Abstract
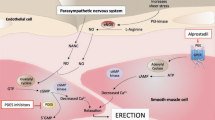
Erectile dysfunction (ED), defined as the inability to initiate or maintain an erection sufficient for satisfactory sexual intercourse, is common, particularly in men aged ≥50 years. Existing treatments have significant limitations, and there remains a need for a fast-acting (to facilitate spontaneity during intercourse) and well tolerated local therapy. Topical glyceryl trinitrate (GTN) may meet this need because GTN undergoes rapid metabolism in penile smooth muscle and endothelial cells to produce nitric oxide, which plays a key role in the development of erection. This paper describes the rationale for the development of MED2005, a topical GTN formulation using DermaSys® technology, which is undergoing clinical trials for the treatment of ED. Pharmacokinetic studies have shown that MED2005 provides rapid delivery of GTN following application to the glans penis, and a Phase 2(a) trial in men with ED showed that MED2005 produced significant improvements in erectile function, compared with placebo. MED2005 was well tolerated in this trial, with only 21 cases of headache in 1003 intercourse attempts. It is anticipated that MED2005 will provide an effective therapy for ED, with a fast onset of action, good local tolerability, and fewer contraindications than phosphodiesterase 5 inhibitors, the current cornerstone of ED therapy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Yafi FA, Jenkins L, Albersen M, et al. Erectile dysfunction. Nat Rev Dis Prim. 2016;2:16003.
Hatzimouratidis K, Giuliano F, Moncada I, et al. Male sexual dysfunction. Eur Assoc Urol. https://uroweb.org/guideline/male-sexual-dysfunction/#3_1. Accessed 27 June 2019.
Lewis RW, Fugl-Meyer KS, Corona G, Hayes RD, Laumann EO, Moreira ED, et al. Definitions/epidemiology/risk factors for sexual dysfunction. J Sex Med. 2010;7:1598–607.
Braun M, Wassmer G, Klotz T, Reifenrath B, Mathers M, Engelmann U. Epidemiology of erectile dysfunction: results of the ‘Cologne Male Survey’. Int J Impot Res. 2000;12:305–11.
Mola JR. Erectile dysfunction in the older adult male. Urol Nurs. 2015;35:87–93.
Selvin E, Burnett AL, Platz EA. Prevalence and risk factors for erectile dysfunction in the US. Am J Med. 2007;120:151–7.
Kubin M, Wagner G, Fugl-Meyer AR. Epidemiology of erectile dysfunction. Int J Impot Res. 2003;15:63–71.
Corona G, Rastrelli G, Filippi S, Vignozzi L, Mannucci E, Maggi M. Erectile dysfunction and central obesity: an Italian perspective. Asian J Androl. 2014;16:581–91.
Lotti F, Rastrelli G, Maseroli E, Cipriani S, Guaraldi F, Krausz C, et al. Impact of metabolically healthy obesity in patients with andrological problems. J Sex Med. 2019;16:821–32.
Capogrosso P, Colicchia M, Ventimiglia E, Castagna G, Clementi MC, Suardi N, et al. One patient out of four with newly diagnosed erectile dysfunction is a young man–worrisome picture from the everyday clinical practice. J Sex Med. 2013;10:1833–41.
Nguyen HMT, Gabrielson AT, Hellstrom WJG. Erectile dysfunction in young men-a review of the prevalence and risk factors. Sex Med Rev. 2017;5:508–20.
Tomlinson J, Wright D. Impact of erectile dysfunction and its subsequent treatment with sildenafil: qualitative study. BMJ. 2004;328:1037.
Litwin MS, Nied RJ, Dhanani N. Health-related quality of life in men with erectile dysfunction. J Gen Intern Med. 1998;13:159–66.
Sánchez-Cruz JJ, Cabrera-León A, Martín-Morales A, Fernández A, Burgos R, Rejas J. Male erectile dysfunction and health-related quality of life. Eur Urol. 2003;44:245–53.
Corona G, Ricca V, Bandini E, Mannucci E, Petrone L, Fisher AD, et al. Association between psychiatric symptoms and erectile dysfunction. J Sex Med. 2008;5:458–68.
Latini DM, Penson DF, Lubeck DP, Wallace KL, Henning JM, Lue TF. Longitudinal differences in disease specific quality of life in men with erectile dysfunction: results from the Exploratory Comprehensive Evaluation of Erectile Dysfunction study. J Urol. 2003;169:1437–42.
Park NC, Kim TN, Park HJ. Treatment strategy for non-responders to PDE5 inhibitors. World J Mens Health. 2013;31:31–5.
Corona G, Rastrelli G, Burri A, Serra E, Gianfrilli D, Mannucci E, et al. First-generation phosphodiesterase type 5 inhibitors dropout: a comprehensive review and meta-analysis. Andrology. 2016;4:1002–9.
Carvalheira AA, Pereira NM, Maroco J, Forjaz V. Dropout in the treatment of erectile dysfunction with PDE5: a study on predictors and a qualitative analysis of reasons for discontinuation. J Sex Med. 2012;9:2361–9.
Huang SA, Lie JD. Phosphodiesterase-5 (PDE5) inhibitors in the management of erectile dysfunction. P T. 2013;38:407–19.
Yuan J, Zhang R, Yang Z, Lee J, Liu Y, Tian J, et al. Comparative effectiveness and safety of oral phosphodiesterase type 5 inhibitors for erectile dysfunction: a systematic review and network meta-analysis. Eur Urol. 2013;63:902–12.
Buvat J, Büttner H, Hatzimouratidis K, Vendeira PA, Moncada I, Boehmer M, et al. Adherence to initial PDE-5 inhibitor treatment: randomized open-label study comparing tadalafil once a day, tadalafil on demand, and sildenafil on demand in patients with erectile dysfunction. J Sex Med. 2013;10:1592–602.
Smith WB 2nd, McCaslin IR, Gokce A, Mandava SH, Trost L, Hellstrom WJ. PDE5 inhibitors: considerations for preference and long-term adherence. Int J Clin Pract. 2013;67:768–80.
Carvalheira A, Forjaz V, Pereira NM. Adherence to phosphodiesterase type 5 inhibitors in the treatment of erectile dysfunction in long-term users: how do men use the inhibitors? Sex Med. 2014;2:96–102.
Hsieh CH, Huang YP, Tsai MH, Chen HS, Huang PC, Lin CW, et al. Tunical outer layer plays an essential role in penile veno-occlusive mechanism evidenced from electrocautery effects to the corpora cavernosa in defrosted human cadavers. Urology. 2015;86:1129–35.
Cartledge J, Minhas S, Eardley I. The role of nitric oxide in penile erection. Expert Opin Pharmacother. 2001;2:95–107.
Salvemini D, Mollace V, Pistelli A, Anggard E, Vane J. Metabolism of glyceryl trinitrate to nitric oxide by endothelial cells and smooth muscle cells and its induction by Escherichia coli lipopolysaccharide. Proc Natl Acad Sci USA. 1992;89:982–6.
Diallo D, Zaitouna M, Alsaid B, Quillard J, Droupy S, Benoit G, et al. What is the origin of the arterial vascularization of the corpora cavernosa? A computer-assisted anatomic dissection study. J Anat. 2013;223:489–94.
Droupy S, Giuliano F, Jardin A, Benôit G. Cavernospongious shunts: anatomical study of intrapenile vascular pathways. Eur Urol. 1999;36:123–8.
Pezzoni F. Physiological interrelationships between the venous shunts of penile corpus spongiosum and cavernous compartments during erection used in the pharmacotherapy of erectile dysfunction. Ann Ital Chir. 2017;88:242–6.
Vardi Y, Saenz de Tejada I. Functional and radiologic evidence of vascular communication between the spongiosal and cavernosal compartments of the penis. Urology. 1997;49:749–52.
Tam PY, Keller T, Poppiti R, Gesundheit N, Padma-Nathan H. Hemodynamic effects of transurethral alprostadil measured by color duplex ultrasonography in men with erectile dysfunction. J Urol. 1998;160:1321–4.
Cawello W, Schweer H, Dietrich B, Seyberth HW, Albrecht D, Fox A, et al. Pharmacokinetics of prostaglandin E1 and its main metabolites after intracavernous injection and short-term infusion of prostaglandin E1 in patients with erectile dysfunction. J Urol. 1997;158:1403–7.
Hakenberg O, Wetterauer U, Koppermann U, Lühmann R. Systemic pharmacokinetics of papaverine and phentolamine: comparison of intravenous and intracavernous application. Int J Impot Res. 1990;2 Suppl 2:247–8.
van Ahlen H, Peskar BA, Sticht G, Hertfelder HJ. Pharmacokinetics of vasoactive substances administered into the human corpus cavernosum. J Urol. 1994;151:1227–30.
Cordero JA, Camacho M, Obach R, Domenech J, Vila L. In vitro based index of topical anti-inflammatory activity to compare a series of NSAIDs. Eur J Pharm Biopharm. 2001;51:135–42.
Minghetti P, Casiraghi A, Cilurzo F, Montanari L, Marazzi M, Falcone L, et al. Comparison of different membranes with cultures of keratinocytes from man for percutaneous absorption of nitroglycerine. J Pharm Pharmacol. 1999;51:673–8.
Hadgraft J, Beutner D, Wolff HM. In vivo-in vitro comparisons in the transdermal delivery of nitroglycerin. Int J Pharm. 1993;89:R1–4.
Foldvari M, Oguejiofor CJ, Wilson TW, Afridi SK, Kudel TA. Transcutaneous delivery of prostaglandin E1: in vitro and laser doppler flowmetry study. J Pharm Sci. 1998;87:721–5.
Jeager JL, Buyuktimkin N, Buyuktimkin S. Prostaglandin compositions and methods of treatment for male erectile dysfunction. US Patent 6,323,241, 27 Nov 2001. https://patentimages.storage.googleapis.com/8c/fa/e5/8cd491a5ba44a/US6323241.pdf. Accessed 2 July 2019.
Taub HC, Lerner SE, Melman A, Christ GJ. Relationship between contraction and relaxation in human and rabbit corpus cavernosum. Urology. 1993;42:698–704.
Christ GJ, Kim DC, Taub HC, Gondré CM, Melman A. Characterization of nitroglycerine-induced relaxation in human corpus cavernosum smooth muscle: implications to erectile physiology and dysfunction. Can J Physiol Pharmacol. 1995;73:1714–26.
Cold CJ, Taylor JR. The prepuce. BJU Int. 1999;83 Suppl 1:34–44.
Yang CC, Bradley WE. Innervation of the human glans penis. J Urol. 1999;161:97–102.
Funke AP, Schiller R, Motzkus HW, Günther C, Müller RH, Lipp R. Transdermal delivery of highly lipophilic drugs: in vitro fluxes of antiestrogens, permeation enhancers, and solvents from liquid formulations. Pharm Res. 2002;19:661–8.
Davis AF, Hadgraft J. Effect of supersaturation on membrane transport: 1. Hydrocortisone acetate. Int J Pharm. 1991;76:1–8.
Li A, Yalkowsky SH. Solubility of organic solutes in ethanol/water mixtures. J Pharm Sci. 1994;83:1735–40.
Lubrizol Advanced Materials Inc. Pharmaceutical bulletin 7. Flow and suspension properties. 2008. https://www.lubrizol.com/-/media/Lubrizol/Life-Sciences/Documents/Literature/Bulletin/Bulletin-07-Flow-and-Suspension-Properties.pdf. Accessed 3 July 2019.
Yap PS, Fung HL. Pharmacokinetics of nitroglycerin in rats. J Pharm Sci. 1978;67:584–6.
Holland T, James K, Hutchings S, Francombe D. A randomized study of the pharmacokinetics of MED2005, a novel topical glyceryl trinitrate formulation for the treatment of erectile dysfunction, in healthy volunteers. Unpublished manuscript.
Ralph DJ, Eardley I, Taubel J, Terrill P, Holland T. Efficacy and safety of MED2005, a topical glyceryl trinitrate formulation, in the treatment of erectile dysfunction: a randomized crossover study. J Sex Med. 2018;15:167–75.
Molodysky E, Liu SP, Huang SJ, Hsu GL. Penile vascular surgery for treating erectile dysfunction: current role and future direction. Arab J Urol. 2013;11:254–66.
Acknowledgements
Medical writing assistance in the development of this paper was provided by Dr Michael Shaw (MScript Ltd, Hove, UK), and funded by Futura Medical Developments Ltd (Guildford, UK).
Funding
Medical writing assistance in the development of this paper was funded by Futura Medical Developments Ltd (Guildford, UK).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
AD provides consultancy services to Futura Medical Developments Ltd, and holds stock options and shares in the company. YR reports no conflicts of interest in relation to this paper. The medical writer, Dr Michael Shaw, reports no conflicts of interest in relation to this paper.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Davis, A., Reisman, Y. Development of a novel topical formulation of glyceryl trinitrate for the treatment of erectile dysfunction. Int J Impot Res 32, 569–577 (2020). https://doi.org/10.1038/s41443-019-0227-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-019-0227-7