Abstract
Gitelman syndrome (GS) is caused by biallelic mutations in SLC12A3 as an autosomal recessive trait. A patient with a de novo 16q12.2q21 microdeletion showed clinical features of GS. SLC12A3 included in the deletion was analyzed, and a rare missense variant (c.1222A>C [p.N406H]) was identified as hemizygous. Consequently, GS was caused by the revealed SLC12A3 variant owing to chromosomal microdeletion.
Similar content being viewed by others
Gitelman syndrome (GS; MIM #263800) is a rare salt-losing tubulopathy characterized by hypokalemic metabolic alkalosis, renal magnesium wasting, and low urinary calcium excretion1. Patients with GS may be asymptomatic or have mild symptoms and most commonly manifest muscle weakness. Chronic growth retardation can also be observed. Thus, the age at diagnosis ranges from late childhood to young adulthood.
Biallelic mutations in the solute carrier family 12 (sodium/chloride transporters) member 3 gene (SLC12A3), which encodes the thiazide-sensitive NaCl cotransporter, are responsible for GS, indicating an autosomal recessive trait of this condition2. Because not all GS patients showed biallelic mutations3, mutations in the homologous alleles have never been proven in some cases, and nucleotide alterations in the noncoding regions and genomic copy number aberrations may be unidentified in such cases. Herein, we report a boy with GS caused by a hemiallelic missense mutation in SLC12A3, which was revealed by chromosomal deletion.
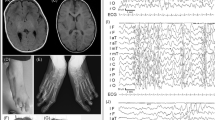
The male patient was born after 36 weeks of gestation by elective cesarean section. His birth weight and length were 2376 g (mean) and 44.5 cm (10–50th centile), respectively. His parents were healthy and nonconsanguineous. He was admitted to the neonatal intensive care unit and treated with thoracic drainage, medium-chain triglyceride milk, and somatostatin. Afterward, he showed developmental delay and seizure, and some minor anomalies, such as upslanting eyebrows, anteverted nares, and overlapping toes were noted. Chromosomal microarray testing identified a 16q12.2q21 microdeletion (Fig. 1a). The details of this patient have previously been reported4.
a The genome map around the chromosomal deletion identified in this patient (chr16:54,965,673_60,340,122) captured through UCSC genome browser (https://genome.ucsc.edu/). SLC12A3, indicated by blue and white inversion, is included in the deletion region. b Electropherograms of the Sanger sequence for the family. Whereas the mother can be diagnosed as a heterozygous carrier of the N406H variant, the patient shows only this variant.
At 8 years of age, his height was 108.9 cm (<3rd centile) and his weight was 16.2 kg (<3rd centile), indicating postnatal growth failure. Routine blood examination revealed hypokalemia with metabolic alkalosis but a normal level of serum magnesium (Table 1). Further examination revealed elevated levels of serum aldosterone (143 pg/mL) and plasma renin activity (16 ng/mL/h). The urinary calcium/creatinine clearance ratio was 0.03. These laboratory findings suggested the existence of tubulopathy in this patient5. Because SLC12A3, the gene related to GS, is included in the 16q12.2-q21 deletion and GS is an autosomal recessive disorder, we suspected the existence of the SLC12A3 mutation in the remaining allele.
After obtaining written informed consent, nucleotide sequences of all 26 exons and the flanking introns of SLC12A3 were analyzed using standard Sanger sequencing, and a missense variant, NM_000339.2(SLC12A3):c.1222A>C (p.N406H), was identified as hemizygous (the only minor allele was detected; Fig. 1b) in accordance with our hypothesis. This variant is included in the single nucleotide polymorphism database (dbSNPs: https://www.ncbi.nlm.nih.gov/snp/) with rs759532318.
To confirm parental origins, both parents were also analyzed, and c.1222A>C was identified only in his mother as heterozygous (Fig. 1b). Therefore, the c.1222A>C allele was inherited from this mother, and the 16q12.2q21 microdeletion was suspected to occur on the paternally derived allele as a de novo origin. As a result, the maternally derived c.1222A>C was revealed by paternally derived deletion.
The identified SLC12A3 variant (p.N406H) is rare, with a global frequency of 0.00009798 and classified as “uncertain significance” in the ClinVar database (https://www.ncbi.nlm.nih.gov/clinvar/). However, most of the prediction scores calculated through wANNOVAR (http://wannovar.wglab.org/) suggested “Damaging”, as shown in Supplementary Table S1. The p.N406H was revealed by a rare event of de novo microdeletion on the homologous allele, as shown by us previously in other clinical conditions6.
During the clinical course, serum magnesium levels of this patient often decreased slightly below the lower normal limit (Table 1), which is compatible with the findings in GS7,8. Furthermore, after molecular diagnosis, 10 mg potassium gluconate per day (2.5 mEq/kg/day as potassium) was prescribed, and the patient’s serum potassium level was corrected5. Then, his body weight gain increased after prescription of oral potassium supplementation from 16.2 kg (−11.3% in obesity degree) to 20.0 kg (−0.6%). For these reasons, we believe that the p.N406H variant identified in this study would be responsible for the clinical features of this patient, and the clinical diagnosis of GS was supported by this molecular diagnosis. According to the database of the National Center for Biotechnology Information (NCBI: https://www.ncbi.nlm.nih.gov/nuccore/NM_000339.2?report=graph), the affected codon 406 is a glycosylation site located in exon 10. Thus, the alteration of asparagine (N) to histidine (H) would prevent normal N-linked glycosylation.
The present patient shows neurological features, including developmental delay and epilepsy, which cannot be explained by GS but would be derived from haploinsufficiency of the genes included in the 16q12.2q21 microdeletion. Although the patient’s weight caught up, his height showed no remarkable improvement (from 108.9 cm [−3.09 SD] to 114.3 cm [−3.04 SD]) after 1 year of potassium supplementation. Thus, his short stature would be caused not only by GS but also by haploinsufficiency of the genes included in the 16q12.2-q21 region.
In conclusion, we presented a patient with GS who developed the disease owing to the monoallelic missense mutation in SLC12A3, which was revealed by complete deletion of another allele. Because the 16q12.2q21 microdeletion is of de novo origin, the recurrent risk of GS in this family can be ignored. This information would be beneficial for genetic counseling. Patients with 16q13 deletions should be closely monitored for the onset of GS.
HGV Database
The relevant data from this Data Report are hosted at the Human Genome Variation Database at https://doi.org/10.6084/m9.figshare.hgv.2853.
References
Nakhoul, F. et al. Gitelman’s syndrome: a pathophysiological and clinical update. Endocrine 41, 53–57 (2012).
Simon, D. B. et al. Gitelman’s variant of Bartter’s syndrome, inherited hypokalaemic alkalosis, is caused by mutations in the thiazide-sensitive Na-Cl cotransporter. Nat. Genet. 12, 24–30 (1996).
Vargas-Poussou, R. et al. Spectrum of mutations in Gitelman syndrome. J. Am. Soc. Nephrol. 22, 693–703 (2011).
Yamamoto, T., Shimojima, K., Yamazaki, S., Ikeno, K. & Tohyama, J. A 16q12.2q21 deletion identified in a patient with developmental delay, epilepsy, short stature, and distinctive features. Congenit. Anom. 56, 253–255 (2016).
Blanchard, A. et al. Gitelman syndrome: consensus and guidance from a Kidney Disease: Improving Global Outcomes (KDIGO) controversies conference. Kidney Int. 91, 24–33 (2017).
Shimada, S. et al. An unmasked mutation of EIF2B2 due to submicroscopic deletion of 14q24.3 in a patient with vanishing white matter disease. Am. J. Med. Genet. A 158A, 1771–1777 (2012).
Fulchiero, R. & Seo-Mayer, P. Bartter syndrome and Gitelman syndrome. Pediatr. Clin. N. Am. 66, 121–134 (2019).
Matsunoshita, N. et al. Differential diagnosis of Bartter syndrome, Gitelman syndrome, and pseudo-Bartter/Gitelman syndrome based on clinical characteristics. Genet. Med. 18, 180–188 (2016).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Abe, Y., Yamamoto, T., Izumita, Y. et al. Gitelman syndrome caused by a novel hemiallelic missense mutation in SLC12A3 revealed by 16q12.2q21 microdeletion. Hum Genome Var 7, 17 (2020). https://doi.org/10.1038/s41439-020-0104-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41439-020-0104-4