Abstract
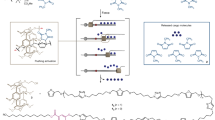
Neuromuscular interfaces are required to translate bioelectronic technologies for application in clinical medicine. Here, by leveraging the robotically controlled ink-jet deposition of low-viscosity conductive inks, extrusion of insulating silicone pastes and in situ activation of electrode surfaces via cold-air plasma, we show that soft biocompatible materials can be rapidly printed for the on-demand prototyping of customized electrode arrays well adjusted to specific anatomical environments, functions and experimental models. We also show, with the monitoring and activation of neuronal pathways in the brain, spinal cord and neuromuscular system of cats, rats and zebrafish, that the printed bioelectronic interfaces allow for long-term integration and functional stability. This technology might enable personalized bioelectronics for neuroprosthetic applications.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Data availability
The main data supporting the results in this study are available within the paper and its Supplementary Information file. The raw and analysed datasets generated during the study are too large to be publicly shared, but they are available for research purposes from the corresponding authors on reasonable request.
Code availability
The code used to program the printer paths can be found at https://sourceforge.net/projects/g-code-processor.
References
Wagner, F. B. et al. Targeted neurotechnology restores walking in humans with spinal cord injury. Nature 563, 65–71 (2018).
Granata, G. et al. Phantom somatosensory evoked potentials following selective intraneural electrical stimulation in two amputees. Clin. Neurophysiol. 129, 1117–1120 (2018).
Ajiboye, A. B. et al. Restoration of reaching and grasping movements through brain-controlled muscle stimulation in a person with tetraplegia: a proof-of-concept demonstration. Lancet 389, 1821–1830 (2017).
Liu, Y. et al. Soft and elastic hydrogel-based microelectronics for localized low-voltage neuromodulation. Nat. Biomed. Eng. 3, 58–68 (2019).
Minev, I. R. et al. Electronic dura mater for long-term multimodal neural interfaces. Science 347, 159–163 (2015).
Fu, T.-M., Hong, G., Viveros, R. D., Zhou, T. & Lieber, C. M. Highly scalable multichannel mesh electronics for stable chronic brain electrophysiology. Proc. Natl Acad. Sci. USA 114, E10046–E10055 (2017).
Boutry, C. M. et al. A stretchable and biodegradable strain and pressure sensor for orthopaedic application. Nat. Electron. 1, 314–321 (2018).
Kim, T.-i et al. Injectable, cellular-scale optoelectronics with applications for wireless optogenetics. Science 340, 211–216 (2013).
Reeder, J. et al. Mechanically adaptive organic transistors for implantable electronics. Adv. Mater. 26, 4967–4973 (2014).
Lu, C. et al. Flexible and stretchable nanowire-coated fibers for optoelectronic probing of spinal cord circuits. Sci. Adv. https://doi.org/10.1126/sciadv.1600955 (2017).
Sengeh, D. M. & Herr, H. A variable-impedance prosthetic socket for a transtibial amputee designed from magnetic resonance imaging data. J. Prosthet. Orthot. 25, 129–137 (2013).
Filardo, G. et al. Novel alginate biphasic scaffold for osteochondral regeneration: an in vivo evaluation in rabbit and sheep models. J. Mater. Sci. Mater. Med. 29, 74 (2018).
Ploch, C. C., Mansi, C. S., Jayamohan, J. & Kuhl, E. Using 3D printing to create personalized brain models for neurosurgical training and preoperative planning. World Neurosurg. 90, 668–674 (2016).
Valentine, A. D. et al. Hybrid 3D printing of soft electronics. Adv. Mater. 29, 1703817 (2017).
Lind, J. U. et al. Instrumented cardiac microphysiological devices via multimaterial three-dimensional printing. Nat. Mater. 16, 303–308 (2017).
Bachmann, B. et al. All-inkjet-printed gold microelectrode arrays for extracellular recording of action potentials. Flex. Print. Electron. 2, 035003 (2017).
Athanasiadis, M. et al. Printed elastic membranes for multimodal pacing and recording of human stem-cell-derived cardiomyocytes. npj Flex. Electron. https://doi.org/10.1038/s41528-020-0075-z (2020).
Minev, I. R., Wenger, N., Courtine, G. & Lacour, S. P.Research update: platinum-elastomer mesocomposite as neural electrode coating.APL Mater. 3, 014701 (2015).
Mo, L. et al. Nano-silver ink of high conductivity and low sintering temperature for paper electronics. Nanoscale Res. Lett. 14, 197 (2019).
Van Noort, R., Black, M. M., Martin, T. R. P. & Meanley, S. A study of the uniaxial mechanical properties of human dura mater preserved in glycerol. Biomaterials 2, 41–45 (1981).
Kwan, M. K., Wall, E. J., Massie, J. & Garfin, S. R. Strain, stress and stretch of peripheral nerve rabbit experiments in vitro and in vivo. Acta Orthop. Scand. 63, 267–272 (1992).
Calvo, B. et al. Passive nonlinear elastic behaviour of skeletal muscle: experimental results and model formulation. J. Biomech. 43, 318–325 (2010).
Nicholson, K. J. & Winkelstein, B. A. in Neural Tissue Biomechanics (ed. Bilston, L. E.) 203–229 (Springer, 2011).
Harrison, D. E., Cailliet, R., Harrison, D. D., Troyanovich, S. J. & Harrison, S. O. A review of biomechanics of the central nervous system—part II: spinal cord strains from postural loads. J. Manipulative Physiol. Ther. 22, 322–332 (1999).
Diani, J., Fayolle, B. & Gilormini, P. A review on the Mullins effect. Eur. Polym. J. 45, 601–612 (2009).
Neto, J. P. et al. Does impedance matter when recording spikes with polytrodes? Front. Neurosci. https://doi.org/10.3389/fnins.2018.00715 (2018).
Cogan, S. F. Neural stimulation and recording electrodes. Annu. Rev. Biomed. Eng. 10, 275–309 (2008).
Biegler, T. An electrochemical and electron microscopic study of activation and roughening of platinum electrodes. J. Electrochem. Soc. 116, 1131 (1969).
Tondera, C. et al. Highly conductive, stretchable, and cell-adhesive hydrogel by nanoclay doping. Small 15, 1901406 (2019).
Won, S. M. et al. Recent advances in materials, devices, and systems for neural interfaces. Adv. Mater. 30, 1800534 (2018).
Capogrosso, M. et al. A brain–spine interface alleviating gait deficits after spinal cord injury in primates. Nature 539, 284–288 (2016).
Musienko, P. E. et al. Spinal and supraspinal control of the direction of stepping during locomotion. J. Neurosci. 32, 17442–17453 (2012).
Harkema, S. et al. Effect of epidural stimulation of the lumbosacral spinal cord on voluntary movement, standing, and assisted stepping after motor complete paraplegia: a case study. Lancet 377, 1938–1947 (2011).
Courtine, G. et al. Transformation of nonfunctional spinal circuits into functional states after the loss of brain input. Nat. Neurosci. 12, 1333–1342 (2009).
Wenger, N. et al. Spatiotemporal neuromodulation therapies engaging muscle synergies improve motor control after spinal cord injury. Nat. Med. 22, 138–145 (2016).
Hoffman, P.Beitrage zur kenntnis der menschlichen reflexe mit besonderer berucksichtigung der elektrischen erscheinungen.Arch. F. Physiol. 1, 223–256 (1910).
Shik, M. L. Control of walking and running by means of electrical stimulation of the midbrain. Biofizika 11, 659–666 (1966).
Fry, C. H., Wu, C. & Sui, G. P. Electrophysiological properties of the bladder. Int. Urogynecol. J. 9, 291–298 (1998).
Liu, D. W. & Westerfield, M. Function of identified motoneurones and co-ordination of primary and secondary motor systems during zebra fish swimming. J. Physiol. 403, 73–89 (1988).
Hains, B. C. & Waxman, S. G. Activated microglia contribute to the maintenance of chronic pain after spinal cord injury. J. Neurosci. 26, 4308–4317 (2006).
Sierra, A. et al. The “Big-Bang” for modern glial biology: translation and comments on Pío del Río-Hortega 1919 series of papers on microglia.Glia 64, 1801–1840 (2016).
Musienko, P. et al. Somatosensory control of balance during locomotion in decerebrated cat. J. Neurophysiol. 107, 2072–2082 (2012).
Nonnekes, J. et al. Neurological disorders of gait, balance and posture: a sign-based approach. Nat. Rev. Neurol. 14, 183–189 (2018).
Musienko, P. E. et al. Neuronal control of posture and locomotion in decerebrated and spinalized animals. Ross. Fiziol. Zh. Im. I. M. Sechenova 99, 392–405 (2013).
Gill, M. L. et al. Neuromodulation of lumbosacral spinal networks enables independent stepping after complete paraplegia. Nat. Med. https://doi.org/10.1038/s41591-018-0175-7 (2018).
Kim, Y. et al. A bioinspired flexible organic artificial afferent nerve. Science 360, 998–1003 (2018).
Vu, P. P. et al. A regenerative peripheral nerve interface allows real-time control of an artificial hand in upper limb amputees. Sci. Transl. Med. 12, eaay2857 (2020).
Vachicouras, N. et al. Microstructured thin-film electrode technology enables proof of concept of scalable, soft auditory brainstem implants. Sci. Transl. Med. 11, eaax9487 (2019).
Borton, D. et al. Corticospinal neuroprostheses to restore locomotion after spinal cord injury. Neurosci. Res. 78, 21–29 (2014).
Athanasiadis, M., Pak, A., Afanasenkau, D. & Minev, I. R. Direct writing of elastic fibers with optical, electrical, and microfluidic functionality. Adv. Mater. Technol. 4, 1800659 (2019).
Hudak, E. M., Mortimer, J. T. & Martin, H. B. Platinum for neural stimulation: voltammetry considerations. J. Neural Eng. 7, 026005 (2010).
Whelan, P. J. Control of locomotion in the decerebrate cat. Prog. Neurobiol. 49, 481–515 (1996).
Shik, M. L. & Orlovsky, G. N. Neurophysiology of locomotor automatism. Physiol. Rev. 56, 465–501 (1976).
Mori, S., Kawahara, K., Sakamoto, T., Aoki, M. & Tomiyama, T. Setting and resetting of level of postural muscle tone in decerebrate cat by stimulation of brain stem. J. Neurophysiol. 48, 737–748 (1982).
Iwahara, T., Atsuta, Y., Garcia-Rill, E. & Skinner, R. D. Spinal cord stimulation-induced locomotion in the adult cat. Brain Res. Bull. 28, 99–105 (1992).
Gerasimenko, Y. P. et al. Formation of locomotor patterns in decerebrate cats in conditions of epidural stimulation of the spinal cord. Neurosci. Behav. Physiol. 35, 291–298 (2005).
Merkulyeva, N. et al. Activation of the spinal neuronal network responsible for visceral control during locomotion. Exp. Neurol. 320, 112986 (2019).
Kruse, M. N. & de Groat, W. C. Spinal pathways mediate coordinated bladder/urethral sphincter activity during reflex micturition in decerebrate and spinalized neonatal rats. Neurosci. Lett. 152, 141–144 (1993).
Shefchyk, S. J. & Buss, R. R. Urethral pudendal afferent-evoked bladder and sphincter reflexes in decerebrate and acute spinal cats. Neurosci. Lett. 244, 137–140 (1998).
Gerasimenko, Y. et al. Propriospinal bypass of the serotonergic system that can facilitate stepping. J. Neurosci. 29, 5681–5689 (2009).
Westerfield, M. The Zebrafish Book. A Guide for the Laboratory Use of Zebrafish (Danio rerio) 4th edn (Univ. Oregon Press, 2000).
Martins, T., Valentim, A. M., Pereira, N. & Antunes, L. M. Anaesthesia and analgesia in laboratory adult zebrafish: a question of refinement. Lab. Anim. 50, 476–488 (2016).
Capogrosso, M. et al. Configuration of electrical spinal cord stimulation through real-time processing of gait kinematics. Nat. Protoc. 13, 2031–2061 (2018).
Jorfi, M., Skousen, J. L., Weder, C. & Capadona, J. R. Progress towards biocompatible intracortical microelectrodes for neural interfacing applications. J. Neural Eng. 12, 011001 (2014).
Kirik, O. V., Sukhorukova, E. G. & Korzhevskiĭ, D. E. Calcium-binding Iba-1/AIF-1 protein in rat brain cells. Morfologiia 137, 5–8 (2010).
Schindelin, J. et al. Fiji: an open-source platform for biological-image analysis. Nat. Methods 9, 676–682 (2012).
Kreutzberg, G. W. Microglia: a sensor for pathological events in the CNS. Trends Neurosci. 19, 312–318 (1996).
Refolo, V. & Stefanova, N. Neuroinflammation and glial phenotypic changes in alpha-synucleinopathies. Front. Cell. Neurosci. https://doi.org/10.3389/fncel.2019.00263 (2019).
Pistohl, T., Schulze-Bonhage, A., Aertsen, A., Mehring, C. & Ball, T. Decoding natural grasp types from human ECoG. NeuroImage 59, 248–260 (2012).
Acknowledgements
We acknowledge funding from the following sources: the European Research Council (804005; IntegraBrain), Saint-Petersburg State University (project 51134206; funding to O.G. and N.M. for animal facility and biocompatibility studies, and validation of the implants on in vivo models), Technische Universität Dresden, the Russian Foundation for Basic Research (grants 20-015-00568-a (for the urodynamic study) and 18-33-20062-mol_a_ved (for developing the optimal electrode array configuration)), Deutsche Forschungsgemeinschaft (MI 2117/1-1) and the Volkswagen Foundation (Freigeist 91 690). We thank D. E. Korzhevskiy (immunohistochemistry), Y. I. Sysoev (zebrafish model), A. V. Goriainova (functional tests) and T. Kurth (electron microscopy) for help and expertise.
Author information
Authors and Affiliations
Contributions
I.R.M. and P.M. conceived of and initiated the project and wrote the manuscript. D.A., D.K., C.T., O.G., N.P., I.R.M. and P.M. designed and performed the experiments. D.A., D.K., V.L., C.T., S.M., N.M., A.V.K., I.R.M. and P.M. analysed the data and contributed to writing the manuscript. P.M. and I.R.M. supervised the study.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Figs. 1–18, captions for Supplementary Videos 1–3 and references.
Supplementary Video 1
Hybrid printing technology for personalized soft neuromuscular interfaces (NeuroPrint).
Supplementary Video 2
Facilitation of the spinal locomotor network by the NeuroPrint array.
Supplementary Video 3
Long-term biointegration of the NeuroPrint technology.
Rights and permissions
About this article
Cite this article
Afanasenkau, D., Kalinina, D., Lyakhovetskii, V. et al. Rapid prototyping of soft bioelectronic implants for use as neuromuscular interfaces. Nat Biomed Eng 4, 1010–1022 (2020). https://doi.org/10.1038/s41551-020-00615-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-020-00615-7
This article is cited by
-
Gradient matters via filament diameter-adjustable 3D printing
Nature Communications (2024)
-
Motion artefact management for soft bioelectronics
Nature Reviews Bioengineering (2024)
-
Omnidirectional printing of stretchable electronics
Nature Electronics (2023)
-
Highly conductive tissue-like hydrogel interface through template-directed assembly
Nature Communications (2023)
-
3D printable high-performance conducting polymer hydrogel for all-hydrogel bioelectronic interfaces
Nature Materials (2023)