Abstract
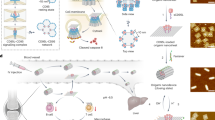
Microporous annealed particle (MAP) scaffolds are flowable, in situ crosslinked, microporous scaffolds composed of microgel building blocks and were previously shown to accelerate wound healing. To promote more extensive tissue ingrowth before scaffold degradation, we aimed to slow MAP degradation by switching the chirality of the crosslinking peptides from l- to d-amino acids. Unexpectedly, despite showing the predicted slower enzymatic degradation in vitro, d-peptide crosslinked MAP hydrogel (d-MAP) hastened material degradation in vivo and imparted significant tissue regeneration to healed cutaneous wounds, including increased tensile strength and hair neogenesis. MAP scaffolds recruit IL-33 type 2 myeloid cells, which is amplified in the presence of d-peptides. Remarkably, d-MAP elicited significant antigen-specific immunity against the d-chiral peptides, and an intact adaptive immune system was required for the hydrogel-induced skin regeneration. These findings demonstrate that the generation of an adaptive immune response from a biomaterial is sufficient to induce cutaneous regenerative healing despite faster scaffold degradation.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding authors upon reasonable request. Source data are provided with this paper.
References
Griffin, D. R., Weaver, W. M., Scumpia, P., Di Carlo, D. & Segura, T. Accelerated wound healing by injectable microporous gel scaffolds assembled from annealed building blocks. Nat. Mater. 14, 737–744 (2015).
Nih, L. R., Sideris, E., Carmichael, S. T. & Segura, T. Injection of microporous annealing particle (MAP) hydrogels in the stroke cavity reduces gliosis and inflammation and promotes NPC migration to the lesion. Adv. Mater. 29, 1606471 (2017).
Xu, Q. et al. Injectable hyperbranched poly(β-amino ester) hydrogels with on-demand degradation profiles to match wound healing processes. Chem. Sci. 9, 2179–2187 (2018).
Zhu, S., Nih, L., Carmichael, S. T., Lu, Y. & Segura, T. Enzyme-responsive delivery of multiple proteins with spatiotemporal control. Adv. Mater. 27, 3620–3625 (2015).
Sela, M. & Zisman, E. Different roles of d-amino acids in immune phenomena. FASEB J. 11, 449–456 (1997).
Doloff, J. C. et al. Colony stimulating factor-1 receptor is a central component of the foreign body response to biomaterial implants in rodents and non-human primates. Nat. Mater. 16, 671–680 (2017).
Mishra, P. K. et al. Sterile particle-induced inflammation is mediated by macrophages releasing IL-33 through a Bruton’s tyrosine kinase-dependent pathway. Nat. Mater. 18, 289–297 (2019).
Chung, L., Maestas, D. R., Housseau, F. & Elisseeff, J. H. Key players in the immune response to biomaterial scaffolds for regenerative medicine. Adv. Drug Deliv. Rev. 114, 184–192 (2017).
Sadtler, K. et al. Developing a pro-regenerative biomaterial scaffold microenvironment requires T helper 2 cells. Science 352, 366–370 (2016).
Galiano, R. D., Michaels, J., Dobryansky, M., Levine, J. P. & Gurtner, G. C. Quantitative and reproducible murine model of excisional wound healing. Wound Repair Regen 12, 485–492 (2004).
Ito, M. et al. Wnt-dependent de novo hair follicle regeneration in adult mouse skin after wounding. Nature 447, 316–320 (2007).
Seifert, A. W. et al. Skin shedding and tissue regeneration in African spiny mice (Acomys). Nature 489, 561–565 (2012).
Nelson, A. M. et al. dsRNA released by tissue damage activates TLR3 to drive skin regeneration. Cell Stem Cell 17, 139–151 (2015).
Guerrero-Juarez, C. F. et al. Wound regeneration deficit in rats correlates with low morphogenetic potential and distinct transcriptome profile of epidermis. J. Invest. Dermatol. 138, 1409–1419 (2018).
Marshall, C. D. et al. Sanativo wound healing product does not accelerate reepithelialization in a mouse cutaneous wound healing model. Plast. Reconstr. Surg. 139, 343–352 (2017).
Lim, C. H. et al. Hedgehog stimulates hair follicle neogenesis by creating inductive dermis during murine skin wound healing. Nat. Commun. 9, 4903 (2018).
Carlson, M. A. & Chakkalakal, D. Tensile properties of the murine ventral vertical midline incision. PLoS ONE 6, e24212 (2011).
Plikus, M. V. et al. Regeneration of fat cells from myofibroblasts during wound healing. Science 355, 748–752 (2017).
Guerrero-Juarez, C. F. et al. Single-cell analysis reveals fibroblast heterogeneity and myeloid-derived adipocyte progenitors in murine skin wounds. Nat. Commun. 10, 650 (2019).
Warren, K. S. A functional classification of granulomatous inflammation. Ann. NY Acad. Sci. 278, 7–18 (1976).
Chensue, S. W. et al. Cytokine responses during mycobacterial and schistosomal antigen-induced pulmonary granuloma formation. Production of Th1 and Th2 cytokines and relative contribution of tumor necrosis factor. Am. J. Pathol. 145, 1105–1113 (1994).
Wills-Karp, M. et al. Trefoil factor 2 rapidly induces interleukin 33 to promote type 2 immunity during allergic asthma and hookworm infection. J. Exp. Med. 209, 607–622 (2012).
Hardman, C. S., Panova, V. & McKenzie, A. N. J. IL-33 citrine reporter mice reveal the temporal and spatial expression of IL-33 during allergic lung inflammation. Eur. J. Immunol. 43, 488–498 (2013).
de Kouchkovsky, D. A., Ghosh, S. & Rothlin, C. V. Induction of sterile type 2 inflammation. Nat. Mater. 18, 193–194 (2019).
Koh, J. et al. Enhanced in vivo delivery of stem cells using microporous annealed particle scaffolds. Small 15, e1903147 (2019).
Purbey, P. K. et al. Defined sensing mechanisms and signaling pathways contribute to the global inflammatory gene expression output elicited by ionizing radiation. Immunity 47, 421–434 (2017).
Scumpia, P. O. et al. Opposing roles of Toll-like receptor and cytosolic DNA-STING signaling pathways for Staphylococcus aureus cutaneous host defense. PLoS Pathog. 13, e1006496 (2017).
Tong, A.-J. et al. A stringent systems approach uncovers gene-specific mechanisms regulating inflammation. Cell 165, 165–179 (2016).
Kim, S. D. et al. The agonists of formyl peptide receptors prevent development of severe sepsis after microbial infection. J. Immunol. 185, 4302–4310 (2010).
Kang, H. K. et al. The synthetic peptide Trp-Lys-Tyr-Met-Val-d-Met inhibits human monocyte-derived dendritic cell maturation via formyl peptide receptor and formyl peptide receptor-like 2. J. Immunol. 175, 685–692 (2005).
Schepetkin, I. A. et al. 3-(1 H-indol-3-yl)-2-[3-(4-nitrophenyl)ureido]propanamide enantiomers with human formyl-peptide receptor agonist activity: molecular modeling of chiral recognition by FPR2. Biochem. Pharmacol. 85, 404–416 (2013).
Zisman, E., Dayan, M., Sela, M. & Mozes, E. Ia-antigen–T-cell interactions for a thymus-independent antigen composed of d amino acids. Proc. Natl Acad. Sci. USA 90, 994–998 (1993).
Cernysiov, V., Gerasimcik, N., Mauricas, M. & Girkontaite, I. Regulation of T-cell-independent and T-cell-dependent antibody production by circadian rhythm and melatonin. Int. Immunol. 22, 25–34 (2010).
Honda, S. et al. Enhanced humoral immune responses against T-independent antigens in Fc alpha/muR-deficient mice. Proc. Natl Acad. Sci. USA 106, 11230–11235 (2009).
Mongini, P. K., Stein, K. E. & Paul, W. E. T cell regulation of IgG subclass antibody production in response to T-independent antigens. J. Exp. Med. 153, 1–12 (1981).
Weinstein, J. S. et al. Maintenance of anti-Sm/RNP autoantibody production by plasma cells residing in ectopic lymphoid tissue and bone marrow memory B cells. J. Immunol. 190, 3916–3927 (2013).
Germann, T. et al. Interleukin-12 profoundly up-regulates the synthesis of antigen-specific complement-fixing IgG2a, IgG2b and IgG3 antibody subclasses in vivo. Eur. J. Immunol. 25, 823–829 (1995).
Boehler, R. M., Graham, J. G. & Shea, L. D. Tissue engineering tools for modulation of the immune response. BioTechniques 51, 239–254 (2011).
Song, J. et al. A mouse model for the human pathogen Salmonella typhi. Cell Host Microbe 8, 369–376 (2010).
Park, C. G. et al. Extended release of perioperative immunotherapy prevents tumor recurrence and eliminates metastases. Sci. Transl. Med. 10, eaar1916 (2018).
Kim, J. et al. Injectable, spontaneously assembling, inorganic scaffolds modulate immune cells in vivo and increase vaccine efficacy. Nat. Biotechnol. 33, 64–72 (2015).
Ramirez-Carrozzi, V. R. et al. A unifying model for the selective regulation of inducible transcription by CpG islands and nucleosome remodeling. Cell 138, 114–128 (2009).
Acknowledgements
We thank the National Institutes of Health F32EB018713-01A1 (D.R.G.), T32-GM008042 (M.M.A.), T32AR071307 (M.M.A), U01AR073159 (M.V.P.), R01NS094599 (T.S.), R01HL110592 (T.S.), R03AR073940 (P.O.S.), K08AR066545 (P.O.S.), Pew Charitable Trust (M.V.P.), LEO Foundation (M.V.P.), the National Science Foundation grant DMS1763272, Simons Foundation Grant (594598, QN) (M.V.P.), and the Presidential Early Career Award for Scientists and Engineers (N00014-16-1-2997) (D.D.) for funding. We thank S. C. Lesher-Perez and M. Bogumil for their assistance with MATLAB coding. We thank Y. Liu for assistance with running the endotoxin texts. We also thank the Advanced Light Microscopy and Spectroscopy at California NanoSystems Institute and Electron Microscopy Core Laboratory of the Brain Research Institute at UCLA and, particularly, for the significant help of M. Cilluffo.
Author information
Authors and Affiliations
Contributions
D.R.G., P.O.S. and T.S. conceived the experiments. D.R.G., W.M.W., E.S., M.M.A. and J.K. carried out the microfluidic design and fabrication, and D.D.C. oversaw the microfluidic design and fabrication. D.R.G., M.M.A., C.-H.K., W.M.W, J.S.W., A.C.F., E.S., A.R., V.R. and P.O.S. performed the experiments. D.R.G., M.M.A., J.S.W., A.R., M.V.P., T.S. and P.O.S. analysed and interpreted the data. D.R.G., M.M.A., P.O.S. and T.S. wrote the manuscript and all the authors discussed the results and contributed to writing portions of the manuscript and editing the manuscript. D.R.G. and M.M.A. contributed equally to this work. The co-principal investigators are P.O.S. and T.S.
Corresponding authors
Ethics declarations
Competing interests
D.R.G., W.M.W., D.D.C., T.S., and P.O.S. have a financial interest in Tempo Therapeutics, which aims to commercialize MAP technology.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Figs. 1–5 and Supplementary Notes.
Source data
Source Data Fig. 1
Raw data for gel degradation and wound characterization.
Source Data Fig. 2
Figure 2 replicate images.
Source Data Fig. 3
Source data for cell infiltration and gene expression.
Source Data Fig. 4
Source data for antibody production and cell infiltration.
Source Data Fig. 5
Source data for wound characterization.
Source Data Supplementary Fig 2
Assessment of wound size.
Source Data Supplementary Fig 3
Quantification of F4/80+CD11b+ macrophages in the edge of L-MAP and D-MAP implant.
Rights and permissions
About this article
Cite this article
Griffin, D.R., Archang, M.M., Kuan, CH. et al. Activating an adaptive immune response from a hydrogel scaffold imparts regenerative wound healing. Nat. Mater. 20, 560–569 (2021). https://doi.org/10.1038/s41563-020-00844-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41563-020-00844-w
This article is cited by
-
Biomaterial-based mechanical regulation facilitates scarless wound healing with functional skin appendage regeneration
Military Medical Research (2024)
-
Senescent fibroblast facilitates re-epithelization and collagen deposition in radiation-induced skin injury through IL-33-mediated macrophage polarization
Journal of Translational Medicine (2024)
-
Nanoconfined polymerization limits crack propagation in hysteresis-free gels
Nature Materials (2024)
-
Modelling and targeting mechanical forces in organ fibrosis
Nature Reviews Bioengineering (2024)
-
Monolithic-to-focal evolving biointerfaces in tissue regeneration and bioelectronics
Nature Chemical Engineering (2024)