Abstract
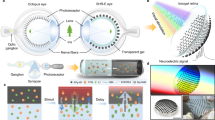
The prevalence of myopia has increased worldwide over the last 50 years. Its incidence in the United States and Europe is now almost twice that 50 years ago, and it is even more prevalent in East Asia. Spectacles and contact lenses remain the most common means of vision correction, but the permanent correction of refractive errors, by refractive surgery, has emerged as an attractive alternative. However, such surgery is an invasive procedure that may compromise corneal structure, and post-surgical complications have been reported. We propose a novel, non-invasive approach to permanent vision correction based on a different mode of laser–cornea interaction. Our approach induces the formation of a low-density plasma that produces reactive oxygen species, which react with the surrounding proteins, forming crosslinks and triggering spatially resolved changes in mechanical properties. We show that the proposed method changes the refractive power of the eye, and confirm its safety and stability.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Dolgin, E. The myopia boom. Nature 519, 276–278 (2015).
Fredrick, D. R. Myopia. Br. Med. J. 324, 1195–1199 (2002).
Richdale, K., Sinnott, L. T., Skadahl, E. & Nichols, J. J. Frequency of and factors associated with contact lens dissatisfaction and discontinuation. Cornea 26, 168–174 (2007).
Solomon, K. D. et al. LASIK world literature review: quality of life and patient satisfaction. Ophthalmology 116, 691–701 (2009).
Elling, M., Kersten-Gomez, I. & Dick, H. B. Photorefractive intrastromal corneal crosslinking for the treatment of myopic refractive errors: six-month interim findings. J. Cataract Refract. Surg. 43, 789–795 (2017).
Gamaly, E. G., Rode, A. V., Luther-Davies, B. & Tikhonchuk, V. T. Ablation of solids by femtosecond lasers: ablation mechanism and ablation thresholds for metals and dielectrics. Phys. Plasmas 9, 949–957 (2002).
Stuart, B. C. et al. Nanosecond-to-femtosecond laser-induced breakdown in dielectrics. Phys. Rev. B Condens. Matter 53, 1749–1761 (1996).
Vogel, A., Noack, J., Hüttmann, G. & Paltauf, G. Low-density plasmas below the optical breakdown threshold: potential hazard for multiphoton microscopy, and a tool for the manipulation of intracellular events. Proc. SPIE 4620, 202–216 (2002).
Vogel, A., Noack, J., Huttman, G. & Paltauf, G. Mechanisms of femtosecond laser nanosurgery of cells and tissues. Appl. Phys. B Lasers Opt. 81, 1015–1047 (2005).
Schaffer, C. B., Jamison, A. O. & Mazur, E. Morphology of femtosecond laser-induced structural changes in bulk transparent materials. Appl. Phys. Lett. 84, 1441–1443 (2004).
Guo, Y., Wang, C., Celi, N. & Vukelic, S. Femtosecond laser collagen cross-linking without traditional photosensitizers. Proc. SPIE 9321, 932103 (2015).
Wang, C. et al. Femtosecond laser irradiation as novel paradigm for treatment of early osteoarthritis. In Orthopaedic Research Society 2017 Annual Meeting poster 563 (2017).
Wollensak, G., Spoerl, E. & Seiler, T. Stress–strain measurements of human and porcine corneas after riboflavin–ultraviolet-A-induced cross-linking. J. Cataract Refract. Surg. 29, 1780–1785 (2003).
Heisterkamp, A. et al. Intrastromal refractive surgery with ultrashort laser pulses: in vivo study on the rabbit eye. Graefes Arch. Clin. Exp. Ophthalmol. 241, 511–517 (2003).
Mountford, J, Ruston, D. & Dave, T. Orthokeratology: Principles and Practice (Butterworth-Heinemann, London, 2004).
Teng, S. W. et al. Multiphoton autofluorescence and second-harmonic generation imaging of the ex vivo porcine eye. Invest. Ophthalmol. Vis. Sci. 47, 1216–1224 (2006).
Zipfel, W. R. et al. Live tissue intrinsic emission microscopy using multiphoton-excited native fluorescence and second harmonic generation. Proc. Natl Acad. Sci. USA 100, 7075–7080 (2003).
Raub, C. B. et al. Noninvasive assessment of collagen gel microstructure and mechanics using multiphoton microscopy. Biophys. J. 92, 2212–2222 (2007).
Steven, P., Hovakimyan, M., Guthoff, R. F., Huttmann, G. & Stachs, O. Imaging corneal crosslinking by autofluorescence 2-photon microscopy, second harmonic generation, and fluorescence lifetime measurements. J. Cataract Refract. Surg. 36, 2150–2159 (2010).
Mencucci, R. et al. Ultrasound thermal damage to rabbit corneas after simulated phacoemulsification. J. Cataract Refract. Surg. 31, 2180–2186 (2005).
Zyablitskaya, M. et al. Evaluation of therapeutic tissue crosslinking (TXL) for myopia using second harmonic generation signal microscopy in rabbit sclera. Invest. Ophthalmol. Vis. Sci. 58, 21–29 (2017).
Zhang, W. et al. Rabbit model of corneal endothelial injury established using the Nd:YAG laser. Cornea 36, 1274–1281 (2017).
Steven, P., Hovakimyan, M., Guthoff, R. F., Hüttmann, G. & Stachs, O. Imaging corneal crosslinking by autofluorescence 2-photon microscopy, second harmonic generation, and fluorescence lifetime measurements. J. Cataract Refract. Surg. 36, 2150–2159 (2010).
Mastropasqua, L. Collagen cross-linking: when and how? A review of the state of the art of the technique and new perspectives. Eye Vision 2, 19 (2015).
Migus, A., Gauduel, Y., Martin, J. L. & Antonetti, A. Excess electrons in liquid water: first evidence of a prehydrated state with femtosecond lifetime. Phys. Rev. Lett. 58, 1559–1562 (1987).
Nikogosyan, D. N., Oraevsky, A. A. & Rupasov, V. I. Two-photon ionization and dissociation of liquid water by powerful laser UV radiation. J. Chem. Phys. 77, 131–143 (1983).
Keldysh, L. Ionization in the field of a strong electromagnetic wave. J. Exp. Theor. Phys. 20, 1307–1314 (1965).
Williams, F., Varma, S. & Hillenius, S. Liquid water as a lone‐pair amorphous semiconductor. J. Chem. Phys. 64, 1549–1554 (1976).
Kamaev, P., Friedman, M. D., Sherr, E. & Muller, D. Photochemical kinetics of corneal cross-linking with riboflavin. Invest. Ophthalmol. Vis. Sci. 53, 2360–2367 (2012).
Davies, K., Delsignore, M. & Lin, S. Protein damage by oxygen radicals. II. Modification of amino acids. J. Biol. Chem. 262, 9902–9907 (1987).
Meek, K. M. & Hayes, S. Corneal cross-linking—a review. Ophthalmic Physiol. Opt. 33, 78–93 (2013).
Shen, H. R., Spikes, J. D., Smith, C. J. & Kopecek, J. Photodynamic cross-linking of proteins: V. Nature of the tyrosine–tyrosine bonds formed in the FMN-sensitized intermolecular cross-linking of N-acetyl-l-tyrosine. J. Photochem. Photobiol. 133, 115–122 (2000).
Park, C. Y., Lee, J. K. & Chuck, R. S. Second harmonic generation imaging analysis of collagen arrangement in human cornea. Invest. Ophthalmol. Vis. Sci. 56, 5622–5629 (2015).
Wang, C. et al. A new paradigm for use of utrafast lasers in ophthalmology for enhancement of corneal mechanical properties and permanent correction of refractive errors. Proc. SPIE 10066, 100660Y (2017).
del Buey, M. A., Lanchares, E., Cristóbal, J. Á., Gotor, C. Y. & Calvo, B. Immediate effect of ultraviolet-A collagen cross-linking therapy on the biomechanics and histology of the human cornea. J. Refract. Surg. 31, 70–71 (2015).
Alhayek, A. & Lu, P. R. Corneal collagen crosslinking in keratoconus and other eye disease. Int. J. Ophthalmol. 8, 407 (2015).
Mazzotta, C. et al. Treatment of progressive keratoconus by riboflavin-UVA-induced cross-linking of corneal collagen: ultrastructural analysis by Heidelberg Retinal Tomograph II in vivo confocal microscopy in humans. Cornea 26, 390–397 (2007).
Wollensak, G., Iomdina, E., Dittert, D. D. & Herbst, H. Wound healing in the rabbit cornea after corneal collagen cross-linking with riboflavin and UVA. Cornea 26, 600–605 (2007).
Wollensak, G., Spoerl, E., Wilsch, M. & Seiler, T. Endothelial cell damage after riboflavin–ultraviolet-A treatment in the rabbit. J. Cataract Refract. Surg. 29, 1786–1790 (2003).
Kim, S., Cha, D., Song, Y. B., Choi, J. Y. & Han, Y. K. Effects of senofilcon A mechanical protector on corneal endothelial cells during phacoemulsification in rabbit eyes: pilot study. J. Cataract Refract. Surg. 43, 394–399 (2017).
Kymionis, G. D. et al. Corneal collagen cross-linking with riboflavin and ultraviolet-A irradiation in patients with thin corneas. Am. J. Ophthalmol. 153, 24–28 (2012).
Spoerl, E., Mrochen, M., Sliney, D., Trokel, S. & Seiler, T. Safety of UVA–riboflavin cross-linking of the cornea. Cornea 26, 385–389 (2007).
Schindelin, J. et al. Fiji: an open-source platform for biological-image analysis. Nat. Methods 9, 676–682 (2012).
Petroll, W. M., Boettcher, K., Barry, P., Cavanagh, H. D. & Jester, J. V. Quantitative assessment of anteroposterior keratocyte density in the normal rabbit cornea. Cornea 14, 3–9 (1995).
Twa, M. D. & Giese, M. J. Assessment of corneal thickness and keratocyte density in a rabbit model of laser in situ keratomileusis using scanning laser confocal microscopy. Am. J. Ophthalmol. 152, 941–953 (2011).
Liang, H. et al. In vivo confocal microscopy and ex vivo flow cytometry: new tools for assessing ocular inflammation applied to rabbit lipopolysaccharide-induced conjunctivitis. Mol. Vis. 12, 1392–1402 (2006).
Mantopoulos, D., Cruzat, A. & Hamrah, P. Semin. Ophthalmol. 25, 178–185 (2010).
Lagali, N. et al. Confocal Laser Microscopy—Principles and Applications in Medicine, Biology, and the Food Sciences (InTech Open Limited, London, 2013).
Gupta, P. et al. Depth resolved differences after corneal crosslinking with and without epithelial debridement using multimodal imaging. Transl. Vis. Sci. Technol. 3, 5 (2014).
Van Horn, D. L., Sendele, D. D., Seideman, S. & Buco, P. J. Regenerative capacity of the corneal endothelium in rabbit and cat. Invest. Ophthalmol. Vis. Sci. 16, 597–613 (1977).
Wollensak, G. & Iomdina, E. Biomechanical and histological changes after corneal crosslinking with and without epithelial debridement. J. Cataract Refract. Surg. 35, 540–546 (2009).
Davis, F. A. The anatomy and histology of the eye and orbit of the rabbit. Trans. Am. Ophthalmol. Soc. 27, 400–402 (1929).
Zhang, Z.-Y. et al. Refractive change in the adult rabbit eye after corneal relaxation with the femtosecond laser. BMC Ophthalmol. 14, 8 (2014).
Fagerholm, P. Wound healing after photorefractive keratectomy. J. Cataract Refract. Surg. 26, 432–447 (2000).
Shojaei, A. et al. Short-time mitomycin-C application during photorefractive keratectomy in patients with low myopia. J. Cataract Refract. Surg. 39, 197–203 (2013).
Zhivov, A., Stachs, O., Stave, J. & Guthoff, R. F. In vivo three-dimensional confocal laser scanning microscopy of corneal surface and epithelium. Br. J. Ophthalmol. 93, 667–672 (2009).
Dalle-Donne, I., Milzani, A. & Colombo, R. Fluorometric detection of dityrosine coupled with HPLC separation for determining actin oxidation. Am. Biotechnol. Lab. 19, 34–39 (2001).
Takaoka, A. et al. An evaluation of lysyl oxidase-derived cross-linking in keratoconus by liquid chromatography/mass spectrometry. Invest. Ophthalmol. Vis. Sci. 57, 126–136 (2016).
Morishige, N. et al. Quantitative analysis of collagen lamellae in the normal and keratoconic human cornea by second harmonic generation imaging microscopy. Invest. Ophthalmol. Vis. Sci. 55, 8377–8385 (2014).
Acknowledgements
This research was partly funded by the Wallace H. Coulter Foundation. The authors thank S. Trokel for helpful discussions and comments on the manuscript, D. Paik for allowing us to use the equipment in his laboratory, J. Yu, F. Ji, C. Diao and J. Fan for assisting with laser treatment, the experimental set-up and figure preparation, D. Bian for performing the refractive index measurements, and W.D.A.M. De Boer and W. Yang for running TPF experiments. The authors also thank S. Jockusch for help with running EPR spectroscopy experiments. The authors acknowledge Fundação para a Ciência e Tecnologia (FCT) projects PTDC/SAU-ENB/122128/2010 and PEST-C/SAU/UI3282/2013 and COMPETE programmes FCOMP-01-0124-FEDER-021163 and FCOMP-01-0124-FEDER-037299 for support for the multiphoton microscopy equipment. The authors thank JenLab GmbH for providing the required equipment and A. Kaiser for transporting the pig eyes.
Author information
Authors and Affiliations
Contributions
C.W. and S.V. designed the ex vivo and in vivo treatments, as well as tissue culturing studies. C.W. performed these experiments. M.F., G.M. and M.Z. assisted C.W. with the characterization. M.F. and S.V. designed the ROS trapping experiment, tyrosine crosslinking and SHG analysis of treated corneal tissue. M.F. performed the experiments, and C.W. assisted. M.Z. performed the in vivo CLSM measurements, and C.W. analysed them. C.W. and G.M. built the experimental set-up. S.V. initiated, designed and supervised the project. C.W., M.F. and S.V. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary discussion; Supplementary data; Supplementary Figures 1–12; Supplementary References 1–12.
Rights and permissions
About this article
Cite this article
Wang, C., Fomovsky, M., Miao, G. et al. Femtosecond laser crosslinking of the cornea for non-invasive vision correction. Nature Photon 12, 416–422 (2018). https://doi.org/10.1038/s41566-018-0174-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41566-018-0174-8
This article is cited by
-
Effects of corneal crosslinking on corneal shape stabilization after orthokeratology
Scientific Reports (2020)