Abstract
Renin–angiotensin system (RAS) inhibitors are often used as a first-line treatment for hypertensive patients with diabetes because of purported benefits, such as reno-protection. However, there is no clear evidence for the superiority of RAS inhibitors to other classes of antihypertensives for clinically important outcomes in this population. We conducted a meta-analysis to assess whether RAS inhibitors are better than other classes of antihypertensives for reducing mortality, and cardiovascular and renal events in hypertensive patients with diabetes. From June to December 2017, we searched Medline, Cochrane Library, and the database of the Japan Medical Abstracts Society (ICHUSHI) for relevant published randomized controlled trials that directly compared the effects of RAS inhibitors to other classes of antihypertensives as first-line treatments for reducing adverse outcomes among hypertensive patients with diabetes. Our predetermined outcomes included all-cause death, cardiovascular death, incidence of cardiovascular disease, and renal dysfunction. We identified 16 trials, including a total of 35,052 patients. No significant benefits for RAS inhibitors were found compared to other classes of antihypertensives for all-cause death (relative risk (RR) 0.95, 95% confidence interval (CI) 0.85–1.05, p = 0.29), cardiovascular death (RR 0.84, 95% CI 0.68–1.04, p = 0.11), incidence of cardiovascular disease (RR 0.93, 95% CI 0.84–1.03, p = 0.16), and incidence of renal dysfunction (RR 0.91, 95% CI 0.77–1.06, p = 0.22). In conclusion, RAS inhibitors are not superior to other classes of antihypertensive drugs for reducing all-cause and cardiovascular mortalities, cardiovascular events, and renal events in hypertensive patients with diabetes.
Similar content being viewed by others
Introduction
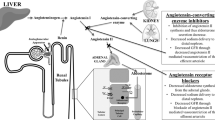
Hypertension is common among patients with both type 1 and 2 diabetes [1, 2]. Controlling blood pressure has been demonstrated to be effective for lowering the risk of microvascular (renal, ocular, or neural) and macrovascular (atherosclerotic cardiovascular disease) complications in patients with diabetes [3,4,5]. Clinical guidelines in Europe and in the US [6,7,8] indicate that the degree of blood pressure reduction is considered the major determinant of reduction in cardiovascular risk rather than the choice of antihypertensive drug class. Consequently, those guidelines recommend any of the drug classes shown to reduce cardiovascular events for patients with diabetes, such as angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), thiazide-like diuretics, or dihydropyridine calcium-channel blockers (CCBs), as a first-line treatment for hypertensive patients with diabetes.
Renin–angiotensin system (RAS) inhibitors, which are mainly ACE inhibitors and ARBs, have the best efficacy for decreasing urinary albumin excretion [9] among antihypertensives. Since albuminuria is a known risk factor for cardiovascular events, RAS inhibitors have a potential benefit over other antihypertensive classes as the first-line treatment of hypertensives with diabetes for reducing cardiovascular risk. In fact, the Guidelines for the Management of Hypertension 2014 by the Japanese Society of Hypertension [10] and the Japanese Clinical Practice Guideline for Diabetes 2016 by the Japanese Diabetes Society [11] recommend RAS inhibitors as a first-line treatment for hypertension in patients with diabetes primarily because of their renoprotective properties (i.e., reduction in intraglomerular pressure and albuminuria) in addition to their metabolically favorable effects (i.e., improved insulin resistance not affecting the lipid level) [12,13,14,15,16]. However, there is no clear evidence favoring RAS inhibitors over other classes of drugs for reducing clinically important adverse outcomes, such as cardiovascular events or all-cause death for hypertensive patients with diabetes.
Therefore, in this meta-analysis, we sought to assess whether RAS inhibitors are superior to other classes of antihypertensive drugs as first-line pharmacological blood pressure (BP) treatments for hypertensive patients with diabetes in terms of reducing the risk of all-cause mortality and cardiovascular or renal events.
Methods
We conducted a systematic review and meta-analysis of the literature following the Preferred Reporting Items for Systematic reviews and Meta-Analyses statement for the conduct of meta-analyses of intervention studies [17]. We performed all the procedures from June 2017 to December 2017.
Data sources and search strategy
We searched Medline, the Cochrane Library database, and the database of Japan Medical Abstracts Society (Igaku Chuo Zasshi; ICHUSHI) for relevant published randomized controlled trials (RCTs). The search was limited to studies published in English or Japanese, but otherwise no restrictions, such as publication year, age, ethnicity/race, and countries/areas of study participants, were included. For the literature search, we used the key words including “diabetes mellitus”, “angiotensin-converting enzyme inhibitor”, “ACEI”, “angiotensin receptor antagonists”, “angiotensin receptor blocker”, “receptor blocker”, “ARB”, “mineralocorticoid receptor antagonists”, “renin inhibitor”, “alpha blocker”, “beta blocker”, “calcium channel blocker”, “CCB”, “channel blocker”, “diuretic”, “thiazide”, and specific names of each typical antihypertensive drug (Supplementary Table 1).
Study selection
In the primary screening, reviewers (AK, AF, HS, NH, and HO) screened the titles and abstracts of all identified studies independently and in duplicate. In the secondary screening, the same reviewers independently screened the full texts of possibly eligible studies and evaluated their eligibility. Disagreements in evaluations were resolved through adjudication among the reviewers.
We included only RCTs that directly compared the effects of RAS inhibitors (ACE inhibitors, ARBs, mineralocorticoid receptor antagonists, and renin inhibitors) and other classes of antihypertensive drugs as a first-line pharmacological treatment for lowering BP in hypertensive patients with diabetes. The exclusion criteria were the following: RAS inhibitor(s) were added to an existing pharmacological treatment; a combined regimen of RAS inhibitors was compared against other regimens of antihypertensives; no pharmacological treatment was given (i.e., placebo only) to a comparison group; and either nonhypertensive patients or nondiabetic patients were included (or did not have the measurements attributed only to hypertensive diabetics) in the study.
Our predetermined outcomes of interest were all-cause death, cardiovascular death, incidence of cardiovascular disease, and incidence of renal dysfunction. Cardiovascular disease was defined as a composite of myocardial infarction, cerebrovascular events, congestive heart failure, angina pectoris, coronary revascularization, arrhythmia (ventricular tachycardia, ventricular fibrillation, and atrial fibrillation), dissecting aortic aneurysm, peripheral artery disease, and sudden cardiac death. Renal dysfunction was defined as a composite of a doubling of serum creatinine concentration and development of end-stage renal disease requiring regular dialysis or renal transplantation. Additionally, we planned to conduct stratified analyses by renal impairment at baseline, repeating the comparison between RAS inhibitors versus other classes of antihypertensives according to the presence or absence of either a reduced estimated glomerular filtration rate or proteinuria/albuminuria at baseline.
Data extraction and risk of bias assessment
The data including general study information (authors, titles, publication year, sample size, and study design), study population details (age, gender, mean systolic and diastolic BP levels at baseline and at the end of the trial as well as the follow-up duration), details on the intervention and comparison (the class of antihypertensive drug), and the outcome events were extracted.
Reviewers independently assessed the risk of the bias in each individual RCT by evaluating selection bias (randomization, concealment), performance bias (blinding), detection bias (blinding), and attrition bias (use of intention-to-treat analysis, incomplete outcome data) [18, 19].
Data synthesis and statistical analysis
In this analysis, tabular data were used because the individual patient data of each study were not available. Relative risk (RR) ratios and 95% confidence intervals (CIs) for each outcome of the individual studies were calculated before integration. We used a random effects model to obtain the summary estimates of RR ratios given that our included trials are likely heterogeneous because we set no restrictions for inclusion, except the language requirement. Statistical heterogeneity was determined with an I2 statistic. We used an inverse-variance method for the meta-analysis of each outcome. We examined publication bias using funnel plots of the natural log of the RR vs its standard error for each outcome. In addition to producing a quantitative summary estimate (i.e., RR and 95% CI) for an outcome, we also assessed the quality of evidence for each summary estimate by considering the risk of bias, inconsistency, imprecision, indirectness, and publication bias. Then, we rated the quality of the evidence as “high”, “moderate”, “low”, or “very low” [19]. Any disagreement in the rating among reviewers was adjudicated. A two-sided p value less than 0.05 was considered statistically significant. The data were analyzed with RevMan 5.3 (London, UK).
Results
Search results and characteristics of included trials
Through the literature search, we identified 1797 articles and reviewed 95 of them in full text. For qualitative synthesis, we included 16 RCTs (Fig. 1) [20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35].
Among the 16 RCTs, 8 trials were open-label RCTs [21, 26, 29,30,31,32, 34, 35] and the rest of the 8 trials were double-blinded RCTs [20, 22,23,24,25, 27, 28, 33]. Twelve trials compared RAS inhibitors with CCBs [21,22,23,24,25,26, 29, 31,32,33,34,35], four trials compared RAS inhibitors with beta-blockers [20, 26, 27, 30], and five trials compared RAS inhibitors with diuretics [26, 28, 30, 31, 33]. The mean duration of follow-up for each trial ranged from 1 to 9 years, but it was less than 5 years for most trials (Table 1). The risk of bias of the included trials varied substantially (Supplementary Table 2).
The mean baseline BP levels in the trials ranged between 137/76 and 196/97 (systolic/diastolic BP in mmHg). In most trials, no significant differences in achieved BP were found between RAS inhibitors and other classes of antihypertensive drugs during follow-up. However, in two trials, systolic BP during follow-up was significantly lower in individuals who were assigned diuretics [33] or CCB [32] compared to individuals who were assigned RAS inhibitors (Table 1).
Outcomes
All-cause death
Data on all-cause death (Figs. 2 and 3) were available from 12 trials that included 26,196 patients and 4106 events [20, 24,25,26,27,28,29,30, 32,33,34,35]. No significantly beneficial effect of RAS inhibitors for all causes of death was observed (RR 0.95, 95% CI 0.85–1.05, p = 0.29), and there was relatively weak evidence of heterogeneity in the magnitude of the effects across the included trials (I2 = 41%, p = 0.05). A funnel plot revealed no publication bias among the included trials. The quality of evidence for the summary estimate was rated as “moderate” (Table 2).
Effects of renin–angiotensin system inhibitors on a all-cause death, b cardiovascular death, c the incidence of cardiovascular disease, and d the incidence of renal dysfunction. Boxes and horizontal lines represent the relative risk ratios and 95% CI for each trial. Diamonds represent the 95% CI for pooled estimates of the effect and are centered on the pooled relative risk ratio. CCB, calcium-channel blocker; CI, confidence interval; conventional, conventional drugs; RAS, renin–angiotensin system
Funnel plots of the natural log of the relative risk ratio vs its standard error for a all-cause death, b cardiovascular death, c the incidence of cardiovascular disease, and d the incidence of renal dysfunction. The funnel plots revealed no publication bias among the included trials. RR, relative risk; SE, standard error
Cardiovascular death
Data on cardiovascular death were available from nine trials that included 7587 patients and 580 events [20, 22,23,24, 26, 27, 29, 30, 35]. No significantly beneficial effect of RAS inhibitors on cardiovascular death was observed (RR 0.84, 95% CI 0.68–1.04, p = 0.11), and there was weak evidence of heterogeneity in the magnitude of the effect across the included trials (I2 = 33%, p = 0.15). A funnel plot revealed there was no publication bias among the included trials. The quality of evidence for the summary estimate was rated as “moderate” (Table 2).
Incidence of cardiovascular disease
Data on the incidence of cardiovascular disease were available from 14 trials that included 27,778 patients and 4702 events [20,21,22, 24,25,26,27,28,29,30, 32,33,34,35]. No significantly beneficial effect of RAS inhibitors on the incidence of cardiovascular disease was observed (RR 0.93, 95% CI 0.84–1.03, p = 0.16). However, substantial heterogeneity in the magnitude of the effect across included trials was found (I2 = 59%, p = 0.002). We performed a subgroup analysis to explore the sources of heterogeneity by excluding apparently heterogeneous trials in the estimates one by one (ABCD [24], FACET [32], J-MIND [21], and NESTOR [28]). However, these exclusions did not alter the overall results of our summary estimate (Table 2). A funnel plot revealed there was no publication bias among the included trials. The quality of evidence for the summary estimate was rated as “moderate” (Table 2).
Incidence of renal dysfunction
Data on the incidence of renal dysfunction were available from six trials that included 19,671 patients and 590 events [20, 23, 25, 29, 31, 35]. No significantly beneficial effect of RAS inhibitors on the incidence of renal dysfunction was observed (RR 0.91, 95% CI 0.77–1.06, p = 0.22), and there was no evidence of heterogeneity in the magnitude of the effect across the included trials (I2 = 0%, p = 0.58). A funnel plot revealed there was no publication bias among the included trials. The quality of evidence for the summary estimate was rated as “high” (Table 2).
Outcomes in patients with or without renal dysfunction at baseline
We were unable to perform stratified analyses for the presence/absence of renal impairment, which was defined as either reduced estimated glomerular filtration rate or albuminuria/proteinuria, at baseline, because of the following reasons: (1) many trials excluded patients with serum creatinine concentrations ≥ 1.7 mg/dl at baseline and (2) many trials did not perform analyses that were stratified for renal impairment.
We performed subgroup analyses that excluded four trials that were rated as having a higher risk of bias (STOP-2 [26], J-MIND [21], JMIC-B [35], and CASE-J [29]) than other trials. The exclusions resulted in similar estimates to the main analyses (data not shown).
Discussion
In this meta-analysis of trials directly comparing RAS inhibitors and other drug class(es), we found that RAS inhibitors were no better than other classes of drugs as a first-line antihypertensive treatment for reducing all-cause death, cardiovascular death, the incidence of cardiovascular disease, and the incidence of renal dysfunction in hypertensive patients with diabetes. The summary point estimates of each outcome suggested that there was a reduced risk overall, but all the estimates were statistically nonsignificant. The results were consistent with recent meta-analyses [36, 37] and the recommendations from relevant major guidelines [6,7,8].
Apparent differences between our results and recommendation statements made by some guidelines are likely due, in part, to our strict inclusion criteria for trials (i.e., head-to-head comparison of RAS inhibitors vs other antihypertensives), and our predetermined outcomes included only clinically important adverse outcomes for hypertensive patients with diabetes [38]. For example, the 2014 guidelines by the Japanese Society of Hypertension [10] and 2016 guidelines by the Japanese Diabetes Society [11] recommended RAS inhibitors as a first-line treatment. However, these recommendations were not necessarily based on a systematic assessment of available trials that made a direct comparison between RAS inhibitors and other antihypertensive class(es) of drugs on the effects of death and cardiovascular events. Rather, the recommendation was largely based on the protective effect of RAS inhibitors over placebo from diabetic nephropathy. Another possible reason for the discrepancy is that we did not include the reduction of albuminuria/proteinuria as an outcome of our interest. It is noteworthy, however, that the 2014 Guidelines by the Japanese Society of Hypertension acknowledged the need for further studies to examine the purported superiority of ACEI over CCBs in preventing macrovascular complications in hypertensive patients with diabetes. Likewise, the 2016 Guidelines by the Japanese Diabetes Society stated that both ACEI and CCBs were shown to be effective in reducing macrovascular events. Putting all these conclusions together, our results are consistent with the detailed descriptions and understanding of the relevant literature from those guidelines. The results of our study imply that not only RAS inhibitors but also other classes of antihypertensive drugs that are proven to be effective in reducing important adverse outcomes in relevant patient groups should be recommended as a first-line antihypertensive treatment in diabetic patients as long as their blood pressure-lowering effects are equivalent. In cases in which a multidrug regimen is required to achieve a target BP, including an RAS inhibitor in that regimen may be reasonable given its protective effect against nephropathy [9, 37]. Such clinical judgments are endorsed by the recently updated guidelines by European Society of Cardiology and European Society of Hypertension 2018 [39].
For patients with diabetes and albuminuria, the guidelines and statements mentioned above recommend including an ACE inhibitor or ARB in the initial treatment with the primary reason being the risk reduction of kidney disease progression. The recommendations were based on a few trials in relevant patients [40]. Unfortunately, in our meta-analysis, we were unable to assess the question of whether this trend is also true with regard to reductions in total death and/or cardiovascular events, although we had initially planned to investigate the trend in the stratified analyses by the presence/absence of renal impairment at baseline. Nevertheless, even for this subgroup of patients (i.e., hypertensive patients with diabetic nephropathy), the supporting evidence for the superiority of RAS inhibitors in reducing total death and cardiovascular events remains relatively weak. The paucity of strong evidence is manifested in the 2017 American Hospital Association/American College of Cardiology Guidelines because they categorized their relevant recommendation as Class IIb (“weak”) [7]. Further studies are clearly needed to explore this question.
Study limitations
Several limitations of our study should be mentioned. First, most trials included in our meta-analysis compared RAS inhibitors with CCBs. Therefore, the results of this meta-analysis were mainly determined from comparisons of RAS inhibitors with CCBs rather than with β-blockers or diuretics. Second, many trials allowed multiple classes of blood pressure-lowering medication to achieve the target blood pressure when the effects of the assigned drugs (RAS inhibitors vs CCBs, β-blockers, and diuretics) were not enough. Therefore, differences in class-specific effects on outcomes may have been obscured. Third, the relatively short follow-up period of included trials (an average of < 5 years in most studies) may have prevented us from detecting a smaller but true difference between the effects of RAS inhibitors and other classes on the outcomes that would require a longer duration to emerge. Fourth, many trials included in this meta-analysis excluded patients with elevated serum creatinine at baseline. Fifth, we did not perform stratified analyses for the presence/absence of history of cardiovascular disease at baseline because many trials did not make this distinction. Thus, we could not discuss the primary and secondary prevention against each outcome separately. Finally, we have not assessed the potential harms associated with each treatment. We have to take these limitations into consideration when we generalize the results of this meta-analysis.
Conclusion
In this meta-analysis of head-to-head comparison RCTs, RAS inhibitors were not superior to other classes of antihypertensive drugs in reducing mortality, cardiovascular events, and renal events in hypertensive patients with diabetes. However, for diabetic patients with proteinuria, we were unable to conduct an assessment due to the lack of available data.
References
Espinola-Klein C, Weisser G, Jagodzinski A, Savvidis S, Warnholtz A, Ostad MA, et al. beta-Blockers in patients with intermittent claudication and arterial hypertension: results from the nebivolol or metoprolol in arterial occlusive disease trial. Hypertension. 2011;58:148–54.
Wijkman M, Lanne T, Engvall J, Lindstrom T, Ostgren CJ, Nystrom FH. Masked nocturnal hypertension--a novel marker of risk in type 2 diabetes. Diabetologia. 2009;52:1258–64.
American Diabetes Association. Role of cardiovascular risk factors in prevention and treatment of macrovascular disease in diabetes. Diabetes Care. 1989;12:573–9.
Adler AI, Stratton IM, Neil HA, Yudkin JS, Matthews DR, Cull CA, et al. Association of systolic blood pressure with macrovascular and microvascular complications of type 2 diabetes (UKPDS 36): prospective observational study. Br Med J (Clin Res Ed). 2000;321:412–9.
Emdin CA, Rahimi K, Neal B, Callender T, Perkovic V, Patel A. Blood pressure lowering in type 2 diabetes: a systematic review and meta-analysis. JAMA. 2015;313:603–15.
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Bohm M, et al. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34:2159–219.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr., Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2018;71:e127–e248.
American Diabetes Association. Standards of Medical Care in Diabetes-2018. Diabetes Care. 2018;41:S86–s104.
Schmieder RE, Hilgers KF, Schlaich MP, Schmidt BM. Renin-angiotensin system and cardiovascular risk. Lancet. 2007;369:1208–19.
The Japanese Society of Hypertension. The guidelines for the management of hypertension 2014: The Japanese society of hypertension. 2014.
Haneda M, Noda M, Origasa H, Noto H, Yabe D, Fujita Y, et al. Japanese Clinical Practice Guideline for Diabetes 2016. J Diabetes Investig. 2018;9:657–97.
Ogihara T, Nakao K, Fukui T, Fukiyama K, Ueshima K, Oba K, et al. Effects of candesartan compared with amlodipine in hypertensive patients with high cardiovascular risks: candesartan antihypertensive survival evaluation in Japan trial. Hypertension. 2008;51:393–8.
Julius S, Kjeldsen SE, Weber M, Brunner HR, Ekman S, Hansson L, et al. Outcomes in hypertensive patients at high cardiovascular risk treated with regimens based on valsartan or amlodipine: the VALUE randomised trial. Lancet. 2004;363:2022–31.
The EUCLID Study Group. Randomised placebo-controlled trial of lisinopril in normotensive patients with insulin-dependent diabetes and normoalbuminuria or microalbuminuria. Lancet. 1997;349:1787–92.
ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA. 2002;288:2981–97.
Iimura O, Shimamoto K, Matsuda K, Masuda A, Takizawa H, Higashiura K, et al. Effects of angiotensin receptor antagonist and angiotensin converting enzyme inhibitor on insulin sensitivity in fructose-fed hypertensive rats and essential hypertensives. Am J Hypertens. 1995;8:353–7.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. Br Med J (Clin Res Ed). 2009;339:b2700.
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. Br Med J (Clin Res Ed). 2011;343:d5928.
Fukui T, Yamaguchi N. Minds: The guide book to develop clinical practice guideline 2014. Igakushoin, Tokyo; 2014.
UK Prospective Diabetes Study Group. Efficacy of atenolol and captopril in reducing risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 39. Br Med J (Clin Res Ed). 1998;317:713–20.
Baba S. Nifedipine and enalapril equally reduce the progression of nephropathy in hypertensive type 2 diabetics. Diabetes Res Clin Pract. 2001;54:191–201.
Berl T, Hunsicker LG, Lewis JB, Pfeffer MA, Porush JG, Rouleau JL, et al. Cardiovascular outcomes in the Irbesartan Diabetic Nephropathy Trial of patients with type 2 diabetes and overt nephropathy. Ann Intern Med. 2003;138:542–9.
Chan JC, Ko GT, Leung DH, Cheung RC, Cheung MY, So WY, et al. Long-term effects of angiotensin-converting enzyme inhibition and metabolic control in hypertensive type 2 diabetic patients. Kidney Int. 2000;57:590–600.
Estacio RO, Jeffers BW, Hiatt WR, Biggerstaff SL, Gifford N, Schrier RW. The effect of nisoldipine as compared with enalapril on cardiovascular outcomes in patients with non-insulin-dependent diabetes and hypertension. N Engl J Med. 1998;338:645–52.
Lewis EJ, Hunsicker LG, Clarke WR, Berl T, Pohl MA, Lewis JB, et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med. 2001;345:851–60.
Lindholm LH, Hansson L, Ekbom T, Dahlof B, Lanke J, Linjer E, et al. Comparison of antihypertensive treatments in preventing cardiovascular events in elderly diabetic patients: results from the Swedish Trial in Old Patients with Hypertension-2. STOP Hypertension-2 Study Group. J Hypertens. 2000;18:1671–5.
Lindholm LH, Ibsen H, Dahlof B, Devereux RB, Beevers G, de Faire U, et al. Cardiovascular morbidity and mortality in patients with diabetes in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet. 2002;359:1004–10.
Marre M, Puig JG, Kokot F, Fernandez M, Jermendy G, Opie L, et al. Equivalence of indapamide SR and enalapril on microalbuminuria reduction in hypertensive patients with type 2 diabetes: the NESTOR Study. J Hypertens. 2004;22:1613–22.
Nakao K, Hirata M, Oba K, Yasuno S, Ueshima K, Fujimoto A, et al. Role of diabetes and obesity in outcomes of the candesartan antihypertensive survival evaluation in Japan (CASE-J) trial. Hypertens Res. 2010;33:600–6.
Niskanen L, Hedner T, Hansson L, Lanke J, Niklason A. Reduced cardiovascular morbidity and mortality in hypertensive diabetic patients on first-line therapy with an ACE inhibitor compared with a diuretic/beta-blocker-based treatment regimen: a subanalysis of the Captopril Prevention Project. Diabetes Care. 2001;24:2091–6.
Rahman M, Pressel S, Davis BR, Nwachuku C, Wright JT Jr, Whelton PK, et al. Renal outcomes in high-risk hypertensive patients treated with an angiotensin-converting enzyme inhibitor or a calcium channel blocker vs a diuretic: a report from the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). Arch Intern Med. 2005;165:936–46.
Tatti P, Pahor M, Byington RP, Di Mauro P, Guarisco R, Strollo G, et al. Outcome results of the Fosinopril Versus Amlodipine Cardiovascular Events Randomized Trial (FACET) in patients with hypertension and NIDDM. Diabetes Care. 1998;21:597–603.
Whelton PK, Barzilay J, Cushman WC, Davis BR, Iiamathi E, Kostis JB, et al. Clinical outcomes in antihypertensive treatment of type 2 diabetes, impaired fasting glucose concentration, and normoglycemia: Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). Arch Intern Med. 2005;165:1401–9.
Yamashita K, Kondo T, Muramatsu T, Matsushita K, Nagahiro T, Maeda K, et al. Effects of valsartan versus amlodipine in diabetic hypertensive patients with or without previous cardiovascular disease. Am J Cardiol. 2013;112:1750–6.
Yui Y, Sumiyoshi T, Kodama K, Hirayama A, Nonogi H, Kanmatsuse K, et al. Nifedipine retard was as effective as angiotensin converting enzyme inhibitors in preventing cardiac events in high-risk hypertensive patients with diabetes and coronary artery disease: the Japan Multicenter Investigation for Cardiovascular Diseases-B (JMIC-B) subgroup analysis. Hypertens Res. 2004;27:449–56.
Bangalore S, Fakheri R, Toklu B, Messerli FH. Diabetes mellitus as a compelling indication for use of renin angiotensin system blockers: systematic review and meta-analysis of randomized trials. Br Med J (Clin Res Ed). 2016;352:i438.
Palmer SC, Mavridis D, Navarese E, Craig JC, Tonelli M, Salanti G, et al. Comparative efficacy and safety of blood pressure-lowering agents in adults with diabetes and kidney disease: a network meta-analysis. Lancet. 2015;385:2047–56.
Gandhi GY, Murad MH, Fujiyoshi A, Mullan RJ, Flynn DN, Elamin MB, et al. Patient-important outcomes in registered diabetes trials. JAMA. 2008;299:2543–9.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Euro Heart J. 2018;39:3021–104.
Strippoli GF, Craig M, Deeks JJ, Schena FP, Craig JC. Effects of angiotensin converting enzyme inhibitors and angiotensin II receptor antagonists on mortality and renal outcomes in diabetic nephropathy: systematic review. Br Med J (Clin Res Ed). 2004;329:828.
Acknowledgements
We thank Professor Masahiro Yoshida for his valuable advice and support in conducting this systematic review and meta-analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Kunimura, A., Himuro, N., Fujiyoshi, A. et al. The effects of renin–angiotensin system inhibitors on mortality, cardiovascular events, and renal events in hypertensive patients with diabetes: a systematic review and meta-analysis of randomized controlled trials. Hypertens Res 42, 669–680 (2019). https://doi.org/10.1038/s41440-019-0234-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-019-0234-6
Keywords
This article is cited by
-
Hypertension in diabetes
Pediatric Nephrology (2023)
-
Rising serum potassium and creatinine concentrations after prescribing renin–angiotensin–aldosterone system blockade: how much should we worry?
World Journal of Pediatrics (2021)
-
The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019)
Hypertension Research (2019)