Abstract
Purpose
Newborn screening (NBS) for Krabbe disease (KD) is performed by measurement of galactocerebrosidase (GALC) activity as the primary test. This revealed that GALC activity has poor specificity for KD. Psychosine (PSY) was proposed as a disease marker useful to reduce the false positive rate for NBS and for disease monitoring. We report a highly sensitive PSY assay that allows identification of KD patients with minimal PSY elevations.
Methods
PSY was extracted from dried blood spots or erythrocytes with methanol containing d5-PSY as internal standard, and measured by liquid chromatography–tandem mass spectrometry.
Results
Analysis of PSY in samples from controls (N = 209), GALC pseudodeficiency carriers (N = 55), GALC pathogenic variant carriers (N = 27), patients with infantile KD (N = 26), and patients with late-onset KD (N = 11) allowed for the development of an effective laboratory screening and diagnostic algorithm. Additional longitudinal measurements were used to track therapeutic efficacy of hematopoietic stem cell transplantion (HSCT).
Conclusion
This study supports PSY quantitation as a critical component of NBS for KD. It helps to differentiate infantile from later onset KD variants, as well as from GALC variant and pseudodeficiency carriers. Additionally, this study provides further data that PSY measurement can be useful to monitor KD progression before and after treatment.
Similar content being viewed by others

INTRODUCTION
Krabbe disease (KD; globoid cell leukodystrophy; OMIM 245200), is an autosomal recessive lysosomal storage disorder caused by variants in the GALC gene that encodes lysosomal galactocerebrosidase (EC 3.2.1.46). KD has a variable neurodegenerative phenotype broadly categorized as infantile (IKD) and late-onset KD (LOKD). IKD usually presents in the first 3–6 months of life beginning with extreme irritability, episodic fever, hypertonia of limbs, and hypersensitivity to external stimuli. Progression is rapid, with a plateau of motor and cognitive development followed by regression and death in early childhood. Later onset variants of KD generally present with developmental regression, spastic paraplegia, ataxia, wide gait, and visual loss.1,2 Some atypical cases have been reported where initial symptoms have not been observed until the third decade of life or later, which poses a diagnostic challenge.3,4 Disease presentation at less than 1 year of age generally correlates with a more severe, rapid disease course than later presentation.2 In this study, we consider as affected with LOKD those patients who presented clinically or would be considered likely to present clinically after 1 year of age. No consistent correlation has been established between genotype and disease severity, except for a deletion of GALC exons 11–17.3,5 Furthermore, analysis of residual GALC activity in white blood cells (WBCs) using nominally sensitive assays has not correlated better with phenotype than GALC activity measurement in dried blood spots (DBS) as used for screening.6
Treatment of KD has historically been palliative. Hematopoietic stem cell transplantion (HSCT) is currently the only treatment shown to slow progression of neurological sequelae, but to achieve best outcomes HSCT needs to occur before onset of symptoms, for patients with IKD prior to 30 days old.7,8,9 To achieve early identification and treatment of KD, in 2006, newborn screening (NBS) for KD was implemented in the state of New York by analysis of GALC enzyme activity followed by molecular analysis of the GALC gene as a 2nd tier test when GALC activity was reduced. Results of the first 2 million newborns screened in New York revealed a lower than expected incidence of KD (approximately 1:400,000 births). Of 346 cases referred for follow up, only 5, 2 of whom were biological siblings, were predicted by reduced GALC activity and genotype to be affected with IKD, which was confirmed by follow-up investigations.6 The reason for this screening performance was a high rate of previously uncharacterized variants and genotypes that lead to biochemical pseudodeficiency of GALC activity. Despite critical and discouraging review of the performance of this screening approach10,11,12 several other states began NBS for KD, specifically Illinois, Kentucky, Missouri, New Jersey, Tennessee, and Ohio.
Attempts have been made to improve upon the New York experience by including other lysosomal enzymes in the screening assay to allow for additional bioinformatics analysis and help exclude false positive cases where numerous enzyme activities are artifactually reduced, and exploring the use of psychosine (PSY, galactosylsphingosine), one of three substrates of GALC, as a biomarker indicative of KD.13,14,15,16,17 PSY serves as an indicator of disease status and the longstanding “psychosine hypothesis” was recently confirmed by ablation of acid ceramidase in twitcher mice, which eliminated PSY accumulation and effectively cured KD in these animals.18 However, the exact role of psychosine in Krabbe disease pathogenesis remains uncertain, but is likely multifactorial.19,20,21,22,23
PSY is a biomarker that can identify patients with IKD and likely also with LOKD. In addition, it may have utility in monitoring patients to determine when HSCT should be initiated and to monitor the efficacy of HSCT.15,24 The Kentucky NBS program employs PSY measurement as a 2nd tier test, and this has resulted in an absence of false positive cases to date and led to the rapid identification and initiation of HSCT in one infant with IKD and a GALC genotype that includes a variant of uncertain significance.14,15 The observation of subtle elevations of PSY in some LOKD patients has necessitated optimization of the current PSY assay15 to achieve higher sensitivity and also led to the investigation of additional specimen types for PSY analysis, specifically red blood cells (RBC). A new GALC enzyme activity assay in white blood cells (WBCs)25 was also adapted to further enhance the ability to differentiate not only KD from pseudodeficiency states, but also IKD from LOKD variants.
MATERIALS AND METHODS
Samples
Dried blood spots (N = 209) and whole-blood samples (N = 153) that were submitted for unrelated testing were used after de-identification for method validation and generation of reference ranges for PSY. Samples from confirmed patients with IKD (DBS: N = 26; RBC: N = 5), suspected LOKD (DBS: N = 11; RBC: N = 4), GALC pseudodeficiency (DBS: N = 55), and GALC pathogenic variant carriers also harboring pseudodeficiency alleles (DBS: N = 27; RBC: N = 2) were used to establish condition-specific PSY concentration ranges. The DBS included nine original newborn screening specimens obtained in accordance with the relevant state’s specimen release requirements. Leftover, de-identified WBC samples from 130 unaffected individuals were used to establish reference ranges for GALC activity. Condition-specific GALC activity ranges were determined using WBCs from 11 patients with IKD, 7 patients with LOKD, 5 individuals with genotype confirmed GALC pseudodeficiency, and 14 carriers of a pathogenic GALC variant. This study was approved by the Mayo Clinic Institutional Review Board (#14–009619 and #15–005393). Data was retrospectively abstracted from health records, and prospectively collected specimens were obtained with informed consent.
Materials
Psychosine (galactosyl β sphingosine) and d5-psychosine were purchased from Avanti Polar Lipids, EDTA and ammonium acetate from Sigma-Aldrich, acetonitrile and acetone from Fisher Scientific, isopropanol from VWR, and glacial acetic acid from Mallinckrodt.
Preparation of DBS calibrators and controls
Dried blood spots for calibration, recovery, stability, and imprecision studies were prepared as follows: aliquots of pooled whole EDTA blood adjusted to a hematocrit of 0.5 were spiked to achieve PSY concentrations of 0, 1, 5, 10, 25, 50, 100, and 200 nM, then spotted on filter paper (Whatman ProteinSaver 903) and dried at room temperature for a minimum of 3 hours. The spotted cards were then transferred to a zip-lock bag with desiccator and stored at −20 °C.
Preparation of RBC lysate and calibrators
Packed RBCs were washed twice with equal volumes 0.9% saline and then frozen at −70 °C overnight. The lysed cells were then diluted with water to generate RBC lysate with a hemoglobin concentration between 5 and 15 g/L. RBC lysate was spiked to PSY concentrations of 0, 0.5, 1, 2, 5, and 10 nM and stored at −20 °C to be used for assay calibration and quality control.
DBS sample preparation
A 3.2-mm DBS disc was placed in a 96-well filter plate (AcroPrep Advance 96 Filter Plate, 0.45 µm GHP, PALL #8084). Methanol (250 µL) containing d5-PSY (0.25 nM) as internal standard was added and PSY extracted over 30 minutes by rotation at ambient conditions with a plastic cover in place. The extract was then collected by centrifugation (829g, 5 minutes) into a receiving plate, dried under nitrogen gas, and then reconstituted with 50:50 methanol:acetonitrile (250 µL).
RBC sample preparation
In a microcentrifuge tube, 0.1% formic acid in water (100 µL), methanol containing 6.25 nM d5-PSY (10 µL) and RBC lysate (50 µL) were combined. A graphite spin column (Thermo Scientific Pierce #PI-88302) was conditioned by adding 1 M ammonium hydroxide (100 µL) twice, acetonitrile (100 µL) once, and 0.1% formic acid in water (100 µL) twice with centrifugation (1000g, 1 minute) following each addition. The sample solution was applied to the conditioned graphite spin column that was vortexed to bind PSY and d5-PSY to the graphite medium. The medium was then washed with 0.1% formic acid in water (100 µL) twice and with 0.1% formic acid in water:acetonitrile 90:10 (100 µL) once with centrifugation (1000g, 1 minute) following each addition to remove signal suppressing interferences. Graphite bound PSY and d5-PSY were eluted in two 100 µL fractions with 0.1% formic acid in 25:75 water:acetonitrile. The combined eluents were dried under nitrogen gas and then reconstituted with 50 µL of 50:50 methanol:acetonitrile.
Liquid chromatography–tandem mass spectrometry (LC-MS/MS) procedure
Prepared sample (8 µL) was injected into a 5-µL sample loop using an AB Sciex M3 micro flow LC system coupled to a SCIEX API 5500 tandem mass spectrometer. PSY was chromatographically separated from glucosylsphingosine by gradient elution using a 1 × 50 mm, 1.7-µm Acquity UPLC BEH HILIC column (Waters #186003457) at 45 °C. Mobile phase A (acetonitrile, 0.5% acetic acid) and mobile phase B (90% isopropanol, 10% water, 0.5% acetic acid, 25 mM ammonium acetate) were delivered with a total flow of 175 µL/min using the following program: 70% B for 0.5 minutes, ramp to 95% B for 3 minutes, return to 70% B and hold for 1 minute. The MS was operated in positive electrospray ionization mode to monitor multiple reaction monitoring (MRM) transitions for PSY (quantifier m/z 462.3 to m/z 282.4, qualifier m/z 462.3 to m/z 264.4) and d5-PSY (quantifier m/z 467.3 to m/z 287.4, qualifier m/z 467.3 to m/z 269.4). Run time was 4.5 minutes per sample (Supplemental Fig. 1).
GALC enzyme activity assay
White blood cells were isolated from ACD or EDTA whole blood using dextran. After sonication in an ice water bath, the protein concentration was determined using the BioRad DC protein assay and the lysates were diluted to a concentration of 0.2–0.8 g/L protein. GALC activity in the WBC lysate was measured using LC-MS/MS as recently described.25
RESULTS
Linearity and Imprecision of PSY analysis
Eight DBS calibrators (0, 1, 5, 10, 25, 50, 100, and 200 nM of added PSY) were prepared and analyzed across three batches. Linear regression using 1/x weighting yielded consistent and linear responses (r ≥ 0.99). For RBCs, six calibrators (0, 0.5, 1, 2, 5, and 10 nM of added PSY) were prepared and analyzed across three batches, which also yielded consistent and linear responses (r ≥ 0.99). Intra-assay and interassay imprecision studies were performed in DBS and RBC lysate at three levels yielding acceptable results (Supplemental Table 1).
PSY in DBS method comparison
The method was compared with the previously published assay15 using 47 DBS specimens (Supplemental Fig. 2). Linear regression applied to a bivariate analysis of these data yielded moderate discordance (r2 = 0.9722, m = 1.02, b = −1.39) because the new assay has the desired higher sensitivity at low PSY concentrations.
Recovery
Recovery was evaluated by analysis of DBS spiked with PSY concentrations of 7.5 and 15 nM with recoveries of 89% and 91%, respectively. PSY recovery in three sets of RBC lysates was assessed at 1 and 5 nM, which yielded recoveries ranging from 85% to 111%.
Limit of detection
The limit of detection was defined as the concentration at which a signal-to-noise ratio of 3:1 is reached. The limits of detection for DBS and RBC lysate were 1.5 and 0.06 nM respectively.
Interference studies
Glucosylsphingosine is structurally similar to PSY and is the only structural isomer likely to interfere with the measurement of PSY unless separation is achieved by liquid chromatography as in this assay. Differences in measured PSY before and after addition of glucosylsphingosine to DBS extracts (50 nM added) and RBC lysates (2.5 nM added) were −9% for DBS and −3% for RBC lysate samples documenting an interference-free analysis of PSY. Representative chromatograms for control, IKD, and LOKD cases acquired in DBS and RBC lysate are shown in Supplemental Fig. 1.
PSY reference ranges in DBS and RBC
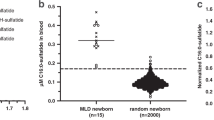
Reference ranges were determined by the analysis of PSY in leftover DBS and RBC specimens from 209 and 153 unaffected individuals, respectively. Specimens from patients with IKD (DBS: N = 26; RBC: N = 5; Table 1), suspected LOKD (DBS: N = 11; RBC: N = 4; Table 1), GALC pseudodeficiency (DBS: N = 55), and GALC pathogenic variant carrier (DBS: N = 27; RBC: N = 2) cases were used to establish condition-specific PSY concentration ranges (Fig. 1a, b). The groups composed of individuals with GALC pseudodeficiency and GALC variant carriers had DBS and RBC PSY concentrations within the normal control range. In contrast the PSY concentration in DBS and RBCs from IKD and LOKD patients were elevated.
Quantitation of psychosine (PSY) in dried blood spots (DBS) (a) and red blood cell (RBC) lysate (b) and galactocerebrosidase (GALC) enzyme activity assayed in white blood cell (WBC) lysate (c) of controls, individuals with GALC pseudodeficiency, and GALC variant carrier status, as well as patients with late-onset Krabbe disease (LOKD) and infantile Krabbe disease (IKD). Box and whisker plots display the 99%, 90%, 50%, 10%, and 1% percentiles, respectively. Green bars represent the 1st to 99th percentile of controls for each sample type. Control DBS (N = 209) include data from 110 unaffected neonates (1–2 days old), 56 pediatric (9 days to 17 years; mean: 6.5 years; median: 3.4 years) and 43 adult individuals (18–81 years; mean: 48.5 years; median: 51.2 years). Control RBC (N = 153) include data from 76 pediatric (4 days to 17 years; mean: 1.2 years; median: 21 days) and 77 adult individuals (18–90 years; mean: 50.9 years; median: 50.8 years). Control WBC (N = 130) comprise data from 26 pediatric (7 months to 17 years; mean: 4.8 years; median: 2.6 years) and 104 adult individuals (18–78 years; mean: 43.5 years; median: 38.3 years).
Galactocerebrosidase enzyme activity in leukocytes
GALC activity was measured in WBCs25 and reference ranges were determined by analysis of leftover clinical samples from 130 unaffected individuals. WBC GALC pseudodeficiency cases (N = 5), pathogenic GALC variant carriers (N = 14), IKD patients (N = 11; Table 1), and LOKD patients (N = 7; Table 1) were also analyzed. The GALC activity of individuals with GALC pseudodeficiency and GALC mutant carriers was decreased when compared with normal controls (Fig. 1c). However, activity was lower in the IKD and LOKD cohorts than either the pseudodeficiency or pathogenic GALC variant carrier cohorts.
Patients
Biochemical, clinical, and/or genotype data were available from 26 patients with evidence of IKD and 11 patients with evidence of LOKD (Table 1). Nine (35%) of the 26 IKD patients and 9 (82%) of 11 LOKD patients were identified by NBS. Results of WBC GALC activity and DBS PSY measurement from an IKD patient (Table 1, patient 4), an LOKD patient (Table 1, patient 27), and an individual with pseudodeficiency (genotype: homozygous p.I562T, heterozygous p.R184C) segregate with the expected ranges for their respective conditions (Fig. 2a–c).
Comparison of white blood cell (WBC) galactocerebrosidase (GALC) activity and dried blood spot (DBS) psychosine (PSY) in patients with infantile Krabbe disease (IKD) (a, patient 4 of Table 1), late-onset Krabbe disease (LOKD) (b, patient 27), pseudodeficient GALC activity (c), patient 35 (d), and patient 36 (e). Patient values are represented as black diamonds in each figure. Box and whisker plots display the 99%, 90%, 50%, 10%, and 1% percentiles, respectively. Green bars represent the 1st to 99th percentile of controls (see legend to Fig. 1). Patient 35 (d, Fig. 3b, Table 1) was identified by newborn screening (NBS) with low GALC activity and mildly elevated DBS PSY. GALC activity in WBCs was at the high end of values observed in LOKD patients, and PSY levels have alternated between mild elevations and normal values. This patient has symptoms that could be consistent with KD, including developmental delay and seizures. When patient 36 (e, Fig. 3b and Table 1) was first evaluated at 14 months old, DBS PSY was mildly elevated (3.1 nmol/L) in the range of LOKD patients, but WBC GALC activity was consistent with IKD. The original NBS specimen of this patient could be retrieved, was analyzed 15 months after collection, and the PSY concentration (1.2 nmol/L) was normal. This patient was born at 30 weeks gestation, and had developed normally until 14 months of age when, following a respiratory tract infection, the patient began to lose developmental and motor skills. Intravenous immunoglobulin treatment was initiated under the assumption of an inflammatory process and seemed to be of benefit. However, magnetic resonance image (MRI) showed signs of leukodystrophy (abnormal T2 and fluid-attenuated inversion recovery [FLAIR] hyperintensity within the frontoparietal white matter, hyperintensity of the globus pallidus, and hypointensity of the anterior thalamus). Subsequently, the clinical status began to deteriorate again and PSY in DBS increased to 8.9 nM by 18 months old at which time the diagnosis was considered to be LOKD.
Longitudinal PSY analysis in KD patients
Quantitation of PSY in DBS at multiple time points was possible for ten IKD and eight LOKD patients for the purpose of longitudinal monitoring (Fig. 3). Of these, six IKD patients had PSY measured before and after HSCT (Fig. 3c). The initial DBS collection for all patients occurred at or before the age of 11 days as a result of NBS. All initial PSY measurements were elevated (median = 58 nmol/L, range 10–94) compared with control values. Multiple pre-HSCT DBS samples were obtained in three cases, and several showed a trend of decreased PSY levels between the initial measurement and the HSCT procedure with further reductions in all cases after HSCT. Longitudinal PSY measurements were also possible in three LOKD patients detected by NBS who went on to receive HSCT (Fig. 3d). Patients 27 and 28, fraternal twin siblings with identical variants, had extensive neurodiagnostic monitoring that included consistent PSY measurements in the LOKD range with reduction of PSY to the control range after HSCT.
Longitudinal plots of psychosine (PSY) concentrations in dried blood spots (DBS) from untreated (a) and transplanted infantile Krabbe disease (IKD) (c) cases as well as untreated (b) and transplanted late-onset Krabbe disease (LOKD) (d) patients. X indicates age at hematopoietic stem cell transplantation (HSCT). Dots indicate other nontransplanted IKD and LOKD cases in respective graphs. Green bar represents the 1st to 99th percentile of controls (see legend to Fig. 1). NBS newborn screening.
DISCUSSION
Newborn screening for KD in New York has been complicated by the fact that measurement of GALC activity and GALC sequencing in DBS proved to be a poor prognostic indicator for KD unless genotypes involving known pathogenic variants were detected. Moreover, the WBC-based GALC activity assays available at the time were equally unable to reliably differentiate affected from unaffected infants. This led to a large number of false positive results, unnecessary clinical follow up of patients who screened positive due to carrier status of pathogenic GALC variants and pseudodeficiency alleles, and calls to abandon screening for KD.10,11,12 Nonetheless, KD screening has been adopted by additional states through patient advocacy efforts to enable maximum benefit from early HSCT as the only intervention currently available for KD patients.7,8,9 Therefore, an effective NBS program for KD requires rapid identification of patients with IKD without exposing unaffected newborns with GALC pseudodeficiency or GALC variant carrier status to lengthy, expensive, and ultimately unnecessary follow-up investigations. The previously demonstrated utility of PSY as a biomarker indicative of KD has already led to its implementation in some state NBS programs and our data reinforce that PSY can be used to accurately identify, at a minimum, IKD patients. However, while PSY analysis appears to be a better primary marker for KD, it cannot yet replace the GALC enzyme assay as the primary screening test because the analysis takes 4.5 minutes per sample and requires very sensitive equipment, which is currently cost prohibitive for population screening. To date, the processes applied by state programs to NBS for KD remain variable.26 An abnormal low GALC activity in an NBS sample can be followed by either (1) immediate clinical referral (Ohio), (2) molecular interrogation of the GALC gene only for the common 30-kb deletion (Missouri), (3) multivariate pattern recognition14 and full molecular analysis of the GALC gene (New York), (4) full molecular analysis of the GALC gene and PSY quantitation (Illinois, Tennessee), or (5) multivariate pattern recognition, PSY quantitation, and GALC analysis for the 30-kb deletion (Kentucky).14 To the best of our knowledge, programs relying primarily on PSY concentration as a 2nd tier test achieve the lowest false positive rates and fastest referral to KD specialists, enabling early treatment.14,26
In the current study, sequence information was available for 31 of the 37 patients. Only 3 (8.1%) were homozygous for the 30-kb deletion (Table 1), which is similar to the experience in New York where 3 (21.4%) of 14 infants classified as “high risk” proved to be homozygous for this deletion.6 Therefore, NBS programs relying on 30-kb deletion detection will often have insufficient information about the newborn’s disease status, which could cause delays in referral to specialty care centers. We recommend that PSY quantitation be used as a 2nd tier NBS test when GALC activity is reduced and to stratify the required response into one of three categories (Fig. 4):
- 1.
A normal level of psychosine does not require further biochemical or molecular investigation or additional sample collection from the patient.
- 2.
High PSY levels trigger immediate referral to specialty care centers where patients can be rapidly evaluated as presumptive IKD patients. Additional characterization including biochemical GALC enzyme activity in WBC, PSY in RBC, along with genotyping of the GALC gene, and a thorough neurodiagnostic workup in preparation for HSCT should occur as previously described to enable this procedure to be performed before 30 days of age.26
- 3.
Intermediate levels of psychosine must be evaluated in consultation with and eventual referral to a specialty care center. During the initial patient evaluation, laboratory testing should include GALC enzyme activity in WBC, PSY in RBC, and genotyping of the GALC gene. In these cases, there is less urgency and these tests should be sufficient to determine if the patient is affected with a KD variant that requires further assessment and long-term monitoring for eventual HSCT.
When PSY is elevated immediate referral to a specialty center is required to ensure timely confirmation of infantile Krabbe disease (IKD) and hematopoietic stem cell transplantation (HSCT). When PSY is in an intermediate range, the primary care provider in consultation with specialists will determine the follow-up plan that includes the listed laboratory tests. A normal PSY level is not consistent with IKD and indicates that GALC activity was low due to pseudodeficiency or carrier status, although very rare cases with late-onset Krabbe disease (LOKD) are not excluded (see text). 1Ruling out Saposin A deficiency requires molecular genetic analysis of PSAP1. 2Evaluations may include a neurologic exam, brain magnetic resonance image (MRI) with diffusion tensor imaging (DTI), neurophysiologic studies (brainstem auditory evoked potential [BAER], visually evoked potential [VEP], electroencephalogram [EEG], nerve conduction, neurocognitive testing), cerebrospinal fluid (CSF) protein, psychosine (blood, CSF). RBC red blood cells (erythrocytes), WBC white blood cells (leukocytes).
For diagnostic purposes, the only known non-KD condition that may be associated with elevated PSY is Saposin A deficiency where GALC activity is normal, but PSY was measured and found to be elevated in one of the three cases reported to date.27 These patients will likely not be detected by NBS where in vitro analysis of GALC activity is essentially normal.
Very high levels of PSY at birth correlate well with IKD. However, several LOKD patients have now been identified with intermediate levels of PSY,24 revealing a need for the more sensitive and accurate PSY measurement at single-digit nanomolar concentrations to better differentiate potential LOKD patients from all other groups (IKD, GALC pseudodeficiency, and GALC variant carriers). They also prompted the development of a more precise GALC enzyme assay in WBCs.25 The method described here is similar to our previous method of PSY quantitation, but has improved sensitivity (Supplemental Fig. 2). Indeed our data indicate that it is possible to differentiate IKD and most LOKD patients not only from normal controls, but also from pathogenic GALC variant carriers and pseudodeficiency carriers (Fig. 1).
Findings in three cases (patients 33, 35, and 36; Table 1) demonstrate variability among possible LOKD patients and highlight the need for continued clinical and biochemical monitoring. Patient 33 had elevated PSY in the range of LOKD patients with an overall decreasing trend over time (Fig. 3b). At 20 months old this patient has remained asymptomatic and is being monitored for possible disease progression. In contrast, four PSY measurements in DBS were obtained for patient 35; two were mildly elevated while two were within the control range (Figs. 2d and 3b). The PSY assay presented here is sensitive enough to differentiate patient PSY values at these low concentrations, but the clinical significance of minimal PSY elevations is still uncertain. This patient has symptoms that could be consistent with KD, including developmental delay and seizures. Because this presentation is not sufficient to make a confident diagnosis of KD, exome sequencing was performed but was uninformative beyond the known GALC genotype. Patient 36 developed normally until approximately 14 months of age before experiencing regression of development and motor skills. Measurement of WBC GALC activity was consistent with IKD, but PSY values were within the range observed in LOKD patients, although with a trend of increasing PSY concentrations over time (Figs. 2e and 3b). Regardless of the biochemical findings, the age of symptom onset is more consistent with LOKD. Retrospective analysis of this patient’s original NBS specimen revealed a normal PSY concentration, which along with the intermittently normal follow-up PSY analyses for patient 35 raises concern because these cases could represent a subpopulation of LOKD that would be very difficult to detect with PSY analysis and potentially result in negative NBS results. However, assessment of an NBS specimen 15 months after collection (patient 35) and storage at room temperature may result in falsely low values because of PSY degradation or insufficient extraction from the DBS. PSY appears to be stable in NBS specimens for at least 96 days,15 however, minimal PSY degradation could prove problematic when evaluating retrospectively stored DBS samples of LOKD patients with only minimally abnormal PSY. Nevertheless, the possibility of a limitation of PSY analysis is also suggested by Zhao et al., who found normal PSY concentrations in plasma for three of six LOKD patients.4 Of note, however, is that in plasma PSY is less abundant compared with blood, RBCs, or WBCs (C. Turgeon, personal communication). Our new method to measure PSY in RBCs that allows normalization of PSY to hemoglobin may provide improved longitudinal PSY monitoring capabilities after NBS because it also eliminates the variability inherent in DBS collection.
In addition to NBS and short-term follow up, longitudinal measurement of PSY in DBS has been assessed as a marker of HSCT efficacy both by Escolar et al. and in this study (Fig. 3).24 In three IKD cases PSY could be measured multiple times before HSCT. While the concentration of PSY in NBS samples is typically higher than in follow-up specimens (likely due to the relatively high cell count in neonates), the concentration of PSY had decreased further in these patients prior to HSCT (Fig. 3c), but remained multifold over the control range and consistent with IKD. The significance of these findings is uncertain in particular as it pertains to the utility of PSY as a marker of disease progression in infants considered to have LOKD. Otherwise, in all IKD and LOKD cases the PSY concentration dropped significantly following HSCT but did not normalize within 4 to 24 months in patients with IKD. Extended follow up and monitoring are required to determine the clinical significance of reduced but not normalized PSY concentrations in transplanted patients. Overall, PSY quantitation is a valuable tool for minimally invasive assessment of HSCT efficacy and disease/treatment monitoring, but PSY in RBC lysate may ultimately prove to be a more useful test for monitoring of asymptomatic patients, in particular patients with LOKD.
In summary, the new, more sensitive assay for PSY measurement in DBS not only identifies IKD patients but also differentiates most LOKD patients from pathogenic GALC variant and pseudodeficiency carriers. In the setting of NBS this assay meets the need to detect IKD and most LOKD cases.26 NBS stakeholders and program administrators must decide if the possibility of not identifying unusual and likely rare patients with low GALC activity, GALC genotypes of uncertain significance, and normal PSY is acceptable to avoid false positive results and the associated unnecessary cost and anxiety. Following an abnormal NBS result for KD (Fig. 4) or when evaluating a clinically suspicious patient, the accurate measurement of PSY and GALC activity allows differentiating not only affected from unaffected patients, but IKD from LOKD as well as KD from reduced GALC activity due to pseudodeficiency or carrier status for a GALC variant. More studies, however, are needed to determine the value of PSY measurement in DBS, RBCs, and cerebrospinal fluid (CSF) when following asymptomatic LOKD patients for disease progression and HSCT planning, or to monitor the success of HSCT or other treatment modalities that may become available in the future.18,28,29
References
Lyon G, Hagberg B, Evrard P, Allaire C, Pavone L, Vanier M. Symptomatology of late onset Krabbe’s leukodystrophy: the European experience. Dev Neurosci. 1991;13:240–244.
Bascou N, DeRenzo A, Poe MD, Escolar ML. A prospective natural history study of Krabbe disease in a patient cohort with onset between 6 months and 3 years of life. Orphanet J Rare Dis. 2018;13:126.
Duffner PK, Barczykowski A, Kay DM, et al. Later onset phenotypes of Krabbe disease: results of the world-wide registry. Pediatr Neurol. 2012;46:298–306.
Zhao S, Zhan X, Wang Y, et al. Large-scale study of clinical and biochemical characteristics of Chinese patients diagnosed with Krabbe disease. Clin Genet. 2018;93:248–254.
Rafi MA, Luzi P, Chen YQ, Wenger DA. A large deletion together with a point mutation in the GALC gene is a common mutant allele in patients with infantile Krabbe disease. Hum Mol Genet. 1995;4:1285–1289.
Orsini JJ, Kay DM, Saavedra-Matiz CA, et al. Newborn screening for Krabbe disease in New York State: the first eight years’ experience. Genet Med. 2016;18:239–248.
Escolar ML, Poe MD, Provenzale JM, et al. Transplantation of umbilical-cord blood in babies with infantile Krabbe’s disease. N Engl J Med. 2005;352:2069–2081.
Wright MD, Poe MD, DeRenzo A, Haldal S, Escolar ML. Developmental outcomes of cord blood transplantation for Krabbe disease: a 15-year study. Neurology. 2017;89:1365–1372.
Allewelt H, Taskindoust M, Troy J, et al. Long-term functional outcomes after hematopoietic stem cell transplant for early infantile Krabbe disease. Biol Blood Marrow Transplant. 2018;24:2233–2238.
Steiner RD. Commentary on: “Newborn screening for Krabbe Disease: the New York State model” and “the long-term outcomes of presymptomatic infants transplanted for Krabbe disease. A report of the workshop held on July 11 and 12, 2008, Holiday Valley, New York”. Genet Med. 2009;11:411–413.
Wasserstein MP, Andriola M, Arnold G, et al. Clinical outcomes of children with abnormal newborn screening results for Krabbe disease in New York State. Genet Med. 2016;18:1235–1243.
Dimmock DP. Should states adopt newborn screening for early infantile Krabbe disease? Genet Med. 2016;18:217–220.
Tortorelli S, Turgeon CT, Gavrilov DK, et al. Simultaneous testing for 6 lysosomal storage disorders and X-adrenoleukodystrophy in dried blood spots by tandem mass spectrometry. Clin Chem. 2016;62:1248–1254.
Minter Baerg MM, Stoway SD, Hart J, et al. Precision newborn screening for lysosomal disorders. Genet Med. 2018;20:847–854.
Turgeon CT, Orsini JJ, Sanders KA, et al. Measurement of psychosine in dried blood spots-a possible improvement to newborn screening programs for Krabbe disease. J Inherit Metab Dis. 2015;38:923–929.
Chuang WL, Pacheco J, Zhang XK, et al. Determination of psychosine concentration in dried blood spots from newborns that were identified via newborn screening to be at risk for Krabbe disease. Clin Chim Acta. 2013;419:73–76.
Miyatake T, Suzuki K. Globoid cell leukodystrophy: additional deficiency of psychosine galactosidase. Biochem Biophys Res Commun. 1972;48:539–543.
Li Y, Xu Y, Benitez BA, et al. Genetic ablation of acid ceramidase in Krabbe disease confirms the psychosine hypothesis and identifies a new therapeutic target. Proc Natl Acad Sci USA. 2019;116:20097–20103.
Cantuti Castelvetri L, Givogri MI, Hebert A, et al. The sphingolipid psychosine inhibits fast axonal transport in Krabbe disease by activation of GSK3beta and deregulation of molecular motors. J Neurosci. 2013;33:10048–10056.
D’Auria L, Reiter C, Ward E, et al. Psychosine enhances the shedding of membrane microvesicles: Implications in demyelination in Krabbe’s disease. PLoS ONE. 2017;12:e0178103.
Hawkins-Salsbury JA, Parameswar AR, Jiang X, et al. Psychosine, the cytotoxic sphingolipid that accumulates in globoid cell leukodystrophy, alters membrane architecture. J Lipid Res. 2013;54:3303–3311.
Reddy AS, Patel JR, Vogler C, Klein RS, Sands MS. Central nervous system pathology progresses independently of KC and CXCR2 in globoid-cell leukodystrophy. PLoS ONE. 2014;8:e64647.
White AB, Givogri MI, Lopez-Rosas A, et al. Psychosine accumulates in membrane microdomains in the brain of krabbe patients, disrupting the raft architecture. J Neurosci. 2009;29:6068–6077.
Escolar ML, Kiely BT, Shawgo E, et al. Psychosine, a marker of Krabbe phenotype and treatment effect. Mol Genet Metab. 2017;121:271–278.
Liao HC, Spacil Z, Ghomashchi F, et al. Lymphocyte galactocerebrosidase activity by LC-MS/MS for post-newborn screening evaluation of Krabbe disease. Clin Chem. 2017;63:1363–1369.
Kwon JM, Matern D, Kurtzberg J, et al. Consensus guidelines for newborn screening, diagnosis and treatment of infantile Krabbe disease. Orphanet J Rare Dis. 2018;13:30.
Calderwood L, Wenger DA, Matern D, Dahmoush H, Watiker V, Lee C. Rare saposin A deficiency: novel variant and psychosine analysis. Mol Genet Metab. 2020;129:161–164.
Pan X, Sands SA, Yue Y, Zhang K, LeVine SM, Duan D. An engineered galactosylceramidase construct improves AAV gene therapy for Krabbe disease in twitcher mice. Hum Gene Ther. 2019;30:1039–1051.
Marshall MS, Issa Y, Jakubauskas B, et al. Long-term improvement of neurological signs and metabolic dysfunction in a mouse model of Krabbe’s disease after global gene therapy. Mol Ther. 2018;26:874–889.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
The authors declare no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Guenzel, A.J., Turgeon, C.T., Nickander, K.K. et al. The critical role of psychosine in screening, diagnosis, and monitoring of Krabbe disease. Genet Med 22, 1108–1118 (2020). https://doi.org/10.1038/s41436-020-0764-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41436-020-0764-y
Keywords
This article is cited by
-
“Atypical” Krabbe disease in two siblings harboring biallelic GALC mutations including a deep intronic variant
European Journal of Human Genetics (2022)