Abstract
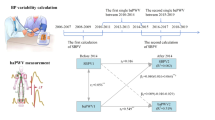
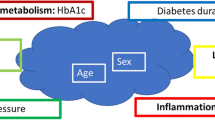
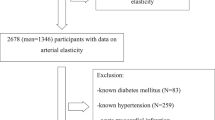
The present prospective observational study was conducted to examine the differences in longitudinal associations of the conventional risk factors for cardiovascular disease (CVD) with arterial stiffness and with abnormal pressure wave reflection using repeated measurement data. In 4016 healthy middle-aged (43 ± 9 years) Japanese men without CVD at baseline, the conventional risk factors for CVD, brachial–ankle pulse wave velocity (brachial–ankle PWV) and radial augmentation index (rAI) were measured annually over a 9-year period. Mixed-model linear regression analysis demonstrated a significant independent positive longitudinal association of the mean blood pressure with both the brachial–ankle PWV (estimate = 5.51, standard error = 0.30, P < 0.01) and the rAI (estimate = 0.19, standard error = 0.02, P < 0.01). On the other hand, the serum levels of glycohemoglobin, low-density lipoprotein cholesterol and triglycerides showed longitudinal associations only with the brachial–ankle PWV and not the rAI. In addition, while the radial AI was found to show a significant longitudinal association with the brachial–ankle PWV, the inverse association was not significant. In conclusion, the conventional risk factors for CVD showed heterogeneous longitudinal associations with arterial stiffness and/or abnormal pressure wave reflection. Elevated blood pressure showed independent longitudinal associations with both arterial stiffness (macrovascular damage) and abnormal pressure wave reflection, suggesting that BP is also longitudinally associated, at least in part, with microvascular damage. On the other hand, abnormal glucose metabolism and dyslipidemia showed independent longitudinal associations with only arterial stiffness (macrovascular damage).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Ohkuma T, Ninomiya T, Tomiyama H, Kario K, Hoshide S, Kita Y, et al. Brachial-ankle pulse wave velocity and the risk prediction of cardiovascular disease: an individual participant data meta-analysis. Hypertension. 2017;69:1045–52. https://doi.org/10.1161/HYPERTENSIONAHA.117.09097.
Ben-Shlomo Y, Spears M, Boustred C, May M, Anderson SG, Benjamin EJ, et al. Aortic pulse wave velocity improves cardiovascular event prediction: an individual participant meta-analysis of prospective observational data from 17,635 subjects. J Am Coll Cardiol. 2014;63:636–46. https://doi.org/10.1016/j.jacc.2013.09.063.
Vlachopoulos C, Aznaouridis K, O’Rourke MF, Safar ME, Baou K, Stefanadis C. Prediction of cardiovascular events and all-cause mortality with central haemodynamics: a systematic review and meta-analysis. Eur Heart J. 2010;31:1865–71. https://doi.org/10.1093/eurheartj/ehq024.
O’Rourke MF, Hashimoto J. Mechanical factors in arterial aging: a clinical perspective. J Am Coll Cardiol. 2007;50:1–13. https://doi.org/10.1016/j.jacc.2006.12.050.
Tomiyama H, Komatsu S, Shiina K, Matsumoto C, Kimura K, Fujii M, et al. Effect of wave reflection and arterial stiffness on the risk of development of hypertension in Japanese men. J Am Heart Assoc. 2018;7:e008175. https://doi.org/10.1161/JAHA.117.008175.
Climie RED, Picone DS, Blackwood S, Keel SE, Qasem A, Rattigan S, et al. Pulsatile interaction between the macro-vasculature and micro-vasculature: proof-of-concept among patients with type 2 diabetes. Eur J Appl Physiol. 2018;118:2455–63. https://doi.org/10.1007/s00421-018-3972-2.
Tomiyama H, Yamashina A. Non-invasive vascular function tests: their pathophysiological background and clinical application. Circ J. 2010;74:24–33. https://doi.org/10.1253/circj.cj-09-0534.
Rizzoni D, De Ciuceis C, Salvetti M, Paini A, Rossini C, Agabiti-Rosei C, et al. Interactions between macro- and micro-circulation: are they relevant? High Blood Press Cardiovasc Prev. 2015;22:119–28. https://doi.org/10.1007/s40292-015-0086-3.
Climie RE, van Sloten TT, Bruno RM, Taddei S, Empana JP, Stehouwer CDA, et al. Macrovasculature and microvasculature at the crossroads between type 2 diabetes mellitus and hypertension. Hypertension. 2019;73:1138–49. https://doi.org/10.1161/HYPERTENSIONAHA.118.11769.
Laurent S, Boutouyrie P. The structural factor of hypertension: large and small artery alterations. Circ Res. 2015;116:1007–21. https://doi.org/10.1161/CIRCRESAHA.116.303596.
Milwidsky A, Kivity S, Kopel E, Klempfner R, Berkovitch A, Segev S, et al. Time dependent changes in high density lipoprotein cholesterol and cardiovascular risk. Int J Cardiol. 2014;173:295–9. https://doi.org/10.1016/j.ijcard.2014.03.022.
Bangalore S, Fayyad R, DeMicco DA, Colhoun HM, Waters DD. Body weight variability and cardiovascular outcomes in patients with type 2 diabetes mellitus. Circ Cardiovasc Qual Outcomes. 2018;11:e004724. https://doi.org/10.1161/CIRCOUTCOMES.118.004724.
Yang J, Zaitlen NA, Goddard ME, Visscher PM, Price AL. Advantages and pitfalls in the application of mixed-model association methods. Nat Genet. 2014;46:100–6. https://doi.org/10.1038/ng.2876.
Tomiyama H, Shiina K, Matsumoto-Nakano C, Ninomiya T, Komatsu S, Kimura K, et al. The contribution of inflammation to the development of hypertension mediated by increased arterial stiffness. J Am Heart Assoc. 2017;30:e005729. https://doi.org/10.1161/JAHA.117.005729.
Tomiyama H, Shiina K, Vlachopoulos C, Iwasaki Y, Matsumoto C, Kimura K, et al. Involvement of arterial stiffness and inflammation in hyperuricemia-related development of hypertension. Hypertension. 2018;72:739–45. https://doi.org/10.1161/HYPERTENSIONAHA.118.11390.
Smulyan H, Lieber A, Safar ME. Hypertension, diabetes type II, and their association: role of arterial stiffness. Am J Hypertens. 2016;29:5–13. https://doi.org/10.1093/ajh/hpv107.
Cypienė A, Dadonienė J, Rugienė R, Ryliškytė L, Kovaitė M, Petrulionienė Z, et al. The influence of mean blood pressure on arterial stiffening and endothelial dysfunction in women with rheumatoid arthritis and systemic lupus erythematosus. Medicina. 2010;46:522–30. https://doi.org/10.3390/medicina46080075.
Safar ME, Boudier HS. Vascular development, pulse pressure, and the mechanisms of hypertension. Hypertension. 2005;46:205–9. https://doi.org/10.1161/01.HYP.0000167992.80876.26.
Tomiyama H, Yamazaki M, Sagawa Y, Teraoka K, Shirota T, Miyawaki Y, et al. Synergistic effect of smoking and blood pressure on augmentation index in men, but not in women. Hypertens Res. 2009;32:122–6. https://doi.org/10.1038/hr.2008.20.
Yamashina A, Tomiyama H, Takeda K, Tsuda H, Arai T, Hirose K, et al. Validity, reproducibility, and clinical significance of noninvasive brachial-ankle pulse wave velocity measurement. Hypertens Res. 2002;25:359–64. https://doi.org/10.1291/hypres.25.359.
Committee of the Japan Diabetes Society on the Diagnostic Criteria of Diabetes Mellitus, Seino Y, Nanjo K, Tajima N, Kadowaki T, Kashiwagi A, et al. Report of the committee on the classification and diagnostic criteria of diabetes mellitus. J Diabetes Investig. 2010;1:212–28. https://doi.org/10.1111/j.2040-1124.2010.00074.x.
Horio M, Imai E, Yasuda Y, Watanabe T, Matsuo S. Modification of the CKD epidemiology collaboration (CKD-EPI) equation for Japanese: accuracy and use for population estimates. Am J Kidney Dis. 2010;56:32–8. https://doi.org/10.1053/j.ajkd.2010.02.344.
Cecelja M, Chowienczyk P. Dissociation of aortic pulse wave velocity with risk factors for cardiovascular disease other than hypertension: a systematic review. Hypertension. 2009;54:1328–36. https://doi.org/10.1161/HYPERTENSIONAHA.109.137653.
Scuteri A, Morrell CH, Orrù M, Strait JB, Tarasov KV, Ferreli LA, et al. Longitudinal perspective on the conundrum of central arterial stiffness, blood pressure, and aging. Hypertension. 2014;64:1219–27. https://doi.org/10.1161/HYPERTENSIONAHA.114.04127.
McEniery CM, Spratt M, Munnery M, Yarnell J, Lowe GD, Rumley A, et al. An analysis of prospective risk factors for aortic stiffness in men: 20-year follow-up from the Caerphilly prospective study. Hypertension. 2010;56:36–43. https://doi.org/10.1161/HYPERTENSIONAHA.110.150896.
Mitchell GF, Conlin PR, Dunlap ME, Lacourcière Y, Arnold JM, Ogilvie RI, et al. Aortic diameter, wall stiffness, and wave reflection in systolic hypertension. Hypertension. 2008;51:105–11. https://doi.org/10.1161/HYPERTENSIONAHA.107.099721.
Zhang M, Bai Y, Ye P, Luo L, Xiao W, Wu H, et al. Type 2 diabetes is associated with increased pulse wave velocity measured at different sites of the arterial system but not augmentation index in a Chinese population. Clin Cardiol. 2011;34:622–7. https://doi.org/10.1002/clc.20956.
McEniery CM, Wilkinson IB, Johansen NB, Witte DR, Singh-Manoux A, Kivimaki M, et al. Nondiabetic glucometabolic status and progression of aortic stiffness: the Whitehall II study. Diabetes Care. 2017;40:599–606. https://doi.org/10.2337/dc16-1773.
Zhao X, Wang H, Bo L, Zhao H, Li L, Zhou Y. Serum lipid level and lifestyles are associated with carotid femoral pulse wave velocity among adults: 4.4-year prospectively longitudinal follow-up of a clinical trial. Clin Exp Hypertens. 2018;40:487–94. https://doi.org/10.1080/10641963.2017.1384486.
Wilkinson IB, Prasad K, Hall IR, Thomas A, MacCallum H, Webb DJ, et al. Increased central pulse pressure and augmentation index in subjects with hypercholesterolemia. J Am Coll Cardiol. 2002;39:1005–11. https://doi.org/10.1016/S0735-1097(02)01723-0.
Wang X, Ye P, Cao R, Yang X, Xiao W, Zhang Y, et al. Triglycerides are a predictive factor for arterial stiffness: a community-based 4.8-year prospective study. Lipids Health Dis. 2016;15:97. https://doi.org/10.1186/s12944-016-0266-8.
Otsuka T, Kawada T, Ibuki C, Kusama Y. Radial arterial wave reflection is associated with the MEGA risk prediction score, an indicator of coronary heart disease risk, in middle-aged men with mild to moderate hypercholesterolemia. J Atheroscler Thromb. 2010;17:688–94. https://doi.org/10.5551/jat.2949.
Wilkinson I, Cockcroft JR. Cholesterol, lipids and arterial stiffness. Adv Cardiol. 2007;44:261–77. https://doi.org/10.1159/000096747.
Prenner SB, Chirinos JA. Arterial stiffness in diabetes mellitus. Atherosclerosis. 2015;238:370–9. https://doi.org/10.1016/j.atherosclerosis.2014.12.023.
Badhwar S, Chandran DS, Jaryal AK, Narang R, Deepak KK. Regional arterial stiffness in central and peripheral arteries is differentially related to endothelial dysfunction assessed by brachial flow-mediated dilation in metabolic syndrome. Diab Vasc Dis Res. 2018;15:106–13. https://doi.org/10.1177/1479164117748840.
Wen J, Huang Y, Lu Y, Yuan H. Associations of non-high-density lipoprotein cholesterol, triglycerides and the total cholesterol/HDL-c ratio with arterial stiffness independent of low-density lipoprotein cholesterol in a Chinese population. Hypertens Res. 2019;42:1223–30. https://doi.org/10.1038/s41440-019-0251-5.
Roes SD, Alizadeh Dehnavi R, Westenberg JJ, Lamb HJ, Mertens BJ, Tamsma JT, et al. Assessment of aortic pulse wave velocity and cardiac diastolic function in subjects with and without the metabolic syndrome: HDL cholesterol is independently associated with cardiovascular function. Diabetes Care. 2008;31:1442–4. https://doi.org/10.2337/dc08-0055.
Adams SP, Tiellet N, Alaeiilkhchi N, Wright JM. Cerivastatin for lowering lipids. Cochrane Database Syst Rev. 2020;1:CD012501. https://doi.org/10.1002/14651858.CD012501.pub2.
Upala S, Wirunsawanya K, Jaruvongvanich V, Sanguankeo A. Effects of statin therapy on arterial stiffness: a systematic review and meta-analysis of randomized controlled trial. Int J Cardiol. 2017;227:338–41. https://doi.org/10.1016/j.ijcard.2016.11.073.
Upadhyay A, Hwang SJ, Mitchell GF, Vasan RS, Vita JA, Stantchev PI, et al. Arterial stiffness in mild-to-moderate CKD. J Am Soc Nephrol. 2009;20:2044–53. https://doi.org/10.1681/ASN.2009010074.
Tomiyama H, Tanaka H, Hashimoto H, Matsumoto C, Odaira M, Yamada J, et al. Arterial stiffness and declines in individuals with normal renal function/early chronic kidney disease. Atherosclerosis. 2010;212:345–50. https://doi.org/10.1016/j.atherosclerosis.2010.05.033.
Tomiyama H, Matsumoto C, Shiina K, Yamashina A, Brachial-Ankle PWV. Current status and future directions as a useful marker in the management of cardiovascular disease and/or cardiovascular risk factors. J Atheroscler Thromb. 2016;23:128–46. https://doi.org/10.5551/jat.32979.
Huang J, Chen Z, Yuan J, Zhang C, Chen H, Wu W, et al. Association between body mass index (BMI) and brachial-ankle pulse wave velocity (bapwv) in males with hypertension: a community-based cross-section study in North China. Med Sci Monit. 2019;25:5241–57. https://doi.org/10.12659/MSM.914881.
Hernandez-Martinez A, Martinez-Rosales E, Alcaraz-Ibañez M, Soriano-Maldonado A, Artero EG. Influence of body composition on arterial stiffness in middle-aged adults: healthy UAL cross-sectional study. Medicina. 2019;55:E334. https://doi.org/10.3390/medicina55070334.
Maple-Brown LJ, Piers LS, O’Rourke MF, Celermajer DS, O’Dea K. Central obesity is associated with reduced peripheral wave reflection in Indigenous Australians irrespective of diabetes status. J Hypertens. 2007;23:1403–7. https://doi.org/10.1097/01.hjh.0000173524.80802.5a.
Tang B, Luo F, Zhao J, Ma J, Tan I, Butlin M, et al. Relationship between body mass index and arterial stiffness in a health assessment Chinese population. Medicine. 2020;99:e18793. https://doi.org/10.1097/MD.0000000000018793.
Tomiyama H, Hashimoto H, Tanaka H, Matsumoto C, Odaira M, Yamada J, et al. Continuous smoking and progression of arterial stiffening: a prospective study. J Am Coll Cardiol. 2010;55:1979–87. https://doi.org/10.1016/j.jacc.2009.12.042.
Wilkinson IB, Mäki-Petäjä KM, Mitchell GF. Uses of arterial stiffness in clinical practice. Arterioscler Thromb Vasc Biol. 2020;40:1063–7. https://doi.org/10.1161/ATVBAHA.120.313130.
Acknowledgements
This study was supported by Omron Health Care Company (Kyoto, Japan), Asahi Calpis Wellness Company (Tokyo, Japan) and Teijin Pharma Company (Tokyo, Japan), which awarded funds to Professors Akira Yamashina and Hirofumi Tomiyama.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The sponsor (Omron Health Care Company) assisted in the data formatting (i.e., the data of the brachial–ankle PWV stored in the hard disc of the equipment used for measurement of the brachial–ankle PWV were transferred to an Excel file). Other than this, the company played no role in the design or conduct of the study, i.e., in the data collection, management, analysis or interpretation of the data or in the preparation, review or approval of the paper. The authors have no other disclosures to make.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fujii, M., Tomiyama, H., Nakano, H. et al. Differences in longitudinal associations of cardiovascular risk factors with arterial stiffness and pressure wave reflection in middle-aged Japanese men. Hypertens Res 44, 98–106 (2021). https://doi.org/10.1038/s41440-020-0523-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-020-0523-0
Keywords
This article is cited by
-
Vascular function: a key player in hypertension
Hypertension Research (2023)
-
Differential impact of antihypertensive drugs on cardiovascular remodeling: a review of findings and perspectives for HFpEF prevention
Hypertension Research (2022)
-
Vascular functional tests and preemptive medicine
Hypertension Research (2021)
-
Efficacy of intensive lipid-lowering therapy with statins stratified by blood pressure levels in patients with type 2 diabetes mellitus and retinopathy: Insight from the EMPATHY study
Hypertension Research (2021)