Abstract
Background/objectives
To evaluate serum 25(OH)D concentrations and determine a cutoff point for cardiometabolic risk in children.
Subject/methods
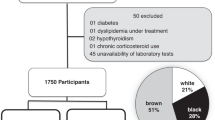
This is a cross-sectional study with a representative sample of 378 8–9-year-old children from all urban schools in the city of Viçosa, MG, Brazil. Sociodemographic data and information on lifestyle, and food consumption were collected. Biochemical evaluation included glucose, triglycerides, leptin, calcidiol [25(OH)D], and parathormone. Body composition was assessed by dual energy X-ray absorptiometry. Cardiometabolic risk was considered when nontraditional risk markers were detected, including triglyceride × glycemia index (TyG index), hyperleptinemia, and hypertriglyceridemic waist phenotype (HWP). The receiver operating characteristic curve (ROC) was used to define the cutoff point for serum 25(OH)D to predict cardiometabolic risk.
Results
25(OH)D showed better predictive capacity for grouping of cardiometabolic risk markers than for either single or paired markers. The area under the curve for grouping of risk markers was 0.636 (95% CI: 0.585, 0.685, P < 0.001). The cutoff point to predict cardiometabolic risk was defined as 32.0 ng/mL.
Conclusion
25(OH)D presented good predictive capacity for cardiometabolic risk and 25(OH)D concentration higher than 32 ng/mL was associated with a 49% reduction of cardiometabolic risk prevalence in prepubertal Brazilian children.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Norman AW. From vitamin D to hormone D: fundamentals of the vitamin D endocrine system essential for good health. Am J Clin Nutr. 2008;88:491–9.
Hilger J, Friedel A, Herr R, Rausch T, Roos F, Wahl DA, et al. A systematic review of vitamin D status in populations worldwide. Br J Nutr. 2014;111:23–45.
Cashman KD, Dowling KG, Skrabakova Z, Gonzalez-Gross M, Valtueña J, Henauw S, et al. Vitamin D deficiency in Europe: pandemic? Am J Clin Nutr. 2016;103:1033–44.
Maeda SS, Borba VZC, Camargo MBR, Silva DMW, Borges JLC, Bandeira F. Recomendações da Sociedade Brasileira de Endocrinologia e Metabologia para o diagnóstico e tratamento da hipovitaminose D. Arq Bras Endocrinol Metabol. 2014;58:411–33.
Milagres LC, Rocha NP, Filgueiras MS, Albuquerque FM, Castro APP, Pessoa MC, et al. Vitamin D insufficiency/deficiency is associated with insulin resistance in Brazilian children, regardless of body fat distribution. Public Health Nutr. 2017;20:2878–86.
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP. Endocrine Society et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96:1911–30.
Munns CF, Shaw N, Kiely M, Specker BL, Thacher TD, Ozono K, et al. Global Consensus recommendations on prevention and management of nutritional rickets. J Clin Endocrinol Metab. 2016;101:394–415.
Lips P, Duong T, Oleksik A, Black D, Cummings S, Cox D, et al. A global study of vitamin D status and parathyroid function in postmenopausal women with osteoporosis: baseline data from the multiple outcomes of raloxifene evaluation clinical trial. J Clin Endocrinol Metab. 2001;86:1212–21.
Bouillon R, Van Schoor NM, Gielen E, Boonen S, Mathieu C, Vanderschueren D, et al. Optimal vitamin D status: a critical analysis on the basis of evidence-based medicine. J Clin Endocrinol Metab. 2013;98:1283–304.
Holick MF. Vitamin D deficiency. N Engl J Med. 2007;357:266–81.
Theodoratou E, Tzoulaki I, Zgaga L, Ioannidis JP. Vitamin D and multiple health outcomes: umbrella review of systematic reviews and meta-analyses of observational studies and randomised trials. Br Med J. 2014;348:g2035.
Mandarino NR, Júnior FCM, Salgado JVL, Lages JS, Filho NS. Is vitamin D deficiency a new risk factor for cardiovascular disease? Open Cardiovasc Med J. 2015;9:40–49.
Sharifi F, Mousavinasab N, Mellati AA. Defining a cutoff point for vitamin D deficiency based on insulin resistance in children. Diabetes Metab Clin Res Rev. 2013;7:210–3.
Pourshahidi LK. Vitamin D and obesity: current perspectives and future directions. Proc Nutr Soc. 2015;74:115–24. 2015
Wamberg L, Christiansen T, Paulsen SK, Fisker S, Rask P, Rejnmark L, et al. Expression of vitamin D metabolizing enzymes in human adipose tissue – the effect of obesity and diet-induced weight loss. Int J Obes. 2013;37:651–7.
Kong J, Chen Y, Zhu G, ZHAO Q, Li YC. 1,25Dihydroxyvitamin D3 upregulates leptina expression in mouse adipose tissue. J Endocrinol. 2013;21:265–71.
Bouillon R, Carmeliet G, Lieben L, et al. Vitamin D and energy homeostasis of mice and men. Nat Rev Endocrinol. 2014;10:79–87.
Chung SJ, Lee YA, Hong H, Kang MJ, Kwon HJ, Shin CH, et al. Inverse relationship between vitamin D status and insulin resistance and the risk of impaired fasting glucose in Koren Children and adolescentes: the Joren National Health and Nutrition Examination Survey (KNHANES) 2009–2010. Public Health Nutr. 2014;17:795–802.
Jorde R, Sneve M, Emaus N, Figenschau Y, Grimnes G. Cross-sectional and longitudinal relation between serum 25-hydroxyvitamin D and body mass index: the Tromso study. Eur J Nutr. 2010;49:401–7.
Sun X, Cao ZB, Tanisawa K, Ito T, Oshima S, Ishimi Y, et al. Associations between the sérum 25(OH)D concentration and lipid profiles in Japanese men. J Atheroscler Thromb. 2015;22:355–62.
Bischoff-Ferrari HA, Giovannucci E, Willett WC, Dietrich T, Dawson-Hughes B. Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. Am J Clin Nutr. 2006;84:18–28.
Leu M, Giovannucci E. Vitamin D: epidemiology of cardiovascular risks and events. Best Pract Res Clin Endocrinol Metab. 2011;25:633–46. 2011
Shenoy M, Tuliani T, Yeeranna V, Zalawadiya S, Patel KH, Afonso L. Vitamin D deficiency is associated with hypertriglyceridemic Waist Phenotype. Circulation. 2012;125:375.
Kelishadi R, Salek S, Salek M, Hashemipour M, Movahedian M. Effects of vitamin D supplementation on insulin resistance and cardiometabolic risk factors in children with metabolic syndrome: a triple-masked controlled trial. J Pediatr. 2014;90:28–34.
Hajimohammadi M, Shab-Bidar S, Neyestani TR. Vitamin D and serum leptin: a systematic review and metaanalysis of observational studies and randomized controlled trials. Eur J Clin Nutr. 2017;71:1144–53.
Santos A, Andaki ACR, Amorim PRS, Mendes EL. Fatores associados ao comportamento sedentário em escolares de 9-12 anos de idade. Motriz. 2013;19:S25–S34.
American Academy of Pediatrics. Children, adolescents, and the media. Council on communications and media. Pediatrics. 2013;132:958–61.
World Health Organization. Waist circumference and waist-hip ratio: report of a WHO expert consultation. Geneva: WHO; 2008.
De Ferranti SD, Gauvreau K, Ludwig DS, Neufeld EJ, Newburger JW, Rifai N. Prevalence of the metabolic syndrome in American adolescents: findings from the third national health and nutrition examination survey. Circulation. 2004;110:2494–7.
Lohman TG. Assessing fat distribution. In: Advances in body composition assessment: current issues in exercise science. Champaign, IL: Human Kinetics; 1992. p. 57–63.
Cox KL, Devanarayan V, Kriauciunas A, Manetta J, Montrose C, Sittampalam S. Immunoassay methods. In: Sittampalam GS, Grossman A, Brimacombe K, editors. Assay guidance manual. Bethesda (MD): Eli Lilly & Company and the National Center for Advancing Translational Sciences; 2012. https://www.ncbi.nlm.nih.gov/books/NBK92434/.
Sociedade Brasileira de Cardiologia. Atualização da Diretriz Brasileira de Dislipidemias e Prevenção da Aterosclerose—2017. Arq Bras Cardiol. 2017;109:1–76.
Hutchinson K, Healy M, Crowley V, Louw M, Rochev Y. Verification of Abbott 25-OH-vitamin D assay on the architect system. Pract Lab Med. 2017;17:27–35.
Simental-Mendia LE, Rodriguez-Moran M, Guerrero-Romero F. The product of fasting glucose and triglycerides as surrogate for identifying insulin resistance in apparently healthy subjects. Metab Syndr Relat Disord. 2008;6:299–304.
Gomez-Huelgas R, Bernal-López MR, Villalobos A, Mancera-Romero J, Baca-Osorio AJ, Jansen S, et al. Hypertriglyceridemic waist: an alternative to the metabolic syndrome? Results of the IMAP Study (multidisciplinary intervention in primary care). Int J Obes. 2011;35:292–9.
Blackburn P, Lemieux I, Lamarche B, Bergeron J, Perron P, Tremblay G, et al. Hypertriglyceridemic waist: a simple clinical phenotype associated with coronary artery disease in women. Metabolism. 2012;61:56–64.
Galan I, Rodriguez-Artalejo F, Tobias A, Diez-Ganan L, Gandarillas A, Zorrilla B. Clustering of behavior-related risk factors and its association with subjective health. Gac Sanit. 2005;19:370–8.
Poortinga W. The prevalence and clustering of four major lifestyle risk factors in an English adult population. Prev Med. 2007;44:124–8.
Thomas GN, Hartaigh BO, Bosch JA, Pilz S, Loerbroks A, Kleber ME, et al. Vitamin D levels predict all-cause and cardiovascular disease mortality in subjects with the metabolic syndrome: the Ludwigshafen Risk and Cardiovascular Health (LURIC) Study. Diabetes Care. 2012;35:1158–64.
Newberry SJ, Chung M, Shekelle PG, Booth MS, Liu JL, Maher AR, et al. Vitamin D and calcium: a systematic review of health outcomes (Update). Evid Rep Technol Assess. 2014;217:1–929.
Giovannucci E, Liu Y, Hollis BW, Rimm EB. 25-hydroxyvitamin D and risk of myocardial infarction in men: a prospective study. Arch Intern Med. 2008;168:1174–80.
Fiscella K, Frank P. Vitamin D, race, and cardiovascular mortality: findings from national US sample. Ann Fam Med. 2010;8:11–8.
Schierbeck LL, Rejnmark L, Tofteng CL, Stilgren L, Eiken P, Mosekilde L, et al. Vitamin D deficiency in postmenopausal, healthy women predicts increased cardiovascular events: a 16-year follow-up study. Eur J Endocrinol. 2012;167:553–60.
Zhao G, Ford ES, Li C, Croft JB. Serum 25-hydroxyvitamin D levels and all-cause and cardiovascular disease mortality among US adults with hypertension: the NHANES linked mortality study. J Hypertens. 2012;30:284–9.
Hanley DA, Cranney A, Jones G, Whiting SJ, Leslie WD, Cole DE, et al. Vitamin D in adult health and disease: a review and guideline statement from Osteoporosis Canada. Can Med Assoc J. 2010;182:610–8.
Institute Of Medicine. Dietary reference intakes for calcium and vitamin D. Washington, DC: National Academies Press; 2011.
Maeda SS, Kunii IS, Hayashi L, Lazaretti-Castro M. The effect of sun exposure on 25-hydroxyvitamin D concentrations in young healthy subjects living in the city of Sao Paulo, Brazil. Braz J Med Biol Res. 2007;40:1653–9.
Almeida CA, Pinho AP, Ricco RG, Elias CP. Abdominal circumference as an indicator of clinical and laboratory parameters associated with obesity in children and adolescents: comparison between two reference tables. J Pediatr. 2007;83:181–5.
Foschini D, Santos RVT, Prado WL, Piano A, Lofrano MC, Martins AC, et al. Plaqueta e leptina em adolescentes com obesidade. J Pediatr. 2008;84:516–21.
Xiao CW, Wood CM, Swist E, Nagasaka R, Sarafin K, Gagnon C, et al. Cardio-metabolic disease risks and their associations with circulating 25-hydroxyvitamin D and omega-3 levels in South Asian and White Canadians. PLoS One. 2016;11:e0147648.
Zhang M, Gao Y, Tian L, Zheng L, Wang X, Liu W, et al. Association of serum 25-hydroxyvitamin D3 with adipokines and inflammatory marker in persons with prediabetes mellitus. Clin Chim Acta. 2017;468:152–8.
Ayesha I, Bala TS, Reddy CV, Raghuramulu N. Vitamin D deficiency reduces insulin secretion and turnover in rats. Diabetes Nutr Metab. 2001;14:78–84.
Zeitz U, Weber K, Soegiart DW. Impaired insulin secretory capacity in mice lacking a functional vitamin D receptor. FASEB J. 2003;17:509–11.
Schuit AJ, Van Loon AJ, Tijhuis M, Ocké M. Clustering of lifestyle risk factors in a general adult population. Prev Med. 2002;35:219–24.
Funding
This work was funded by the National Council for Scientific and Technological Development (CNPq), grant number 478910/2013–4 and 407547/2012–6. The CNPQ had no role in the design, analysis, or writing of this article.
Author information
Authors and Affiliations
Contributions
LCM assisted in the conception and design of this work, data collection, analysis and interpretation of the data, conducted the literature search, and writing of the manuscript. MSF, NP, LGS, and FMA assisted in the conception and design of this work, data collection, analysis and interpretation, as well as revising and approval of the final version to be published. LJL supervised data analysis, assisted in the interpretation of results and approval of the final manuscript to submission. SCCF assisted in the interpretation of results and approval of the final manuscript to submission. JFN designed the study, including the data collection, coordinated and supervised, and approved the final manuscript to submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Milagres, L.C., Filgueiras, M.D.S., Rocha, N.P. et al. Cutoff point estimation for serum vitamin D concentrations to predict cardiometabolic risk in Brazilian children. Eur J Clin Nutr 74, 1698–1706 (2020). https://doi.org/10.1038/s41430-020-0624-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-0624-5
This article is cited by
-
The effect of vitamin D supplementation on attacks in PFAPA syndrome patients with low vitamin D levels
Irish Journal of Medical Science (1971 -) (2023)