Abstract
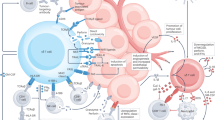
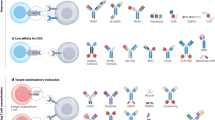
Clinical responses to checkpoint inhibitors used for cancer immunotherapy seemingly require the presence of αβT cells that recognize tumour neoantigens, and are therefore primarily restricted to tumours with high mutational load. Approaches that could address this limitation by engineering αβT cells, such as chimeric antigen receptor T (CAR T) cells, are being investigated intensively, but these approaches have other issues, such as a scarcity of appropriate targets for CAR T cells in solid tumours. Consequently, there is renewed interest among translational researchers and commercial partners in the therapeutic use of γδT cells and their receptors. Overall, γδT cells display potent cytotoxicity, which usually does not depend on tumour-associated (neo)antigens, towards a large array of haematological and solid tumours, while preserving normal tissues. However, the precise mechanisms of tumour-specific γδT cells, as well as the mechanisms for self-recognition, remain poorly understood. In this Review, we discuss the challenges and opportunities for the clinical implementation of cancer immunotherapies based on γδT cells and their receptors.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Chien, Y. H., Meyer, C. & Bonneville, M. Gammadelta T cells: first line of defense and beyond. Annu. Rev. Immunol. 32, 121–155 (2014).
Girardi, M. et al. Regulation of cutaneous malignancy by γδ T cells. Science 294, 605–609 (2001).
Silva-Santos, B., Serre, K. & Norell, H. Gammadelta T cells in cancer. Nat. Rev. Immunol. 15, 683–691 (2015).
Ma, Y. et al. Contribution of IL-17-producing γ δ T cells to the efficacy of anticancer chemotherapy. J. Exp. Med. 208, 491–503 (2011).
Dadi, S. et al. Cancer immunosurveillance by tissue-resident innate lymphoid cells and innate-like T cells. Cell 164, 365–377 (2016).
Donia, M., Ellebaek, E., Andersen, M. H., Straten, P. T. & Svane, I. M. Analysis of Vδ1 T cells in clinical grade melanoma-infiltrating lymphocytes. Oncoimmunology 1, 1297–1304 (2012).
Wang, J. et al. Tumor-infiltrating γδT cells predict prognosis and adjuvant chemotherapeutic benefit in patients with gastric cancer. Oncoimmunology 6, e1353858 (2017).
Meraviglia, S. et al. Distinctive features of tumor-infiltrating γδ T lymphocytes in human colorectal cancer. Oncoimmunology 6, e1347742 (2017).
Wu, P. et al. γδT17 cells promote the accumulation and expansion of myeloid-derived suppressor cells in human colorectal cancer. Immunity 40, 785–800 (2014).
Gentles, A. J. et al. The prognostic landscape of genes and infiltrating immune cells across human cancers. Nat. Med. 21, 938–945 (2015). This is an excellent but also controversial unbiased description of the immunological landscape of tumour-infiltrating lymphocytes that puts γδT cells at the centre of attention. Recommended to be read in combination with Deniger et al.
Tosolini, M. et al. Assessment of tumor-infiltrating TCR Vγ9Vδ2 γδ lymphocyte abundance by deconvolution of human cancers microarrays. Oncoimmunology 6, e1284723 (2017). This article presents a critical view of the impact of tumour-infiltrating γδT cells on clinical outcomes.
Chitadze, G., Oberg, H. H., Wesch, D. & Kabelitz, D. The ambiguous role of γδ t lymphocytes in antitumor immunity. Trends Immunol. 38, 668–678 (2017).
Pizzolato, G. et al. Single-cell RNA sequencing unveils the shared and the distinct cytotoxic hallmarks of human TCRVδ1 and TCRVδ2 γδ T lymphocytes. Proc. Natl Acad. Sci. USA 116, 11906–11915 (2019).
Godder, K. T. et al. Long term disease-free survival in acute leukemia patients recovering with increased γδ T cells after partially mismatched related donor bone marrow transplantation. Bone Marrow Transplant. 39, 751–757 (2007).
Perko, R. et al. Gamma delta T cell reconstitution is associated with fewer infections and improved event-free survival after hematopoietic stem cell transplantation for pediatric leukemia. Biol. Blood Marrow Transplant. 21, 130–136 (2015).
Scheper, W. et al. GammadeltaT cells elicited by CMV reactivation after allo-SCT cross-recognize CMV and leukemia. Leukemia 27, 1328–1338 (2013).
Couzi, L., Pitard, V., Moreau, J. F., Merville, P. & Dechanet-Merville, J. Direct and indirect effects of cytomegalovirus-induced γδ T cells after kidney transplantation. Front. Immunol. 6, 3 (2015).
Scheper, W., Grunder, C., Straetemans, T., Sebestyen, Z. & Kuball, J. Hunting for clinical translation with innate-like immune cells and their receptors. Leukemia 28, 1181–1190 (2014).
Litjens, N. H. R., van der Wagen, L., Kuball, J. & Kwekkeboom, J. Potential beneficial effects of cytomegalovirus infection after transplantation. Front. Immunol. 9, 389 (2018).
Handgretinger, R. & Schilbach, K. The potential role of γδ T cells after allogeneic HCT for leukemia. Blood 131, 1063–1072 (2018).
Couzi, L. et al. Cytomegalovirus-induced γδ T cells associate with reduced cancer risk after kidney transplantation. J. Am. Soc. Nephrol. 21, 181–188 (2009).
Halary, F. et al. Shared reactivity of Vδ2– γδ T cells against cytomegalovirus-infected cells and tumor intestinal epithelial cells. J. Exp. Med. 201, 1567–1578 (2005).
Deniger, D. C., Moyes, J. S. & Cooper, L. J. Clinical applications of γ δ T cells with multivalent immunity. Front. Immunol. 5, 636 (2014). This is a comprehensive review describing multiple failures in clinical trials that have dealt with γδT cells in the past.
Eberl, M. et al. Microbial isoprenoid biosynthesis and human γδT cell activation. FEBS Lett. 544, 4–10 (2003).
Gu, S., Borowska, M. T., Boughter, C. T. & Adams, E. J. Butyrophilin3A proteins and Vγ9Vδ2 T cell activation. Semin. Cell Dev. Biol. 84, 65–74 (2018).
Moulin, M. et al. Vγ9Vδ2 T cell activation by strongly agonistic nucleotidic phosphoantigens. Cell Mol. Life Sci. 74, 4353–4367 (2017).
Wilhelm, M. et al. Gammadelta T cells for immune therapy of patients with lymphoid malignancies. Blood 102, 200–206 (2003).
Dieli, F. et al. Targeting human γδ T cells with zoledronate and interleukin-2 for immunotherapy of hormone-refractory prostate cancer. Cancer Res. 67, 7450–7457 (2007).
Poccia, F. et al. Zoledronic acid and interleukin-2 treatment improves immunocompetence in HIV-infected persons by activating Vγ9Vδ2 T cells. AIDS 23, 555–565 (2009).
Bennouna, J. et al. Phase I study of bromohydrin pyrophosphate (BrHPP, IPH 1101), a Vγ9Vδ2 T lymphocyte agonist in patients with solid tumors. Cancer Immunol. Immunother. 59, 1521–1530 (2010).
Meraviglia, S. et al. In vivo manipulation of Vγ9Vδ2 T cells with zoledronate and low-dose interleukin-2 for immunotherapy of advanced breast cancer patients. Clin. Exp. Immunol. 161, 290–297 (2010).
Lang, J. M. et al. Pilot trial of interleukin-2 and zoledronic acid to augment γδ T cells as treatment for patients with refractory renal cell carcinoma. Cancer Immunol. Immunother. 60, 1447–1460 (2011).
Kunzmann, V. et al. Tumor-promoting versus tumor-antagonizing roles of γδ T cells in cancer immunotherapy: results from a prospective phase I/II trial. J. Immunother. 35, 205–213 (2012).
Pressey, J. G. et al. In vivo expansion and activation of γδ T cells as immunotherapy for refractory neuroblastoma: a phase 1 study. Medicine (Baltimore) 95, e4909 (2016).
Bregeon, D. et al. Synthesis of phosphoantigens: scalable accesses to enantiomers of BrHPP and studies on N-HDMAPP synthesis. Bioorg. Med. Chem. Lett. 22, 5807–5810 (2012).
Kobayashi, H. et al. Safety profile and anti-tumor effects of adoptive immunotherapy using γ-δ T cells against advanced renal cell carcinoma: a pilot study. Cancer Immunol. Immunother. 56, 469–476 (2007).
Bennouna, J. et al. Phase-I study of Innacell γδ, an autologous cell-therapy product highly enriched in γ9δ2 T lymphocytes, in combination with IL-2, in patients with metastatic renal cell carcinoma. Cancer Immunol. Immunother. 57, 1599–1609 (2008).
Abe, Y. et al. Clinical and immunological evaluation of zoledronate-activated Vγ9γδ T-cell-based immunotherapy for patients with multiple myeloma. Exp. Hematol. 37, 956–968 (2009).
Nakajima, J. et al. A phase I study of adoptive immunotherapy for recurrent non-small-cell lung cancer patients with autologous γδ T cells. Eur. J. Cardiothorac. Surg. 37, 1191–1197 (2010).
Kobayashi, H., Tanaka, Y., Yagi, J., Minato, N. & Tanabe, K. Phase I/II study of adoptive transfer of γδ T cells in combination with zoledronic acid and IL-2 to patients with advanced renal cell carcinoma. Cancer Immunol. Immunother. 60, 1075–1084 (2011).
Nicol, A. J. et al. Clinical evaluation of autologous γ δ T cell-based immunotherapy for metastatic solid tumours. Br. J. Cancer 105, 778–786 (2011).
Noguchi, A. et al. Zoledronate-activated Vγ9γδ T cell-based immunotherapy is feasible and restores the impairment of γδ T cells in patients with solid tumors. Cytotherapy 13, 92–97 (2011).
Sakamoto, M. et al. Adoptive immunotherapy for advanced non-small cell lung cancer using zoledronate-expanded γδT cells: a phase I clinical study. J. Immunother. 34, 202–211 (2011).
Cui, J. et al. Combination of radiofrequency ablation and sequential cellular immunotherapy improves progression-free survival for patients with hepatocellular carcinoma. Int. J. Cancer 134, 342–351 (2014).
Izumi, T. et al. Ex vivo characterization of γδ T-cell repertoire in patients after adoptive transfer of Vγ9Vδ2 T cells expressing the interleukin-2 receptor beta-chain and the common γ-chain. Cytotherapy 15, 481–491 (2013).
Wada, I. et al. Intraperitoneal injection of in vitro expanded Vγ9Vδ2 T cells together with zoledronate for the treatment of malignant ascites due to gastric cancer. Cancer Med. 3, 362–375 (2014).
Aoki, T. et al. Adjuvant combination therapy with gemcitabine and autologous γδ T-cell transfer in patients with curatively resected pancreatic cancer. Cytotherapy 19, 473–485 (2017).
Lamb, L. S. Jr et al. Increased frequency of TCR γδ+ T cells in disease-free survivors following T cell-depleted, partially mismatched, related donor bone marrow transplantation for leukemia. J. Hematother. 5, 503–509 (1996). This article is the first clinical description of the potential benefit of γδT cells after allogeneic stem cell transplantation.
Wilhelm, M. et al. Successful adoptive transfer and in vivo expansion of haploidentical γδ T cells. J. Transl Med. 12, 45 (2014).
Rock, E. P., Sibbald, P. R., Davis, M. M. & Chien, Y. H. CDR3 length in antigen-specific immune receptors. J. Exp. Med. 179, 323–328 (1994).
Schild, H. et al. The nature of major histocompatibility complex recognition by γ δ T cells. Cell 76, 29–37 (1994).
Elliott, J. F., Rock, E. P., Patten, P. A., Davis, M. M. & Chien, Y. H. The adult T-cell receptor δ-chain is diverse and distinct from that of fetal thymocytes. Nature 331, 627–631 (1988).
Casorati, G., De Libero, G., Lanzavecchia, A. & Migone, N. Molecular analysis of human γ/δ+ clones from thymus and peripheral blood. J. Exp. Med. 170, 1521–1535 (1989).
Ravens, S. et al. Human γδ T cells are quickly reconstituted after stem-cell transplantation and show adaptive clonal expansion in response to viral infection. Nat. Immunol. 18, 393–401 (2017). This is a comprehensive analysis of the γδT cell repertoire after allogeneic stem cell transplantation.
Sherwood, A. M. et al. Deep sequencing of the human TCRγ and TCRβ repertoires suggests that TCRβ rearranges after αβ and γδ T cell commitment. Sci. Transl Med. 3, 90ra61 (2011).
Dimova, T. et al. Effector Vγ9Vδ2 T cells dominate the human fetal γδ T-cell repertoire. Proc. Natl Acad. Sci. USA 112, E556–E565 (2015).
Davey, M. S. et al. The human Vδ2+ T-cell compartment comprises distinct innate-like Vγ9+ and adaptive Vγ9− subsets. Nat. Commun. 9, 1760 (2018).
Fisch, P. et al. Recognition by human Vγ9/Vδ2 T cells of a GroEL homolog on Daudi Burkitt’s lymphoma cells. Science 250, 1269–1273 (1990).
Grunder, C. et al. Gamma9 and δ2CDR3 domains regulate functional avidity of T cells harboring γ9δ2TCRs. Blood 120, 5153–5162 (2012). This article describes the impacts of different CDR3 domains on the functional avidity of TEGs.
Starick, L. et al. Butyrophilin 3 A (BTN3A, CD277)-specific antibody 20.1 differentially activates Vγ9Vδ2 TCR clonotypes and interferes with phosphoantigen activation. Eur. J. Immunol. 47, 982–992 (2017).
Wang, H., Fang, Z. & Morita, C. T. Vγ2Vδ2 T. cell receptor recognition of prenyl pyrophosphates is dependent on all CDRs. J. Immunol. 184, 6209–6222 (2010).
Willcox, C. R., Davey, M. S. & Willcox, B. E. Development and Selection of the Human Vγ9Vδ2(+) T-Cell Repertoire. Front. Immunol. 9, 1501 (2018).
Davey, M. S. et al. Clonal selection in the human Vδ1 T cell repertoire indicates γδ TCR-dependent adaptive immune surveillance. Nat. Commun. 8, 14760 (2017).
Pitard, V. et al. Long-term expansion of effector/memory Vδ2-γδ T cells is a specific blood signature of CMV infection. Blood 112, 1317–1324 (2008). This article analyses the correlation between cytomegalovirus infection and γδT cell expansion.
Dechanet, J. et al. Major expansion of γδ T lymphocytes following cytomegalovirus infection in kidney allograft recipients. J. Infect. Dis. 179, 1–8 (1999).
Dechanet, J. et al. Implication of γδ T cells in the human immune response to cytomegalovirus. J. Clin. Invest 103, 1437–1449 (1999).
Kallemeijn, M. J. et al. Next-generation sequencing analysis of the human TCRγδ+ T-cell repertoire reveals shifts in vγ- and vδ-usage in memory populations upon aging. Front. Immunol. 9, 448 (2018).
Scheper, W., Sebestyen, Z. & Kuball, J. Cancer immunotherapy using γδt cells: dealing with diversity. Front. Immunol. 5, 601 (2014).
Carding, S. R. & Egan, P. J. γδ T cells: functional plasticity and heterogeneity. Nat. Rev. Immunol. 2, 336–345 (2002).
McCarthy, N. E. & Eberl, M. Human γδ T-cell control of mucosal immunity and inflammation. Front. Immunol. 9, 985 (2018).
Melandri, D. et al. The γδTCR combines innate immunity with adaptive immunity by utilizing spatially distinct regions for agonist selection and antigen responsiveness. Nat. Immunol. 19, 1352–1365 (2018).
Di Marco Barros, R. et al. Epithelia use butyrophilin-like molecules to shape organ-specific γδ T cell compartments. Cell 167, 203–218 (2016).
Sandrock, I. et al. Genetic models reveal origin, persistence and non-redundant functions of IL-17-producing γδ T cells. J. Exp. Med. 215, 3006–3018 (2018).
Willcox, C. R. et al. Cytomegalovirus and tumor stress surveillance by binding of a human γδ T cell antigen receptor to endothelial protein C receptor. Nat. Immunol. 13, 872–879 (2012).
Sebestyen, Z. et al. Rhob mediates phosphoantigen recognition by Vγ9Vδ2 T cell receptor. Cell Rep. 15, 1973–1985 (2016). This is the first article to describe the key role of the small GTPase RhoB in regulation of CD277J.
Pavlova, N. N. & Thompson, C. B. The emerging hallmarks of cancer metabolism. Cell Metab. 23, 27–47 (2016).
Snyder, A. et al. Genetic basis for clinical response to CTLA-4 blockade in melanoma. N. Engl. J. Med. 371, 2189–2199 (2014).
Gober, H. J. et al. Human T cell receptor γδ cells recognize endogenous mevalonate metabolites in tumor cells. J. Exp. Med. 197, 163–168 (2003).
Tanaka, Y. et al. Natural and synthetic non-peptide antigens recognized by human γ δ T cells. Nature 375, 155–158 (1995).
Vantourout, P. et al. Specific requirements for Vγ9Vδ2 T cell stimulation by a natural adenylated phosphoantigen. J. Immunol. 183, 3848–3857 (2009).
Ashihara, E. et al. Isopentenyl pyrophosphate secreted from Zoledronate-stimulated myeloma cells, activates the chemotaxis of γδT cells. Biochem. Biophys. Res. Commun. 463, 650–655 (2015).
Harly, C. et al. Key implication of CD277/butyrophilin-3 (BTN3A) in cellular stress sensing by a major human γδ T-cell subset. Blood 120, 2269–2279 (2012). This article emphasizes the key role of CD277 in Vγ9Vδ2 T cell recognition.
Boutin, L. & Scotet, E. Towards deciphering the hidden mechanisms that contribute to the antigenic activation process of human Vγ9Vδ2 T cells. Front. Immunol. 9, 828 (2018).
Gu, S. et al. Phosphoantigen-induced conformational change of butyrophilin 3A1 (BTN3A1) and its implication on Vγ9Vδ2 T cell activation. Proc. Natl Acad. Sci. USA 114, E7311–E7320 (2017).
Peigne, C. M. et al. The juxtamembrane domain of butyrophilin btn3a1 controls phosphoantigen-mediated activation of human Vγ9Vδ2 T cells. J. Immunol. 198, 4228–4234 (2017).
Nguyen, K. et al. The butyrophilin 3A1 intracellular domain undergoes a conformational change involving the juxtamembrane region. FASEB J. 31, 4697–4706 (2017).
Rhodes, D. A. et al. Activation of human γδ T cells by cytosolic interactions of BTN3A1 with soluble phosphoantigens and the cytoskeletal adaptor periplakin. J. Immunol. 194, 2390–2398 (2015).
Vantourout, P. et al. Heteromeric interactions regulate butyrophilin (BTN) and BTN-like molecules governing γδ T cell biology. Proc. Natl Acad. Sci. USA 115, 1039–1044 (2018).
Dai, Y., Chen, H., Mo, C., Cui, L. & He, W. Ectopically expressed human tumor biomarker MutS homologue 2 is a novel endogenous ligand that is recognized by human γδ T cells to induce innate anti-tumor/virus immunity. J. Biol. Chem. 287, 16812–16819 (2012).
Mo, C., Dai, Y., Kang, N., Cui, L. & He, W. Ectopic expression of human MutS homologue 2 on renal carcinoma cells is induced by oxidative stress with interleukin-18 promotion via p38 mitogen-activated protein kinase (MAPK) and c-Jun N-terminal kinase (JNK) signaling pathways. J. Biol. Chem. 287, 19242–19254 (2012).
Scotet, E. et al. Tumor recognition following Vγ9Vδ2 T cell receptor interactions with a surface F1-ATPase-related structure and apolipoprotein A-I. Immunity 22, 71–80 (2005).
Chen, H. et al. Chaperonin-containing T-complex protein 1 subunit zeta serves as an autoantigen recognized by human Vδ2 γδ T cells in autoimmune diseases. J. Biol. Chem. 291, 19985–19993 (2016).
Boyden, L. M. et al. Skint1, the prototype of a newly identified immunoglobulin superfamily gene cluster, positively selects epidermal γδ T cells. Nat. Genet. 40, 656–662 (2008).
Vermijlen, D., Gatti, D., Kouzeli, A., Rus, T. & Eberl, M. Gammadelta T cell responses: how many ligands will it take till we know? Semin. Cell Dev. Biol. 84, 75–86 (2018).
Simoes, A. E., Di Lorenzo, B. & Silva-Santos, B. Molecular determinants of target cell recognition by human γδ T cells. Front. Immunol. 9, 929 (2018).
Adams, E. J., Gu, S. & Luoma, A. M. Human γ δ T cells: evolution and ligand recognition. Cell Immunol. 296, 31–40 (2015).
Luoma, A. M., Castro, C. D. & Adams, E. J. γδ T cell surveillance via CD1 molecules. Trends Immunol. 35, 613–621 (2014).
Uldrich, A. P. et al. CD1d-lipid antigen recognition by the γδ TCR. Nat. Immunol. 14, 1137–1145 (2013).
Luoma, A. M. et al. Crystal structure of Vδ1 T cell receptor in complex with CD1d-sulfatide shows MHC-like recognition of a self-lipid by human γδ T cells. Immunity 39, 1032–1042 (2013).
Mangan, B. A. et al. Cutting edge: CD1d restriction and Th1/Th2/Th17 cytokine secretion by human Vδ3 T cells. J. Immunol. 191, 30–34 (2013).
Lepore, M. et al. A novel self-lipid antigen targets human T cells against CD1c(+) leukemias. J. Exp. Med. 211, 1363–1377 (2014).
Roy, S. et al. Molecular analysis of lipid-reactive vδ1 γδ T cells identified by CD1C tetramers. J. Immunol. 196, 1933–1942 (2016).
Hayday, A. & Vantourout, P. A long-playing CD about the γδ TCR repertoire. Immunity 39, 994–996 (2013).
Groh, V. et al. Broad tumor-associated expression and recognition by tumor-derived γδ T cells of MICA and MICB. Proc. Natl Acad. Sci. USA 96, 6879–6884 (1999).
Willcox, C. R., Mohammed, F. & Willcox, B. E. Resolving the mystery of pyrophosphate antigen presentation. Nat. Immunol. 14, 886–887 (2013).
Reeves, S. A., Chavez-Kappel, C., Davis, R., Rosenblum, M. & Israel, M. A. Developmental regulation of annexin II (Lipocortin 2) in human brain and expression in high grade glioma. Cancer Res. 52, 6871–6876 (1992).
Marlin, R. et al. Sensing of cell stress by human γδ TCR-dependent recognition of annexin A2. Proc. Natl Acad. Sci. USA 114, 3163–3168 (2017).
Almeida, A. R. et al. Delta one t cells for immunotherapy of chronic lymphocytic leukemia: clinical-grade expansion/differentiation and preclinical proof of concept. Clin. Cancer Res. 22, 5795–5804 (2016). This article presents a comprehensive description of the DOT cell concept.
Halary, F. et al. Control of self-reactive cytotoxic T lymphocytes expressing γ δ T cell receptors by natural killer inhibitory receptors. Eur. J. Immunol. 27, 2812–2821 (1997).
Couzi, L. et al. Common features of γδ T cells and CD8(+) alphabeta T cells responding to human cytomegalovirus infection in kidney transplant recipients. J. Infect. Dis. 200, 1415–1424 (2009).
Trichet, V. et al. Complex interplay of activating and inhibitory signals received by Vγ9Vδ2 T cells revealed by target cell beta2-microglobulin knockdown. J. Immunol. 177, 6129–6136 (2006).
Orr, M. T. & Lanier, L. L. Natural killer cell education and tolerance. Cell 142, 847–856 (2010).
Benveniste, P. M. et al. Generation and molecular recognition of melanoma-associated antigen-specific human γδ T cells. Sci. Immunol. 3, eaav4036 (2018).
Kierkels, G. et al. Identification of a tumor-specific allo-HLA-restricted γδTCR. Blood Adv. (in the press).
de Witte, M. A., Kierkels, G. J., Straetemans, T., Britten, C. M. & Kuball, J. Orchestrating an immune response against cancer with engineered immune cells expressing alphabetaTCRs, CARs, and innate immune receptors: an immunological and regulatory challenge. Cancer Immunol. Immunother. 64, 893–902 (2015).
Gibbons, D. L. et al. Neonates harbour highly active γδ T cells with selective impairments in preterm infants. Eur. J. Immunol. 39, 1794–1806 (2009).
Ribot, J. C., Ribeiro, S. T., Correia, D. V., Sousa, A. E. & Silva-Santos, B. Human γδ thymocytes are functionally immature and differentiate into cytotoxic type 1 effector T cells upon IL-2/IL-15 signaling. J. Immunol. 192, 2237–2243 (2014).
Ryan, P. L. et al. Heterogeneous yet stable Vδ2+ T-cell profiles define distinct cytotoxic effector potentials in healthy human individuals. Proc. Natl Acad. Sci. USA 113, 14378–14383 (2016). This article analyses the heterogeneity in profiles of Vδ2 + γδT cells.
Daley, D. et al. Gammadelta T cells support pancreatic oncogenesis by restraining alphabeta T cell activation. Cell 166, 1485–1499 e1415 (2016).
Lo Presti, E., Dieli, F. & Meraviglia, S. Tumor-infiltrating γδ T lymphocytes: pathogenic role, clinical significance, and differential programing in the tumor microenvironment. Front. Immunol. 5, 607 (2014).
Fleming, C., Morrissey, S., Cai, Y. & Yan, J. Gammadelta T cells: unexpected regulators of cancer development and progression. Trends Cancer 3, 561–570 (2017).
Rei, M. et al. Murine CD27– Vγ6(+) γδ T cells producing IL-17A promote ovarian cancer growth via mobilization of protumor small peritoneal macrophages. Proc. Natl Acad. Sci. USA 111, E3562–E3570 (2014).
Wakita, D. et al. Tumor-infiltrating IL-17-producing γδ T cells support the progression of tumor by promoting angiogenesis. Eur. J. Immunol. 40, 1927–1937 (2010).
McAllister, F. et al. Oncogenic Kras activates a hematopoietic-to-epithelial IL-17 signaling axis in preinvasive pancreatic neoplasia. Cancer Cell 25, 621–637 (2014).
Coffelt, S. B. et al. IL-17-producing γδ T cells and neutrophils conspire to promote breast cancer metastasis. Nature 522, 345–348 (2015).
Caccamo, N. et al. Differentiation, phenotype, and function of interleukin-17-producing human Vγ9Vδ2 T cells. Blood 118, 129–138 (2011).
Patil, R. S. et al. IL17 producing γδT cells induce angiogenesis and are associated with poor survival in gallbladder cancer patients. Int. J. Cancer 139, 869–881 (2016).
Peng, G. et al. Tumor-infiltrating γδ T cells suppress T and dendritic cell function via mechanisms controlled by a unique toll-like receptor signaling pathway. Immunity 27, 334–348 (2007).
Ma, C. et al. Tumor-infiltrating γδ T lymphocytes predict clinical outcome in human breast cancer. J. Immunol. 189, 5029–5036 (2012).
Ye, J. et al. Specific recruitment of γδ regulatory T cells in human breast cancer. Cancer Res. 73, 6137–6148 (2013).
Ye, J. et al. Tumor-derived γδ regulatory T cells suppress innate and adaptive immunity through the induction of immunosenescence. J. Immunol. 190, 2403–2414 (2013).
de Bruin, R. C. G. et al. A bispecific nanobody approach to leverage the potent and widely applicable tumor cytolytic capacity of Vγ9Vδ2-T cells. Oncoimmunology 7, e1375641 (2017).
Kontermann, R. E. & Brinkmann, U. Bispecific antibodies. Drug Discov. Today 20, 838–847 (2015).
Lamb, L. S. Jr et al. Engineered drug resistant γδ T cells kill glioblastoma cell lines during a chemotherapy challenge: a strategy for combining chemo- and immunotherapy. PLoS ONE 8, e51805 (2013).
de Weerdt, I. et al. Improving CLL Vγ9Vδ2-T-cell fitness for cellular therapy by ex vivo activation and ibrutinib. Blood 132, 2260–2272 (2018).
Wistuba-Hamprecht, K. et al. Proportions of blood-borne Vδ1+ and Vδ2+ T-cells are associated with overall survival of melanoma patients treated with ipilimumab. Eur. J. Cancer 64, 116–126 (2016).
Correia, D. V. et al. Differentiation of human peripheral blood Vδ1+ T cells expressing the natural cytotoxicity receptor NKp30 for recognition of lymphoid leukemia cells. Blood 118, 992–1001 (2011).
Di Lorenzo, B. et al. Broad cytotoxic targeting of acute myeloid leukemia by polyclonal δ1 T cells. Cancer Immunol. Res. 7, 552–558 (2019).
Capsomidis, A. et al. Chimeric antigen receptor-engineered human γδ T cells: enhanced cytotoxicity with retention of cross presentation. Mol. Ther. 26, 354–365 (2018).
Fisher, J. & Anderson, J. Engineering approaches in human γδ T cells for cancer immunotherapy. Front. Immunol. 9, 1409 (2018).
Li, Y., Hermanson, D. L., Moriarity, B. S. & Kaufman, D. S. Human IPSC-derived natural killer cells engineered with chimeric antigen receptors enhance anti-tumor activity. Cell Stem Cell 23, 181–192 (2018).
de Witte, M. A. et al. Early reconstitution of nk and γδ T cells and its implication for the design of post-transplant immunotherapy. Biol. Blood Marrow Transplant. 24, 1152–1162 (2018).
Hartmann, J., Schussler-Lenz, M., Bondanza, A. & Buchholz, C. J. Clinical development of CAR T cells-challenges and opportunities in translating innovative treatment concepts. EMBO Mol. Med. 9, 1183–1197 (2017).
Scheper, W., Grunder, C. & Kuball, J. Multifunctional γδ T cells and their receptors for targeted anticancer immunotherapy. Oncoimmunology 2, e23974 (2013).
Marcu-Malina, V. et al. Redirecting alphabeta T cells against cancer cells by transfer of a broadly tumor-reactive γδT-cell receptor. Blood 118, 50–59 (2011).
Straetemans, T. et al. Untouched GMP-ready purified engineered immune cells to treat cancer. Clin. Cancer Res. 21, 3957–3968 (2015).
Bouchie, A., DeFrancesco, L., Sheridan, C. & Webb, S. Nature Biotechnology’s academic spinouts of 2016. Nat. Biotechnol. 35, 322–333 (2017).
Braham, M. V. J. et al. Cellular immunotherapy on primary multiple myeloma expanded in a 3D bone marrow niche model. Oncoimmunology 7, e1434465 (2018).
Straetemans, T. et al. GMP-grade manufacturing of T cells engineered to express a defined γδTCR. Front. Immunol. 9, 1062 (2018). This article presents a detailed description of the production of TEGs for clinical use.
Netherlands Trial Register. A phase I study to investigate the safety of TEG001 cell suspension for infusion in patients with relapsed/refractory acute myeloid leukemia, high-risk myelodysplastic syndrome (IPSS-R score > 4,5) or multiple myeloma. NTR https://www.trialregister.nl/trial/6357 (2017).
Linette, G. P. et al. Cardiovascular toxicity and titin cross-reactivity of affinity-enhanced T cells in myeloma and melanoma. Blood 122, 863–871 (2013).
Bhullar, K. S. et al. Kinase-targeted cancer therapies: progress, challenges and future directions. Mol. Cancer 17, 48 (2018).
Tanaka, Y. et al. Synthesis of pyrophosphate-containing compounds that stimulate Vγ2Vδ2 T cells: application to cancer immunotherapy. Med. Chem. 3, 85–99 (2007).
van de Donk, N. & Usmani, S. Z. CD38 antibodies in multiple myeloma: mechanisms of action and modes of resistance. Front. Immunol. 9, 2134 (2018).
McCarthy, N. E. et al. Azathioprine therapy selectively ablates human Vδ2(+) T cells in Crohn’s disease. J Clin. Invest. 125, 3215–3225 (2015).
Johanna, I. et al. Evaluating in vivo efficacy — toxicity profile of TEG001 in humanized mice xenografts against primary human AML disease and healthy hematopoietic cells. J. Immunother. Cancer 7, 69 (2019).
Hanahan, D. & Weinberg, R. A. Hallmarks of cancer: the next generation. Cell 144, 646–674 (2011).
Blokzijl, F. et al. Tissue-specific mutation accumulation in human adult stem cells during life. Nature 538, 260–264 (2016).
Chen, Z. W. Protective immune responses of major Vγ2Vδ2 T-cell subset in M. tuberculosis infection. Curr. Opin. Immunol. 42, 105–112 (2016).
Qaqish, A. et al. Adoptive transfer of phosphoantigen-specific γδ T cell subset attenuates mycobacterium tuberculosis infection in nonhuman primates. J. Immunol. 198, 4753–4763 (2017).
Manickam, C., Shah, S. V., Nohara, J., Ferrari, G. & Reeves, R. K. Monkeying around: using non-human primate models to study NK cell biology in HIV infections. Front. Immunol. 10, 1124 (2019).
Drost, J. & Clevers, H. Organoids in cancer research. Nat. Rev. Cancer 18, 407–418 (2018).
Dijkstra, K. K. et al. Generation of tumor-reactive T cells by co-culture of peripheral blood lymphocytes and tumor organoids. Cell 174, 1586–1598 (2018).
Ledford, H., Else, H. & Warren, M. Cancer immunologists scoop medicine Nobel Prize. Nature 562, 20–21 (2018).
Harly, C., Peigne, C. M. & Scotet, E. Molecules and mechanisms implicated in the peculiar antigenic activation process of human Vγ9Vδ2 T cells. Front. Immunol. 5, 657 (2014).
Acknowledgements
The authors appreciate the support of D. Beringer for the illustrations provided here of chemicals and crystal structures. Funding for this study was provided by grants ZonMW 43400003, VIDI-ZonMW 917.11.337, KWF UU 2013-6426, UU 2014-6790, UU 2015-7601, UU2018-11979 and GADETA to J.K.; UU2017-11393 to Z.S. and J.K.; European Research Council grant CoG_646701 to B.S.S.; and DFG grant FOR 2799-PR727/11-1 to I.P.; as well as by Ligue Contre le Cancer (Equipe labellisée 2017) and SIRIC BRIO grants to J.D.M.
Author information
Authors and Affiliations
Contributions
The authors contributed equally to all aspects of the article.
Corresponding author
Ethics declarations
Competing interests
J.D.M. is scientific adviser of American Gene Technologies; B.S.S. is a cofounder of Lymphact SA, a shareholder and scientific adviser of GammaDelta Therapeutics, and an inventor on patents dealing with DOT cells. J.K. is cofounder, shareholder and scientific adviser of GADETA and inventor on multiple patents dealing with gdTCR and their ligands, as well as with isolation techniques for engineered immune cells. Z.S. is an inventor of patents dealing with gdTCR and their ligands. I.P. declares no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
Adicet Bio announces the transition of founder, president and chief executive officer Dr. Aya Jakobovits: https://www.prnewswire.com/news-releases/adicet-bio-announces-the-transition-of-founder-president-and-chief-executive-officer-dr-aya-jakobovits-300608616.html
American Gene Technologies: https://www.americangene.com
Boehringer Ingelheim, PureTech to partner on cancer immunotherapies: https://www.genengnews.com/news/boehringer-ingelheim-puretech-to-partner-on-cancer-immunotherapies/
Company profile: PhosphoGam: https://cednc.org/company-profile/PhosphoGam
Gadeta: https://www.gadeta.nl
GammaCell Biotechnologies: https://www.gammacelltech.com
GammaDelta Therapeutics: https://gammadeltatx.com
ImCheck therapeutics: http://www.imchecktherapeutics.com
Immatics: https://immatics.com/company.html
Incysus Therapeutics: https://www.incysus.com
Lava Therapeutics: https://lavatherapeutics.com
TC BioPharm: http://www.tcbiopharm.com
Glossary
- Vγ9Vδ2 T cells
-
The main circulating human γδT cells, in which their γδ T cell receptor (TCR) heterodimer is built by a TCRγ chain that uses a Vγ9 segment and a TCRδ chain using the variable (V) segment Vδ2. Vγ9Vδ2 T cells display a relatively limited diversity of their individually rearranged TCR sequences, and are therefore regarded as semi-invariant.
- Vδ1+ T cells
-
A subset of human γδT cells in which their T cell receptor (TCR) uses a Vδ1 segment for its TCRδ chain. TCRδ sequences of Vδ1+ T cells are more diverse than those of Vγ9Vδ2 T cells, and the repertoire of Vδ1+ T cells is further expanded by pairing with different TCRγ chains (using Vγ2, 3,4,5,8, and non-invariant Vγ9 segments). Vδ1+ T cells have been reported to recognize a wide range of cancer cells.
- non-Vγ9Vδ2 γδT cells
-
All human γδT cells except Vγ9Vδ2 γδT cells, including TCRδ chain 1 or 3 to 8, and any Vγ chains (Vγ2, 3, 4, 5, 8, 9).
- Phosphoantigens
-
Intracellular metabolites of the mevalonate pathway, such as isopentenyl pyrophosphate (IPP), or metabolites derived from the mevalonate-independent 1-deoxy-d-xylulose 5-phosphate (DOXP) pathway in bacteria or parasites. (E)-4-hydroxy-3-methyl-but-2-enyl pyrophosphate (HMBPP) is produced by several bacteria and parasites and is the most powerful stimulant for Vγ9Vδ2 T cells. Also, synthetic phosphoantigens have been reported, such as bromohydrin pyrophosphate (BrHPP) and 2-methyl-3-butenyl-1-pyrophosphate (2M3B1PP).
- Aminobisphosphonates
-
Metabolites such as pamidronate or zoledronate that partially block the natural mevalonate pathway after the production of isopentenyl pyrophosphate (IPP), through inhibiting farnesyl pyrophosphate synthase, and thereby increase IPP levels. Aminobisphosphonates have been used in daily clinical practice for decades — for example, in patients with multiple myeloma — to stabilize bone formation, mainly because of their inhibitory effect on osteoclasts.
- Natural killer T cells
-
(NKT cells). Immune cells that share properties of αβT cells and NK cells. The αβTCR of NKT cells expresses the invariant TCR Vα24 chain, characterized by their usage of the Jα18 segment in humans. Most NKT cells recognize through their αβTCR lipids expressed within the context of CD1c or CD1d.
- Cytotoxic type 1 phenotype
-
Ability in αβ and γδ T cells to mediate the killing of target cells through the secretion of granzymes and perforin. Such T cells usually also produce IFNγ and TNF.
- Anergy
-
State of an immune cell, which correlates with loss of function and can also result in deletion, and thus the complete loss of defined γδT cells.
- Regulatory γδT cells
-
(Treg cells). A subpopulation of T cells that modulate the immune system. Until recently regulatory cells have been attributed solely to αβT cells, and they are characterized by the expression of CD4, CD25 and FOXP3, with a subset also producing IL-17. Now it has also been proposed that γδT cells have regulatory properties and that regulatory γδT cells secrete IL-17 and mediate tolerance against cancer cells.
- Tolerogeneic profile
-
Immune cells secreting cytokines that induce tolerance, such as IL-10 and IL-17, or enhance the expression of inhibitory checkpoint molecules in their microenvironment.
- Ipilimumab
-
Monoclonal antibody that activates immune cells by targeting CTLA4.
- Cytokine release syndrome
-
Mild to life-threatening syndrome caused by a rapid release of cytokines after adoptive transfer of CAR T cells or other types of immune therapy.
Rights and permissions
About this article
Cite this article
Sebestyen, Z., Prinz, I., Déchanet-Merville, J. et al. Translating gammadelta (γδ) T cells and their receptors into cancer cell therapies. Nat Rev Drug Discov 19, 169–184 (2020). https://doi.org/10.1038/s41573-019-0038-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41573-019-0038-z
This article is cited by
-
Evolution of T cells in the cancer-resistant naked mole-rat
Nature Communications (2024)
-
Divergent immune microenvironments in two tumor nodules from a patient with mismatch repair-deficient prostate cancer
npj Genomic Medicine (2024)
-
TACE responser NDRG1 acts as a guardian against ferroptosis to drive tumorgenesis and metastasis in HCC
Biological Procedures Online (2023)
-
Gamma delta T-cell-based immune checkpoint therapy: attractive candidate for antitumor treatment
Molecular Cancer (2023)
-
The cytotoxicity of γδT cells in non-small cell lung cancer mediated via coordination of the BCL-2 and AKT pathways
Oncogene (2023)