Abstract
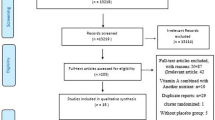
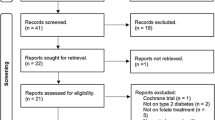
Taurine (Tau) has modulatory effects on inflammatory and oxidative stress biomarkers; however, the results of clinical studies are not comprehensive enough to determine the effect of different durations and doses of Tau supplementation on inflammatory and oxidative stress biomarkers. The current study was conducted based on the preferred reporting items for systematic reviews and meta-analyses (PRISMA) guidelines. For this purpose, PubMed/Medline, Scopus, and Embase databases were systematically searched to obtain the relevant studies published before 30th March 2021. Meta-analysis was performed on controlled clinical trials by using the random-effects method. Non-linear relationship between variables and effect size was performed using dose–response and time–response analyses. The Cochrane Collaboration’s tool was used to evaluate the quality of included studies. Tau supplementation can reduce the levels of malondialdehyde (MDA) (SMD = −1.17 µmol/l; 95% CI: −2.08, − 0.26; P = 0.012) and C-reactive protein (CRP) (SMD = −1.95 mg/l; 95% CI: −3.20, − 0.71; P = 0.002). There have been no significant effects of Tau supplementation on the levels of tumor necrosis factors-alpha (TNF-α) (SMD = −0.18 pg/ml; 95% CI: −0.56, 0.21; P = 0.368), and interleukin-6 (IL-6) (SMD = −0.49 pg/ml; 95% CI: −1.13, 0.16; P = 0.141). Besides, Tau has more alleviating effect on oxidative stress and inflammation on 56 days after supplementation (P < 0.05). Tau can decrease the levels of CRP and MDA. Based on the currently available evidence, Tau has no significant effect on the level of TNF-α and IL-6. Eight-week of Tau supplementation has more beneficial effects on inflammatory and oxidative stress biomarkers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Furman D, Campisi J, Verdin E, Carrera-Bastos P, Targ S, Franceschi C, et al. Chronic inflammation in the etiology of disease across the life span. Nat Med. 2019;25:1822–32. https://doi.org/10.1038/s41591-019-0675-0.
Khansari N, Shakiba Y, Mahmoudi M. Chronic inflammation and oxidative stress as a major cause of age-related diseases and cancer. Recent Pat Inflamm Allergy Drug Discov. 2009;3:73–80. https://doi.org/10.2174/187221309787158371.
Minoguchi K, Yokoe T, Tanaka A, Ohta S, Hirano T, Yoshino G, et al. Association between lipid peroxidation and inflammation in obstructive sleep apnoea. Eur Respir J. 2006;28:378–85. https://doi.org/10.1183/09031936.06.00084905.
Maleki V, Mahdavi R, Hajizadeh-Sharafabad F, Alizadeh M. The effects of taurine supplementation on oxidative stress indices and inflammation biomarkers in patients with type 2 diabetes: a randomized, double-blind, placebo-controlled trial. Diabetol Metab Syndr. 2020;12:9 https://doi.org/10.1186/s13098-020-0518-7.
Qaradakhi T, Gadanec LK, McSweeney KR, Abraham JR, Apostolopoulos V, Zulli A. The anti-inflammatory effect of taurine on cardiovascular disease. Nutrients. 2020;12. https://doi.org/10.3390/nu12092847.
Rosa FT, Freitas EC, Deminice R, Jordão AA, Marchini JS. Oxidative stress and inflammation in obesity after taurine supplementation: a double-blind, placebo-controlled study. Eur J Nutr. 2014;53:823–30. https://doi.org/10.1007/s00394-013-0586-7.
Bouckenooghe T, Remacle C, Reusens B. Is taurine a functional nutrient? Curr Opin Clin Nutr Metab Care. 2006;9:728–33. https://doi.org/10.1097/01.mco.0000247469.26414.55.
Murakami S. Role of taurine in the pathogenesis of obesity. Mol Nutr Food Res. 2015;59:1353–63. https://doi.org/10.1002/mnfr.201500067.
Sirdah MM. Protective and therapeutic effectiveness of taurine in diabetes mellitus: a rationale for antioxidant supplementation. Diabetes Metab Syndr. 2015;9:55–64. https://doi.org/10.1016/j.dsx.2014.05.001.
Oudit GY, Trivieri MG, Khaper N, Husain T, Wilson GJ, Liu P, et al. Taurine supplementation reduces oxidative stress and improves cardiovascular function in an iron-overload murine model. Circulation. 2004;109:1877–85. https://doi.org/10.1161/01.Cir.0000124229.40424.80.
Schaffer S, Solodushko V, Azuma J. Taurine-deficient cardiomyopathy: role of phospholipids, calcium and osmotic stress. Adv Exp Med Biol. 2000;483:57–69. https://doi.org/10.1007/0-306-46838-7_6.
Biasetti M, Dawson R Jr. Effects of sulfur containing amino acids on iron and nitric oxide stimulated catecholamine oxidation. Amino Acids. 2002;22:351–68. https://doi.org/10.1007/s007260200020.
De Carvalho FG, Galan BSM, Santos PC, Pritchett K, Pfrimer K, Ferriolli E, et al. Taurine: a potential ergogenic aid for preventing muscle damage and protein catabolism and decreasing oxidative stress produced by endurance exercise. Front Physiol. 2017;8:710–710. https://doi.org/10.3389/fphys.2017.00710.
Lu C-L, Tang S, Meng Z-J, He Y-Y, Song L-Y, Liu Y-P, et al. Taurine improves the spatial learning and memory ability impaired by sub-chronic manganese exposure. J Biomed Sci. 2014;21:51–51. https://doi.org/10.1186/1423-0127-21-51.
Shao A, Hathcock JN. Risk assessment for the amino acids taurine, L-glutamine and L-arginine. Regul Toxicol Pharmacol. 2008;50:376–99. https://doi.org/10.1016/j.yrtph.2008.01.004.
Seol S-I, Kim HJ, Choi EB, Kang IS, Lee H-K, Lee J-K, et al. Taurine protects against postischemic brain injury via the antioxidant activity of taurine chloramine. Antioxidants. 2021;10:372.
Dallak M. A synergistic protective effect of selenium and taurine against experimentally induced myocardial infarction in rats. Arch Physiol Biochem. 2017;123:344–55. https://doi.org/10.1080/13813455.2017.1347687.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;62:e1–34.
Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, et al. Cochrane handbook for systematic reviews of interventions version 6.2 [updated February 2021]. Cochrane, 2021. Available at http://training.cochrane.org/handbook. (accessed on 28 March 2021).
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336:924–6. https://doi.org/10.1136/bmj.39489.470347.AD.
Liyan C, Jie Z, Yonghua W, Xiaozhou H. Assay of ischemia-modified albumin and C-reactive protein for early diagnosis of acute coronary syndromes. J Clin Lab Anal. 2008;22:45–9. https://doi.org/10.1002/jcla.20223.
Manco M, Marcellini M, Giannone G, Nobili V. Correlation of serum TNF-alpha levels and histologic liver injury scores in pediatric nonalcoholic fatty liver disease. Am J Clin Pathol. 2007;127:954–60. https://doi.org/10.1309/6vj4dwgydu0xyj8q.
Giannoudis PV, Harwood PJ, Loughenbury P, Van Griensven M, Krettek C, Pape H-C. Correlation between IL-6 levels and the systemic inflammatory response score: can an IL-6 cutoff predict a SIRS state?. J Trauma Acute Care Surg. 2008;65:646–652.
Pande D, Negi R, Karki K, Khanna S, Khanna RS, Khanna HD. Oxidative damage markers as possible discriminatory biomarkers in breast carcinoma. Transl Res. 2012;160:411–8. https://doi.org/10.1016/j.trsl.2012.07.005.
Islambulchilar M, Asvadi I, Sanaat Z, Esfahani A, Sattari M. Effect of taurine on attenuating chemotherapy-induced adverse effects in acute lymphoblastic leukemia. J Cancer Res Ther. 2015;11:426–32. https://doi.org/10.4103/0973-1482.151933.
Lak S, Ostadrahimi A, Nagili B, Asghari-Jafarabadi M, Beigzali S, Salehi F, et al. Anti-Inflammatory effect of taurine in burned patients. Adv Pharm Bull. 2015;5:531–6. https://doi.org/10.15171/apb.2015.072.
Ahmadian M, Roshan VD, Aslani E, Stannard SR. Taurine supplementation has anti-atherogenic and anti-inflammatory effects before and after incremental exercise in heart failure. Ther Adv Cardiovasc Dis. 2017;11:185–94. https://doi.org/10.1177/1753944717711138.
Haidari F, Asadi M, Mohammadi-Asl J, Ahmadi-Angali K. Effect of weight-loss diet combined with taurine supplementation on body composition and some biochemical markers in obese women: a randomized clinical trial. Amino Acids. 2020;52:1115–24. https://doi.org/10.1007/s00726-020-02876-7.
Shirvani H, Rostamkhani F, Sobhani V. The interactive effect of taurine supplementation and intensive training protocols on serum inflammatory cytokines (IL-6 and TNF-α) levels in elite soccer players. Iran J Nutr Sci Food Technol. 2015;10:29–38.
da Silva LA, Tromm CB, Bom KF, Mariano I, Pozzi B, da Rosa GL, et al. Effects of taurine supplementation following eccentric exercise in young adults. Appl Physiol Nutr Metab. 2014;39:101–4. https://doi.org/10.1139/apnm-2012-0229.
Chupel MU, Minuzzi LG, Furtado G, Santos ML, Hogervorst E, Filaire E, et al. Exercise and taurine in inflammation, cognition, and peripheral markers of blood-brain barrier integrity in older women. Appl Physiol Nutr Metab. 2018;43:733–41. https://doi.org/10.1139/apnm-2017-0775.
Ra SG, Choi Y, Akazawa N, Ohmori H, Maeda S. Taurine supplementation attenuates delayed increase in exercise-induced arterial stiffness. Appl Physiol Nutr Metab. 2016;41:618–23. https://doi.org/10.1139/apnm-2015-0560.
Van Stijn MF, Bruins AA, Vermeulen MA, Witlox J, Teerlink T, Schoorl MG, et al. Effect of oral taurine on morbidity and mortality in elderly hip fracture patients: a randomized trial. Int J Mol Sci. 2015;16:12288–306. https://doi.org/10.3390/ijms160612288.
Shari F. Study effect of sulfur containing amino acid supplementation on oxidative stress, inflammatory markers and serum lipid in relation to obese subjects. Trop J Pharm Res. 2020;12.
Hsieh YL, Yeh YH, Lee YT, Huang CY. Effect of taurine in chronic alcoholic patients. Food Funct. 2014;5:1529–35. https://doi.org/10.1039/c3fo60597c.
Cantafora A, Mantovani A, Masella R, Mechelli L, Alvaro D. Effect of taurine administration on liver lipids in guinea pig. Experientia. 1986;42:407–8. https://doi.org/10.1007/bf02118631.
Jakaria M, Azam S, Haque ME, Jo S-H, Uddin MS, Kim I-S. et al. Taurine and its analogs in neurological disorders: focus on therapeutic potential and molecular mechanisms. Redox Biol. 2019;24:101223. https://doi.org/10.1016/j.redox.2019.101223.
Terrill JR, Pinniger GJ, Nair KV, Grounds MD, Arthur PG. Beneficial effects of high dose taurine treatment in juvenile dystrophic mdx mice are offset by growth restriction. PLoS ONE. 2017;12:e0187317. https://doi.org/10.1371/journal.pone.0187317.
Benihoud K, Esselin S, Descamps D, Jullienne B, Salone B, Bobé P, et al. Respective roles of TNF-α and IL-6 in the immune response-elicited by adenovirus-mediated gene transfer in mice. Gene Ther. 2007;14:533–44. https://doi.org/10.1038/sj.gt.3302885.
Ghandforoush-Sattari M, Mashayekhi S, Krishna CV, Thompson JP, Routledge PA. Pharmacokinetics of oral taurine in healthy volunteers. J Amino Acids. 2010;2010:346237–346237. https://doi.org/10.4061/2010/346237.
Helal I, Zerelli L, Krid M, ElYounsi F, Ben Maiz H, Zouari B, et al. Comparison of C-reactive protein and high-sensitivity C-reactive protein levels in patients on hemodialysis. Saudi J Kidney Dis Transpl. 2012;23:477–83.
Siddique YH, Ara G, Afzal M. Estimation of lipid peroxidation induced by hydrogen peroxide in cultured human lymphocytes. Dose Response. 2012;10:1–10. https://doi.org/10.2203/dose-response.10-002.Siddique.
Domijan AM, Ralić J, Radić Brkanac S, Rumora L, Žanić-Grubišić T. Quantification of malondialdehyde by HPLC-FL - application to various biological samples. Biomed Chromatogr. 2015;29:41–6. https://doi.org/10.1002/bmc.3361.
Siddique YH, Jyoti S, Naz F, Afzal M. Validation of 1-methyl-2-phenylindole method for estimating lipid peroxidation in the third instar larvae of transgenic Drosophila melanogaster (hsp70-lacZ)Bg (9.). Pharm Methods. 2012;3:94–7. https://doi.org/10.4103/2229-4708.103883.
Lin S, Hirai S, Yamaguchi Y, Goto T, Takahashi N, Tani F, et al. Taurine improves obesity-induced inflammatory responses and modulates the unbalanced phenotype of adipose tissue macrophages. Mol Nutr Food Res. 2013;57:2155–65. https://doi.org/10.1002/mnfr.201300150.
Schaffer S, Kim HW. Effects and mechanisms of taurine as a therapeutic agent. Biomol Ther. 2018;26:225–41. https://doi.org/10.4062/biomolther.2017.251.
Scicchitano BM, Sica G. The beneficial effects of taurine to counteract sarcopenia. Curr Protein Pept Sci. 2018;19:673–80. https://doi.org/10.2174/1389203718666161122113609.
Ulfig A, Leichert LI. The effects of neutrophil-generated hypochlorous acid and other hypohalous acids on host and pathogens. Cell Mol Life Sci. 2021;78:385–414. https://doi.org/10.1007/s00018-020-03591-y.
Kim C, Cha YN. Taurine chloramine produced from taurine under inflammation provides anti-inflammatory and cytoprotective effects. Amino Acids. 2014;46:89–100. https://doi.org/10.1007/s00726-013-1545-6.
Jong CJ, Ito T, Schaffer SW. The ubiquitin-proteasome system and autophagy are defective in the taurine-deficient heart. Amino Acids. 2015;47:2609–22. https://doi.org/10.1007/s00726-015-2053-7.
Anand P, Rajakumar D, Jeraud M, Felix AJ, Balasubramanian T. Effects of taurine on glutathione peroxidase, glutathione reductase and reduced glutathione levels in rats. Pak J Biol Sci. 2011;14:219–25. https://doi.org/10.3923/pjbs.2011.219.225.
Acknowledgements
The research protocol was approved and supported by the Student Research Committee, Tabriz University of Medical Sciences (grant number: 67856).
Author information
Authors and Affiliations
Contributions
Conceptualization: AHF and EF. Database searching: AHF. Screening: SP and PF. Data extraction: AHF and SMSS. Drafting of the paper: AHF, SMSS, and PF. Statistical analysis: AHF. Critical revision: AO, MAS, and EF. All the authors approved the final version to be submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Faghfouri, A.H., Seyyed Shoura, S.M., Fathollahi, P. et al. Profiling inflammatory and oxidative stress biomarkers following taurine supplementation: a systematic review and dose-response meta-analysis of controlled trials. Eur J Clin Nutr 76, 647–658 (2022). https://doi.org/10.1038/s41430-021-01010-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-021-01010-4