Abstract
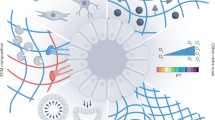
Bioprinting promises enormous control over the spatial deposition of cells in three dimensions1,2,3,4,5,6,7, but current approaches have had limited success at reproducing the intricate micro-architecture, cell-type diversity and function of native tissues formed through cellular self-organization. We introduce a three-dimensional bioprinting concept that uses organoid-forming stem cells as building blocks that can be deposited directly into extracellular matrices conducive to spontaneous self-organization. By controlling the geometry and cellular density, we generated centimetre-scale tissues that comprise self-organized features such as lumens, branched vasculature and tubular intestinal epithelia with in vivo-like crypts and villus domains. Supporting cells were deposited to modulate morphogenesis in space and time, and different epithelial cells were printed sequentially to mimic the organ boundaries present in the gastrointestinal tract. We thus show how biofabrication and organoid technology can be merged to control tissue self-organization from millimetre to centimetre scales, opening new avenues for drug discovery, diagnostics and regenerative medicine.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The datasets supporting the conclusions of this article are included within the article and its additional files. Source data are provided with this paper.
References
Murphy, S. V. & Atala, A. 3D bioprinting of tissues and organs. Nat. Biotechnol. 32, 773–785 (2014).
Liu, W. et al. Rapid continuous multimaterial extrusion bioprinting. Adv. Mater. 29, 1604630 (2017).
Keriquel, V. et al. In situ printing of mesenchymal stromal cells, by laser-assisted bioprinting, for in vivo bone regeneration applications. Sci. Rep. 7, 1778 (2017).
Hinton, T. J. et al. Three-dimensional printing of complex biological structures by freeform reversible embedding of suspended hydrogels. Sci. Adv. 1, e1500758–e1500758 (2015).
Lee, A. et al. 3D bioprinting of collagen to rebuild components of the human heart. Science 365, 482–487 (2019).
Bhattacharjee, T. et al. Writing in the granular gel medium. Sci. Adv. 1, e1500655–e1500655 (2015).
Highley, C. B., Rodell, C. B. & Burdick, J. A. Direct 3D printing of shear-thinning hydrogels into self-healing hydrogels. Adv. Mater. 27, 5075–5079 (2015).
Jamal, M. et al. Bio-origami hydrogel scaffolds composed of photocrosslinked PEG bilayers. Adv. Healthc. Mater. 2, 1142–1150 (2013).
Villar, G., Graham, A. D. & Bayley, H. A tissue-like printed material. Science 340, 48–52 (2013).
Clevers, H. Modeling development and disease with organoids. Cell 165, 1586–1597 (2016).
Lancaster, M. A. & Knoblich, J. A. Organogenesis in a dish: modeling development and disease using organoid technologies. Science 345, 1247125–1247125 (2014).
Laurent, J. et al. Convergence of microengineering and cellular self-organization towards functional tissue manufacturing. Nat. Biomed. Eng. 1, 939 (2017).
Brassard, J. A. & Lutolf, M. P. Engineering stem cell self-organization to build better organoids. Cell Stem Cell 24, 860–876 (2019).
Sato, T. et al. Long-term expansion of epithelial organoids from human colon, adenoma, adenocarcinoma, and Barrett’s epithelium. Gastroenterology 141, 1762–1772 (2011).
Blatchley, M. R. & Gerecht, S. Reconstructing the vascular developmental milieu in vitro. Trends Cell Biol. 30, 15–31 (2020).
Sato, T. et al. Single Lgr5 stem cells build crypt-villus structures in vitro without a mesenchymal niche. Nature 459, 262 (2009).
Sato, T. et al. Paneth cells constitute the niche for Lgr5 stem cells in intestinal crypts. Nature 469, 415–418 (2011).
Es, J. Hvan et al. Enteroendocrine and tuft cells support Lgr5 stem cells on Paneth cell depletion. Proc. Natl Acad. Sci. USA 116, 26599–26605 (2019).
Yokoi, Y. et al. Paneth cell granule dynamics on secretory responses to bacterial stimuli in enteroids. Sci. Rep. 9, 2710 (2019).
Dekkers, J. F. et al. A functional CFTR assay using primary cystic fibrosis intestinal organoids. Nat. Med. 19, 939–945 (2013).
Wells, J. M. & Spence, J. R. How to make an intestine. Development 141, 752–760 (2014).
Stzepourginski, I. et al. CD34+ mesenchymal cells are a major component of the intestinal stem cells niche at homeostasis and after injury. Proc. Natl Acad. Sci. USA 114, E506–E513 (2017).
Farin, H. F., Van Es, J. H. & Clevers, H. Redundant sources of Wnt regulate intestinal stem cells and promote formation of Paneth cells. Gastroenterology 143, 1518–1529.e7 (2012).
Sachs, N., Tsukamoto, Y., Kujala, P., Peters, P. J. & Clevers, H. Intestinal epithelial organoids fuse to form self-organizing tubes in floating collagen gels. Development 144, 1107–1112 (2017).
Reid, J. A., Mollica, P. A., Bruno, R. D. & Sachs, P. C. Consistent and reproducible cultures of large-scale 3D mammary epithelial structures using an accessible bioprinting platform. Breast Cancer Res. 20, 122 (2018).
Muzumdar, M. D., Tasic, B., Miyamichi, K., Li, L. & Luo, L. A global double-fluorescent Cre reporter mouse. Genesis 45, 593–605 (2007).
Bartfeld, S. & Clevers, H. Organoids as model for infectious diseases: culture of human and murine stomach organoids and microinjection of Helicobacter pylori. J. Vis. Exp. https://doi.org/10.3791/53359 (2015).
Miyoshi, H. & Stappenbeck, T. S. In vitro expansion and genetic modification of gastrointestinal stem cells as organoids. Nat Protoc. 8, 2471–2482 (2013).
Koliaraki, V. & Kollias, G. Isolation of intestinal mesenchymal cells from adult mice. Bio-Protocol 6, e1940 (2016).
Acknowledgements
We thank N. Gjorevski and A. Martinez Arias for valuable feedback on the manuscript. We thank S. Li and D. Dutta for deriving organoid lines from intestinal tissues of mTmG and Lys-dsRED reporter mice, respectively. We thank O. Mitrofanova for help with human intestinal organoid culture and tube printing, S. Giger for providing hMSCs and A. Manfrin and A. Chrisnandy for the qPCR primers for intestinal genes. We thank R. Guiet and O. Burri from EPFL’s BioImaging and Optics Platform for help with intestinal tube analysis. We thank J. van Es and H. Clevers for providing intestinal tissues of Lys-dsRED reporter mice and J. McKinney for providing intestinal tissues of mTmG reporter mice. This work was funded by support from the EU Horizon 2020 Project INTENS (no. 668294-2), the Swiss National Science Foundation research grant no. 310030_179447, the National Center of Competence in Research (NCCR) ‘Bio-Inspired Materials’ (https://www.bioinspired-materials.ch/), the PHRT-PM/PH Research Project Proposal 2017, the Wellcome Trust Collaborative Award 211944/Z/18/Z, and EPFL.
Author information
Authors and Affiliations
Contributions
M.P.L. and M.N. conceived the initial idea. J.A.B., M.N., T.H. and M.P.L. conceived the study, designed experiments and analysed the data. M.P.L. and J.A.B. wrote the manuscript. T.H. performed multi-gastrointestinal cell-type printing. M.H. was involved in performing and analysing stomach tube printing experiments. All authors provided feedback on the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Bioprinter set-up and proof-of-concept.
Picture of the nozzle to be mounted on the microscope. The nozzle after pulling and breaking of the tip has a long taper and a clear cut. Scale bar, 200 µm. b, Printing with beads showing that resolution and printing thickness can be modulated by changing the nozzle size or (c) the speed of the stage movement. Images are representative of n = 3 independent experiments. Scale bars, 200 µm. d, Printing with HUVECs showing that resolution and cell density can be controlled by modifying the flow rate (syringe-based extrusion) or the printing speed (stage movement). Images are representative of n = 3 biologically independent experiments. Scale bar, 200 µm. e, Viability of C2C12 (circles) and HUVECs (squares) right after printing and 24 hours later. Data represented as percentage of live cells for three replicates (n = 3 biologically independent experiments), with the mean for each condition shown as a dotted line.
Extended Data Fig. 2 Printing human intestinal tubes.
Bright-field images showing the evolution of human intestinal stem cells printed as a line. Differentiation medium promotes the rapid formation of a continuous lumen. Increasing the matrix stiffness, by addition of collagen in the support hydrogel, allows to maintain the printed geometry better, preventing collapse of the tube due to cell-mediated matrix remodelling. Images are representative of n = 3 biologically independent experiments. Scale bars, 500 µm.
Extended Data Fig. 3 BATE of colon and stomach epithelial tubes from mouse and human primary cells.
a, Bright-field images of tube evolution from human and (b) mouse colon stem cells and (c) mouse stomach stem cells. In all cases, a thick tubular epithelium is formed by colony growth and fusion at high density. Images are representative of n = 3 biologically independent experiments. Scale bars, 500 µm.
Extended Data Fig. 4 BATE of vascular endothelial tubes.
a, Evolution of a printed line of HUVECs, showing rapid reorganization into an endothelial tube with a single macroscopic lumen. Images are representative of n = 3 biologically independent experiments. Scale bars, 500 µm. b, Different geometries can be printed to form branched vascular tubes and other complex structures. Images are representative of n = 3 biologically independent experiments. Scale bar, 1000 µm. c, Bright-field and fluorescent images showing vascular tube perfusion with fluorescently labelled dextran (2000 kDa) or fluorescently labelled beads (0.1 µm). Images are representative of n = 3 biologically independent experiments. Scale bars, 1000 µm.
Extended Data Fig. 5 Induction of angiogenesis in bioprinted vascular tubes.
a, Evolution of a printed vascular tube exposed to high VEGF concentration. Many capillaries are formed de novo while maintaining the continuous lumen. Scale bars, 250 µm. b, Evolution of a printout with straight angles showing good conservation of the printing geometry over time. Scale bar, 1000 µm. c, Complex geometries can also be printed, resulting in branched vascular networks with strong angiogenesis potential. Scale bar, 1000 µm. d, Bright-field images showing the evolution of printed vascular tube with addition of VEGF at different time points. Angiogenesis can be triggered at a desired time, promoting formation of capillaries that can connect with other tubes. Images are representative of n = 3 biologically independent experiments. Scale bar, 1000 µm.
Extended Data Fig. 6 Intestinal tube morphogenesis: influence of collagen content in the support hydrogel.
Addition of collagen I increases the stiffness of the support hydrogel, limiting extensive budding of the tubes. Of note: when the gel is disrupted, budding can occur even at later time points also for initially stiffer hydrogels. Images are representative of n = 3 biologically independent experiments. Scale bars, 200 µm.
Extended Data Fig. 7 Intestinal epithelial tube staining.
a, Confocal fluorescent images showing the formation of a continuous lumen by colony fusion. Images are representative of n = 3 biologically independent experiments. Scale bars, 100 µm. b, Staining of the intestinal tubes after six days of culture. Proliferation (EdU, left) and Paneth cells (Lyz, right) are restricted to the crypt-like structures whereas enterocytes (LFAB, middle) are found on flatter surfaces. Images are representative of n = 3 biologically independent experiments. Scale bars, 100 µm. c, fluorescent image of LGR5-eGFP and corresponding bright-field image of a tube after seven days, showing darker Paneth cells intercalated in between stem cells inside the crypts. Note that the autofluorescence of dead cells in the lumen does not overlap with the intact epithelium in the merged picture. Images are representative of n = 3 biologically independent experiments. Scale bars, 100 µm.
Extended Data Fig. 8 Influence of printing cell density on tube formation and diameter.
a, Representative tube printed from small intestinal organoids (that is not single cells). Top: 1 hour after printing, Middle: 72h after printing, Bottom: staining (Dapi labelling the nuclei, Actin) of the tube showing a lumen and crypt structures. Scale bars, 200 µm. b, Change of mean tube diameter over time at three different cell densities: 12,5 million (white symbol), 25 million (white and black symbol) and 50 million (black symbol) cells/ml. The experiment was repeated three times and two tubes are shown for each cell density. c, Evolution over time of one representative tube for each initial cell density from one of the three experiment is shown. Scale bars, 1000 µm.
Extended Data Fig. 9 Effect of IMC co-culture in bioprinted intestinal tubes.
a, Bright-field images and corresponding fluorescent images of Lgr5-eGFP three days after printing, showing the effect of IMC co-culture on tube formation. IMCs were either deposited after printing for adherence on the well bottom and hydrogel (left), or directly suspended inside the hydrogel before and during printing (right). In all cases, a continuous lumen was formed after only one day, and the tubes comprise many Lgr5+ buds after 3 days. Images are representative of n = 3 biologically independent experiments. Scale bars, 250 µm. b, Difference in evolution of the tube diameter if co-cultured with IMCs or not. For each day, the mean diameter (dotted line) of tubes with and without myofibroblasts were compared (n=3 tubes for each day).
Extended Data Fig. 10 Continuous epithelial tube composed of mouse small intestine and colon stem cells.
Top: merged (max Z projection) image of the tube in bright-field as well as showing red (mT) and green (Lgr5-eGFP) fluorescent cells, each color being shown separately below. Middle: colon cells expressing mT and intestinal cells expressing Lgr5-eGFP. Bottom: bright-field. Images are representative of n = 3 biologically independent experiments. Scale bar, 1000 µm.
Supplementary information
Supplementary Information
Supplementary Table 1.
Supplementary Video 1
BATE technology. Real-time demonstration of BATE technology, with sequential cellular aspiration and deposition within liquid ECM precursors.
Supplementary Video 2
Angiogenesis of the bioprinted vascular network. Z-stacks of bright-field and fluorescent images showing the morphology of the vascular network, highlighting the formation and maintenance of a continuous lumen in the presence and absence of VEGF supplementation. The stacks also show connections between different vascular tube through angiogenesis.
Supplementary Video 3
Intestinal tube morphogenesis. Five-day time-lapse showing the evolution of the intestinal tube. Right after the printing process, cells condense into a tightly packed line before starting to polarize and giving rise to Paneth cell emergence and subsequent budding formation.
Supplementary Video 4
Matrix softening promotes intestinal crypt morphogenesis. Three-day time-lapse showing intestinal crypt morphogenesis after treatment of the tube with collagenase. Matrix degradation results in homogeneous elongation of budding structure into crypts with darker Paneth cells at the bottom.
Supplementary Video 5
Physiological response to chemical stimuli in intestinal tubes. Carbamylcholine treatment triggers release of lysozyme granules from Paneth cells. Intestinal tubes exposed to Forskolin rapidly swelled, as a response to the activation of the cystic fibrosis transmembrane conductance regulator channels.
Supplementary Video 6
Multicellular self-assembly of intestinal epithelial and stromal cells. Two-day time-lapse showing the evolution of intestinal tube morphogenesis when mouse ISC are printed together with mouse IMCs. Tube formation and lumen genesis are faster. Some IMC migrating at the periphery of the tube can also be seen.
Supplementary Video 7
Large-scale self-organization allows lumen accessibility and perfusion. Demonstration of the perfusion process of the intestinal tube to remove the dead cells that are shed during culture as in the normal turnover of the tissue.
Source data
Figure 4
Source data for Fig. 4m. log10 fold change. Normalized to GAPDH and to organoids in standard culture conditions. Mean of two tubes.
Extended Data Fig. 1
Source data for Extended Data Fig. 1e. Live/dead cell count.
Extended Data Fig. 8
Source data for Extended Data Fig. 8b. Mean tube diameter (μm).
Extended Data Fig. 9
Source data for Extended Data Fig. 9b. Mean tube diameter without or with myofibroblasts (MF) (μm).
Rights and permissions
About this article
Cite this article
Brassard, J.A., Nikolaev, M., Hübscher, T. et al. Recapitulating macro-scale tissue self-organization through organoid bioprinting. Nat. Mater. 20, 22–29 (2021). https://doi.org/10.1038/s41563-020-00803-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41563-020-00803-5
This article is cited by
-
Ultrasound-assisted tissue engineering
Nature Reviews Bioengineering (2024)
-
Gradient matters via filament diameter-adjustable 3D printing
Nature Communications (2024)
-
From Pluripotent Stem Cells to Organoids and Bioprinting: Recent Advances in Dental Epithelium and Ameloblast Models to Study Tooth Biology and Regeneration
Stem Cell Reviews and Reports (2024)
-
From cells to organs: progress and potential in cartilaginous organoids research
Journal of Translational Medicine (2023)
-
Applications of lung cancer organoids in precision medicine: from bench to bedside
Cell Communication and Signaling (2023)