Abstract
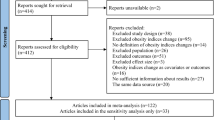
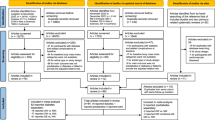
We aimed to examine the association of weight gain during adulthood with the risk of cardiovascular disease (CVD) in the general population. We performed a systematic search of PubMed and Scopus, from inception to June 2019. Prospective cohort studies investigating the association of weight gain during adulthood with the risk of CVD were included. The relative risks (RRs) were calculated by using random-effect models. Twenty-three prospective cohort studies with 1,093,337 participants were included. The RRs for a 5-kg increment in body weight were 1.11 (95% CI: 1.04, 1.19; I2 = 80%, n = 11) for CVD mortality, 1.18 (95% CI: 1.04, 1.32; I2 = 90%, n = 8) for coronary heart disease (CHD), 1.08 (95% CI: 1.04, 1.12; I2 = 0%, n = 3) for stroke, 1.18 (95% CI: 1.12, 1.25; I2 = 0%, n = 2) for myocardial infarction and 1.05 (95% CI: 0.86, 1.23; I2 = 80%, n = 2) for heart failure. A dose–response analysis demonstrated that the risk of CVD mortality was unchanged with weight gain of 0–5 kg, and then increased sharply and linearly (P for nonlinearity < 0.001). The analysis of CHD indicated a sharp increase in risk from baseline up to weight gain equal to 25 kg (P for nonlinearity = 0.12). Adult weight gain may be associated with a higher risk of CVD. Measuring weight gain during adulthood may be better than static, cross-sectional assessment of weight because it considers trend over time, and thus, can be used as a supplementary approach to predict CVD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Jayedi A, Rashidy-Pour A, Khorshidi M, Shab-Bidar S. Body mass index, abdominal adiposity, weight gain and risk of developing hypertension: a systematic review and dose-response meta-analysis of more than 2.3 million participants. Obes Rev. 2018;19:654–67.
Mongraw-Chaffin ML, Peters SAE, Huxley RR, Woodward M. The sex-specific association between BMI and coronary heart disease: a systematic review and meta-analysis of 95 cohorts with 1·2 million participants. Lancet Diabetes Endocrinol. 2015;3:437–49.
Aune D, Sen A, Norat T, Janszky I, Romundstad P, Tonstad S, et al. Body mass index, abdominal fatness, and heart failure incidence and mortality: a systematic review and dose-response meta-analysis of prospective studies. Circulation. 2016;133:639–49.
Riaz H, Khan MS, Siddiqi TJ, Usman MS, Shah N, Goyal A, et al. Association between obesity and cardiovascular outcomes: a systematic review and meta-analysis of mendelian randomization studies. JAMA Netw Open. 2018;1:e183788.
Ballard-Barbash R. Anthropometry and breast cancer. Body size—a moving target. Cancer. 1994;74:1090–100.
French S, Folsom A, Jeffery R, Zheng W, Mink P, Baxter J. Weight variability and incident disease in older women: the Iowa Women’s Health Study. Int J Obes. 1997;21:217.
Li TY, Rana JS, Manson JE, Willett WC, Stampfer MJ, Colditz GA, et al. Obesity as compared with physical activity in predicting risk of coronary heart disease in women. Circulation 2006;113:499–506.
Nordstoga AL, Zotcheva E, Svedahl ER, Nilsen TI, Skarpsno ES. Long-term changes in body weight and physical activity in relation to all-cause and cardiovascular mortality: the HUNT study. Int J Behav Nutr Phys Act. 2019;16:45.
Bowman TS, Kurth T, Sesso HD, Manson JE, Gaziano JM. Eight-year change in body mass index and subsequent risk of cardiovascular disease among healthy non-smoking men. Prev Med 2007;45:436–41.
Karahalios A, English DR, Simpson JA. Change in body size and mortality: a systematic review and meta-analysis. Int J Epidemiol. 2016;46:526–46.
Chou W-T, Kakizaki M, Tomata Y, Nagai M, Sugawara Y, Kuriyama S, et al. Impact of weight change since age 20 and cardiovascular disease mortality risk. Circulation J 2013;77:679–86.
Janszky I, Romundstad P, Laugsand L, Vatten LJ, Mukamal KJ, Mørkedal B. Weight and weight change and risk of acute myocardial infarction and heart failure–the HUNT Study. J Intern Med. 2016;280:312–22.
Mulligan AA, Lentjes MA, Luben RN, Wareham NJ, Khaw K-T. Weight change and 15 year mortality: results from the European Prospective Investigation into Cancer in Norfolk (EPIC-Norfolk) cohort study. Eur J Epidemiol. 2018;33:37–53.
Park S-Y, Wilkens LR, Maskarinec G, Haiman CA, Kolonel LN, Marchand L. Weight change in older adults and mortality: the Multiethnic Cohort Study. Int J Obes. 2018;42:205.
Zheng Y, Manson JE, Yuan C, Liang MH, Grodstein F, Stampfer MJ, et al. Associations of weight gain from early to middle adulthood with major health outcomes later in life. JAMA. 2017;318:255–69.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–9.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25:603–5.
Symons M, Moore D. Hazard rate ratio and prospective epidemiological studies. J Clin Epidemiol. 2002;55:893–9.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Controlled Clin trials. 1986;7:177–88.
Berlin JA, Longnecker MP, Greenland S. Meta-analysis of epidemiologic dose-response data. Epidemiology. 1993;4:218–28.
Orsini N, Bellocco R, Greenland S. Generalized least squares for trend estimation of summarized dose–response data. Stata J. 2006;6:40–57.
Jayedi A, Rashidy-Pour A, Parohan M, Zargar MS, Shab-Bidar S. Dietary antioxidants, circulating antioxidant concentrations, total antioxidant capacity, and risk of all-cause mortality: a systematic review and dose-response meta-analysis of prospective observational studies. Adv Nutr. 2018;9:701–16.
Schwingshackl L, Schwedhelm C, Hoffmann G, Lampousi AM, Knuppel S, Iqbal K, et al. Food groups and risk of all-cause mortality: a systematic review and meta-analysis of prospective studies. Am J Clin Nutr. 2017;105:1462–73.
Hamling J, Lee P, Weitkunat R, Ambühl M. Facilitating meta-analyses by deriving relative effect and precision estimates for alternative comparisons from a set of estimates presented by exposure level or disease category. Stat Med. 2008;27:954–70.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. Bmj 2003;327:557–60.
Egger M, Smith GD, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. Bmj 1997;315:629–34.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.
Higgins JP, Green S (editors). Cochrane handbook for systematic reviews of interventions, version 5.1.0 [updated March 2011]. The Cochrane Collaboration. 2011. Available from www.cochrane-handbook.org.
Orsini N, Li R, Wolk A, Khudyakov P, Spiegelman D. Meta-analysis for linear and nonlinear dose-response relations: examples, an evaluation of approximations, and software. Am J Epidemiol. 2011;175:66–73.
Adams KF, Leitzmann MF, Ballard-Barbash R, Albanes D, Harris TB, Hollenbeck A, et al. Body mass and weight change in adults in relation to mortality risk. Am J Epidemiol. 2014;179:135–44.
Breeze E, Clarke R, Shipley MJ, Marmot MG, Fletcher AE. Cause-specific mortality in old age in relation to body mass index in middle age and in old age: follow-up of the Whitehall cohort of male civil servants. Int J Epidemiol. 2005;35:169–78.
Chei C, Iso H, Yamagishi K, Inoue M, Tsugane S. Body mass index and weight change since 20 years of age and risk of coronary heart disease among Japanese: the Japan Public Health Center-Based Study. Int J Obes. 2008;32:144.
Cui R, Iso H, Tanabe N, Watanabe Y, Tamakoshi A, Group JS. Association between weight change since 20 years of age with mortality from myocardial infarction and chronic heart failure in the Japan collaborative cohort (JACC) study. Circulation J. 2013;78:CJ-13-1057.
de Hollander EL, Bemelmans WJ, de Groot LC. Associations between changes in anthropometric measures and mortality in old age: a role for mid-upper arm circumference? J Am Med Dir Assoc. 2013;14:187–93.
Galanis DJ, Harris T, Sharp DS, Petrovitch H. Relative weight, weight change, and risk of coronary heart disease in the Honolulu Heart Program. Am J Epidemiol. 1998;147:379–86.
Iribarren C, Sharp DS, Burchfiel CM, Petrovitch H. Association of weight loss and weight fluctuation with mortality among Japanese American men. N. Engl J Med. 1995;333:686–92.
Karahalios A, Simpson JA, Baglietto L, MacInnis RJ, Hodge AM, Giles GG, et al. Change in body size and mortality: results from the Melbourne collaborative cohort study. PLoS ONE 2014;9:e99672.
Lee I-M, Paffenbarger RS. Change in body weight and longevity. JAMA 1992;268:2045–9.
Manson JE, Willett WC, Stampfer MJ, Colditz GA, Hunter DJ, Hankinson SE, et al. Body weight and mortality among women. N. Engl J Med. 1995;333:677–85.
Nanri A, Mizoue T, Takahashi Y, Noda M, Inoue M, Tsugane S. Weight change and all-cause, cancer and cardiovascular disease mortality in Japanese men and women: the Japan Public Health Center-Based Prospective Study. Int J Obes. 2010;34:348.
Rexrode KM, Hennekens CH, Willett WC, Colditz GA, Stampfer MJ, Rich-Edwards JW, et al. A prospective study of body mass index, weight change, and risk of stroke in women. JAMA. 1997;277:1539–45.
Rimm EB, Stampfer MJ, Giovannucci E, Ascherio A, Spiegelman D, Colditz GA, et al. Body size and fat distribution as predictors of coronary heart disease among middle-aged and older US men. Am J Epidemiol. 1995;141:1117–27.
Willett WC, Manson JE, Stampfer MJ, Colditz GA, Rosner B, Speizer FE, et al. Weight, weight change, and coronary heart disease in women: risk within the’normal’weight range. JAMA. 1995;273:461–5.
Williamson DF, Pamuk E, Thun M, Flanders D, Byers T, Heath C. Prospective study of intentional weight loss and mortality in overweight white men aged 40–64 years. Am J Epidemiol. 1999;149:491–503.
Yaari S, Goldbourt U. Voluntary and involuntary weight loss: associations with long term mortality in 9,228 middle-aged and elderly men. Am J Epidemiol. 1998;148:546–55.
Yarnell JW, Patterson CC, Thomas HF, Sweetnam PM. Comparison of weight in middle age, weight at 18 years, and weight change between, in predicting subsequent 14 year mortality and coronary events: Caerphilly Prospective Study. J Epidemiol Community Health. 2000;54:344–8.
Keum N, Greenwood DC, Lee DH, Kim R, Aune D, Ju W, et al. Adult weight gain and adiposity-related cancers: a dose-response meta-analysis of prospective observational studies. J Natl Cancer Inst. 2015;107:djv088.
Aune D, Sen A, Schlesinger S, Norat T, Janszky I, Romundstad P, et al. Body mass index, abdominal fatness, fat mass and the risk of atrial fibrillation: a systematic review and dose-response meta-analysis of prospective studies. Eur J Epidemiol. 2017;32:181–92.
Strazzullo P, D’Elia L, Cairella G, Garbagnati F, Cappuccio FP, Scalfi L. Excess body weight and incidence of stroke: meta-analysis of prospective studies with 2 million participants. Stroke 2010;41:e418–26.
Ma C, Avenell A, Bolland M, Hudson J, Stewart F, Robertson C, et al. Effects of weight loss interventions for adults who are obese on mortality, cardiovascular disease, and cancer: systematic review and meta-analysis. BMJ. 2017;359:j4849.
Van LG, Wauters M, De IL. The beneficial effects of modest weight loss on cardiovascular risk factors. Int J Obes Relat Metab Disord. 1997;21:S5–9.
Van Gaal LF, Mertens IL, Ballaux D. What is the relationship between risk factor reduction and degree of weight loss? Eur Heart J Suppl. 2005;7:L21–6.
Wing RR, Lang W, Wadden TA, Safford M, Knowler WC, Bertoni AG, et al. Benefits of modest weight loss in improving cardiovascular risk factors in overweight and obese individuals with type 2 diabetes. Diabetes Care. 2011;34:1481–6.
Wenger NK. Prevention of cardiovascular disease: highlights for the clinician of the 2013 American College of Cardiology/American Heart Association guidelines. Clin Cardiol. 2014;37:239–51.
Poirier P, Giles TD, Bray GA, Hong Y, Stern JS, Pi-Sunyer FX, et al. Obesity and cardiovascular disease: pathophysiology, evaluation, and effect of weight loss: an update of the 1997 American Heart Association Scientific Statement on Obesity and Heart Disease from the Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism. Circulation. 2006;113:898–918.
Gurunathan U, Myles PS. Limitations of body mass index as an obesity measure of perioperative risk. Br J Anaesth. 2016;116:319–21. https://doi.org/10.1093/bja/aev541.
Palta M, Prineas RJ, Berman R, Hannan P. Comparison of self-reported and measured height and weight. Am J Epidemiol. 1982;115:223–30.
Perry GS, Byers TE, Mokdad AH, Serdula MK, Williamson DF. The validity of self-reports of past body weights by U.S. adults. Epidemiology. 1995;6:61–6.
Stevens J, Keil JE, Waid LR, Gazes PC. Accuracy of current, 4-year, and 28-year self-reported body weight in an elderly population. Am J Epidemiol. 1990;132:1156–63.
Choi S, Kim K, Kim SM, Lee G, Jeong S-M, Park SY, et al. Association of obesity or weight change with coronary heart disease among young adults in South Korea. JAMA Intern Med. 2018;178:1060–8.
Author information
Authors and Affiliations
Contributions
AJ, SS-B, and ARP conceived and designed the study; AE and MSZ conducted systematic search, screened articles and selected eligible articles; AE and SS extracted information from eligible studies; AJ, SS-B, and ARP performed analyses and interpreted the results; AJ, AE, SS, and MSZ wrote the first draft of the paper; SS-B and ARP critically revised the paper. SS-B is the guarantor. All authors have read and approved the final paper. All authors had full access to all the data and take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Jayedi, A., Rashidy-pour, A., Soltani, S. et al. Adult weight gain and the risk of cardiovascular disease: a systematic review and dose–response meta-analysis of prospective cohort studies. Eur J Clin Nutr 74, 1263–1275 (2020). https://doi.org/10.1038/s41430-020-0610-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-020-0610-y
This article is cited by
-
COVID-19-related cardiovascular disease risk due to weight gain: a nationwide cohort study
European Journal of Medical Research (2024)
-
Body weight, weight change and the risk of cardiovascular disease in patients with hypertension: a primary-care cohort study
International Journal of Obesity (2023)
-
Three-year weight change and risk of all-cause, cardiovascular, and cancer mortality among Iranian adults: over a decade of follow-up in the Tehran Lipid and Glucose Study
BMC Public Health (2022)
-
Dietary networks identified by Gaussian graphical model and general and abdominal obesity in adults
Nutrition Journal (2021)