Abstract
Prediction of the transition from stable to acute coronary syndromes driven by vascular inflammation, thrombosis with subsequent microembolization, and vessel occlusion leading to irreversible myocardial damage is still an unsolved problem. Here, we introduce a multi-targeted and multi-color nanotracer platform technology that simultaneously visualizes evolving danger patterns in the development of progressive coronary inflammation and atherothrombosis prior to spontaneous myocardial infarction in mice. Individual ligand-equipped perfluorocarbon nanoemulsions are used as targeting agents and are differentiated by their specific spectral signatures via implementation of multi chemical shift selective 19F MRI. Thereby, we are able to identify areas at high risk of and predictive for consecutive development of myocardial infarction, at a time when no conventional parameter indicates any imminent danger. The principle of this multi-targeted approach can easily be adapted to monitor also a variety of other disease entities and constitutes a technology with disease-predictive potential.
Similar content being viewed by others
Introduction
Cardiovascular disease is worldwide a major cause of mortality and morbidity1 and, thus, has made the identification of patients at high risk for myocardial infarction (MI) or stroke a key challenge. A major driver towards vessel occlusion is vascular thromboinflammation, resulting in the activation of pro-thrombotic and pro-inflammatory functions of endothelial cells, which in turn leads to dysregulation of coagulation, complement, platelet activation, and leukocyte recruitment in the microvasculature2. For risk assessment and therapeutic decision making, one ideally would like to monitor the entire underlying pathophysiological cascade with early endothelial activation, vascular inflammation, thrombus formation at the arterial wall, and subsequent microembolization, finally culminating into total vessel occlusion and acute MI3,4. Simultaneous identification of these interlaced processes would require a multi-level approach for timely visualization of the emerging danger patterns at the culprit site of the coronary circulation, causing transition from stable to acute coronary syndromes with plaque formation over erosion to rupture5. Data of the present study demonstrate that this goal can be achieved within a single imaging session using a novel multi-targeted MRI-based approach.
Among the molecular imaging approaches, fluorine (19F) MRI has recently emerged as a promising tool for visualizing disease markers that offer information beyond anatomical alterations. 19F is an intrinsically sensitive nucleus for MRI6; there is negligible endogenous 19F in the body and, thus, no background signal which allows the detection and exact localization of fluorinated materials as ‘hotspots’ by combined 1H/19F MRI7. In addition, there is a family of compounds, perfluorocarbons, which exhibits a very high fluorine pay-load and that is biochemically and physiologically inert8. Perfluorocarbon nanoemulsions (PFCs) are readily ingested by blood monocytes allowing us and others to track their migration into inflammatory foci in vivo9,10,11,12. Using an ’active targeting’ approach by equipping PFCs with an α2-antiplasmin peptide (α2AP) cross-linking to the developing fibrin network by FXIIIa13,14, also the occurrence of freshly formed thrombi could lately be monitored in vivo15.
In the present study, we have raised this approach to the next level for simultaneous detection of multiple specific imaging signatures that we have termed cardiovascular danger patterns. We demonstrate that this allows the reliable identification of arterial vasculature at risk for imminent occlusive thrombosis thus predicting the occurrence of MI in the ‘HypoE’ mouse model16,17. This diet-induced model of spontaneous MI closely recapitulates human pathophysiology, including the entire cascade of inflammatory coronary plaque development, atherothrombosis, microembolization, and vessel occlusion with subsequent MI. To visualize the individual steps of thromboinflammation in this model, we developed multi-targeted PFCs with distinct spectral properties for concomitant monitoring of major biological hallmarks of disease progression. For the true simultaneous imaging of multiple PFC signals, we further evolved multi chemical shift selective 19F MRI allowing the time-saving and artefact-free acquisition of, in principle, any number of 19F resonance frequencies.
Results
Early detection of cardiovascular inflammation prior to loss of endothelial integrity
First, we explored whether our approach can identify inflammatory patterns at exquisitely early stages in this mouse model. For this, repetitive injections of neat (untargeted) perfluorocrown ether emulsions (PFCE) together with late gadolinium (Gd) enhancement (LGE) were employed for longitudinal monitoring of infiltrating immune cells and occurrence of ischemia, respectively (see timeline in Supplementary Fig. 1). Animals received PFCs two days prior to MRI allowing for adequate 19F loading of immune cells and their subsequent migration into inflammatory foci. LGE was carried out only after 19F MRI to avoid alterations of 19F relaxation times impacting on quantification.
Serial 19F MRI was performed over 15 days as shown in Fig. 1: As early as day 5 after the initiation of atherogenic diet, 19F signal was detected at the branching site of right common carotid and subclavian artery; an area known as prone to premature plaque development (Fig. 1a, 19F superimposed in red over anatomical 1H MRI (greyscale)). Follow-up on day 10 revealed increased PFC depositions in the aortic arch and beginning inflammation at the base of the heart (Fig. 1b, c, left). Of note, no signal enhancement was observed at the site of 19F signal upon Gd application, excluding any loss of membrane integrity at this time (Fig. 1b, c right (LGE) vs. middle (native)). Five days later (day 15), there was a further increase of 19F signal at the same site indicative of progressing annular inflammation now associated with a congruent LGE pattern (Fig. 1d); the same was observed in the apex consistent with previous reports on MI location16 in this model (Supplementary Fig. 2). Post mortem 3D high resolution 1H/19F MRI demonstrated that the 19F label was co-located with the proximal large coronary arteries, reflecting infiltration of PFC-loaded immune cells into inflammatory hotspots within the coronary ostia and aortic valves as classical predilection sites of atherosclerosis (Fig. 1e, left and middle). Similar time courses were regularly observed in all mice from a cohort of six (see below and Supplementary Figs. 3–7).
Tracking of PFC-loaded immune cells in the same mouse 5 days (a), 10 days (b+c) and 15 days (d+e) after onset of the diet. 19F MRI data are superimposed in red over anatomical 1H MRI data (greyscale). a First investigation on day 5: Long axis view (left) showing 19F signal only at the cusp of the aortic arch. The presence of 19F signal at the branching site of right common carotid and subclavian artery at the brachiocephalic trunk was further confirmed by merging of 19F and time-of-flight MR angiography data (middle). b+c Follow-up on day 10 revealed increased PFC deposition in the aortic arch and concomitantly onset of inflammation at the base of the heart (left). The dashed rectangle (middle) indicates the perpendicular view illustrated in c. Upon Gd application, in both views no signal enhancement was observed at the site of inflammation (b+c) right (LGE) vs middle (native). d Further check-up on day 15 demonstrated progressing annular infiltration of immune cells at the heart base, now associated with congruent LGE pattern. Thus, tracking of PFC-loaded immune cells early identified myocardial tissue later prone to myocardial ischemia. e Post mortem 3D 1H/19F MRI at an isotropic resolution of 40 µm revealed that the 19F label was primarily co-located with the proximal large coronary arteries at the base of the heart (left and middle, white arrows point to the aortic root; dashed rectangle in the short axis view represents spatial orientation of the long axis view), indicating infiltration of PFC-loaded immune cells into inflammatory hotspots within the coronary ostia and aortic valves as classical predilection sites of atherosclerosis.
Subsequent pathohistological analyses combined with ex vivo MRI always and reliably corroborated the in vivo findings and confirmed (i) PFC deposition at the luminal site of the truncus brachiocephalicus and immune cells in the aortic wall on day 5 (Supplementary Fig. 3), (ii) inflammation at the base of the heart without any signs for MI or necrosis on day 10 (Supplementary Fig. 4), (iii) co-localization of immune cells and myocardial scar tissue at an advanced disease stage on day 15 (Supplementary Fig. 5), and (iv) robust detection of 19F signals irrespective of the individually different disease progression (Supplementary Fig. 6).
Altogether, these results demonstrated that—in a model exhibiting a continuum from coronary inflammation to vessel occlusion and MI—19F MRI allowed an early visualization of inflammatory processes in the coronary circulation prior to any signs of structural damage. Passive distribution of emulsion particles (∅ ≥ 100 nm) within the tissue can be excluded (→ no LGE), which is an important prerequisite for the specific targeting of epitopes inside the vascular wall. No cardiac 19F signals whatsoever were observed in mice of the same genotype but without atherogenic diet (Supplementary Fig. 7).
Multi chemical shift selective imaging for artefact-free detection of different PFCs
Next, we turned to the concurrent detection of ongoing thrombotic processes in this model. To this end, we employed ligands specific for markers of early and chronic thrombosis, such as α2AP15 and fbn (based on EP-2104R18) for targeting of FXIIIa and fibrin, respectively, that we attached to the surface of PFCs with spectral signatures distinct from PFCE: perfluorooctyl bromide (PFOB) and perfluoro-1,3,5-trimethylcyclohexane (PFCH), respectively (Fig. 2b left). Importantly, all targeted PFCs were additionally PEGylated for stealth against uptake by monocytes15 (Supplementary Fig. 8).
a Schematic presentation of the multi chemical shift selective imaging (mCSSI) pulse sequence. It can be considered as a multi-slice 3D rapid acquisition with relaxation enhancement (RARE) variant, in which slice selection is replaced by frequency selective excitation (NPE = number of phase encoding steps, NRARE = RARE factor). Narrow bandwidth excitation is followed by phase encoding of the third dimension and acquisition of the echo train with selective refocussing pulses. Gradient spoiling is required to destroy remaining transverse magnetization at the end of each cycle. This procedure is repeated for the number of excitation frequencies within one repetition time which is similar to TR of the standard RARE sequence. The method provides a complete 3D dataset for each of the excitation frequencies and allows the simultaneous acquisition of several frequencies within one scan. Either individual or (user-defined) sum images can be created from these datasets using dedicated reconstruction software. b Left: 19F MR spectra of pure PFCH (top), a mixture of PFOB + PFCE (middle) and a combination of all three PFCs (bottom). The arrows in the bottom spectrum indicate which signals were used for mCSSI. Chemical structures of PFCH, PFOB, and PFCE are given next to the spectra and signal assignments are indicated in bold. Right: 19F mCSSI images acquired from the individual resonance frequencies indicated on the left clearly demonstrate artefact-free imaging of the respective five signals. c 19F mCSSI of PFCE, PFCOB and PFCH and a composition of all PFCs (mix). Images are axial cross-sections through five microfuge tubes. The 1H image (left) shows the position of the samples with a large water phantom in the middle. Adjacent, the reconstructed 19F images for PFCE (red), PFOB (cyan), and PFCH (magenta) with the last two merged from the individual images #1 and #2, respectively (cf. b right). Note, that in the PFC mixture all three signals were found and that there are no false-positive signals.
For simultaneous, artefact-free and rapid detection of individual PFCs in a single scan, we developed a multi chemical shift selective imaging (mCSSI) sequence as schematically shown in Fig. 2a. It can be considered as a multi-slice 3D rapid acquisition with relaxation enhancement (RARE) variant, in which slice selection is replaced by frequency selective excitation. Narrow bandwidth excitation is followed by phase encoding of the third dimension and acquisition of the echo train with selective refocusing pulses. Gradient spoiling destroys remaining transverse magnetization at the end of each cycle and the entire procedure is repeated for the number of excitation frequencies within one repetition time. This approach can be applied in principle to any number of frequencies.
This sequence allowed us to specifically detect all individual 19F signals without any spill-over of neighboring 19F peaks and to image the three perfluorocarbons by simultaneous acquisition of five distinct 19F frequencies (Supplementary Table 1 and indicated by colored arrows in Fig. 2b left). As shown in Fig. 2c, 19F mCSSI enabled artefact-free detection of both separated and mixed emulsions in the same experiment. For PFCE (red), its single frequency was used, while for PFOB (cyan) and PFCH (magenta) two frequencies were excited, resulting in two images for each compound (Fig. 2b). An in-house developed software module permitted separation and image reconstruction for each frequency (Fig. 2b right) as well as summation of the individual free induction decays, in order to increase SNR for PFCs with multiple signals (Fig. 2c). There was only a minor effect of homonuclear J modulation on the utilized frequencies (Supplementary Fig. 9), well-known to occur in the linear PFOB skeleton19,20. Thus, a reliable quantification for each signal was provided by 19F mCSSI (Supplementary Fig. 10).
This flexible multi-color detection of distinct PFCs was then applied for visualization of acute and chronic thrombosis. Individual binding characteristics of α2APPFOB and fbnPFCH were verified in ex vivo generated human thrombi (Supplementary Fig. 11) and validated in a murine model of deep venous thrombosis in vivo (Supplementary Fig. 12). As expected, α2APPFOB specifically labeled only freshly developed thrombi, while fbnPFCH bound also to thrombi in later stages as robustly detected by 19F mCSSI (Supplementary Figs. 11b and 12b+c).
Multi-targeted PFCs for thromboinflammatory states in the heart
To longitudinally track the interplay of inflammation and thrombosis in the HypoE mouse we applied a mixture of PFCE/α2APPFOB/fbnPFCH after onset of the diet. Of note, all emulsions had similar physicochemical properties and comparable 19F content (Supplementary Fig. 13). Figure 3 illustrates the concurrent monitoring of PFCs targeting inflammation (red), FXIIIa (cyan) and fibrin (magenta) in the same mouse over 15 days, with 19F mCSSI data superimposed over anatomical 1H MRI data (greyscale): On day 5, low level cardiac inflammation was found at the heart base (Fig. 3a) indicative for emerging coronary inflammation without any signs of thrombosis and accompanied by normal heart function (Fig. 3b, left ventricular ejection fraction (LVEF) 67.5%). On day 10, inflammation was clearly enhanced and signals for freshly developed thrombi (FXIIIa + fibrin) as well as chronic thrombi (fibrin only) were detected at sites of inflammation that had been identified on day 5 (Fig. 3a,↔3c). This points to pathological tissue alterations without yet functional impairment as LVEF was still preserved (Fig. 3d, LVEF 66.4%). On day 15, however, left ventricular diastolic dilation with severely impaired systolic function had developed (Fig. 3e, LVEF 25.7%) indicative of a functionally relevant MI. These results strongly imply that the initial imaging signals observed within the different fluorine ‘channels’ have identified regions affected by silent thromboinflammation constituting a danger pattern predictive of a subsequent major MI.
Concurrent monitoring of PFCs targeting inflammation (red), FXIIIa (cyan) and fibrin (magenta) in the same mouse 5 days (a+b), 10 days (c+d) and 15 (e) days after onset of the diet. 19F mCSSI data are superimposed over anatomical 1H MRI data (greyscale). First investigation on day 5 indicated a low cardiac inflammation at base level and b normal function in long axis views in diastole and systole (LVEF 67.5%). The dashed rectangle indicates the perpendicular view shown in a+c. Follow-up on day 10 revealed c enhanced infiltration of immune cells and both freshly developed (FXIIIa + fibrin) and persisting thrombosis (fibrin only) at sites of preceding inflammation (cf. a). d Despite incipient thrombosis in the left ventricle cardiac function still is preserved at this time (LVEF 66.4%). e Further check-up on day 15 depicts diastolic dilation and massively impaired systolic function (LVEF 25.7%).
Premature detection of pulmonary thromboinflammation turns into right heart failure
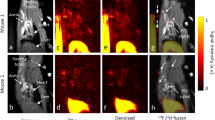
Finally, our imaging approach coincidentally identified pulmonary thromboembolism as a pathological entity hereto unknown in this model. On day 5, multi-targeted 19F MRI had identified central (hilus) acute (FXIIIa + fibrin) and chronic thrombi (fibrin only) in the lung along with pulmonary areas exhibiting low grade inflammation (red); (Fig. 4a). Interestingly, left and right ventricular (RV) function were yet uncompromized (Fig. 4b; LVEF 70.4%, RVEF 71.1%), that had sharply changed only 5 days later, where massive RV dilation and functional impairment had developed (Fig. 4c; LVEF 54.6%, RVEF 17.8%), a hallmark of pulmonary thromboembolism. As with MI, the emerging signals in the 19F ‘channels’ had identified danger patterns indicative for subsequent severe pulmonary thromboembolism (confirmed post mortem by histology, Supplementary Fig. 14).
Multi-targeted PFCs for detection of inflammation (red), FXIIIa (cyan) and fibrin (magenta) in the same mouse 5 days (a+b) and 10 days (c) after onset of the diet. a 19F mCSSI data are superimposed over anatomical 1H MRI data (greyscale) and first investigation on day 5 indicated differentially affected tissue sites mainly in pulmonary areas with b normal function in long axis views in diastole and systole (LVEF 70.4%, RVEF 71.1%). The dashed rectangle indicates the perpendicular view shown in a. c Follow-up on day 10 revealed that preceding pulmonary thromboinflammation (a) leads to severe right ventricular impairment (LVEF 54.6%, RVEF 17.8%).
Occurrence, distribution, and prognostic value of detected PFC signals
Quantification of all 19F MRI experiments (n = 50 in 23/17/10 mice on days 5/10/15) for occurrence and distribution of detected danger patterns revealed that the predominantly affected sites were the basal part of the left ventricle containing the coronary ostia/aortic valves and the pulmonary system (Fig. 5a). Linear regression analysis for the 19F signal at day x and cardiac function on day x+5 (i.e. the investigation five days later) for all follow-up measurements with detectable 19F patterns (n = 36 in 9/17/10 mice on days 5/10/15) revealed an excellent correlation (Fig. 5b). This strongly indicates that simultaneous visualization of different danger patterns by multi-targeted 1H/19F MRI can be successfully used to predict further functional impairment.
a Occurrence and distribution of detected danger patterns are expressed as percentage of animals affected by inflammation (red), acute (cyan) and chronic (magenta) thrombosis in different anatomical regions (n = 50 in 23/17/10 mice on days 5/10/15; LV, RV = left and right ventricle). b Linear regression analysis for detectable 19F signal at day x and cardiac function at day x+5, i.e. the follow-up investigation five days later (n = 36 in 9/17/10 mice on days 5/10/15, adjusted R2 = 0.84811, P = 2.926 × 10−15). The measure of center for the error band is given by the regression line of the linear fit with y = −0.0004x + 72.816 and the P value was determined from ANOVA sum of squares. Source data are provided as a source data file.
Discussion
Our findings demonstrate that multi-targeted PFCs allow the reliable identification of still silent but prognostically highly relevant thromboinflammation prior to any subsequent ischemic or thromboembolic event. By concurrent detection of several hallmarks of disease progression, it maps the entire transition from beginning coronary inflammation to microembolization, vessel occlusion and MI (Fig. 6). In principle, other disease entities, target epitopes or cell types could be approached by the same technology assuming the design of suitable ligands e.g. against neutrophils and/or platelet-leukocyte aggregates. Thus, the presented approach provides a general and versatile platform for molecular imaging with a diversity that cannot be offered by any other whole-body imaging technique at this time. The mCSSI sequence allows a highly variable spectral readout and simultaneous detection of several different targeting agents taking advantage of the broad chemical shift range for 19F (~400 vs. ~10 ppm for 1H). Although multispectral imaging efforts have been undertaken before and are not limited to MRI21,22,23, all of the reported attempts24,25,26,27 do not offer the flexibility and specificity of the in situ multi-targeting approach validated in our study.
Schematic drawing of the pathophysiological cascade from beginning coronary inflammation to atherothrombosis and vessel occlusion and the respective epitopes identified by multi-color 19F MRI. Top: Overview of the atherosclerotic continuum from coronary inflammation to occlusion in HypoE mice upon exposure to atherogenic high-fat diet. White rectangles indicate the magnified areas shown below. Bottom: 1st column: Uptake of injected PFCE droplets by circulating monocytes and early infiltration of 19F-loaded cells into inflamed endothelium; 2nd column: acute thrombosis leads to (i) incorporation of α2APPFOB into the developing fibrin network via cross-linking by FXIIIa and (ii) binding of fbnPFCH to fibrin strands; 3rd column: Advanced thrombi are labeled by fbnPFCHs only with no detectable signal for α2APPFOB due to lack of FXIIIa. Acute and advanced thrombosis are accompanied by progressing infiltration of PFCE-loaded monocytes into surrounding tissue; 4th column: Vessel occlusion results in ischemia accompanied by loss of endothelial integrity and late gadolinium enhancement.
The developed sequence is in principle applicable to any number of frequencies. Thus, we already identified another PFC, i.e. perfluoro[(tert-butyl)cyclohexane], with a clearly separated resonance frequency (Supplementary Fig. 15 top) as additional ‘color’. In proof-of-concept experiments, we verified whether this could be exploited to also visualize another key player in cardiovascular thromboinflammation: Since acute arterial thrombosis is usually platelet-rich, we employed as targeting ligand a unique single-chain antibody (scFv28), that specifically binds to the activated conformation of GPIIb/IIIa and thus to activated platelets. As demonstrated in Supplementary Fig. 15 middle and bottom, this enabled us to also track the progressive accumulation of activated platelets in diet-exposed mice. Importantly, these experiments corroborated pulmonary thrombosis as up to now unknown pathological characteristic in our mouse model, since we observed substantial platelet aggregation not only in the heart but also in the lung of mice over time (Supplementary Fig. 15 middle and bottom).
The toolbox provided by the present study thus holds the potential to map the transition from stable to unstable coronary syndromes covering the entire cascade from local inflammation, subsequent platelet adhesion, microembolization, and thromboembolism finally culminating in MI. The full encompassment of this process will allow the exact characterization of the ongoing disease state which will not only be useful for mechanistic studies in basic research but also to monitor the effectiveness of novel anti-inflammatory approaches and cellular targets to treat coronary artery disease29. Our approach holds as well translational promise for tailored patient therapy: The precise identification in which stage of this pathophysiological sequence the patient is currently in clearly goes beyond exclusive plaque recognition with surrogate parameters of inflammation and/or destabilization of the vascular wall as provided by established clinical imaging techniques. These include adverse coronary plaque characteristics and overall calcified plaque burden30, microcalcification using NaF31, enhanced glucose turnover and activated macrophages32, high intensity plaques in MRI33, activation of perivascular fat34, and direct characterization of the arterial wall by invasive approaches35,36. Unfortunately, the acuity of inflammation within atherosclerotic plaques not always matches metabolic turnover or degree of plaque activation and exhibits varying specificity depending on the vessel region32,37. Furthermore, the diagnostic triad of symptoms, changes in ECG, and elevation of troponin has been shown to reliably identify patients in whom the transition from stable coronary syndromes to acute coronary myocardial damage has already been occurred38,39,40. Similarly, microembolization currently is only detectable at late stage in MRI as microvascular obstruction41. Thus, none of these imaging or laboratory-based approaches can fully map the progressive continuum of the entire spectrum of danger patterns indicating the destabilization of arterial culprit lesions with simultaneous detection of vascular inflammation, local atherothrombosis, distal microembolization culminating in thromboembolic events such as acute MI or stroke in a single investigation.
Of course, additional investigations are needed to show that the PFC modifications carried out for specific targeting (PEGylation, ligand equipment) maintain the required safety profile for human use. Several untargeted PFCs have already been evaluated in clinical trials as artificial blood substitutes (e.g. perflubron)8,42. Although promising the application of PFCs for this purpose did not really take off, but this was less related to unexpected side effects than that they were not better than the standard of care, i.e. blood42,43. Apart from that, anti-PEG antibodies in patients could be a problem for administration of PEGylated contrast agents44. On the other hand, PEG is frequently incorporated into drug formulations to improve therapeutic efficacy and in 2020, there were 21 PEGylated drugs approved by the FDA and over 20 others in clinical trials45. Nevertheless, much effort is currently undertaken to explore the capacity of other polymers to suppress unspecific nanoparticle uptake as candidates with comparable or superior properties to PEG46,47. The modifications made to the nanoparticles may also impact on excretion pathways and biological half-life of the targeted PFCs. It is generally accepted that PFCs are released from the organism by exhalation via the lung which is consistent with the observation that the excretion rate primarily depends on their vapor pressure and permeability through the membrane48. However, also PFC transit to the gut has been observed, but this seems to be of minor relevance for humans and non-rodent species49. Importantly, there are recent reports about quickly clearing and more sustainable PFC formulations50,51, which will be helpful for bridging the gap between experimental animal studies and human applications. Nevertheless, doses and biological half-lives have to be specifically tailored for human use, but this is clearly beyond the scope of the present study and has to be adjusted in clinical trials.
In summary, PFCs with unique spectral signatures can be equipped with specific targeting ligands and utilized to simultaneously track loco-regional alterations of different specific danger patterns by multi chemical shift selective 19F MRI. Using a murine model of atherothrombotic MI mimicking the human situation, we demonstrate that this technology can be applied to serial in vivo imaging of the entire pathophysiological cascade resulting in MI and heart failure and furthermore to identify hereto unknown pathological entities in already well-characterized animal models. Of note, human scanners can readily be equipped with 19F interfaces52,53 and improved scanning algorithms54, coil design55 and relaxometry of PFCs56 will facilitate the transmission of preclinical high field findings to the clinical setting. Provided that possible side-effects as discussed above can be overcome, our approach thus offers a potentially translational perspective for identifying patients at risk for myocardial infarction, stroke, or pulmonary thromboembolism but for whom there is no anatomic correlate of risk in conventional diagnosis, allowing for individualized, informed interventions. In addition to more precisely identify the transition from stable to acute vascular disorders, our MRI-based multi-targeted nanotracer platform enables the opportunity to detect early inflammatory changes in plaque formation allowing primary prevention and to monitor effectiveness of novel anti-inflammatory targets and therapies overall enhancing the option of individualized precision medicine in disorders of vascular inflammation.
Methods
Chemicals and reagents
Chemicals
Cholesterol-PEG2000-maleimide (Nanocs); Na2HPO4, NaH2PO4, glycerol (CarlRoth GmbH); thrombin, ADP (Sigma Aldrich); E80S (Lipoid GmbH); perfluoro-15-crown-5 ether (PFCE), perfluoro-1,3,5-trimethylcyclohexane (PFCH), perfluorooctyl bromide (PFOB), diblock, i.e. F6H10, perfluoro-n-hexyl decane (Abcr chemicals). Buffer: Phosphate glycerol buffer (3 mM NaH2PO4, 7 mM Na2HPO4, glycerol 2.5% m/V, pH 7.4), phosphate buffer (PBS, CarlRoth). Targeting peptides: Peptides which were derived from α2-antiplasmin (α2AP = Ac–Gly–Asn–Gln–Glu–Gln–Val–Ser–Pro–Leu–Thr–Leu–Leu–Lys(Cys)–Trp–Lys13,15) and a peptide which was modified on the basis of EP2104-R57 (here called fbn = Tyr–D-Glu–Cys–Hyp–Tyr[3-Cl]–Gly–Leu–Cys–Tyr–Ile–Gln–Gly–Gly–Gly–Cys) were utilized for targeting. As control for α2AP, we used a peptide where the glutamic acid at position Q3 which is cross-linked to the fibrin network was replaced by alanine. The control peptide for fbn (FAM–Ser–Asp–Gly–Gly–Als–Asn–Leu–Gly–Gly–Ile–Glu–Gly–Gly–Gly–Cys) was generated by replacing and randomizing all of the amino acids which are responsible for fibrin binding58. All peptides were commercially manufactured (Genaxxon Bioscience) and fbn and its control were equipped with an additional C-terminal GGG-Cys tag and a carboxyfluorescein at the N-terminus to enable fluorescence imaging. The FXIIIa specific peptide α2AP and its control contained an additional Cys- on the ε-amino group of K13 and the carboxyfluorescein was conjugated to K15. Delivered lyophilized peptides were suspended in phosphate glycerol buffer and stored at −20 °C.
Preparation and characterization of perfluorocarbon nanoemulsions (PFCs)
Preparation
PFCs which contained perfluoro-15-crown-5 ether (PFCE), perfluorooctyl bromide (PFOB) or perfluoro-1,3,6-trimethylcyclohexane (PFCH) were prepared by microfluidization with E80S lipids as emulsifier using a laboratory processor (LV1, Microfluidics Corp.) operating at 1000 bar. PFCH and PFOB emulsions were further stabilized by adding (equimolar to the lipid content) a semifluorinated fluorocarbon/hydrocarbon diblock59. In brief, 2.4% (w/w) E80S was dissolved in 10 mM phosphate glycerol buffer. Subsequently, either PFCE (20% w/w), PFCH (40% w/w) or PFOB (40% w/w) was added to the lipid suspension. For PFCH and PFOB 35 mM diblock was additionally added. The suspensions were preemulsified by high shear mixing (Ultra Turrax TP 18/10) and processed with the LV1 at 1000 bar and for 5 cycles. PFCs were autoclaved (121 °C, 1 bar, 30 min), aliquoted in glass vials, and stored at 4 °C under light protection.
Characterization
PFCs were characterized by dynamic light scattering (DLS) using a Nanotrac instrument (Microtrac) to determine the hydrodynamic diameter, the polydispersity index (PDI) and the ζ potential. For this, 20 µl of PFCs were diluted in 1 ml Milli-Q water and analyzed for 90 s. These measurements were repeated for 10 times for calculation of mean values. To gain information on several preparations, the mean values and standard deviations of individual particle size measurements were averaged. For determination of the 19F amount, 10 µl of PFCE, PFOB, PFCH were diluted with 20 µl H2O and filled into a 200 µl reaction tube. Additionally, a 30 µl mixture of PFCs (10 µl each) was prepared. Subsequently, the reaction tubes were fixed to a 2 ml water tube and subjected to 1H/19F MRI (see below).
Functionalization of PFCs
PFCs were equipped with peptide ligands using the sterol-based post-insertion technique (SPIT)15,60. For this, peptides were coupled via free cysteines to cholesterol-PEG2000-maleimide anchors exploiting the formation of a stable thioether after reaction of the cysteine SH-group with the maleimide of the anchor. For conjugation, 280 µg of the peptide (suspended in phosphate glycerol buffer) was added to 300 µl of cholesterol-PEG2000-maleimide (1 µg/µl, suspended in phosphate glycerol buffer) and the volume was adjusted to 650 µl with phosphate glycerol buffer. The solution was incubated overnight at 22 °C under constant stirring. On the next day, 650 µl of the cholesterol-PEG2000-peptide conjugate was mixed with 650 µl of preformed PFCs and incubated at 22 °C for 3 h which led to the spontaneous insertion of the cholesterol conjugate into the lipid layer of the PFCs15,60. For targeting of activated platelets, PFCs were equipped with a unique human single-chain antibody (scFv) as previously described28. Functionalized PFCs were stored at 4 °C under light protection.
Ethics
Animal experiments were performed in accordance with the European Union guidelines described in the directive 2010/63/EU and were approved by North Rhine Westphalian State Agency for Nature, Environment and Consumer Protection (LANUV = Landesamt für Natur, Umwelt und Verbraucherschutz Nordrhein-Westfalen), Germany. In vitro studies with blood samples from healthy humans were conducted to the declaration of Helsinki and approved by Ethics Committee of the Heinrich Heine University, Düsseldorf, Germany. All healthy volunteers gave written informed consent to the collection and use of blood samples in this study.
Animals
Mice expressing a hypomorphic mutant form of ApoE (ApoE-Rh/h) and lacking the scavenger receptor class B type I (SR-BI−/−) were bred and housed with a 12L/12D cycle (light switch 6:00/18:00) at an ambient temperature of approximately 22 ± 2 °C and a humidity of 55% at the central animal facility of the Heinrich Heine University Düsseldorf, Germany. Mice were fed a standard chow diet and received tap water ad libidum. For induction of the disease model16,17, mice were exposed to a high fat/high cholesterol diet (7.5% cocoa butter, 15.8% fat, 1.25% cholesterol, 0.5% sodium cholate; Altromin). For visualization of thromboinflammatory processes by 19F MRI, mice received an intravenous bolus injection of PFCs (3 mM/kg BW) 48 h prior to MRI to ensure appropriate PFC deposition at the sites of interest9.
A total of 33 mice (males and females, 25–30 g body weight; 8–10 weeks of age) were used in this study. Twenty-three of them were subjected to the main protocol illustrated in Supplementary Fig. 1. All mice received baseline 1H MRI, PFC injections on day 3 after onset of the diet and 1H/19F MRI on day 5. Thereafter, 6 mice were sacrificed for 3D high resolution 1H/19F MRI and histology. For follow-up, 17 mice were subjected to PFC injection on day 8 and 1H/19F MRI on day 10, whereupon again 6 mice were sacrificed for post mortem analyses. Afterwards, one mouse died spontaneously, so that 10 mice received the final PFC injection on day 13 and 1H/19F MRI on day 15. Thereafter, the remaining mice were sacrificed for 3D 1H/19F MRI and pathohistological analyses. Additional 4 mice were used for the explorative study of the fourth color with scFvPFCs (Supplementary Fig. 15) and further 6 mice served as control and were not subjected to the diet but received PFC injections as indicated above (Supplementary Fig. 7).
Magnetic resonance imaging
General
Data were recorded at a Bruker AVANCEIII 9.4T wide bore NMR spectrometer driven by ParaVision 5.1 (Bruker) and operating at frequencies of 400.21 MHz for 1H and 376.54 MHz for 19F measurements9,15. Images were acquired using the Bruker microimaging unit Micro 2.5 with actively shielded gradient sets (1.5 T/m) and a 25 mm birdcage resonator (Bruker) tunable to both 1H and 19F. Mice were anaesthetized with 1.5% isoflurane and kept at 37 °C. To prevent dehydration of eye surfaces and mucous membranes, the anesthesia gas mixture was moisturized by passing the mixture through a gas-washing bottle filled with water. The front-paws and the left hind-paw were attached to ECG electrodes (Klear-Trace; CAS Medical Systems) and respiration was monitored by means of a pneumatic pillow positioned at the animal’s back. Vital functions were acquired by a M1025 system (SA Instruments) and used to synchronize data acquisition with cardiac and respiratory motion if necessary. After acquisition of initial 1H pilot scans, the resonator was immediately tuned to 19F to screen the entire thorax above the liver up to the carotid bifurcation for 19F hotspots. Thereafter, the resonator was tuned back to 1H to acquire the corresponding anatomical information for detected 19F signals and functional analysis. For superimposing the images of both nuclei, the ‘hot iron’ color look-up table provided by ParaVision was applied to 19F images. To fade out the background noise from 19F images a constant threshold was applied to 19F data and signals originating from the liver were masked for sake of clarity (cf. Supplementary Fig. 7 for a representative example of a mouse 10 days after onset of the diet illustrating a comparable 19F signal intensity in inflamed myocardium as compared to the liver as major site of PFC deposition). For subsequent intraperitoneal Gd contrast agent application (bolus of 0.2 mmol Gd-DTPA per kg body weight), the animal handling system was shortly removed from the magnet and afterwards re-inserted with exactly the same positioning. The entire scanning protocol took around 80 min and was well tolerated by all animals, which recovered within 2 min from anesthesia.
For functional and morphometric analysis, high resolution images of mouse hearts were acquired using an ECG- and respiratory-gated segmented fast gradient echo cine sequence with steady state precession (FISP). A flip angle (FA) of 15°, echo time (TE) of 1.2 ms, 128 segments and a repetition time (TR) of about 6-8 ms (depending on the heart rate) were used to acquire 16 frames per heart cycle with a field of view (FOV), 30 × 30 mm2; matrix size after zero filling (MS), 256 × 256; slice thickness (ST), 1 mm; number of averages (NA), 2; acquisition time (TAcq) per slice for one cine loop, ∼1 min. In cases of inadequate ECG recording, images were acquired with a retrospectively gated fast low angle shot sequence (IntragateFLASH, Bruker) using a FA 10°, TE 1.26 ms, TR 5.82 ms, FOV 30 × 30 mm2, MS 256 × 256, TAcq 1.5 min. For retrospective gating, a navigator slice was placed near the base of the heart, where the signal is primarily modulated by the periodically changing atrial and aortic blood volume61. Routinely, 8–10 contiguous short axis slices were required for complete coverage of the LV. Longitudinal slices orientated perpendicular to the atrio-ventricular level served to ensure appropriate scanning of the entire heart from base to apex. For evaluation of functional parameters, ventricular demarcations in end-diastole and -systole were manually drawn with the ParaVision Region-of-Interest (ROI) tool.
MR angiography (MRA) of aortic arch and carotid arteries was carried out using a flow-compensated 2D time-of-flight (TOF) FLASH sequence (FA 80°, TE 2.2 ms, TR 12.3 ms, NA 4, TAcq 4.4 min, FOV 30 × 30 mm2, MS 384 × 384)62,63. In z-direction the FOV was set to cover the entire vessel system from the aortic root up to carotid bifurcation (40 overlapping slices with a slice thickness (ST) of 0.4 mm and an interslice distance of 0.25 mm resulting in a package extent of 10.15 mm). For 3D visualization, data were imported into Amira 4.0 (Mercury Computer Systems) and resampled to isotropic voxel size using a Lanzcos filter. Afterwards, 1H MRA data were visualized in greyscale by texture-based volume rendering (VRT). For overlay, anatomical corresponding 19F MRI data (see below) were rendered by application of the ‘glow’ colormap.
19F MRI
For the initial experiments with PFCE only, 19F RARE images were essentially recorded as previously described9,64,65,66 using the following parameters: RARE factor 32, TR 2500 ms; TE 4.37 ms, MS 128 × 128, ST 2 mm, averages 256, TAcq 21.3 min. For multi-color experiments, the mCSSI pulse sequence schematically shown in Fig. 2a was developed. It can be considered as a multi-slice 3D RARE variant in which slice selection is replaced by frequency selective excitation. This allows for simultaneous imaging of molecules with complex spectra (Fig. 2b) and/or different substances. Narrow bandwidth excitation is followed by phase encoding of the third dimension and the echo train acquisition with selective refocusing pulses. Gradient spoiling is required to destroy remaining transverse magnetization at the end of each cycle. This procedure is repeated for the number of excitation frequencies within one repetition time which is similar to TR of the standard RARE sequence. Reconstruction is straightforwardly performed like for a standard multislice RARE dataset, in which slice selection is replaced by different narrow band excitation loops, and provides either a complete image set for each frequency or—to omit a manual calculation step afterwards—the user can also choose to directly create sum images from individual frequencies of a PFC with multiple resonances (such as PFOB) to improve SNR. For this, dedicated reconstruction software was developed in-house based on the LabVIEW package (National Instruments). Multi-color 19F datasets were recorded with this sequence using the following parameters: TR 2500 ms, RARE factor 32, TE 4.49 ms; bandwidths 1370 and 1610 Hz for excitation and refocussing Gaussian pulses, respectively; MS 64 × 64, ST 2 mm, NA 512; TAcq 21.3 min. The frequencies for excitation/refocussing were adjusted to the resonances of PFOB, PFCE, PFCH, and PFTBCH as listed in Supplementary Table 1. All chemical shifts relative to the CF3 resonance of PFOB were derived from non-selective spectroscopic measurements. The standard deviation of the average frequencies never exceeded 40 Hz and were well below the bandwidth of the Lorentzian-shaped lines. For 19F mCSSI, it is therefore adequate to define only one absolute excitation frequency and to assume constant chemical shifts for the other resonances.
For post mortem high resolutions measurements and subsequent histology, hearts were excised and fixed in a 1.5 ml Eppendorf cap filled with paraformaldehyde. 19F data were acquired with a 3D RARE sequence (RARE factor 32, FOV 22 × 16 × 16 mm3, MS 384 × 256 × 256, TE 21.4 ms, TR 2500 ms, NA 72, TAcq 25.36 h), while anatomical reference data were recorded with a 3D FISP sequence from the same FOV using the following parameters: TE 3.4 ms, TR, 6.8 ms, MS 512 × 384 × 256, NA 24, TAcq 51 min. After MRI measurements, serial 5 µm sections of the entire heart were stained with hematoxylin and eosin (H&E).
MRI data were imported into 3D visualization software Amira and resampled to isotropic voxel size using a Lanzcos filter. 1H MRI data were visualized in greyscale by VRT adapting the lower and upper intensity thresholds for rendering in a way that the surrounding fluid got invisible. For overlay, the ‘glow’ colormap was used to render the morphologic corresponding 19F data. After coregistration, data were analyzed in multi-planar view for exact anatomical localization of the 19F label in the hearts. For confirmation of the 19F label to be localized at the luminal site of the aorta (Supplemental Fig. 3), the vessel wall was manually segmented and its surface calculated with unconstrained smoothing. For overlay, semi-transparent surface views of the wall were generated and anatomic corresponding 19F data were rendered as described above.
Phantom experiments
To prove reliable quantification of the 19F mCSSI signals, phantom measurements were performed using the same PFCs as in in vivo experiments. PFCs were filled into 200 µl microfuge tubes and fixed in the resonator with in-house constructed specimen holder. MRI data were acquired with same parameters given above and afterwards SNR was determined for each individual excitation frequency (see below).
19F MR image analysis
19F MRI data were analyzed using an in-house developed software module based on the LabVIEW package (National Instruments) which allowed (i) an overlay on anatomical corresponding 1H MRI data, (ii) an easy separation and image reconstruction for each frequency, and (iii) also a summation of the individual free induction decays to increase SNR for PFCs with multiple signals. For quantification of the 19F signal, ROIs were drawn around the area of interest, whereas background ROIs of similar geometry were placed outside the samples. The signal-to-noise ratio was calculated from the mean of the background-corrected 19F signal divided by the standard deviation of the noise. For phantom measurements, single frequency as well as sum images were quantified from identical ROIs covering the cross sections of the individual PFC-filled vials. For a more detailed description of the 19F MRI approach, acquisition parameters, and quantification procedures, please refer to references9,64.
Cellular uptake of neat, PEGylated and PEGylated functionalized PFCs
Preparation of Atto647PFCs
Atto647 labeled PFCs were prepared as described above. In brief 100 µg of Atto647-DPPE (DPPE = 1,2-dipalmitoyl-sn-glycero-3-phosphoethanolamine; ATTO-TEC GmbH) was resuspended in phosphate-glycerol buffer containing solubilized E80S lipids and stirred for 30 min at room temperature. Subsequently, PFCs were added and a pre-emulsion was generated by high-shear mixing. The crude emulsion was subjected to five cycles of microfluidization (LV1, Microfluidics) at 1000 bar.
PEGylation and functionalization of PFCs
PEGylated PFCs were generated by incubation of 100 µl of Atto647PFCs with 100 µl of cholesterol-PEG2000-CH3 (45 µl PEG + 55 µl buffer). To generate ligand-functionalized PFCs, Fbn or α2AP were conjugated to cholesterol-PEG2000-maleimide and then inserted into the lipid surface of the PFCs by SPIT. To this end, 12.2 µl Fbn or 13.4 µl α2AP (2.5 µg/µl each) were incubated with 39.2 µl cholesterol-PEG2000-maleimide. The volume was adjusted to 100 µl with phosphate glycerol buffer and incubated overnight at 20 °C under constant motion. On the next day, 100 µl of the Fbn/α2AP conjugate and additional 12 µl of cholesterol-PEG2000-CH3 (10 µg/µl) were added to 100 µl of Atto647PFCs and incubated for 3 h at 20 °C.
Cellular uptake of PFCs by RAW macrophages and murine monocytes
RAW macrophages were detached from the culture flask by strong shaking of the flask. Approximately 5 × 105 cells were taken up in 500 µl of culture medium and incubated with 25 µl of PFCs at 37 °C for 20 min. Subsequently, cells were transferred into a FACS tube filled with 1 ml of ice cold FACS buffer (PBS, 2% FBS, 1% EDTA). Cells were washed twice with FACS buffer, finally resuspended in 500 µl FACS buffer with DAPI (1 µg/ml; to label dead cells) and analyzed on a FACS Canto II (BD Biosciences). For analysis of PFC uptake by murine monocytes, blood was obtained by venous puncture of heparinized mice. Subsequently, the withdrawn blood (~100 µl) was subjected to hypotonic erythrocyte lysis (3 ml) for 5 min at room temperature, pelleted by centrifugation and washed with ice cold FACS buffer. Incubation with PFCs was again carried out for 20 min at 37 °C. Afterward, cells were washed and labeled with antibodies against CD11b (CD11b-PE, clone M1/17; BD Biosciences) and Ly6G (Ly6G-FITC, clone 1A8, BioLegend) for 30 min at 4 °C, washed twice with FACS buffer, stained with DAPI and analyzed by flow cytometry. Monocytes were identified as CD11b+/SSClow and Ly6G negative. Mean fluorescence signals of RAW macrophages and murine monocytes were recorded in the APC channel and fluorescence signals of cells which were not exposed to PFCs were subtracted from the data of cells incubated with neat, PEGylated, and PEGylated functionalized PFCs. Please refer to Supplementary Fig. 16 for the gating scheme used to analyse RAW macrophages and murine monocytes.
In vitro generation and labeling of thrombi
Platelet rich plasma (PRP) was obtained by venous puncture from healthy volunteers and immediately centrifuged at 200 g for 10 min. The white PRP on the top of the sample was carefully withdrawn, separated in 1 ml aliquots and stored at −20 °C. For generation of acute thrombi, 1 ml of the PRP was melted on ice and mixed with 100 µl of thrombin (5 U/ml) and 10 µl of ADP (1 mM). Then 100 µl samples were transferred to wells of a round-bottom 96-well plate and incubated for 5 min. Next, α2APPFOB and/or fbnPFCH were added and incubated for additional 90 min. Thrombi were removed and washed three times with 5 ml of PBS and analyzed by IVIS (see below) or 19F MRI. To obtain subacute thrombi, PRP was activated with thrombin and ADP (as described above) and 100 µl samples were incubated in a round-bottom 96-well plate for 90 min. Formed thrombi were removed from the well, washed with PBS and incubated with fbn or ctr peptide or fbnPFCH/α2APPFOB (or the respective controls). To determine the binding of PFCs to chronic thrombi, thrombi were stored in PBS for 24 h, three days and five days at 4 °C and then incubated with the targeting probes, intensively washed with PBS and analyzed by IVIS.
Imaging of in vitro generated thrombi
Thrombi labeled with fbn/α2AP-peptides or fbn/α2APPFCs were spotted on a glass plate and the fluorescence signal of the carboxyfluorescein was determined by an IVIS Lumina II imaging system (Perkin Elmer). For quantification, ROIs were drawn around the thrombus-associated fluorescence signals and the background-corrected mean values were determined. For 19F MRI, thrombi were placed in 200 µl reaction tubes filled with PBS which were fixed at a 2 mL water tube.
Induction of deep venous thrombi in vivo
Mice were kept under anesthesia with 1.5% isoflurane and buprenorphin (0.3 mg/kg) was injected s.c. 30 min prior to surgery for analgesia. A median laparotomy was performed, and the inferior vena cava was exposed at the anatomical level of both kidneys. Subsequently, a filter paper (1 × 2 mm2) soaked with 10% FeCl3 was placed on the top of the vessel and incubated for 4 min15. To prevent any leakage of the FeCl3 to the surrounding tissue, two stretches of parafilm were placed on both sides of the vessel. After removal of the filter paper the vessel was washed with 0.9% NaCl to remove residual FeCl3. PFCs (3 mmol/kg body weight) were injected into the tail vein approximately 5 min prior to or 24 h post thrombus induction. Combined 1H/19F MRI scans were performed 24 h after PFC injection.
Data reporting
No statistical methods were used to predetermine sample size. The experiments were not randomized and the investigators were not blinded during experiments and outcome assessment. Due to the highly variable phenotype of the used animal model, each animal was analyzed on its own and included into the study.
Statistics and reproducibility
Unless otherwise indicated, all values are given as mean ± standard deviation (SD). Statistical and regression analysis was performed using OriginPro 2016 (Originlab Corporation, Wellesley Hills, USA). Data were tested for Gaussian distribution using D’Agostino and Pearson omnibus normality test. Statistical significance was assessed by Student’s two-sided t test compared to the respective control group. Histology was carried out in 22 mice and the representative findings displayed in the supplement were confirmed in at least 6 independent experiments.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
All data supporting the findings of this study are available within the article and its supplementary material. Any remaining raw data are available from the corresponding author upon reasonable request. Source data are provided with this paper.
Code availability
All in-house developed LABView modules used for raw data reconstruction are available on request.
References
Virani, S. S. et al. Heart disease and stroke statistics − 2020 update: a report from the American heart association. Circulation 141, e139–e596 (2020).
Jackson, S. P., Darbousset, R. & Schoenwaelder, S. M. Thromboinflammation: challenges of therapeutically targeting coagulation and other host defense mechanisms. Blood 133, 906–918 (2019).
Partida, R. A., Libby, P., Crea, F. & Jang, I.-K. Plaque erosion: a new in vivo diagnosis and a potential major shift in the management of patients with acute coronary syndromes. Eur. Heart J. 39, 2070–2076 (2018).
Chen, Y.-C., Huang, A. L., Kyaw, T. S., Bobik, A. & Peter, K. Atherosclerotic plaque rupture: Identifying the straw that breaks the camel’s back. Arterioscler. Thromb. Vasc. Biol. 36, e63–e72 (2016).
Libby, P., Pasterkamp, G., Crea, F. & Jang, I.-K. Reassessing the mechanisms of acute coronary syndromes. Circ. Res. 124, 150–160 (2019).
Holland, G. N., Bottomley, P. A. & Hinshaw, W. S. 19F magnetic resonance imaging. J. Magn. Reson. 28, 133–136 (1977).
Bulte, J. W. M. Hot spot MRI emerges from the background. Nat. Biotechnol. 23, 945–946 (2005).
Krafft, M. P. & Riess, J. G. Chemistry, physical chemistry, and uses of molecular fluorocarbon–hydrocarbon diblocks, triblocks, and related compounds–unique ‘apolar’ components for self-assembled colloid and interface engineering. Chem. Rev. 109, 1714–1792 (2009).
Flögel, U. et al. In vivo monitoring of inflammation after cardiac and cerebral ischemia by fluorine magnetic resonance imaging. Circulation 118, 140–148 (2008).
Ye, Y.-X. et al. Monitoring of monocyte recruitment in reperfused myocardial infarction with intramyocardial hemorrhage and microvascular obstruction by combined fluorine 19 and proton cardiac magnetic resonance imaging. Circulation 128, 1878–1888 (2013).
Balducci, A. et al. A novel probe for the non-invasive detection of tumor-associated inflammation. Oncoimmunology 2, e23034 (2013).
van Heeswijk, R. B. et al. Fluorine MR imaging of inflammation in atherosclerotic plaque in vivo. Radiology 275, 421–429 (2015).
Tung, C.-H. et al. Novel factor XIII probes for blood coagulation imaging. ChemBioChem 4, 897–899 (2003).
Miserus, R.-J. J. H. M. et al. Molecular MRI of early thrombus formation using a bimodal α2-antiplasmin–based contrast agent. JACC: Cardiovascular Imaging 2, 987–996 (2009).
Temme, S. et al. Noninvasive imaging of early venous thrombosis by 19F magnetic resonance imaging with targeted perfluorocarbon nanoemulsions. Circulation 131, 1405–1414 (2015).
Zhang, S. et al. Diet-induced occlusive coronary atherosclerosis, myocardial infarction, cardiac dysfunction, and premature death in scavenger receptor class B type I-deficient, hypomorphic apolipoprotein ER61 mice. Circulation 111, 3457–3464 (2005).
Hermann, S. et al. Imaging reveals the connection between spontaneous coronary plaque ruptures, atherothrombosis, and myocardial infarctions in hypoE/SRBI−/− mice. J. Nucl. Med. 57, 1420–1427 (2016).
Spuentrup, E. et al. Molecular magnetic resonance imaging of atrial clots in a swine model. Circulation 112, 396–399 (2005).
Shukla, H. P., Mason, R. P., Woessner, D. E. & Antich, P. P. A comparison of three commercial perfluorocarbon emulsions as high-field 19F NMR probes of oxygen tension and temperature. J. Magn. Reson. 106, 131–141 (1995).
Giraudeau, C. et al. A new paradigm for high-sensitivity 19F magnetic resonance imaging of perfluorooctylbromide. Magn. Reson. Med. 63, 1119–1124 (2010).
Ferrauto, G., Delli Castelli, D., Terreno, E. & Aime, S. In vivo MRI visualization of different cell populations labeled with PARACEST agents. Magn. Reson. Med. 69, 1703–1711 (2013).
Cormode, D. P. et al. Atherosclerotic plaque composition: analysis with multicolor CT and targeted gold nanoparticles. Radiology 256, 774–782 (2010).
Rahmer, J., Halkola, A., Gleich, B., Schmale, I. & Borgert, J. First experimental evidence of the feasibility of multi-color magnetic particle imaging. Phys. Med. Biol. 60, 1775–1791 (2015).
Schoormans, J. et al. An iterative sparse deconvolution method for simultaneous multicolor 19 F-MRI of multiple contrast agents. Magn. Reson. Med. 83, 228–239 (2020).
Partlow, K. C. et al. 19F magnetic resonance imaging for stem/progenitor cell tracking with multiple unique perfluorocarbon nanobeacons. FASEB J. 21, 1647–1654 (2007).
Chirizzi, C. et al. Multispectral MRI with dual fluorinated probes to track mononuclear sell activity in mice. Radiology 291, 351–357 (2019).
Akazawa, K. et al. Perfluorocarbon-based 19F MRI nanoprobes for in vivo multicolor imaging. Angew. Chem. Int. Ed. 57, 16742–16747 (2018).
Wang, X. et al. Fluorine-19 magnetic resonance imaging of activated platelets. J. Am. Heart Assoc. 9, e016971 (2020).
Adamstein, N. H. et al. The neutrophil-lymphocyte ratio and incident atherosclerotic events: analyses from five contemporary randomized trials. Eur. Heart J. 42, 896–903 (2021).
Williams, M. C. et al. Coronary artery plaque characteristics associated with adverse outcomes in the SCOT-HEART study. J. Am. Coll. Cardiol. 73, 291–301 (2019).
Joshi, N. V. et al. 18F-fluoride positron emission tomography for identification of ruptured and high-risk coronary atherosclerotic plaques: a prospective clinical trial. Lancet 383, 705–713 (2014).
Tarkin, J. M. et al. Detection of atherosclerotic inflammation by 68Ga-DOTATATE PET compared to [18F]FDG PET imaging. J. Am. Coll. Cardiol. 69, 1774–1791 (2017).
Noguchi, T. et al. High-intensity signals in coronary plaques on noncontrast T1-weighted magnetic resonance imaging as a novel determinant of coronary events. J. Am. Coll. Cardiol. 63, 989–999 (2014).
Oikonomou, E. K. et al. Non-invasive detection of coronary inflammation using computed tomography and prediction of residual cardiovascular risk (the CRISP CT study): a post-hoc analysis of prospective outcome data. Lancet 392, 929–939 (2018).
Waksman, R. et al. Identification of patients and plaques vulnerable to future coronary events with near-infrared spectroscopy intravascular ultrasound imaging: a prospective, cohort study. Lancet 394, 1629–1637 (2019).
Räber, L. et al. Changes in coronary plaque composition in patients with acute myocardial infarction treated with high-intensity statin therapy (IBIS-4): A serial optical coherence tomography study. JACC Cardiovasc. Imaging 12, 1518–1528 (2019).
Fernández-Friera, L. et al. Vascular inflammation in subclinical atherosclerosis detected by hybrid PET/MRI. J. Am. Coll. Cardiol. 73, 1371–1382 (2019).
Collet, J.-P. et al. 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur. Heart J. https://doi.org/10.1093/eurheartj/ehaa575, (2020).
Neumann, F.-J. et al. 2018 ESC/EACTS guidelines on myocardial revascularization. Eur. Heart J. 40, 87–165 (2019).
Knuuti, J. et al. 2019 ESC guidelines for the diagnosis and management of chronic coronary syndromes. Eur. Heart J. 41, 407–477 (2020).
Ibanez, B. et al. Cardiac MRI endpoints in myocardial infarction experimental and clinical trials: JACC scientific expert panel. J. Am. Coll. Cardiol. 74, 238–256 (2019).
Keipert, P. E. Perflubron emulsion (Oxygent(tm)): a temporary intravenous oxygen carrier. Anasthesiol. Intensivmed. Notfallmed. Schmerzther. 36(Suppl 2), S104–S106 (2001).
Castro, C. I. & Briceno, J. C. Perfluorocarbon-based oxygen carriers: Review of products and trials. Artif. Organs 34, 622–634 (2010).
Richter, A. W. & Akerblom, E. Antibodies against polyethylene glycol produced in animals by immunization with monomethoxy polyethylene glycol modified proteins. Int. Arch. Allergy Appl. Immunol. 70, 124–131 (1983).
Freire Haddad, H., Burke, J. A., Scott, E. A. & Ameer, G. A. Clinical relevance of pre-existing and treatment-induced anti-poly(ethylene glycol) antibodies. Regen. Eng. Transl. Med. 1–11 https://doi.org/10.1007/s40883-021-00198-y, (2021).
Hoang Thi, T. T. et al. The importance of poly(ethylene glycol) alternatives for overcoming PEG immunogenicity in drug delivery and bioconjugation. Polymers (Basel) 12, (2020).
Gheibihayat, S. M., Jaafari, M. R., Hatamipour, M. & Sahebkar, A. Improvement of the pharmacokinetic characteristics of liposomal doxorubicin using CD47 biomimickry. J. Pharm. Pharm. 73, 169–177 (2021).
Spahn, D. R. Blood substitutes. Artificial oxygen carriers: perfluorocarbon emulsions. Crit. Care 3, R93–R97 (1999).
Bulte, J. W. M. et al. MR cholangiography demonstrates unsuspected rapid biliary clearance of nanoparticles in rodents: Implications for clinical translation. Nanomedicine 10, 1385–1388 (2014).
Staal, A. H. J. et al. In vivo clearance of 19F MRI imaging nanocarriers is strongly influenced by nanoparticle ultrastructure. Biomaterials 261, 120307 (2020).
Tirotta, I. et al. A superfluorinated molecular probe for highly sensitive in vivo 19F-MRI. J. Am. Chem. Soc. 136, 8524–8527 (2014).
Ahrens, E. T., Helfer, B. M., O’Hanlon, C. F. & Schirda, C. Clinical cell therapy imaging using a perfluorocarbon tracer and fluorine-19 MRI. Magn. Reson. Med. 72, 1696–1701 (2014).
Rothe, M. et al. In vivo 19F MR inflammation imaging after myocardial infarction in a large animal model at 3 T. Magn. Reson. Mater. Phy. 32, 5–13 (2019).
Zhong, J., Mills, P. H., Hitchens, T. K. & Ahrens, E. T. Accelerated fluorine-19 MRI cell tracking using compressed sensing. Magn. Reson. Med. 69, 1683–1690 (2013).
Keupp, J. et al. Simultaneous dual-nuclei imaging for motion corrected detection and quantification of 19F imaging agents. Magn. Reson Med 66, 1116–1122 (2011).
Kislukhin, A. A. et al. Paramagnetic fluorinated nanoemulsions for sensitive cellular fluorine-19 magnetic resonance imaging. Nat. Mater. 15, 662–668 (2016).
Overoye-Chan, K. et al. EP-2104R: a fibrin-specific gadolinium-Based MRI contrast agent for detection of thrombus. J. Am. Chem. Soc. 130, 6025–6039 (2008).
Kolodziej, A. F., Zhang, Z., Overoye-Chan, K., Jacques, V. & Caravan, P. Peptide optimization and conjugation strategies in the development of molecularly targeted magnetic resonance imaging contrast agents. Methods Mol. Biol. 1088, 185–211 (2014).
Cornélus, C., Krafft, M. P. & Riess, J. G. Improved control over particle sizes and stability of concentrated fluorocarbon emulsions by using mixed fluorocarbon/hydrocarbon molecular dowels. Artif. Cells Blood Substit. Immobil. Biotechnol. 22, 1183–1191 (1994).
Gantert, M. et al. Receptor-specific targeting with liposomes in vitro based on sterol-PEG(1300) anchors. Pharm. Res. 26, 529–538 (2009).
Heijman, E. et al. Comparison between prospective and retrospective triggering for mouse cardiac MRI. NMR Biomed. 20, 439–447 (2007).
Jacoby, C. & Flögel, U. MR for the investigation of murine vasculature. Methods Mol. Biol. 771, 439–456 (2011).
Böring, Y. C. et al. Lack of ecto-5’-nucleotidase (CD73) promotes arteriogenesis. Cardiovasc. Res. 97, 88–96 (2013).
Ebner, B. et al. Early assessment of pulmonary inflammation by 19F MRI in vivo. Circ. Cardiovasc. Imaging 3, 202–210 (2010).
Flögel, U. et al. Noninvasive detection of graft rejection by in vivo 19F MRI in the early stage. Am. J. Transplant. 11, 235–244 (2011).
Flögel, U. et al. Selective activation of adenosine A2A receptors on immune cells by a CD73-dependent prodrug suppresses joint inflammation in experimental rheumatoid arthritis. Sci. Transl. Med. 4, 146ra108 (2012).
Acknowledgements
We thank Bodo Steckel for excellent technical assistance. This work was supported by the Deutsche Forschungsgemeinschaft (SFB 1116 to U.F., M.G., J.S., M.K., B.L.; TRR 259 to U.F., F.B., M.G., M.K.; FL303/6-1 to U.F.; INST 208/764-1 FUGG to U.F., TE1209/1-1 to S.T.) and the European Commission (MSCA-ITN-2019 ‘NOVA-MRI’ to U.F., J.S.; MSCA-RISE-2019 ‘PRISAR2’ to U.F.).
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
U.F. and B.L. conceived of the main concept and guided the project; S.T., F.B., and M.K. contributed to the study design; U.F., S.T, C.J., and V.F. performed MRI experiments and analyzed the data; S.T. prepared and characterized PFC emulsions; C.J. developed dedicated software modules for MRI data reconstruction and analysis, T.O. developed the mCSSI sequence; P.K. and B.L. carried out histopathological analysis; X.W. and K.P. developed and provided the scFA; F.N. contributed to MRI experiments; F.B., J.S., M.G., and M.K. helped with critical advice and discussion. U.F. and M.G. drafted the manuscript and all authors discussed the results and contributed to the writing of the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Nature Communications thanks Zahi Fayad and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Flögel, U., Temme, S., Jacoby, C. et al. Multi-targeted 1H/19F MRI unmasks specific danger patterns for emerging cardiovascular disorders. Nat Commun 12, 5847 (2021). https://doi.org/10.1038/s41467-021-26146-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-021-26146-6
This article is cited by
-
Quantitative assessment of angioplasty-induced vascular inflammation with 19F cardiovascular magnetic resonance imaging
Journal of Cardiovascular Magnetic Resonance (2023)
-
Biodegradable polyphosphoester micelles act as both background-free 31P magnetic resonance imaging agents and drug nanocarriers
Nature Communications (2023)
-
In vivo monitoring of neutrophil trafficking to sites of injury
Nature Cardiovascular Research (2023)
-
Real-time 31P NMR reveals different gradient strengths in polyphosphoester copolymers as potential MRI-traceable nanomaterials
Communications Chemistry (2023)
-
Aktives Targeting zur Visualisierung von thrombotischen Prozessen mittels 19F-MRT
Gefässchirurgie (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.