Abstract
Background/objectives
Small for gestational age (SGA) may be associated with increased rates of mortality and morbidity not only during the infantile period but also in later life. This study was performed to determine the dose–response relationships of maternal height and weight with risk of SGA.
Subjects/methods
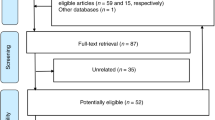
Dose–response meta-analyses were performed to summarize adjusted relative risks of SGA per 1-cm in maternal height and 1-kg increase in weight (linear model) and for varying levels relative to 160 cm in height and 55 kg in weight (nonlinear model). The adjustments for potential confounders were made using the Hamling method. Eight databases, including PubMed (MEDLINE), were searched. Study quality was assessed using the Newcastle–Ottawa scale (NOS).
Results
Totals of 117,114 and 13,049 subjects were extracted from high-quality studies (e.g., NOS score ≥ 8) to evaluate maternal height (n = 7) and weight (n = 3), respectively. Corresponding to P for nonlinearity (P < 0.05), the dose–response relationships were nonlinear rather than linear. The nonlinear model showed that maternal height and weight were significantly and inversely associated with the risk of SGA, regardless of the levels below or above their means (i.e., 160 cm or 55 kg, respectively).
Conclusions
SGA risk may be reduced by increasing maternal height and weight.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Tsai LY, Chen YL, Tsou KI, Mu SC, Taiwan Premature Infant Developmental Collaborative Study Group. The impact of small for gestational age on neonatal outcome among very low birth weight infants. Pediatr Neonatol. 2015;56:101–107.
Jaquet D, Deghmoun S, Chevenne D, Czernichow P, Lévy-Marchal C. Low serum adiponectin levels in subjects born small for gestational age: impact on insulin sensitivity. Int J Obes (Lond). 2006;30:83–87.
Goto E. Dose-response association between maternal body mass index and small for gestational age: a meta-analysis. J Matern Fetal Neonatal Med. 2017;30:213–218.
Hamling J, Lee P, Weitkunat R, Ambühl M. Facilitating meta-analyses by deriving relative effect and precision estimates for alternative comparisons from a set of estimates presented by exposure level or disease category. Stat Med. 2008;27:954–970.
Wells GA Shea B, O’Connell D, Peterson J, Welch V, Losos M et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. [cited 2019 January 12] Available from: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp.
Orsini N, Bellocco R, Greenland S. Generalized least squares for trend estimation of summarized dose-response data. Stata J. 2006;6:40–57.
The Organisation for Economic Co-operation and Development. DAC list of ODA recipients: effective for reporting on 2014, 2015,2016, and 2017 flows. [cited 2019 January 12]. Available from: https://www.oecd.org/dac/stats/documentupload/DAC_List_ODA_Recipients2014to2017_flows_En.pdf.
Orsini N, Li R, Wolk A, Khudyakov P, Spiegelman D. Meta-analysis for linear and nonlinear dose-response relations: examples, an evaluation of approximations, and software. Am J Epidemiol. 2012;175:66–73.
Clausson B, Cnattingius S, Axelsson O. Preterm and term births of small for gestational age infants: a population-based study of risk factors among nulliparous women. Br J Obstet Gynaecol. 1998;105:1011–1017.
Kozuki N, Katz J, LeClerq SC, Khatry SK, West KP Jr., Christian P. Risk factors and neonatal/infant mortality risk of small-for-gestational-age and preterm birth in rural Nepal. J Matern Fetal Neonatal Med. 2015;28:1019–1025.
Mavalankar DV, Trivedi CC, Gray RH. Maternal weight, height and risk of poor pregnancy outcome in Ahmedabad, India. Indian Pediatr. 1994;31:1205–1212.
Mavalankar DV, Gray RH, Trivedi CR, Parikh VC. Risk factors for small for gestational age births in Ahmedabad, India. J Trop Pediatr. 1994;40:285–290.
Muhihi A, Sudfeld CR, Smith ER, Noor RA, Mshamu S, Briegleb C, et al. Risk factors for small-for-gestational-age and preterm births among 19,269 Tanzanian newborns. BMC Pregnancy Childbirth. 2016;16:110.
Rodrigues T, Barros H. Comparison of risk factors for small-for-gestational-age and preterm in a Portuguese cohort of newborns. Matern Child Health J. 2007;11:417–424.
Yunis KA, Beydoun H, Tamim H. National Collaborative Perinatal Neonatal Network. Maternal predictors of small-for-gestational age in uncomplicated births. Int J Gynaecol Obstet. 2002;79:33–35.
Yunis KA, Beydoun H, Tamim H, Nassif Y, Khogali M. National Collaborative Perinatal Neonatal Network. Risk factors for term or near-term fetal growth restriction in the absence of maternal complications. Am J Perinatol. 2004;21:227–234.
Rasmussen KM, Yaktine AL (eds). Weight Gain During Pregnancy: Reexamining the Guidelines. Washington DC: The National Academic Press; 2009.
Santos S, Voerman E, Amiano P, Barros H, Beilin LJ, Bergström A et al. Impact of maternal body mass index and gestational weight gain on pregnancy complications: An individual participant data meta-analysis of European, North American and Australian cohorts. BJOG. 2019; e-pub ahead of print 2019; https://doi.org/10.1111/1471-0528.15661.
McCowan LM, Figueras F, Anderson NH. Evidence-based national guidelines for the management of suspected fetal growth restriction: comparison, consensus, and controversy. Am J Obstet Gynecol. 2018;218:S855–S868.
Rochow N, AlSamnan M, So HY, Olbertz D, Pelc A, Däbritz J, et al. Maternal body height is a stronger predictor of birth weight than ethnicity: analysis of birth weight percentile charts. J Perinat Med. 2018;47:22–29.
Villar J, Papageorghiou AT, Pang R, Ohuma EO, Cheikh Ismail L, Barros FC, et al. The likeness of fetal growth and newborn size across non-isolated populations in the INTERGROWTH-21st Project: the Fetal Growth Longitudinal Study and Newborn Cross-Sectional Study. Lancet Diabetes Endocrinol. 2014;2:781–792.
The Cochrane Collaboration. Glossary. 2019. [cited 2019 March 2] Available from: https://community.cochrane.org/glossary#about-cochrane.
Egger M, Smith GD, Altman DG (eds). Systematic reviews in healthcare: meta-analysis in context. 2nd edn. (BMJ Published group, London, 2008).
Acknowledgements
I am grateful to the staff of the Medical Library of the Japan Medical Association (Tokyo, Japan) for help in retrieving the full texts of the articles. A native check in English language is made at Dolphin Corporation (1005 Kichijyoji Nagatami City Plaza 1-20-1 Kichijyojihonmachi. Musashino, 180–0004, Japan, trust@dolphin-tr.com).
Author information
Authors and Affiliations
Contributions
EG, the corresponding author, is responsible for literature search, figures, study design, data collection, data analysis, data interpretation, and writing.
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Goto, E. Dose–response associations of maternal height and weight with small for gestational age: a meta-analysis. Eur J Clin Nutr 74, 106–111 (2020). https://doi.org/10.1038/s41430-019-0432-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-019-0432-y
This article is cited by
-
Difference in risk of preterm and small-for-gestational-age birth depending on maternal occupations in Japan
BMC Research Notes (2023)
-
Association of high maternal blood alpha-fetoprotein level with risk of delivering small for gestational age: a meta-analysis
Pediatric Research (2021)
-
Novel sex-specific influence of parental factors on small-for-gestational-age newborns
Scientific Reports (2020)