Abstract
Background/Objectives
The roles of potential inflammation of diet and lifestyle in the risk of insulin-related disorders are unclear. In the current study, we aimed to assess the relationship between dietary inflammation scores (DIS), lifestyle inflammation scores (LIS), and dietary and lifestyle inflammation score (DLIS) and the risk of insulin resistance (IR) and hyperinsulinemia in Tehranian adults.
Subjects/Methods
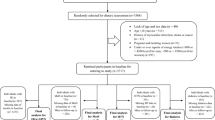
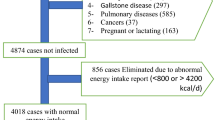
A total of 1,244 participants, aged ≥20 years, who were free of insulin-related disorders at baseline (2006–08), were followed for 3.2 years (2009–11) to ascertain the incidence of hyperinsulinemia and IR. A food frequency questionnaire was used to determine the score of DIS, LIS, and DLIS at baseline. Logistic regression models were used to determine the odds ratio (ORs) of insulin-related disorders across tertiles of DIS, LIS, and DLIS.
Results
Mean ± SD age of participants (42.7% men) was 43.0 ± 13.0 years. During the 3.2 years follow-up, the incidence of IR and hyperinsulinemia was 30.0% and 20.0%, respectively. In the multivariable model, there was a direct association between the higher score of DLIS (OR = 2.10; 95% CI: 1.17–3.74) and DIS (OR = 1.84; 95% CI: 1.09–3.11) with the risk of IR incident (P for trend <0.05). Also, the higher score of LIS was related to increased risk of IR (OR = 2.28; 95% CI: 1.19–4.37) and hyperinsulinemia (OR = 1.69; 95% CI: 1.02–2.85) (P for trend <0.05). However, no significant association was observed between the higher score of DLIS and DIS with risk of hyperinsulinemia
Conclusion
The higher inflammatory potential of diet and lifestyle, determined by DLIS, DIS, and LIS scores, were associated with a higher risk of IR. Also, individuals with a higher score of LIS are more prone to hyperinsulinemia risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The datasets analyzed in the current study are available from the corresponding author on reasonable request.
References
Utzschneider KM, Van de Lagemaat A, Faulenbach MV, Goedecke JH, Carr DB, Boyko EJ, et al. Insulin resistance is the best predictor of the metabolic syndrome in subjects with a first-degree relative with type 2 diabetes. Obes (Silver Spring) 2010;18:1781–7.
Cerf ME. Beta cell dysfunction and insulin resistance. Front Endocrinol (Lausanne). 2013;4:37.
Thomas DD, Corkey BE, Istfan NW, Apovian CM. Hyperinsulinemia: an early indicator of metabolic dysfunction. J Endocr Soc. 2019;3:1727–47.
Corkey BE. Banting lecture 2011: hyperinsulinemia: cause or consequence? Diabetes 2012;61:4–13.
Rehman K, Akash MSH. Mechanisms of inflammatory responses and development of insulin resistance: how are they interlinked? J Biomed Sci. 2016;23:87.
Wang C, Guan Y, Yang J. Cytokines in the progression of pancreatic β-cell dysfunction. Int J Endocrinol. 2010;2010:515136.
Galland L. Diet and inflammation. Nutrition in clinical practice: official publication of the American Society for Parenteral and Enteral. Nutrition 2010;25:634–40.
Calder PC, Ahluwalia N, Brouns F, Buetler T, Clement K, Cunningham K, et al. Dietary factors and low-grade inflammation in relation to overweight and obesity. Br J Nutr. 2011;106:S5–78. Suppl 3
Shivappa N, Steck SE, Hurley TG, Hussey JR, Hébert JRJPHN. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014;17:1689–96.
Tabung FK, Smith-Warner SA, Chavarro JE, Wu K, Fuchs CS, Hu FB, et al. Development and validation of an empirical dietary inflammatory index. J Nutr. 2016;146:1560–70.
Shakeri Z, Mirmiran P, Khalili-Moghadam S, Hosseini-Esfahani F, Ataie-Jafari A, Azizi F. Empirical dietary inflammatory pattern and risk of metabolic syndrome and its components: Tehran Lipid and Glucose Study. Diabetol Metab Syndr. 2019;11:16.
Denova-Gutiérrez E, Muñoz-Aguirre P, Shivappa N, Hébert JR, Tolentino-Mayo L, Batis C, et al. Dietary Inflammatory Index and Type 2 Diabetes Mellitus in Adults: The Diabetes Mellitus Survey of Mexico City. Nutrients 2018;10:385.
Lee DH, Li J, Li Y, Liu G, Wu K, Bhupathiraju S, et al. Dietary inflammatory and insulinemic potential and risk of type 2 diabetes: results from three prospective U.S. cohort studies. Diabetes Care. 2020;43:2675–2683.
Soltani S, Moslehi N, Hosseini-Esfahani F, Vafa M. The association between empirical dietary inflammatory pattern and metabolic phenotypes in overweight/obese adults. Int J Endocrinol Metab. 2018;16:e60048.
Petersen AM, Pedersen BK. The anti-inflammatory effect of exercise. J Appl Physiol (1985) 2005;98:1154–62.
Wu H, Ballantyne CM. Metabolic inflammation and insulin resistance in. Obesity 2020;126:1549–64.
Attard R, Dingli P, Doggen CJ, Cassar K, Farrugia R, Wettinger SBJOH. The impact of passive and active smoking on inflammation, lipid profile and the risk of myocardial infarction. 2017;4:e000620.
Byrd DA, Judd SE, Flanders WD, Hartman TJ, Fedirko V, Bostick RMJTJON. Development and validation of novel dietary and lifestyle inflammation scores. J Nutr. 2019;149:2206–18.
Farhadnejad H, Parastouei K, Rostami H, Mirmiran P, Azizi FJD. Syndrome M Dietary and lifestyle inflammatory scores are associated with increased risk of metabolic syndrome in Iranian adults. 2021;13:1–10.
Byrd DA, Judd SE, Flanders WD, Hartman TJ, Fedirko V, Agurs-Collins T, et al. Associations of Novel Dietary and Lifestyle Inflammation Scores With Incident Colorectal Cancer in the NIH-AARP Diet and Health Study. JNCI Cancer Spectrum. 2020;4:pkaa009.
Li Z, Gao Y, Byrd DA, Gibbs DC, Prizment AE, Lazovich D, et al. Novel dietary and lifestyle inflammation scores directly associated with all-cause, all-cancer, and all-cardiovascular disease mortality risks among women. The J Nutr. 2021;151:930–9.
Byrd DA, Judd S, Flanders WD, Hartman TJ, Fedirko V, Bostick RMJCE, et al. Associations of novel dietary and lifestyle inflammation scores with incident, sporadic colorectal adenoma. Cancer Epidemiol Biomarkers Prev.2020;29:2300–8.
Farazi M, Jayedi A, Noruzi Z, Janbozorgi N, Djafarian K, Shab-Bidar S. Association of dietary and lifestyle inflammation score with cardiorespiratory fitness. Frontiers in Nutrition. 2022;9:730841
Azizi F, Ghanbarian A, Momenan AA, Hadaegh F, Mirmiran P, Hedayati M, et al. Prevention of non-communicable disease in a population in nutrition transition: Tehran Lipid and Glucose Study phase II. Trials 2009;10:5.
Willett W. Implications of total energy intake for epidemiologic analyses. Nutritional epidemiology, 3rd ed. New York: Oxford University Press; 2013: 260–86.
Esfahani FH, Asghari G, Mirmiran P, Azizi F. Reproducibility and relative validity of food group intake in a food frequency questionnaire developed for the Tehran Lipid and Glucose Study. J Epidemiol. 2010;20:150–8.
Asghari G, Rezazadeh A, Hosseini-Esfahani F, Mehrabi Y, Mirmiran P, Azizi F. Reliability, comparative validity and stability of dietary patterns derived from an FFQ in the Tehran Lipid and Glucose Study. Br J Nutr. 2012;108:1109–17.
Mirmiran P, Esfahani FH, Mehrabi Y, Hedayati M, Azizi F. Reliability and relative validity of an FFQ for nutrients in the Tehran lipid and glucose study. Public health Nutr. 2010;13:654–62.
Byrd DA, Judd SE, Flanders WD, Hartman TJ, Fedirko V, Bostick RM. Development and validation of novel dietary and lifestyle inflammation scores. J Nutr. 2019;149: 2206–2218.
Momenan AA, Delshad M, Sarbazi N, REZAEI GN, Ghanbarian A, AZIZI F. Reliability and validity of the Modifiable Activity Questionnaire (MAQ) in an Iranian urban adult population. Arch Iran Med. 2012;15:279-82.
Ghasemi A, Tohidi M, Derakhshan A, Hasheminia M, Azizi F, Hadaegh F. Cut-off points of homeostasis model assessment of insulin resistance, beta-cell function, and fasting serum insulin to identify future type 2 diabetes: Tehran Lipid and Glucose Study. Acta diabetologica. 2015;52:905–15.
Mokhtari E, Teymoori F, Farhadnejad H, Mirmiran P, Azizi F. Development and validation of dietary and lifestyle insulinemic indices among Iranian adult population. Nutr Metab (Lond). 2022;19:5.
Holt EM, Steffen LM, Moran A, Basu S, Steinberger J, Ross JA, et al. Fruit and vegetable consumption and its relation to markers of inflammation and oxidative stress in adolescents. J Am Diet Assoc. 2009;109:414–21.
Zhu F, Du B, Xu B. Anti-inflammatory effects of phytochemicals from fruits, vegetables, and food legumes: a review. Crit Rev food Sci Nutr. 2018;58:1260–70.
Bonaccio M, Pounis G, Cerletti C, Donati MB, Iacoviello L, de Gaetano G, et al. Mediterranean diet, dietary polyphenols and low grade inflammation: results from the MOLI-SANI study. Br J Clin Pharm. 2017;83:107–13.
Farhadnejad H, Emamat H, Teymoori F, Tangestani H, Hekmatdoost A, Mirmiran P. Role of dietary approaches to stop hypertension diet in risk of metabolic syndrome: Evidence from observational and interventional studies. Int J Preventive Med. 2021;12:24.
Esfandiari S, Bahadoran Z, Mirmiran P, Tohidi M, Azizi F. Adherence to the dietary approaches to stop hypertension trial (DASH) diet is inversely associated with incidence of insulin resistance in adults: the Tehran lipid and glucose study. J Clin Biochem Nutr. 2017;61:123–9.
Esmaillzadeh A, Kimiagar M, Mehrabi Y, Azadbakht L, Hu FB, Willett WC. Dietary patterns and markers of systemic inflammation among Iranian Women. J Nutr. 2007;137:992–8.
Bawaked RA, Schröder H, Ribas-Barba L, Izquierdo-Pulido M, Pérez-Rodrigo C, Fíto M, et al. Association of diet quality with dietary inflammatory potential in youth. Food Nutr Res. 2017;61:1328961.
Lyon CJ, Law RE, Hsueh WA. Minireview: adiposity, inflammation, and atherogenesis. Endocrinology 2003;144:2195–200.
Elks CM, Francis J. Central adiposity, systemic inflammation, and the metabolic syndrome. Curr Hypertension Rep. 2010;12:99–104.
Okura T, Nakamura R, Fujioka Y, Kawamoto-Kitao S, Ito Y, Matsumoto K, et al. Body mass index ≥23 is a risk factor for insulin resistance and diabetes in Japanese people: a brief report. Plos one. 2018;13:e0201052.
Furukawa S, Fujita T, Shimabukuro M, Iwaki M, Yamada Y, Nakajima Y, et al. Increased oxidative stress in obesity and its impact on metabolic syndrome. J Clin Investig. 2017;114:1752–61.
Stadler M, Tomann L, Storka A, Wolzt M, Peric S, Bieglmayer C, et al. Effects of smoking cessation on β-cell function, insulin sensitivity, body weight, and appetite. Eur J Endocrinol. 2014;170:219–7.
Anan F, Takahashi N, Shinohara T, Nakagawa M, Masaki T, Katsuragi I, et al. Smoking is associated with insulin resistance and cardiovascular autonomic dysfunction in type 2 diabetic patients. Eur J Clin Investig. 2006;36:459–65.
Gomez-Cabrera M-C, Domenech E, Viña J. Moderate exercise is an antioxidant: upregulation of antioxidant genes by training. Free Radic Biol Med. 2008;44:126–31.
Jiménez-Pavón D, Ruiz JR, Ortega FB, Martínez-Gómez D, Moreno S, Urzanqui A, et al. Physical activity and markers of insulin resistance in adolescents: role of cardiorespiratory fitness levels—the HELENA study. Pediatr Diabetes. 2013;14:249–58.
Fischer C, Berntsen A, Perstrup L, Eskildsen P, Pedersen B. Plasma levels of interleukin‐6 and C‐reactive protein are associated with physical inactivity independent of obesity. Scand J Med Sci Sports. 2007;17:580–7.
Acknowledgements
Research reported in this publication was supported by Elite Researcher Grant Committee under award number [No.996622] from the National Institutes for Medical Research Development (NIMAD), Tehran, Iran. We express appreciation to the participants in the Tehran Lipid and Glucose Study for their enthusiastic support and to the staff of the Research Institute for Endocrine Sciences, Tehran Lipid and Glucose Study Unit, for their valuable help.
Funding
Research reported in this publication was supported by Elite Researcher Grant Committee under award number [No.996622] from the National Institute for Medical Research Development (NIMAD), Tehran, Iran.
Author information
Authors and Affiliations
Contributions
HF and FT conceptualized and designed the study. FT, EM, and HF drafted the initial manuscript; FT and EM analyzed and interpreted the data; PM and FA supervised the project; all authors have read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Written informed consent was obtained from all participants. The study protocol was approved by the ethics research committee of the Research Institute for Endocrine Sciences, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Farhadnejad, H., Teymoori, F., Mokhtari, E. et al. Higher scores of dietary and lifestyle inflammatory indices are associated with increased risk of insulin-related disorders in Iranian adults. Eur J Clin Nutr 76, 1566–1575 (2022). https://doi.org/10.1038/s41430-022-01143-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-022-01143-0
This article is cited by
-
The association of meal-specific food-based dietary inflammatory index with cardiovascular risk factors and inflammation in a sample of Iranian adults
BMC Endocrine Disorders (2023)
-
Association of dietary and lifestyle inflammation scores with muscle strength and muscle endurance among Tehranian adults
Scientific Reports (2022)