Abstract
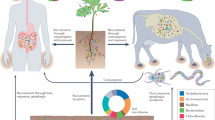
The Hippocratic text On Airs, Waters, Places advises physicians to attend to all aspects of the environment—the seasons, the wind direction, and the soil and water quality, i.e., the ecosystem—when addressing people’s health. Hippocrates emphasizes that the ecosystem influences health, disease, and therapeutic choices. Now is the time to consider how this medical wisdom can be integrated into healthcare systems and utilized for people’s health. This review discusses how the ecosystem can affect blood pressure (BP) in humans and provides a synthesis of the related resources available in the literature to inform the actions of healthcare providers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Forouzanfar MH, Liu P, Roth GA, Ng M, Biryukov S, Marczak L, et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990–2015. JAMA. 2017;317:165–82.
World Health Organization. https://www.who.int/globalchange/ecosystems/en/. Accessed Dec 23 2019.
Shahu A, Herrin J, Dhruva SS, Desai NR, Davis BR, Krumholz HM, et al. Disparities in socioeconomic context and association with blood pressure control and cardiovascular outcomes in ALLHAT. J Am Heart Assoc. 2019;8:e012277.
Lang T. Social and economic factors as obstacles to blood pressure control. Am J Hypertens. 1998;11:900–2.
Yano Y, Hoshide S, Tamaki N, Inokuchi T, Nagata M, Yokota N, et al. Regional differences in hypertensive cardiovascular remodeling between fishing and farming communities in Japan. Am J Hypertens. 2011;24:437–43.
Bravo MA, Batch BC, Miranda ML. Residential racial isolation and spatial patterning of hypertension in Durham, North Carolina. Prev Chronic Dis. 2019;16:E36.
Morenoff JD, House JS, Hansen BB, Williams DR, Kaplan GA, Hunte HE. Understanding social disparities in hypertension prevalence, awareness, treatment, and control: the role of neighborhood context. Soc Sci Med. 2007;65:1853–66.
Margolis KL, Asche SE, Bergdall AR, Dehmer SP, Groen SE, Kadrmas HM, et al. Effect of home blood pressure telemonitoring and pharmacist management on blood pressure control: a cluster randomized clinical trial. JAMA. 2013;310:46–56.
Mileski M, Kruse CS, Catalani J, Haderer T. Adopting telemedicine for the self-management of hypertension: systematic review. JMIR Med Inf. 2017;5:e41.
Mills KT, Obst KM, Shen W, Molina S, Zhang HJ, He H, et al. Comparative effectiveness of implementation strategies for blood pressure control in hypertensive patients: a systematic review and meta-analysis. Ann Intern Med. 2018;168:110–20.
Hammond G, Joynt Maddox KE. A theoretical framework for clinical implementation of social determinants of health. JAMA Cardiol. 2019. https://doi.org/10.1001/jamacardio.2019.3805. No abstract available. PMID: 31596433.
Bradley EH, Canavan M, Rogan E, Talbert-Slagle K, Ndumele C, Taylor L, et al. Variation In health outcomes: the role of spending on social services, public health, and health care, 2000–09. Health Aff. 2016;35:760–8.
Campbell F, Conti G, Heckman JJ, Moon SH, Pinto R, Pungello E, et al. Early childhood investments substantially boost adult health. Science. 2014;343:1478–85.
Turnbaugh PJ, Ley RE, Hamady M, Fraser-Liggett CM, Knight R, Gordon JI. The human microbiome project. Nature. 2007;449:804–10.
Faith JJ, Guruge JL, Charbonneau M, Subramanian S, Seedorf H, Goodman AL, et al. The long-term stability of the human gut microbiota. Science. 2013;341:1237439.
Sun S, Lulla A, Sioda M, Winglee K, Wu MC, Jacobs DR Jr, et al. Gut microbiota composition and blood pressure. Hypertension. 2019;73:998–1006.
Kelly TN, Bazzano LA, Ajami NJ, He H, Zhao J, Petrosino JF, et al. Gut microbiome associates with lifetime cardiovascular disease risk profile among bogalusa heart study participants. Circ Res. 2016;119:956–64.
Yu Y, Mao G, Wang J, Zhu L, Lv X, Tong Q, et al. Gut dysbiosis is associated with the reduced exercise capacity of elderly patients with hypertension. Hypertens Res. 2018;41:1036–44.
Zimmermann M, Zimmermann-Kogadeeva M, Wegmann R, Goodman AL. Mapping human microbiome drug metabolism by gut bacteria and their genes. Nature. 2019;570:462–7.
Blum WEH, Zechmeister-Boltenstern S, Keiblinger KM. Does soil contribute to the human gut microbiome? Microorganisms. 2019;7:E287. https://doi.org/10.3390/microorganisms7090287.
Duffy JE, Godwin CM, Cardinale BJ. Biodiversity effects in the wild are common and as strong as key drivers of productivity. Nature. 2017;549:261–4.
Soliveres S, van der Plas F, Manning P, Prati D, Gossner MM, Renner SC, et al. Biodiversity at multiple trophic levels is needed for ecosystem multifunctionality. Nature. 2016;536:456–9.
Inda ME, Broset E, Lu TK, de la Fuente-Nunez C. Emerging frontiers in microbiome engineering. Trends Immunol. 2019;40:952–73.
Kaczmarek JL, Thompson SV, Holscher HD. Complex interactions of circadian rhythms, eating behaviors, and the gastrointestinal microbiota and their potential impact on health. Nutr Rev. 2017;75:673–82.
Claesson MJ, Jeffery IB, Conde S, Power SE, O’Connor EM, Cusack S, et al. Gut microbiota composition correlates with diet and health in the elderly. Nature. 2012;488:178–84.
Dill-McFarland KA, Tang ZZ, Kemis JH, Kerby RL, Chen G, Palloni A, et al. Close social relationships correlate with human gut microbiota composition. Sci Rep. 2019;9:703.
Crowther TW, van den Hoogen J, Wan J, Mayes MA, Keiser AD, Mo L, et al. The global soil community and its influence on biogeochemistry. Science. 2019;365:eaav0550. https://doi.org/10.1126/science.aav0550.
Rook GA. Review series on helminths, immune modulation and the hygiene hypothesis: the broader implications of the hygiene hypothesis. Immunology. 2009;126:3–11.
Liu Y, Wang S, Wang Z, Zhang Z, Qin H, Wei Z, et al. Soil microbiome mediated nutrients decline during forest degradation process. Soil Ecol Lett. 2019;1:59–71.
Ideno Y, Hayashi K, Abe Y, Ueda K, Iso H, Noda M, et al. Blood pressure-lowering effect of Shinrin-yoku (Forest bathing): a systematic review and meta-analysis. BMC Complement Alter Med. 2017;17:409.
Bowyer RCE, Jackson MA, Pallister T, Skinner J, Spector TD, Welch AA, et al. Use of dietary indices to control for diet in human gut microbiota studies. Microbiome. 2018;6:77.
Partula V, Mondot S, Torres MJ, Kesse-Guyot E, Deschasaux M, Assmann K, et al. Associations between usual diet and gut microbiota composition: results from the Milieu Intérieur cross-sectional study. Am J Clin Nutr. 2019;109:1472–83.
Monda V, Villano I, Messina A, Valenzano A, Esposito T, Moscatelli F, et al. Exercise modifies the gut microbiota with positive health effects. Oxid Med Cell Longev. 2017;2017:3831972.
Smith RP, Easson C, Lyle SM, Kapoor R, Donnelly CP, Davidson EJ, et al. Gut microbiome diversity is associated with sleep physiology in humans. PLoS One. 2019;14:e0222394.
Mills JG, Weinstein P, Gellie NJC, Weyrich LS, Lowe AJ, Breed MF. Urban habitat restoration provides a human health benefit through microbiome rewilding: the microbiome rewilding hypothesis. Restor Ecol. 2017;25:866.
Eckburg PB, Bik EM, Bernstein CN, Purdom E, Dethlefsen L, Sargent M, et al. Diversity of the human intestinal microbial flora. Science. 2005;308:1635–8.
De Filippo C, Cavalieri D, Di Paola M, Ramazzotti M, Poullet JB, Massart S, et al. Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa. Proc Natl Acad Sci USA. 2010;107:14691–6.
Yang T, Santisteban MM, Rodriguez V, Li E, Ahmari N, Carvajal JM, et al. Gut dysbiosis is linked to hypertension. Hypertension. 2015;65:1331–40.
Santisteban MM, Qi Y, Zubcevic J, Kim S, Yang T, Shenoy V, et al. Hypertension-linked pathophysiological alterations in the gut. Circ Res. 2017;120:312–23.
Huart J, Leenders J, Taminiau B, Descy J, Saint-Remy A, Daube G, et al. Gut microbiota and fecal levels of short-chain fatty acids differ upon 24-hour blood pressure levels in men. Hypertension. 2019;74:1005–13.
O’Mahony SM, Clarke G, Borre YE, Dinan TG, Cryan JF. Serotonin, tryptophan metabolism and the brain-gut-microbiome axis. Behav Brain Res. 2015;277:32–48.
Pluznick JL, Protzko RJ, Gevorgyan H, Peterlin Z, Sipos A, Han J, et al. Olfactory receptor responding to gut microbiota-derived signals plays a role in renin secretion and blood pressure regulation. Proc Natl Acad Sci USA. 2013;110:4410–5.
Yang T, Magee KL, Colon-Perez LM, Larkin R, Liao YS, Balazic E, et al. Impaired butyrate absorption in the proximal colon, low serum butyrate and diminished central effects of butyrate on blood pressure in spontaneously hypertensive rats. Acta Physiol. 2019;226:e13256.
Kim S, Goel R, Kumar A, Qi Y, Lobaton G, Hosaka K, et al. Imbalance of gut microbiome and intestinal epithelial barrier dysfunction in patients with high blood pressure. Clin Sci. 2018;132:701–71.
Khalesi S, Sun J, Buys N, Jayasinghe R. Effect of probiotics on blood pressure: a systematic review and meta-analysis of randomized, controlled trials. Hypertension. 2014;64:897–903.
Van Staden Adu P, Heunis T, Smith C, Deane S, Dicks LM. Efficacy of lantibiotic treatment of staphylococcus aureus-induced skin infections, monitored by in vivo bioluminescent imaging. Antimicrob Agents Chemother. 2016;60:3948–55.
Kingwell K. Bacteriophage therapies re-enter clinical trials. Nat Rev Drug Disco. 2015;14:515–6.
National Centers for Environmental Information. Global climate report. Washington, DC: National Centers for Environmental Information: 2018. https://www.ncdc.noaa.gov/sotc/global/201804.
Ahima RS. Global warming threatens human thermoregulation and survival. J Clin Invest. 2020:135006. https://doi.org/10.1172/JCI135006.
Haines A, Ebi K. The imperative for climate action to protect health. N Engl J Med. 2019;380:263–73.
Bond-Lamberty B, Bailey VL, Chen M, Gough CM, Vargas R. Globally rising soil heterotrophic respiration over recent decades. Nature. 2018;560:80–83.
Dietz WH. Climate change and malnutrition: we need to act now. J Clin Invest. 2020:135004. https://doi.org/10.1172/JCI135004.
Tsao TM, Tsai MJ, Hwang JS, Su TC. Health effects of seasonal variation in cardiovascular hemodynamics among workers in forest environments. Hypertens Res. 2019;42:223–32.
Modesti PA, Rapi S, Rogolino A, Tosi B, Galanti G. Seasonal blood pressure variation: implications for cardiovascular risk stratification. Hypertens Res. 2018;41:475–82.
Japan Times. https://www.japantimes.co.jp/news/2019/08/06/national/57-dead-18000-taken-hospitals-one-week-amid-japan-heat-wave/#.XjHmYHdFw2z (2019).
Protsiv M, Ley C, Lankester J, Hastie T, Parsonnet J. Decreasing human body temperature in the United States since the industrial revolution. Elife. 2020;9:e49555. https://doi.org/10.7554/eLife.49555.
Hausfater P, Megarbane B, Dautheville S, Patzak A, Andronikof M, Santin A, et al. Prognostic factors in non-exertional heatstroke. Intensive Care Med. 2010;36:272–80.
Sommet A, Durrieu G, Lapeyre-Mestre M, Montastruc JL. Association of French PharmacoVigilance Centres. A comparative study of adverse drug reactions during two heat waves that occurred in France in 2003 and 2006. Pharmacoepidemiol Drug Saf. 2012;21:285–8.
Salas RN, Jha AK. Climate change threatens the achievement of effective universal healthcare. BMJ. 2019;366:l5302.
Mobula LM, Fisher ML, Lau N, Estelle A, Wood T, Plyler W. Prevalence of hypertension among patients attending mobile medical clinics in the Philippines after typhoon Haiyan. PLoS Curr. 2016;8:ecurrents.dis.5aaeb105e840c72370e8e688835882ce. https://doi.org/10.1371/currents.dis.5aaeb105e840c72370e8e688835882ce.
Acknowledgements
I gratefully acknowledge my great mentors in Japan and the US as well as the numerous study investigators, fellows, nurses, and research coordinators at each of the study sites. I also gratefully acknowledge my family and friends; their continued support is essential in my journey as a physician and researcher.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that he has no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yano, Y. Blood pressure management in an ecosystem context. Hypertens Res 43, 989–994 (2020). https://doi.org/10.1038/s41440-020-0464-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-020-0464-7
Keywords
This article is cited by
-
Digital hypertension towards to the anticipation medicine
Hypertension Research (2023)
-
Role of housing in blood pressure control: a review of evidence from the Smart Wellness Housing survey in Japan
Hypertension Research (2023)
-
Air pollution impairs endothelial function and blood pressure
Hypertension Research (2022)
-
Role of the microbiota in hypertension and antihypertensive drug metabolism
Hypertension Research (2022)
-
Catheter-based ultrasound renal denervation in patients with resistant hypertension: the randomized, controlled REQUIRE trial
Hypertension Research (2022)