Abstract
Purpose
We estimated penetrance of actionable genetic variants and assessed near-term outcomes following return of results (RoR).
Methods
Participants (n = 2,535) with hypercholesterolemia and/or colon polyps underwent targeted sequencing of 68 genes and 14 single-nucleotide variants. Penetrance was estimated based on presence of relevant traits in the electronic health record (EHR). Outcomes occurring within 1-year of RoR were ascertained by EHR review. Analyses were stratified by tier 1 and non–tier 1 disorders.
Results
Actionable findings were present in 122 individuals and results were disclosed to 98. The average penetrance for tier 1 disorder variants (67%; n = 58 individuals) was higher than in non–tier 1 variants (46.5%; n = 58 individuals). After excluding 45 individuals (decedents, nonresponders, known genetic diagnoses, mosaicism), ≥1 outcomes were noted in 83% of 77 participants following RoR; 78% had a process outcome (referral to a specialist, new testing, surveillance initiated); 68% had an intermediate outcome (new test finding or diagnosis); 19% had a clinical outcome (therapy modified, risk reduction surgery). Risk reduction surgery occurred more often in participants with tier 1 than those with non–tier 1 variants.
Conclusion
Relevant phenotypic traits were observed in 57% whereas a clinical outcome occurred in 19% of participants with actionable genomic variants in the year following RoR.
Similar content being viewed by others
INTRODUCTION
Several genome sequencing projects are being conducted in diverse health-care and population settings including in the eMERGE network, the Implementing Genomics in Practice (IGNITE) network, Clinical Sequencing Evidence-Generating Research (CSER) consortium, and Geisinger Health System’s MyCode initiative. Additional large population scale projects such as the All of Us Research Program, which aims to sequence 1 million US participants; the UK Biobank project comprising 500,000 individuals; and the Genomics England project sequencing 100,000 genomes, plan to return results from genome sequencing. Several health systems in the United States and other countries1 have begun to integrate genomic sequencing data into patient care and disease prevention. However, knowledge gaps in two key areas need to be addressed to enable the appropriate implementation of genomic medicine.
First, estimates of penetrance of pathogenic/likely pathogenic (P/LP) variants identified by genome sequencing are needed.2 Initial reports suggest that P/LP variants in several genes may have low penetrance3,4 and the American College of Medical Genetics and Genomics (ACMG) has highlighted the need for more accurate estimates of penetrance obtained through genotype–phenotype correlation studies.2 Previous attempts to refine penetrance estimates have been limited in their size and scope5 and large population-based sequencing studies may contribute substantially to our understanding of the pathogenicity of rare genetic variants.6
Second, the effects of returning actionable genomic variants on health-related outcomes are largely unknown.7,8,9,10,11 Genome sequencing has potential applications in medical diagnosis, risk assessment, treatment, and prevention of both rare and common diseases.12 Currently there is limited evidence supporting clinical utility of genome sequencing to guide health service delivery and disease prevention in the general population.13 Few studies8,11 have examined the effect of genome sequencing on participant outcomes, including the influence of return of results (RoR) on testing and changes in therapy or intervention. Such information is necessary to develop an evidence base that will inform clinical practice recommendations, guidelines for reimbursement, and insurance coverage decisions.
The Return of Actionable Variants Empiric (RAVE) Study, conducted as part of phase III of the National Human Genome Research Institute (NHGRI) funded eMERGE network, aimed to begin to address these gaps in knowledge. The eMERGEseq panel comprised 68 medically relevant genes including the ACMG 56™ (ACMG™, ACMG SF™, ACMG 59™, ACMG 56™, and related words and designs incorporating ACMG™, are trademarks of the American College of Medical Genetics and Genomics and may not be used without permission)13 plus 12 genes selected by eMERGE investigators.14 The panel also included 14 single-nucleotide variants (SNVs) for which homozygosity for risk alleles was considered actionable. Our objectives were (1) to estimate penetrance of actionable variants by reviewing electronic health record (EHR) data for presence of relevant phenotypic traits and (2) assess near-term (1-year) outcomes after returning clinically actionable findings. Such data are needed to assess the broader medical impact of genome sequencing, including referral for additional medical evaluation, clinical management of genetic risk, and initiation of risk mitigation strategies.
MATERIALS AND METHODS
Study design
The design of the RAVE study, an eMERGE network genomic medicine implementation study, has been previously described.15 The study prospectively recruited individuals for targeted genomic sequencing. The genes included those associated with tier 1 conditions (defined by the CDC’s Office of Public Health Genomics as “those having significant potential for positive impact on public health based on available evidence-based guidelines and recommendations”), as well as genes with established clinical associations but less evidence on clinical utility (e.g., non–tier 1 genomic conditions).15,16 This report follows the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) reporting guideline.17
Setting
Participants were recruited from biobanks established at Mayo Clinic, Rochester Minnesota, primarily the Mayo Clinic Biobank and the Mayo Clinic Vascular Diseases Biorepository. The Mayo Clinic Biobank was established in 2009 and contains biological specimens, patient-provided health information, and EHR clinical data (see https://www.mayo.edu/research/centers-programs/mayo-clinic-biobank/for-researchers). RAVE study candidates were asked to complete a study consent form, health questionnaires, and provide a blood sample (if an existing sample was not available) to participate in this study. This study and the informed consent process were approved by the Mayo Institutional Review Board. Information about the Mayo Clinic Biobank’s collection and enrollment methods are described here.18 Data are deposited in dbGaP (accession code phs001616.v2.p2).
Participants
Participants (n = 2,535) were ascertained based on the presence of an elevated low-density lipoprotein (LDL) cholesterol (≥155 mg/dL) and/or at least one polyp on colonoscopy to undergo targeted sequencing of 68 genes and 14 SNVs using the eMERGEseq panel.14 DNA samples were sent to Baylor College of Medicine Human Genome Sequencing Center (BCM-HGSC), a CLIA-certified facility, for targeted sequencing. Additional details of sequencing methods and variant annotation have been previously described.14,15,19 The ACMG/AMP five-tier classification system was used to classify variants as pathogenic, likely pathogenic, uncertain significance, likely benign, and, benign.19 The BCM-HGSC Laboratory identified actionable variants, confirmed these by Sanger sequencing, and issued clinical reports that were reviewed by investigators at the Mayo Clinic prior to disclosure to participants and placement of results in the EHR. Variants of uncertain significance were not returned.
Return of results (RoR)
Participants with an actionable variant (a P/LP variant in any of the 68 genes, or actionable genotypes at any of the 14 SNVs) were contacted by postal mail informing them that a medically important result had been detected and advised that they attend an assigned study genetic counselor (GC) to review the finding.20 Participants who were unable to attend an in-person GC appointment had the option to receive results by telephone. Participants could opt-out from receiving their result consistent with ACMG guidelines.21 A detailed family history was obtained by the GC and a family pedigree chart (family tree) was constructed. Familial implications of the findings were discussed in all cases and information regarding family screening was provided to all participants. Following consultation with a GC, participants were referred to a specialist or to their primary care provider. In cases where a genetic diagnosis had been previously established and associated with appropriate follow up, no referral took place.
Data sources
The study sample consisted of 122 participants who had actionable genomic results (Fig. 1). Data including demographics, and prior diagnoses were abstracted from the Mayo Clinic EHR.22 Family history of the condition relevant to the actionable genomic result was ascertained from the detailed family pedigree drawn by the GC. A positive family history was defined as the presence of the relevant trait or condition in a first or second degree relative (Table 1 of the Supplement).
Outcomes were reviewed and categorized by tier 1 and non–tier 1 variants. For each participant with an actionable variant (list of actionable variants is in Table 2 of the Supplement), EHR data were abstracted separately by two of the three authors (C.L., L.A., F.F.). Any discrepancies in the abstraction were flagged and reviewed by a third author (O.E.) for resolution. Pre-RoR and post-RoR investigations were recorded as well as specialist evaluation.
Estimation of penetrance
Of 122 participants with actionable variants, we excluded 8 from the penetrance analyses (Fig. 1). A variant was considered penetrant if a relevant trait or diagnosis was noted on EHR review (these traits/diagnoses are listed in Table 3 of the Supplement). To estimate penetrance, a detailed review of the EHR including results of new tests ordered after RoR was performed by at least two of three authors (C.L., L.A., F.F.); any discrepancies were flagged and reviewed by a third author (O.E.). We considered P/LP variants in BRCA1/BRCA2 to be penetrant if the participant had undergone prophylactic bilateral mastectomy. Penetrance was compared between tier 1 and non–tier 1 variants.
Measurement of outcomes
Outcomes were ascertained by manual EHR review by at least two of three authors (C.L., L.A., F.F.); any discrepancies were flagged and reviewed by a third author (O.E.). Only outcomes clearly attributable to RoR based on EHR review were counted. For outcomes analyses we excluded participants who did not respond for result disclosure (n = 20) and those who had previously known of the results or had somatic mosaicism (n = 21). The latter group comprised 13 participants with returned tier 1 variants of whom 12 already knew their results and 1 participant with a large 13q deletion likely secondary to mosaicism, and 8 participants with returned non–tier 1 returned variants of whom 6 already knew their results and 2 with suspected mosaicism (Fig. 1). Outcomes in participants with a previously recognized variant prior to study RoR (n = 18) are presented in Table 4 of the Supplement. We classified outcomes based on a framework previously suggested by Williams23 and Peterson et al.24 as (1) process outcomes (referral to a specialist, new tests, initiation of surveillance); (2) intermediate outcomes (new diagnoses, positive findings on tests); and (3) clinical outcomes (modification of drug therapy, risk reducing surgery or procedure). The intermediate outcome “new diagnoses” includes any new diagnoses related to the returned results. This includes diagnoses such as “carrier of high-risk variant for hereditary breast and ovarian cancer (HBOC)” in addition to diagnoses that reflect the presence of a known related phenotype such as breast cancer. Process, intermediate, and clinical outcomes were compared between tier 1 and non–tier 1 conditions.
Bias
The diversity in the study cohort was limited; the majority of participants who had results returned were white (96.7%), with a high proportion having college (59%) or graduate (19%) education. The efficiency of a tertiary care center and the available resources may not be representative of other health-care settings.25 The average age of participants with returned variants was 62.5 years, possibly conferring a survivor bias. Ascertainment of the study cohort based on hypercholesterolemia and colon polyps may affect generalizability of this study to the population.
Study size
The maximal sample size was determined by the funding agency. Each eMERGE site could enroll up to 3,000 participants. This report is based on the 2,535 individuals enrolled at Rochester, Minnesota.
Quantitative variables/groupings
Outcomes were analyzed stratifying by tier 1 versus tier 2 conditions. Tier 1 conditions include familial hypercholesterolemia (LDLR, APOB, PCSK9), HBOC syndrome (BRCA1 and BRCA2), and Lynch syndrome (MLH1, MSH2, MSH6, PMS2).26
Statistical methods
Initial evaluations of the data included general inspection of the raw data, examination of outliers and group distributions, and evaluation of missing data. The ages of participants with tier 1 and non–tier 1 conditions were compared by t-test. The frequencies (%) of categorical factors were compared between tier 1 and non–tier 1 conditions using two-tail Fisher’s exact test.
RESULTS
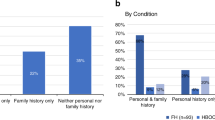
Of 2,535 participants, 122 (4.8%) had actionable results and 2% had actionable variants in genes related to tier 1 disorders.20 Table 2 of the Supplement lists each variant returned along with its pathogenicity classification and whether a relevant phenotype was present. Of 122 participants with actionable results, 20 did not respond to invitations for RoR, 2 opted out of receiving their results, and 2 died prior to RoR. Of the remaining participants, 18 had an existing diagnosis of the exact variant discovered as part of this study, as confirmed by EHR review (Fig. 1); 77 participants had results returned and outcomes were assessed at 1-year post-RoR. Actionable variants were categorized as related to either tier 1 or non–tier 1 conditions. Participant characteristics, overall and stratified by the presence of a tier 1 disorder, are summarized in Table 1. The median age of participants at the time of RoR was 63 years (IQR = 8 years, range 34–73) and 59.8% were female. Results were disclosed by a GC in person in 86 (70.4%) cases and by telephone in 12 cases (9.8%). Family history relevant to the actionable genomic result was present in 24 (31%) of 77 participants enrolled in the outcomes analysis; those with a variant related to a tier 1 condition were more likely to have a positive family history than those with a variant related to a non–tier 1 condition (44.4% vs. 19.5%, P = 0.026).
Penetrance
An estimate of penetrance for each actionable variant is presented in Table 2. On average, the penetrance was higher in tier 1 variants than non–tier 1 variants; 67.2% (n = 58 individuals) versus 46.5% (n = 58 individuals) (P = 0.03). Table 3 of the Supplement lists elements on EHR review that were used to determine whether a variant was penetrant. The penetrance of FH related variants was 92%; for HBOC related variants, the penetrance was 91% in females and 20% in males; and for Lynch syndrome variants, the penetrance was 20%. Penetrance varied in the three main subsets of non–tier 1 variants: 7.7% in cardiomyopathy variants versus 53.8% in arrhythmia variants and 75% in hemochromatosis variants. Cumulatively, 1 of 13 participants with cardiomyopathy variants and 7 of the 13 participants with long QT/Brugada syndrome variants (SCN5A, KCNQ1, KCNH2) manifested relevant traits. Relevant traits were present in 12 (4 male and 8 female) of the 16 participants (7 male and 9 female) homozygous for the c.845G>A variant in HFE that is associated with hemochromatosis. History of venous thromboembolism was present in one of four participants homozygous for the factor V Leiden variant.27
Outcomes
The occurrence of outcomes was stratified by tier 1 (FH, HBOC, and Lynch syndrome) versus non–tier 1 variants, as summarized in Table 3. Of 77 participants with newly identified P/LP variants or actionable SNVs as part of our study, 83% had one or more outcomes following RoR; 78% had a process outcome—referral to a specialist (65%), new testing (66%), surveillance initiation (39%); 68% had an intermediate outcome—new test finding (19.48%) or diagnosis (62.3%); 19.2% had a clinical outcome—risk reduction surgery (7.8%) or modification of therapy (11.7%). Risk reduction surgery occurred more often in participants with tier 1 than those with non–tier 1 actionable variants. Clinical outcomes in 18 participants with a previous genetic diagnosis are summarized in Table 4 of the Supplement.
Tier 1 conditions
Outcomes observed in participants who received tier 1 results are summarized in Table 4. Of 36 participants with newly identified P/LP tier 1 variants, 72% of participants had one or more outcomes following RoR; 72% had a process outcome—referral to a specialist (64%), new testing (66.7%), surveillance initiation (50%); 64% had an intermediate outcome—new test finding (16.7%) or diagnosis (58%); 25% had a clinical outcome—risk reduction surgery (16.7%) or modification of therapy (8.3%). Additional details are available in the Supplemental material (Table 4; Tables 5–7 and Figs. 1–3 of the Supplement).
Non–tier 1 conditions
Of 41 participants with newly identified non–tier 1 P/LP variants or actionable SNVs, 92.7% had one or more outcomes following RoR; 83% had a process outcome—referral to a specialist (65.8%), new testing (65.8%), surveillance initiation (29%); 71.4% had an intermediate outcome—new test finding (22%) or diagnosis (65.8%); 14.3% had a clinical outcome—risk reduction surgery (0%) or therapy modified (14.63%). Additional details are available in the Supplemental material (Table 4; Tables 8–10 and Figs. 4, 5 of the Supplement).
Comparison of outcomes in participants with tier 1 vs. non–tier 1 variants
Overall, outcomes occurred more frequently in those with non–tier 1 variants (92.7%) versus participants with tier 1 variants (72.2%) (Table 3). This was because participants with non–tier 1 variants tended to have higher occurrence of process and intermediate outcomes.
DISCUSSION
Essential elements of translational research to evaluate use of genome sequencing in primary care and population screening have been proposed,28 and there is an urgent need to develop this agenda, given the relatively sparse data for clinical validity and utility.11 In particular, data about penetrance of actionable variants and outcomes after their return are needed prior to adoption of genome sequencing in the clinical setting. In the present study, placing genome sequencing results in the EHR enabled subsequent assessment of penetrance and outcomes. The penetrance of actionable variants, on average was 67% for tier 1 variants and 46.5% for non–tier 1 variants. While the majority (78%) of the 77 participants who received a previously unknown actionable result, experienced a process outcome, 68% had intermediate outcomes, and 19% had clinical outcomes, motivating longer term follow up of larger cohorts to assess changes in health outcomes.
Penetrance
Estimates of penetrance of P/LP variants have not been fully defined4,29,30,31 and are needed to guide patients, family members, and clinicians on appropriate health management decisions. Linkage of genomic data to phenotypes in the EHR in the present study enabled us to ascertain traits/conditions relevant to an actionable variant that we used as a surrogate for penetrance. The penetrance of FH related P/LP variants was 92%, likely an inflated estimate resulting from selection of participants based on elevated cholesterol levels. Prior studies have reported penetrance of 70–90% for FH variants.32 For HBOC related variants, penetrance was 91% in females and 20% in males, similar to what has been previously reported (87% in females and 20% in males).33 The penetrance of Lynch syndrome variants was 20%, lower than prior reports of 50–60%.34,35 This may be due to the predominance of PMS2 variants (n = 9), which are associated with a substantially lower risk of cancer compared with the other variants associated with colorectal cancer.36 The penetrance of non–tier 1 variants was 46.5%, with variability in the three main subsets: 7.7% in cardiomyopathy variants versus 53.8% in arrhythmia variants and 75% in hemochromatosis variants.
For several reasons our estimates of penetrance should be considered preliminary. First, as mentioned above, penetrance estimates for FH variants could be inflated given the ascertainment of participants based on presence of elevated LDL cholesterol. Second, new evidence of “penetrance” could manifest with additional testing in the future and with longer follow up; however, the likelihood in this cohort is low, given the mean age of the participants at the time of testing (~63 years). Third, absence of clinical features that are associated with a P/LP variant may be due to truly reduced penetrance, absence of relevant phenotyping information (e.g., electrocardiogram [ECG] or echocardiograms), or an insufficient follow-up period.37 Fourth, survival bias may affect the estimates.
In 2013, the ACMG issued a statement recommending consideration of the return of actionable variants from 56 genes (ACMG 56™)13 sequenced in a clinical setting, to participants/patients. However, several of the P/LP variants in the genes on this list appear to have uncertain or low penetrance in asymptomatic individuals, prompting the ACMG to issue a recent statement discouraging the return of secondary findings detected as part of population screening.2 Further, the statement highlights the need for reliable estimates of penetrance obtained through robust genotype–phenotype correlation studies and research to establish the efficacy of interventions in asymptomatic patients with P/LP variants.2 Of note we did not find penetrance estimates to be different in P versus LP variants (55.2% vs. 60%, P = 0.69; analyses not shown).
Outcomes
For appropriate adoption of genomic medicine it is important to measure outcomes consequent to return of sequencing results.24 Clinical utility encompasses several domains.38 As a step toward assessing clinical utility after RoR in a targeted genomic medicine study, we ascertained near-term (1-year) outcomes (process, intermediate, and clinical) using a previously recommended framework.24 Most outcomes were process outcomes, but intermediate and clinical outcomes occurred in significant proportions (68% and 19%, respectively). When examining specific subsets of outcomes, risk reduction surgery occurred more often in participants with tier 1 than in those with non–tier 1 actionable variants (Table 3) but no significant differences were noted for the remaining subsets of outcomes.
The prevalence of actionable variants in the RAVE study was 4.8%, higher than previously reported,39 and the prevalence of tier 1 variants was 2%, twice what was expected in a population-based sample, likely due to enrichment for participants with hypercholesterolemia. Less than half of individuals with tier 1 variants had family history of the related disorder, indicating that population genomic screening would identify a substantial proportion of individuals at risk for coronary heart disease, HBOC, and colorectal cancer, who would not have had an indication for genomic testing. These findings are consistent with those of a UK Biobank study, in which ~60% of individuals with tier 1 variants did not have a relevant family history.40 Several participants in our study underwent potentially life-altering interventions. For example, after learning about having a pathogenic BRCA2 variant and a subsequent abnormal mammogram, a female participant opted for bilateral mastectomy and bilateral salpingo-oophorectomy.
It has been argued that genomic testing should focus on diseases with high penetrance, and options for prevention and/or treatment, and the net costs incurred are acceptable for the health gains achieved.41 Compared with those with tier 1 variants, participants with non–tier 1 variants tended to experience process outcomes more often, manifested the relevant trait/s in the EHR less often, and had a lower prevalence of family history of the relevant disease. These results motivate additional scrutiny of the costs and long-term outcomes following return of non–tier 1 secondary findings, to assess the balance between risk reduction versus increased health-care overutilization.11,42
Strengths of this study include selection of the participants based on the presence of hypercholesterolemia and/or colon polyps to emulate real world practice patterns where at-risk individuals are likely to undergo sequencing to screen for tier 1 disorders. Participants were recruited from a defined geographic area of southeast Minnesota, enabling nearly complete capture of outcomes one year after RoR since the majority of individuals residing in this area receive care at the Mayo Clinic in Rochester, Minnesota, or the Mayo Health System, and have associated follow up and referrals completed within this system.
Several limitations of the present study should be noted. Our data are observational since randomized controlled trials to assess outcomes based on returning versus not returning results are challenging to conduct given the actionable nature of genetic findings. The number of participants with actionable results was relatively modest and a meta-analysis of multiple genomic sequencing studies will be necessary to create an evidence base to inform appropriate implementation of genomic sequencing in clinical and public health contexts.12,43 Our report is limited to near-term outcomes and further work is needed to assess costs and health-care utilization, sharing of genetic results with family members, psychosocial outcomes, and long-term changes in health outcomes.
Conclusion
We report penetrance and 1-year clinical outcomes of actionable variants identified by targeted sequencing as part of a genomic medicine implementation study. Penetrance, estimated based on presence of relevant traits in the EHR, was 57% on average; process outcomes were noted in the majority (78%), whereas intermediate and clinical outcomes occurred in 68% and 19% of participants, respectively. Both penetrance and outcomes differed based on tier 1 vs. non–tier status. Penetrance was higher in participants with tier 1 actionable variants (67% vs. 46.5%). Overall, outcomes occurred more frequently in those with non–tier 1 variants (92.7% vs. 72.2%) whereas risk reduction surgery occurred more often in participants with tier 1 actionable variants (16.7% vs. 0%). Our study provides estimates of penetrance of actionable genomic variants identified by targeted sequencing and adds to the growing body of literature reporting outcomes following return of such variants to patients and clinicians. Additional studies of larger cohorts followed over a longer period are necessary to assess changes in health outcomes.
Data availability
Data is deposited in dbGaP (accession code phs001616.v2.p2) at website https://www.ncbi.nlm.nih.gov/projects/gap/cgi-bin/study.cgi?study_id=phs001616.v2.p2.
References
Feero, W. G., Wicklund, C. A. & Veenstra, D. Precision medicine, genome sequencing, and improved population health. JAMA. 319, 1979–1980 (2018).
ACMG Board of Directors. The use of ACMG secondary findings recommendations for general population screening: a policy statement of the American College of Medical Genetics and Genomics (ACMG). Genet. Med. 21, 1467–1468 (2019).
Hosseini, S. M. et al. Reappraisal of reported genes for sudden arrhythmic death: Evidence-based evaluation of gene validity for Brugada syndrome. Circulation. 138, 1195–1205 (2018).
Natarajan, P. et al. Aggregate penetrance of genomic variants for actionable disorders in European and African Americans. Sci. Transl. Med. 8, 364ra151 (2016).
Shah, N. et al. Identification of misclassified ClinVar variants via disease population prevalence. Am. J. Hum. Genet. 102, 609–619 (2018).
Wright, C. F. et al. Assessing the pathogenicity, penetrance, and expressivity of putative disease-causing variants in a population setting. Am. J. Hum. Genet. 104, 275–286 (2019).
Khoury, M. J. No shortcuts on the long road to evidence-based genomic medicine. JAMA. 318, 27–28 (2017).
Jones, L. K. et al. Healthcare utilization and patients’ perspectives after receiving a positive genetic test for familial hypercholesterolemia. Circ. Genom. Precis. Med. 11, e002146 (2018).
Buchanan, A. H. et al. Clinical outcomes of a genomic screening program for actionable genetic conditions. Genet. Med. 22, 1874–1882 (2020).
Williams, J. L. et al. Harmonizing outcomes for genomic medicine: comparison of eMERGE outcomes to ClinGen outcome/intervention pairs. Healthcare (Basel). 6, 83 (2018).
Hart, M. R. et al. Secondary findings from clinical genomic sequencing: prevalence, patient perspectives, family history assessment, and health-care costs from a multisite study. Genet. Med. 21, 1100–1110 (2019).
Vassy, J. L. et al. The impact of whole-genome sequencing on the primary care and outcomes of healthy adult patients: a pilot randomized trial. Ann. Intern. Med. 167, 159–169 (2017).
Kalia, S. S. et al. Recommendations for reporting of secondary findings in clinical exome and genome sequencing, 2016 update (ACMG SF v2.0): a policy statement of the American College of Medical Genetics and Genomics. Genet. Med. 19, 249–255 (2017).
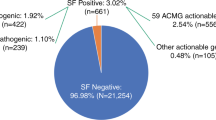
eMERGE Clinical Annotation Working Group. Frequency of genomic secondary findings among 21,915 eMERGE network participants. Genet. Med. 22, 1470–1477 (2020).
Kullo, I. J. et al. The Return of Actionable Variants Empirical (RAVE) study, a Mayo Clinic genomic medicine implementation study: design and initial results. Mayo Clin Proc 93, 1600–1610 (2018).
Dotson, W. D. et al. Prioritizing genomic applications for action by level of evidence: a horizon-scanning method. Clin. Pharmacol. Ther. 95, 394–402 (2014).
von Elm, E. et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 370, 1453–1457 (2007).
Olson, J. E. et al. The Mayo Clinic Biobank: a building block for individualized medicine. Mayo Clin. Proc. 88, 952–962 (2013).
Richards, S. et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet. Med. 17, 405–424 (2015).
Kochan, D. C. et al. Challenges in returning results in a genomic medicine implementation study: the Return of Actionable Variants Empirical (RAVE) study. NPJ Genomic Med. 5, 19 (2020).
ACMG Board of Directors. ACMG policy statement: updated recommendations regarding analysis and reporting of secondary findings in clinical genome-scale sequencing. Genet. Med. 17, 68–69 (2015).
Harris, P. A. et al. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inform. 42, 377–381 (2009).
Williams, M. S. Early lessons from the implementation of genomic medicine programs. Annu. Rev. Genomics Hum. Genet. 20, 389–411 (2019).
Peterson, J. F. et al. Building evidence and measuring clinical outcomes for genomic medicine. Lancet. 394, 604–610 (2019).
Shaibi, G. Q. et al. Returning genomic results in a federally qualified health center: the intersection of precision medicine and social determinants of health. Genet. Med. 22, 1552–1559 (2020).
US Centers for Disease Control and Prevention. Tier 1 genomics applications and their importance to public health. https://www.cdc.gov/genomics/implementation/toolkit/tier1.htm (2019).
Gallego, C. J. et al. Penetrance of hemochromatosis in HFE genotypes resulting in p.Cys282Tyr and p.[Cys282Tyr];[His63Asp] in the eMERGE Network. Am. J. Hum. Genet. 97, 512–520 (2015).
Khoury, M. J. et al. Correction: A collaborative translational research framework for evaluating and implementing the appropriate use of human genome sequencing to improve health. PLoS Med. 15, e1002650 (2018).
Manickam, K. et al. Exome sequencing-based screening for BRCA1/2 expected pathogenic variants among adult biobank participants. JAMA Netw. Open. 1, e182140 (2018).
Johnston, J. J. et al. Individualized iterative phenotyping for genome-wide analysis of loss-of-function mutations. Am. J. Hum. Genet. 96, 913–925 (2015).
Haer-Wigman, L. et al. 1 in 38 individuals at risk of a dominant medically actionable disease. Eur. J. Hum. Genet. 27, 325–330 (2019).
Youngblom, E. et al. in GeneReviews. (eds Adam, M. P., Ardinger, H. H., Pagon, R. A., et al.) Familial hypercholesterolemia (University of Washington, Seattle, 2016).
Petrucelli, N., Daly, M. B. & Pal, T. in GeneReviews (eds Adam, M. P., Ardinger, H. H., Pagon, R. A., et al.) BRCA1- and BRCA2-associated hereditary breast and ovarian cancer (University of Washington, Seattle, 2016).
Kohlmann, W. & Gruber, S. B. in GeneReviews (eds Adam, M. P., Ardinger, H. H., Pagon, R. A., et al.) Lynch syndrome (University of Washington, Seattle, 2018).
Møller, P. et al. Cancer incidence and survival in Lynch syndrome patients receiving colonoscopic and gynaecological surveillance: first report from the prospective Lynch syndrome database. Gut. 66, 464–472 (2017).
Senter, L. et al. The clinical phenotype of Lynch syndrome due to germ-line PMS2 mutations. Gastroenterology. 135, 419–428 (2008).
Van Driest, S. L. et al. Association of arrhythmia-related genetic variants with phenotypes documented in electronic medical records. JAMA. 315, 47–57 (2016).
Grosse, S. D. & Khoury, M. J. What is the clinical utility of genetic testing? Genet. Med. 8, 448–450 (2006).
Dorschner, M. O. et al. Actionable, pathogenic incidental findings in 1,000 participants’ exomes. Am. J. Hum. Genet. 93, 631–640 (2013).
Patel, A. P. et al. Association of rare pathogenic DNA variants for familial hypercholesterolemia, Hereditary breast and ovarian cancer syndrome, and Lynch syndrome with disease risk in adults according to family history. JAMA Netw. Open. 3, e203959 (2020).
Doble, B., Schofield, D. J., Roscioli, T. & Mattick, J. S. Prioritising the application of genomic medicine. NPJ Genomic Med. 2, 35 (2017).
Zhang, L. et al. Population genomic screening of all young adults in a health-care system: a cost-effectiveness analysis. Genet. Med. 21, 1958–1968 (2019).
McMurry, A. J. et al. SHRINE: enabling nationally scalable multi-site disease studies. PLoS One. 8, e55811 (2013).
Acknowledgements
The RAVE study was funded as part of the NHGRI-supported eMERGE (Electronic Records and Genomics) Network (U01HG006379) and by the Mayo Center for Individualized Medicine. I.J.K. was additionally funded by K24 HL137010.
Author information
Authors and Affiliations
Contributions
Conceptualization: I.J.K., R.S., N.L. Data curation: D.K., O.E., C.L. Formal analysis: O.E. Funding acquisition: I.J.K. Investigation: O.E., C.L., F.F., L.A. Resources: I.J.K. Supervision; I.J.K. Visualization: O.E. Writing—original draft: I.J.K., O.E., C.L. Writing—review & editing: I.J.K., O.E., C.L.
Corresponding author
Ethics declarations
Ethics Declaration
RAVE study candidates were asked to complete a study consent form and health questionnaires, and provide a blood sample (if an existing sample was not available) to participate in this study. This study and the informed consent process were approved by the Mayo Institutional Review Board. Information about the Mayo Clinic Biobank’s collection and enrollment methods are described here: https://pubmed.ncbi.nlm.nih.gov/24001487/.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
About this article
Cite this article
Lee, C., Elsekaily, O., Kochan, D.C. et al. Penetrance and outcomes at 1-year following return of actionable variants identified by genome sequencing. Genet Med 23, 1192–1201 (2021). https://doi.org/10.1038/s41436-021-01142-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41436-021-01142-9