Abstract
The COVID-19 outbreak due to SARS-CoV-2 has raised several concerns for its high transmission rate and unavailability of any treatment to date. Although major routes of its transmission involve respiratory droplets and direct contact, the infection through faecal matter is also possible. Conventional sewage treatment methods with disinfection are expected to eradicate SARS-CoV-2. However, for densely populated countries like India with lower sewage treatment facilities, chances of contamination are extremely high; as SARS-CoVs can survive up to several days in untreated sewage; even for a much longer period in low-temperature regions. With around 1.8 billion people worldwide using faecal-contaminated source as drinking water, the risk of transmission of COVID-19 is expected to increase by several folds, if proper precautions are not being taken. Therefore, preventing water pollution at the collection/distribution/consumption point along with proper implementation of WHO recommendations for plumbing/ventilation systems in household is crucial for resisting COVID-19 eruption.
Similar content being viewed by others
Introduction
A coronavirus (CoV) linked disease was identified in Wuhan, the capital of Hubei province, China in December 2019. On 12th February 2020, it was officially named as COVID-19, abbreviated form of coronavirus disease 2019, by the World Health Organisation (WHO). The virus responsible for this pneumonia associated COVID-19 outbreak, was initially designated as 2019-nCoV. However, it was later changed to severe acute respiratory syndrome coronavirus-2 or SARS-CoV-2, because of its close genetic resemblance (88% similarity) with two bat-originated SARS-like coronaviruses (bat-SL-CoVZC45 and bat-SL-CoVZXC21)1. Apart from that, the SARS-CoV-2 shows approximately 79% genetic similarity to SARS-CoV and ~50% similarity to middle east respiratory syndrome coronavirus (MERS-CoV)1,2. On 11th March 2020, WHO declared COVID-19 a pandemic, indicating the huge risk of global exposure that it possesses; furthermore, pointing towards the need for protective measures. Reports from affected countries suggested droplets and direct contact to be the major modes of transmission of SARS-CoV-2 among humans3. However, transmission through the faecal–oral route can never be undermined considering the historical evidence of SARS-CoV and MERS-CoV led wastewater contamination through human waste4,5,6.
If the freshwater or sewage is adulterated with SARS-CoV-2, it can pose a potential threat to a larger amount of population worldwide. Even when infected patients are isolated in quarantine centres, the freshwater source or sewer systems in public places or hospitals contaminated with SARS-CoV-2 might defeat the purpose of quarantine with awful consequences7. The possibility of spreading of COVID-19 cannot be neglected even if the infected individuals are exiled from a particular area. The presence of SARS-CoV-2 in water and sewage undermined the quarantine practice, unless proper attention is not sought to prevent the possible contamination of receiving water bodies along with proper biomedical waste disposal. This review elaborately summarises the current scenario on the possibility of faecal–oral transmission of COVID-19 and related water contamination along with the precautionary measures that need to be taken by the government as well as by the individuals with an eye on knowledge-based scientific resolution to confront the COVID-19 outbreak.
What is SARS-CoV-2 and how does it transmit?
SARS-CoV-2s are single-stranded; spherical shaped; positive-sense RNA viruses (genome size: 29,903 nucleotides)3 with helical symmetry, belonging to the family Coronaviridae8,9. These beta coronaviruses express dense glycosylated spiked (9–12 nm long)2 proteins on their surface and show high-affinity binding to the human angiotensin-converting enzyme 2 (ACE2) receptors10. The ACE2s are membrane glycoproteins, highly expressed in organs like lungs, kidney, heart, etc., and play an important role in cardiovascular as well as in the immunoregulation system11,12. However, in human body, expression of ACE2 receptor has been observed to be highest in intestinal enterocytes13. The SARS-CoV-2 infects its host cells, especially alveolar epithelial cells, via receptor (ACE2) mediated endocytosis, thereby affecting mainly the lower airways14. As far as transmissibility is concerned, several published reports suggested that SARS-CoV-2 has a basic reproduction number (R0; average new infections triggered by an infected person in a totally unaffected population) of 1.40–6.49, which is far more than that of presumed by WHO (1.4–2.5)15.
In general, the transmission of COVID-19 takes place via two basic routes. The first and the foremost route involves respiratory droplets. The respiratory droplets in the form of aerosols coming out of the protruding parts of the infected person’s face while sneezing or coughing can bring the risk of contaminating other people in close contact16. The other route is contact transmission, where the respiratory droplets may land on surfaces, which if come in contact with a healthy person can cause infection. This is corroborative to the previously reported investigations performed while analyzing the transmission of various CoVs through contaminated water droplets and aerosols7; similar to respiratory pathogen, Legionella, and an enteric pathogen, Cryptosporidium, which can spread upon inhaling or ingesting the contaminated water aerosols17,18. Apart from that, earlier reports suggest that aerosolization and desiccation of body fluids and faecal matter resulted in ingestion and inhalation of the dried particles, ultimately causing infection by pathogens like norovirus19 and hantavirus20. Transmission of CoVs through insect vectors like houseflies and cockroaches, who may carry the virus while in contact with infected faeces on its body or in intestinal tract, can also be a possible route of spreading COVID-19 as reported elsewhere21.
Possibility of transmission of COVID-19 through wastewater contaminated with human waste
A plethora of investigations suggests that c.a. 2–10% of the confirmed COVID-19 cases are showing diarrhoeal symptoms on the very first day of admission and have persisted even for several days after hospitalization22,23,24. Moreover, few investigations have already detected viral RNA fragments of SARS-CoV-2 in the faecal particles of infected patients24,25,26,27. These results indicate that the indirect transmission of contaminated fomites may also play a crucial role in spreading COVID-1928,29. During the 2002–2003s SARS outbreak, stool samples were tested to be positive for the outsourcing of the virus30 and RNA traces of SARS-CoV were also reported to be present in patients’ stool samples, even after 10 weeks of symptom onset6.
In case of COVID-19, the gastrointestinal (GI) symptoms like indigestion/dyspepsia, bloating and constipation at times precede the respiratory symptoms and fevers for ~10% of the cases23,26,31. Moreover, there are instances, when the patients had recuperated from the illness, however, still tested positive for the presence of viral RNA in stool samples32,33,34. In a recent investigation, detection of SARS-CoV-2 from stool sample of an asymptomatic child of 10 years of age was an eye-opener for considering stool to be an additional routine diagnostic sample apart from the respiratory tract specimens35.
Although the current investigations indicate shedding of the SARS-CoV-2 through the stool samples of a subset of patients, however, only the detection of viral-RNA does not inevitably indicate the presence of live virus in faecal matter and spread of COVID-19 through faecal–oral transmission36. Researchers from around the globe have been working in this matter and a few of them have come up with some positive results with the presence of live SARS-CoV-2 in the stool samples, which further confirms the possible faecal–oral transmission of COVID-1937. Moreover, from the virological perspective, this intestinal tropism of enveloped SARS-CoV-2 is a bit unusual as most of the diarrhoea-related viruses (i.e. adenovirus, rotavirus, norovirus etc.) are non-enveloped. These have more resistance and a lot better chances of survival in intestinal tract. However, in a recent investigation by Xing et al.38, the intestinal tropism of SARS-CoV-2 indicates much higher resistance than other enveloped viruses in the intestinal tract, which is also in corroborative to the investigation done by Leung et al. in case of SARS-CoV6.
It has been well documented that the SARS-CoV-2 utilizes ACE2 receptors to enter the host’s body39,40 and after that, the multiple copies of viral RNA and proteins are synthesized in the host cytoplasm to assemble the new virions41, which can then be released in the GI tract. In an investigation, faeces of 73 hospitalized patients with SARS-CoV-2 were tested using real-time reverse transcriptase-polymerase chain reaction (rRT-PCR) and 53.42% of the cases resulted positive in stool samples42. Surprisingly, 23.29% of the patients with viral RNA untraceable in respiratory tracts showed the presence of SARS-CoV-2 in their faeces42. Moreover, the gastric, rectal, and duodenal epithelia exhibited positive immune-fluorescent staining of viral host receptor ACE2 and viral nucleo-capsid protein in case of COVID-19 patients. Moreover, the investigators also successfully isolated infectious SARS-CoV-2 from the stool sample indicating the presence of infectious virions in the GI tract (claimed unpublished data)42. These outcomes decidedly highlighted the potential of the faecal–oral transmission route of SARS-CoV-2 in the recent worldwide outbreak31,42.
Furthermore, in a recent investigation, Wang et al. have cultured stool specimens of four COVID-19 patients with very high viral RNA copies and could observe live viruses in two of them43. Moreover, they also reported the presence of live SARS-CoV-2 in the anal swabs or blood samples; whereas, oral swabs tested negative for the same in few of the cases. Therefore, these patients would likely to be considered as COVID-19 negative through routine surveillance despite posing threat to other people by faecal–oral transmission43.
In another investigation, occasional presence of subgenomic messenger-RNA containing cells was reported in stool samples, indicating occurrence of independent active replication of SARS-CoV-2 in the GI systems24. The investigators suggested the containment measures for viral transmission to focus more on droplets rather than on fomites, as they detected infectious viral strain while cell-culturing only in lungs and throat-derived samples but not from stool samples24. However, they also emphasized on the need for further investigation to validate the same, as they had only cultured 13 samples from four patients with only one mild intermittent diarrhoea case24. In another case-study, the Chinese Centre for Disease Control and Prevention (CCDC) reported isolation of live SARS-CoV-2 from the stool sample of a laboratory confirmed patient from Heilongjiang Province, China, about 15 days after the onset of disease44. As the findings are only from a small dataset of patients, hence, further investigations are required to understand the frequency of presence of infectious viral strain and the range of viral load in faeces, which is of major concern for transmissibility in the present scenario45.
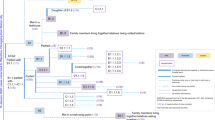
On the other hand, saliva has also been found to be positive with SARS-CoV-2, and can lead to spread of COVID-19 through aerosol transmission; or mixing of infected saliva with drinking water source; or water contaminated with infected saliva if unknowingly used for washing hands/face by the healthy individuals46. Hence, considering our current knowledge of huge SARS-Cov-2 load on saliva, sputum as well as in stool samples of COVID-19 patients, it can easily contaminate a large amount of wastewater being generated from the hospitals, quarantine centres and domestic households from the areas with positive COVID-19 cases. It can then contribute towards the elevated concentration of SARS-CoV-2 in the receiving water bodies if not being treated properly (Fig. 1).
(1) Spread of SARS-CoV-2 among humans in contact with infected animals, (2) SARS-CoV-2 may enter the sewerage system through faeces, urine, or vomit of the infected person, (3) Hospitals and quarantine centres, (4) Wastewater escaped from in-situ treatment facilities of hospitals/quarantine centres and reaching to the sewerage system, (5) Mishandling of biomedical wastes and careless disposal causing water contamination, (6) Wastewater generated from the public places, (7) Treated wastewater discharge to the receiving water bodies, (8) Bypassing of untreated, contaminated wastewater directly into the receiving water bodies, (9) Direct consumption of contaminated water by rural people or people having no access to water treatment facilities, (10) Contaminated water if properly disinfected/treated in water treatment plants can curb the spread of COVID-19 (leaky conveyance lines can also lead to contamination in water distribution systems), (11) Direct consumption of contaminated water by the urban people bypassing water treatment line, (12) Contaminated water consumption can infect healthy people in urban areas, (13) Human exposure to SARS-CoV-2 through toilet flushing and defective indoor plumbing systems, (14) Rain water and snowmelt excess water can further cause spreading of COVID-19 among unaffected human beings during major wet weather events, (15) Community spreading of COVID-19.
Current treatment options for SARS-CoV-2 contaminated wastewater
Various reports suggest that it is possible to detect faecal–oral transmitted viruses (like adenovirus, norovirus, hepatovirus, rotavirus, even CoVs) in sewage47. In a recent report, the SARS-CoV-2 load was estimated in the municipal wastewater to be in the range of 56.6 million to 11.3 billion viral genomes/infected person.day48. It was based on the previous reports on the presence of 600,00049 to 30,000,00024 number of viral genomes/ml of faecal matter, considering the faecal load to be around 100 g of faeces/person.day with 1.06 g/ml of specific density50.
The analysis of incoming sewage may thus be a useful tool to reveal the presence of excreted faecal-based viral strains to warn the government about the possible outbreak in the near vicinity of the sewage contaminated area51. Global Water Pathogen Project dynamically reported the current available technologies to control the outbreak of different enteric viruses by sewage treatment plants52. Therefore, the wastewater coming out of the contaminated areas can thus be treated by several processes in municipal wastewater treatment facilities in order to reduce the impact on the receiving water bodies53. Otherwise, if the treatment is not ensured, the enteric transmission of SARS-CoV-2 is possible and the contaminated wastewater with the viral load can pose threat to the people utilizing that water source at downstream points54.
It is well documented that the presence of predatory microorganisms like protozoa can proliferate the rate of inactivation of viruses with the catalytic action of proteases and nucleases55,56,57. In general, the conventional secondary treatment processes can remove the virus content up to 2–3 log-scale through the process of adsorption to the solid particles or enmeshment to the flocs of activated sludge58. The treatment processes involving filtration membranes (nano-filtration or reverse osmosis, RO) have proven to be another efficient approach towards the removal of viruses by filtering the solids (like cell monolayer, etc.) and solid-associated viruses. Although, the membrane filtration process apparently depends on molecular weight cut-offs (MWCO) for a higher degree of virus removal, which generally ranges from as low as 0.2 log-scale in microfiltration to more than 6.5 log-scale in RO process58.
However, the removal of viruses in all the above cases is due to the action of mechanical straining and not by inactivation of the viruses. The tertiary treatment systems like chlorine dosing, ozonation, or UV irradiation are reported to be effective for inducing inactivation of the viruses. Although, ozonation and UV irradiation are more effective than chlorine induced reactive oxygen species formation; however, the former cannot provide residual disinfection as chlorine does in the distribution pipelines58,59. Nevertheless, further scientific investigations are required on these disinfectants to decide dose and contact time for this specific SARS-CoV-2 inactivation.
Risk associated with the treatment of SARS-CoV-2 contaminated wastewater
The SARS-CoV and MERS-CoV were experimented extensively to assess the chances of transmission through the faecal–oral route60. During the 2003 SARS-CoV outbreak, it was reported that the RNA of SARS-CoV was found in the sewage treatment facilities of two hospitals in Beijing, China, where infected patients were being treated30. It was also investigated that SARS-CoV can survive up to 14 days at 4 °C, and for only 2 days at 20 °C in untreated sewage61. Moreover, the current COVID-19 situation has also raised similar concerns, due to which the Centres for disease control and prevention (CDC), USA has suggested that, transmission of SARS-CoV-2 through untreated sewage may also be possible61. Most recently, investigations performed in The Netherlands62, Australia63, Italy64, Spain65 and France66 also corroborates the same as they were successful in detecting SARS-CoV-2 in untreated sewage. Hence, if such developments occur, it will be very difficult to control the community transmission rates in subsequent days.
As per reports by the National Green Tribunal (NGT) on the effluent-discharge standards of sewage treatment plants (last updated on 8th May 2019), from densely populated developing countries like India, only 22,963 million liters per day (MLD) of sewage is treated67. However, the total generated sewage stands at 61,754 MLD, leaving behind 38,791 MLD (>60%) of sewage untreated to the receiving water bodies67. Moreover, situations like rain and snowmelt can further deteriorate the conditions causing combined sewer overflows, and ultimately resulting in untreated sewage dumping in water bodies at a larger magnitude68. In an overall health risk assessment study, the risk of infection due to the ingestion of urban floodwater for a number of waterborne pathogens like Campylobacter, Cryptosporidium, Giardia, norovirus and enterovirus, which can cause gastrointestinal diseases, was quantified69. The report showed a mean risk of infection for children in the community, who are exposed to the floodwater coming out of combined sewer overflows, storm sewers and from the surface runoff generated due to rainfall was 33%, 23% and 3.5%, respectively. However, for the adults, the corresponding mean risk of infection was 3.9%, 0.58% and 0.039%, respectively, mainly due to noroviruses and enteroviruses present in floodwater69. Therefore, the factor of risk can never be undermined for COVID-19 to spread through the human waste contaminated wastewater specifically at wet weather events.
There is further risk associated with the decentralized wastewater treatment systems, like septic tanks, because such systems do not disinfect the effluent at all. Therefore, it can contaminate the water bodies with shallow groundwater depth or areas prone to flooding or if open well used for drinking water is located within a distance of 30 m from the septic tank if appropriate precautions are not being taken70. In case of situations like disaster response, Sphere Project in 2011 has also recommended a minimum standard lateral distance of 30 m in between the onsite sanitation structures and the freshwater sources71.
On the other hand, there is a high chance of spreading SARS-CoV-2 through the aerosols formed over the uncovered aerobic wastewater treatment facilities like activated sludge process, etc.72. In an investigation, the detection of three different virus strains (norovirus, adenovirus, and the hepatitis E virus) was done over the air samples of 31 different wastewater treatment plants (WWTPs) for two seasons of two consecutive years72. The results indicated that the adenovirus was present in almost all the samples (100% in summer and 97% in winter), with the highest airborne concentration of 2.27 × 106 genome equivalent/m3. Whereas, the norovirus was sparsely detected and hepatitis E remained undetected from the air-samples obtained from the plants over time. Thus, this investigation showed the presence of potential pathogenic viral particles in the aerosols coming out of different units of WWTPs72. Although, according to the WHO interim guidance (Water, sanitation, hygiene, and waste management for the COVID-19 virus), there were no such evidences, of people working in WWTPs contracting SARS-CoV during the 2002–2003s outbreak16, it is however not to be neglected considering the chances of contamination to the workers handling these units in the current COVID-19 scenario72.
During the 2003s SARS-CoV outbreak, it was reported that defective plumbing/ ventilation systems contributed to the spreading of SARS-CoV through aerosols at the Amoy Gardens housing complex, Hong Kong, where more than 300 infections and 42 deaths occurred73,74. In the present COVID-19 outbreak, similar kind of suspected cases of infection were observed among two positive cases of residents of a high-rise tower named Hong Mei House, at north-western Hong Kong’s Tsing Yi, possibly due to faulty pipes; although later, the claims were denied by the authority75. A total of 58 COVID-19 cases were reported from a building at Kapashera in Southwest Delhi, India, question further the possibility of same because of common toilets being used by the affected persons76. Therefore, the possibility of transmission of COVID-19 can never be neglected because of faulty plumbing/ventilation systems specifically in high-rise buildings.
Current freshwater treatment options for mitigating SARS-CoV-2 contamination
The surface water treatment plants are most susceptible to viral contamination specifically during the current COVID-19 outbreak situation. Although at present, there are no reliable data available on the load of viable SARS-CoV-2 causing infection through drinking, bathing, or recreational activities, the best way to halt any chances of the same is to treat the water before ingestion at the consumer end.
The techniques including the stress due to sunlight exposure, chemical dosing for reactive oxidative species formation, or predation by other microorganisms are employed in water treatment plants to mitigate the viral contamination in general. In the case of conventional centralized water treatment plants, filtration followed by disinfection is expected to be sufficient enough to get rid of SARS-CoV-2. Although the fragile vitality of SARS-CoV-2 in open sunlight condition reduces the threat to raw water contamination, the application of chlorination and UV disinfection poses further assured inactivation of SARS-CoV-2 to an extent that it represents a low health risk to the consumer16. Furthermore, the application of secondary disinfection measures, like dosing of chloramines to maintain a certain residual chlorine level in the distribution network adds to further protection from contamination77.
Risk associated with the freshwater supply with possible SARS-CoV-2 contamination
The water treatment systems with downstream (surface water) or down gradient (groundwater) sources have rough chances of getting SARS-CoV-2 contaminated raw water supply. This happens either because of discharge from combined sewer overflows or incomplete disinfection at wastewater treatment systems or from faecal matter of infected patients present in near vicinity. The faecal–oral based or waterborne transmission of viruses is on the whole challenging in places with poor sanitation and very limited access to the uncontaminated drinking water36,60. Moreover, it has been reported that ~884 million people worldwide do not have access to fresh water, with around 1.8 billion people using the faecal contaminated source of drinking water with 4.2 billion people bereft of safely-managed sanitation; which can possibly make the COVID-19 outbreak situation even worse in days to come78,79,80.
The SARS-CoV-2 has not yet been found in any drinking water facilities and as per current pieces of evidence, it is safe to comment that the risk to drinking water supplies is low, if proper precautions are being taken. Laboratory investigations on different surrogate coronaviruses showed that they could remain infectious in the water contaminated with faecal matter for days to weeks81. Duan et al. reported that SARS-CoV can survive for at least 96 h in sputum (testing condition—1:20 dilution in phosphate buffer solution, PBS), serum, and faecal (testing condition—1:20 dilution in PBS) samples, whereas in urine for no less than 72 h though with lower infectivity82. In another investigation, it was found that the SARS-CoV could sustain for 2 days in domestic sewage, hospital wastewater, and dechlorinated tap-water4. Furthermore, SARS-CoV sustained for 3 days in faecal matter, 14 days in PBS and for 17 days in urine at 20 °C, however, at 4 °C, it could sustain for more than 17 days in both faecal matter and urine4.
Over the years, several CoV strains like transmissible gastroenteritis virus or TGEV, a Group 1 CoV-based diarrhoeal swine pathogen and mouse hepatitis virus or MHV, a Group 2 CoV-based enteric and respiratory pathogen of laboratory mice, were also investigated extensively83. Casanova et al. experimented the time needed for reduction of 99% infectious titer at 25 °C in reagent-grade water was 22 days and 17 days for TGEV and MHV, respectively7. However, there was no substantial deterioration in the infectious titer of both the viruses over a period of 49 days of observation at 4 °C in reagent grade water7. Moreover, in the natural water body (lake water in this case), a 99% reduction in infectious titer was witnessed over 13 days for TGEV and 10 days for MHV at 25 °C. In wastewater contaminated with human faecal waste, a 99% decline in infectious titer was witnessed over 9 and 7 days for TGEV and MHV, respectively at 25 °C. However, in both the cases, at 4 °C, no significant decline was witnessed even after a considerable amount of observational period7. During another investigation, survival times of CoVs in tap water and wastewater was estimated using representative CoVs like, feline infectious peritonitis virus (FIPV) and human coronavirus 229E (HCoV), where required time for both the virus titers to reduce by 99.9% (T99.9) in tap water was 10 days at 23 °C compared to more than 100 days at 4 °C, whereas in wastewater the T99.9 values were around 2–3 days at 23 °C84. Apart from these, during the most recent COVID-19 outbreak; serum, sputum, faeces and urine samples have also tested positive for SARS-CoV-2 for up to 2–14 days, 3–14 days, 1–12 days and ~7 days, respectively, in different investigations26,27,35,42,85,86.
Therefore, from the above observations, it is clearly evident that the incubation time and temperature are significant factors for viral reduction or inactivation in the water distribution system, which is corroborative to the previous researches on the survival of different viruses in water87,88,89. Therefore, the possibility of long term survival and related airborne faecal-droplet transmission system showed that faecal-contaminated media (aqueous) could stance a major health risk in the COVID-19 outbreak if proper precautions are not being taken (Table 1).
Precationary measures to be taken to control further spreading of COVID-19
-
In order to ensure appropriate control over water quality, necessary measures required to be taken include: preventing pollution of water at the point source, i.e. proper water treatment at the distribution/collection/consumption point; storing treated water properly in clean and well-covered vessels, etc. Unlike coxsackieviruses, SARS-CoV-2s are surrounded by a non-robust lipid membrane, making them susceptible to inactivation by chlorine or other disinfectants. Therefore, efficient disinfection of water using conventional methods should be followed in order to maintain the free residual chlorine concentration of ≥0.5 mg/L after 30 min of exposure at pH < 8.0 throughout the distribution system90. In a recent investigation, a successful approach has been showcased how a sewage disinfection pool with sodium hypochlorite solution can completely eradicate the SARS-CoV-2 load from the sewage generated from the isolation wards of First Affiliated Hospital of Zhejiang University, China91. Moreover, the technical persons working in the close vicinity of WWTPs should take proper precautions like usage of personal protection equipment (masks, gloves, gowns and eye protection), to minimize the viral transmission through aerosols coming out of treatment units.
-
Adoption of a wastewater-based epidemiology approach will be useful for establishing an effective early warning system followed by implementation of a prompt intervention system for rapid on-site detection of SARS-CoV-2 at the wastewater source or at collection points48,92. For this, paper-based biosensors can serve as a portable and robust option for detecting SARS-CoV-2 in wastewater93. Apart from that, inexpensive and high throughput diagnostic platforms like Pathogen-Oriented Low-Cost Assembly & Re-Sequencing (POLAR) can also be exploited for SARS-CoV-2 monitoring in municipal WWTPs94. Such approaches could not only provide continuous real-time monitoring, however, these can also help local agencies/governments to track the possibility of community spread of COVID-19 at different waves of re-emergence at worst case scenario93. The lockdown in the United States is costing them around US$11.5 billion/day95, which can be drastically put down with proper policy-making; given the real-time data available on the presence of SARS-CoV-2 while monitoring the wastewater discharged from the places well before in hand.
-
Apart from conventional methods, in case of places, where safe piped water supplies and centralized water treatment facilities are not available, water disinfection techniques for households like boiling, nanofiltration, solar/UV irradiation or addition of free chlorine (bleaching powder) in appropriate doses, are also effective. The SARS-CoV-2 is sensitive to heating and can be completely inactivated when heated at 92 °C for 15 minutes (>6 log-scale removal)96. The irradiation by UV for a duration of 60 min can also be a good option for the destruction of CoVs activity to an undetectable level as reported elsewhere82. The SARS-CoV could be inactivated from the faeces or urine samples well within a few minutes by 500–1000 mg/L of chlorine or peracetic acid dosing as reported by Wang et al.4. Moreover, the SARS-CoV is highly susceptible to the disinfectants like free chlorine compared to chlorine dioxide than E. coli and f2 phage4.
-
When properly installed, a septic system should be located at a distance and location should be suitably designed to avoid impacting a water supply well. In the case of small health care setups at low-resource areas, where conventional treatment facilities are unavailable, pit latrines can be constructed and operated with lime addition to prevent contamination of water sources. However, one should confirm the distance between the groundwater table and the pit bottom of at least 1.5 m; horizontal separation distance between groundwater source (both shallow wells and boreholes) and latrines of at least 30 m shall be followed70.
-
According to WHO recommendations, bathroom drains should be properly sealed, plumbing systems should be well-maintained and sprayers/faucets should have backflow valves to restrict entry of faecal aerosols into pumping/ ventilation systems. Furthermore, to prevent the spreading of droplets or generation of aerosol clouds, flush toilets should have operational drain traps as details reported by Gormley et al.97. Also, while flushing, the lid of the toilet should be kept down. Apart from that, appropriate risk assessment should also be done for those healthcare setups connected to sewerage, to prevent leakage of the contaminated wastewater before reaching to the disposal sites98.
Conclusions
The alternate route of transmission of SARS-CoV-2 like human waste contaminated wastewater sources can cause further implications in restricting the COVID-19 outbreak. Steps like the confinement of the infected patients at the quarantine centres other than existing healthcare treatment facilities without proper in-situ wastewater treatment systems can further worsen the situation. In general, the conventional tertiary wastewater treatment systems like chlorination, UV irradiation are expected to be capable of eradicating SARS-CoV-2 for possible contamination. However, for densely populated countries like India, where more than 60% sewage is currently left untreated even in urban areas, chances of contamination of water bodies are extremely high with SARS-CoV-2. Therefore, preventing pollution of water at the point sources i.e. at the collection/distribution/consumption point along with the proper implementation of WHO recommendations for plumbing/ventilation systems in a household is highly necessary to control COVID-19. The perseverance of CoVs in water and sewage further advocates that the measures like quarantining, which ascertained effective containment at previous SARS outbreak, might not be effective enough if proper precautions are not being taken with the fate of biomedical wastes and wastewater discharges. Proper hygiene, social distancing and adequate onsite treatment to the sewage generated from quarantine wards, and ensuring the presence of sufficient free residual chlorine in the drinking water received at consumer end are thus some of the important aspects to get rid of SARS-CoV-2 and related health issues to control the COVID-19 outbreak.
Data availability
Data sharing not applicable to this article as no datasets were generated or analysed during the current study.
References
Lai, C.-C., Shih, T.-P., Ko, W.-C., Tang, H.-J. & Hsueh, P.-R. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and coronavirus disease-2019 (COVID-19): the epidemic and the challenges. Int. J. Antimicrob. Agents 55, 105924 (2020).
Zu, Z. Y. et al. Coronavirus Disease 2019 (COVID-19): a perspective from China. Radiology. https://doi.org/10.1148/radiol.2020200490 (2020).
Wu, F. et al. A new coronavirus associated with human respiratory disease in China. Nature 579, 265–269 (2020).
Wang, X. W. et al. Study on the resistance of severe acute respiratory syndrome-associated coronavirus. J. Virol. Methods 126, 171–177 (2005).
Drosten, C. et al. Clinical features and virological analysis of a case of Middle East respiratory syndrome coronavirus infection. Lancet Infect. Dis. 13, 745–751 (2013).
Leung, W. K. et al. Enteric involvement of severe acute respiratory syndrome - Associated coronavirus infection. Gastroenterology 125, 1011–1017 (2003).
Casanova, L., Rutala, W. A., Weber, D. J. & Sobsey, M. D. Survival of surrogate coronaviruses in water. Water Res. 43, 1893–1898 (2009).
Dhama, K. et al. COVID-19, an emerging coronavirus infection: advances and prospects in designing and developing vaccines, immunotherapeutics, and therapeutics. Hum. Vaccin. Immunother. https://doi.org/10.1080/21645515.2020.1735227 (2020).
Rodriguez-morales, A. J. et al. COVID-19, an emerging coronavirus infection: current scenario and recent developments—an overview. J. Pure Appl. Microbiol. 14, 5–12 (2020).
del Rio, C. & Malani, P. N. COVID-19—new insights on a rapidly changing epidemic. JAMA 323, 1339–1340 (2020).
Zheng, Y.-Y., Ma, Y.-T., Zhang, J.-Y. & Xie, X. COVID-19 and the cardiovascular system. Nat. Rev. Cardiol. 17, 259–260 (2020).
Tikellis, C. & Thomas, M. C. Angiotensin-converting enzyme 2 (ACE2) is a key modulator of the renin angiotensin system in health and disease. Int. J. Pept. https://doi.org/10.1155/2012/256294 (2012).
Lamers, M. M. et al. SARS-CoV-2 productively infects human gut enterocytes. Science. https://doi.org/10.1126/science.abc1669 (2020).
Jiang, F. et al. Review of the Clinical Characteristics of Coronavirus Disease 2019 (COVID-19). J. Gen. Intern. Med. 35, 1545–1549 (2020).
Liu, Y., Gayle, A. A., Wilder-Smith, A. & Rocklöv, J. The reproductive number of COVID-19 is higher compared to SARS coronavirus. J. Travel Med. 27, taaa021 (2020).
Organization (WHO), W. H. Water, sanitation, hygiene, and waste management for the COVID-19 virus. https://apps.who.int/iris/bitstream/handle/10665/331499/WHO-2019-nCoV-IPC_WASH-2020.2-eng.pdf?sequence=1&isAllowed=y (2020).
Patel, R., Moore, M. R. & Fields, M. S. Legionellosis. Bact. Infect. Humans: Epidemiol. Control 19, 395–413 (2009).
Outbreak of Cryptosporidiosis associated with a water sprinkler Fountain—Minnesota, 1997. Morb. Mortal. Wkly. Rep. https://www.cdc.gov/mmwr/preview/mmwrhtml/00055289.htm (1998).
Marks, P. J. et al. A school outbreak of Norwalk-like virus: evidence for airborne transmission. Epidemiol. Infect. 131, 727–736 (2003).
LeDuc, J. W. Hantaviruses. in Viral Infections of Humans. Springer, Boston, MA. https://doi.org/10.1007/978-1-4899-0036-4_12 (1997).
Dehghani, R. & Kassiri, H. A brief review on the possible role of houseflies and cockroaches in the mechanical transmission of Coronavirus Disease 2019 (COVID-19). Arch. Clin. Infect. Dis. https://doi.org/10.5812/archcid.102863 (2020).
Chen, N. et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet 395, 507–13 (2020).
Wang, D. et al. Clinical characteristics of 138 hospitalized patients with 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA - J. Am. Med. Assoc. 323, 1061–1069 (2020).
Wölfel, R. et al. Virological assessment of hospitalized patients with COVID-2019. Nature 581, 465–469 (2020).
Huang, C. et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 395, 497–506 (2020).
Holshue, M. L. et al. First case of 2019 Novel Coronavirus in the United States. N. Engl. J. Med. 382, 929–936 (2020).
Zhou, P. et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579, 270–273 (2020).
Mallapaty, S. How sewage could reveal true scale of coronavirus outbreak. Nature 580, 176–177 (2020).
Lesté-Lasserre, C. Coronavirus found in Paris sewage points to early warning system. Science. https://doi.org/10.1126/science.abc3799 (2020).
Wang, X. W. et al. Concentration and detection of SARS coronavirus in sewage from Xiao Tang Shan hospital and the 309th Hospital of the Chinese People’s Liberation Army. Water Sci. Technol. 52, 213–221 (2005).
Gu, J., Han, B. & Wang, J. COVID-19: gastrointestinal manifestations and potential fecal–oral transmission. Gastroenterology 158, 1518–1519 (2020).
Kam, K. et al. A well infant with coronavirus disease 2019 with high viral load. Clin. Infect. Dis. https://doi.org/10.1093/cid/ciaa201 (2020).
Ling, Y. et al. Persistence and clearance of viral RNA in 2019 novel coronavirus disease rehabilitation patients. Chin. Med. J. (Engl.). 133, 1039–1043 (2020).
Wang, W. et al. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA - J. Am. Med. Assoc. 323, 1843–1844 (2020).
Tang, A. et al. Detection of Novel Coronavirus by RT-PCR in stool specimen from asymptomatic child, China. Emerg. Infect. Dis. 26, 1337–1339 (2020).
de Graaf, M. et al. Sustained fecal-oral human-to-human transmission following a zoonotic event. Curr. Opin. Virol. 22, 1–6 (2017).
Xu, Y. et al. Characteristics of pediatric SARS-CoV-2 infection and potential evidence for persistent fecal viral shedding. Nat. Med. 26, 502–505 (2020).
Xing, Y.-H. et al. Prolonged viral shedding in feces of pediatric patients with Coronavirus Disease 2019. J. Microbiol. Immunol. Infect. https://doi.org/10.1016/j.jmii.2020.03.021 (2020).
Munster, V. J., Koopmans, M., van Doremalen, N., van Riel, D. & de Wit, E. A novel coronavirus emerging in China—key questions for impact assessment. N. Engl. J. Med. 382, 692–694 (2020).
Harmer, D., Gilbert, M., Borman, R. & Clark, K. L. Quantitative mRNA expression profiling of ACE 2, a novel homologue of angiotensin converting enzyme. FEBS Lett. 532, 107–110 (2002).
Weiss, S. R. & Navas-Martin, S. Coronavirus pathogenesis and the emerging pathogen severe acute respiratory syndrome Coronavirus. Microbiol. Mol. Biol. Rev. 69, 635–664 (2005).
Xiao, F. et al. Evidence for gastrointestinal infection of SARS-CoV-2. Gastroenterology 158, 1831–1833 (2020).
Zhang, W. et al. Molecular and serological investigation of 2019-nCoV infected patients: implication of multiple shedding routes. Emerg. Microbes Infect. 9, 386–389 (2020).
Zhang, Y. et al. Isolation of 2019-nCoV from a Stool Specimen of a Laboratory-Confirmed Case of the Coronavirus Disease 2019 (COVID-19). China CDC Wkly. 2, 123–124 (2020).
Lee, P. I. & Hsueh, P. R. Emerging threats from zoonotic coronaviruses-from SARS and MERS to 2019-nCoV. J. Microbiol. Immunol. Infect. https://doi.org/10.1016/j.jmii.2020.02.001 (2020).
Xu, R. et al. Saliva: potential diagnostic value and transmission of 2019-nCoV. Int. J. Oral. Sci. 12, 11 (2020).
Bosch, A. Human enteric viruses in the water environment: a minireview. Int. Microbiol. 1, 191–196 (1998).
Hart, O. E. & Halden, R. U. Computational analysis of SARS-CoV-2/COVID-19 surveillance by wastewater-based epidemiology locally and globally: Feasibility, economy, opportunities and challenges. Sci. Total Environ. 730, 138875 (2020).
Zhang, N. et al. Virus shedding patterns in nasopharyngeal and fecal specimens of COVID-19 patients. Preprint at https://doi.org/10.1101/2020.03.28.20043059v1 (2020).
Brown, D. M., Butler, D., Orman, N. R. & Davies, J. W. Gross solids transport in small diameter sewers. Water Sci. Technol. 33, 25–30 (1996).
Hellmér, M. et al. Detection of pathogenic viruses in sewage provided early warnings of hepatitis A virus and norovirus outbreaks. Appl. Environ. Microbiol. 80, 6771–6781 (2014).
Global Water Pathogen Project. In Part four. Management of risk from excreta and wastewater. Global Water Pathogen Project. http://www.waterpathogens.org/node/103 (2019).
Bhowmick, G. D., Das, S., Ghangrekar, M. M., Mitra, A. & Banerjee, R. Improved wastewater treatment by combined system of microbial fuel cell with activated carbon/TiO2 cathode catalyst and membrane bioreactor. J. Inst. Eng. Ser. A. 100, 675–682 (2019).
Lodder, W. & de Roda Husman, A. M. SARS-CoV-2 in wastewater: potential health risk, but also data source. Lancet Gastroenterol. Hepatol. 5, 533–534 (2020).
Gerba, C. P., Stagg, C. H. & Abadie, M. G. Characterization of sewage solid-associated viruses and behavior in natural waters. Water Res. 12, 805–812 (1978).
John, D. E. & Rose, J. B. Review of factors affecting microbial survival in groundwater. Environ. Sci. Technol. 39, 7345–7356 (2005).
Yang, H. et al. Design of wide-spectrum inhibitors targeting coronavirus main proteases. PLoS Biol. 3, 1742–1752 (2005).
Zhang, C. M., Xu, L. M., Xu, P. C. & Wang, X. C. Elimination of viruses from domestic wastewater: requirements and technologies. World J. Microbiol. Biotechnol. 32, 1–9 (2016).
Du, Y. et al. Formation and control of disinfection byproducts and toxicity during reclaimed water chlorination: a review. J. Environ. Sci. 58, 51–63 (2017).
Yeo, C., Kaushal, S. & Yeo, D. Enteric involvement of coronaviruses: is faecal–oral transmission of SARS-CoV-2 possible? Lancet Gastroenterol. Hepatol. 5, 335–337 (2020).
Coronavirus Disease 2019 (COVID-19). Centers for Disease Control and Prevention (CDC). https://www.cdc.gov/coronavirus/2019-ncov/php/water.html (2020).
Medema, G., Heijnen, L., Elsinga, G., Italiaander, R. & Brouwer, A. Presence of SARS-Coronavirus-2 RNA in Sewage and Correlation with Reported COVID-19 Prevalence in the Early Stage of the Epidemic in The Netherlands. Environ. Sci. Technol. Lett. A-F. https://doi.org/10.1021/acs.estlett.0c00357 (2020).
Ahmed, W. et al. First confirmed detection of SARS-CoV-2 in untreated wastewater in Australia: a proof of concept for the wastewater surveillance of COVID-19 in the community. Sci. Total Environ. 728, 138764 (2020).
La Rosa, G. et al. First detection of SARS-CoV-2 in untreated wastewaters in Italy. Sci. Total Environ. 736, 139652 (2020).
Randazzo, W., Cuevas-Ferrando, E., Sanjuan, R., Domingo-Calap, P. & Sanchez, G. Metropolitan wastewater analysis for COVID-19 epidemiological surveillance. Preprint at https://doi.org/10.1101/2020.04.23.20076679v2 (2020).
Wurtzer, S., Marechal, V., Mouchel, J.-M. & Moulin, L. Time course quantitative detection of SARS-CoV-2 in Parisian wastewaters correlates with COVID-19 confirmed cases. Preprint at https://doi.org/10.1101/2020.04.12.20062679v1.full.pdf (2020).
National status of waste water generation & treatment. ENVIS Centre on Hygiene, Sanitation, Sewage Treatment Systems and Technology. http://www.sulabhenvis.nic.in/Database/STST_wastewater_2090.aspx (2019).
Tibbetts, J. Combined sewer systems: down, dirty, and out of date. Environ. Health Perspect. 113, A 465–A 467 (2005).
De Man, H. et al. Quantitative assessment of infection risk from exposure to waterborne pathogens in urban floodwater. Water Res. 48, 90–99 (2014).
Banks, D., Karnachuk, O. V., Parnachev, V. P., Holden, W. & Frengstad, B. Groundwater contamination from rural pit latrines: examples from Siberia and Kosova. J. Chart. Inst. Water Environ. Manag. 16, 147–152 (2002).
The Sphere Project & The Sphere Project. 4. Minimum Standards in Water Supply, Sanitation and Hygiene Promotion. in Humanitarian Charter and Minimum Standards in Humanitarian Response. https://doi.org/10.3362/9781908176202.004 (2011).
Masclaux, F. G., Hotz, P., Gashi, D., Savova-Bianchi, D. & Oppliger, A. Assessment of airborne virus contamination in wastewater treatment plants. Environ. Res. 133, 260–265 (2014).
Wigginton, K. R., Ye, Y. & Ellenberg, R. M. Emerging investigators series: The source and fate of pandemic viruses in the urban water cycle. Environ. Sci.: Water Res. Technol. 1, 735–746 (2015).
Yu, I. T. S., Qiu, H., Tse, L. A. & Wong, T. W. Severe acute respiratory syndrome beyond amoy gardens: completing the incomplete legacy. Clin. Infect. Dis. 58, 683–686 (2014).
Regan, H. How can the coronavirus spread through bathroom pipes? Experts are investigating in Hong Kong. CNN. https://edition.cnn.com/2020/02/12/asia/hong-kong-coronavirus-pipes-intl-hnk/index.html (2020).
Press Trust of India. Kapashera hot spot: No space for social-distancing in cramped rooms, common toilets. INDIA TODAY. https://www.indiatoday.in/india/story/kapashera-hot-spot-no-space-for-social-distancing-in-cramped-rooms-common-toilets-1673968-2020-05-03 (2020).
Li, R. A., McDonald, J. A., Sathasivan, A. & Khan, S. J. Disinfectant residual stability leading to disinfectant decay and by-product formation in drinking water distribution systems: a systematic review. Water Res. 153, 335–348 (2019).
Naidoo, S. & Olaniran, A. O. Treated wastewater effluent as a source of microbial pollution of surface water resources. Int. J. Environ. Res. Public Health 11, 249–270 (2013).
Water Quality and Wastewater. United Nations. https://www.unwater.org/water-facts/quality-and-wastewater/ (2020).
Heller, L., Mota, C. R. & Greco, D. B. COVID-19 faecal-oral transmission: Are we asking the right questions? Sci. Total Environ. 729, 138919 (2020).
Rabenau, H. F. et al. Stability and inactivation of SARS coronavirus. Med. Microbiol. Immunol. 194, 1–6 (2005).
Duan, S. M. et al. Stability of SARS Coronavirus in human specimens and environment and its sensitivity to heating and UV irradiation. Biomed. Environ. Sci. 16, 246–55 (2003).
Jackwood, M. W. The relationship of severe acute respiratory syndrome Coronavirus with avian and other Coronaviruses. Avian Dis. 50, 315–320 (2006).
Gundy, P. M., Gerba, C. P. & Pepper, I. L. Survival of Coronaviruses in Water and Wastewater. Food Environ. Virol. 1, 10–14 (2009).
Peng, L. et al. SARS-CoV-2 can be detected in urine, blood, anal swabs, and oropharyngeal swabs specimens. J. Med. Virol. 1–5. https://doi.org/10.1002/jmv.25936 (2020).
World Health Organization. Laboratory testing for 2019 novel coronavirus (2019-nCoV) in suspected human cases. https://www.who.int/publications-detail/laboratory-testing-for-2019-novel-coronavirus-in-suspected-human-cases-20200117 (2020).
Yates, M. V., Gerba, C. P. & Kelley, L. M. Virus persistence in groundwater. Appl. Environ. Microbiol. 49, 778–781 (1985).
Hurst, C. J., Benton, W. H. & McClellan, K. A. Thermal and water source effects upon the stability of enteroviruses in surface freshwaters. Can. J. Microbiol. 35, 474–480 (1989).
Enriquez, C. E., Hurst, C. J. & Gerba, C. P. Survival of the enteric adenoviruses 40 and 41 in tap, sea, and waste water. Water Res. 29, 2548–2553 (1995).
World Health Organization. Guidelines for Drinking-Water Quality: Fourth Edition Incorporating the First Addendum. Guidelines for Drinking-Water Quality: Fourth Edition Incorporating the First Addendum. https://www.ncbi.nlm.nih.gov/pubmed/28759192 (2017).
Wang, J. et al. SARS-CoV-2 RNA detection of hospital isolation wards hygiene monitoring during the Coronavirus Disease 2019 outbreak in a Chinese hospital. Int. J. Infect. Dis. 94, 103–106 (2020).
Ghernaout, D. & Elboughdiri, N. Environmental engineering for stopping viruses pandemics. Open Access Library J. https://doi.org/10.4236/oalib.1106299 (2020).
Mao, K., Zhang, H. & Yang, Z. Can a paper-based device trace COVID-19 sources with wastewater-based epidemiology? Environ. Sci. Technol. 54, 3733–3735 (2020).
Hilaire, B. G. S. et al. A rapid, low cost, and highly sensitive SARS-CoV-2 diagnostic based on whole genome sequencing. Preprint at https://doi.org/10.1101/2020.04.25.061499 (2020).
Cornwall, W. Can you put a price on COVID-19 options? Experts weigh lives versus economics. Science. https://doi.org/10.1126/science.abb9969 (2020).
Pastorino, B., Touret, F., Gilles, M., de Lamballerie, X. & Charrel, R. N. Evaluation of heating and chemical protocols for inactivating SARS-CoV-2. Preprint at https://doi.org/10.1101/2020.04.11.036855v1.full (2020).
Gormley, M., Aspray, T. J. & Kelly, D. A. COVID-19: mitigating transmission via wastewater plumbing systems. Lancet Glob. Heal. 8, E643 (2020).
Bartram, J., Brocklehurst, C., Bradley, D., Muller, M. & Evans, B. Policy review of the means of implementation targets and indicators for the sustainable development goal for water and sanitation. npj Clean. Water 1, 3 (2018).
Acknowledgements
This work was financially supported by the ReWater project, Aditya Choubey Center for Re-Water Research, Indian Institute of Technology Kharagpur, India [Project code: IIT/SRIC/EF/CRW/2018-19/045].
Author information
Authors and Affiliations
Contributions
All authors contributed literature review, data analysis and intellectual input to this review article. G.D.B., D.D. and D.N. drafted the first version of the article with the help from M.M.G. and content guidance from M.M.G., R.B., S.D. and J.C.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bhowmick, G.D., Dhar, D., Nath, D. et al. Coronavirus disease 2019 (COVID-19) outbreak: some serious consequences with urban and rural water cycle. npj Clean Water 3, 32 (2020). https://doi.org/10.1038/s41545-020-0079-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41545-020-0079-1
This article is cited by
-
Exposure risks to SARS-CoV-2 (COVID-19) in wastewater treatment plants: a review
Sustainable Water Resources Management (2024)
-
Optimization of food-energy-water-waste nexus in a sustainable food supply chain under the COVID-19 pandemic: a case study in Iran
Environment, Development and Sustainability (2023)
-
Water and wastewater digital surveillance for monitoring and early detection of the COVID-19 hotspot: industry 4.0
International Journal of Environmental Science and Technology (2023)
-
Impact of COVID-19 pandemic on aircraft noise levels, annoyance, and health effects in an urban area in Oman
Environmental Science and Pollution Research (2022)
-
Investigating SARS-CoV-2 RNA in five municipal wastewater treatment plants, hospital wastewater and wastewater collection networks during the COVID-19 pandemic in Ardabil Province, Iran
Applied Water Science (2022)