Abstract
Objective
Although previous epidemiological studies have demonstrated that serum uric acid (SUA) is associated with major depressive disorder (MDD), these analyses are prone to biases. Here, we applied the Mendelian Randomization approach to determine whether SUA is causally associated with MDD.
Methods
We conducted a meta-analysis to evaluate the relationship between SUA and MDD, then applied summary data from the Global Urate Genetics Consortium and the Psychiatric Genomics Consortium to estimate their causal effect using a two-sample bidirectional Mendelian Randomization (MR) analysis. Thereafter, the causal effect was further researched using genetic risk scores (GRS) as instrumental variables (IVs).
Results
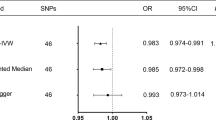
Results of a meta-analysis of articles comprising 6975 and 13,589 MDD patients and controls, respectively, revealed that SUA was associated with MDD (SMD = −0.690, 95% CI: −0.930 to −0.440, I2 = 97.4%, P < 0.001). In addition, the five MR methods revealed no causal relationship existed between SUA and MDD, which corroborated the results obtained via the GRS approach.
Conclusion
This paper found little evidence that this association between SUA and MDD is casual. Genetically, there was no significant causal association between SUA and MDD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
All datasets used in this study are publicly available, included in the main manuscript or its supplementary information files.
Code availability
The codes used for all analyses are available on request.
References
Otte C, Gold SM, Penninx BW, Pariante CM, Etkin A, Fava M, et al. Major depressive disorder. Nat Rev Dis Prim. 2016;2:16065.
Daniel HG, Jonathan F. Genetics and genomics of psychiatric disease. Science. 2015;349:1489–1494.
Ronald CK, Evelyn JB. The epidemiology of depression across cultures. Annu Rev Public Health. 2013;34:119–138.
Ron de G, Margreet ten H, Marlous T, Saskia van D. First-incidence of DSM-IV mood, anxiety and substance use disorders and its determinants: results from the Netherlands Mental Health Survey and Incidence Study-2. J Affect Disord. 2013;149:100–107.
Evelyn B, Laura HA, Irving H, Nancy AS, Jordi A, Giovanni de G, et al. Cross-national epidemiology of DSM-IV major depressive episode. BMC Med. 2011;9:90.
Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet (London, England) 2015;386:743-800.
Gilles P, Antonio S, Patrik V. Brain mechanisms for emotional influences on perception and attention: what is magic and what is not. Biol Psychol. 2013;92:492–512.
Edward C, Guy MG, Seena F. Risks of all-cause and suicide mortality in mental disorders: a meta-review. World Psychiatry. 2014;13:153–160.
Camougrand N, Rigoulet M. Aging and oxidative stress: studies of some genes involved both in aging and in response to oxidative stress. Respiration Physiol. 2001;128:393–401.
de Melo LGP, Nunes SOV, Anderson G, Vargas HO, Barbosa DS, Galecki. P, et al. Shared metabolic and immune-inflammatory, oxidative and nitrosative stress pathways in the metabolic syndrome and mood disorders. Prog Neuropsychopharmacol Biol Psychiatry. 2017;78:34–50.
Sarandol A, Sarandol E, Eker SS, Erdinc S, Vatansever E, Kirli S. Major depressive disorder is accompanied with oxidative stress: short-term antidepressant treatment does not alter oxidative–antioxidative systems. Hum Psychopharmacol: Clin Exp. 2007;22:67–73.
Tao R, Li H. High serum uric acid level in adolescent depressive patients. J Affect Disord. 2015;174:464–466.
Bartoli F, Burnstock G, Crocamo C, Carra G. Purinergic Signaling and Related Biomarkers in Depression. Brain Sci. 2020;10.
Mazzali M, Hughes J, Kim YG, Jefferson JA, Kang DH, Gordon KL, et al. Elevated uric acid increases blood pressure in the rat by a novel crystal-independent mechanism. Hypertension. 2001;38:1101–1106.
Capuron L, Su S, Miller AH, Bremner JD, Goldberg J, Vogt GJ, et al. Depressive symptoms and metabolic syndrome: is inflammation the underlying link? Biol Psychiatry. 2008;64:896–900.
Wium-Andersen MK, Ørsted DD, Nordestgaard BG. Elevated C-reactive protein and late-onset bipolar disorder in 78 809 individuals from the general population. Br J Psychiatry. 2016;208:138–145.
Lucca G, Comim CM, Valvassori SS, Réus GZ, Vuolo F, Petronilho F, et al. Increased oxidative stress in submitochondrial particles into the brain of rats submitted to the chronic mild stress paradigm. J Psychiatr Res. 2009;43:864–869.
Ames BN, Cathcart R, Schwiers E, Hochstein P. Uric acid provides an antioxidant defense in humans against oxidant- and radical-caused aging and cancer: a hypothesis. Proc Natl Acad Sci USA. 1981;78:6858–6862.
Gene LB, Jackilen S, Balz F, Jeffrey AK, Joseph FQ. Uric acid as a CNS antioxidant. J Alzheimer’s Dis. 2010;19:1331–1336.
Bartoli F, Trotta G, Crocamo C, Malerba MR, Clerici M, Carra G. Antioxidant uric acid in treated and untreated subjects with major depressive disorder: a meta-analysis and meta-regression. Eur Arch Psychiatry Clin Neurosci. 2018;268:119–127.
Catherine NB, Mariska B, Peter GS, Harold S, Brenda WJHP. Uric acid in major depressive and anxiety disorders. J Affect Disord. 2018;225:684–690.
Wium-Andersen MK, Kobylecki CJ, Afzal S, Nordestgaard BG. Association between the antioxidant uric acid and depression and antidepressant medication use in 96 989 individuals. Acta Psychiatr Scandinavica. 2017;136:424–433.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. eLife. 2018;7.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25:603–605.
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–1558.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–560.
Kottgen A, Albrecht E, Teumer A, Vitart V, Krumsiek J, Hundertmark C, et al. Genome-wide association analyses identify 18 new loci associated with serum urate concentrations. Nat Genet. 2013;45:145–154.
Efstathiadou A, Gill D, McGrane F, Quinn T, Dawson J. Genetically Determined Uric Acid and the Risk of Cardiovascular and Neurovascular Diseases: A Mendelian Randomization Study of Outcomes Investigated in Randomized Trials. J Am Heart Assoc. 2019;8:e012738.
Luo Q, Wen Z, Li Y, Chen Z, Long X, Bai Y, Huang S, et al. Assessment Causality in Associations Between Serum Uric Acid and Risk of Schizophrenia: A Two-Sample Bidirectional Mendelian Randomization Study. Clin Epidemiol. 2020;12:223–233.
Keenan T, Zhao W, Rasheed A, Ho WK, Malik R, Felix JF, Young R, et al. Causal Assessment of Serum Urate Levels in Cardiometabolic Diseases Through a Mendelian Randomization Study. J Am Coll Cardiol. 2016;67:407–416.
Tang B, Yuan S, Xiong Y, He Q, Larsson SC. Major depressive disorder and cardiometabolic diseases: a bidirectional Mendelian randomisation study. Diabetologia. 2020.
Howard DM, Adams MJ, Clarke TK, Hafferty JD, Gibson J, Shirali M, et al. Genome-wide meta-analysis of depression identifies 102 independent variants and highlights the importance of the prefrontal brain regions. Nat Neurosci. 2019;22:343–352.
Pierce BL, Ahsan H, Vanderweele TJ. Power and instrument strength requirements for Mendelian randomization studies using multiple genetic variants. Int J Epidemiol. 2011;40:740–752.
Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol. 2015;44:512–525.
Bowden J, Davey, Smith G, Haycock PC, Burgess S. Consistent Estimation in Mendelian Randomization with Some Invalid Instruments Using a Weighted Median Estimator. Genet Epidemiol. 2016;40:304–314.
Hartwig FP, Davey Smith G, Bowden J. Robust inference in summary data Mendelian randomization via the zero modal pleiotropy assumption. Int J Epidemiol. 2017;46:1985–1998.
Lewis CM, Vassos E. Prospects for using risk scores in polygenic medicine. Genome Med. 2017;9:96.
Walter S, Mejía-Guevara I, Estrada K, Liu SY, Glymour MM. Association of a Genetic Risk Score With Body Mass Index Across Different Birth Cohorts. Jama. 2016;316:63–69.
Meng X, Huang X, Deng W, Li J, Li T. Serum uric acid a depression biomarker. PLoS One. 2020;15:e0229626.
Sohn H, Kwon M-S, Lee S-W, Oh J, Kim M-K, Lee S-H, et al. Effects of Uric Acid on the Alterations of White Matter Connectivity in Patients with Major Depression. Psychiatry Investig. 2018;15:593–601.
Oliveira SR, Kallaur AP, Lopes J, Colado Simao AN, Vissoci Reiche EM, Delicato de Almeida ER, et al. Insulin resistance, atherogenicity, and iron metabolism in multiple sclerosis with and without depression: Associations with inflammatory and oxidative stress biomarkers and uric acid. Psychiatry Res. 2017;250:113–120.
Peng Y-F, Xiang Y, Wei Y-S. The significance of routine biochemical markers in patients with major depressive disorder. Sci Rep. 2016;6.
Wiener C, Rassier GT, Kaster MP, Jansen K, Pinheiro RT, Klamt F, et al. Gender-based differences in oxidative stress parameters do not underlie the differences in mood disorders susceptibility between sexes. Eur Psychiatry. 2014;29:58–63.
Wen S, Cheng M, Wang H, Yue J, Wang H, Li G, et al. Serum uric acid levels and the clinical characteristics of depression. Clin Biochem. 2012;45:49–53.
Yanik M, Erel O, Kati M. The relationship between potency of oxidative stress and severity of depression. Acta Neuropsychiatrica. 2004;16:200–203.
Kotan VO, Sarandol E, Kirhan E, Ozkaya G, Kirli S. Effects of long-term antidepressant treatment on oxidative status in major depressive disorder: a 24-week follow-up study. Prog Neuropsychopharmacol Biol Psychiatry. 2011;35:1284–1290.
Chaudhari K, Khanzode S, Khanzode S, Dakhale G, Saoji A, Sarode S. Clinical correlation of alteration of endogenous antioxidant-uric acid level in major depressive disorder.pdf. 2010.
Mondin TC, Cardoso TDA, Moreira FP, Wiener C, Oses JP, de Mattos Souza LD, et al. Circadian preferences, oxidative stress and inflammatory cytokines in bipolar disorder: A community study. J Neuroimmunol. 2016;301:23–29.
Wang L, Song R, Chen Z, Wang J, Ling F. Prevalence of depressive symptoms and factors associated with it in type 2 diabetic patients: a cross-sectional study in China. BMC Public Health 2015;15.
Bartoli F, Crocamo C, Gennaro GM, Castagna G, Trotta G, Clerici M, et al. Exploring the association between bipolar disorder and uric acid: A mediation analysis. J Psychosom Res. 2016;84:56–59.
Li Y, Zhao L, Yu D, Ding G. Associations between serum uric acid and depression among middle-aged and elderly participants in China. Psychol Health Med. 2019;24:1277–1286.
Kobrosly R, van Wijngaarden E. Associations between immunologic, inflammatory, and oxidative stress markers with severity of depressive symptoms: an analysis of the 2005-2006 National Health and Nutrition Examination Survey. Neurotoxicology. 2010;31:126–133.
Black CN, Bot M, Scheffer PG, Snieder H, Penninx BWJH. Uric acid in major depressive and anxiety disorders. J Affect Disord. 2018;225:684–690.
Li G, Miao J, Sun W, Song X, Lan Y, Zhao X, et al. Lower Serum Uric Acid Is Associated With Post-Stroke Depression at Discharge. Front Psychiatr. 2020;11.
Gu Y, Han B, Wang L, Chang Y, Zhu L, Ren W, et al. Low Serum Levels of Uric Acid are Associated With Development of Poststroke Depression. Medicine. 2015;94:e1897.
Kesebir S, Yaylaci ET, Suner O, Gultekin BK. Uric acid levels may be a biological marker for the differentiation of unipolar and bipolar disorder: The role of affective temperament. J Affect Disord. 2014;165:131–134.
Wigner P, Czarny P, Galecki P, Su K-P, Sliwinski T. The molecular aspects of oxidative & nitrosative stress and the tryptophan catabolites pathway (TRYCATs) as potential causes of depression. Psychiatry Res. 2018;262:566–574.
Gałecki P, Szemraj J, Bieńkiewicz M, Zboralski K, Gałecka E. Oxidative stress parameters after combined fluoxetine and acetylsalicylic acid therapy in depressive patients. Hum Psychopharmacol. 2009;24:277–286.
Morris G, Berk M, Klein H, Walder K, Galecki P, Maes M. Nitrosative Stress, Hypernitrosylation, and Autoimmune Responses to Nitrosylated Proteins: New Pathways in Neuroprogressive Disorders Including Depression and Chronic Fatigue Syndrome. Mol Neurobiol. 2017;54:4271–4291.
Maes M, Mihaylova I, Kubera M, Uytterhoeven M, Vrydags N, Bosmans E. Coenzyme Q10 deficiency in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) is related to fatigue, autonomic and neurocognitive symptoms and is another risk factor explaining the early mortality in ME/CFS due to cardiovascular disorder. Neuro Endocrinol Lett. 2009;30:470–476.
Kodydková J, Vávrová L, Zeman M, Jirák R, Macásek J, Stanková B, et al. Antioxidative enzymes and increased oxidative stress in depressive women. Clin Biochem. 2009;42:1368–1374.
Gautam M, Agrawal M, Gautam M, Sharma P, Gautam A, Gautam S. Role of antioxidants in generalised anxiety disorder and depression. Indian J Psychiatry. 2012;54:244–247.
Acknowledgements
We would like to acknowledge the Global Urate Genetics Consortium (GUGC) and the Psychiatric Genomics Consortium (PGC) for supplying the summary data. This study was funded by the Major Project of Guangxi Innovation Driven (AA18118016), National Key Research and Development Program of China (2017YFC0908000), Scientific Research and Technology Development Program of Guangxi (15277004).
Author information
Authors and Affiliations
Contributions
ZC and SL designed research; YB and JL conducted research; JL and ZM analyzed data, and ML, SX and SSH wrote the paper. ZC had primary responsibility for the final content. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, Z., Liang, S., Bai, Y. et al. Serum uric acid is not associated with major depressive disorder in European and South American populations: a meta-analysis and two-sample bidirectional Mendelian Randomization study. Eur J Clin Nutr 76, 1665–1674 (2022). https://doi.org/10.1038/s41430-022-01165-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-022-01165-8