Abstract
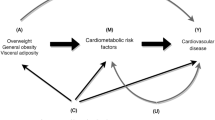
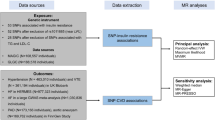
Studies on leptin and blood pressure (BP) associations have yielded inconsistent findings. The current study aimed to evaluate the effect of genetically determined leptin on BP and to explore whether smoking status modified this effect. We conducted a Mendelian randomization analysis using the baseline data of 3860 participants in the Framingham Heart Study 3rd generation cohort. Pairwise associations among leptin genetic risk score (GRS), log-transformed leptin (log-leptin), and BP were assessed by multivariate linear regression models. Age and sex were adjusted in the base model, and education, smoking, drinking, and physical activity were adjusted in the full model. The interaction between leptin GRS and smoking was evaluated by adding an interaction term, GRS × smoking, in the fully adjusted model. In the age- and sex-adjusted analyses, log-leptin was positively associated with systolic BP (SBP) (P = 2.35 × 10−79), diastolic BP (DBP) (P = 6.19 × 10−76), mean arterial pressure (MAP) (P = 1.10 × 10−90), and pulse pressure (P = 4.38 × 10−19). Leptin GRS significantly increased log-leptin (P = 0.00001). Leptin GRS was associated with reduced SBP (P = 0.04), DBP (P = 0.006), and MAP (P = 0.008) among current smokers. In the fully adjusted model, significant interactions between GRS and smoking were identified for SBP (P = 0.02), DBP (P = 0.002), and MAP (P = 0.003). Sensitivity analyses among participants not taking antihypertensive or glucose-lowering medications revealed similar associations. Our study provided evidence for a potentially causal relationship between leptin and BP among current smokers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Muntner P, Carey RM, Gidding S, Jones DW, Taler SJ, Wright JT, et al. Potential US population impact of the 2017 ACC/AHA High Blood Pressure Guideline. Circulation. 2018;137:109–18.
Hall JE, do Carmo JM, da Silva AA, Wang Z, Hall ME. Obesity-induced hypertension: interaction of neurohumoral and renal mechanisms. Circ Res. 2015;116:991–1006.
Simonds SE, Pryor JT, Ravussin E, Greenway FL, Dileone R, Allen AM, et al. Leptin mediates the increase in blood pressure associated with obesity. Cell. 2014;159:1404–16.
Huby AC, Otvos L, Belin de Chantemèle EJ. Leptin induces hypertension and endothelial dysfunction via aldosterone-dependent mechanisms in obese female mice. Hypertension. 2016;67:1020–8.
Allison MA, Ix JH, Morgan C, McClelland RL, Rifkin D, Shimbo D, et al. Higher leptin is associated with hypertension: the multi-ethnic study of atherosclerosis. J Hum Hypertens. 2013;27:617–22.
Sheu WH, Lee WJ, Chen YT. High plasma leptin concentrations in hypertensive men but not in hypertensive women. J Hypertens. 1999;17:1289–95.
Kokot F, Adamczak M, Wiecek A, Cieplok J. Does leptin play a role in the pathogenesis of essential hypertension? Kidney Blood Press Res. 1999;22:154–60.
Schorr U, Blaschke K, Turan S, Distler A, Sharma AM. Relationship between angiotensinogen, leptin and blood pressure levels in young normotensive men. J Hypertens. 1998;16:1475–80.
Ma D, Feitosa MF, Wilk JB, Laramie JM, Yu K, Leiendecker-Foster C, et al. Leptin is associated with blood pressure and hypertension in women from the National Heart, Lung, and Blood Institute Family Heart Study. Hypertension. 2009;53:473–9.
Smith W, Schutte R, Huisman HW, Van Rooyen JM, Ware LJ, Fourie CM, et al. Leptin is positively associated with blood pressure in african men with a low body mass index: the SAfrEIC study. Horm Metab Res. 2015;47:145–51.
Schutte R, Huisman HW, Schutte AE, Malan NT. Leptin is independently associated with systolic blood pressure, pulse pressure and arterial compliance in hypertensive African women with increased adiposity: the POWIRS study. J Hum Hypertens. 2005;19:535–41.
Brown RJ, Meehan CA, Gorden P. Leptin does not mediate hypertension associated with human obesity. Cell. 2015;162:465–6.
Kamimura D, Suzuki T, Wang W, deShazo M, Hall JE, Winniford MD, et al. Higher plasma leptin levels are associated with reduced left ventricular mass and left ventricular diastolic stiffness in black women: insights from the Genetic Epidemiology Network of Arteriopathy (GENOA) study. Hypertens Res. 2018;41:629–38.
Reseland JE, Mundal HH, Hollung K, Haugen F, Zahid N, Anderssen SA, et al. Cigarette smoking may reduce plasma leptin concentration via catecholamines. Prostaglandins, Leukotrienes, Essent Fat Acids. 2005;73:43–9.
Kryfti M, Dimakou K, Toumbis M, Daniil Z, Hatzoglou C, Gourgoulianis KI. Effects of smoking cessation on serum leptin and adiponectin levels. Tob Induc Dis. 2015;13:30.
Nagayasu S, Suzuki S, Yamashita A, Taniguchi A, Fukushima M, Nakai Y, et al. Smoking and adipose tissue inflammation suppress leptin expression in Japanese obese males: potential mechanism of resistance to weight loss among Japanese obese smokers. Tob Induc Dis. 2012;10:3.
Hughes K, Leong WP, Sothy SP, Lun KC, Yeo PP. Relationships between cigarette smoking, blood pressure and serum lipids in the Singapore general population. Int J Epidemiol. 1993;22:637–43.
Primatesta P, Falaschetti E, Gupta S, Marmot MG, Poulter NR. Association between smoking and blood pressure: evidence from the health survey for England. Hypertension. 2001;37:187–93.
Li J, Cui R, Eshak ES, Yamagishi K, Imano H, Muraki I, et al. Association of cigarette smoking with radial augmentation index: the Circulatory Risk in Communities Study (CIRCS). Hypertens Res. 2018;41:1054–62.
Splansky GL, Corey D, Yang Q, Atwood LD, Cupples LA, Benjamin EJ, et al. The Third Generation Cohort of the National Heart, Lung, and Blood Institute's Framingham Heart Study: design, recruitment, and initial examination. Am J Epidemiol. 2007;165:1328–35.
Kilpeläinen TO, Carli JF, Skowronski AA, Sun Q, Kriebel J, Feitosa MF, et al. Genome-wide meta-analysis uncovers novel loci influencing circulating leptin levels. Nat Commun. 2016;7:10494.
Beaumont RN, Warrington NM, Cavadino A, Tyrrell J, Nodzenski M, Horikoshi M, et al. Genome-wide association study of offspring birth weight in 86577 women identifies five novel loci and highlights maternal genetic effects that are independent of fetal genetics. Hum Mol Genet. 2018;27:742–56.
Auton A, Brooks LD, Durbin RM, Garrison EP, Kang HM, Korbel JO, et al. A global reference for human genetic variation. Nature. 2015; 526:68–74.
Das S, Forer L, Schönherr S, Sidore C, Locke AE, Kwong A, et al. Next-generation genotype imputation service and methods. Nat Genet. 2016;48:1284–7.
Andersson C, Lyass A, Larson MG, Robins SJ, Vasan RS. Low-density-lipoprotein cholesterol concentrations and risk of incident diabetes: epidemiological and genetic insights from the Framingham Heart Study. Diabetologia. 2015;58:2774–80.
Zachariah JP, Quiroz R, Nelson KP, Teng Z, Keaney JF, Sullivan LM, et al. Prospective relation of circulating adipokines to incident metabolic syndrome: the Framingham Heart Study. J Am Heart Assoc. 2017;6.
von Jeinsen B, Short MI, Xanthakis V, Carneiro H, Cheng S, Mitchell GF, et al. Association of circulating adipokines with echocardiographic measures of cardiac structure and function in a community-based cohort. J Am Heart Assoc. 2018;7.
Li C, Kim YK, Dorajoo R, Li H, Lee IT, Cheng CY, et al. Genome-wide association study meta-analysis of long-term average blood pressure in East Asians. Circ Cardiovasc Genet. 2017;10:e001527.
Li C, He J, Chen J, Zhao J, Gu D, Hixson JE, et al. Genome-wide gene-potassium interaction analyses on blood pressure: the GenSalt Study (Genetic Epidemiology Network of Salt Sensitivity). Circ Cardiovasc Genet. 2017;10.
Kannel WB, Sorlie P. Some health benefits of physical activity. The Framingham Study. Arch Intern Med. 1979;139:857–61.
Faul F, Erdfelder E, Lang AG, Buchner A. G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;39:175–91.
Faul F, Erdfelder E, Buchner A, Lang AG. Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav Res Methods. 2009;41:1149–60.
Heymsfield SB, Greenberg AS, Fujioka K, Dixon RM, Kushner R, Hunt T, et al. Recombinant leptin for weight loss in obese and lean adults: a randomized, controlled, dose-escalation trial. JAMA. 1999;282:1568–75.
Fei H, Okano HJ, Li C, Lee GH, Zhao C, Darnell R, et al. Anatomic localization of alternatively spliced leptin receptors (Ob-R) in mouse brain and other tissues. Proc Natl Acad Sci USA. 1997;94:7001–5.
Morris DL, Rui L. Recent advances in understanding leptin signaling and leptin resistance. Am J Physiol Endocrinol Metab. 2009;297:E1247–59.
Tu H, Kastin AJ, Hsuchou H, Pan W. Soluble receptor inhibits leptin transport. J Cell Physiol. 2008;214:301–5.
Pan W, Kastin AJ. Adipokines and the blood-brain barrier. Peptides. 2007;28:1317–30.
Al Mutairi SS, Mojiminiyi OA, Shihab-Eldeen AA, Al Sharafi A, Abdella N. Effect of smoking habit on circulating adipokines in diabetic and non-diabetic subjects. Ann Nutr Metab. 2008;52:329–34.
Park HK, Ahima RS. Physiology of leptin: energy homeostasis, neuroendocrine function and metabolism. Metabolism. 2015;64:24–34.
Kraja AT, Vaidya D, Pankow JS, Goodarzi MO, Assimes TL, Kullo IJ, et al. A bivariate genome-wide approach to metabolic syndrome: STAMPEED consortium. Diabetes. 2011;60:1329–39.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Shen, L., Cordero, J.F., Wang, JS. et al. The effect of leptin on blood pressure considering smoking status: a Mendelian randomization study. Hypertens Res 43, 342–349 (2020). https://doi.org/10.1038/s41440-019-0376-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-019-0376-6