Abstract
Background
Few studies have used multiple measurements of fasting plasma glucose (FPG) to examine the impact of long-term FPG trajectory patterns on lifetime risk of cardiovascular disease (CVD). We aimed to identify the long-term patterns in FPG trajectories and to estimate the lifetime risk of CVD according to FPG trajectories.
Methods
Individuals free of CVD at index ages 35 (n = 72,324), 45 (n = 62,049), and 55 (n = 38,113) years were included. FPG concentrations were measured in 2006, 2008, and 2010. The FPG trajectories were identified by latent mixture modeling. The modified Kaplan-Meier method was used to calculate lifetime risk of CVD.
Results
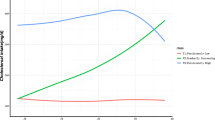
We identified five distinct FPG trajectories and named them according to FPG range and changing pattern over time: low-stable, moderate-stable, moderate-increasing, elevated-decreasing, and elevated-stable. At index age 35 years, we documented 3110 CVD events in men during 371,219 person-years of follow-up and 357 CVD events in women during 107,447 person-years of follow-up. Among all participants, the elevated-stable FPG pattern experienced the highest lifetime risk of CVD (44.8%, 95% CI: 37.8–51.9%), low-stable pattern was lowest (24.3%, 95% CI: 23.3–25.2%). At index age 55 years, although the elevated-stable and elevated-decreasing FPG patterns had similar original FPG concentrations, individuals with elevated-decreasing pattern (30.0%, 95% CI: 23.9–36.1%) had approximately one-third less lifetime risk of CVD than those with elevated-stable pattern (43.6%, 95% CI: 31.8–55.3%).
Conclusions
FPG trajectories were significantly associated with the lifetime risk of CVD. Both decrease in FPG over time and consistently lower FPG over 4 years were associated with lower lifetime risk of CVD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Collaborators GBDRF. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392:1923–94. https://doi.org/10.1016/S0140-6736(18)32225-6.
Collaborators GBDCoD. Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392:1736–88. https://doi.org/10.1016/S0140-6736(18)32203-7.
Berry JD, Dyer A, Cai X, Garside DB, Ning H, Thomas A, et al. Lifetime risks of cardiovascular disease. N. Engl J Med. 2012;366:321–9. https://doi.org/10.1056/NEJMoa1012848.
Wang Y, Liu J, Wang W, Wang M, Qi Y, Xie W, et al. Lifetime risk for cardiovascular disease in a Chinese population: the Chinese Multi-Provincial Cohort Study. Eur J Prev Cardiol. 2015;22:380–8. https://doi.org/10.1177/2047487313516563.
Park C, Guallar E, Linton JA, Lee DC, Jang Y, Son DK, et al. Fasting glucose level and the risk of incident atherosclerotic cardiovascular diseases. Diabetes Care. 2013;36:1988–93. https://doi.org/10.2337/dc12-1577.
Fox CS, Pencina MJ, Wilson PW, Paynter NP, Vasan RS, D’Agostino RB Sr. Lifetime risk of cardiovascular disease among individuals with and without diabetes stratified by obesity status in the Framingham heart study. Diabetes Care. 2008;31:1582–4. https://doi.org/10.2337/dc08-0025.
Lloyd-Jones DM, Leip EP, Larson MG, D’Agostino RB, Beiser A, Wilson PW, et al. Prediction of lifetime risk for cardiovascular disease by risk factor burden at 50 years of age. Circulation. 2006;113:791–8. https://doi.org/10.1161/CIRCULATIONAHA.105.548206.
Song M, Hu FB, Wu K, Must A, Chan AT, Willett WC, et al. Trajectory of body shape in early and middle life and all cause and cause specific mortality: results from two prospective US cohort studies. BMJ. 2016;353:i2195 https://doi.org/10.1136/bmj.i2195.
Franklin JM, Shrank WH, Pakes J, Sanfelix-Gimeno G, Matlin OS, Brennan TA, et al. Group-based trajectory models: a new approach to classifying and predicting long-term medication adherence. Med Care. 2013;51:789–96. https://doi.org/10.1097/MLR.0b013e3182984c1f.
Wang C, Yuan Y, Zheng M, Pan A, Wang M, Zhao M, et al. Association of age of onset of hypertension with cardiovascular diseases and mortality. J Am Coll Cardiol. 2020;75:2921–30. https://doi.org/10.1016/j.jacc.2020.04.038.
Wu Z, Jin C, Vaidya A, Jin W, Huang Z, Wu S, et al. Longitudinal patterns of blood pressure, incident cardiovascular events, and all-cause mortality in normotensive diabetic people. Hypertension. 2016;68:71–77. https://doi.org/10.1161/HYPERTENSIONAHA.116.07381.
Jin C, Chen S, Vaidya A, Wu Y, Wu Z, Hu FB, et al. Longitudinal change in fasting blood glucose and myocardial infarction risk in a population without diabetes. Diabetes Care. 2017;40:1565–72. https://doi.org/10.2337/dc17-0610.
Wang L, Cui L, Wang Y, Vaidya A, Chen S, Zhang C, et al. Resting heart rate and the risk of developing impaired fasting glucose and diabetes: the Kailuan prospective study. Int J Epidemiol. 2015;44:689–99. https://doi.org/10.1093/ije/dyv079.
Wang L, Lee Y, Wu Y, Zhang X, Jin C, Huang Z, et al. A prospective study of waist circumference trajectories and incident cardiovascular disease in China: the Kailuan Cohort Study. Am J Clin Nutr. 2021;113:338–47. https://doi.org/10.1093/ajcn/nqaa331.
Tunstall-Pedoe H, Kuulasmaa K, Amouyel P, Arveiler D, Rajakangas AM, Pajak A. Myocardial infarction and coronary deaths in the World Health Organization MONICA Project. Registration procedures, event rates, and case-fatality rates in 38 populations from 21 countries in four continents. Circulation. 1994;90:583–612. https://doi.org/10.1161/01.cir.90.1.583.
Stroke-1989. Recommendations on stroke prevention, diagnosis, and therapy. Report of the WHO Task Force on Stroke and other Cerebrovascular Disorders. Stroke. 1989;20:1407–31. https://doi.org/10.1161/01.str.20.10.1407.
Jones BL, Nagin DS, Roeder KA. SAS procedure based on mixture models for estimating developmental trajectories. Sociol Methods Res. 2001;29:374–93.
Odgers DSNCL. Group-based trajectory modeling in clinical research. Ann. Rev. Clin. Psychol. 2010;6:109–38.
Beiser A, D’Agostino RB,Sr, Seshadri S, Sullivan LM, Wolf PA. Computing estimates of incidence, including lifetime risk: Alzheimer’s disease in the Framingham Study. The Practical Incidence Estimators (PIE) macro. Stat Med. 2000;19:1495–522. https://doi.org/10.1002/(sici)1097-0258(20000615/30)19:11/123.0.co;2-e.
Lawes CM, Parag V, Bennett DA, Suh I, Lam TH, Whitlock G, et al. Blood glucose and risk of cardiovascular disease in the Asia Pacific region. Diabetes Care. 2004;27:2836–42. https://doi.org/10.2337/diacare.27.12.2836.
Preiss D, Welsh P, Murray HM, Shepherd J, Packard C, Macfarlane P, et al. Fasting plasma glucose in non-diabetic participants and the risk for incident cardiovascular events, diabetes, and mortality: results from WOSCOPS 15-year follow-up. Eur Heart J. 2010;31:1230–6. https://doi.org/10.1093/eurheartj/ehq095.
Sinha A, Ning H, Ahmad FS, Bancks MP, Carnethon MR, O’Brien MJ, et al. Association of fasting glucose with lifetime risk of incident heart failure: the Lifetime Risk Pooling Project. Cardiovasc Diabetol. 2021;20:66 https://doi.org/10.1186/s12933-021-01265-y.
Streiner DL. Breaking up is hard to do: the heartbreak of dichotomizing continuous data. Can J Psychiatry. 2002;47:262–6. https://doi.org/10.1177/070674370204700307.
Yuan Z, Yang Y, Wang C, Liu J, Sun X, Liu Y, et al. Trajectories of long-term normal fasting plasma glucose and risk of coronary heart disease: a prospective cohort study. J Am Heart Assoc. 2018;7. https://doi.org/10.1161/JAHA.117.007607.
Ogata S, Watanabe M, Kokubo Y, Higashiyama A, Nakao YM, Takegami M, et al. Longitudinal trajectories of fasting plasma glucose and risks of cardiovascular diseases in middle age to elderly people within the general Japanese population: the Suita Study. J Am Heart Assoc. 2019;8:e010628 https://doi.org/10.1161/JAHA.118.010628.
Edwards A, Elwyn G, Mulley A. Explaining risks: turning numerical data into meaningful pictures. BMJ. 2002;324:827–30. https://doi.org/10.1136/bmj.324.7341.827.
Edwards A, Elwyn G, Stott N. Communicating risk reductions. Researchers should present results with both relative and absolute risks. BMJ. 1999;318:603.
Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;140:e596–e646. https://doi.org/10.1161/CIR.0000000000000678.
Timmis A, Townsend N, Gale CP, Torbica A, Lettino M, Petersen SE, et al. European Society of Cardiology: cardiovascular disease statistics 2019. Eur Heart J. 2020;41:12–85. https://doi.org/10.1093/eurheartj/ehz859.
Decode Study Group EDEG. Is the current definition for diabetes relevant to mortality risk from all causes and cardiovascular and noncardiovascular diseases? Diabetes Care. 2003;26:688–96. https://doi.org/10.2337/diacare.26.3.688.
Meigs JB, Nathan DM, D’Agostino RB Sr, Wilson PW, Framingham Offspring S. Fasting and postchallenge glycemia and cardiovascular disease risk: the Framingham Offspring Study. Diabetes Care. 2002;25:1845–50. https://doi.org/10.2337/diacare.25.10.1845.
Sui X, Jackson AS, Church TS, Lee DC, O’Connor DP, Liu J, et al. Effects of cardiorespiratory fitness on aging: glucose trajectory in a cohort of healthy men. Ann Epidemiol. 2012;22:617–22. https://doi.org/10.1016/j.annepidem.2012.05.005.
Li G, Zhang P, Wang J, An Y, Gong Q, Gregg EW, et al. Cardiovascular mortality, all-cause mortality, and diabetes incidence after lifestyle intervention for people with impaired glucose tolerance in the Da Qing Diabetes Prevention Study: a 23-year follow-up study. Lancet Diabetes Endocrinol. 2014;2:474–80. https://doi.org/10.1016/S2213-8587(14)70057-9.
O’Connor EA, Evans CV, Rushkin MC, Redmond N, Lin JS. Behavioral counseling to promote a healthy diet and physical activity for cardiovascular disease prevention in adults with cardiovascular risk factors: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2020;324:2076–94. https://doi.org/10.1001/jama.2020.17108.
Salas-Salvado J, Diaz-Lopez A, Ruiz-Canela M, Basora J, Fito M, Corella D, et al. Effect of a lifestyle intervention program with energy-restricted mediterranean diet and exercise on weight loss and cardiovascular risk factors: one-year results of the PREDIMED-plus trial. Diabetes Care. 2019;42:777–88. https://doi.org/10.2337/dc18-0836.
Author information
Authors and Affiliations
Contributions
LS, DL, YT, and SW conceived the study. LS, DL, YT, SW, and YW contributed to the study design. SW and SC prepared and cleaned the data. LS, LW, DL, and YY conducted the data analysis. DL, LS and YT drafted the manuscript. LS, DL, YT, SW, YW, and YH critically revised the manuscript for important intellectual content. All authors approved the final version of the manuscript. YT and SW act as guarantors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, D., Song, L., Wang, L. et al. Association of fasting plasma glucose trajectory with lifetime risk of cardiovascular disease. Eur J Clin Nutr 77, 335–341 (2023). https://doi.org/10.1038/s41430-022-01243-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-022-01243-x