Abstract
X-linked hypophosphataemia (XLH) is the most frequent cause of hypophosphataemia-associated rickets of genetic origin and is associated with high levels of the phosphaturic hormone fibroblast growth factor 23 (FGF23). In addition to rickets and osteomalacia, patients with XLH have a heavy disease burden with enthesopathies, osteoarthritis, pseudofractures and dental complications, all of which contribute to reduced quality of life. This Consensus Statement presents the outcomes of a working group of the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Diseases, and provides robust clinical evidence on management in XLH, with an emphasis on patients’ experiences and needs. During growth, conventional treatment with phosphate supplements and active vitamin D metabolites (such as calcitriol) improves growth, ameliorates leg deformities and dental manifestations, and reduces pain. The continuation of conventional treatment in symptom-free adults is still debated. A novel therapeutic approach is the monoclonal anti-FGF23 antibody burosumab. Although promising, further studies are required to clarify its long-term efficacy, particularly in adults. Given the diversity of symptoms and complications, an interdisciplinary approach to management is of paramount importance. The focus of treatment should be not only on the physical manifestations and challenges associated with XLH and other FGF23-mediated hypophosphataemia syndromes, but also on the major psychological and social impact of the disease.
Similar content being viewed by others
Introduction
Renal phosphate wasting syndromes comprise a heterogeneous group of diseases with multiple causes that manifest biochemically as hypophosphataemia. The differential diagnoses of hypophosphataemia are many and the first step is to check whether reduced serum levels of phosphate are due to decreased renal tubular reabsorption of phosphate (TRP). After exclusion of parathyroid hormone (PTH)-driven decreased renal tubular phosphate reabsorption, two other main causes of renal phosphate wasting should be investigated: defects in intrinsic renal phosphate transport and fibroblast growth factor 23 (FGF23)-related causes, such as X-linked hypophosphataemia (XLH)1.
This Consensus Statement focuses on XLH as a cause of renal phosphate wasting and mentions acquired tumour-induced osteomalacia (TIO) as a differential diagnosis. XLH is a genetic disease characterized by rickets and osteomalacia and caused by pathogenic variants in PHEX (which encodes phosphate-regulating neutral endopeptidase PHEX)2. Owing to the variety of symptoms that can manifest, patients with XLH require the care of a large range of medical specialities, including paediatricians, rheumatologists, endocrinologists, nephrologists, orthopaedic surgeons, neurologists, rehabilitation specialists and dentists, across the life-course. All specialities are complementary, fulfilling an interdisciplinary patient-centred approach. In 2021, an international expert working group was convened by the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Diseases (ESCEO) to discuss the features of this interdisciplinary management strategy to address patients’ demands as well as unmet needs. The result of the working group discussions is this Consensus Statement, which provides the most current and robust clinical evidence on management of XLH.
After a brief review of the normal mineralization process and the key components involved, this Consensus Statement covers the clinical manifestations of phosphate depletion, the evaluation of a patient with hypophosphataemia and the diagnostic work-up that leads to the diagnosis of hypophosphataemia related to FGF23 excess. The Consensus Statement is centred on XLH and its main differential diagnoses in terms of clinical manifestations, as well as management via a multidisciplinary approach.
Since the last clinical practice recommendations for XLH that were released in 2019 (ref.3), several original studies have been published that cover the clinical manifestations of the disease and describe the clinical efficacy of the anti-FGF23 monoclonal antibody burosumab in treating this condition, including patient-reported outcomes. This more robust evidence base now permits, in this Consensus Statement, revised and updated clinical recommendations on the use of this novel agent in the treatment of XLH.
Methodology
This Consensus Statement provides the consensus of an expert working group of ESCEO in Geneva (Switzerland), under the auspices of the WHO Collaborating Centre for Public Health Aspects of Musculoskeletal Health and Aging (Liège, Belgium). The group comprised a diverse panel of 25 expert clinicians from 14 countries chosen for their expertise and publication record in XLH and related disorders, including orthopaedic surgeons, physical and rehabilitation medicine specialists, rheumatologists, endocrinologists, nephrologists, paediatricians, geriatricians, clinical biochemists and clinical pharmacologists. The group also included two patients with XLH and one relative.
In advance of the first hybrid in-person–virtual meeting on 5 February 2021, experts were assigned specific topics on which they conducted extensive narrative literature reviews. Topics considered by the group included: pathophysiology of phosphate wasting syndromes; laboratory assessment; burden of XLH disease; management of phosphate wasting syndromes in children and adolescents; management of phosphate wasting syndromes in adults; management of TIO; and the role of dentists and orthopaedic surgeons in the management of patients with phosphate wasting syndromes. At the meeting, the experts presented the results of these reviews, together with draft recommendations, to the wider group, which included patient representatives. During the discussion, the 2019 Evidence-Based Guideline3 was updated with the literature released since its publication. Discussions were held and experts deliberated on the quality, scope and context of the collected evidence, and the recommendations made. Further evidence was incorporated as suggested by members at the meeting. Agreement on statements and recommendations between all co-authors, including the patients, was obtained after extensive discussions, and during critical iterative revisions of the manuscript drafts, leading to consensus on all items. We did not grade the strength of the recommendations.
An executive writing group (A.T., R.R.) was appointed to undertake preparation of the first draft of the manuscript based on draft recommendations as agreed by all participants at the meeting. This draft manuscript was then circulated to all the members of the expert group, and patient representatives, for critical revision. Any additionally identified high-quality evidence published following the expert group meeting was subsequently incorporated by the executive writing group. The first author coordinated the preparation of the final version of the manuscript, which was circulated to the entire expert group for final approval of the content and of the contained recommendations, which had been provisionally approved unanimously at the group meeting. Following the unanimous final endorsement of the recommendations and content by all members of the expert group, the Consensus Statement was submitted for publication. The patient representatives were invited to provide their comments at all steps of the discussions.
Physiology of bone mineralization
Phosphate is involved in a wide variety of essential cellular functions4. For example, phosphate is a constituent of molecules such as ATP, as well as nucleotides in DNA and RNA. Furthermore, phosphate contributes to intracellular signalling molecules, such as cAMP and membranous glycerophospholipids, and signal transduction pathways. Phosphate has an important role as an extracellular fluid (ECF) buffer in blood and urine. Importantly, phosphate is a major constituent of bone and teeth in the form of calcium phosphate crystals (hydroxyapatite)5.
Intestinal absorption of phosphate occurs by passive paracellular and active transcellular vitamin D-dependent mechanisms, with 1,25-dihydroxyvitamin D (1,25(OH)2D or calcitriol) enhancing the expression of sodium-dependent phosphate transport protein 2B6. Renal tubular phosphate reabsorption adapts blood concentrations of phosphate to the needs of the organism in relation to growth, and cartilage and bone mineralization. Indeed, the kidney is able to regulate the maximal reabsorptive capacity, which is expressed as the ratio of maximal TRP to glomerular filtration rate (TmPi/GFR) in the proximal tubule in response to variations in dietary phosphate intake. Concentrations of phosphate in ECF and phosphate homeostasis are regulated by serum PTH along with other mechanisms, with a central role played by FGF23 (refs7,8). Secreted by osteocytes and osteoblasts, FGF23 increases renal phosphate excretion by downregulating the expression of sodium-dependent phosphate transport protein 2A and sodium-dependent phosphate transport protein 2C, and triggering their internalization and degradation in the apical brush border membrane of the proximal tubule7,9,10. FGF23 also directly decreases renal proximal tubule production of 1,25(OH)2D, by suppressing the expression of 25-OHD-1 α-hydroxylase (encoded by CYP27B1). By increasing expression of vitamin D3 24-hydroxylase, FGF23 also catabolizes 25-hydroxy vitamin D (25(OH)D or calcifediol) and 1,25(OH)2D into inactive forms11, which leads to reduced intestinal phosphate and calcium absorption12.
The maintenance of a normal concentration of phosphate in ECF is important for hydroxyapatite crystal formation and the mineralization process. With chronic hypophosphataemia, phosphate availability at the mineralization front is reduced. This deficit is responsible for the development of rickets in children and adolescents, and osteomalacia in adults. Whether 1,25(OH)2D has a role in mineralization that is independent of its effect on intestinal mineral absorption is a matter of debate. Indeed, in experimental models of severely vitamin D-deficient rats, infusion of calcium and phosphate without vitamin D permitted bone growth, cartilage and osteoid mineralization similar to that observed with vitamin D administration alone. This finding supports the view that vitamin D exerts an indirect effect on bone mineralization through maintenance of normal serum levels of calcium and phosphate13,14. Other experimental studies in vitamin D receptor-null mice and in mice with mutations in Cyp27b1 (ref.15) showed that provision of sufficient amounts of calcium and phosphate rescues the rickets phenotype16. Hypophosphataemia leads to rickets by impairing caspase-mediated apoptosis of hypertrophic chondrocytes17. On the other hand, 1,25(OH)2D might directly promote osteoblast differentiation and production of matrix vesicles in vitro, thereby enabling mineralization18,19. Moreover, numerous proteins that promote mineralization are regulated by 1,25(OH)2D (ref.19). A 2020 clinical case report described an infant girl with concomitant hypophosphatasia and vitamin D-deficiency rickets despite normal serum values of calcium and phosphate, which was treated by cholecalciferol (vitamin D3) administration20, consistent with a direct effect of vitamin D on the mineralization process.
Manifestations of phosphate depletion
Disorders with hypophosphataemia have a variety of manifestations that depend upon the underlying pathophysiological mechanism as well as the severity and the duration of phosphate depletion, and whether hypophosphataemia presents during the growth period or in adulthood1. Intracellular phosphate depletion leads to a decrease in red blood cell 2,3-diphosphoglycerate and ATP concentrations; the latter has multiple cellular functions in the central nervous system and in skeletal and smooth muscle cells, and decreased ATP levels in skeletal muscle possibly contribute to proximal myopathy that has been described in hypophosphataemia21. Severe hypophosphataemia can be associated with neuromuscular symptoms and altered cardiac or respiratory function, even though only weak evidence demonstrates a causal relationship1. In hypophosphataemia, the changes that occur at the growth plate and mineralization defects contribute to the skeletal deformities and growth alterations that are the dominant clinical manifestations in childhood. The clinical features of genetic forms of hypophosphataemia manifesting in early life are listed in Box 1. Of note, osteomalacia, which manifests in adults with hypophosphataemia, is a risk factor for pseudofractures2.
Evaluating patients with hypophosphataemia
Age-adjusted references of phosphate values need to be considered when evaluating patients with suspected hypophosphataemia. In addition, serum levels of phosphate exhibit a circadian rhythm, with a peak at around 3.00 a.m. and a nadir at around 11.00 a.m.22. In some rare cases, phosphate assay interference can occur due to the presence of monoclonal immunoglobulin23, medications (such as high-dose liposomal amphotericin B, niacin or excessive use of phosphate binders)24 or hyperbilirubinaemia25, which can result in pseudohypophosphataemia. This interference should be ruled out before any further evaluation.
In children, the maximal TRP can be calculated from fasting blood and urine samples using the formula: TmPi/GFR = plasma phosphate concentration − ((urinary phosphate concentration × plasma creatinine concentration)/urinary creatinine concentration)26,27. Although non-fasting specimens can be sampled, a fasting state usually implies a morning sample collection, ensuring some consistency in the measurements during the phosphate circadian rhythm. An appropriate reference range according to the formula used should be applied.
To evaluate renal tubular phosphate reabsorption in adults, TmPi/GFR is calculated from fasting paired plasma and second morning void urine samples (obtained 2 h after the first void urine) for phosphate and creatinine measurement28. This parameter can be obtained using the nomogram of Walton and Bijvoet28 or using the algorithm of Kenny and Glen29. According to Kenny and Glen, if fractional TRP is less than or equal to 0.86, then TmPi/GFR = TRP × serum phosphate concentration. By contrast, if TRP is greater than 0.86, then TmPi/GFR = α × serum phosphate concentration, where α = 0.3 × TRP/(1 − (0.8 × TRP)). The ratio of maximal TRP to GFR varies with age, and higher values are seen during the accelerated growth period in children than are seen in adults30. Normal values of TmPi/GFR range from 0.8 to 1.35 mmol/l GFR in adults.
Once renal phosphate wasting is demonstrated in children or adults, four important regulating hormones of phosphate metabolism should be evaluated; these are: FGF23, PTH (both phosphaturic factors), 25(OH)D and 1,25(OH)2D, which is the active form of vitamin D. After skin synthesis of vitamin D or ingestion of vitamin D-containing foods or supplements, vitamin D is hydroxylated in the liver to produce 25(OH)D, which is the most abundant vitamin D metabolite. 25(OH)D has a half-life of several weeks and its blood concentration reflects vitamin D status of the individual. A second hydroxylation event occurs on 25(OH)D in the kidneys by 25-OHD-1 α-hydroxylase to produce 1,25(OH)2D. This second hydroxylation is tightly regulated by variations in the circulating levels of PTH and ECF concentrations of calcium or phosphate. Serum concentrations of 1,25(OH)2D can be normal even in individuals with severe vitamin D deficiency. The half-life of 1,25(OH)2D is between 5 and 8 h, depending on the method used to assess it and the study31,32,33. In the past, 1,25(OH)2D was measured by poorly specific radioimmunoassays. Over the past 10 years, automated immunoassays and liquid chromatography tandem mass spectrometry methods have become available, and these offer improved specificity34; however, precision errors remain high according to the Vitamin D External Quality Assessment Scheme external control. Furthermore, no standard reference calibrator nor reference method exists for 1,25(OH)2D measurement35. As is the case for serum levels of phosphate, 1,25(OH)2D levels also vary with age. Values are highest during the first three years of life and then decrease, remaining stable thereafter36,37. Age-specific reference intervals should thus be used. A low or inappropriately normal plasma level of calcitriol in the presence of hypophosphataemia might be suggestive of FGF23 excess.
FGF23 is an endocrine member of the family of fibroblast growth factors and is primarily produced by osteocytes and osteoblasts38. FGF23 is a protein with 251 amino acids; however, a 24-amino acid signal peptide is removed before secretion and the mature secreted FGF23 protein is approximately 32 kDa39. The production of FGF23 is mainly stimulated by 1,25(OH)2D and a high phosphate diet40,41. Many other factors are known to affect FGF23 production, such as PTH, calcium and inflammation. However, the balance between production and degradation by cleavage of the mature FGF23 protein is maintained during inflammation42,43. Mature FGF23 is cleaved by proprotein convertases at the carboxy terminus between amino acids 179 and 180 (ref.44). Of note, mutations that cause loss of function of PHEX result in increased circulating levels of FGF23 and this increase explains many but not all XLH-associated complications45.
FGF23 assays can either detect the intact (full-length) and biologically active form of mature 227-amino acid FGF23, or both the intact protein and C-terminal fragments that result from cleavage. The antibodies used in the assays recognize epitopes within the amino-terminal and C-terminal domains, which flank the cleavage point, or they recognize only the epitopes within the C-terminal portion. These FGF23 assays are generally considered as reliable46. Nine assays recognizing only the ‘intact’ form are commercially available: seven manual enzyme-linked immunosorbent assays (ELISA) and two automated chemiluminescent assays47,48. In addition, three ELISAs that recognize both the intact form and the C-terminal fragments (generally called ‘C-terminal’ assays) are available. Most of these FGF23 assays are for research use only. The various FGF23 assays are described in Supplementary Table 1 (ref.49). The units used for the results of all FGF23 assays differ between the C-terminal (relative units, RU, per millilitre) and the intact methods (picograms per millilitre or picomoles per millilitre). No synthetic or purified natural FGF23 is available for use as a standard method nor a reference method. Of note, FGF23 is more stable in EDTA plasma (plasma with an excess of a powerful chelating agent) than in serum at room temperature. Furthermore, FGF23 values obtained in EDTA plasma are also higher than those obtained in serum47,50. Nevertheless, whether plasma or serum should be used for FGF23 assessment is very assay-specific. Although some assays can be accurate with either plasma or serum, best practice is to use the sample type recommended by the manufacturer.
For initial diagnostic purposes, fasting phosphate and FGF23 plasma samples should be collected 1 to 2 weeks after phosphate and calcitriol discontinuation, if the patient under evaluation is already receiving some treatment. Interestingly, the 2018 approved treatment for XLH (the monoclonal antibody against FGF23, burosumab) can interfere with the FGF23 assay51. A reference range of 22.7 to 93.1 ng/l was established in 908 healthy individuals aged 18 to 89 years for the Diasorin Liaison FGF23 assay47. Of note, individuals older than 60 years and men have slightly higher blood concentrations of FGF23 than younger individuals and women47. For paediatric use, age-dependent and sex-dependent reference range data have been published with the C-terminal FGF23 assay of Immutopics52. However, intact FGF23 measurements are probably more reliable for the diagnosis of FGF23-mediated hypophosphataemia, as they can reveal inappropriately normal levels of intact FGF23, such as those seen in XLH or TIO48,53.
Once elevated or inappropriately normal blood levels of FGF23 are demonstrated in a patient with hypophosphataemia, different possible causes can be considered. Table 1 shows the main differential diagnoses of FGF23-mediated hypophosphataemia.
Evaluation of the patient with hypophosphataemia: recommendations
-
When measuring circulating phosphate levels in a patient with suspected hypophosphataemia, consider assay interference by monoclonal immunoglobulin, medications or hyperbilirubinaemia.
-
Discriminate between renal and non-renal causes of hypophosphataemia by measuring TmPi/GFR.
-
Evaluate the four important hormones that regulate phosphate metabolism; these are FGF23, PTH, 25OHD and 1,25(OH)2D.
-
A low or inappropriately normal plasma level of calcitriol in the presence of hypophosphataemia might be suggestive of FGF23 excess.
-
Detecting inappropriately normal or elevated blood levels of intact FGF23 in a patient with hypophosphataemia using an intact FGF23 assay is compatible with the diagnosis of FGF23-mediated hypophosphataemia.
Genetic causes of FGF23-mediated hypophosphataemia
XLH is due to a loss-of-function pathogenic variant in PHEX, which is located on Xp22.11. PHEX is a membrane protein expressed in bone and teeth tissues54. The precise mechanism by which PHEX mutations lead to FGF23 gene overexpression and/or its decreased catabolism is unknown. With an incidence estimated at 3.9 affected individuals per 100,000 live births55,56, XLH is the most frequent cause of hypophosphataemic rickets of genetic origin (80% of individuals with genetic phosphate wasting syndromes have XLH). The UK prevalence is estimated to be 1.5 patients per 100,000 children and 1.6 patients per 100,000 adults, with an excess mortality57. By contrast, in Norway, XLH prevalence is 1.7 patients per 100,000 children58 and in southern Denmark prevalence is 4.8 patients per 100,000 children55. Such variation in the prevalence (which ranges from 1 in 20,000 to 1 in 60,000) of the disease could be related to selection bias or different genetic backgrounds across populations.
A second inherited form of hypophosphataemia related to FGF23 excess is autosomal dominant hypophosphataemic rickets (ADHR). This condition is caused by pathogenic variants at the cleavage site of FGF23, which precisely target Arg179 and Ser180, thus inducing a resistance to proteolytic degradation in FGF23 (ref.59). The clinical and biochemical phenotype of ADHR seem particularly sensitive to iron deficiency. In normal individuals, iron deficiency stimulates FGF23 transcription but also increases FGF23 cleavage, which results in normal circulating levels of intact FGF23 (ref.60). In ADHR, iron deficiency stimulates production of FGF23 as usual, but it is not efficiently cleaved and thus becomes elevated61,62.
Autosomal recessive hypophosphataemic rickets (ARHR) exists in three forms. First, ARHR type 1 is caused by biallelic variants in DMP1, which encodes an extracellular matrix protein that is important for proper mineralization of bone and dentin63. Second, ARHR type 2 is caused by biallelic variants in ENPP1 (ref.64), which encodes an enzyme involved in the generation of pyrophosphate. Biallelic pathogenic variants in ENPP1 lead to generalized arterial calcification of infancy (GACI). Children who survive GACI can go on to develop ARHR type 2 (ref.65). In one series of 247 adults and children with GACI, 11 initially presented with ARHR type 2. All had ENNP1 pathogenic variants and seven had evidence of ectopic calcifications66. Third, ARHR type 3 is associated with biallelic pathogenic variants that inactivate FAM20C (which encodes a secreted protein kinase that induces posttranslational modification of FGF23 and enhances the processing of FGF23 protein), preventing FGF23 degradation67. Of note, a de novo translocation adjacent to KL (which encodes α-klotho) between chromosomes 9 and 13 has been described, which results in elevated circulating levels of α-klotho and FGF23 (ref.68). The disorder featured hypophosphataemic rickets and severe hyperparathyroidism, with a phenotype characterized by specific facial features and skull anomalies.
Diagnosis of genetic causes of FGF23-mediated hypophosphataemia: recommendations
-
In addition to the main biochemical features, the diagnosis of XLH is based on the clinical evidence of rickets, radiographic signs and when possible, a positive family history (which is seen in 50–70% of patients) with a dominant transmission69,70.
-
Given the difficulties in the differentiation of the multiple possible diagnoses, and given also that the anti-FGF23 antibody, burosumab, is only approved for use in XLH (and in TIO in certain countries), the diagnosis of XLH should be confirmed by genetic analysis of PHEX in children and adults.
-
In case of a negative family history, a panel of other forms of genetic hypophosphataemia should be tested3,69,71. 20–30% of patients with XLH are estimated to have spontaneous disease with no family history69,72.
-
In the absence of a genetic finding or family history, a diagnosis of TIO should be considered (see later text).
Acquired causes of FGF23-mediated hypophosphataemia
Intravenous iron therapy
Administration of ferric carboxymaltose to individuals with iron deficiency is responsible for acquired hypophosphataemia. Other intravenous iron preparations can also induce hypophosphataemia, although less frequently than ferric carboxymaltose. In the setting of iron deficiency, which stimulates FGF23 expression, intravenous iron therapy interferes with the cleavage of FGF23, producing high circulating levels of intact FGF23, and an increased ratio of intact FGF23 to C-terminal FGF23 (refs60,73,74).
Tumour-induced osteomalacia
TIO is a rare acquired disorder mediated by FGF23 that is produced by often benign mesenchymal tumours. This condition has also been observed in several cancers (for example, prostate and breast)75,76. The biochemical features of TIO are similar to those of XLH, with hypophosphataemia, low TmPi/GFR, low or inappropriately normal circulating levels of 1,25(OH)2D, and high or inappropriately normal circulating levels of FGF23 (ref.77). However, clinical features such as dental complications, enthesopathy or osteoarthritis are less commonly found in TIO than in XLH. This difference might be due to the development of the disorder during adulthood and/or a short disease duration78. Although XLH can be associated with increased BMD in certain patients, BMD is typically low in TIO79, with an important deterioration in bone microarchitecture80. The tumours in TIO are usually small, with slow growth and can be located anywhere in the body. Once the diagnosis is established, identifying the location of the tumour might be difficult despite a multitude of sophisticated imaging modalities currently available (for example, PET–CT with 68Ga-DOTATATE or fluorodeoxyglucose). These examinations can be followed up with targeted venous sampling to determine if suspect lesions found on imaging are secreting FGF23 (ref.81). Effort should be made to find the tumour, with repeated scans at annual or 2-year intervals, as complete surgical tumour resection is curative and leads to a spectacular clinical improvement and increases in BMD79. When tumour resection is not possible, due to an inability to locate or access the tumour, medical treatment and management are similar to those in XLH. Among new therapeutic procedures, image-guided tumour ablation82 and the anti-FGF23 monoclonal antibody burosumab have shown promising results83.
Diversity of XLH clinical manifestations
XLH has clinical manifestations that affect many different organs and tissues. Box 2 summarizes pathophysiological changes and clinical implications by organ in XLH. In a 2019 survey that involved 232 adults and 90 children with XLH84, bowing of the femur was reported in 63% and bowing of the tibia was reported in 72% of children. A similar prevalence was found in adults. Of note, 47% of children and 94% of adults reported surgical interventions, most commonly osteotomy, followed by epiphysiodesis. History of fracture or pseudofractures was reported in 44% of adults. In a meta-analysis, 18% to 52% of adult patients with XLH experienced fractures or pseudofractures85. Despite conventional treatment with phosphate supplements and vitamin D metabolites during childhood, 57% reported a history of orthopaedic surgery. Another study showed an unexpected reduction in survival in adult patients with XLH57.
In some children with XLH, craniosynostosis results from premature fusion of the cranial sutures during growth86,87. The pathophysiology of this complication has not been fully elucidated but might involve an upregulation of FGF receptor 2 (FGFR2) or FGFR3 signalling and cross-binding of FGF23 with FGFR2 and FGFR3, which affects intramembranous and endochondral ossification of the skull88. Patients with XLH can also have a disproportionately short stature3, which does not correct even with treatment from birth onwards and despite correction of leg deformities.
Besides the clinical and radiological evidence of rickets that is present in a large proportion of patients with XLH, muscle weakness has been reported in 30% of children and 60% of adults84. Compared to an age-matched and sex-matched population, affected individuals display normal muscle volume, but a lower muscle density and lower muscle strength and power89. The reasons for muscle weakness are unknown and might be linked with hypophosphataemia and deficient energy delivery to the muscle by decreased muscle ATP synthesis, as well as with limb deformities and deconditioning. This manifestation will require further efforts to be completely understood90.
Early osteoarthritis and enthesopathy (calcification of the tendons and ligaments in close proximity to bone) can limit the mobility of patients with XLH and cause pain. In one study in adult patients with XLH (aged >30 years), 80% of patients had early osteoarthritis and 100% of patients had enthesopathy91, which explains the high proportion of individuals with XLH who live with pain. Enthesopathy and spinal stenosis are common (affecting 27% and 19% of adults with XLH, respectively), as are dental abscesses, which affect 51% of children and 82% of adults with XLH. Nearly all adults with XLH experienced pain in another study84. The mechanism of enthesophyte development is poorly understood and might result from a direct effect of FGF23 (refs92,93). Conventional therapy does not notably influence enthesopathy94,95. The bowing of the long bones might potentially increase strain on the entheses. The mechanisms underlying early osteoarthritis development are not completely understood and cannot be fully explained by abnormal mechanical loading due to skeletal deformities. However, the mechanisms through which increased FGF23 might interfere with cartilage development require further investigation96.
Among extra-skeletal manifestations, neurological manifestations also occur due to spinal stenosis or type I Chiari malformation (defined as brain tissue that extends into the cervical spinal canal)97. Clinically important spinal canal stenosis and spinal cord or nerve compression are the consequence of ossification of the posterior longitudinal ligament in conjunction with hypertrophy of the facet joints, thickening of the laminae and calcification of the ligamenta flava98,99. Of note, hearing loss has been reported in 16% to 76% of individuals with XLH2,100,101,102. However, the mechanism is unclear103.
Nephrocalcinosis has not been reported in untreated patients with XLH but is considered an adverse effect of conventional treatment (particularly phosphate supplements) and occurs through treatment-related development of hypercalciuria, hyperphosphaturia and/or secondary hyperparathyroidism104. FGF23 has also been suggested to enhance renal calcium reabsorption via the transient receptor potential cation channel subfamily V member 5 (TRPV5) channel in the distal tubule, which could potentially promote cellular calcium accumulation and calcification, as does PTH105,106,107. The frequency of nephrocalcinosis is highly variable and ranges from 30% to 70% in patients with XLH3. Nephrocalcinosis might be associated with hypertension and left ventricular hypertrophy105. In patients with XLH, FGF23 might also have a direct effect on cardiomyocytes and vessels, as is seen in chronic renal failure; however, circulating levels of FGF23 in XLH are well below those encountered in renal failure, making a myocardial direct toxic effect less likely108.
Some limited data exist supporting the view that patients with XLH might be prone to develop early-onset hypertension and display a higher prevalence of hypertension as compared with the general population. For example, 27% of adult patients with XLH were found to be affected by hypertension in a previous study105. In patients with XLH, hypertension seems to be associated with the presence of secondary or tertiary hyperparathyroidism, nephrocalcinosis and/or reduced GFR109. FGF23-induced renal sodium reabsorption could have a role in this phenomenon106. Children and adults with XLH also have a high prevalence of obesity, partly due to impaired mobility in relation to chronic bone complications102,110. Obesity substantially reduces gait quality in children with XLH111. In addition, some patients with XLH also experience glycosuria, which could confuse the clinical diagnosis and might lead clinicians to suspect a Fanconi-type syndrome rather than FGF23-mediated hypophosphataemia112,113,114,115.
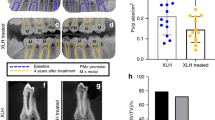
Of note, the earlier that appropriate treatment is initiated in childhood, the lower the severity of clinical symptoms and consequences observed in adulthood116,117,118. Moreover, adults with XLH display specific symptoms related to early development of osteoarthritis, osteomalacia with pseudofractures, impaired muscle function, chronic bone and joint pain, stiffness, impaired mobility and disability, depression119 and early susceptibility to dental abscesses. All these manifestations negatively affect the patient’s quality of life120 (Box 3; Figs 1,2).
Radiographic images in a 16-year-old girl with X-linked hypophosphataemia (XLH)-associated rickets. The patient had sporadic disease with a confirmed PHEX pathogenic variant. Conventional therapy (oral phosphate supplements and calcitriol) was started in the second year of life. a | Severe and complex multi-apical varus deformity and maltorsion. b | Bilateral deformity correction and body height increase (9.5 cm) was achieved by performing multiple osteotomies and stabilization with external fixators (a Taylor Spatial Frame). c | Last follow-up at age 25 years (5 years after the last surgical procedure) with high patient satisfaction, high daily activity, no joint or muscle pains and excellent limb alignment. This patient illustrates the severity of bone deformities in XLH and the clinical efficacy of orthopaedic surgery in conjunction with conventional therapy. Image courtesy of C. Radler, Orthopaedic Hospital Speising, Vienna.
Radiographic images in a 48-year-old man with X-linked hypophosphataemia (XLH)-associated rickets that manifested with short stature, bowing of the limbs and recurrent abscesses during childhood. Phosphate supplements and active vitamin D metabolites were administered until the age of 18 years. The patient had important varus deformities of the tibias and underwent corrective surgical procedures: the first operation was a bilateral tibial osteotomy at age 20 years and a second operation was performed on the right side at age 22 years. The osteotomy site on the right fibula did not consolidate until the age of 25. a | At the age of 43 years, in the context of diffuse pain, X-ray evaluation showed multiple pseudofractures located on the left femur, and right and left tibias, with important deformations. b | Conventional treatment was started, which was associated with rapid improvement in the pain and progressive healing of the pseudofractures. c | At the age of 48 years, he developed symptomatic spinal cord compression at the level of thoracic vertebra 7 and thoracic vertebra 8 due to enthesopathy affecting the ligamentum flavum. He underwent a posterior decompression at the levels of compression sites (arrows indicate compression).
Management of XLH
Conventional treatment
During growth, conventional treatment with phosphate supplements and active vitamin D metabolites can be offered to all children with XLH, as soon as the diagnosis is established. The dose should be adapted to the severity of the phenotype, with starting doses ranging from 20 mg/kg to 60 mg/kg body weight per day (0.7–2.0 mmol/kg) of elemental phosphate2 in four to six divided doses. Calcitriol should be given at a starting dose of 20–30 ng/kg body weight per day in one or two doses. Owing to a longer half-life than calcitriol, alfacalcidol can be given once daily at an initial dose of 30–50 ng/kg per day. A more aggressive approach has been suggested that uses high calcitriol doses of up to 40 ng/kg per day2, or even short-term higher doses as a loading dose, which might help in preventing hyperparathyroidism but could also result in an increased risk of nephrocalcinosis121. Less frequent dosing with phosphate or vitamin D metabolites can be considered when serum levels of alkaline phosphatase (ALP) are in the normal range, in order to improve adherence in adolescents. Of note, reference ranges for ALP are both age-specific and sex-specific. Vitamin D deficiency should also be corrected to prevent the development of secondary hyperparathyroidism, which can worsen renal phosphate wasting.
In children, the clinical efficacy of conventional treatment is well established, in terms of improved growth and reduced severity of leg deformities, decreased occurrence of dental complications and pain control122,123,124,125,126,127,128. As serum phosphate is measured under fasting conditions and given the short half-life of phosphate supplements (serum levels of phosphate return to baseline concentrations within 1.5 h after intake129), fasting phosphate values might be lower than in a post-absorptive state. Thus, conventional treatment usually fails to normalize serum levels of phosphate, and to target the normalization of serum levels of phosphate is not a suitable goal. The goal of treatment is to prevent or cure rickets2,116. Importantly, overtreating with phosphate supplements should be avoided owing to the risk of nephrocalcinosis and of secondary hyperparathyroidism.
In adults, the considerable variety of phenotypes of XLH can substantially influence the appropriate treatment. Furthermore, the condition is rarely misdiagnosed as ankylosing spondylitis, early osteoarthritis or Forestier disease. In 2021, a middle-aged man was reported as being misdiagnosed with achondroplasia all through childhood and adulthood owing to his short stature and deformed extremities130.
Long-term treatment with phosphate supplements131 and decreased production of calcitriol by FGF23 excess contribute to the development of hyperparathyroidism. Adults with XLH are particularly prone to developing secondary and eventually tertiary hyperparathyroidism with hypercalcaemia, which affected 25% and 10% of patients with XLH respectively, in one study132. If available, paricalcitol could be added to conventional therapy for PTH suppression. Paricalcitol was tested in a randomized trial in patients with XLH without prevalent hypercalcaemia133. Tertiary hyperparathyroidism should primarily be treated by parathyroid surgery132. If there are contraindications to surgery or if the patient declines this intervention, the calcimimetic cinacalcet could be considered134,135.
The continuation of conventional treatment in adults is still debated. In a cohort of 52 adults with XLH, continuation of conventional treatment during adulthood tended to prevent dental abscess136, and to reduce periodontitis frequency and severity137. However, conventional treatment in adults does not seem to affect the course of enthesopathy136. By contrast, in Hyp mice (a model of human XLH), conventional treatment did not improve enthesopathy95 or exacerbated the mineralization of enthesis138. Neither hearing loss nor osteoarthritis seem to be influenced by conventional treatment3. Evidence, mostly obtained from case reports, suggests the efficacy of conventional treatment on bone pain related to osteomalacia, pseudofractures and fracture healing2,139. However, robust evidence that asymptomatic adults should be treated is still missing. Transient treatment regimens can be considered in those undergoing orthopaedic or dental surgery to promote bone mineralization and the healing process. If so, treatment should be started before and continued 3–6 months after the surgical intervention2. When growth is completed, the dose of oral phosphate must be progressively decreased down to the lowest dose consistent with relief of symptoms. The doses of alfacalcidol or calcitriol should be adjusted to the required dose of phosphate to ensure normal mineral metabolism, as reflected by normal serum levels of ALP, PTH and calcium, without signs of nephrocalcinosis. In some instances, low-dose active vitamin D analogues might be sufficient to achieve normal mineral metabolism and symptom relief without additional phosphate supplements.
During pregnancy, the need for phosphate increases, particularly during the third trimester, with an active maternal–fetal transport by the placenta. For those patients not receiving any treatment before pregnancy, conventional treatment could be considered and continued until the end of breastfeeding. Neonates born from mothers with XLH do not display skeletal abnormalities at birth91 but preliminary findings suggest that they might have a birthweight slightly lower than normal (A. Linglart, unpublished work). In summary, we suggest that clinicians consider monitoring mineral metabolism in pregnant and lactating women and administering conventional XLH treatment if needed. Genetic testing of PHEX should be performed in the newborn baby. Given the time needed to get the results of such testing, we recommend screening the newborn baby at 7 days and, if the first survey is normal, 1 month after birth with the following parameters: plasma creatinine, ALP, PTH, 25OHD and phosphate, and urinary phosphate and creatinine. These parameters can be used to calculate the TmPi/GFR, as this ratio and the serum levels of phosphate might remain in the lower normal range during the first months of life. Genetic testing is not absolutely necessary when there is a well-known family history and biochemical findings consistent with XLH. Also, in some settings, genetic testing is not available or is prohibitively expensive. Conversely, targeted genetic testing can be done fairly rapidly and inexpensively when the pathogenic variant in the relative is already known.
Adverse effects of conventional treatment
Adverse effects of conventional treatment include intestinal discomfort due to phosphate supplements, with nausea, diarrhoea, hypercalciuria and nephrocalcinosis reported in 30% to 70% of patients3. Excessive oral phosphate intake might also promote nephrocalcinosis140. Secondary and tertiary hyperparathyroidism due to long-standing stimulation of parathyroid glands by phosphate supplements and further suppression of 1,25(OH)2D production by FGF23 might also be seen in patients with XLH141.
Conventional treatment in children: recommendations
-
Vitamin D analogues and phosphate supplements can be offered to all children with XLH, as soon as the diagnosis is established.
-
Starting doses of elemental phosphate range from 20 to 60 mg/kg body weight per day (0.7–2.0 mmol/kg)2 in four to six divided doses, according to the severity of the disease.
-
Calcitriol should be given at a starting dose of 20–30 ng/kg body weight per day, in one or two doses, or alfacalcidol once daily at an initial dose of 30–50 ng/kg per day.
Conventional treatment in adults: recommendations
-
Treatment in adults should include: vitamin D analogues (alfacalcidol 0–1.5 μg per day, once per day, or calcitriol 0–1.0 μg per day, in one or two doses) alone or with phosphate supplements (ideally smaller doses (than in children), which are evenly distributed across the day, 0–2,000 mg per day).
-
Management of bone pain might be required in adults with XLH owing to osteomalacia, fractures or pseudofractures.
-
In adults with XLH, clinicians should evaluate the need for orthopaedic surgery or the presence of dental complications.
-
We suggest considering treatment with vitamin D analogues and phosphate supplements during pregnancy and breastfeeding. No data, to our knowledge, are available regarding the effect of therapy in postmenopausal women. Consistent evidence is still missing for treating enthesopathies.
-
We do not recommend treatment of asymptomatic adult patients, unless they develop pseudofractures, even without symptoms.
Growth hormone treatment in children
Not enough evidence is available to recommend routine treatment with recombinant human growth hormone in short children with XLH142.
Rehabilitation
Specific programmes of regular physical exercises and physiotherapy should be followed by individuals with XLH to prevent or improve muscle weakness, back pain, joint pain and stiffness, and to increase mobility143. Physiotherapy should promote muscle strength, improve balance, joint motion and general mobility, by resistance exercise training in combination with other muscle function therapy3. Leisure sport activities are recommended. Specific and tailored programme rehabilitation is often necessary after orthopaedic surgery and in those with enthesopathy or osteoarthritis3.
Burosumab treatment in children
Conventional treatment counteracts two consequences of high circulating levels of FGF23, which are hypophosphataemia and low circulating levels of 1,25(OH)2D; however, conventional treatment does not fully correct the XLH phenotype due to the PHEX pathogenic variant. Furthermore, conventional therapy increases the circulating levels of FGF23 and PTH, potentially exacerbating hypophosphataemia. Thus, a logical treatment approach is to use burosumab, a recombinant, monoclonal IgG antibody against FGF23. It is recommended that health-care providers consider burosumab treatment in children with XLH aged 1 year or older (or from 6 months, as approved in some countries, such as the USA) and in adolescents with radiographic evidence of bone disease. The indications that were recommended in the 2019 guidelines3 are overt bone disease (active rickets on plain radiography) and disease that is refractory to conventional therapy, the presence of associated complications such as pseudofractures and an inability to adhere to conventional treatment.
The superiority of burosumab over conventional treatment has been shown in terms of serum phosphate control144,145, healing of rachitic bone and/or of mineralization defects, improvements in bowing of legs, improved physical ability (as measured by walking distance in the 6-min walking test) and pain control. Burosumab can also be considered as first-line therapy in children with XLH. Of note, patients included in the comparative trial were severely affected and might not have represented the full spectrum of disease severity encountered in daily practice. In addition, patients with secondary hyperparathyroidism were excluded. The effect of burosumab on longitudinal growth in children during treatment periods of up to 64 weeks was rather small (about +0.2 s.d. score), which suggests the existence of additional pathogenic factors; for example, a PHEX mutation-related osteoblast defect that impairs growth in children with XLH145. Whether burosumab confers advantages in mildly affected individuals remains to be seen. Long-term studies are also needed to evaluate the effect of this therapy on the clinical burden of XLH, such as bone deformities, dental complications and the number of surgical interventions. Thus, in children with mild disease who are easily managed with conventional therapy, treatment with burosumab is probably not warranted because of the large annual cost of the drug (around US $200,000). In this population, a trial of conventional therapy is indicated rather than considering burosumab as first-line therapy at present. As all the studies evaluated children aged 1–12 years144,145, in some countries, the use of burosumab is limited to children in this age range. We consider this position highly questionable and recommend continuing treatment until end of growth.
The starting dose of burosumab in children with XLH is 0.8 mg/kg every 2 weeks subcutaneously, and this dose is adjusted to bring fasting serum levels of phosphate within the lower end of the normal reference range for age (maximum dose 2 mg/kg per 14 days or 90 mg per 14 days). As the peak serum concentration of burosumab is reached by 7 to 11 days after injection, serum levels of phosphate should ideally be measured during that period to determine whether the treatment is causing hyperphosphataemia and between days 12 and 14 to demonstrate treatment efficacy3. The level that serum phosphate should increase to influence bone healing is currently unclear.
Burosumab treatment in children: recommendations
-
Consider burosumab treatment as first-line therapy in children with XLH aged 1 year or older (6 months in some countries, such as the USA), and in adolescents with radiographic evidence of severe bone disease.
-
In children with mild disease, a trial of conventional therapy is suggested rather than considering burosumab as a first-line therapy.
-
Once started, treatment with burosumab should be continued until the closure of the growth plate. A multidisciplinary evaluation should be conducted with the adult team to consider the follow-up of burosumab through adulthood.
Burosumab treatment in adults
In adults with XLH, when burosumab was administered subcutaneously every 4 weeks at a starting dose of 1 mg/kg rounded to the nearest 10 mg, the treatment was shown to normalize the serum levels of phosphate to above the lower limit of the normal range in most patients studied. Clinically, the Western Ontario and McMaster Universities Arthritis Index stiffness subscale score was improved, as was the Worst Pain Score and Physical Function sub-score of the SF-36 quality of life questionnaire146,147,148,149,150. In a randomized double-blind placebo-controlled study, burosumab treatment in adults with XLH resulted in improved fracture healing (overt fractures and pseudofractures) at week 24 compared with placebo, and this improvement continued up to 48 weeks151. Treatment was also associated with improvement in histomorphometric features of mineralization defects150.
Adverse effects of burosumab treatment
Burosumab treatment is well tolerated, with minor injection-site reactions, pain in the extremities, fever, rash, myalgia and headaches reported144. In adults, restless legs syndrome (11.8%) was more frequently observed in the treated group than in the placebo group (7.6%)149.
Burosumab treatment in adults: recommendations
-
Burosumab could be suggested as a second-line therapy in adults with XLH with overt osteomalacia, with pseudofractures that are not responding to conventional treatment or in patients intolerant to conventional treatment.
Follow-up of patients with XLH
Follow-up of both treated and untreated patients with XLH is an important aspect of management. A multidisciplinary team should be involved in the follow-up, and the examination and evaluation of the patient should be done at regular intervals (Boxes 4,5). In addition, clearly identified pathways should exist for health-care access in case of urgent clinical queries from both the patient and the patient’s local health-care team. This access is best facilitated by a nominated clinician or a clinical specialist nurse.
The recommended clinical follow-up in children is shown in Boxes 4 and 5. As bone-specific ALP represents 90% of total circulating ALP in children, total ALP is a suitable biochemical parameter for the evaluation of rickets activity. In addition, the circulating levels of 25OHD and PTH should be followed, as vitamin D deficiency is frequent in these patients. Together with phosphate supplementation, vitamin D deficiency can stimulate secondary hyperparathyroidism. Of note, the use of active vitamin D metabolites is contraindicated in patients on burosumab treatment. The use of active vitamin D metabolites as part of conventional therapy is associated with the risk of hypercalcaemia and hypercalciuria; therefore, patients need to be monitored closely to identify these biochemical abnormalities.
Severity of rickets can be assessed with plain radiography examination of the wrist and/or knees. Systematic plain radiography is not recommended, but it should be done in children who are not responding to therapy, such as those with worsening of bone deformities despite medical treatment. Use of low-dose radiography (such as the EOS imaging system used in a standing position) might be an option to limit radiation exposure. Other recommendations for monitoring are listed in Boxes 4 and 5.
Multidisciplinary approach
Genetic counselling
XLH is transmitted in an X-linked dominant manner. With each pregnancy, an affected woman has a 50% chance of passing the pathogenic PHEX variant to her child. Mosaicism could affect the expected transmission of the gene and rare instances of mosaicism in XLH have altered the expected transmission pattern152. An affected man passes the pathogenic variant to all of his daughters and to none of his sons. Offspring who receive the pathogenic variant will be affected; however, the severity of the phenotype cannot be firmly predicted because of large intrafamilial variations3. Prenatal testing for a pregnancy at increased risk can be considered if the PHEX pathogenic variant has been detected in the family153. In that case, as discussed above, targeted genetic testing can be done easily and inexpensively when the pathogenic variant in the relative is already known. Molecular genetic testing might include a single gene, such as PHEX sequencing, or a panel of several genes causing genetic forms of hypophosphataemia (Table 1). If a pathogenic variant is not detected, further assessment can include gene-targeted deletion or duplication analysis. For XLH, genetic diagnosis is established or confirmed by demonstrating a hemizygous PHEX pathogenic variant in an individual with XY chromosomes and a heterozygous PHEX pathogenic variant in an individual with XX chromosomes.
Genetic counselling: recommendations
-
Genetic counselling is recommended for patients who have been diagnosed with XLH, to understand the risk of transmission. Genetic testing during pregnancy can be performed if the patient so wishes.
-
Testing for XLH in newborn babies of families affected by XLH should also be done to properly diagnose the condition, as early as possible. Delayed diagnosis or misdiagnosis can result in delayed or no treatment and consequently in poor patient outcome.
Oral heath
Oral health is altered in patients with XLH. The disease impairs mineralization of the dentin and cementum154 and also of the alveolar bone155. The most frequently reported complications are ‘spontaneous’ dental necrosis with severe abscesses that occur in deciduous or permanent teeth, with no history of trauma or decay. These episodes can evolve to maxillofacial cellulitis. The risk of periodontitis is also increased in adults with XLH, even in young adults, due to alterations of the periodontal tissues155, which favours early tooth loss137.
Regarding dental features, enamel looks normal but is slightly thinner in patients with XLH and wears out more rapidly than sound enamel in healthy individuals, and displays microscopic cracks. The most affected tissue in XLH is the dentin. Radiographic dental images from patients with XLH show low mineral density and enlarged pulp chambers. A characteristic sign is prominent pulp horns that extend to the dental enamel junction117,156. Microscopically the dentin shows large unmineralized spaces with unmerged mineralization foci157. In these unmineralized spaces, peptides derived from small integrin-binding ligand N-linked glycoproteins (known as SIBLINGs) accumulate, such as C-terminal acidic serine-rich and aspartate-rich motif (ASARM) peptides derived from matrix extracellular phosphoglycoprotein (MEPE) and osteopontin abnormal cleavage, which are strong inhibitors of biomineralization156,158,159,160,161. Taken together, these dental features explain the increased susceptibility of patients with XLH to spontaneous necrosis and abscesses, whose origin is difficult to diagnose by medical practitioners and dentists not familiar with this disorder.
As stressed before, the earlier that conventional treatment is started in individuals with XLH during the growth period and in adulthood, the lower the incidence of dental abscesses117 and periodontitis137. This effect occurs through an improvement in dentin and cementum mineralization as shown in observational studies117,137. The effects of burosumab on dental abnormalities are rather disappointing, with a phase III comparative study in children with XLH showing more events such as spontaneous dental necrosis in the burosumab arm than with conventional treatment145. A longer period of follow-up than carried out in this study might be required to observe a positive outcome on dentin and cementum mineralization. Overall, the quality of life of patients with XLH is strongly affected by dental events162,163.
Oral health: recommendations
-
Patients with XLH require specific and regular dental examination (at least yearly) and appropriate care to prevent infections and early tooth loss, as well as aesthetic and functional damage, by a dental team with expertise in XLH3.
Orthopaedic intervention
Regular paediatric orthopaedic assessment during the growth period is recommended in patients with XLH3. If surgery is needed, the orthopaedic surgeon can define the surgical plan and technique through a careful clinical examination, analysis of the deformities with full-length anteroposterior and lateral radiographs (hip to ankle) of both lower limbs in the standing position (with a calibration ball) and MRI. The type of orthopaedic management depends on the age of the patient and the type of deformity. Braces for deformity prevention with guidance of growth are no longer used in XLH because convincing evidence of efficacy is lacking164. The surgical options in XLH include guided growth, osteotomies, complex deformity corrections, internal fixation and stabilization of pseudofractures, as well as joint replacement. Guided growth or temporary hemi-epiphysiodesis are used to correct coronal deformity (valgus or varus). A small plate is fixed on the medial or lateral distal femur or proximal tibia that blocks the open growth plate. After successful correction, the plate is removed. This procedure is effective in children and adolescents, minimally invasive and has a low rate of complications165. The procedure has been tested in patients with XLH164,166,167,168 with success and could decrease the need of osteotomies. A limitation of this technique is that it needs growth potential. Furthermore, this technique corrects only the frontal deformity and cannot correct rotation or sagittal and diaphyseal bending of bone. A risk of recurrence is also present169.
Osteotomies are another option enabling 3D correction of complex deformities. Subsequent stabilization can be performed both using internal devices as well as external fixators. Osteotomies are required when epiphyses are closed and guided surgery is no longer possible or in patients with complex deformities. Finally, arthroplasties of the hip and knee joints are possible in patients with XLH; however, these procedures require at times the simultaneous use of corrective osteotomies and special implants in patients with severe deformities170,171.
Disease-specific gait deviations have been analysed in children and adults with XLH111,172,173; however, they require further evaluation, as many patients with XLH report abnormal gait84. Of note, any orthopaedic surgery should be considered only in patients with XLH who are undergoing medical treatment that corrects the underlying metabolic abnormalities, otherwise there is a notable risk of recurrence or failure of surgery. Patients who are considered for orthopaedic surgery should be referred to counselling services to prepare for and develop coping strategies for undertaking major surgery.
Symptomatic spinal cord compression due to spinal stenosis can be severe in patients with XLH and can occur at multiple levels. This complication might require neurosurgical posterior decompression and long-term follow-up98. Chiari malformations in children with XLH can progress in adulthood and lead to severe occipitocervical headache and a variety of respiratory symptoms, and are related to sudden unexpected death.
Patient organizations and research
Patients with XLH should be informed about the potential help and additional information that can be provided by patient organizations, and should be asked to contact them if needed. This information is particularly important for the patient at the time the diagnosis is received. These organizations and patient representatives can share practical information about living with the condition, and the usefulness and adverse effects of medications, and suggest support strategies for special needs. Sharing of information and educational materials, and provision of counselling or psychosocial support, are also critical for the parents of children with XLH or the partners of affected adult patients. For parents of a child with XLH, caring for the affected child can be extremely daunting and isolating, given the rarity of the disease and the lack of support networks and information available. For spouses or partners, the disease raises fundamental questions, including uncertainties about pregnancy and the risk and impact to both the mother and the child. Establishing patient networks and ensuring access to services including genetic counselling, psychologists and counsellors, are critical in the interdisciplinary approach.
In certain parts of the world, centres of expertise can have connections with patient representatives and patient organizations. These representatives and organizations contribute to the planning, functioning and evaluation of these centres174. However, such centres can be absent in other parts of the world where misdiagnoses are still common, access to treatment is not readily available and support networks are scarce, if not non-existent.
National guidelines issued from XLH centres of expertise should integrate and reflect patient preferences. In most clinical studies, treatment efficacy is evaluated through measurement of surrogate outcomes, such as serum levels of phosphate. However, how these surrogate outcomes relate to clinical benefits is unclear. Direct measures of patients’ perceptions and feelings should be complementary to the evaluation of treatment effectiveness. Although disease-specific measures of patient-related outcome (PRO) are not available in XLH, concept-specific instruments measuring pain, fatigue and physical function, for example, can be used — for example, the Patient-Reported Outcomes Measurement Information System measures175. Patient representatives and patient organizations are crucial in developing and establishing such measures. Such an instrument was used in a phase III clinical study of children with XLH and showed that burosumab improved PRO measures as compared with conventional treatment175. Finally, given the rarity of XLH, patients should be offered information about local, regional, national and international studies they might be eligible for.
Family members
As mentioned above, parents, legal guardians and/or family members have a critical role in supporting patients with XLH, even in those affected with only a mild form of the disease. It is paramount that they are also supported when caring for patients with XLH and have adequate access to information about the disease. This access is especially important given the rarity of this disease. For parents, especially those with XLH themselves, the burden starts even before the child is born. Having children can raise fundamental questions about the rate or risk of transmission, testing during pregnancy and treatment once the child is born. It also poses questions for the parents themselves; for example, to know if there are any known risks in pregnancy for women with XLH (beyond the ‘usual’ risks associated with pregnancy). Parents should be made aware of the physical, psychological, social and emotional effects of the disease, to support their child and to be able to cope themselves. The same goes for spouses, partners and other family members.
Conclusions
Given the diversity of symptoms and complications in XLH, an interdisciplinary approach is of paramount importance, with special mention paid to dental, orthopaedic, and psychological and emotional care. Multidisciplinary follow-up of patients with XLH is mandatory and should be coordinated by a metabolic bone disease specialist. Paediatric and adult patients should be evaluated twice-yearly by a dentist, and paediatric patients should be followed up yearly by a paediatric orthopaedic surgeon specialized in XLH. Follow-up can involve dieticians, physiotherapists, occupational therapists, social workers and psychologists. Physiotherapy and occupational therapy can be helpful after surgery or to treat musculoskeletal symptoms such as stiffness, muscular weakness and disability. A dietician can help in the prevention and treatment of obesity, which is highly prevalent in patients with XLH102,110. Patients should be referred to XLH patient organizations and patient representatives for information and genetic counselling. The information they provide is particularly important when patients receive the diagnosis and at critical moments later in life (for example, when considering major life choices such as pregnancy). Interaction between patients, who can share their experiences, is important and could ensure optimal adherence to follow-up and therapy and thereby a successful outcome. Some important unanswered questions remain to be explored in the area of the understanding of the pathogenesis of some complications of XLH or the effects of treatment (Box 6).
References
Imel, E. A. & Econs, M. J. Approach to the hypophosphatemic patient. J. Clin. Endocrinol. Metab. 97, 696–706 (2012).
Carpenter, T. O., Imel, E. A., Holm, I. A., Jan de Beur, S. M. & Insogna, K. L. A clinician’s guide to X-linked hypophosphatemia. J. Bone Miner. Res. 26, 1381–1388 (2011).
Haffner, D. et al. Clinical practice recommendations for the diagnosis and management of X-linked hypophosphataemia. Nat. Rev. Nephrol. 15, 435–455 (2019).
Rizzoli, R. & Bonjour, J. P. in Dynamics of Bone and Cartilage Metabolism 2nd edn (eds Seibel, M. J., Robins S. P. & Bilezikian J. P.) 345–360 (Academic Press, 2006).
Arnold, A. et al. Hormonal regulation of biomineralization. Nat. Rev. Endocrinol. 17, 261–275 (2021).
Xu, H., Bai, L., Collins, J. F. & Ghishan, F. K. Age-dependent regulation of rat intestinal type IIb sodium-phosphate cotransporter by 1,25-(OH)(2) vitamin D(3). Am. J. Physiol. Cell Physiol. 282, C487–C493 (2002).
Shimada, T. et al. FGF-23 is a potent regulator of vitamin D metabolism and phosphate homeostasis. J. Bone Miner. Res. 19, 429–435 (2004).
Feng, J. Q. et al. Loss of DMP1 causes rickets and osteomalacia and identifies a role for osteocytes in mineral metabolism. Nat. Genet. 38, 1310–1315 (2006).
Liu, S. et al. Regulation of fibroblastic growth factor 23 expression but not degradation by PHEX. J. Biol. Chem. 278, 37419–37426 (2003).
Baum, M., Schiavi, S., Dwarakanath, V. & Quigley, R. Effect of fibroblast growth factor-23 on phosphate transport in proximal tubules. Kidney Int. 68, 1148–1153 (2005).
Chanakul, A. et al. FGF-23 regulates CYP27B1 transcription in the kidney and in extra-renal tissues. PLoS ONE 8, e72816 (2013).
Christakos, S. et al. Vitamin D and the intestine: review and update. J. Steroid Biochem. Mol. Biol. 196, 105501 (2020).
Underwood, J. L. & DeLuca, H. F. Vitamin D is not directly necessary for bone growth and mineralization. Am. J. Physiol. 246, E493–E498 (1984).
Lieben, L. et al. Normocalcemia is maintained in mice under conditions of calcium malabsorption by vitamin D-induced inhibition of bone mineralization. J. Clin. Invest. 122, 1803–1815 (2012).
Dardenne, O., Prud’homme, J., Hacking, S. A., Glorieux, F. H. & St-Arnaud, R. Correction of the abnormal mineral ion homeostasis with a high-calcium, high-phosphorus, high-lactose diet rescues the PDDR phenotype of mice deficient for the 25-hydroxyvitamin D-1α-hydroxylase (CYP27B1). Bone 32, 332–340 (2003).
Amling, M. et al. Rescue of the skeletal phenotype of vitamin D receptor-ablated mice in the setting of normal mineral ion homeostasis: formal histomorphometric and biomechanical analyses. Endocrinology 140, 4982–4987 (1999).
Sabbagh, Y., Carpenter, T. O. & Demay, M. B. Hypophosphatemia leads to rickets by impairing caspase-mediated apoptosis of hypertrophic chondrocytes. Proc. Natl Acad. Sci. USA 102, 9637–9642 (2005).
Woeckel, V. J. et al. 1α,25-(OH)2D3 acts in the early phase of osteoblast differentiation to enhance mineralization via accelerated production of mature matrix vesicles. J. Cell Physiol. 225, 593–600 (2010).
Goltzman, D. Functions of vitamin D in bone. Histochem. Cell Biol. 149, 305–312 (2018).
Lin, E. L. et al. Healing of vitamin D deficiency rickets complicating hypophosphatasia suggests a role beyond circulating mineral sufficiency for vitamin D in musculoskeletal health. Bone 136, 115322 (2020).
Ravid, M. & Robson, M. Proximal myopathy caused by latrogenic phosphate depletion. JAMA 236, 1380–1381 (1976).
Portale, A. A., Halloran, B. P. & Morris, R. C. Jr Dietary intake of phosphorus modulates the circadian rhythm in serum concentration of phosphorus. Implications for the renal production of 1,25-dihydroxyvitamin D. J. Clin. Invest. 80, 1147–1154 (1987).
Kerr, S., Kindt, J. & Daram, S. R. Hypophosphatemia associated with paraproteinemia: a case report and review of the literature. WMJ 106, 490–493 (2007).
Mays, J. A., Greene, D. N., Poon, A. & Merrill, A. E. Pseudohypophosphatemia associated with high-dose liposomal amphotericin B therapy. Clin. Biochem. 50, 967–971 (2017).
Duncanson, G. O. & Worth, H. G. Pseudohypophosphataemia as a result of bilirubin interference. Ann. Clin. Biochem. 27, 253–257 (1990).
Alon, U. & Hellerstein, S. Assessment and interpretation of the tubular threshold for phosphate in infants and children. Pediatr. Nephrol. 8, 250–251 (1994).
Brodehl, J., Krause, A. & Hoyer, P. F. Assessment of maximal tubular phosphate reabsorption: comparison of direct measurement with the nomogram of Bijvoet. Pediatr. Nephrol. 2, 183–189 (1988).
Walton, R. J. & Bijvoet, O. L. Nomogram for derivation of renal threshold phosphate concentration. Lancet 2, 309–310 (1975).
Kenny, A. P. & Glen, A. C. Tests of phosphate reabsorption. Lancet 2, 158 (1973).
Bistarakis, L., Voskaki, I., Lambadaridis, J., Sereti, H. & Sbyrakis, S. Renal handling of phosphate in the first six months of life. Arch. Dis. Child. 61, 677–681 (1986).
Seeman, E. et al. Production, degradation, and circulating levels of 1,25-dihydroxyvitamin D in health and in chronic glucocorticoid excess. J. Clin. Invest. 66, 664–669 (1980).
Cianferotti, L. et al. The clinical use of vitamin D metabolites and their potential developments: a position statement from the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO) and the International Osteoporosis Foundation (IOF). Endocrine 50, 12–26 (2015).
Makris, K., Sempos, C. & Cavalier, E. The measurement of vitamin D metabolites part II–the measurement of the various vitamin D metabolites. Hormones 19, 97–107 (2020).
Makris, K. et al. Recommendations on the measurement and the clinical use of vitamin D metabolites and vitamin D binding protein – a position paper from the IFCC Committee on Bone Metabolism. Clin. Chim. Acta 517, 171–197 (2021).
Herrmann, M., Farrell, C. L., Pusceddu, I., Fabregat-Cabello, N. & Cavalier, E. Assessment of vitamin D status–a changing landscape. Clin. Chem. Lab. Med. 55, 3–26 (2017).
Souberbielle, J. C. et al. Serum calcitriol concentrations measured with a new direct automated assay in a large population of adult healthy subjects and in various clinical situations. Clin. Chim. Acta 451, 149–153 (2015).
Higgins, V. et al. Pediatric reference intervals for 1,25-dihydroxyvitamin D using the DiaSorin LIAISON XL assay in the healthy CALIPER cohort. Clin. Chem. Lab. Med. 56, 964–972 (2018).
Yoshiko, Y. et al. Mineralized tissue cells are a principal source of FGF23. Bone 40, 1565–1573 (2007).
Liu, S. & Quarles, L. D. How fibroblast growth factor 23 works. J. Am. Soc. Nephrol. 18, 1637–1647 (2007).
Ferrari, S. L., Bonjour, J. P. & Rizzoli, R. Fibroblast growth factor-23 relationship to dietary phosphate and renal phosphate handling in healthy young men. J. Clin. Endocrinol. Metab. 90, 1519–1524 (2005).
Saito, H. et al. Circulating FGF-23 is regulated by 1α,25-dihydroxyvitamin D3 and phosphorus in vivo. J. Biol. Chem. 280, 2543–2549 (2005).
Gohil, A. & Imel, E. A. FGF23 and associated disorders of phosphate wasting. Pediatr. Endocrinol. Rev. 17, 17–34 (2019).
Edmonston, D. & Wolf, M. FGF23 at the crossroads of phosphate, iron economy and erythropoiesis. Nat. Rev. Nephrol. 16, 7–19 (2020).
Benet-Pages, A. et al. FGF23 is processed by proprotein convertases but not by PHEX. Bone 35, 455–462 (2004).
Liu, S. et al. Pathogenic role of Fgf23 in Hyp mice. Am. J. Physiol. Endocrinol. Metab. 291, E38–E49 (2006).
Heijboer, A. C. et al. Determination of fibroblast growth factor 23. Ann. Clin. Biochem. 46, 338–340 (2009).
Souberbielle, J. C. et al. Evaluation of a new fully automated assay for plasma intact FGF23. Calcif. Tissue Int. 101, 510–518 (2017).
Ito, N. et al. Clinical performance of a novel chemiluminescent enzyme immunoassay for FGF23. J. Bone Miner. Metab. 39, 1066–1075 (2021).
Donate-Correa, J., Muros de Fuentes, M., Mora-Fernandez, C. & Navarro-Gonzalez, J. F. Pathophysiological implications of fibroblast growth factor-23 and Klotho and their potential role as clinical biomarkers. Clin. Chem. 60, 933–940 (2014).
El-Maouche, D. et al. Stability and degradation of fibroblast growth factor 23 (FGF23): the effect of time and temperature and assay type. Osteoporos. Int. 27, 2345–2353 (2016).
Piketty, M. L. et al. FGF23 measurement in burosumab-treated patients: an emerging treatment may induce a new analytical interference. Clin. Chem. Lab. Med. 58, e267–e269 (2020).
Fischer, D. C. et al. Paediatric reference values for the C-terminal fragment of fibroblast-growth factor-23, sclerostin, bone-specific alkaline phosphatase and isoform 5b of tartrate-resistant acid phosphatase. Ann. Clin. Biochem. 49, 546–553 (2012).
Endo, I. et al. Clinical usefulness of measurement of fibroblast growth factor 23 (FGF23) in hypophosphatemic patients: proposal of diagnostic criteria using FGF23 measurement. Bone 42, 1235–1239 (2008).
Beck, L. et al. Pex/PEX tissue distribution and evidence for a deletion in the 3′ region of the Pex gene in X-linked hypophosphatemic mice. J. Clin. Invest. 99, 1200–1209 (1997).
Beck-Nielsen, S. S., Brock-Jacobsen, B., Gram, J., Brixen, K. & Jensen, T. K. Incidence and prevalence of nutritional and hereditary rickets in southern Denmark. Eur. J. Endocrinol. 160, 491–497 (2009).
Endo, I. et al. Nationwide survey of fibroblast growth factor 23 (FGF23)-related hypophosphatemic diseases in Japan: prevalence, biochemical data and treatment. Endocr. J. 62, 811–816 (2015).
Hawley, S. et al. Prevalence and mortality of individuals with X-linked hypophosphatemia: a United Kingdom real-world data analysis. J. Clin. Endocrinol. Metab. 105, e871–e878 (2020).
Rafaelsen, S., Johansson, S., Raeder, H. & Bjerknes, R. Hereditary hypophosphatemia in Norway: a retrospective population-based study of genotypes, phenotypes, and treatment complications. Eur. J. Endocrinol. 174, 125–136 (2016).
Liu, C. et al. Earlier onset in autosomal dominant hypophosphatemic rickets of R179 than R176 mutations in fibroblast growth factor 23: report of 20 Chinese cases and review of the literature. Calcif. Tissue Int. 105, 476–486 (2019).
Wolf, M., Koch, T. A. & Bregman, D. B. Effects of iron deficiency anemia and its treatment on fibroblast growth factor 23 and phosphate homeostasis in women. J. Bone Miner. Res. 28, 1793–1803 (2013).
Imel, E. A. et al. Iron modifies plasma FGF23 differently in autosomal dominant hypophosphatemic rickets and healthy humans. J. Clin. Endocrinol. Metab. 96, 3541–3549 (2011).
Imel, E. A., Gray, A. K., Padgett, L. R. & Econs, M. J. Iron and fibroblast growth factor 23 in X-linked hypophosphatemia. Bone 60, 87–92 (2014).
Lorenz-Depiereux, B. et al. DMP1 mutations in autosomal recessive hypophosphatemia implicate a bone matrix protein in the regulation of phosphate homeostasis. Nat. Genet. 38, 1248–1250 (2006).
Levy-Litan, V. et al. Autosomal-recessive hypophosphatemic rickets is associated with an inactivation mutation in the ENPP1 gene. Am. J. Hum. Genet. 86, 273–278 (2010).
Kotwal, A. et al. Clinical and biochemical phenotypes in a family with ENPP1 mutations. J. Bone Miner. Res. 35, 662–670 (2020).
Ferreira, C. R. et al. Ectopic calcification and hypophosphatemic rickets: natural history of ENPP1 and ABCC6 deficiencies. J. Bone Miner. Res. 36, 2193–2202 (2021).
Rafaelsen, S. H. et al. Exome sequencing reveals FAM20c mutations associated with fibroblast growth factor 23-related hypophosphatemia, dental anomalies, and ectopic calcification. J. Bone Miner. Res. 28, 1378–1385 (2013).
Brownstein, C. A. et al. A translocation causing increased α-Klotho level results in hypophosphatemic rickets and hyperparathyroidism. Proc. Natl Acad. Sci. USA 105, 3455–3460 (2008).
Gaucher, C. et al. PHEX analysis in 118 pedigrees reveals new genetic clues in hypophosphatemic rickets. Hum. Genet. 125, 401–411 (2009).
Whyte, M. P., Schranck, F. W. & Armamento-Villareal, R. X-linked hypophosphatemia: a search for gender, race, anticipation, or parent of origin effects on disease expression in children. J. Clin. Endocrinol. Metab. 81, 4075–4080 (1996).
Thiele, S., Werner, R., Stubbe, A., Hiort, O. & Hoeppner, W. Validation of a next-generation sequencing (NGS) panel to improve the diagnosis of X-linked hypophosphataemia (XLH) and other genetic disorders of renal phosphate wasting. Eur. J. Endocrinol. 183, 497–504 (2020).
Beck-Nielsen, S. S., Brixen, K., Gram, J. & Brusgaard, K. Mutational analysis of PHEX, FGF23, DMP1, SLC34A3 and CLCN5 in patients with hypophosphatemic rickets. J. Hum. Genet. 57, 453–458 (2012).
Wolf, M. et al. Effects of iron isomaltoside vs ferric carboxymaltose on hypophosphatemia in iron-deficiency anemia: two randomized clinical trials. JAMA 323, 432–443 (2020).
Kalantar-Zadeh, K. et al. Parenteral iron therapy and phosphorus homeostasis: a review. Am. J. Hematol. 96, 606–616 (2021).
Minisola, F. et al. Mineral metabolism abnormalities in patients with prostate cancer: a systematic case controlled study. Endocrine 59, 338–343 (2018).
Savva, C., Adhikaree, J., Madhusudan, S. & Chokkalingam, K. Oncogenic osteomalacia and metastatic breast cancer: a case report and review of the literature. J. Diabetes Metab. Disord. 18, 267–272 (2019).
Abrahamsen, B., Smith, C. D. & Minisola, S. Epidemiology of tumor-induced osteomalacia in Denmark. Calcif. Tissue Int. 109, 147–156 (2021).
Jiajue, R. et al. Early discrimination between tumor-induced rickets/osteomalacia and X-linked hypophosphatemia in Chinese children and adolescents: a retrospective case-control study. J. Bone Miner. Res. 36, 1739–1748 (2021).
Colangelo, L. et al. Long-term bone mineral density changes after surgical cure of patients with tumor-induced osteomalacia. Osteoporos. Int. 31, 1383–1387 (2020).
Zanchetta, M. B. et al. Impaired bone microarchitecture and strength in patients with tumor-induced osteomalacia. J. Bone Miner. Res. 36, 1502–1509 (2021).
Takeuchi, Y. et al. Venous sampling for fibroblast growth factor-23 confirms preoperative diagnosis of tumor-induced osteomalacia. J. Clin. Endocrinol. Metab. 89, 3979–3982 (2004).
Hesse, E., Rosenthal, H. & Bastian, L. Radiofrequency ablation of a tumor causing oncogenic osteomalacia. N. Engl. J. Med. 357, 422–424 (2007).
Jan de Beur, S. M. et al. Burosumab for the treatment of tumor-induced osteomalacia. J. Bone Miner. Res. 36, 627–635 (2021).
Skrinar, A. et al. The lifelong impact of X-linked hypophosphatemia: results from a burden of disease survey. J. Endocr. Soc. 3, 1321–1334 (2019).
Seefried, L., Smyth, M., Keen, R. & Harvengt, P. Burden of disease associated with X-linked hypophosphataemia in adults: a systematic literature review. Osteoporos. Int. 32, 7–22 (2021).
Imerslund, O. Craniostenosis and vitamin D resistant rickets. Acta Paediatr. 40, 449–456 (1951).
Vega, R. A. et al. Hypophosphatemic rickets and craniosynostosis: a multicenter case series. J. Neurosurg. Pediatr. 17, 694–700 (2016).
Murthy, A. S. X-linked hypophosphatemic rickets and craniosynostosis. J. Craniofac. Surg. 20, 439–442 (2009).
Veilleux, L. N., Cheung, M., Ben Amor, M. & Rauch, F. Abnormalities in muscle density and muscle function in hypophosphatemic rickets. J. Clin. Endocrinol. Metab. 97, E1492–E1498 (2012).
Schubert, L. & DeLuca, H. F. Hypophosphatemia is responsible for skeletal muscle weakness of vitamin D deficiency. Arch. Biochem. Biophys. 500, 157–161 (2010).
Reid, I. R. et al. X-linked hypophosphatemia: a clinical, biochemical, and histopathologic assessment of morbidity in adults. Medicine 68, 336–352 (1989).
Liang, G., Katz, L. D., Insogna, K. L., Carpenter, T. O. & Macica, C. M. Survey of the enthesopathy of X-linked hypophosphatemia and its characterization in Hyp mice. Calcif. Tissue Int. 85, 235–246 (2009).
Faraji-Bellee, C. A. et al. Development of enthesopathies and joint structural damage in a murine model of X-linked hypophosphatemia. Front. Cell Dev. Biol. 8, 854 (2020).
Econs, M. J. Conventional therapy in adults with XLH improves dental manifestations, but not enthesopathy. J. Clin. Endocrinol. Metab. 100, 3622–3624 (2015).
Cauliez, A. et al. Impact of early conventional treatment on adult bone and joints in a murine model of X-linked hypophosphatemia. Front. Cell Dev. Biol. 8, 591417 (2020).
Orfanidou, T., Iliopoulos, D., Malizos, K. N. & Tsezou, A. Involvement of SOX-9 and FGF-23 in RUNX-2 regulation in osteoarthritic chondrocytes. J. Cell Mol. Med. 13, 3186–3194 (2009).
Rothenbuhler, A. et al. High incidence of cranial synostosis and Chiari I malformation in children with X-linked hypophosphatemic rickets (XLHR). J. Bone Miner. Res. 34, 490–496 (2019).
Riccio, A. R. et al. Minimally invasive surgical management of thoracic ossification of the ligamentum flavum associated with X-linked hypophosphatemia. World Neurosurg. 94, 580.e5–580.e10 (2016).
Chesher, D. et al. Outcome of adult patients with X-linked hypophosphatemia caused by PHEX gene mutations. J. Inherit. Metab. Dis. 41, 865–876 (2018).
Meister, M., Johnson, A., Popelka, G. R., Kim, G. S. & Whyte, M. P. Audiologic findings in young patients with hypophosphatemic bone disease. Ann. Otol. Rhinol. Laryngol. 95, 415–420 (1986).
Davies, M., Kane, R. & Valentine, J. Impaired hearing in X-linked hypophosphataemic (vitamin-D-resistant) osteomalacia. Ann. Intern. Med. 100, 230–232 (1984).
Beck-Nielsen, S. S. et al. Phenotype presentation of hypophosphatemic rickets in adults. Calcif. Tissue Int. 87, 108–119 (2010).
Beck-Nielsen, S. S. et al. FGF23 and its role in X-linked hypophosphatemia-related morbidity. Orphanet J. Rare Dis. 14, 58 (2019).
Patzer, L. et al. Urinary supersaturation of calcium oxalate and phosphate in patients with X-linked hypophosphatemic rickets and in healthy schoolchildren. J. Pediatr. 135, 611–617 (1999).
Nakamura, Y., Takagi, M., Takeda, R., Miyai, K. & Hasegawa, Y. Hypertension is a characteristic complication of X-linked hypophosphatemia. Endocr. J. 64, 283–289 (2017).
Andrukhova, O. et al. FGF23 regulates renal sodium handling and blood pressure. EMBO Mol. Med. 6, 744–759 (2014).
Mitchell, D. M., Juppner, H. & Burnett-Bowie, S. M. FGF23 is not associated with age-related changes in phosphate, but enhances renal calcium reabsorption in girls. J. Clin. Endocrinol. Metab. 102, 1151–1160 (2017).
Schnedl, C., Fahrleitner-Pammer, A., Pietschmann, P. & Amrein, K. FGF23 in acute and chronic illness. Dis. Markers 2015, 358086 (2015).
Alon, U. S. et al. Hypertension in hypophosphatemic rickets–role of secondary hyperparathyroidism. Pediatr. Nephrol. 18, 155–158 (2003).
Zhukouskaya, V. V. et al. Increased prevalence of overweight and obesity in children with X-linked hypophosphatemia. Endocr. Connect. 9, 144–153 (2020).
Mindler, G. T. et al. Disease-specific gait deviations in pediatric patients with X-linked hypophosphatemia. Gait Posture 81, 78–84 (2020).
Muhlbauer, R. C. & Fleisch, H. Abnormal renal glucose handling in X-linked hypophosphataemic mice. Clin. Sci. 80, 71–76 (1991).
Rasmussen, H. & Anast, C. in The Metabolic Basis of Inherited Disease 5th edn (eds Stanbury, J. B., Wyngaarden, J. B., Goldstein, J.L. & Brown, M. S.) 1743–1773 (McGraw Hill, 1983).
Dent, C. E. & Harris, H. Hereditary forms of rickets and osteomalacia. J. Bone Jt. Surg. Br. 38-B, 204–226 (1956).
Freeman, S. & Dunsky, I. Resistant rickets. Am. J. Dis. Child. 79, 409–427 (1950).
Linglart, A. et al. Therapeutic management of hypophosphatemic rickets from infancy to adulthood. Endocr. Connect. 3, R13–R30 (2014).
Chaussain-Miller, C. et al. Dental abnormalities in patients with familial hypophosphatemic vitamin D-resistant rickets: prevention by early treatment with 1-hydroxyvitamin D. J. Pediatr. 142, 324–331 (2003).
Makitie, O. et al. Early treatment improves growth and biochemical and radiographic outcome in X-linked hypophosphatemic rickets. J. Clin. Endocrinol. Metab. 88, 3591–3597 (2003).
Hawley, S. et al. Higher prevalence of non-skeletal comorbidity related to X-linked hypophosphataemia: a UK parallel cohort study using CPRD. Rheumatology 60, 4055–4062 (2021).
Che, H. et al. Impaired quality of life in adults with X-linked hypophosphatemia and skeletal symptoms. Eur. J. Endocrinol. 174, 325–333 (2016).
Imel, E. A. & Carpenter, T. O. A practical clinical approach to paediatric phosphate disorders. Endocr. Dev. 28, 134–161 (2015).
Verge, C. F. et al. Effects of therapy in X-linked hypophosphatemic rickets. N. Engl. J. Med. 325, 1843–1848 (1991).
Sochett, E. et al. Growth and metabolic control during puberty in girls with X-linked hypophosphataemic rickets. Horm. Res. 61, 252–256 (2004).
Quinlan, C. et al. Growth in PHEX-associated X-linked hypophosphatemic rickets: the importance of early treatment. Pediatr. Nephrol. 27, 581–588 (2012).
Balsan, S. & Tieder, M. Linear growth in patients with hypophosphatemic vitamin D-resistant rickets: influence of treatment regimen and parental height. J. Pediatr. 116, 365–371 (1990).
Costa, T. et al. X-linked hypophosphatemia: effect of calcitriol on renal handling of phosphate, serum phosphate, and bone mineralization. J. Clin. Endocrinol. Metab. 52, 463–472 (1981).
Harrell, R. M., Lyles, K. W., Harrelson, J. M., Friedman, N. E. & Drezner, M. K. Healing of bone disease in X-linked hypophosphatemic rickets/osteomalacia. Induction and maintenance with phosphorus and calcitriol. J. Clin. Invest. 75, 1858–1868 (1985).
Glorieux, F. H., Marie, P. J., Pettifor, J. M. & Delvin, E. E. Bone response to phosphate salts, ergocalciferol, and calcitriol in hypophosphatemic vitamin D-resistant rickets. N. Engl. J. Med. 303, 1023–1031 (1980).
Bettinelli, A., Bianchi, M. L., Mazzucchi, E., Gandolini, G. & Appiani, A. C. Acute effects of calcitriol and phosphate salts on mineral metabolism in children with hypophosphatemic rickets. J. Pediatr. 118, 372–376 (1991).
Chin, Y. A. et al. Delayed diagnosis, difficult decisions: novel gene deletion causing X-linked hypophosphatemia in a middle-aged man with achondroplastic features and tertiary hyperparathyroidism. Case Rep. Endocrinol. 2021, 9944552 (2021).
Makitie, O., Kooh, S. W. & Sochett, E. Prolonged high-dose phosphate treatment: a risk factor for tertiary hyperparathyroidism in X-linked hypophosphatemic rickets. Clin. Endocrinol. 58, 163–168 (2003).
Lecoq, A. L. et al. Hyperparathyroidism in patients with X-linked hypophosphatemia. J. Bone Miner. Res. 35, 1263–1273 (2020).
Carpenter, T. O. et al. Effect of paricalcitol on circulating parathyroid hormone in X-linked hypophosphatemia: a randomized, double-blind, placebo-controlled study. J. Clin. Endocrinol. Metab. 99, 3103–3111 (2014).
Neal, M. D., Deslouches, B. & Ogilvie, J. The use of pre-operative imaging and intraoperative parathyroid hormone level to guide surgical management of tertiary hyperparathyroidism from X-linked hypophosphatemic rickets: a case report. Case J. 2, 7572 (2009).
Alon, U. S. et al. Calcimimetics as an adjuvant treatment for familial hypophosphatemic rickets. Clin. J. Am. Soc. Nephrol. 3, 658–664 (2008).
Connor, J. et al. Conventional therapy in adults with X-linked hypophosphatemia: effects on enthesopathy and dental disease. J. Clin. Endocrinol. Metab. 100, 3625–3632 (2015).
Biosse Duplan, M. et al. Phosphate and vitamin D prevent periodontitis in X-linked hypophosphatemia. J. Dent. Res. 96, 388–395 (2017).
Karaplis, A. C., Bai, X., Falet, J. P. & Macica, C. M. Mineralizing enthesopathy is a common feature of renal phosphate-wasting disorders attributed to FGF23 and is exacerbated by standard therapy in Hyp mice. Endocrinology 153, 5906–5917 (2012).
Sullivan, W., Carpenter, T., Glorieux, F., Travers, R. & Insogna, K. A prospective trial of phosphate and 1,25-dihydroxyvitamin D3 therapy in symptomatic adults with X-linked hypophosphatemic rickets. J. Clin. Endocrinol. Metab. 75, 879–885 (1992).
Goodyer, P. R., Kronick, J. B., Jequier, S., Reade, T. M. & Scriver, C. R. Nephrocalcinosis and its relationship to treatment of hereditary rickets. J. Pediatr. 111, 700–704 (1987).
Alon, U., Lovell, H. B. & Donaldson, D. L. Nephrocalcinosis, hyperparathyroidism, and renal failure in familial hypophosphatemic rickets. Clin. Pediatr. 31, 180–183 (1992).
Smith, S. & Remmington, T. Recombinant growth hormone therapy for X-linked hypophosphatemia in children. Cochrane Database Syst. Rev. 10, CD004447 (2021).
Laurent, M. R. et al. Consensus recommendations for the diagnosis and management of X-linked hypophosphatemia in Belgium. Front. Endocrinol. 12, 641543 (2021).
Carpenter, T. O. et al. Burosumab therapy in children with X-linked hypophosphatemia. N. Engl. J. Med. 378, 1987–1998 (2018).
Imel, E. A. et al. Burosumab versus conventional therapy in children with X-linked hypophosphataemia: a randomised, active-controlled, open-label, phase 3 trial. Lancet 393, 2416–2427 (2019).
Carpenter, T. O. et al. Randomized trial of the anti-FGF23 antibody KRN23 in X-linked hypophosphatemia. J. Clin. Invest. 124, 1587–1597 (2014).
Imel, E. A. et al. Prolonged correction of serum phosphorus in adults with X-linked hypophosphatemia using monthly doses of KRN23. J. Clin. Endocrinol. Metab. 100, 2565–2573 (2015).
Ruppe, M. D. et al. Effect of four monthly doses of a human monoclonal anti-FGF23 antibody (KRN23) on quality of life in X-linked hypophosphatemia. Bone Rep. 5, 158–162 (2016).
Insogna, K. L. et al. A randomized, double-blind, placebo-controlled, phase 3 trial evaluating the efficacy of burosumab, an anti-FGF23 antibody, in adults with X-linked hypophosphatemia: week 24 primary analysis. J. Bone Miner. Res. 33, 1383–1393 (2018).
Insogna, K. L. et al. Burosumab improved histomorphometric measures of osteomalacia in adults with X-linked hypophosphatemia: a phase 3, single-arm, international trial. J. Bone Miner. Res. 34, 2183–2191 (2019).
Portale, A. A. et al. Continued beneficial effects of burosumab in adults with X-linked hypophosphatemia: results from a 24-week treatment continuation period after a 24-week double-blind placebo-controlled period. Calcif. Tissue Int. 105, 271–284 (2019).
Goji, K., Ozaki, K., Sadewa, A. H., Nishio, H. & Matsuo, M. Somatic and germline mosaicism for a mutation of the PHEX gene can lead to genetic transmission of X-linked hypophosphatemic rickets that mimics an autosomal dominant trait. J. Clin. Endocrinol. Metab. 91, 365–370 (2006).
Ruppe, M. D. X-Linked Hypophosphatemia. GeneReviews https://www.ncbi.nlm.nih.gov/books/NBK83985/ (2017).
Opsahl Vital, S. et al. Tooth dentin defects reflect genetic disorders affecting bone mineralization. Bone 50, 989–997 (2012).
Coyac, B. R. et al. Tissue-specific mineralization defects in the periodontium of the Hyp mouse model of X-linked hypophosphatemia. Bone 103, 334–346 (2017).
Boukpessi, T. et al. Dentin alteration of deciduous teeth in human hypophosphatemic rickets. Calcif. Tissue Int. 79, 294–300 (2006).
Murayama, T., Iwatsubo, R., Akiyama, S., Amano, A. & Morisaki, I. Familial hypophosphatemic vitamin D-resistant rickets: dental findings and histologic study of teeth. Oral. Surg. Oral. Med. Oral. Pathol. Oral. Radiol. Endod. 90, 310–316 (2000).
Gaucher, C. et al. Dentin noncollagenous matrix proteins in familial hypophosphatemic rickets. Cell Tissues Organs 189, 219–223 (2009).
Boukpessi, T. et al. Abnormal presence of the matrix extracellular phosphoglycoprotein-derived acidic serine- and aspartate-rich motif peptide in human hypophosphatemic dentin. Am. J. Pathol. 177, 803–812 (2010).
Boukpessi, T. et al. Osteopontin and the dento-osseous pathobiology of X-linked hypophosphatemia. Bone 95, 151–161 (2017).
Barros, N. M. et al. Proteolytic processing of osteopontin by PHEX and accumulation of osteopontin fragments in Hyp mouse bone, the murine model of X-linked hypophosphatemia. J. Bone Miner. Res. 28, 688–699 (2013).
Gjorup, H., Beck-Nielsen, S. S., Hald, J. D. & Haubek, D. Oral health-related quality of life in X-linked hypophosphataemia and osteogenesis imperfecta. J. Oral. Rehabil. 48, 160–168 (2021).
Hanisch, M., Bohner, L., Sabandal, M. M. I., Kleinheinz, J. & Jung, S. Oral symptoms and oral health-related quality of life of individuals with x-linked hypophosphatemia. Head. Face Med. 15, 8 (2019).
Novais, E. & Stevens, P. M. Hypophosphatemic rickets: the role of hemiepiphysiodesis. J. Pediatr. Orthop. 26, 238–244 (2006).
Danino, B. et al. Guided growth: preliminary results of a multinational study of 967 physes in 537 patients. J. Child. Orthop. 12, 91–96 (2018).
Stevens, P. M. & Klatt, J. B. Guided growth for pathological physes: radiographic improvement during realignment. J. Pediatr. Orthop. 28, 632–639 (2008).
Sharkey, M. S., Grunseich, K. & Carpenter, T. O. Contemporary medical and surgical management of X-linked hypophosphatemic rickets. J. Am. Acad. Orthop. Surg. 23, 433–442 (2015).
Horn, A., Wright, J., Bockenhauer, D., Van’t Hoff, W. & Eastwood, D. M. The orthopaedic management of lower limb deformity in hypophosphataemic rickets. J. Child. Orthop. 11, 298–305 (2017).
Masquijo, J. J., Firth, G. B. & Sepulveda, D. Failure of tension band plating: a case series. J. Pediatr. Orthop. B 26, 449–453 (2017).
Larson, A. N. et al. Hip and knee arthroplasty in hypophosphatemic rickets. J. Arthroplast. 25, 1099–1103 (2010).
Mills, E. S., Iorio, L., Feinn, R. S., Duignan, K. M. & Macica, C. M. Joint replacement in X-linked hypophosphatemia. J. Orthop. 16, 55–60 (2019).
Steele, A. et al. Osteoarthritis, osteophytes, and enthesophytes affect biomechanical function in adults with X-linked hypophosphatemia. J. Clin. Endocrinol. Metab. 105, e1798–e1814 (2020).
Mindler, G. T. et al. Lower limb deformity and gait deviations among adolescents and adults with X-linked hypophosphatemia. Front. Endocrinol. 12, 754084 (2021).
Ammann, P. Patient involvement in centres of expertise for rare diseases. ProRaris https://www.proraris.ch/data/documents/Teilbericht_PIinCentresofExpertiseforRD_September2016_final.pdf (2016).
Padidela, R. et al. Patient-reported outcomes from a randomized, active-controlled, open-label, phase 3 trial of burosumab versus conventional therapy in children with X-linked hypophosphatemia. Calcif. Tissue Int. 108, 622–633 (2021).
Acknowledgements
The Working Group was entirely funded by the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis and Musculoskeletal Diseases (ESCEO). ESCEO received unrestricted educational grants to support its educational and scientific activities from non-governmental organizations, not-for-profit organizations, and non-commercial and corporate partners. The choice of topics, participants, content and agenda of the Working Groups, as well as the writing, editing, submission and reviewing of the manuscript are under the sole responsibility of ESCEO, without any influence from third parties. We thank A. Banerjee, Y. Sumi and R. Sadana (Department of Ageing and Life Course, World Health Organization, Geneva, Switzerland) for their participation and support of the working group meeting.
Author information
Authors and Affiliations
Contributions
A.T. and R.R. contributed to all aspects of the article. E.C., C. Chaussain, D.H., N.C.H., A. Linglart, G.T.M., S.M. and L.S. researched data for the article, contributed substantially to the discussion of content, and reviewed and/or edited the manuscript before submission. N.A.-D., M.L.B., J.B.C.-A., M.C., L.C., C. Cooper, P.H., M.K.J., F.J., J.A.K., A. Laslop, M.R.L., A.M., M.C.P.Y., M.M.R., M.V. and M.B.Z. contributed substantially to the discussion of content, and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
A.T. has received fees for consulting from VIFOR. M.L.B. has received honoraria, consultancy and lecture fees and/or research grants from Abiogen, Alexion, Amgen, Amolyt, Bruno Farmaceutici, Calcilytix, Echolight, Eli Lilly, Kyowa Kirin, Servier, SPA, Theramex and UCB. E.C. is a consultant for DiaSorin, Fujirebio, IDS and Nittobo. C. Cooper has received lecture fees and consulting honoraria from Amgen, MSD, Eli Lilly, Procter & Gamble, Aventis, GSK/Roche, Novartis, Nycomed, Radius, Servier and Wyeth Pharmaceuticals. D.H. has received consultancy and lecture fees and/or research grants from Amgen, Chiesi and Kyowa Kirin. P.H. is an employee of GSK, but in that capacity has no financial interest in any project associated with the topic of this article. N.C.H. has received consultancy, lecture fees and honoraria from Alliance for Better Bone Health, AMGEN, MSD, Eli Lilly, Servier, UCS, Shire, Consilient Healthcare, Kyowa Kirin and Internis Pharma. M.K.J. has received grants and honoraria from Kyowa Kirin. M.R.L. has received consultancy and lecture fees from Alexion, Amgen, Kyowa Kirin, Menarini, Orifarm, Sandoz, Takeda, UCB and Will Pharma. A. Linglart has received lecture fees and/or research grants from NovoNordisk, Pfizer, Merck, Alexion and Kyowa Kirin. S.M. served as speaker for Abiogen, Amgen, Bruno Farmaceutici, Diasorin, Eli Lilly, Shire, Sandoz and Takeda, and on the advisory board of Abiogen, Kyowa Kirin, Pfizer and UCB. L.S. has received honoraria for lectures and advice from Abbvie, Amgen, Alexion, GSK, Kyowa Kirin, Eli Lilly, MSD, Novartis, Servier, Theramex and UCB, and research grants from Alexion, KyowaKirin and Novartis. M.B.Z. has received consultancy fees and lecture fees from Amgen, Eli Lilly and Ultragenyx. R.R. has received fees for lectures or advisory boards from Abiogen, Amgen, Danone, Echolight, European Milk Forum, Mithra, Nestlé, ObsEva, Pfizer Consumer Health, Radius Health, Rejunevate and Theramex. The remaining authors declare no competing interests.
Peer review
Peer review information
Nature Reviews Endocrinology thanks Thomas Carpenter, S. Fukomoto and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Trombetti, A., Al-Daghri, N., Brandi, M.L. et al. Interdisciplinary management of FGF23-related phosphate wasting syndromes: a Consensus Statement on the evaluation, diagnosis and care of patients with X-linked hypophosphataemia. Nat Rev Endocrinol 18, 366–384 (2022). https://doi.org/10.1038/s41574-022-00662-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41574-022-00662-x
This article is cited by
-
XLH Matters 2022: Insights and recommendations to improve outcomes for people living with X-linked hypophosphataemia (XLH)
Orphanet Journal of Rare Diseases (2023)
-
Dental impact of anti-fibroblast growth factor 23 therapy in X-linked hypophosphatemia
International Journal of Oral Science (2023)
-
Latin-American consensus on the transition into adult life of patients with X-linked hypophosphatemia
Endocrine (2023)
-
Dissociation of clinical, laboratory, and bone biopsy findings in adult X-linked hypophosphatemia: a case report
Wiener Medizinische Wochenschrift (2023)
-
Growth pattern in children with X-linked hypophosphatemia treated with burosumab and growth hormone
Orphanet Journal of Rare Diseases (2022)