Abstract
Background/objectives
Eating a variety of foods has been recommended in the dietary guidelines of many developed nations, as well as global dietary guidelines. We investigated the potential effect of dietary diversity on the risk of total mortality and major causes of mortality in a large-scale cohort study involving the Japanese population.
Subjects/methods
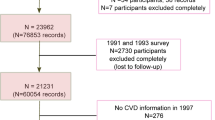
From 1995 to 2012, 79,904 participants (37,240 men and 42,664 women) aged 45 to 74 years, without histories of ischemic heart disease, stroke, or cancer were followed-up for a median of 14.9 years. We used 133 food and beverage items listed on a 5-year follow-up food frequency questionnaire, and the daily frequency of consumption for each item (excluding five alcoholic beverages) was counted. Multivariable-adjusted Cox proportional hazards regression models were used to calculate hazard ratios (HRs) and corresponding 95% confidence intervals (CIs) to compare the highest and lowest quintiles.
Results
An inverse association was identified between total dietary diversity and mortality rates in women (highest quintile HR: 0.81; 95% CI: 0.71, 0.92; p for trend = 0.002) but the same trend was not observed in men (highest quintile HR: 0.96; 95% CI: 0.87, 1.10; p for trend = 0.266). In addition, fruit diversity was associated with lower mortality rates in men (highest quintile HR: 0.87; 95% CI: 0.79, 0.95; p for trend = 0.006), whereas soy diversity was associated with lower mortality rates in women (highest quintile HR: 0.89; 95% CI: 0.79, 1.00; p for trend = 0.004). With regard to men, meat and fish diversity were associated with higher mortality rates (highest quintiles of meat and fish diversity HR: 1.15 [95% CI: 1.06, 1.25] and 1.12 [95% CI: 1.02, 1.22], respectively).
Conclusions
These findings indicate that consuming a greater diversity of total foods and increasing the diversity of fruit and soy consumed have considerable public health implications.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Montagnese C, Santarpia L, Buonifacio M, Nardelli A, Caldara AR, Silvestri E, et al. European food-based dietary guidelines: a comparison and update. Nutrition. 2015;31:908–15. https://doi.org/10.1016/j.nut.2015.01.002.
U.S. Department of Health and Human Services and U.S. Department of Agriculture. Dietary guidelines for Americans. 8th ed., Health and Human Services Dept. and Agriculture Dept., Washington, DC; 2015.
Food and Agriculture Organization of the United Nations. Food-based dietary guidelines. 2016.
Kant AK, Schatzkin A, Harris TB, Ziegler RG, Block G. Dietary diversity and subsequent mortality in the First National Health and Nutrition Examination Survey Epidemiologic Follow-up Study. Am J Clin Nutr. 1993;57:434–40.
La Vecchia C, Munoz SE, Braga C, Fernandez E, Decarli A. Diet diversity and gastric cancer. Int J Cancer. 1997;72:255–7.
Garavello W, Giordano L, Bosetti C, Talamini R, Negri E, Tavani A, et al. Diet diversity and the risk of oral and pharyngeal cancer. Eur J Nutr. 2008;47:280–4. https://doi.org/10.1007/s00394-008-0722-y.
Lucenteforte E, Garavello W, Bosetti C, Talamini R, Zambon P, Franceschi S, et al. Diet diversity and the risk of squamous cell esophageal cancer. Int J Cancer. 2008;123:2397–2400. https://doi.org/10.1002/ijc.23761.
Ministry of Health and Welfare HSB, Health Promotion Division. Dietary guidelines for Health promotion in Japan: explanation and educational guideline. Daiichi Shuppan; 1985.
Lee MS, Huang YC, Su HH, Lee MZ, Wahlqvist ML. A simple food quality index predicts mortality in elderly Taiwanese. J Nutr, Health & Aging. 2011;15:815–21.
Tian X, Wu M, Zang J, Zhu Y, Wang H. Dietary diversity and adiposity in Chinese men and women: an analysis of four waves of cross-sectional survey data. Eur J Clin Nutr. 2017;71:506–11. https://doi.org/10.1038/ejcn.2016.212.
Vadiveloo M, Dixon LB, Mijanovich T, Elbel B, Parekh N. Dietary variety is inversely associated with body adiposity among US adults using a novel food diversity index. J Nutr. 2015;145:555–63. https://doi.org/10.3945/jn.114.199067.
Kant AK, Schatzkin A, Ziegler RG. Dietary diversity and subsequent cause-specific mortality in the NHANES I epidemiologic follow-up study. J Am Coll Nutr. 1995;14:233–8.
Larsson SC, Akesson A, Wolk A. Overall diet quality and risk of stroke: a prospective cohort study in women. Atherosclerosis. 2014;233:27–29. https://doi.org/10.1016/j.atherosclerosis.2013.11.072.
Kaluza J, Hakansson N, Brzozowska A, Wolk A. Diet quality and mortality: a population-based prospective study of men. Eur J Clin Nutr. 2009;63:451–7. https://doi.org/10.1038/sj.ejcn.1602968.
Michels KB, Wolk A. A prospective study of variety of healthy foods and mortality in women. Int J Epidemiol. 2002;31:847–54.
Kant AK, Schatzkin A, Graubard BI, Schairer C. A prospective study of diet quality and mortality in women. Jama. 2000;283:2109–15.
Tsugane S, Sawada N. The JPHC study: design and some findings on the typical Japanese diet. Jpn J Clin Oncol. 2014;44:777–82. https://doi.org/10.1093/jjco/hyu096.
Sasaki S, Kobayashi M, Ishihara J, Tsugane S. Self-administered food frequency questionnaire used in the 5-year follow-up survey of the JPHC Study: questionnaire structure, computation algorithms, and area-based mean intake. J Epidemiol/Jpn Epidemiol Assoc. 2003;13(1 Suppl):S13–22.
Kobayashi MT,S. Dietary diversity and healthy lifestyle, nutrient adequacy in Japan (in Japanese). J Health Welf Stat. 2006;53:7–15.
Watanabe S, Tsugane S, Sobue T, Konishi M, Baba S. Study design and organization of the JPHC study. Japan Public Health Center-based Prospective Study on Cancer and Cardiovascular Diseases. J Epidemiol / Jpn Epidemiol Assoc. 2001;11(6 Suppl):S3–7. e-pub ahead of print 2002/01/05.
Ministry of Health, Labour and Welfare. Vital statistics in Japan—the latest trends. 2009.
Schwingshackl L, Hoffmann G. Diet quality as assessed by the Healthy Eating Index, the Alternate Healthy Eating Index, the Dietary Approaches to Stop Hypertension score, and health outcomes: a systematic review and meta-analysis of cohort studies. J Acad Nutr Diet. 2015;115:780–800 e785. https://doi.org/10.1016/j.jand.2014.12.009.
Vargas AJ, Neuhouser ML, George SM, Thomson CA, Ho GY, Rohan TE, et al. Diet quality and colorectal cancer risk in the women’s health initiative observational study. Am J Epidemiol. 2016. https://doi.org/10.1093/aje/kwv304.
Harmon BE, Boushey CJ, Shvetsov YB, Ettienne R, Reedy J, Wilkens LR, et al. Associations of key diet-quality indexes with mortality in the Multiethnic Cohort: the Dietary Patterns Methods Project. Am J Clin Nutr. 2015;101:587–97. https://doi.org/10.3945/ajcn.114.090688.
Boggs DA, Ban Y, Palmer JR, Rosenberg L. Higher diet quality is inversely associated with mortality in African-American women. J Nutr. 2015;145:547–54. https://doi.org/10.3945/jn.114.195735.
George SM, Ballard-Barbash R, Manson JE, Reedy J, Shikany JM, Subar AF, et al. Comparing indices of diet quality with chronic disease mortality risk in postmenopausal women in the Women’s Health Initiative Observational Study: evidence to inform national dietary guidance. Am J Epidemiol. 2014;180:616–25. https://doi.org/10.1093/aje/kwu173.
Drake I, Gullberg B, Sonestedt E, Wallstrom P, Persson M, Hlebowicz J, et al. Scoring models of a diet quality index and the predictive capability of mortality in a population-based cohort of Swedish men and women. Public Health Nutr. 2013;16:468–78. https://doi.org/10.1017/s1368980012002789.
McNaughton SA, Bates CJ, Mishra GD. Diet quality is associated with all-cause mortality in adults aged 65 years and older. J Nutr. 2012;142:320–5. https://doi.org/10.3945/jn.111.148692.
Akbaraly TN, Ferrie JE, Berr C, Brunner EJ, Head J, Marmot MG, et al. Alternative Healthy Eating Index and mortality over 18 y of follow-up: results from the Whitehall II cohort. Am J Clin Nutr. 2011;94:247–53. https://doi.org/10.3945/ajcn.111.013128.
Seymour JD, Calle EE, Flagg EW, Coates RJ, Ford ES, Thun MJ. Diet Quality Index as a predictor of short-term mortality in the American Cancer Society Cancer Prevention Study II Nutrition Cohort. Am J Epidemiol. 2003;157:980–8.
Oba S, Nagata C, Nakamura K, Fujii K, Kawachi T, Takatsuka N, et al. Diet based on the Japanese Food Guide Spinning Top and subsequent mortality among men and women in a general Japanese population. J Am Diet Assoc. 2009;109:1540–7. https://doi.org/10.1016/j.jada.2009.06.367.
Kurotani K, Akter S, Kashino I, Goto A, Mizoue T, Noda M, et al. Quality of diet and mortality among Japanese men and women: Japan Public Health Center based prospective study. BMJ. 2016;352:i1209 https://doi.org/10.1136/bmj.i1209.
Onvani S, Haghighatdoost F, Surkan PJ, Larijani B, Azadbakht L. Adherence to the Healthy Eating Index and Alternative Healthy Eating Index dietary patterns and mortality from all causes, cardiovascular disease and cancer: a meta-analysis of observational studies. J Human Nutr Diet. 2016. https://doi.org/10.1111/jhn.12415.
Isa F, Xie LP, Hu Z, Zhong Z, Hemelt M, Reulen RC, et al. Dietary consumption and diet diversity and risk of developing bladder cancer: results from the South and East China case-control study. Cancer Causes Control. 2013;24:885–95. https://doi.org/10.1007/s10552-013-0165-5.
Fernandez E, Negri E, La Vecchia C, Franceschi S. Diet diversity and colorectal cancer. Prev Med. 2000;31:11–14. https://doi.org/10.1006/pmed.2000.0667.
Mai V, Kant AK, Flood A, Lacey JV Jr., Schairer C, Schatzkin A. Diet quality and subsequent cancer incidence and mortality in a prospective cohort of women. Int J Epidemiol. 2005;34:54–60. https://doi.org/10.1093/ije/dyh388.
Masala G, Assedi M, Bendinelli B, Ermini I, Sieri S, Grioni S, et al. Fruit and vegetables consumption and breast cancer risk: the EPIC Italy study. Breast Cancer Res Treat. 2012;132:1127–36. https://doi.org/10.1007/s10549-011-1939-7.
Buchner FL, Bueno-de-Mesquita HB, Ros MM, Overvad K, Dahm CC, Hansen L, et al. Variety in fruit and vegetable consumption and the risk of lung cancer in the European prospective investigation into cancer and nutrition. Cancer Epidemiol Biomark Prev. 2010;19:2278–86. https://doi.org/10.1158/1055-9965.epi-10-0489.
Jeurnink SM, Buchner FL, Bueno-de-Mesquita HB, Siersema PD, Boshuizen HC, Numans ME, et al. Variety in vegetable and fruit consumption and the risk of gastric and esophageal cancer in the European Prospective Investigation into Cancer and Nutrition. Int J Cancer. 2012;131:E963–73. https://doi.org/10.1002/ijc.27517.
Leenders M, Siersema PD, Overvad K, Tjonneland A, Olsen A, Boutron-Ruault MC, et al. Subtypes of fruit and vegetables, variety in consumption and risk of colon and rectal cancer in the European Prospective Investigation into Cancer and Nutrition. Int J Cancer. 2015;137:2705–14. https://doi.org/10.1002/ijc.29640.
Buchner FL, Bueno-de-Mesquita HB, Ros MM, Kampman E, Egevad L, Overvad K, et al. Variety in vegetable and fruit consumption and risk of bladder cancer in the European Prospective Investigation into Cancer and Nutrition. Int J Cancer. 2011;128:2971–9. https://doi.org/10.1002/ijc.25636.
Bhupathiraju SN, Wedick NM, Pan A, Manson JE, Rexrode KM, Willett WC, et al. Quantity and variety in fruit and vegetable intake and risk of coronary heart disease. Am J Clin Nutr. 2013;98:1514–23. https://doi.org/10.3945/ajcn.113.066381.
Oude Griep LM, Verschuren WM, Kromhout D, Ocke MC, Geleijnse JM. Variety in fruit and vegetable consumption and 10-year incidence of CHD and stroke. Public Health Nutr. 2012;15:2280–6. https://doi.org/10.1017/s1368980012000912.
Takata Y, Shu XO, Gao YT, Li H, Zhang X, Gao J, et al. Red meat and poultry intakes and risk of total and cause-specific mortality: results from cohort studies of Chinese adults in Shanghai. PloS One. 2013;8:e56963 https://doi.org/10.1371/journal.pone.0056963.
Nagao M, Iso H, Yamagishi K, Date C, Tamakoshi A. Meat consumption in relation to mortality from cardiovascular disease among Japanese men and women. Eur J Clin Nutr. 2012;66:687–93. https://doi.org/10.1038/ejcn.2012.6.
Zhao LG, Sun JW, Yang Y, Ma X, Wang YY, Xiang YB. Fish consumption and all-cause mortality: a meta-analysis of cohort studies. Eur J Clin Nutr. 2016;70:155–61. https://doi.org/10.1038/ejcn.2015.72.
Song M, Fung TT, Hu FB, Willett WC, Longo VD, Chan AT, et al. Association of animal and plant protein intake with all-cause and cause-specific mortality. JAMA Intern Med. 2016;176:1453–63. https://doi.org/10.1001/jamainternmed.2016.4182.
Allen NE, Appleby PN, Davey GK, Kaaks R, Rinaldi S, Key TJ. The associations of diet with serum insulin-like growth factor I and its main binding proteins in 292 women meat-eaters, vegetarians, and vegans. Cancer Epidemiol Biomark Prev. 2002;11:1441–8.
Holmes MD, Pollak MN, Willett WC, Hankinson SE. Dietary correlates of plasma insulin-like growth factor I and insulin-like growth factor binding protein 3 concentrations. Cancer Epidemiol Biomark Prev. 2002;11:852–61.
Nagata C, Wada K, Tamura T, Konishi K, Goto Y, Koda S, et al. Dietary soy and natto intake and cardiovascular disease mortality in Japanese adults: the Takayama study. Am J Clin Nutr. 2017;105:426–31. https://doi.org/10.3945/ajcn.116.137281.
Barrett-Connor E. Gender differences and disparities in all-cause and coronary heart disease mortality: epidemiological aspects. Best Pract Res Clin Endocrinol Metab. 2013;27:481–500. https://doi.org/10.1016/j.beem.2013.05.013.
Acknowledgements
We thank the staff and participants involved in this work for their important contributions. This study was funded by the National Cancer Center Research and Development Fund (23-A-31 and 26-A-2) (since 2011), a grant-in-aid of cancer research from the Japanese Ministry of Health, Labour and Welfare (from 1989 to 2010), and a grant for a project study commissioned by the Japanese Ministry of Agriculture, Fishery, and Forestry (MAFF-CPS-2016-1-1). Editorial support in the form of medical writing was provided by Editage.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix 1 The JPHC members are listed at the following site (as of February 2017): http://epi.ncc.go.jp/en/jphc/781/3838.html
Appendix 2 List of 133 food items included in the total diversity score.
Rights and permissions
About this article
Cite this article
Kobayashi, M., Sasazuki, S., Shimazu, T. et al. Association of dietary diversity with total mortality and major causes of mortality in the Japanese population: JPHC study. Eur J Clin Nutr 74, 54–66 (2020). https://doi.org/10.1038/s41430-019-0416-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-019-0416-y
This article is cited by
-
Traditional japanese diet score and the sustainable development goals by a global comparative ecological study
Nutrition Journal (2024)
-
Socio-demographic characteristics associated with the dietary diversity of Thai community-dwelling older people: results from the national health examination survey
BMC Public Health (2022)
-
Interaction of Eating Status and Dietary Variety on Incident Functional Disability among Older Japanese Adults
The Journal of nutrition, health and aging (2022)
-
Why has Japan become the world’s most long-lived country: insights from a food and nutrition perspective
European Journal of Clinical Nutrition (2021)