, S. B. et al. A seven-transmembrane, G protein-coupled receptor, FPRL1, mediates the chemotactic activity of serum amyloid A for human phagocytic cells. J. Exp. Med. 189, 395–402 (1999).
Lee, H. Y., Oh, E., Kim, S. D., Seo, J. K. & Bae, Y. S. Oxidized low-density lipoprotein-induced foam cell formation is mediated by formyl peptide receptor 2. Biochem. Biophys. Res. Commun. 443, 1003–1007 (2014).
Eklund, K. K., Niemi, K. & Kovanen, P. T. Immune functions of serum amyloid A. Crit. Rev. Immunol. 32, 335–348 (2012).
Di Pietro, N., Formoso, G. & Pandolfi, A. Physiology and pathophysiology of oxLDL uptake by vascular wall cells in atherosclerosis. Vasc. Pharmacol. 84, 1–7 (2016).
Greenspan, P., Yu, H., Mao, F. & Gutman, R. L. Cholesterol deposition in macrophages: foam cell formation mediated by cholesterol-enriched oxidized low density lipoprotein. J. Lipid Res. 38, 101–109 (1997).
Chen, Y. et al. ATP release guides neutrophil chemotaxis via P2Y2 and A3 receptors. Science 314, 1792–1795 (2006).
Elliott, M. R. et al. Nucleotides released by apoptotic cells act as a find-me signal to promote phagocytic clearance. Nature 461, 282–286 (2009). Chen et al. and Elliott et al. show that ATP and UTP can promote the recruitment of macrophages and neutrophils through the activation of P2Y2 receptors.
Cekic, C. & Linden, J. Purinergic regulation of the immune system. Nat. Rev. Immunol. 16, 177–192 (2016).
Myrtek, D. & Idzko, M. Chemotactic activity of extracellular nucleotideson human immune cells. Purinergic Signal. 3, 5–11 (2007).
Ferrari, D. et al. Activation of human eosinophils via P2 receptors: novel findings and future perspectives. J. Leukoc. Biol. 79, 7–15 (2006).
Stachon, P. et al. Extracellular ATP Induces vascular inflammation and atherosclerosis via purinergic receptor Y2 in Mice. Arterioscler. Thromb. Vasc. Biol. 36, 1577–1586 (2016).
Dorsam, R. T. & Kunapuli, S. P. Central role of the P2Y12 receptor in platelet activation. J. Clin. Invest. 113, 340–345 (2004).
Li, D. et al. Roles of purinergic receptor P2Y, G protein-coupled 12 in the development of atherosclerosis in apolipoprotein E-deficient mice. Arterioscler Thromb. Vasc. Biol. 32, e81–e89 (2012).
Olszak, I. T. et al. Extracellular calcium elicits a chemokinetic response from monocytes in vitro and in vivo. J. Clin. Invest. 105, 1299–1305 (2000).
Lee, G. S. et al. The calcium-sensing receptor regulates the NLRP3 inflammasome through Ca2+ and cAMP. Nature 492, 123–127 (2012).
Munoz-Planillo, R. et al. K(+) efflux is the common trigger of NLRP3 inflammasome activation by bacterial toxins and particulate matter. Immunity 38, 1142–1153 (2013).
Moran, M. M., McAlexander, M. A., Biro, T. & Szallasi, A. Transient receptor potential channels as therapeutic targets. Nat. Rev. Drug Discov. 10, 601–620 (2011).
Di Virgilio, F., Dal Ben, D., Sarti, A. C., Giuliani, A. L. & Falzoni, S. The P2X7 receptor in infection and inflammation. Immunity 47, 15–31 (2017).
Brennan, T. V., Rendell, V. R. & Yang, Y. Innate immune activation by tissue injury and cell death in the setting of hematopoietic stem cell transplantation. Front. Immunol. 6, 101 (2015).
Knowles, H. et al. Transient receptor potential melastatin 2 (TRPM2) ion channel is required for innate immunity against Listeria monocytogenes. Proc. Natl Acad. Sci. USA 108, 11578–11583 (2011).
Yamamoto, S. et al. TRPM2-mediated Ca2+ influx induces chemokine production in monocytes that aggravates inflammatory neutrophil infiltration. Nat. Med. 14, 738–747 (2008).
Haraguchi, K. et al. TRPM2 contributes to inflammatory and neuropathic pain through the aggravation of pronociceptive inflammatory responses in mice. J. Neurosci. 32, 3931–3941 (2012). Yamamoto et al. and Haraguchi et al. demonstrate that TRPM2 controls ROS-induced Ca 2+ influx and the production of the chemokine CXCL2, both in vitro and in vivo.
Zhong, Z. et al. TRPM2 links oxidative stress to NLRP3 inflammasome activation. Nat. Commun. 4, 1611 (2013).
Fernandes, E. S., Fernandes, M. A. & Keeble, J. E. The functions of TRPA1 and TRPV1: moving away from sensory nerves. Br. J. Pharmacol. 166, 510–521 (2012).
Hoffmeister, C. et al. Participation of the TRPV1 receptor in the development of acute gout attacks. Rheumatology 53, 240–249 (2014).
Moilanen, L. J., Hamalainen, M., Lehtimaki, L., Nieminen, R. M. & Moilanen, E. Urate crystal induced inflammation and joint pain are reduced in transient receptor potential ankyrin 1 deficient mice-potential role for transient receptor potential ankyrin 1 in gout. PLOS ONE 10, e0117770 (2015).
Hiroi, T. et al. Neutrophil TRPM2 channels are implicated in the exacerbation of myocardial ischaemia/reperfusion injury. Cardiovasc. Res. 97, 271–281 (2013).
Gelderblom, M. et al. Transient receptor potential melastatin subfamily member 2 cation channel regulates detrimental immune cell invasion in ischemic stroke. Stroke 45, 3395–3402 (2014).
Caceres, A. I. et al. A sensory neuronal ion channel essential for airway inflammation and hyperreactivity in asthma. Proc. Natl Acad. Sci. USA 106, 9099–9104 (2009).
Savio, L. E. B., de Andrade Mello, P., da Silva, C. G. & Coutinho-Silva, R. The P2X7 receptor in inflammatory diseases: angel or demon? Front. Pharmacol. 9, 52 (2018).
Kurashima, Y. et al. Extracellular ATP mediates mast cell-dependent intestinal inflammation through P2X7 purinoceptors. Nat. Commun. 3, 1034 (2012).
Shiratori, M., Tozaki-Saitoh, H., Yoshitake, M., Tsuda, M. & Inoue, K. P2X7 receptor activation induces CXCL2 production in microglia through NFAT and PKC/MAPK pathways. J. Neurochem. 114, 810–819 (2010).
Karmakar, M., Katsnelson, M. A. & Dubyak, G. R. Neutrophil P2X7 receptors mediate NLRP3 inflammasome-dependent IL-1beta secretion in response to ATP. Nat. Commun. 7, 10555 (2016).
Riteau, N. et al. Extracellular ATP is a danger signal activating P2X7 receptor in lung inflammation and fibrosis. Am. J. Respir. Crit. Care Med. 182, 774–783 (2010).
Vergani, A. et al. Long-term heart transplant survival by targeting the ionotropic purinergic receptor P2X7. Circulation 127, 463–475 (2013).
Wang, X. et al. P2X7 receptor inhibition improves recovery after spinal cord injury. Nat. Med. 10, 821–827 (2004).
Tian, J. et al. Toll-like receptor 9-dependent activation by DNA-containing immune complexes is mediated by HMGB1 and RAGE. Nat. Immunol. 8, 487–496 (2007). This study shows that HMGB1 can bind to endogenous DNA and augment DNA-induced TLR9 activation and cytokine release.
Babelova, A. et al. Biglycan, a danger signal that activates the NLRP3 inflammasome via toll-like and P2X receptors. J. Biol. Chem. 284, 24035–24048 (2009).
Bertheloot, D. & Latz, E. HMGB1, IL-1alpha, IL-33 and S100 proteins: dual-function alarmins. Cell Mol. Immunol. 14, 43–64 (2017).
Lu, B. et al. Novel role of PKR in inflammasome activation and HMGB1 release. Nature 488, 670–674 (2012).
Zarember, K. A. & Godowski, P. J. Tissue expression of human Toll-like receptors and differential regulation of Toll-like receptor mRNAs in leukocytes in response to microbes, their products, and cytokines. J. Immunol. 168, 554–561 (2002).
Ma, F. et al. Positive feedback regulation of type I IFN production by the IFN-inducible DNA sensor cGAS. J. Immunol. 194, 1545–1554 (2015).
Liu, Q. et al. Cytosolic sensors of viral RNA are involved in the production of interleukin-6 via toll-like receptor 3 signaling in human glomerular endothelial cells. Kidney Blood Press. Res. 44, 62–71 (2019).
Lotfi, R. et al. Eosinophils oxidize damage-associated molecular pattern molecules derived from stressed cells. J. Immunol. 183, 5023–5031 (2009). This study shows that ROS can oxidize and inactivate HMGB1 in order to control inflammation.
Bamboat, Z. M. et al. Conventional DCs reduce liver ischemia/reperfusion injury in mice via IL-10 secretion. J. Clin. Invest. 120, 559–569 (2010).
Kong, D., Shen, Y. & Liu, G. PKA regulatory IIalpha subunit is essential for PGD2-mediated resolution of inflammation. J. Exp. Med. 213, 2209–2226 (2016).
Wang, Y. et al. Inflammasome activation triggers caspase-1-mediated cleavage of cGAS to regulate responses to DNA virus infection. Immunity 46, 393–404 (2017). This study demonstrates that inflammasome activation inhibits cGAS signalling through the caspase-1-mediated cleavage of cGAS.
Trenk, D., Kristensen, S. D., Hochholzer, W. & Neumann, F. J. High on-treatment platelet reactivity and P2Y12 antagonists in clinical trials. Thromb. Haemost. 109, 834–845 (2013).
Bartlett, R., Stokes, L. & Sluyter, R. The P2X7 receptor channel: recent developments and the use of P2X7 antagonists in models of disease. Pharmacol. Rev. 66, 638–675 (2014).
Coll, R. C. et al. A small-molecule inhibitor of the NLRP3 inflammasome for the treatment of inflammatory diseases. Nat. Med. 21, 248 (2015).
Coll, R. C. et al. MCC950 directly targets the NLRP3 ATP-hydrolysis motif for inflammasome inhibition. Nat. Chem. Biol. 15, 556–559 (2019).
He, H. et al. Oridonin is a covalent NLRP3 inhibitor with strong anti-inflammasome activity. Nat. Commun. 9, 2550 (2018).
Jiang, H. et al. Identification of a selective and direct NLRP3 inhibitor to treat inflammatory disorders. J. Exp. Med. 214, 3219–3238 (2017).
Huang, Y. et al. Tranilast directly targets NLRP3 to treat inflammasome-driven diseases. EMBO Mol. Med. 10, e8689 (2018). Coll et al. (2015), Coll et al. (2019), He et al., Jiang et al. amd Huang et al. describe several compounds that target NLRP3 and show potent therapeutic effects for NLRP3-related diseases in mouse models.
Vincent, J. et al. Small molecule inhibition of cGAS reduces interferon expression in primary macrophages from autoimmune mice. Nat. Commun. 8, 750 (2017).
Haag, S. M. et al. Targeting STING with covalent small-molecule inhibitors. Nature 559, 269–273 (2018). This is the first study to show that STING-targeted small-molecule inhibitors attenuate pathological features of autoimmune disease in mice.
Land, W. G. The role of damage-associated molecular patterns in human diseases: part I — promoting inflammation and immunity. Sultan Qaboos Univ. Med. J. 15, e9–e21 (2015).
Land, W. G. Damage-Associated Molecular Patterns in Human Diseases: Volume 1. Injury-Induced Innate Immune Responses (Springer, 2018).
Rubartelli, A. & Sitia, R. Stress as an intercellular signal: the emergence of stress-associated molecular patterns (SAMP). Antioxid. Redox Signal. 11, 2621–2629 (2009).
Liston, A. & Masters, S. L. Homeostasis-altering molecular processes as mechanisms of inflammasome activation. Nat. Rev. Immunol. 17, 208–214 (2017).
Yatim, N., Cullen, S. & Albert, M. L. Dying cells actively regulate adaptive immune responses. Nat. Rev. Immunol. 17, 262–275 (2017).
Shao, Y. et al. Lysophospholipids and their receptors serve as conditional DAMPs and DAMP receptors in tissue oxidative and inflammatory injury. Antioxid. Redox Signal. 28, 973–986 (2018).
Xiahou, Z. et al. NMI and IFP35 serve as proinflammatory DAMPs during cellular infection and injury. Nat. Commun. 8, 950 (2017).
Pradeu, T. & Cooper, E. L. The danger theory: 20 years later. Front. Immunol. 3, 287 (2012).
Matzinger, P. The danger model: a renewed sense of self. Science 296, 301–305 (2002).
Kim, S. et al. Carcinoma-produced factors activate myeloid cells through TLR2 to stimulate metastasis. Nature 457, 102–106 (2009).
Riddell, J. R. et al. Peroxiredoxin 1 controls prostate cancer growth through Toll-like receptor 4-dependent regulation of tumor vasculature. Cancer Res. 71, 1637–1646 (2011).
Acknowledgements
This work was supported by the National Key research and development program of China (grant 2019YFA0508503), the Strategic Priority Research Program of the Chinese Academy of Sciences (grant XDB29030102), the National Natural Science Foundation of China (grants 31770991, 91742202, 81525013, 81722022, 81788101, 81821001) and the Young Talent Support Program and Fundamental Research Funds for the Central Universities.
Author information
Authors and Affiliations
Contributions
All authors contributed to writing and editing the review. T.G. and L.L. share first authorship.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information
Nature Reviews Immunology thanks Michael Lotze and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Glossary
- Pattern recognition receptors
-
(PRRs). A group of germ-line-encoded innate immune sensors that can initiate an innate immune response by detecting highly conserved molecules typical of pathogens. In addition to their well-established roles in pathogen recognition, several PRRs can also recognize endogenous ligands released by distressed or damaged cells and initiate sterile immune responses.
- Ischaemia–reperfusion injury
-
(IRI). Tissue injury that occurs when blood flow returns to tissue after a period of ischaemia, which is accompanied by inflammatory cell infiltration, ROS production and cytokine release. It can occur in various organ systems, including the brain, heart and kidneys, leading to stroke, myocardial infarction and acute kidney injury, respectively.
- β2-Glycoprotein I
-
An abundant plasma glycoprotein, also known as apolipoprotein H, that can bind to negatively charged molecules, including phospholipids, DNA and lipoproteins. It plays an important role in a variety of physiological processes, such as coagulation, apoptosis, lipid metabolism, angiogenesis and the production of antiphospholipid autoantibodies.
- Pyroptosis
-
An inflammatory form of programmed cell death initiated by inflammasome assembly and caspase-1 or caspase-11 (in humans, caspase-1, caspase-4 or caspase-5) activation. The activated caspases cleave gasdermin D (GSDMD), generating an N-terminal GSDMD fragment that can form pores on lipid membranes and induce cell death directly.
- Inflammasome
-
A cytosolic multiprotein complex consisting of a sensor molecule, the adaptor protein ASC and cysteine protease pro-caspase-1. To date, several pattern recognition receptors, including NLRP1, NLRP3, NLRP6, NLRC4, AIM2, IFI16 and pyrin, have been found to act as sensor molecules to trigger the assembly of inflammasomes in response to microbial infection or noninfectious agonists.
- Alu-RNA
-
RNA transcripts that are transcribed from Alu elements, the most abundant repetitive elements in primate genomes. Alu-RNA can exist in two forms: free Alu-RNA is synthesized by RNA polymerase III, whereas embedded Alu-RNA is synthesized by RNA polymerase II and can be embedded in mRNAs. Both of these forms play an important role in the post-transcriptional regulation of gene expression. In addition, the level of free Alu-RNA can increase dramatically under cell stress conditions, which may be sensed by innate immune sensors.
- Non-canonical NLRP3 inflammasome
-
In contrast to canonical inflammasome assembly, the NLRP3 inflammasome can also be activated through a non-canonical pathway that requires mouse caspase 11 (the human counterparts are caspase 4 and 5).
- Aicardi–Goutières syndrome
-
(AGS). An inheritable neuroinflammatory disease that leads to microcephaly and intellectual disability with extraneurological vasculitic skin lesions. This condition is driven by chronic IFN signalling caused by mutations in genes involved in DNA degradation and metabolism or RNA editing and recognition.
- Exosomes
-
Small extracellular vesicles (with a diameter between 30 nm and 100 nm) that are produced by various types of cells, such as mesenchymal stem cells, tumour cells and dendritic cells. Several endogenous molecules, including DNA, RNA, lipids and proteins, are sorted to exosomes and are delivered from donor cells to recipient cells, a process that plays a critical role in both healthy and diseased conditions.
- 5-AZA-2′deoxycytidine
-
A deoxycytidine analogue that can incorporate into DNA strands and inhibit DNA methyltransferase activity, resulting in global DNA demethylation. It can reactivate tumour suppressor genes silenced by aberrant DNA methylation and is used in the treatment of malignancies.
- Ataxia telangiectasia
-
(AT). An autosomal recessive disease caused by mutations of ataxia telangiectasia mutated (ATM), a kinase that plays a central role in the DNA repair pathway. It affects several body systems, including the nervous system and the immune system, and leads to susceptibility to various types of cancer.
- Senescence-associated secretory phenotype
-
(SASP). A characteristic feature of senescent cells, which refers to the secretion of inflammatory cytokines, chemokines, extracellular matrix proteins and growth factors. It not only serves as a marker of senescence but also participates in the senescence process.
- Advanced glycation end products
-
(AGEs). A heterogeneous group of compounds, including proteins, lipids and nucleic acids, that are formed with reducing sugars via a non-enzymatic glycosylation reaction. AGEs play crucial roles in ageing and in the pathogenesis of various chronic and degenerative diseases, such as diabetes, chronic kidney disease, atherosclerosis and Alzheimer disease.
Rights and permissions
About this article
Cite this article
Gong, T., Liu, L., Jiang, W. et al. DAMP-sensing receptors in sterile inflammation and inflammatory diseases. Nat Rev Immunol 20, 95–112 (2020). https://doi.org/10.1038/s41577-019-0215-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41577-019-0215-7
This article is cited by
-
Mass intraoperative endothelial glycocalyx shedding affects postoperative systemic inflammation response
BMC Anesthesiology (2024)
-
Interleukin-6-elicited chronic neuroinflammation may decrease survival but is not sufficient to drive disease progression in a mouse model of Leigh syndrome
Journal of Inflammation (2024)
-
The contribution of pattern recognition receptor signalling in the development of age related macular degeneration: the role of toll-like-receptors and the NLRP3-inflammasome
Journal of Neuroinflammation (2024)
-
Isoproterenol induces MD2 activation by β-AR-cAMP-PKA-ROS signalling axis in cardiomyocytes and macrophages drives inflammatory heart failure
Acta Pharmacologica Sinica (2024)
-
Non-mutational neoantigens in disease
Nature Immunology (2024)