Abstract
Purpose
To investigate the anatomical and functional outcomes and specifically, the effect of 360-degree barrier-laser, in pars plana vitrectomy (PPV) for primary pseudophakic rhegmatogenous retinal detachment (PRD).
Methods
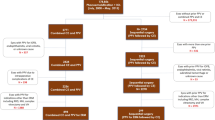
We conducted a single-centre retrospective, continuous and comparative study on eyes that had undergone PPV with focal-retinopexy (laser or cryotherapy) versus 360-laser for PRD repair between 2011–2020 at a single tertiary vitreoretinal centre in the UK. Primary outcomes were single surgery anatomical success (SSAS) rate and final postoperative visual acuity (VA). Multivariable regression covariates for primary re-detachment included age, gender, onset-of-detachment, pre-operative VA, ocular co-morbidities, macula-status, majority inferior (vs superior) PRD, number-of-tears and PRD extent (in clock-hours), 360-laser barricade, and perfluorocarbon liquid (PFCL) use. For VA gain, primary re-detachment was added as a covariate.
Results
We included 467 eyes with a mean follow-up of 388 (161) days. The SSAS was 444/467 (95.1%) overall, and 351/370 (94.9%) and 93/97 (95.9%) in focal-retinopexy and 360-laser groups, respectively (p = 0.798). Compared to the focal-retinopexy group, the 360-laser group had significantly worse post-operative VA but similar logMAR gain (p = 0.812). A multivariable binary logistic regression found that only PFCL use was linked with increased primary re-detachment (OR:5.32 [p = 0.048]) and 360-laser did not contribute to increased SSAS. A multivariable linear regression analysis showed that poor logMAR gain was significantly associated with better pre-operative logMAR, ocular co-morbidities, greater PRD extent, use of 360-laser and primary re-detachment. However, when excluding macula-off RD (n = 211), 360-laser was no longer significant (p = 0.088).
Conclusions
Prophylactic 360-laser does not seem to impact on SSAS and functional outcomes following PPV for primary PRD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others

Data availability
Data are available upon reasonable request.
References
Herrmann W, Helbig H, Heimann H. Pseudophakie-Ablatio. Klin Monbl Augenheilkd. 2011;228:195–200. https://doi.org/10.1055/s-0029-1246116.
Qureshi MH, Steel DHW. Retinal detachment following cataract phacoemulsification—a review of the literature. Eye. 2020;34:616–31. http://www.nature.com/articles/s41433-019-0575-z.
Ferrara M, Mehta A, Qureshi H, Avery P, Yorston D, Laidlaw DA, et al. Phenotype and outcomes of phakic versus pseudophakic primary rhegmatogenous retinal detachments: cataract or cataract surgery related? Am J Ophthalmol. 2021;222:318–27. https://linkinghub.elsevier.com/retrieve/pii/S0002939420305341.
Lois N, Wong D. Pseudophakic retinal detachment. Surv Ophthalmol. 2003;48:467–87. https://linkinghub.elsevier.com/retrieve/pii/S0039625703000833.
Mahroo OA, Dybowski R, Wong R, Williamson TH. Characteristics of rhegmatogenous retinal detachment in pseudophakic and phakic eyes. Eye. 2012;26:1114–21. http://www.nature.com/articles/eye2012112.
Kaweri L, Wavikar C, James E, Pandit P, Bhuta N. Review of current status of refractive lens exchange and role of dysfunctional lens index as its new indication. Indian J Ophthalmol. 2020;68:2797. https://journals.lww.com/ijo/Fulltext/2020/68120/Review_of_current_status_of_refractive_lens.25.aspx.
McLaughlin MD, Hwang JC. Trends in vitreoretinal procedures for medicare beneficiaries, 2000 to 2014. Ophthalmology. 2017;124:667–73. https://linkinghub.elsevier.com/retrieve/pii/S0161642016318437.
Fischer CV, Kulanga M, Hoerauf H. Trends in der Ablatiochirurgie. Ophthalmologe. 2018;115:663–8. https://doi.org/10.1007/s00347-017-0559-y.
Sharma YR, Karunanithi S, Azad RV, Vohra R, Pal N, Singh DV. et al. Functional and anatomic outcome of scleral buckling versus primary vitrectomy in pseudophakic retinal detachment. Acta Ophthalmol Scand. 2005;83:293–7. https://doi.org/10.1111/j.1600-0420.2005.00461.x.
Wu W-C, Chen M-T, Hsu S-Y, Chang C-W. Management of pseudophakic retinal detachment with undetectable retinal breaks. Ophthalmic Surg Lasers Imaging Retin. 2002;33:314–8.
Zhou C, Zheng Z, Qiu Q. Pars plana vitrectomy with 360° versus localized laser retinopexy in the management of retinal detachment with undetected breaks intraoperatively: a retrospective, comparative, interventional study. Lasers Med Sci. 2017;32:583–9. https://doi.org/10.1007/s10103-017-2152-7.
Joseph DP, Ryan EH, Ryan CM, Forbes NJK, Wagley S, Yonekawa Y, et al. Primary retinal detachment outcomes study: pseudophakic retinal detachment outcomes. Ophthalmology. 2020;127:1507–14. https://linkinghub.elsevier.com/retrieve/pii/S0161642020304280.
Walter P, Hellmich M, Baumgarten S, Schiller P, Limburg E, Agostini H. et al. Vitrectomy with and without encircling band for pseudophakic retinal detachment: VIPER Study Report No 2—main results. Br J Ophthalmol. 2017;101:712–8. https://doi.org/10.1136/bjophthalmol-2016-309240.
Machemer R, Thomas A, Freeman HM, Alexander RI, John SL, Ronald MM. An updated classification of retinal detachment with proliferative vitreoretinopathy. Am J Ophthalmol. 1991;112:159–65.
Moussa G, Bassilious K, Mathews N. A novel excel sheet conversion tool from Snellen fraction to LogMAR including ‘counting fingers’, ‘hand movement’, ‘light perception’ and ‘no light perception’ and focused review of literature of low visual acuity reference values. Acta Ophthalmol. 2021;99:aos.14659. https://doi.org/10.1111/aos.14659.
Stangos AN, Petropoulos IK, Brozou CG, Kapetanios AD, Whatham A, Pournaras CJ. Pars-plana vitrectomy alone vs vitrectomy with scleral buckling for primary rhegmatogenous pseudophakic retinal detachment. Am J Ophthalmol. 2004;138:952–8. https://linkinghub.elsevier.com/retrieve/pii/S0002939404008360.
Moussa G, Kalogeropoulos D, Ch’ng SW, Lett KS, Mitra A, Tyagi AK. et al. Effect of deprivation and ethnicity on primary macula-on retinal detachment repair success rate and clinical outcomes: A study of 568 patients. PLoS One. 2021;16:e0259714 https://doi.org/10.1371/journal.pone.0259714.
Moussa G, Qadir MO, Ch’ng SW, Lett KS, Mitra A, Tyagi AK. et al. Sustained impact of COVID-19 on primary retinal detachment repair in a tertiary eye hospital from March to December 2020. Spektrum Augenheilkd. 2023;37:1–8. https://doi.org/10.1007/s00717-022-00521-0.
Moussa G, Kalogeropoulos D, Wai Ch’ng S, Lett KS, Mitra A, Tyagi AK, et al. The effect of supervision and out-of-hours surgery on the outcomes of primary macula-on retinal detachments operated by vitreoretinal fellows: a review of 435 surgeries. Ophthalmologica. 2022;245:239–48. https://www.karger.com/Article/FullText/517879.
Moussa G, Tadros M, Ch’ng SW, Sharma A, Lett KS, Mitra A. et al. Outcomes of Heavy Silicone Oil (Densiron) compared to Silicone Oil in primary rhegmatogenous retinal detachment: a multivariable regression model. Int J Retin Vitreous. 2022;8:61 https://doi.org/10.1186/s40942-022-00413-0.
Jalil A, Ho WO, Charles S, Dhawahir-Scala F, Patton N. Iatrogenic retinal breaks in 20-G versus 23-G pars plana vitrectomy. Graefe’s Arch Clin Exp Ophthalmol. 2013;251:1463–7.
le Rouic J-F, Becquet F, Ducournau D. Does 23-gauge sutureless vitrectomy modify the risk of postoperative retinal detachment after macular surgery? Retina. 2011;31:902–8.
Dirani A, Antaki F, Rhéaume MA, Gauthier D, Corriveau L, Arbour JD, et al. 360-degree intra-operative laser retinopexy for the prevention of retinal re-detachment in patients treated with primary pars plana vitrectomy. Graefes Arch Clin Exp Ophthalmol. 2020;258:249–56.
Iwase T, Jo Y-J, Oveson BC. Effect of prophylactic 360° laser treatment for prevention of retinal detachment after phacovitrectomy: (Prophylactic 360° laser treatment for prevention of retinal detachment). BMC Ophthalmol. 2013;13:77. https://doi.org/10.1186/1471-2415-13-77.
Bilgin AB, Dogan ME, Aysun B, Apaydın KC. Pars plana vitrectomy with or without intraoperative 360° peripheral endolaser for rhegmatogenous retinal detachment treatment. Int Ophthalmol. 2019;39:1687–94.
Wang JC, Ryan EH, Ryan C, Kakulavarapu S, Mardis PJ, Rodriguez M, et al. Factors associated with the use of 360-degree laser retinopexy during primary vitrectomy with or without scleral buckle for rhegmatogenous retinal detachment and impact on surgical outcomes (pro study report number 4). Retina. 2020;40:2070–6.
Mathai M, Godwin KS, Albarracin J, Levinson J, Broderick K, Melamud A. 360 degree endolaser versus focal endolaser in primary rhegmatogenous retinal detachment repair. Retina. 2022;42:2046–50.
Comaratta MR, Chang S. Perfluorocarbon liquids in the management of complicated retinal detachments. Curr Opin Ophthalmol. 1991;2:291–8.
Anteby R, Barzelay A, Barak A. Vitrectomy in patients 85 years of age and older: Surgical outcomes and visual prognosis. Clin Interv Aging. 2018;13:243–9.
Ross WH. Visual recovery after macula-off retinal detachment. Eye. 2002;16:440–6.
Park DH, Choi KS, Sun HJ, Lee SJ. Factors associated with visual outcome after macula-off rhegmatogenous retinal detachment surgery. Retina. 2018;38:137–47.
Author information
Authors and Affiliations
Contributions
All authors have made substantial contributions to the following: (1) the conception and design of the study, or acquisition of data, or analysis and interpretation of data, (2) drafting the article or revising it critically for important intellectual content, (3) final approval of the version to be submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was registered and approved by our local clinical effectiveness team (Clinical Effectiveness Department, Manchester Royal Eye Hospital). As this was a retrospective anonymized study, as per our local protocol from our Clinical Effectiveness Department, and as per national guidelines from the National Code of Clinical Research, and the Health Research Authority (HRA), this study has ethical approval exemption. All procedures were completed prior to the design of this study. Patients were diagnosed and treated according to local guidelines and agreements and written consent from patients was acquired prior to all procedures as clinically indicated. This study does not report on the use of new or experimental protocols.
Consent for publication
Patients and the public were not involved in this study due to its retrospective design.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cristescu, IE., Ivanova, T., Moussa, G. et al. The impact of 360-laser barricade on outcomes of vitrectomy for pseudophakic retinal detachment; The Manchester Pseudophakic Retinal Detachment Study. Eye 37, 3221–3227 (2023). https://doi.org/10.1038/s41433-023-02495-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02495-y
This article is cited by
-
Expansile gas concentration in primary pseudophakic retinal detachment repair, effect on intraocular pressure and outcomes; the Manchester Pseudophakic Retinal Detachment Study
Graefe's Archive for Clinical and Experimental Ophthalmology (2023)