Abstract
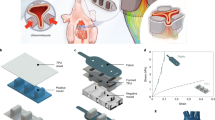
3D printing has been used to create a wide variety of anatomical models and tools for procedural planning and training. Yet, the printing of permanent, soft endocardial implants remains challenging because of the need for haemocompatibility and durability of the printed materials. Here, we describe an approach for the rapid prototyping of patient-specific cardiovascular occluders via 3D printing and static moulding of inflatable silicone/polyurethane balloons derived from volume-rendered computed tomography scans. We demonstrate the use of the approach, which provides custom-made implants made of high-quality, durable and haemocompatible elastomeric materials, in the fabrication of devices for occlusion of the left atrial appendage—a structure known to be highly variable in geometry and the primary source of stroke for patients with atrial fibrillation. We describe the design workflow, fabrication and deployment of patient-specific left atrial appendage occluders and, as a proof-of-concept, show their efficacy using 3D-printed anatomical models, in vitro flow loops and an in vivo large animal model.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Mozaffarian, D. et al. Heart disease and stroke statistics—2015 update: a report from the American Heart Association. Circulation 131, e29–e322 (2015).
Wolf, P. A., Abbott, R. D. & Kannel, W. B. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 22, 983–988 (1991).
Blackshear, J. L. & Odell, J. A. Appendage obliteration to reduce stroke in cardiac surgical patients with atrial fibrillation. Ann. Thorac. Surg. 61, 755–759 (1996).
Di Biase, L. et al. Does the left atrial appendage morphology correlate with the risk of stroke in patients with atrial fibrillation? J. Am. Coll. Cardiol. 60, 531–538 (2012).
Al-Saady, N. M., Obel, O. A. & Camm, A. J. Left atrial appendage: structure, function, and role in thromboembolism. Heart 82, 547–554 (1999).
Stoddard, M. F., Dawkins, P. R., Prince, C. R. & Ammash, N. M. Left atrial appendage thrombus is not uncommon in patients with acute atrial fibrillation and a recent embolic event: a transesophageal echocardiographic study. J. Am. Coll. Cardiol. 25, 452–459 (1995).
Yu, C.-M. et al. Mechanical antithrombotic intervention by LAA occlusion in atrial fibrillation. Nat. Rev. Cardiol. 10, 707–722 (2013).
Kong, B., Liu, Y., Huang, H., Jiang, H. & Huang, C. Left atrial appendage closure for thromboembolism prevention in patients with atrial fibrillation: advances and perspectives. J. Thorac. Dis. 7, 199–203 (2015).
Kanderian, A. S., Gillinov, A. M., Pettersson, G. B., Blackstone, E. & Klein, A. L. Success of surgical left atrial appendage closure. J. Am. Coll. Cardiol. 52, 924–929 (2008).
Katz, E. S. et al. Surgical left atrial appendage ligation is frequently incomplete: a transesophageal echocardiographic study. J. Am. Coll. Cardiol. 36, 468–471 (2000).
Ailawadi, G. et al. Exclusion of the left atrial appendage with a novel device: early results of a multicenter trial. J. Thorac. Cardiovasc. Surg. 142, 1002–1009 (2011).
Snyder, J., Engel, A. M., White, K. C., Budiansky, N. & Smith, J. M. Left atrial appendage occlusion device: evaluation of surgical implant success and in vivo corrosion performance. Surg. Sci. 3, 28–33 (2012).
Wunderlich, N. C., Beigel, R., Swaans, M. J., Ho, S. Y. & Siegel, R. J. Percutaneous interventions for left atrial appendage exclusion. J. Am. Coll. Cardiol. Cardiovasc. Imaging 8, 472–488 (2015).
Toumanides, S., Sideris, E. B., Agricola, T. & Moulopoulos, S. Transcatheter patch occlusion of the left atrial appendage using surgical adhesives in high-risk patients with atrial fibrillation. J. Am. Coll. Cardiol. 58, 2236–2240 (2011).
Moss, J. D. Left atrial appendage exclusion for prevention of stroke in atrial fibrillation: review of minimally invasive approaches. Curr. Cardiol. Rep. 16, 448 (2014).
Aryana, A. et al. Association between incomplete surgical ligation of left atrial appendage and stroke and systemic embolization. Heart Rhythm 12, 1431–1437 (2015).
Badhwar, V. et al. The Society of Thoracic Surgeons 2017 clinical practice guidelines for the surgical treatment of atrial fibrillation. Ann. Thorac. Surg. 103, 329–341 (2017).
Su, P., McCarthy, K. P. & Ho, S. Y. Occluding the left atrial appendage: anatomical considerations. Heart 94, 1166–1170 (2008).
Lee, J. M. et al. Impact of increased orifice size and decreased flow velocity of left atrial appendage on stroke in nonvalvular atrial fibrillation. Am. J. Cardiol. 113, 963–969 (2014).
Viles-Gonzalez, J. F. et al. The clinical impact of incomplete left atrial appendage closure with the Watchman device in patients with atrial fibrillation: a PROTECT AF (Percutaneous Closure of the Left Atrial Appendage Versus Warfarin Therapy for Prevention of Stroke in Patients With Atrial Fibrillation) substudy. J. Am. Coll. Cardiol. 59, 923–929 (2012).
Luis, S. A. et al. Non-pharmacological therapy for atrial fibrillation: managing the left atrial appendage. Cardiol. Res. Pract. 2012, 304626 (2012).
O’Brien, J. et al. Three-dimensional assessment of left atrial appendage orifice geometry and potential implications for device closure. Int. J. Cardiovasc. Imaging 30, 819–823 (2014).
Reed, A. M., Potter, J. & Szycher, M. A solution grade biostable polyurethane elastomer: ChronoFlex AR. J. Biomater. Appl. 8, 210–236 (1994).
Bélanger, M. C. et al. Selection of a polyurethane membrane for the manufacture of ventricles for a totally implantable artificial heart: blood compatibility and biocompatibility studies. Artif. Organs 24, 879–888 (2000).
Braunwald, E., Brockenbrough, E. C., Frahm, C. J. & Ross, J. Left atrial and left ventricular pressures in subjects without cardiovascular disease. Circulation 24, 267–269 (1961).
Vukicevic, M., Mosadegh, B., Min, J. K. & Little, S. H. Cardiac 3D printing and its future directions. J. Am. Coll. Cardiol. Cadiovasc. Imaging 10, 171–184 (2017).
Lao, L. et al. Selective mineralization of tough hydrogel lumens for simulating arterial plaque. Adv. Eng. Mater. 19, 1600591 (2016).
Giannopoulos, A. A. et al. Applications of 3D printing in cardiovascular diseases. Nat. Rev. Cardiol. 13, 701–718 (2016).
Giannopoulos, A. A. et al. 3D printed ventricular septal defect patch: a primer for the 2015 Radiological Society of North America (RSNA) hands-on course in 3D printing. 3D Print. Med. 1, 1–20 (2015).
Anwar, S. et al. 3D printing in complex congenital heart disease: across a spectrum of age, pathology, and imaging techniques. J. Am. Coll. Cardiol. Cardiovasc. Imaging 10, 953–956 (2017).
Mahmood, F. et al. Three-dimensional printing of mitral valve using echocardiographic J. Am. Coll. Cardiol. Cardiovasc. Imaging 8, 226–231 (2015).
Kolesky, D. B., Homan, K. A., Skylar-Scott, M. A. & Lewis, J. A. Three-dimensional bioprinting of thick vascularized tissues. Proc. Natl Acad. Sci. USA 113, 3179–3184 (2016).
Mosadegh, B., Xiong, G., Dunham, S. & Min, J. K. Current progress in 3D printing for cardiovascular tissue engineering. Biomed. Mater. 10, 034002 (2015).
Cheung, D. Y., Duan, B. & Butcher, J. T. Current progress in tissue engineering of heart valves: multiscale problems, multiscale solutions. Expert Opin. Biol. Ther. 15, 1155–1172 (2015).
Murphy, S. V. & Atala, A. 3D bioprinting of tissues and organs. Nat. Biotechnol. 32, 773–785 (2014).
Derby, B. Printing and prototyping of tissues and scaffolds. Science 338, 921–926 (2012).
Sündermann, S. H. et al. Implantation of personalized, biocompatible mitral annuloplasty rings: feasibility study in an animal model. Interact. Cardiovasc. Thorac. Surg. 16, 417–422 (2013).
Acknowledgements
The authors thank A. A. Amiri Moghadam for advice and support throughout the project. Scanning electron microscopy of this work was carried out in the City University of New York Advanced Science Research Center NanoFabrication Facility.
Author information
Authors and Affiliations
Contributions
S.S.R., B.M., S.N.D. and J.K.M. designed and supervised the study. S.S.R., B.M. and S.A. contributed to the writing. S.S.R. and S.A. analysed the data and performed the statistical analysis. S.S.R., S.A., H.S., J.A., K.A-F. and S.D.H. fabricated the samples and collected the data. S.S.R., B.M., S.N.D., S.A., L.B., J.K.M. and R.F.S. provided constructive comments and revised and edited the manuscript. All authors discussed the results and commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary methods and figures.
Rights and permissions
About this article
Cite this article
Robinson, S.S., Alaie, S., Sidoti, H. et al. Patient-specific design of a soft occluder for the left atrial appendage. Nat Biomed Eng 2, 8–16 (2018). https://doi.org/10.1038/s41551-017-0180-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-017-0180-z
This article is cited by
-
Low-cost prototyping of nitinol wires/frames using polymeric cores and sacrificial fixtures with application in individualized frames anchoring through the atrial septum
Scientific Reports (2023)
-
A general fruit acid chelation route for eco-friendly and ambient 3D printing of metals
Nature Communications (2022)
-
Utility of Three-Dimensional (3D) Modeling for Planning Structural Heart Interventions (with an Emphasis on Valvular Heart Disease)
Current Cardiology Reports (2020)
-
From genetics to smart watches: developments in precision cardiology
Nature Reviews Cardiology (2019)
-
Personalized occluders for the left atrial appendage
Nature Biomedical Engineering (2018)