Abstract
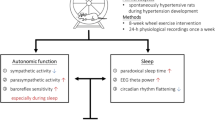
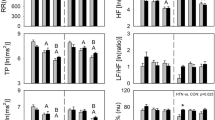
Increased blood pressure (BP) caused by exposure to cold temperatures can partially explain the increased incidence of cardiovascular events in winter. However, the physiological mechanisms involved in cold-induced high BP are not well established. Many studies have focused on physiological responses to severe cold exposure. In this study, we aimed to perform a comprehensive analysis of cardiovascular autonomic function and sleep patterns in rats during exposure to mild cold, a condition relevant to humans in subtropical areas, to clarify the physiological mechanisms underlying mild cold-induced hypertension. BP, electroencephalography, electromyography, electrocardiography, and core body temperature were continuously recorded in normotensive Wistar-Kyoto rats over 24 h. All rats were housed in thermoregulated chambers at ambient temperatures of 23, 18, and 15 °C in a randomized crossover design. These 24-h physiological recordings either with or without sleep scoring showed that compared with the control temperature of 23 °C, the lower ambient temperatures of 18 and 15 °C not only increased BP, vascular sympathetic activity, and heart rate but also decreased overall autonomic activity, parasympathetic activity, and baroreflex sensitivity in rats. In addition, cold exposure reduced the delta power percentage and increased the incidence of interruptions during sleep. Moreover, a correlation analysis revealed that all of these cold-induced autonomic dysregulation and sleep problems were associated with elevation of BP. In conclusion, mild cold exposure elicits autonomic dysregulation and poor sleep quality, causing BP elevation, which may have critical implications for cold-related cardiovascular events.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Wang H, Sekine M, Chen X, Kagamimori S. A study of weekly and seasonal variation of stroke onset. Int J Biometeorol. 2002;47:13–20.
Spencer FA, Goldberg RJ, Becker RC, Gore JM. Seasonal distribution of acute myocardial infarction in the second National Registry of Myocardial Infarction. J Am Coll Cardiol. 1998;31:1226–33.
Marchant B, Ranjadayalan K, Stevenson R, Wilkinson P, Timmis AD. Circadian and seasonal factors in the pathogenesis of acute myocardial infarction: the influence of environmental temperature. Br Heart J. 1993;69:385–7.
Brennan PJ, Greenberg G, Miall WE, Thompson SG. Seasonal variation in arterial blood pressure. Br Med J. 1982;285:919–23.
Minami J, Ishimitsu T, Kawano Y, Matsuoka H. Seasonal variations in office and home blood pressures in hypertensive patients treated with antihypertensive drugs. Blood Press Monit. 1998;3:101–6.
Winnicki M, Canali C, Accurso V, Dorigatti F, Giovinazzo P, Palatini P. Relation of 24-hour ambulatory blood pressure and short-term blood pressure variability to seasonal changes in environmental temperature in stage I hypertensive subjects. Results of the Harvest Trial. Clin Exp Hypertens. 1996;18:995–1012.
Sega R, Cesana G, Bombelli M, Grassi G, Stella ML, Zanchetti A, et al. Seasonal variations in home and ambulatory blood pressure in the PAMELA population. Pressione Arteriose Monitorate E Loro Associazioni. J Hypertens. 1998;16:1585–92.
Kristal-Boneh E, Harari G, Green MS, Ribak J. Summer-winter variation in 24 h ambulatory blood pressure. Blood Press Monit. 1996;1:87–94.
Brook RD. The environment and blood pressure. Cardiol Clin. 2017;35:213–21.
Lavados PM, Olavarria VV, Hoffmeister L. Ambient temperature and stroke risk: evidence supporting a short-term effect at a population level from acute environmental exposures. Stroke. 2018;49:255–61.
Joyner MJ, Charkoudian N, Wallin BG. A sympathetic view of the sympathetic nervous system and human blood pressure regulation. Exp Physiol. 2008;93:715–24.
La Rovere MT, Pinna GD, Raczak G. Baroreflex sensitivity: measurement and clinical implications. Ann Noninvasive Electrocardiol. 2008;13:191–207.
Kiviniemi AM, Tulppo MP, Hautala AJ, Perkiomaki JS, Ylitalo A, Kesaniemi YA, et al. Prognostic significance of impaired baroreflex sensitivity assessed from Phase IV of the Valsalva maneuver in a population-based sample of middle-aged subjects. Am J Cardiol. 2014;114:571–6.
Kuo TBJ, Yang CCH. Sleep-related changes in cardiovascular neural regulation in spontaneously hypertensive rats. Circulation. 2005;112:849–54.
Somers VK, Dyken ME, Mark AL, Abboud FM. Sympathetic-nerve activity during sleep in normal subjects. N Engl J Med. 1993;328:303–7.
Hirata T, Nakamura T, Kogure M, Tsuchiya N, Narita A, Miyagawa K, et al. Reduced sleep efficiency, measured using an objective device, was related to an increased prevalence of home hypertension in Japanese adults. Hypertens Res. 2020;43:23–9.
Stein PK, Pu Y. Heart rate variability, sleep and sleep disorders. Sleep Med Rev. 2012;16:47–66.
Yang YN, Tsai HL, Lin YC, Liu YP, Tung CS. Role of vasopressin V1 antagonist in the action of vasopressin on the cooling-evoked hemodynamic perturbations of rats. Neuropeptides. 2019;76:101939.
Hintsala HE, Kiviniemi AM, Tulppo MP, Helakari H, Rintamaki H, Mantysaari M, et al. Hypertension does not alter the increase in cardiac baroreflex sensitivity caused by moderate cold exposure. Front Physiol. 2016;7:204.
Axsom JE, Nanavati AP, Rutishauser CA, Bonin JE, Moen JM, Lakatta EG. Acclimation to a thermoneutral environment abolishes age-associated alterations in heart rate and heart rate variability in conscious, unrestrained mice. Geroscience. 2020;42:217–32.
Papanek PE, Wood CE, Fregly MJ. Role of the sympathetic nervous system in cold-induced hypertension in rats. J Appl Physiol. 1991;71:300–6.
Stemper B, Hilz MJ, Rauhut U, Neundorfer B. Evaluation of cold face test bradycardia by means of spectral analysis. Clin Auton Res. 2002;12:78–83.
Krauchi K, Gasio PF, Vollenweider S, Von Arb M, Dubler B, Orgul S, et al. Cold extremities and difficulties initiating sleep: evidence of co-morbidity from a random sample of a Swiss urban population. J Sleep Res. 2008;17:420–6.
Okamoto-Mizuno K, Mizuno K. Effects of thermal environment on sleep and circadian rhythm. J Physiol Anthropol. 2012;31:14.
Cerri M, Ocampo-Garces A, Amici R, Baracchi F, Capitani P, Jones CA, et al. Cold exposure and sleep in the rat: effects on sleep architecture and the electroencephalogram. Sleep. 2005;28:694–705.
Xie L, Liu B, Wang X, Mei M, Li M, Yu X, et al. Effects of different stresses on cardiac autonomic control and cardiovascular coupling. J Appl Physiol. 2017;122:435–45.
Cui J, Durand S, Crandall CG. Baroreflex control of muscle sympathetic nerve activity during skin surface cooling. J Appl Physiol. 2007;103:1284–9.
Okamoto-Mizuno K, Tsuzuki K, Mizuno K, Ohshiro Y. Effects of low ambient temperature on heart rate variability during sleep in humans. Eur J Appl Physiol. 2009;105:191–7.
Lin YK, Ho TJ, Wang YC. Mortality risk associated with temperature and prolonged temperature extremes in elderly populations in Taiwan. Environ Res. 2011;111:1156–63.
Kuo TBJ, Shaw FZ, Lai CJ, Yang CCH. Asymmetry in sympathetic and vagal activities during sleep-wake transitions. Sleep. 2008;31:311–20.
Li JY, Kuo TBJ, Yen JC, Tsai SC, Yang CCH. Voluntary and involuntary running in the rat show different patterns of theta rhythm, physical activity, and heart rate. J Neurophysiol. 2014;111:2061–70.
Kuo TBJ, Shaw FZ, Lai CJ, Lai CW, Yang CCH. Changes in sleep patterns in spontaneously hypertensive rats. Sleep. 2004;27:406–12.
Bjorvatn B, Fagerland S, Ursin R. EEG power densities (0.5-20 Hz) in different sleep-wake stages in rats. Physiol Behav. 1998;63:413–7.
Heart Rate Variability. Standards of measurement, physiological interpretation, and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Eur heart J. 1996;17:354–81.
Kuo TBJ, Yien HW, Hseu SS, Yang CC, Lin YY, Lee LC, et al. Diminished vasomotor component of systemic arterial pressure signals and baroreflex in brain death. Am J Physiol. 1997;273(3 Pt 2):H1291–8.
Bertinieri G, Di Rienzo M, Cavallazzi A, Ferrari AU, Pedotti A, Mancia G. Evaluation of baroreceptor reflex by blood pressure monitoring in unanesthetized cats. Am J Physiol. 1988;254(2 Pt 2):H377–83.
Fritsch JM, Eckberg DL, Graves LD, Wallin BG. Arterial pressure ramps provoke linear increases of heart period in humans. Am J Physiol. 1986;251(6 Pt 2):R1086–90.
Munakata M, Imai Y, Takagi H, Nakao M, Yamamoto M, Abe K. Altered frequency-dependent characteristics of the cardiac baroreflex in essential hypertension. J Autonomic Nerv Syst. 1994;49:33–45.
Kuo TBJ, Lin T, Yang CCH, Li CL, Chen CF, Chou P. Effect of aging on gender differences in neural control of heart rate. Am J Physiol. 1999;277(6 Pt 2):H2233–9.
Wang YC, Kuo JS, Lin SZ. The effect of sphenopalatine postganglionic neurotomy on the alteration of local cerebral blood flow of normotensive and hypertensive rats in acute cold stress. Proc Natl Sci Counc Repub China B. 1998;22:122–8.
Cannon B, Nedergaard J. Nonshivering thermogenesis and its adequate measurement in metabolic studies. J Exp Biol. 2011;214(Pt 2):242–53.
Sanchez-Gurmaches J, Hung CM, Guertin DA. Emerging complexities in adipocyte origins and identity. Trends Cell Biol. 2016;26:313–26.
Szymusiak R. Body temperature and sleep. Handb Clin Neurol. 2018;156:341–51.
Fedecostante M, Barbatelli P, Guerra F, Espinosa E, Dessi-Fulgheri P, Sarzani R. Summer does not always mean lower: seasonality of 24 h, daytime, and night-time blood pressure. J Hypertens. 2012;30:1392–8.
Yamazaki F, Sone R. Thermal stress modulates arterial pressure variability and arterial baroreflex response of heart rate during head-up tilt in humans. Eur J Appl Physiol. 2001;84:350–7.
Mourot L, Bouhaddi M, Gandelin E, Cappelle S, Nguyen NU, Wolf JP, et al. Conditions of autonomic reciprocal interplay versus autonomic co-activation: effects on non-linear heart rate dynamics. Auton Neurosci. 2007;137:27–36.
Yamazaki F, Sone R. Modulation of arterial baroreflex control of heart rate by skin cooling and heating in humans. J Appl Physiol. 2000;88:393–400.
Staessen JA, Thijs L, Fagard R, O’Brien ET, Clement D, de Leeuw PW, et al. Predicting cardiovascular risk using conventional vs ambulatory blood pressure in older patients with systolic hypertension. Systolic Hypertension in Europe Trial Investigators. JAMA. 1999;282:539–46.
Dolan E, Stanton A, Thijs L, Hinedi K, Atkins N, McClory S, et al. Superiority of ambulatory over clinic blood pressure measurement in predicting mortality: the Dublin outcome study. Hypertension. 2005;46:156–61.
Kuo TBJ, Chen CY, Wang YP, Lan YY, Mak KH, Lee GS, et al. The role of autonomic and baroreceptor reflex control in blood pressure dipping and nondipping in rats. J Hypertens. 2014;32:806–16.
Acknowledgements
This work was financially supported by a grant (109BRC-B504) from the Brain Research Center, National Yang-Ming University, from The Featured Areas Research Center Program within the framework of the Higher Education Sprout Project by the Ministry of Education in Taiwan; a grant (10601-62-012) from Taipei City Hospital; and grants (MOST 106-2314-B-010-025 and MOST 106-2627-E-010-001) from the Ministry of Science and Technology in Taiwan. The authors received no financial support from any manufacturer. Moreover, the authors thank Ms. Pei-Chi Hsu and Mr. Chen-Wei Huang for their article production support. The authors take full responsibility for the experimental design and the collection, analysis, and interpretation of the data.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Chen, CW., Wu, CH., Liou, YS. et al. Roles of cardiovascular autonomic regulation and sleep patterns in high blood pressure induced by mild cold exposure in rats. Hypertens Res 44, 662–673 (2021). https://doi.org/10.1038/s41440-021-00619-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-021-00619-z
Keywords
This article is cited by
-
Short-term effects of exposure to cold spells on blood pressure among adults in Nanjing, China
Air Quality, Atmosphere & Health (2024)
-
Reduced slow-wave activity and autonomic dysfunction during sleep precede cognitive deficits in Alzheimer’s disease transgenic mice
Scientific Reports (2023)
-
Update on Hypertension Research in 2021
Hypertension Research (2022)