Abstract
Purpose
To evaluate associations between prenatal trio exome sequencing (trio-ES) and psychological outcomes among women with an anomalous pregnancy.
Methods
Trio-ES study enrolling patients with major fetal anomaly and normal microarray. Women completed self-reported measures and free response interviews at two timepoints: pre- (1) and post- (2) sequencing. Pre-sequencing responses were compared with post-sequencing responses; post-sequencing responses were stratified by women who received trio-ES results that may explain fetal findings, secondary findings (medically actionable or couples with heterozygous variants for the same recessive disorder), or negative results.
Results
One hundred fifteen trios were enrolled. Of those, 41/115 (35.7%) received results from trio-ES, including 36 (31.3%) who received results that may explain the fetal phenotype. These women had greater post-sequencing distress compared with women who received negative results, including generalized distress (p = 0.03) and test-related distress (p = 0.2); they also had worse psychological adaptation to results (p = 0.001). Genomic knowledge did not change from pre- to post-sequencing (p = 0.51).
Conclusion
Women show more distress after receiving trio-ES results compared with those who do not, suggesting that women receiving results may need additional support or counseling to inform current and future reproductive decisions.
Similar content being viewed by others
INTRODUCTION
Fetal anomalies affect 3–5% of all pregnancies and account for nearly 20% of perinatal mortality.1 Advances in prenatal genetic screening and diagnosis, ranging from chromosomal microarray to next-generation sequencing strategies, offer an opportunity to provide information to inform reproductive decision-making and more tailored pre- and postnatal pregnancy management. Further, these advances allow for multidisciplinary care planning, and they inform and improve neonatal care and health outcomes.2 Prenatal trio exome sequencing (trio-ES) is one such advance. Evidence thus far suggests that trio-ES increases diagnostic yield when standard genetic testing (karyotype and microarray) is normal.3,4,5 The two largest studies found a diagnostic rate of 8.5% and 10%, overall, and 15.4% and 19% in cases of multisystem abnormalities.4,5 Given emerging evidence showing improved diagnostic rates and the generally rapid uptake of next-generation sequencing strategies in clinical care, it is likely that trio-ES will eventually be integrated into prenatal clinical care.
However, to date, there are no large studies with prospectively collected longitudinal data assessing women’s understanding of trio-ES results, the psychological impact of testing, and influence on future reproductive decisions. Rapid integration of new technologies such as exome sequencing pose significant and unique ethical and counseling challenges.6 Women’s ability to understand and accept information from next-generation sequencing technologies such as trio-ES is likely to depend on factors that influence these responses to other diagnostic strategies. For instance, these factors may include health literacy, socioeconomic status, race/ethnicity, cultural and religious beliefs, attitudes toward termination, experiences with disability, and the methods and mode of information delivery.7,8,9,10,11,12 Furthermore, genetic information provided in this setting may be prone to uncertainty (e.g., variants of uncertain significance) or they may have strong potential to impact parental wellbeing (e.g., medically actionable secondary findings). Thus, psychosocial adjustment and the behavioral impact of prenatal exome sequencing results are important outcomes to understand prior to integration of trio-ES into the diagnostic algorithm. Because of the limited empiric data available to guide best counseling and implementation of trio-ES in this arena, our objective was to understand the association between sequencing outcomes and maternal decisional conflict, psychological adaptation, and future reproductive decisions by leveraging our existing cohort from the UNC–Chapel Hill (UNC-CH) fetal exome sequencing project. We also evaluated genomics knowledge pre- and postcounseling to assess whether baseline genetic knowledge or knowledge gain during counseling may contribute to differences in psychological outcomes. We hypothesized the following: (1) women who received a result from trio-ES that may explain the fetal phenotype would have higher levels of generalized distress and worse psychological adaptation to their results than women who received secondary findings or no reportable results, (2) higher maternal educational level and baseline genomic knowledge would be associated with lower generalized distress and better psychological adaptation post-sequencing, and (3) pre-sequencing genomic knowledge would be higher among women who self-identify as having higher levels of education, income, and prior experience with genetic screening or testing.
MATERIALS AND METHODS
We enrolled trios (parents and fetus) in pregnancies complicated by either isolated or multiple congenital anomalies with a normal karyotype and microarray. Patients were identified from prenatal diagnosis clinics from UNC-CH and from prenatal diagnosis clinics across the United States between July 2014 and December 2019. Providers from outside of the UNC Healthcare system identified patients for referral based on knowledge of our ongoing study and its eligibility criteria. Such patients had already participated in reproductive genetic counseling with their institution and were continuing pregnancy management with their primary obstetric providers. Patients interested in study participation were then referred directly to our study coordinator. After ensuring that the patient met inclusion criteria, a certified prenatal genetic counselor at UNC-CH performed pretest counseling and consent procedures for the study. Non-local families gave consent via secure web-based video calls. Mothers and fathers provided consent separately so that counselors could discuss the chance of non-paternity with mothers and allow them to opt out of the study if they desired. Trios were included in the study if the following inclusion criteria were met: (1) singleton gestation; (2) suspected genetic etiology of congenital anomalies visualized on ultrasound; (3) lack of diagnosis after karyotype, microarray, and if indicated, gene-specific sequencing; and (4) presence of DNA from fetus, mother, and father. Parent–fetus trios were identified both prospectively and retrospectively and were enrolled at various gestational ages or after the pregnancy was completed. Trios enrolled prospectively were only approached for recruitment to the study after they had received standard clinical counseling and had made a decision about pregnancy management (e.g., continuation versus termination of pregnancy). The study was not mentioned prior to this time to avoid impacting parental decision-making. Trios were also identified retrospectively through the UNC Perinatal Database, a repository of patients who received prenatal and delivery care at UNC (1996 to present). Women who previously indicated a desire to be recontacted for additional fetal testing and who had fetal cells archived and available for DNA extraction were also approached for enrollment. Women who were identified retrospectively were not included in this analysis of psychological outcomes.
After enrollment, participants had pretest counseling by a certified prenatal genetic counselor regarding trio-ES and the possible results it can provide (genetic counseling was performed as previously described).13 This counseling specifically reviewed existing data regarding use of trio-ES in the prenatal setting, expected diagnostic yield from trio-ES in the setting of study inclusion criteria, and limitations to result interpretation in the setting of negative results. Additionally, given the novel nature of trio-ES, patients were clearly informed that testing was occurring in the context of study protocols. All participants agreed to learn findings that explained the fetal phenotype, medically actionable secondary findings in a parent, and/or where both parents had heterozygous variants for the same recessive disorder. Participants who chose to opt out of learning any of the former findings at the time of consent were excluded from the study. After enrollment, we obtained maternal and paternal blood and extracted DNA in the Biospecimen Processing Facility, a core UNC-CH laboratory. Fetal DNA was extracted from stored specimens, such as amniocytes, chorionic villi, or umbilical cord blood as appropriate. For nonlocal cases, we directly received extracted fetal DNA from the outside institution. All genetic variants that were identified were confirmed by Sanger sequencing at the UNC Molecular Genetics Laboratory (MGL), a CLIA-certified and College of American Pathologists (CAP)-accredited facility, using a duplicated sample. After confirmation of results, parents were given the option to sign a separate consent form to have their own or their child’s variant placed in the medical record.
Data were collected at two time points. Immediately after presequencing counseling and enrollment, the mother completed a presequencing demographics questionnaire and a measure of genomic knowledge adapted from the NCGENES study (UNC-GKS). This measure includes 25 statements that participants are asked to judge as being true or false. Possible responses included “don’t know/unsure” to reduce guessing. The statements were designed to evaluate recall and understanding of new information received in the study. Correct responses were summed to create a score ranging from 0 (no answers correct) to 25 (all answers correct) (Supplemental material 1).14 Women also completed a validated measure of generalized distress (symptoms of anxiety and depression), the Hospital Anxiety and Depression Scale (HADS),15 and were asked an open-ended question prompting them to describe their expectations of and reasons for pursuing exome sequencing for fetal diagnosis (Fig. 1). After return of results, participants were counseled regarding findings from trio-ES and repeated the measures of genomic knowledge and generalized distress (postsequencing measures). They also completed the following assessments: (1) test-related distress (adapted from the Multidimensional Impact of Cancer Risk Assessment [MICRA]);16 (2) decisional conflict using the Decisional Conflict Scale (DCS);17 (3) psychological adaptation to results (perceptions of nonintrusiveness, support, self-worth, certainty, and self-efficacy) using the Psychological Adaptation to Genetic Information Scale (PAGIS);18 and (4) brief, open-ended question prompting women to summarize their interpretation of findings from trio-ES and experience with sequencing in their own words. The postsequencing assessment was completed 2 weeks after sequencing results were delivered. Interviews and assessments were completed in person, online, by phone, or by web-based video platform dependent on the participant location (Fig. 1).
Participants’ demographic characteristics were analyzed using descriptive statistics. Pre- and postsequencing genomic knowledge and generalized distress were compared. Postsequencing generalized distress, test-related distress, decisional conflict, and psychological adaptation to results were compared for the following groups: (1) women who received negative results from trio-ES, (2) women who received results that may explain the fetal phenotype, and (3) women who received a report of medically actionable secondary findings or couples with heterozygous variants for the same recessive disorder. Additionally, associations between presequencing genomic knowledge test scores, maternal demographic characteristics, and postsequencing self-reported outcomes were assessed. Bivariable analyses were completed using t-test, Wilcoxon rank-sum, Kruskal–Wallis test, Spearman’s correlation, and linear regression, as appropriate. Pairwise comparisons using Tukey’s method was employed as appropriate. P < 0.05 was considered statistically significant.
All analyses were completed using STATA 15 statistical software (College Station, TX).
RESULTS
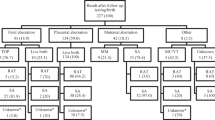
One hundred fifteen trios were enrolled in the study. Of these participants, 41 (35.7%) received results from trio-ES, of which 36 (31.3%) received results that may explain the fetal phenotype. Seven (6.1%) received secondary findings (either medically actionable incidental findings in a parent or couples with heterozygous variants for the same recessive disorder). Maternal demographic characteristics are shown in Table 1. Median age of women enrolled in the study was 31 (IQR 27, 34). Most of the cohort self-identified as Non-Hispanic White (71.3%), married (84.3%), and as having some college education (87%). In addition, over half the cohort has had prior experience with prenatal genetic screening or diagnosis (57.4%). Fetal genetic material for diagnosis was obtained through chorionic villus sampling (CVS), amniocentesis, cord blood, or products of conception. The majority of fetal genetic material was obtained from amniocentesis or CVS (70.4%).
Of the 115 women who participated in trio-ES, 101 (88%) completed the post-sequencing assessment. Overall, women who received results that may explain the fetal phenotype had higher post-sequencing generalized distress, test-related distress, and worse psychological adaptation to testing compared with women who received medically actionable secondary findings or negative trio-ES results. Higher scores on each of these scales are suggestive of the following: increased symptoms of anxiety and depression (HADS), test-related distress and uncertainty (MICRA), and intrusive thoughts and lack of support (PAGIS). Specifically, women who received findings that may explain the fetal phenotype or who received medically actionable secondary findings reported higher test-related distress (MICRA) than women who received negative results (8.1 vs. 4.8 vs. 3.1, p < 0.001). In pairwise comparisons, test-related distress was significantly higher among the group of women who received findings that may explain the fetal phenotype compared with those receiving negative results (mean difference = 5.02, p < 0.001). There was no difference in likelihood to report positive experience with testing on the MICRA between groups. Similar patterns appeared for several subscales of the measure of psychological adaptation to results (PAGIS), including intrusive thoughts (8.3 [SD 5.8] vs. 8.7 [SD 6.7] vs. 4.5 [SD 5.9], p = 0.003) and difficulty with support from family and peers (9.3 [SD 9.2] vs. 7 [SD 4.9] vs. 3.7 [SD 5.0], p < 0.001). Among pairwise comparisons, intrusive thoughts, difficulty with support, and overall worse adaptation to results were significantly different among women who received results that explained the fetal phenotype than those who received negative results (mean difference = 3.7, p = 0.01; mean difference = 5.5, p < 0.001, mean difference = 8.7, p = 0.005, respectively) (Table 2).
Women who received results that explain the fetal phenotype had significantly higher overall score on the HADS (10.1 [SD 6.5], 6.5 [SD 5.7], 7.2 [SD 5.2], p = 0.03), specifically the depression subscale (3.2 [SD 3.3], 1.2 [SD 2.5], 12.0. [SD 2.7)], p = 0.003), compared with women who received medically actionable secondary findings or negative results. Pairwise comparisons demonstrated that there was a significant difference in the depression subscale between women who received results that explain the fetal findings compared with women that received negative results (mean difference = 1.97, p = 0.003) Notably, women who received results did not differ in their decisional conflict when compared with women who had negative results, indicating that they did not differ in their perceptions of feeling informed, clear about their values, and satisfied with their choice (DCS scores 41.8 [SD 5.5] vs. 43.2 [SD 5.4] vs. 40 [SD 0] p = 0.34). Similarly, there was no difference in mean DCS scores between groups when employing pairwise comparisons (p = 0.28, 0.47, 0.23). (Table 2).
Mean generalized distress scores were significantly higher among women at pre-sequencing than post-sequencing, both in terms of the overall score and when we conducted follow-up analyses evaluating the anxiety and depressive symptoms subscales of this measure separately (HADS pre-sequencing mean anxiety scores 7.8 [SD 4.2], post-sequencing mean anxiety scores 5.8 [SD 3.8], p = 0.005; HADS pre-sequencing mean depression scores 4.2 [SD 4.1], post-sequencing mean depression scores 1.8 [SD 2.9], p < 0.001; HADS pre-sequencing mean total score 11.9 [SD 7.3], post-sequencing mean total score 7.6 [SD 6.1], p < 0.001).
There was no significant correlation between post-sequencing psychological outcomes and maternal demographic characteristics such as age, race, marital status, income, educational level, and prior genetic testing. However, receipt of any trio-ES result (either one that may explain the fetal phenotype or a secondary finding) was associated with higher post-sequencing test-related distress (7.2 SD [1.0] vs. 3.2 [SD 0.66], p < 0.001), higher generalized distress (9.4 [SD 1.1] vs. 6.5 [SD 0.75], p = 0.02), and worse psychological adaptation (18.2 [SD 2.3] vs.10.8 [SD 1.6], p = 0.0007) scores.
Within the cohort overall, mean genomic knowledge scores did not change from pre- to post-sequencing (pre-sequencing mean number correct 21.7 [of 25] [SD 0.22], post-sequencing mean number correct 21.9 [SD 0.32], p = 0.51). Pre-sequencing genomic knowledge was associated with higher education level (p = 0.0013). Mean genomic knowledge score among women who did not complete high school was 13.5 correct (of 25) (SD 1.5) whereas women with graduate degrees had a mean score of 22.8 correct (SD 0.6). Regression analysis demonstrated that women with higher education levels (adjusted coefficient 0.37, p < 0.001) and previous genetic testing (adjusted coefficient 0.02, p < 0.001) were more likely to have higher genomic knowledge scores at the pre-sequencing assessment (model adjusted for age, race, marital status, employment, income level). Of note, there was no significant association between pre-sequencing genomic knowledge and post-sequencing psychological outcomes.
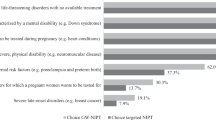
The majority of women in our cohort pursued trio-ES in hopes of having future children (83%), information to guide prenatal diagnosis for future pregnancies (90%), and reassurance to reduce concerns about future children (90%). A significant proportion of women sought trio-ES for a definite explanation for findings in the current pregnancy (90%), despite pretest counseling regarding diagnostic yield. post-sequencing, 70% of women in the cohort reported that trio-ES outcomes did not change their future reproductive plans and nearly half the cohort remained undecided about future pregnancy (47.9%) (Table 3).
DISCUSSION
Our study describes the unique experience of women utilizing trio-ES for prenatal genetic diagnosis. Short answer and survey responses obtained pre-sequencing demonstrate that the majority of women had high expectations of trio-ES to provide an answer related to their current pregnancy and also desired reassurance or answers about future pregnancies. Moreover, mean anxiety and depression scores within the cohort were significantly higher pre-sequencing than post; we hypothesize that this could be driven by the typical series of events required to obtain fetal genetic diagnosis, the burden of recent decision making regarding termination versus continuation of pregnancy, and the uncertainty regarding future reproductive plans. It also may point to a role that information and contextualized support may have in mitigating anxiety. Importantly, the results speak to the significant mental health burden associated with bearing an anomalous pregnancy and the need for additional maternal support and mental health monitoring during the diagnostic process and after receipt of results.
Prior studies have demonstrated the substantial psychological repercussions for women in the setting of an anomalous pregnancy or pregnancy loss.19,20 Our results suggest that there may be additional mental health impacts from test-related anxiety and distress, particularly among women who receive results from testing. This may also be related to uncertainty of shared results and provision of secondary findings. Bernhardt et al. identified that uncertainty and unquantifiable risks particularly impacted maternal psychological wellbeing after receiving microarray results for fetal genetic diagnosis. Ultimately, such results led to an anxiety-ridden pregnancy and postnatal period, increasing decisional conflict regarding testing and leading to results being viewed as “toxic knowledge.”21 While we noted differences in anxiety and depression scores related to study results, it is worth noting that scores decreased after completion of testing. This may relate to the fact that results were provided after decisions about pregnancy continuation were already made, which is in contrast to the study by Barnhardt et al. Still, the results of our study in the context of prior literature suggest that uncertain results and secondary findings may impact long-term maternal psychological outcomes, particularly altering family dynamics, relationships, and support networks. Future studies need to target the longitudinal impact of next-generation sequencing on parental psychosocial wellbeing to determine best practices for implementation and provision of adequate support.
Our study also demonstrates that nearly half of women in our cohort remained uncertain about future reproductive plans after trio-ES even though most women initially pursued advanced sequencing to assist with future reproductive planning. This highlights the importance of goals clarification in pretest counseling. Prior studies have suggested that given the increasingly common role of prenatal genetic screening and testing in the diagnostic algorithm, many women opt for the opportunity to receive additional information without carefully considering the risks and benefits of testing.22,23 Yet limiting pretest counseling to risks and benefits may not provide a true assessment of whether information provided will ultimately be psychologically beneficial or harmful. Instead, there is a significant need for goals clarification prior to pursuit of trio-ES and improvement in pretest counseling to include uncertainty of results and how parents think they would fair in the face of unquantifiable risk.21
Post-sequencing, women who received any trio-ES result were more likely to experience test-related anxiety and distress, test-related uncertainty, and had worse psychological adaptation to the genetic information provided compared with those who had no result. This is in contrast to prior studies that suggest receiving a result, any result, after advanced sequencing strategies is overall viewed very positively by patients, allowing patients to feel empowered about their own health, contributory to the progress of genomic medicine, and receiving closure regarding the workup of their condition.24,25 We posit several reasons this discrepancy may exist in contrast to the prior literature. First, there are limited data about postsequencing psychological outcomes in the prenatal arena. Data about post-sequencing perspectives from other clinical scenarios may be distinctly different given the unique individual, social, and community aspects that inform reproductive decisions. Additionally, receiving results may have also triggered maternal anxiety and distress about existing children or future pregnancies. The longitudinal impact of receiving this data on interparental relationships, relationships with children, and future reproductive decisions was not extensively explored in our study and is an important consideration for future research.
Notably, in our study, there was no association between maternal demographic characteristics, baseline genetic knowledge, and post-sequencing survey scores. As expected, baseline genetic knowledge was strongly associated with education level and previous experience with genetic testing. The lack of association between baseline genetic knowledge and post-sequencing survey results is in contrast to other literature that suggests heath literacy and medical knowledge are critical to medical decision-making, reduction of decisional conflict, and adaptation of health information.14,26,27 It is possible that the association was not easily identified given the homogeneity of our cohort, which was predominantly Non-Hispanic White, educated women. As such, future studies are necessary to determine how psychological outcomes may differ in populations that have lower health literacy or limited experience with genetic testing, or who approach genetic testing with different values or from different cultural contexts. It also brings forward the issue of representation in genetic studies and the importance of identifying barriers to a more diverse group of women electing to participate in the study.
The issues surrounding pre- and post-test counseling, including interpretation of results and potential patient harms associated with anxiety, uncertainty, and missed parental expectations are in line with previously noted challenges of incorporating trio-ES into the prenatal fold.28,29 Previous work from our group discussed specific examples of ethical counseling challenges that have risen from this ongoing prospective cohort, identifying the importance of effective and appropriate communication of uncertainty and how it may impact long-term parental decisions.6 In particular, prior studies have identified the conflict between respect for patient autonomy and the potential harms of uncertainty and unquantifiable risk, ultimately resulting in outcomes that are discordant with robustly autonomous medical decision making.30 Prior studies have suggested that use of evidence-based counseling methods, guidelines on most applicable clinical scenarios for trio-ES, and standardization of reporting of results may improve patient autonomy in decision making.28
Our study has many strengths. It is a large, prospective cohort with longitudinal data. To our knowledge, we are the largest reporting study to date of maternal psychological outcomes after use of prenatal trio-ES. Our diagnostic yield is in line with prior studies. In our cohort, 22.3% of women received results from trio-ES that were suspected to explain fetal findings. Prior studies report a 10–57% diagnostic yield when using trio-ES.31,32 Moreover, we used validated surveys and scales, adapted to assess test-related psychological outcomes in this particular scenario.
Yet, the findings of our study should be interpreted within the context of its limitations. Our cohort is primarily composed of women who identify as Non-Hispanic White, have college or greater education, and fall into high earning income groups. Thus, our results may not be generalizable to the general population. Future studies should work toward understanding and addressing barriers to enrolling women from diverse as well as marginalized populations in prenatal diagnosis studies and enroll a more representative population. These data will be critical in producing more generalizable results and inform a strategy for more equitable use of next-generation sequencing strategies. Women of lower socioeconomic status, educational backgrounds, and from a wider range of ethnicities may have psychosocial outcomes with use of trio-ES that are significantly different from those captured in our study. Expanding our understanding of impact of trio-ES on diverse populations is integral to the development of an equitable and supportive platform to offer this technology.
Future studies should focus on the longitudinal psychosocial ramifications of advanced sequencing strategies, with the goal of developing resources to provide support during the pretest and post-test periods. Examples include use of additional interactions with the prenatal genetic counselor via phone or web-based video platform or development of a pre-established psychological counseling support team for these women. The use of decision aids may also be a method of providing information while clarifying parental values and assessing ability to cope with uncertainty. Critically, such studies should focus on recruiting a diverse cohort to ensure that strategies for implementation are developed with a robust understanding of the impact of advancing technology on parents of various ethnic, educational, and financial backgrounds. Advanced sequencing strategies offer significant prospect to improve the accuracy of prenatal genetic diagnosis. With continued growth in our understanding of parental psychological needs we will be able to improve the manner in which these technologies are offered and provide benefit to parents seeking answers.
Data availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Osterman, M., Kochanek, K., MacDorman, M., Strobino, D. & Guye, B. Annual summary of vital statistics: 2012-2013. Pediatrics 135, 1115–1125 (2015).
Wou, K. et al. Parental perceptions of prenatal whole exome sequencing (PPPWES) study. Prenat. Diagn. 38, 801–811 (2018).
Vora, N. L. & Hui, L. Next-generation sequencing and prenatal’omics: advanced diagnostics and new insights into human development. Genet. Med 20, 791–799 (2018).
Lord, J. et al. Prenatal exome sequencing analysis in fetal structural anomalies detected by ultrasonography (PAGE): a cohort study. Lancet 393, 747–757 (2019).
Petrovski, S. et al. Whole-exome sequencing in the evaluation of fetal structural anomalies: a prospective cohort study. Lancet 393, 758–767 (2019).
Harris, S., Gilmore, K., Hardisty, E., Lyerly, A. D. & Vora, N. L. Ethical and counseling challenges in prenatal exome sequencing. Prenat. Diagn 38, 897–903 (2018).
Kaphingst, K. A. et al. Preferences for return of incidental findings from genome sequencing among women diagnosed with breast cancer at a young age. Clin. Genet 89, 378–384 (2015).
Biesecker, B. B. et al. How do research participants perceive “uncertainty” in genome sequencing? Genet. Med 16, 977–980 (2014).
Case, A. P., Ramadhani, T. A. & Canfield, M. A. W. C. Awareness and attitudes regarding prenatal testing among Texas women of childbearing age. J. Genet. Couns. 16, 655–661 (2007).
Kuppermann, M. & Gates, E. W. A. Racial-ethnic differences in prenatal diagnostic test use and outcomes: preferences, socioeconomics, or patient knowledge? Obstet. Gynecol. 87, 675–682 (1996).
Norton, M., Nakagawa, S. & Kuppermann, M. Women’s attitudes regarding prenatal testing for a range of congenital disorders of varying severity. J. Clin. Med. 3, 144–152 (2014).
Willis, A. M. et al. How do prospective parents prefer to receive information about prenatal screening and diagnostic testing? Prenat. Diagn. 35, 100–102 (2015).
Vora, N. L. et al. An approach to integrating exome sequencing for fetal structural anomalies into clinical practice. Genet. Med. 22, 954–961 (2020).
Langer, M. M. et al. Development and validation of a genomic knowledge scale to advance informed decision-making research in genomic sequencing. MDM Policy Pract. 2, 2381468317692582 (2017).
Snaith, R. P. The hospital anxiety and depression scale. Health Qual. Life Outcomes 1, 6–9 (2003).
Cella, D. et al. A brief assessment of concerns associated with genetic testing for cancer: the Multidimensional Impact of Cancer Risk Assessment (MICRA) questionnaire. Heal. Psychol. 21, 564–572 (2002).
Brehaut, J. C. et al. Validation of a decision regret scale. Med. Decis. Making 23, 281–292 (2003).
Read, C. Y. & Perry, D. J. D. M. Design and psychometric evaluation of the Psychological Adaptation to Genetic Information Scale. J. Nurs. Scholarsh 37, 203–208 (2005).
Lippman, A. Prenatal genetic testing and geneticization: mother matters for all. Fetal Diagn. Ther. 8, 175–188 (1993).
Sandelowski, M. & Barroso, J. The travesty of choosing after positive prenatal diagnosis. J. Obstet. Gynecol. Neonatal Nurs. 34, 307–318 (2005).
Bernhardt, B. A. et al. Women’s experiences receiving abnormal prenatal chromosomal microarray testing results. Genet. Med. 15, 139–145 (2013).
Kenen, R. H. The at-risk health status and technology: a diagnostic invitation and the “gift” of knowing. Soc. Sci. Med. 42, 1545–1553 (1996).
Marteau, T. M. & Dormandy, E. Facilitating informed choice in prenatal testing: how well are we doing? Am. J. Med. Genet. 106, 185–190 (2001).
Clift, K. E. et al. Patients’ views on incidental findings from clinical exome sequencing. Appl. Transl. Genom. 4, 38–43 (2015).
Halverson, C. M. E., Clift, K. E. & McCormick, J. B. Was it worth it? Patients’ perspectives on the perceived value of genomic-based individualized medicine. J. Community Genet. 7, 145–152 (2016).
Bowen, D. J. et al. Theoretical foundations for interventions designed to promote informed decision making for cancer screening. Ann. Behav. Med. 32, 202–210 (2006).
Rini, C. et al. Genomic knowledge in the context of diagnostic exome sequencing: changes over time, persistent subgroup differenes, and associations with psychological sequencing outcomes. Genet. Med. 22, 60–68 (2020).
Narayanan, S., Blumberg, B., Clayman, M. L., Pan, V. & Wicklund, C. Exploring the issues surrounding clinical exome sequencing in the prenatal setting. J. Genet. Couns. 27, 1228–1237 (2018).
Best, S. et al. Promises, pitfalls and practicalities of prenatal whole exome sequencing. Prenat. Diagn. 38, 10–19 (2018).
Wolf, S. M. & Evans, B. J. Defending the return of results and data. Science 362, 1255–1256 (2018).
Drury, S. et al. Exome sequencing for prenatal diagnosis of fetuses with sonographic abnormalities. Prenat. Diagn. 35, 1010–1017 (2015).
Alamillo, C. L. et al. Exome sequencing positively identified relevant alterations in more than half of cases with an indication of prenatal ultrasound anomalies. Prenat. Diagn. 35, 1073–1078 (2015).
Acknowledgements
We acknowledge the support of University of North Carolina Division of Maternal Fetal Medicine and Division of Reproductive Genetics and institutions that have referred patients to our center for participation in the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Author contributions
Conceptualization: A.N.T, K.L.G, E.H, A.D.L, C.R., N.L.V; Data curation: A.N.T, K.L.G, E.H, A.D.L, C.R, N.L.V; Formal Analysis: A.N.T, K.L.G, A.D.L, C.R, N.L.V; Funding Acquisition: K.L.G, C.R., N.L.V; Investigation: A.N.T, K.L.G, E.H, A.D.L, C.R., N.L.V; Methodology: A.N.T, K.L.G, E.H, A.D.L, C.R., N.L.V; Project administration: K.L.G, E.H, N.L.V; Resources: K.L.G, N.L.V; Software: A.N.T Supervision: N.L.V Validation: A.D.L, C.R; Visualization: A.N.T Writing- original draft: A.N.T, K.L.G, E.H, N.L.V; Writing – review & editing: A.N.T, K.L.G, E.H, A.D.L, C.R., N.L.V.
Competing interests
The authors declare no competing interests.
Ethics declaration
The work was funded by Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) grant award number K23HD088742 (principal investigator N.L.V.). The University of North Carolina at Chapel Hill institutional review board (13–4084) provided approval for this study. Informed consent was obtained for each enrolled study participant.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Talati, A.N., Gilmore, K.L., Hardisty, E.E. et al. Impact of prenatal exome sequencing for fetal genetic diagnosis on maternal psychological outcomes and decisional conflict in a prospective cohort. Genet Med 23, 713–719 (2021). https://doi.org/10.1038/s41436-020-01025-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41436-020-01025-5
This article is cited by
-
Can cell-free DNA (cfDNA) testing alleviate psychological distress in early miscarriage? A commentary
Journal of Assisted Reproduction and Genetics (2022)