Abstract
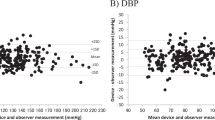
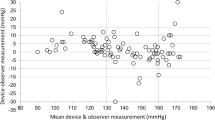
Despite the wide use of automated devices for the self-measurement of home blood pressure (BP), no evidence is available regarding the accuracy of such devices in oldest-old populations. The aim of this study was to validate the accuracy of the automated oscillometric upper arm-cuff BP-monitoring device according to an international protocol in oldest-old individuals. In 35 participants aged over 85 years old, BP was measured on the same arm sequentially using a mercury sphygmomanometer (by two observers) and an Omron HEM-7080IC. The difference between the test device and observer measurements and associated factors were evaluated according to the International Organization for Standardization (ISO) 81060-2:2013 protocol. A total of 105 pairs (three pairs per participant) of the test device and observer BP measurements were obtained. The mean (±standard deviation: SD) differences in systolic BP (SBP) and diastolic BP (DBP) between the methods were −0.7 ± 7.1 and −1.1 ± 4.5 mmHg, respectively, and those for each participant were −0.7 ± 5.8 mmHg for SBP and −1.1 ± 4.1 mmHg for DBP; the device therefore fulfilled the requirements of the ISO protocol. In the multivariate analysis with the linear mixed model, the difference was associated with the cuff size for SBP and pulse pressure for DBP. The Omron HEM-7080IC passed the ISO requirements for oldest-old individuals aged 85 years or older. This device can be recommended for clinical and self/home use in oldest-old populations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
He W, Goodkind D, Kowal P, US Census Bureau. An aging world: 2015, International Population Reports. Washington, DC: U.S. Government Publishing Office; 2016. https://www.census.gov/content/dam/Census/library/publications/2016/demo/p95-16-1.pdf. Accessed 17 Apr 2019.
McDonald M, Hertz RP, Unger AN, Lustik MB. Prevalence, awareness, and management of hypertension, dyslipidemia, and diabetes among United States adults aged 65 and older. J Gerontol A Biol Sci Med Sci. 2009;64:256–63.
Ishine M, Okumiya K, Hirosaki M, Sakamoto R, Fujisawa M, Hotta N, et al. Prevalence of hypertension and its awareness, treatment, and satisfactory control through treatment in elderly Japanese. J Am Geriatr Soc. 2008;56:374–5.
Lloyd-Jones DM, Evans JC, Levy D. Hypertension in adults across the age spectrum: current outcomes and control in the community. JAMA. 2005;294:466–72.
Fujiyoshi A, Ohkubo T, Miura K, Murakami Y, Nagasawa SY, Okamura T, et al. Blood pressure categories and long-term risk of cardiovascular disease according to age group in Japanese men and women. Hypertens Res. 2012;35:947–53.
Dumurgier J, Elbaz A, Dufouil C, Tavernier B, Tzourio C. Hypertension and lower walking speed in the elderly: the Three-City study. J Hypertens. 2010;28:1506–14.
Hajjar I, Lackland DT, Cupples LA, Lipsitz LA. Association between concurrent and remote blood pressure and disability in older adults. Hypertension. 2007;50:1026–32.
Cappuccio FP, Meilahn E, Zmuda JM, Cauley JA. High blood pressure and bone-mineral loss in elderly white women: a prospective study. Study of Osteoporotic Fractures Research Group. Lancet. 1999;354:971–5.
Beckett NS, Peters R, Fletcher AE, Staessen JA, Liu L, Dumitrascu D, et al. Treatment of hypertension in patients 80 years of age or older. N Engl J Med. 2008;358:1887–98.
SPRINT Research Group, Wright JT Jr, Williamson JD, Whelton PK, Snyder JK, Sink KM, et al. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med. 2015;373:2103–16.
American Geriatrics Society Expert Panel on the Care of Older Adults with Multimorbidity. Guiding principles for the care of older adults with multimorbidity: an approach for clinicians. J Am Geriatr Soc. 2012;60:E1–E25.
Pickering TG, Miller NH, Ogedegbe G, Krakoff LR, Artinian NT, Goff D. Call to action on use and reimbursement for home blood pressure monitoring: a joint scientific statement from the American Heart Association, American Society of Hypertension, and Preventive Cardiovascular Nurses Association. Hypertension. 2008;52:10–29.
van Popele NM, Bos WJ, de Beer NA, van Der Kuip DA, Hofman A, Grobbee DE, et al. Arterial stiffness as underlying mechanism of disagreement between an oscillometric blood pressure monitor and a sphygmomanometer. Hypertension. 2000;36:484–8.
Pannarale G, Bebb G, Clark S, Sullivan A, Foster C, Coats AJ. Bias and variability in blood pressure measurement with ambulatory records. Hypertension. 1993;22:591–8.
O’Rourke MF, Nichols WW. Aortic diameter, aortic stiffness, and wave reflection increase with age and isolated systolic hypertension. Hypertension. 2005;45:652–8.
Altunkan S, Iliman N, Altunkan E. Validation of the Omron M6 (HEM-7001-E) upper arm blood pressure measuring device according to the International Protocol in elderly patients. Blood Press Monit. 2008;13:117–22.
Omboni S, Riva I, Giglio A, Caldara G, Groppelli A, Parati G. Validation of the Omron M5-I, R5-I and HEM-907 automated blood pressure monitors in elderly individuals according to the International Protocol of the European Society of Hypertension. Blood Press Monit. 2007;12:233–42.
Rosholm JU, Arnspang S, Matzen L, Jacobsen IA. Auscultatory versus oscillometric measurement of blood pressure in octogenarians. Blood Press. 2012;21:269–72.
ISO 81060-2:2013, Non-invasive Sphygmomanometers—Part 2: Clinical Investigation of Automated Measurement Type. International Organization for Standardization. 2013.
Coleman A, Freeman P, Steel S, Shennan A. Validation of the Omron 705IT (HEM-759-E) oscillometric blood pressure monitoring device according to the British Hypertension Society protocol. Blood Press Monit. 2006;11:27–32.
El Assaad MA, Topouchian JA, Asmar RG. Evaluation of two devices for self-measurement of blood pressure according to the international protocol: the Omron M5-I and the Omron 705IT. Blood Press Monit. 2003;8:127–33.
Stergiou GS, Alpert B, Mieke S, Asmar R, Atkins N, Eckert S, et al. A universal standard for the validation of blood pressure measuring devices: Association for the Advancement of Medical Instrumentation/European Society of Hypertension/International Organization for Standardization (AAMI/ESH/ISO) Collaboration Statement. J Hypertens. 2018;36:472–8.
Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet. 1986;1:307–10.
Kamide K, Kabayama M. Implications of blood pressure variations in older populations. Hypertens Res. 2019;42:19–25.
Jansen RW, Lipsitz LA. Postprandial hypotension: epidemiology, pathophysiology, and clinical management. Ann Intern Med. 1995;122:286–95.
O’Brien E, Petrie J, Littler W, de Swiet M, Padfield PL, Altman DG, et al. An outline of the revised British Hypertension Society protocol for the evaluation of blood pressure measuring devices. J Hypertens. 1993;11:677–9.
O’Brien E, Pickering T, Asmar R, Myers M, Parati G, Staessen J, et al. Working Group on Blood Pressure Monitoring of the European Society of Hypertension International Protocol for validation of blood pressure measuring devices in adults. Blood Press Monit. 2002;7:3–17.
Thijs L, Den Hond E, Nawrot T, Staessen JA. Prevalence, pathophysiology and treatment of isolated systolic hypertension in the elderly. Expert Rev Cardiovasc Ther. 2004;5:761–9.
O’Brien E. Review: a century of confusion; which bladder for accurate blood pressure measurement? J Hum Hypertens. 1996;10:565–72.
Stergiou GS, Yiannes NG, Rarra VC. Validation of the Omron 705 IT oscillometric device for home blood pressure measurement in children and adolescents: the Arsakion School Study. Blood Press Monit. 2006;11:229–34.
Alpert BS. Validation of the Omron HEM-9210T by the ANSI/AAMI/ISO 81060-2: 2013 with two novel cuffs: wide-range and extra-large. Blood Press Monit. 2017;22:166–8.
Bing S, Chen K, Hou H, Zhang W, Li L, Wei J, et al. Validation of the Microlife BP A200 Comfort and W2 Slim automated blood pressure monitors in a general adult population according to the European Society of Hypertension and the ANSI/AAMI/ISO 81060-2: 2013 protocols. Blood Press Monit. 2016;21:118–23.
Hosoya N, Okada T, Muto Y. Japanese Anthropometric reference data: JARD 2001 (in Japanese). Jpn J Nutr Assess. 2002;19(Suppl):1–81.
Gavriilidou NN, Pihlsgard M, Elmstahl S. Anthropometric reference data for elderly Swedes and its disease-related pattern. Eur J Clin Nutr. 2015;69:1066–75.
Bannerman E, Reilly JJ, MacLennan WJ, Kirk T, Pender F. Evaluation of validity of British anthropometric reference data for assessing nutritional state of elderly people in Edinburgh: cross sectional study. BMJ. 1997;315:338–41.
Fryar CD, Gu Q, Ogden CL, Flegal KM. Anthropometric reference data for children and adults: United States, 2011–4. Vital Health Stat 3. 2016;39:1–46.
Barbosa AR, Souza JM, Lebrão ML, Laurenti R, Marucci Mde F. Anthropometry of elderly residents in the city of São Paulo, Brazil. Cad Saude Publica. 2005;21:1929–38.
Imai Y, Obara T, Ohkubo T. How many times should we ask subjects to measure blood pressure at home on each occasion? J Hypertens. 2007;25:1987–91.
Rhee MY, Kim JY, Kim JH, Namgung J, Lee SY, Cho DK, et al. Optimal schedule of home blood-pressure measurements for the diagnosis of hypertension. Hypertens Res. 2018;41:738–47.
Acknowledgements
This study was supported by a research grant from Omron Healthcare Co., Ltd. We thank all patients who participated to this study. We would like to thank Drs. Takeya, Kurinami, and Akasaka from the Department of Geriatric Medicine, Osaka University Hospital for their cooperation with this study. We also thank Ms. Tuo, Mr. Akagi, and other members of the Health Science Division, Osaka University Graduate School of Medicine for their assistance in conducting this study.
Funding
KA, KK, and TO recieved research grants from Omron Healthcare Co., Ltd. The sponsor of this study was not involved in data collection or analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
KSa is a salaried employee of Omron Healthcare Co., Ltd. The remaining authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Godai, K., Kabayama, M., Saito, K. et al. Validation of an automated home blood pressure measurement device in oldest-old populations. Hypertens Res 43, 30–35 (2020). https://doi.org/10.1038/s41440-019-0330-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-019-0330-7
Keywords
This article is cited by
-
In-office and out-of-office blood pressure measurement
Journal of Human Hypertension (2021)
-
Recent status of self-measured home blood pressure in the Japanese general population: a modern database on self-measured home blood pressure (MDAS)
Hypertension Research (2020)
-
Frailty and hypertension in older adults: current understanding and future perspectives
Hypertension Research (2020)
-
Day-to-day blood pressure variability is associated with lower cognitive performance among the Japanese community-dwelling oldest-old population: the SONIC study
Hypertension Research (2020)