Abstract
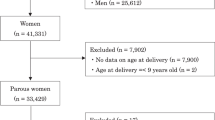
Previous studies have reported that the number of pregnancies and childbirths affected the risk of cardiovascular diseases (CVDs). However, the influence of reproductive history on hypertension and obesity, which are important risk factors for CVDs, is still unclear. Moreover, this association may vary depending on menopausal status. We evaluated the association of reproductive history with hypertension and obesity using a large cross-sectional dataset from the Japan Multi-Institutional Collaborative Cohort Study (J-MICC Study). At the baseline survey, physical data, blood samples, and self-reported health questionnaires were collected. Participants with insufficient data were excluded, and 24,558 women from eight study regions were included in this study. Logistic regression analysis was conducted to evaluate the association of reproductive history with hypertension and obesity using multivariable-adjusted odds ratios. In premenopausal women, childbirth showed a generally protective effect on hypertension but not on obesity. In postmenopausal women, childbirth was positively associated with obesity and hypertension but not with hypertension after adjusting for BMI. In conclusion, reproductive history was associated with hypertension and obesity in a large Japanese population, and this association differed between premenopausal and postmenopausal women.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Mosca L, Benjamin EJ, Berra K, Bezanson JL, Dolor RJ, Lloyd-Jones DM, et al. Effectiveness-based guidelines for the prevention of cardiovascular disease in women–2011 update: a guideline from the american heart association. Circulation. 2011;123:1243–62.
Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, et al. 2019 ACC/AHA Guideline on the Primary Prevention of Cardiovascular Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;140:e596–646.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018;71:e13–5.
Parikh NI, Cnattingius S, Dickman PW, Mittleman MA, Ludvigsson JF, Ingelsson E. Parity and risk of later-life maternal cardiovascular disease. Am Heart J. 2010;159:215–21.
Otsuki S, Saito E, Sawada N, Abe SK, Hidaka A, Yamaji T, et al. Female reproductive factors and risk of all-cause and cause-specific mortality among women: The Japan Public Health Center-based Prospective Study (JPHC study). Ann Epidemiol. 2018;28:597–604.
Tanigawa K, Ikehara S, Kimura T, Imano H, Muraki I, Shirai K, et al. Relationships Between Reproductive History and Mortality From Cardiovascular Diseases Among Japanese Women: The Japan Collaborative Cohort Study for Evaluation of Cancer Risk (JACC) Study. J Epidemiol. 2020;30:509–15.
Lv H, Wu H, Yin J, Qian J, Ge J. Parity and Cardiovascular Disease Mortality: a Dose-Response Meta-Analysis of Cohort Studies. Sci Rep. 2015;5:13411.
Lawlor DA, Emberson JR, Ebrahim S, Whincup PH, Wannamethee SG, Walker M, et al. British Women’s Heart and Health Study, British Regional Heart Study. Is the association between parity and coronary heart disease due to biological effects of pregnancy or adverse lifestyle risk factors associated with child-rearing? Findings from the British Women’s Heart and Health Study and the British Regional Heart Study. Circulation. 2003;107:1260–4.
Jang M, Lee Y, Choi J, Kim B, Kang J, Kim Y, et al. Association between Parity and Blood Pressure in Korean Women: Korean National Health and Nutrition Examination Survey, 2010-2012. Korean J Fam Med. 2015;36:341–8.
Gunderson EP, Chiang V, Lewis CE, Catov J, Quesenberry CP Jr, Sidney S, et al. Long-term blood pressure changes measured from before to after pregnancy relative to nonparous women. Obstet Gynecol. 2008;112:1294–302.
Ness RB, Kramer RA, Flegal KM. Gravidity, blood pressure, and hypertension among white women in the Second National Health and Nutrition Examination Survey. Epidemiology. 1993;4:303–9.
Chen SX, Rasmussen KM, Finkelstein J, Stovring H, Nohr EA, Kirkegaard H. Maternal reproductive history and premenopausal risk of hypertension and cardiovascular disease: a Danish cohort study. BMJ Open. 2019;9:e030702.
Erem C, Hacihasanoglu A, Kocak M, Deger O, Topbas M. Prevalence of prehypertension and hypertension and associated risk factors among Turkish adults: Trabzon Hypertension Study. J Public Health. 2009;31:47–58.
Dratva J, Schneider C, Schindler C, Stolz D, Gerbase M, Pons M, et al. Is there a differential impact of parity on blood pressure by age? J Hypertens. 2014;32:2146–51.
Giubertoni E, Bertelli L, Bartolacelli Y, Origliani G, Modena MG. Parity as predictor of early hypertension during menopausal transition. J Hypertens. 2013;31:501–7.
Lao XQ, Thomas GN, Jiang CQ, Zhang WS, Yin P, Schooling M, et al. Parity and the metabolic syndrome in older Chinese women: the Guangzhou Biobank Cohort Study. Clin Endocrinol. 2006;65:460–9.
Taylor JY, Chambers AN, Funnell B, Wu CY. Effects of parity on blood pressure among African-American women. J Natl Black Nurses Assoc. 2008;19:12–9.
Hamajima N, Group J-MS. The Japan Multi-Institutional Collaborative Cohort Study (J-MICC Study) to detect gene-environment interactions for cancer. Asian Pac J Cancer Prev. 2007;8:317–23.
Takeuchi K, Naito M, Kawai S, Tsukamoto M, Kadomatsu Y, Kubo Y, et al. Study profile of the Japan Multi-institutional Collaborative Cohort (J-MICC) Study. J Epidemiol. 2020. https://doi.org/10.2188/jea.JE20200147.
Tokudome Y, Goto C, Imaeda N, Hasegawa T, Kato R, Hirose K, et al. Relative validity of a short food frequency questionnaire for assessing nutrient intake versus three-day weighed diet records in middle-aged Japanese. J Epidemiol. 2005;15:135–45.
Uemura H, Katsuura-Kamano S, Iwasaki Y, Arisawa K, Hishida A, Okada R, et al. Japan Multi-institutional Collaborative Cohort (J-MICC) Study Group. Independent relationships of daily life activity and leisure-time exercise with metabolic syndrome and its traits in the general Japanese population. Endocrine. 2019;64:552–63.
Clapp JF 3rd, Capeless E. Cardiovascular function before, during, and after the first and subsequent pregnancies. Am J Cardiol. 1997;80:1469–73.
Lupton SJ, Chiu CL, Lujic S, Hennessy A, Lind JM. Association between parity and breastfeeding with maternal high blood pressure. Am J Obstet Gynecol. 2013;208:454 e451–7.
Ashraf MS, Vongpatanasin W. Estrogen and hypertension. Curr Hypertens Rep. 2006;8:368–76.
Hajjar I, Kotchen TA. Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1988-2000. JAMA. 2003;290:199–206.
Ouyang P, Michos ED, Karas RH. Hormone replacement therapy and the cardiovascular system lessons learned and unanswered questions. J Am Coll Cardiol. 2006;47:1741–53.
Nagai K, Hayashi K, Yasui T, Katanoda K, Iso H, Kiyohara Y, et al. Disease history and risk of comorbidity in women’s life course: a comprehensive analysis of the Japan Nurses’ Health Study baseline survey. BMJ Open. 2015;5:e006360.
Mu F, Rich-Edwards J, Rimm EB, Spiegelman D, Missmer SA. Endometriosis and Risk of Coronary Heart Disease. Circ Cardiovasc Qual Outcomes. 2016;9:257–64.
Figuero E, Carrillo-de-Albornoz A, Martin C, Tobias A, Herrera D. Effect of pregnancy on gingival inflammation in systemically healthy women: a systematic review. J Clin Periodontol. 2013;40:457–73.
Lockhart PB, Bolger AF, Papapanou PN, Osinbowale O, Trevisan M, Levison ME, et al. American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee of the Council on Cardiovascular Disease in the Young, Council on Epidemiology and Prevention, Council on Peripheral Vascular Disease, and Council on Clinical Cardiology. Periodontal disease and atherosclerotic vascular disease: does the evidence support an independent association?: a scientific statement from the American Heart Association. Circulation. 2012;125:2520–44.
Gordon JH, LaMonte MJ, Genco RJ, Zhao J, Cimato TR, Hovey KM, et al. Association of clinical measures of periodontal disease with blood pressure and hypertension among postmenopausal women. J Periodontol. 2018;89:1193–202.
Segovia SA, Vickers MH, Reynolds CM. The impact of maternal obesity on inflammatory processes and consequences for later offspring health outcomes. J Dev Orig Health Dis. 2017;8:529–40.
Pendeloski KPT, Ono E, Torloni MR, Mattar R, Daher S. Maternal obesity and inflammatory mediators: a controversial association. Am J Reprod Immunol. 2017;77:e12674.
Hisamatsu T, Segawa H, Kadota A, Ohkubo T, Arima H, Miura K. Epidemiology of hypertension in Japan: beyond the new 2019 Japanese guidelines. Hypertens Res. 2020;43:1344–51.
Acknowledgements
We would like to thank all the participants of the baseline survey of the J-MICC Study, Drs. Nobuyuki Hamajima and Hideo Tanaka (former principal investigators), and the staff in each study region for their cooperation.
the Japan Multi-institutional Collaborative Cohort (J-MICC) Study Group
Kenji Wakai6, Kenji Takeuchi6, Hiroki Nagase19, Haruo Mikami17, Hiroto Narimatsu20, Kiyonori Kuriki11, Sadao Suzuki10, Keitaro Matsuo15, Asahi Hishida6, Yoshikuni Kita18, Katsuyuki Miura1, Teruhide Koyama9, Kokichi Arisawa12, Hiroaki Ikezaki14, Keitaro Tanaka7, Toshiro Takezaki8.
Funding
This study was supported by Grants-in-Aid for Scientific Research on Priority Areas of Cancer (No. 17015018), Innovative Areas (No. 221S0001), and Platform of Supporting Cohort Study and Biospecimen Analysis (JSPS KAKENHI Grant Number JP16H06277[CoBiA]) from the Japanese Ministry of Education, Culture, Sports, Science and Technology. This work was also supported in part by a Grant-in-Aid from the Japan Society for the Promotion of Science (JSPS KAKENHI Grant Numbers 24390165, 20390184, 17390186, 19H03902).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the Japan Multi-institutional Collaborative Cohort (J-MICC) Study Group are listed below the Acknowledgement Section.
Rights and permissions
About this article
Cite this article
Ohashi, M., Miura, K., Takashima, N. et al. The association of reproductive history with hypertension and obesity according to menopausal status: the J-MICC Study. Hypertens Res 45, 708–714 (2022). https://doi.org/10.1038/s41440-021-00820-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-021-00820-0