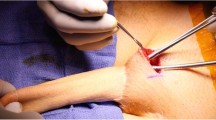
Abstract
This article presents the surgical outcomes of a consecutive series of 71 transmen undergoing pre-expanded suprapubic phalloplasty (SPP) in a specialized center. The median [IQR] duration to finalize this three-stage phalloplasty procedure was 7 months [6–7]. Median [IQR] follow-up was 39.4 months [19.7–81.2]. Among those included, 25 (35.2%) had a urethroplasty, and 40 (56.3%) a penile prosthesis as additional procedures. Complications were the result of disorders of wound healing (dehiscence, infection, partial necrosis) or tissue expander (migration, infection). Sixty patients (84.5%) experienced at least one complication during the phalloplasty procedure, mostly minor complications Clavien < IIIa (81.8%). Among these, 16 (22.5%) underwent at least one reintervention, 2 of whom underwent two reinterventions (18 reinterventions in total for Clavien ≥ IIIa complication). There was no loss of phalloplasty. Among the wide variety of techniques developed for phalloplasty, the suprapubic technique seems to be a valuable option for transmen on the path to genital gender affirming surgery.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Hage JJ, Bout CA, Bloem JJ, Megens JA. Phalloplasty in female-to-male transsexuals: what do our patients ask for? Ann Plast Surg. 1993;30:323–6.
Courtois F, Terrier J-é, Brassard P, Ruffion A, Morel-Journel N. Development of surgical phalloplasty techniques: Is there a gold standard? Sexologies. 2012;21:55–9.
Morrison SD, Shakir A, Vyas KS, Kirby J, Crane CN, Lee GK. Phalloplasty: a review of techniques and outcomes. Plast Reconstr Surg. 2016;138:594–615.
Hadj-Moussa M, Agarwal S, Ohl DA, Kuzon WM. Masculinizing genital gender confirmation surgery. Sex Med Rev. 2019;7:141–55.
Xu KY, Watt AJ. The pedicled anterolateral thigh phalloplasty. Clin Plast Surg. 2018;45:399–406.
Puckett CL, Montie JE. Construction of male genitalia in the transsexual, using a tubed groin flap for the penis and a hydraulic inflation device. Plast Reconstr Surg. 1978;61:523–30.
Sun GC, Huang JJ. One-stage reconstruction of the penis with composite iliac crest and lateral groin skin flap. Ann Plast Surg. 1985;15:519–28.
Bettocchi C, Ralph DJ, Pryor JP. Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int. 2005;95:120–4.
Marco F, Massimiliano T, Marco O, Andrea C, Girolamo M, Mirko P, et al. Suprapubic pedicled phalloplasty in transgender men: a multicentric retrospective cohort analysis. Int J Impot Res. 2020. https://doi.org/10.1038/s41443-020-0238-4. Online ahead of print.
Terrier J-É, Courtois F, Ruffion A, Morel, Journel N. Surgical outcomes and patients’ satisfaction with suprapubic phalloplasty. J Sex Med. 2014;11:288–98.
Selvaggi G, Dhejne C, Landen M, Elander A. The 2011 WPATH standards of care and penile reconstruction in female-to-male transsexual individuals. Adv Urol. 2012;2012:581712.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187–96.
Gilbert DA, Winslow BH, Gilbert DM, Jordan GH, Horton CE. Transsexual surgery in the genetic female. Clin Plast Surg. 1988;15:471–87.
Heston AL, Esmonde NO, Dugi DD, Berli JU. Phalloplasty: techniques and outcomes. Transl Androl Urol. 2019;8:254–65.
Monstrey S, Hoebeke P, Dhont M, Selvaggi G, Hamdi M, Van Landuyt K, et al. Radial forearm phalloplasty: a review of 81 cases. Eur J Plast Surg. 2005;28:206–12.
Garaffa G, Christopher NA, Ralph DJ. Total phallic reconstruction in female-to-male transsexuals. Eur Urol. 2010;57:715–22.
Monstrey SJ, Ceulemans P, Hoebeke P. Sex reassignment surgery in the female-to-male transsexual. Semin Plast Surg. 2011;25:229–44.
Lee WG, Christopher N, Ralph DJ. Penile Reconstruction and the Role of Surgery in Gender Dysphoria. Eur Urol. Focus. 2019;5:337–9.
Morrison SD, Chen ML, Crane CN. An overview of female-to-male gender-confirming surgery. Nat Rev Urol. 2017;14:486–500.
Frey JD, Poudrier G, Chiodo MV, Hazen A. A systematic review of metoidioplasty and radial forearm flap phalloplasty in female-to-male transgender genital reconstruction: is the “ideal” neophallus an achievable goal? Plast Reconstr Surg Glob Open. 2016;4:e1131.
Monstrey S, Hoebeke P, Selvaggi G, Ceulemans P, Van Landuyt K, Blondeel P, et al. Penile reconstruction: is the radial forearm flap really the standard technique? Plast Reconstr Surg. 2009;124:510–8.
Selvaggi G, Monstrey S, Hoebeke P, Ceulemans P, Van Landuyt K, Hamdi M, et al. Donor-site morbidity of the radial forearm free flap after 125 phalloplasties in gender identity disorder. Plast Reconstr Surg. 2006;118:1171–7.
Van Caenegem E, Verhaeghe E, Taes Y, Wierckx K, Toye K, Goemaere S, et al. Long-term evaluation of donor-site morbidity after radial forearm flap phalloplasty for transsexual men. J Sex Med. 2013;10):1644–51.
Garcia MM, Christopher NA, Luca FD, Spilotros M, Ralph DJ. Overall satisfaction, sexual function, and the durability of neophallus dimensions following staged female to male genital gender confirming surgery: the Institute of Urology, London U.K. experience. Transl Androl Urol. 2014;3:156.
Ascha M, Massie JP, Morrison SD, Crane CN, Chen ML. Outcomes of single stage phalloplasty by pedicled anterolateral thigh flap versus radial forearm free flap in gender confirming surgery. J Urol. 2018;199:206–14.
Djordjevic ML, Bumbasirevic MZ, Vukovic PM, Sansalone S, Perovic SV. Musculocutaneous latissimus dorsi free transfer flap for total phalloplasty in children. J Pediatr Urol. 2006;2:333–9.
Elfering L, van der Sluis WB, Bouman M-B, Buncamper ME, van de Grift TC, Lissenberg-Witte BI, et al. Preexpansion in phalloplasty patients: is it effective? Ann Plast Surg. 2019;83:687–92.
Srivastava A, Vashishtha S, Singh UP, Srivastava A, Ansari MS, Kapoor R, et al. Preputial/penile skin flap, as a dorsal onlay or tubularized flap: a versatile substitute for complex anterior urethral stricture. BJU Int. 2012;110:E1101–1108.
Papadopulos NA, Schaff J, Biemer E. The use of free prelaminated and sensate osteofasciocutaneous fibular flap in phalloplasty. Injury. 2008;39:S62–67.
Chang TS, Hwang WY. Forearm flap in one-stage reconstruction of the penis. Plast Reconstr Surg. 1984;74:251–8.
Dabernig J, Shelley OP, Cuccia G, Schaff J. Urethral reconstruction using the radial forearm free flap: experience in oncologic cases and gender reassignment. Eur Urol. 2007;52:547–53.
Garaffa G, Ralph DJ, Christopher N. Total urethral construction with the radial artery-based forearm free flap in the transsexual. BJU Int. 2010;106:1206–10.
Selvaggi G, Monstrey S, Ceulemans P, T’Sjoen G, De Cuypere G, Hoebeke P. Genital sensitivity after sex reassignment surgery in transsexual patients. Ann Plast Surg. 2007;58:427–33.
De Cuypere G, T’Sjoen G, Beerten R, Selvaggi G, De Sutter P, Hoebeke P, et al. Sexual and physical health after sex reassignment surgery. Arch Sex Behav. 2005;34:679–90.
Gilbert DA, Williams MW, Horton CE, Terzis JK, Winslow BH, Gilbert DM, et al. Phallic reinnervation via the pudendal nerve. J Urol. 1988;140:295–9.
Acknowledgements
The authors wish to thank Verena Landel for her proofreading and Vincent Meyer for the drawings.
Funding
The study received financial support from the French Association of Urology (AFU).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Terrier, M., Morel-Journel, N., Carnicelli, D. et al. Suprapubic phalloplasty in transmen: surgical results and critical review. Int J Impot Res 33, 754–761 (2021). https://doi.org/10.1038/s41443-021-00426-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-021-00426-7
This article is cited by
-
Review of Phalloplasty Techniques and Prosthetics in Transgender Male Patients
Current Sexual Health Reports (2022)
-
Functional and surgical outcomes after phalloplasty in cis men
World Journal of Urology (2022)
-
Neophallus Construction and Penile Prosthesis Implantation: Techniques and Complications
Current Sexual Health Reports (2021)