Abstract
Most human tumours are heterogeneous, composed of cellular clones with different properties present at variable frequencies. Highly heterogeneous tumours have poor clinical outcomes, yet the underlying mechanism remains poorly understood. Here, we show that minor subclones of breast cancer cells expressing IL11 and FIGF (VEGFD) cooperate to promote metastatic progression and generate polyclonal metastases composed of driver and neutral subclones. Expression profiling of the epithelial and stromal compartments of monoclonal and polyclonal primary and metastatic lesions revealed that this cooperation is indirect, mediated through the local and systemic microenvironments. We identified neutrophils as a leukocyte population stimulated by the IL11-expressing minor subclone and showed that the depletion of neutrophils prevents metastatic outgrowth. Single-cell RNA-seq of CD45+ cell populations from primary tumours, blood and lungs demonstrated that IL11 acts on bone-marrow-derived mesenchymal stromal cells, which induce pro-tumorigenic and pro-metastatic neutrophils. Our results indicate key roles for non-cell-autonomous drivers and minor subclones in metastasis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
RNA-seq and scRNA-seq data have been deposited in the NCBI GEO database with the accession number GSE109281. The publicly available subset of the MBCP RNA-seq data can be found in GEO database with the accession number GSE121411. Primary breast cancer data, where indicated, were derived from the TCGA dataset (http://cancergenome.nih.gov/). The source data for Figs. 1,3,4,6 and Supplementary Fig. 1–6 have been provided as Supplementary Table 1. All data supporting the findings in this study are available from the corresponding author on request.
Code availability
The mathematical modelling code is available from the corresponding author on request.
References
Marusyk, A., Almendro, V. & Polyak, K. Intra-tumour heterogeneity: a looking glass for cancer? Nat. Rev. Cancer 12, 323–334 (2012).
Burrell, R. A. & Swanton, C. Re-evaluating clonal dominance in cancer evolution. Trends Cancer 2, 263–276 (2016).
Yates, L. R. et al. Genomic evolution of breast cancer metastasis and relapse. Cancer Cell 32, 169–184 (2017).
Brastianos, P. K. et al. Genomic characterization of brain metastases reveals branched evolution and potential therapeutic targets. Cancer Discov. 5, 1164–1177 (2015).
Peinado, H. et al. Pre-metastatic niches: organ-specific homes for metastases. Nat. Rev. Cancer 17, 302–317 (2017).
McAllister, S. S. & Weinberg, R. A. The tumour-induced systemic environment as a critical regulator of cancer progression and metastasis. Nat. Cell Biol. 16, 717–727 (2014).
Marusyk, A. et al. Non-cell-autonomous driving of tumour growth supports sub-clonal heterogeneity. Nature 514, 54–58 (2014).
Chen, Q., Sun, L. & Chen, Z. J. Regulation and function of the cGAS–STING pathway of cytosolic DNA sensing. Nat Immunol. 17, 1142–1149 (2016).
Nikolsky, Y., Nikolskaya, T. & Bugrim, A. Biological networks and analysis of experimental data in drug discovery. Drug Discov. Today 10, 653–662 (2005).
Ernst, M. & Putoczki, T. L. Molecular pathways: IL11 as a tumor-promoting cytokine-translational implications for cancers. Clin. Cancer Res. 20, 5579–5588 (2014).
Retsky, M., Demicheli, R., Hrushesky, W., Baum, M. & Gukas, I. Surgery triggers outgrowth of latent distant disease in breast cancer: an inconvenient truth? Cancers 2, 305–337 (2010).
Tohme, S., Simmons, R. L. & Tsung, A. Surgery for cancer: a trigger for metastases. Cancer Res. 77, 1548–1552 (2017).
Daley, J. M., Thomay, A. A., Connolly, M. D., Reichner, J. S. & Albina, J. E. Use of Ly6G-specific monoclonal antibody to deplete neutrophils in mice. J. Leukoc. Biol. 83, 64–70 (2008).
Turley, S. J., Cremasco, V. & Astarita, J. L. Immunological hallmarks of stromal cells in the tumour microenvironment. Nat. Rev. Immunol. 15, 669–682 (2015).
Cerami, E. et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Discov. 2, 401–404 (2012).
Gao, J. et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci. Signal. 6, pl1 (2013).
Jeselsohn, R. et al. Allele-specific chromatin recruitment and therapeutic vulnerabilities of ESR1 activating mutations. Cancer Cell 33, 173–186 (2018).
Siegel, M. B. et al. Integrated RNA and DNA sequencing reveals early drivers of metastatic breast cancer. J. Clin. Invest. 128, 1371–1383 (2018).
Hoadley, K. A. et al. Tumor evolution in two patients with basal-like breast cancer: a retrospective genomics study of multiple metastases. PLoS Med. 13, e1002174 (2016).
Onnis, B., Fer, N., Rapisarda, A., Perez, V. S. & Melillo, G. Autocrine production of IL-11 mediates tumorigenicity in hypoxic cancer cells. J. Clin. Invest. 123, 1615–1629 (2013).
Putoczki, T. L. et al. Interleukin-11 is the dominant IL-6 family cytokine during gastrointestinal tumorigenesis and can be targeted therapeutically. Cancer Cell 24, 257–271 (2013).
Bockhorn, J. et al. MicroRNA-30c inhibits human breast tumour chemotherapy resistance by regulating TWF1 and IL-11. Nat. Commun. 4, 1393 (2013).
Kang, Y. et al. A multigenic program mediating breast cancer metastasis to bone. Cancer Cell 3, 537–549 (2003).
Hanavadi, S., Martin, T. A., Watkins, G., Mansel, R. E. & Jiang, W. G. Expression of interleukin 11 and its receptor and their prognostic value in human breast cancer. Ann. Surg. Oncol. 13, 802–808 (2006).
Bower, N. I. et al. Vegfd modulates both angiogenesis and lymphangiogenesis during zebrafish embryonic development. Development 144, 507–518 (2017).
Van den Eynden, G. G. et al. Comparison of molecular determinants of angiogenesis and lymphangiogenesis in lymph node metastases and in primary tumours of patients with breast cancer. J. Pathol. 213, 56–64 (2007).
Leach, J., Morton, J. P. & Sansom, O. J. Neutrophils: homing in on the myeloid mechanisms of metastasis. Mol. Immunol. 110, 69–76 (2017).
Wculek, S. K. & Malanchi, I. Neutrophils support lung colonization of metastasis-initiating breast cancer cells. Nature 528, 413–417 (2015).
Coffelt, S. B. et al. IL-17-producing γδ T cells and neutrophils conspire to promote breast cancer metastasis. Nature 522, 345–348 (2015).
Fridlender, Z. G. et al. Polarization of tumor-associated neutrophil phenotype by TGF-beta: “N1” versus “N2” TAN. Cancer Cell 16, 183–194 (2009).
Castano, Z. et al. IL-1β inflammatory response driven by primary breast cancer prevents metastasis-initiating cell colonization. Nat. Cell Biol. 20, 1084–1097 (2018).
Krenn-Pilko, S. et al. The elevated preoperative derived neutrophil-to-lymphocyte ratio predicts poor clinical outcome in breast cancer patients. Tumour Biol. 37, 361–368 (2016).
Granot, Z. et al. Tumor entrained neutrophils inhibit seeding in the premetastatic lung. Cancer Cell 20, 300–314 (2011).
Finisguerra, V. et al. MET is required for the recruitment of anti-tumoural neutrophils. Nature 522, 349–353 (2015).
Voloshin, T. et al. Blocking IL1β pathway following paclitaxel chemotherapy slightly inhibits primary tumor growth but promotes spontaneous metastasis. Mol. Cancer Ther. 14, 1385–1394 (2015).
Kersten, K. et al. Mammary tumor-derived CCL2 enhances pro-metastatic systemic inflammation through upregulation of IL1β in tumor-associated macrophages. Oncoimmunology 6, e1334744 (2017).
St Croix, B. et al. Genes expressed in human tumor endothelium. Science 289, 1197–1202 (2000).
Carson-Walter, E. B. et al. Cell surface tumor endothelial markers are conserved in mice and humans. Cancer Res. 61, 6649–6655 (2001).
Pan, X. et al. Two methods for full-length RNA sequencing for low quantities of cells and single cells. Proc. Natl Acad. Sci. USA 110, 594–599 (2013).
Guo, S. et al. Nonstochastic reprogramming from a privileged somatic cell state. Cell 156, 649–662 (2014).
Satija, R., Farrell, J. A., Gennert, D., Schier, A. F. & Regev, A. Spatial reconstruction of single-cell gene expression data. Nat. Biotechnol. 33, 495–502 (2015).
Heng, T. S. et al. The Immunological Genome Project: networks of gene expression in immune cells. Nat. Immunol. 9, 1091–1094 (2008).
McDonald, T. O. & Michor, F. SIApopr: a computational method to simulate evolutionary branching trees for analysis of tumor clonal evolution. Bioinformatics 33, 2221–2223 (2017).
Haeno, H. et al. Computational modeling of pancreatic cancer reveals kinetics of metastasis suggesting optimum treatment strategies. Cell 148, 362–375 (2012).
Chen, R. et al. Robust transcriptional tumor signatures applicable to both formalin-fixed paraffin-embedded and fresh-frozen samples. Oncotarget 8, 6652–6662 (2017).
Dobin, A. et al. STAR: ultrafast universal RNA-seq aligner. Bioinformatics 29, 15–21 (2013).
Trapnell, C. et al. Transcript assembly and quantification by RNA-Seq reveals unannotated transcripts and isoform switching during cell differentiation. Nat. Biotechnol. 28, 511–515 (2010).
Wang, L., Wang, S. & Li, W. RSeQC: quality control of RNA-seq experiments. Bioinformatics 28, 2184–2185 (2012).
Hanzelmann, S., Castelo, R. & Guinney, J. GSVA: gene set variation analysis for microarray and RNA-seq data. BMC Bioinform. 14, 7 (2013).
Acknowledgements
We thank the members of the Polyak and Michor laboratories for their critical reading of this manuscript and useful discussions. We thank L. Cameron from the DFCI Confocal Microscopy and Z. Herbert from the DFCI Molecular Biology Core Facility for their dedication and technical expertise. We also thank the staff of the DFCI Animal Facility for their help with the imaging studies. This work was supported by the Dana–Farber Cancer Institute Physical Sciences–Oncology Center (grant no. U54CA143798 to F.M. and K.P.) and Center for Cancer Evolution (F.M. and K.P.), CDRMP Breast Cancer Research Program (grant nos W81XWH-09-1-0561 (A.M.) and W81XWH-14-1-0191 (S.S.M)), Swiss National Science Foundation project no. P2EZP2 175139 (S.C.), NIH (grant nos K99/R00 CA201606-01A1 (M.J.) and R35CA197623 (K.P.)), the Ludwig Center at Harvard (F.M. and K.P.), Novartis Oncology (K.P.), and the Breast Cancer Research Foundation (K.P.).
Author information
Authors and Affiliations
Contributions
D.P.T. and M.J. performed the xenograft, molecular profiling and immunohistochemical experiments, and data analyses. M.B.E. and N.W.H. analysed the RNA-seq data. A.M. helped with the study conception and xenograft experiments. N.L.K. and K.C.M. assisted with the immunohistochemical staining. M.K. generated the low-input RNA-seq libraries. Y.Q., Z.C., M.A. and C.G.D.A. performed the FACS analyses. T.L. and S.S. assisted with the animal experiments. K.N.Y. carried out the mathematical modelling. A.L. and K.W.W. assisted with the generation of the scRNA-seq libraries. S.C. analysed the scRNA-seq data. O.C. and N.W. provided the MBCP cohort data and performed analyses. K.P. supervised the research with help from F.M., S.S.M. and R.F. All authors helped to design the study and write the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare competing financial interests. K.P. received research support from and was a consultant to Novartis Oncology during the execution of this study. K.P. also serves on the Scientific Advisory Board of Mitra Biotech.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Tumour growth and clonality.
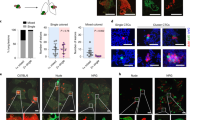
a, Bioluminescence images of mice bearing parental or polyclonal tumours at ~1 cm diameter in size before and after surgery. Surgeries for different groups were performed at different time points, based on the 1cm diameter criterium. b, Quantification of metastatic areas based on bioluminescence. n=5 mice per group, except parental group n=4. p values of two-tailed unpaired t-test are shown. Mean +/- s.d. is shown. c, Flow chart of FACS gating strategy of stromal (unlabelled) and fluorescently-labelled epithelial cells. Viable cells were gated on and from FITC-mCherry- cell population APC+ and PE+ cells were selected. To sort for FITC and mCherry+ cells, viable cells negative for APC and PE were sorted for those markers. See also Supplementary Table 1 for raw data.
Supplementary Figure 2 Gene expression changes in polyclonal tumours and stroma.
a, Clustering of RNA-seq samples using the top 1,000 differentially expressed genes. Units represent VST-transformed expression values. b, PCA plot of RNA-seq samples (n=3 animals per group). c, Top 10 MetaCore GO Processes overrepresented in the indicated comparisons (n=3 animals per group). Dashed line at P = 0.01. Asterisks mark processes associated with immune response. -log(p value) of Enrichment Analysis test is shown. d, Representative images of CD31 and LYVE1 in monoclonal and polyclonal primary tumours and lungs of corresponding animals. Asterisks (*) indicate blood (CD31) or lymphatic (LYVE1) vessels in the lung tissue. Scale bar 100 μm. Staining was repeated twice with similar results. e, Relative frequency of each of the four subclone within primary tumours. See also Supplementary Table 1 for raw data.
Supplementary Figure 3 Polyclonal tumour-induced changes in leukocytes.
a, FACS experiment gating strategy. b, Analysis of myeloid cell populations, not included in Fig. 3, extracted from blood, primary tumour and lungs of mice bearing parental, 100% FIGF or 100% IL11 monoclonal or polyclonal tumours, n = 5 mice per group. Mean +/- s.d. is shown. p values indicate statistical significance of the observed differences defined by unpaired two-tailed t-test. See also Supplementary Table 1 for raw data.
Supplementary Figure 4 The effect of surgery on metastasis and mathematical modelling of metastatic outgrowth.
a, Bioluminescence images of mice bearing parental or polyclonal tumours before and after surgery performed at week 4 post-tumour cell injection. b, Quantification of metastasis area at experimental endpoint (n = 5 mice per group). c, Quantification of CK+ cells in the lungs. On average, 3,500 cells were counted per field, 3 fields per sample. Lungs of 5 mice per group were analysed. b, c, Box-and-whisker plots show mean (midline), 25th-75th percentile (box) and 5th-95th percentile (whiskers). p values indicate statistical significance of the observed differences defined by unpaired two-tailed t-test. d, Quantification of metastatic area at the experimental endpoint. e, Estimated growth rates per week for monoclonal IL11 and polyclonal tumours and metastases (n=5 animals per group). f-i, Predicted numbers of cells at the largest metastatic site six weeks after tumour inoculation of mice with (f) IL11 monoclonal and (g) polyclonal tumours, respectively (n=5 animals per group, 2 tumours per mice). h, i, Predicted numbers of primary cells when the first metastasis was detected in (h) IL11 and (i) polyclonal groups, respectively. Shaded areas represent results from the corresponding experiments. Parameter values used for the panels were r0 = 2.726, r1=4.383 for the IL11 group, and r0 = 2.363, r1=5.552 for the polyclonal group, respectively, and death rate of each Type=0.01×growth rate. j,k, The timing of the first metastatic cells disseminated from the primary site, as predicted by stochastic simulation in the (j) IL11 and (k) polyclonal groups. The parameter values used were r0 = 2.726, r1 = 4.383 for the IL11 group, and r0 = 2.363, r1 = 5.552 for the polyclonal group, respectively, and death rate of each type = 0.01×growth rate. Parameter values used for the panels are the same as those described in f-k. Box-and-whisker plots show the mean (midline), 25th-75th percentile (box) and 5th-95th percentile (whiskers). See also Supplementary Table 1 for raw data.
Supplementary Figure 5 In vivo neutrophil depletion.
a, Experimental design. b, Representative image of neutrophil depletion at week 2 of treatment. Staining was performed on 5 animals with similar results. c, d, Quantification of neutrophil and monocytes from blood of the treated animals at week 2 (c) and week 6 (d). n=4 animals per group in isotype treated, and n=5 per group in anti-Ly6G treated. NTC – non-tumour bearing control animals. Mean ± s.d. shown. Two-tailed unpaired t-test p values are shown.
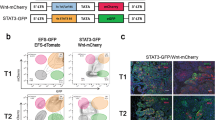
Supplementary Figure 6 Analysis of scRNA-seq data and gating strategy for IL11RA+ cells.
a-c, e and f, Multi-dimensional scaling of single-cell expression profiling. Each dot represents a single cell (n=7,704), and the distance between cells is defined based on the relatedness of their transcriptional profiles. In panels c, e, and f cells expressing the indicated gene are marked in purple, while non-expressors are grey. a, tSNE plot depicting the thirteen cell clusters identified. b, Contribution of cells from different experimental groups to distinct clusters. Cells are coloured according to the sample of origin. c, Expression of cancer cell markers, EGFR, KRT14, and KRT18, within a single cluster identifies cancer cell contamination. d, Heat map representing the top genes differentially expressed by particular clusters of cells. e, Expression of representative marker genes within different tSNE clusters was used to assign cell clusters to cell types. f, Expression of IL11 co-receptor, gp130, and IL11 effector, STAT3, within the different tSNE clusters. g, Heat map represents the expression of the top 30 differentially expressed genes for each cluster identified in our single cell RNA-seq experiment (rows) within the cell type-specific expression data from ImmGen consortium (columns). h, Gating strategy for FACS sorting of ILRA-, ILRA+PLXDC2-, and IL11RA+PLXDC2+ cells from lungs of Vehicle (not shown) or Dox treated tumour-bearing mice. i, Gating of IL11RA+ cells (blue) plotted against all cells (orange) from panel (h). Note clustering of cells in the low SSC (side scatter) and low FCS (forward scatter) area typically corresponding to lymphocytes. j, Flow cytometry analysis of lungs from tumour-free untreated mice stained with IL11RA and PLXDC2 antibodies. We detected the co-expression of PLXDC2 in IL11RAhigh and in a subset of IL11RAlow cells. k, Single staining controls for indicated antibodies. l, Unstained control matching Fig. 5g. A – area, W- width and H - height. See also Supplementary Table 1 for raw data.
Supplementary information
Supplementary Information
Supplementary Figures 1–6, Supplementary Table titles/legends
Supplementary Table 1
Statistics Source Data.
Supplementary Table 2
Antibodies used for immunohistochemistry, immunofluorescence, and FACS.
Supplementary Table 3
Differentially expressed genes within different fractions isolated from polyclonal tumours compared to parental tumour (cancer cell tab; n = 3 animals per group).
Supplementary Table 4
Stroma GO analysis.
Supplementary Table 5
Genes differentially expressed and defining clusters.
Supplementary Table 6
Differentially expressed genes between +DOX and −DOX lung and blood neutrophils and mesenchymal stromal cells, and primary cancer cells (generated based on n = 7,704 single cell profiles).
Supplementary Table 7
JAK–STAT and TGFβ pathway genes.
Supplementary Table 8
Top 200 genes differentially expressed in IL11RA1+ versus other clusters.
Supplementary Table 9
Process networks enriched in genes highly expressed in IL11RAhigh cells.
Rights and permissions
About this article
Cite this article
Janiszewska, M., Tabassum, D.P., Castaño, Z. et al. Subclonal cooperation drives metastasis by modulating local and systemic immune microenvironments. Nat Cell Biol 21, 879–888 (2019). https://doi.org/10.1038/s41556-019-0346-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41556-019-0346-x
This article is cited by
-
Spatial immunophenotypes orchestrate prognosis in triple-negative breast cancer with Miller-Payne grade 4 following neoadjuvant chemotherapy
npj Breast Cancer (2023)
-
Spatial biology of cancer evolution
Nature Reviews Genetics (2023)
-
Cell competition in development, homeostasis and cancer
Nature Reviews Molecular Cell Biology (2023)
-
Spatial genomics maps the structure, nature and evolution of cancer clones
Nature (2022)
-
Clonal barcoding with qPCR detection enables live cell functional analyses for cancer research
Nature Communications (2022)