Abstract
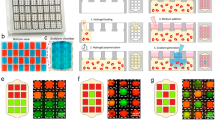
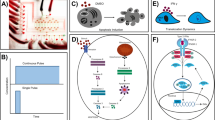
The study of intercellular signalling networks requires organotypic microscale systems that facilitate the culture, conditioning and manipulation of cells. Here, we describe a reconfigurable microfluidic cell-culture system that facilitates the assembly of three-dimensional tissue models by stacking layers that contain preconditioned microenvironments. By using principles of open and suspended microfluidics, the Stacks system is easily assembled or disassembled to provide spatial and temporal manoeuvrability in two-dimensional and three-dimensional assays of multiple cell types, enabling the modelling of sequential paracrine-signalling events, such as tumour-cell-mediated differentiation of macrophages and macrophage-facilitated angiogenesis. We used Stacks to recapitulate the in vivo observation that different prostate cancer tissues polarize macrophages with distinct gene-expression profiles of pro-inflammatory and anti-inflammatory cytokines. Stacks also enabled us to show that these two types of macrophages signal distinctly to endothelial cells, leading to blood vessels with different morphologies. Our proof-of-concept experiments exemplify how Stacks can efficiently model multicellular interactions and highlight the importance of spatiotemporal specificity in intercellular signalling.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The authors declare that all data supporting the findings of this study are available within the paper and its Supplementary Information. Source data for the primary-sample figures are available in Figshare with the identifier https://figshare.com/s/c237024425f6e06e8fcc.
References
Chanmee, T., Ontong, P., Konno, K. & Itano, N. Tumor-associated macrophages as major players in the tumor microenvironment. Cancers 6, 1670–1690 (2014).
Qian, B.-Z. & Pollard, J. W. Macrophage diversity enhances tumor progression and metastasis. Cell 141, 39–51 (2010).
Van Ginderachter, J. A. et al. Classical and alternative activation of mononuclear phagocytes: picking the best of both worlds for tumor promotion. Immunobiology 211, 487–501 (2006).
Mantovani, A. & Allavena, P. The interaction of anticancer therapies with tumor-associated macrophages. J. Exp. Med. 212, 435–445 (2015).
Ostrand-Rosenberg, S. Immune surveillance: a balance between protumor and antitumor immunity. Curr. Opin. Genet. Dev. 18, 11–18 (2008).
Pollard, J. W. Tumour-educated macrophages promote tumour progression and metastasis. Nat. Rev. Cancer 4, 71–78 (2004).
Lee, G. T. et al. Macrophages induce neuroendocrine differentiation of prostate cancer cells via BMP6-IL6 Loop. Prostate 71, 1525–1537 (2011).
Lissbrant, I. F. et al. Tumor associated macrophages in human prostate cancer: relation to clinicopathological variables and survival. Int. J. Oncol. 17, 445–451 (2000).
Mestas, J. & Hughes, C. C. W. Of mice and not men: differences between mouse and human immunology. J. Immunol. 172, 2731–2738 (2004).
Pompano, R. R., Li, H.-W. & Ismagilov, R. F. Rate of mixing controls rate and outcome of autocatalytic processes: theory and microfluidic experiments with chemical reactions and blood coagulation. Biophys. J. 95, 1531–1543 (2008).
Mantovani, A., Schioppa, T., Porta, C., Allavena, P. & Sica, A. Role of tumor-associated macrophages in tumor progression and invasion. Cancer Metast. Rev. 25, 315–322 (2006).
Mantovani, A., Sozzani, S., Locati, M., Allavena, P. & Sica, A. Macrophage polarization: tumor-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Trends Immunol. 23, 549–555 (2002).
Martinez, F. O. Macrophage activation and polarization. Front. Biosci. 13, 453–461 (2008).
Bowdish, D. M. E. in Encyclopedia of Immunobiology (Ratcliffe, M.) 289–292 (Acad. Press, 2016).
Martinez, F. O. & Gordon, S. The M1 and M2 paradigm of macrophage activation: time for reassessment. F1000Prime Rep. 6, 13 (2014).
Rőszer, T. Understanding the mysterious M2 macrophage through activation markers and effector mechanisms. Mediat. Inflamm. 2015, 816460 (2015).
Nahrendorf, M. & Swirski, F. K. Abandoning M1/M2 for a network model of macrophage function. Circ. Res. 119, 414–417 (2016).
Perestrelo, A. R., Águas, A. C. P., Rainer, A. & Forte, G. Microfluidic organ/body-on-a-chip devices at the convergence of biology and microengineering. Sensors 15, 31142–31170 (2015).
Bhatia, S. N. & Ingber, D. E. Microfluidic organs-on-chips. Nat. Biotechnol. 32, 760–772 (2014).
Curtis, A. et al. Patterning of sharp cellular interfaces with a reconfigurable elastic substrate. Integr. Biol. 9, 50–57 (2017).
Ehsan, S. M., Welch-Reardon, K. M., Waterman, M. L., Hughes, C. C. W. & George, S. C. A three-dimensional in vitro model of tumor cell intravasation. Integr. Biol. 6, 603–610 (2014).
Gracz, A. D. et al. A high-throughput platform for stem cell niche co-cultures and downstream gene expression analysis. Nat. Cell Biol. 17, 340–349 (2015).
Yates, C. et al. Novel three-dimensional organotypic liver bioreactor to directly visualize early events in metastatic progression. Adv. Cancer Res. 97, 225–246 (2007).
Berthier, J., Brakke, K. A. & Berthier, E. Open Microfluidics (John Wiley & Sons, 2016).
Casavant, B. P. et al. Suspended microfluidics. Proc. Natl Acad. Sci. USA 110, 10111–10116 (2013).
Bishop, E. T. et al. An in vitro model of angiogenesis: basic features. Angiogenesis 3, 335–344 (1999).
Theberge, A. B. et al. Microfluidic multiculture assay to analyze biomolecular signaling in angiogenesis. Anal. Chem. 87, 3239–3246 (2015).
Sarkanen, J.-R. et al. Intra-laboratory pre-validation of a human cell based in vitro angiogenesis assay for testing angiogenesis modulators. Front. Pharmacol. 1, 147 (2010).
Zhao, B., Moore, J. S. & Beebe, D. J. Surface-directed liquid flow inside microchannels. Science 291, 1023–1026 (2001).
Atencia, J. & Beebe, D. J. Controlled microfluidic interfaces. Nature 437, 648–655 (2005).
de Groot, T. E., Veserat, K. S., Berthier, E., Beebe, D. J. & Theberge, A. B. Surface-tension driven open microfluidic platform for hanging droplet culture. Lab Chip 16, 334–344 (2016).
Biederbick, A., Kern, H. F. & Elsässer, H. P. Monodansylcadaverine (MDC) is a specific in vivo marker for autophagic vacuoles. Eur. J. Cell Biol. 66, 3–14 (1995).
Mosser, D. M. & Edwards, J. P. Exploring the full spectrum of macrophage activation. Nat. Rev. Immunol. 8, 958–969 (2008).
Gordon, S. & Taylor, P. R. Monocyte and macrophage heterogeneity. Nat. Rev. Immunol. 5, 953–964 (2005).
Mantovani, A. et al. The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol. 25, 677–686 (2004).
Duluc, D. et al. Tumor-associated leukemia inhibitory factor and IL-6 skew monocyte differentiation into tumor-associated macrophage-like cells. Blood 110, 4319–4330 (2007).
Wu, H. C. et al. Derivation of androgen-independent human LNCaP prostatic cancer cell sublines: role of bone stromal cells. Int. J. Cancer 57, 406–412 (1994).
Kim, S., Lee, H., Chung, M. & Jeon, N. L. Engineering of functional, perfusable 3D microvascular networks on a chip. Lab Chip 13, 1489–1500 (2013).
Bersini, S. & Moretti, M. 3D functional and perfusable microvascular networks for organotypic microfluidic models. J. Mater. Sci. Mater. Med. 26, 180 (2015).
Guckenberger, D. J., de Groot, T. E., Wan, A. M. D., Beebe, D. J. & Young, E. W. K. Micromilling: a method for ultra-rapid prototyping of plastic microfluidic devices. Lab Chip 15, 2364–2378 (2015).
Chanput, W., Mes, J. J., Savelkoul, H. F. J. & Wichers, H. J. Characterization of polarized THP-1 macrophages and polarizing ability of LPS and food compounds. Food Funct. 4, 266–276 (2013).
Genin, M., Clement, F., Fattaccioli, A., Raes, M. & Michiels, C. M1 and M2 macrophages derived from THP-1 cells differentially modulate the response of cancer cells to etoposide. BMC Cancer 15, 577 (2015).
Tjiu, J.-W. et al. Tumor-associated macrophage-induced invasion and angiogenesis of human basal cell carcinoma cells by cyclooxygenase-2 induction. J. Invest. Dermatol. 129, 1016–1025 (2009).
Schmittgen, T. D. & Livak, K. J. Analyzing real-time PCR data by the comparative CT method. Nat. Protoc. 3, 1101–1108 (2008).
Acknowledgements
This work is funded by a National Science Foundation grant (EFRI-MKIS), University of Wisconsin Carbone Cancer Center Cancer Center Support Grant (P30 CA014520), Research Training in Hematology T32 (NIH T32 HL07899), NIH R01EB010039 BRG, NIH R01 CA185251, NIH K12 DK100022, DOD Prostate Cancer Research Program (W81XWH-16-0543), the Arnold and Mabel Beckman Foundation (Beckman Young Investigator Award), and the University of Washington. We thank D. Kosoff for helpful discussions and assistance with PCR, and undergraduate student B. Horman for facilitating experiments.
Author information
Authors and Affiliations
Contributions
J.Y., E.B., S.S., D.J.B. and A.B.T. designed the research. J.Y., A.C. and S.S. conducted experiments; all of the authors interpreted the data. J.Y., A.B.T., E.B. and D.J.B. wrote the manuscript, and all authors revised it.
Corresponding authors
Ethics declarations
Competing interests
The authors have potential conflicts of interest related to technologies presented here: J.Y. (Stacks to the Future), E.B. (Tasso, Salus Discovery and Stacks to the Future), T.E.d.G. (Stacks to the Future and Lynx Biosciences), A.B.T. (Stacks to the Future), and D.J.B. (Bellbrook Labs, Tasso, Stacks to the Future, Lynx Biosciences, Onexio Biosystems and Salus Discovery). However, none of these companies supported this work.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Figs. 1–6, methods and captions for Supplementary Videos 1–3.
Supplementary Video 1
Stacks layers are open microfluidic devices that can be operated with a pipette.
Supplementary Video 2
Stacks devices can be assembled to enable diffusion.
Supplementary Video 3
Stacks devices are reconfigurable and enable diffusion across layers.
ImageJ macros
ImageJ macros for image processing.
Injection-moulding CAD designs
SolidWorks files for the Stack devices.
Rights and permissions
About this article
Cite this article
Yu, J., Berthier, E., Craig, A. et al. Reconfigurable open microfluidics for studying the spatiotemporal dynamics of paracrine signalling. Nat Biomed Eng 3, 830–841 (2019). https://doi.org/10.1038/s41551-019-0421-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-019-0421-4
This article is cited by
-
Microfluidic high-throughput 3D cell culture
Nature Reviews Bioengineering (2024)
-
Passive-Flow-Based MPS: Emerging Physiological Flow-Mimetic Platforms for Studying Effects of Flow on Single Tissues and Inter-tissue Interactions
BioChip Journal (2024)
-
Miniaturizing chemistry and biology using droplets in open systems
Nature Reviews Chemistry (2023)
-
Recent advances in cancer-on-a-chip tissue models to dissect the tumour microenvironment
Med-X (2023)
-
U-IMPACT: a universal 3D microfluidic cell culture platform
Microsystems & Nanoengineering (2022)