Abstract
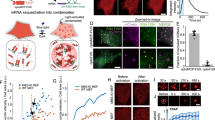
Macrophages respond to chemical/metabolic and physical stimuli, but their effects cannot be readily decoupled in vivo during pro-inflammatory activation. Here, we show that preventing macrophage spreading by spatial confinement, as imposed by micropatterning, microporous substrates or cell crowding, suppresses late lipopolysaccharide (LPS)-activated transcriptional programs (biomarkers IL-6, CXCL9, IL-1β, and iNOS) by mechanomodulating chromatin compaction and epigenetic alterations (HDAC3 levels and H3K36-dimethylation). Mechanistically, confinement reduces actin polymerization, thereby lowers the LPS-stimulated nuclear translocation of MRTF-A. This lowers the activity of the MRTF-A–SRF complex and subsequently downregulates the inflammatory response, as confirmed by chromatin immunoprecipitation coupled with quantitative PCR and RNA sequencing analysis. Confinement thus downregulates pro-inflammatory cytokine secretion and, well before any activation processes, the phagocytic potential of macrophages. Contrarily, early events, including activation of the LPS receptor TLR4, and downstream NF-κB and IRF3 signalling and hence the expression of early LPS-responsive genes were marginally affected by confinement. These findings have broad implications in the context of mechanobiology, inflammation and immunology, as well as in tissue engineering and regenerative medicine.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
Microarray data for HDAC3-KO BMDMs were obtained from ref. 32 and the GEO accession no. is GSE33162. RNA–seq data for Control untreated BMDMs, LPS-treated BMDMs and SRF-KO-LPS-treated BMDMs have been deposited in GEO. The accession codes are GSM3373977–GSM3373979, GSM3373980–GSM3373982 and GSM3373983–GSM3373985 for Control untreated BMDMs, LPS-treated BMDMs and SRF-KO-LPS-treated BMDMs, respectively. The remaining data supporting the findings of this study are available within the Article and its Supplementary Information files and from the corresponding authors upon reasonable request.
References
Mosser, D. M. & Edwards, J. P. Exploring the full spectrum of macrophage activation. Nat. Rev. Immunol. 8, 958–969 (2008).
Glass, C. K. & Natoli, G. Molecular control of activation and priming in macrophages. Nat. Immunol. 17, 26–33 (2016).
Edwards, J. P., Zhang, X., Frauwirth, K. A. & Mosser, D. M. Biochemical and functional characterization of three activated macrophage populations. J. Leukoc. Biol. 80, 1298–1307 (2006).
Lawrence, T. & Natoli, G. Transcriptional regulation of macrophage polarization: enabling diversity with identity. Nat. Rev. Immunol. 11, 750–761 (2011).
Medzhitov, R. & Horng, T. Transcriptional control of the inflammatory response. Nat. Rev. Immunol. 9, 692–703 (2009).
Raza, S. et al. Analysis of the transcriptional networks underpinning the activation of murine macrophages by inflammatory mediators. J. Leukoc. Biol. 96, 167–183 (2014).
Martinez, F. O. & Gordon, S. The M1 and M2 paradigm of macrophage activation: time for reassessment. F1000Prime Rep. 6, 13 (2014).
Lammermann, T. & Germain, R. N. The multiple faces of leukocyte interstitial migration. Semin. Immunopathol. 36, 227–251 (2014).
Makino, A. et al. Mechanotransduction in leukocyte activation: a review. Biorheology 44, 221–249 (2007).
Gruber, E., Heyward, C., Cameron, J. & Leifer, C. Toll-like receptor signaling in macrophages is regulated by extracellular substrate stiffness and Rho-associated coiled-coil kinase (ROCK1/2). Int. Immunol. 30, 267–278 (2018).
Van Goethem, E., Poincloux, R., Gauffre, F., Maridonneau-Parini, I. & Le Cabec, V. Matrix architecture dictates three-dimensional migration modes of human macrophages: differential involvement of proteases and podosome-like structures. J. Immunol. 184, 1049–1061 (2010).
Mennens, S. F. B., van den Dries, K. & Cambi, A. Role for mechanotransduction in macrophage and dendritic cell immunobiology. Results Probl. Cell Differ. 62, 209–242 (2017).
Chen, C. S., Mrksich, M., Huang, S., Whitesides, G. M. & Ingber, D. E. Geometric control of cell life and death. Science 276, 1425–1428 (1997).
Downing, T. L. et al. Biophysical regulation of epigenetic state and cell reprogramming. Nat. Mater. 12, 1154–1162 (2013).
Engler, A. J., Sen, S., Sweeney, H. L. & Discher, D. E. Matrix elasticity directs stem cell lineage specification. Cell 126, 677–689 (2006).
Fu, J. et al. Mechanical regulation of cell function with geometrically modulated elastomeric substrates. Nat. Methods 7, 733–736 (2010).
Vogel, V. & Sheetz, M. Local force and geometry sensing regulate cell functions. Nat. Rev. Mol. Cell Biol. 7, 265–275 (2006).
Huse, M. Mechanical forces in the immune system. Nat. Rev. Immunol. 17, 679–690 (2017).
McWhorter, F. Y., Davis, C. T. & Liu, W. F. Physical and mechanical regulation of macrophage phenotype and function. Cell. Mol. Life Sci. 72, 1303–1316 (2015).
McWhorter, F. Y., Wang, T., Nguyen, P., Chung, T. & Liu, W. F. Modulation of macrophage phenotype by cell shape. Proc. Natl Acad. Sci. USA 110, 17253–17258 (2013).
Shibata, K. et al. Effect of the release from mechanical stress on osteoclastogenesis in RAW264.7 cells. Int. J. Mol. Med. 28, 73–79 (2011).
Sussman, E. M., Halpin, M. C., Muster, J., Moon, R. T. & Ratner, B. D. Porous implants modulate healing and induce shifts in local macrophage polarization in the foreign body reaction. Ann. Biomed. Eng. 42, 1508–1516 (2014).
Chinetti-Gbaguidi, G. et al. Human atherosclerotic plaque alternative macrophages display low cholesterol handling but high phagocytosis because of distinct activities of the PPARɣ and LXRα pathways. Circ. Res. 108, 985–995 (2011).
Stoger, J. L. et al. Distribution of macrophage polarization markers in human atherosclerosis. Atherosclerosis. 225, 461–468 (2012).
Ihalainen, T. O. et al. Differential basal-to-apical accessibility of lamin A/C epitopes in the nuclear lamina regulated by changes in cytoskeletal tension. Nat. Mater. 14, 1252–1261 (2015).
Jain, N., Iyer, K. V., Kumar, A. & Shivashankar, G. V. Cell geometric constraints induce modular gene-expression patterns via redistribution of HDAC3 regulated by actomyosin contractility. Proc. Natl Acad. Sci. USA 110, 11349–11354 (2013).
Mascetti, G., Carrara, S. & Vergani, L. Relationship between chromatin compactness and dye uptake for in situ chromatin stained with DAPI. Cytometry 44, 113–119 (2001).
Xu, G. et al. The histone methyltransferase Smyd2 is a negative regulator of macrophage activation by suppressing interleukin 6 (IL-6) and tumor necrosis factor alpha (TNF-α) production. J. Biol. Chem. 290, 5414–5423 (2015).
Haberland, M., Montgomery, R. L. & Olson, E. N. The many roles of histone deacetylases in development and physiology: implications for disease and therapy. Nat. Rev. Genet. 10, 32–42 (2009).
Das Gupta, K., Shakespear, M. R., Iyer, A., Fairlie, D. P. & Sweet, M. J. Histone deacetylases in monocyte/macrophage development, activation and metabolism: refining HDAC targets for inflammatory and infectious diseases. Clin. Transl. Immunol. 5, e62 (2016).
Shakespear, M. R., Halili, M. A., Irvine, K. M., Fairlie, D. P. & Sweet, M. J. Histone deacetylases as regulators of inflammation and immunity. Trends Immunol. 32, 335–343 (2011).
Chen, X. et al. Requirement for the histone deacetylase Hdac3 for the inflammatory gene expression program in macrophages. Proc. Natl Acad. Sci. USA 109, E2865–E2874 (2012).
Hoeksema, M. A. et al. Targeting macrophage histone deacetylase 3 stabilizes atherosclerotic lesions. EMBO Mol. Med. 6, 1124–1132 (2014).
Chow, J. C., Young, D. W., Golenbock, D. T., Christ, W. J. & Gusovsky, F. Toll-like receptor-4 mediates lipopolysaccharide-induced signal transduction. J. Biol. Chem. 274, 10689–10692 (1999).
Dai, Q. & Pruett, S. B. Ethanol suppresses LPS-induced Toll-like receptor 4 clustering, reorganization of the actin cytoskeleton, and associated TNF-α production. Alcohol. Clin. Exp. Res. 30, 1436–1444 (2006).
Reimer, T., Brcic, M., Schweizer, M. & Jungi, T. W. Poly(I:C) and LPS induce distinct IRF3 and NF-κB signaling during type-I IFN and TNF responses in human macrophages. J. Leukoc. Biol. 83, 1249–1257 (2008).
Connelly, J. T. et al. Actin and serum response factor transduce physical cues from the microenvironment to regulate epidermal stem cell fate decisions. Nat. Cell Biol. 12, 711–718 (2010).
Olson, E. N. & Nordheim, A. Linking actin dynamics and gene transcription to drive cellular motile functions. Nat. Rev. Mol. Cell Biol. 11, 353–365 (2010).
Selvaraj, A. & Prywes, R. Expression profiling of serum inducible genes identifies a subset of SRF target genes that are MKL dependent. BMC Mol. Biol. 5, 13 (2004).
Yu, L. et al. MRTF-A mediates LPS-induced pro-inflammatory transcription by interacting with the COMPASS complex. J. Cell Sci. 127, 4645–4657 (2014).
Xie, L. MKL1/2 and ELK4 co-regulate distinct serum response factor (SRF) transcription programs in macrophages. BMC Genomics 15, 301 (2014).
Sullivan, A. L. et al. Serum response factor utilizes distinct promoter- and enhancer-based mechanisms to regulate cytoskeletal gene expression in macrophages. Mol. Cell. Biol. 31, 861–875 (2011).
Kishi, T., Mayanagi, T., Iwabuchi, S., Akasaka, T. & Sobue, K. Myocardin-related transcription factor A (MRTF-A) activity-dependent cell adhesion is correlated to focal adhesion kinase (FAK) activity. Oncotarget 7, 72113–72130 (2016).
Han, J., Brown, T. & Beutler, B. Endotoxin-responsive sequences control cachectin/tumor necrosis factor biosynthesis at the translational level. J. Exp. Med. 171, 465–475 (1990).
Kruys, V., Marinx, O., Shaw, G., Deschamps, J. & Huez, G. Translational blockade imposed by cytokine-derived UA-rich sequences. Science 245, 852–855 (1989).
MacMicking, J. D. et al. Altered responses to bacterial infection and endotoxic shock in mice lacking inducible nitric oxide synthase. Cell 81, 641–650 (1995).
Gabay, C. Interleukin-6 and chronic inflammation. Arthritis Res. Ther. 8(Suppl. 2), S3 (2006).
Bartneck, M., Heffels, K. H., Bovi, M., Groll, J. & Zwadlo-Klarwasser, G. The role of substrate morphology for the cytokine release profile of immature human primary macrophages. Mater. Sci. Eng. C 33, 5109–5114 (2013).
Wynn, T. A. & Vannella, K. M. Macrophages in tissue repair, regeneration, and fibrosis. Immunity 44, 450–462 (2016).
Brubaker, S. W., Bonham, K. S., Zanoni, I. & Kagan, J. C. Innate immune pattern recognition: a cell biological perspective. Annu. Rev. Immunol. 33, 257–290 (2015).
Jain, N., Iyer, K. V., Kumar, A. & Shivashankar, G. V. Cell geometric constraints induce modular gene-expression patterns via redistribution of HDAC3 regulated by actomyosin contractility. Proc. Natl Acad. Sci. USA 110, 11349–11354 (2013).
Kishi, T., Mayanagi, T., Iwabuchi, S., Akasaka, T. & Sobue, K. Myocardin-related transcription factor A (MRTF-A) activity-dependent cell adhesion is correlated to focal adhesion kinase (FAK) activity. Oncotarget 7, 72113–72130 (2016).
Fang, F. et al. Myocardin-related transcription factor A mediates OxLDL-induced endothelial injury. Circ. Res. 108, 797–807 (2011).
O’Sullivan, N. C., Pickering, M., Di Giacomo, D., Loscher, J. S. & Murphy, K. J. Mkl transcription cofactors regulate structural plasticity in hippocampal neurons. Cereb. Cortex 20, 1915–1925 (2010).
John, G. R. et al. Interleukin-1β induces a reactive astroglial phenotype via deactivation of the Rho GTPase-Rock axis. J. Neurosci. 24, 2837–2845 (2004).
Kamijo, K. et al. Dissecting the role of Rho-mediated signaling in contractile ring formation. Mol. Biol. Cell 17, 43–55 (2006).
Bardai, F. H. & D’Mello, S. R. Selective toxicity by HDAC3 in neurons: regulation by Akt and GSK3β. J. Neurosci. 31, 1746–1751 (2011).
de la Vega, L. et al. A redox-regulated SUMO/acetylation switch of HIPK2 controls the survival threshold to oxidative stress. Mol. Cell 46, 472–483 (2012).
Montgomery, R. L. et al. Histone deacetylases 1 and 2 redundantly regulate cardiac morphogenesis, growth, and contractility. Genes Dev. 21, 1790–1802 (2007).
Clement, M. et al. CD31 is a key coinhibitory receptor in the development of immunogenic dendritic cells. Proc. Natl Acad. Sci. USA 111, E1101–E1110 (2014).
Yim, N. et al. Exosome engineering for efficient intracellular delivery of soluble proteins using optically reversible protein–protein interaction module. Nat. Commun. 7, 12277 (2016).
Avalos Vizcarra, I. et al. How type 1 fimbriae help Escherichia coli to evade extracellular antibiotics. Sci. Rep. 6, 18109 (2016).
Bolger, A. M., Lohse, M. & Usadel, B. Trimmomatic: a flexible trimmer for Illumina sequence data. Bioinformatics 30, 2114–2120 (2014).
Dobin, A. et al. STAR: ultrafast universal RNA–seq aligner. Bioinformatics 29, 15–21 (2013).
Lawrence, M. et al. Software for computing and annotating genomic ranges. PLoS Comput. Biol. 9, e1003118 (2013).
Robinson, M. D., McCarthy, D. J. & Smyth, G. K. edgeR: a Bioconductor package for differential expression analysis of digital gene expression data. Bioinformatics 26, 139–140 (2010).
Huang da, W., Sherman, B. T. & Lempicki, R. A. Systematic and integrative analysis of large gene lists using DAVID bioinformatics resources. Nat. Protoc. 4, 44–57 (2009).
Acknowledgements
The authors thank A. Oxenius and the Mice Facility both at ETH Zurich for donating postmortem animals for bone marrow isolation, S. Farmer (Boston University) for providing bone marrow from MRTF-A-KO mice and for helpful discussions, S. Halene (Animal Modeling Core, Yale Cooperative Center of Excellence in Hematology (YCCEH) NIDDK grant no. U54DK106857, Yale University) for providing bone marrow from SRF-KO mice, and K. Sobue and T. Mayanagi (Iwaka Medical University) for providing CA-MRTF-A plasmid. The authors thank G. V. Shivashankar (MBI, NUS, Singapore) for providing HDAC3-overexpressing plasmid, L. Philipp and U. Kutay (ETH Zurich) and M. O. Hottiger (University of Zurich) for helpful discussions on ChIP experiments. In the Vogel group, I. A. Vizcarra is acknowledged for initial help with BMDM culture, J.-Y. Shiu and V. Hosseini for their advice and the manufacturing of 3D-microwells, C. Spencer for technical support, I. Gerber for acquiring the electron microscopy images, L. A. Branco and I. Schoen for critical comments on the manuscript and finally the FIRST and ScopeM facilities at ETH Zurich for access to microfabrication and confocal microscopy. This work was supported by ETH Zurich and by the Swiss National Science Foundation Grant (grant no. CR32I3_156931 to V.V.) and also in part by the Swiss NCCR Molecular Systems Engineering.
Author information
Authors and Affiliations
Contributions
N.J. and V.V. conceived of the project. N.J designed and performed the experiments. N.J. and V.V. analysed the data and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Video Legends 1–5, Supplementary Figures 1–22, Supplementary Tables 1,2, Supplementary Reference 1
Supplementary Data 1
HDAC3-KO microarray analysis
Supplementary Data 2
Gene ontology analysis of control LPS-treated BMDMs versus control untreated BMDMs
Supplementary Data 3
RNA-Seq analysis and gene ontology analysis of SRF-KO LPS-treated BMDMs versus control LPS-treated BMDMs
Supplementary Video 1
Spreading of control BMDMs
Supplementary Video 2
Spreading of LPS-treated BMDMs
Supplementary Video 3
Spreading of IL-4/IL-13-treated BMDMs
Supplementary Video 4
3D reconstruction of unconfined (UC) BMDM treated with LPS for 6 h and stained for nuclei, F-actin, G-actin and MRTF-A
Supplementary Video 5
3D reconstruction of confined (CC) BMDMs treated with LPS for 6 h and stained for nuclei, F-actin, G-actin and MRTF-A
Rights and permissions
About this article
Cite this article
Jain, N., Vogel, V. Spatial confinement downsizes the inflammatory response of macrophages. Nature Mater 17, 1134–1144 (2018). https://doi.org/10.1038/s41563-018-0190-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41563-018-0190-6
This article is cited by
-
Nanotube patterning reduces macrophage inflammatory response via nuclear mechanotransduction
Journal of Nanobiotechnology (2023)
-
Cell–extracellular matrix mechanotransduction in 3D
Nature Reviews Molecular Cell Biology (2023)
-
Tuning immunity through tissue mechanotransduction
Nature Reviews Immunology (2023)
-
Engineering biomaterials to tailor the microenvironment for macrophage–endothelium interactions
Nature Reviews Materials (2023)
-
Advanced glycation end-products as mediators of the aberrant crosslinking of extracellular matrix in scarred liver tissue
Nature Biomedical Engineering (2023)