Abstract
Background/Objectives
Screening for nutrition risk in community-dwelling older adults increases the likelihood of early intervention to improve nutritional status, with short screening tools preferred. SCREEN-II-AB is a valid 8-item tool. The current study determines whether SCREEN-III, a proposed 3-item version, adequately classifies nutrition risk in comparison.
Subjects/Methods
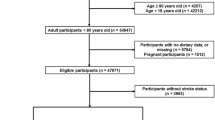
Baseline data from the Canadian Longitudinal Study on Aging were used. Seventy-two percent (n = 24,456) of eligible participants (>55 years, complete SCREEN-II-AB) were included. Sensitivity and specificity of various SCREEN-III values compared with SCREEN-II-AB risk determined a nutrition risk cut-point and the proportion misclassified (False[−]) was calculated. Construct validity was tested against a composite variable summarizing outcomes associated with nutrition risk (e.g., self-reported health, hospitalization) using logistic regression adjusted for individual factors (e.g., marital status).
Results
A SCREEN-III cut-point of <22 performed best on sensitivity (0.83 [95% CI = 0.82, 0.84]) and specificity (0.73 [95% CI = 0.72, 0.74]) compared to SCREEN-II-AB (Cramer’s V = 0.53). Of those at-risk using SCREEN-II-AB, 16.7% were misclassified as False(−) by SCREEN-III. The False(−) group did not differ significantly from the True(−) group. Based on SCREEN-III, 45.3% of individuals were at nutrition risk, 44% of whom reported the outcome composite. SCREEN-III nutrition risk was associated with greater odds of the outcome composite compared to those not at-risk (OR = 1.40, 95% CI = 1.33, 1.48, P < 0.0001).
Conclusion
The proposed version of SCREEN-III demonstrated construct validity, but misclassification of risk may be problematic; further validation of a 3-item version is recommended.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
SCREEN-II, SCREEN-II-AB and other versions are freely available to researchers and clinicians.
References
Bernstein M, Munoz N. Position of the Academy of Nutrition and Dietetics: food and nutrition for older adults: promoting health and wellness. J Acad Nutr Diet. 2012;112:1255–77.
Ahmed T, Haboubi N. Assessment and management of nutrition in older people and its importance to health. Clin Interv Aging. 2010;5:207–16.
Keller HH, Østbye T, Goy R. Nutritional risk predicts quality of life in elderly community-living Canadians. J Gerontol A Biol Sci Med Sci. 2004;59:68–74.
Keller HH, Østbye T. Nutritional risk and time to death; predictive validity of SCREEN (Seniors in the Community Risk Evaluation for Eating and Nutrition). J Nutr Health Aging. 2003;7:274–9.
Hays JC, Keller HH, Østbye T. The effects of nutrition-related factors on four-year mortality among a biracial sample of community-dwelling elders in the North Carolina piedmont. J Nutr Elder. 2005;25:41–67.
Ramage-Morin PL, Garriguet D. Nutritional risk among older Canadians. Health Rep. 2013;24:3–13.
Donini LM, Scardella P, Piombo L, Neri B, Asprino R, Proietti AR, et al. Malnutrition in elderly: social and economic determinants. J Nutr Health Aging. 2013;17:9–15.
Wright L, Vance L, Sudduth C, Epps JB. The impact of a home-delivered meal program on nutritional risk, dietary intake, food security, loneliness, and social well-being. J Nutr Gerontol Geriatr. 2015;34:218–27.
Munk T, Tolstrup U, Beck AM, Holst M, Rasmussen HH, Hovhannisyan K, et al. Individualised dietary counselling for nutritionally at-risk older patients following discharge from acute hospital to home: a systematic review and meta-analysis. J Hum Nutr Diet. 2016;29:196–208.
Keller HH. Promoting food intake in older adults living in the community: a review. Appl Physiol Nutr Metab. 2007;32:991–1000.
Laur CV, Keller HH. Making the case for nutrition screening in older adults in primary care. Nutr Today. 2017;52:129–36.
Keller HH, Hedley MR, Wong Brownlee S. The development of Seniors in the Community: Risk Evaluation for Eating and Nutrition (SCREEN). Can J Diet Pract Res. 2000;61:67–72.
Keller HH, Goy R, Kane SL. Validity and reliability of SCREEN II (Seniors in the community: risk evaluation for eating and nutrition, Version II). Eur J Clin Nutr. 2005;59:1149–57.
Keller HH, McKenzie JD, Goy RE. Construct validation and test-retest reliability of the seniors in the community: risk evaluation for eating and nutrition questionnaire. J Gerontol A Biol Sci Med Sci. 2001;56:M552–M558.
Ramage-Morin PL, Gilmour H, Rotermann M. Nutritional risk, hospitalization and mortality among community-dwelling Canadians aged 65 or older. Health Rep. 2017;28:17–27.
Power L, Mullally D, Gibney ER, Clarke M, Visser M, Volkert D, et al. A review of the validity of malnutrition screening tools used in older adults in community and healthcare settings - a MaNuEL study. Clin Nutr Espen. 2018;24:1–13.
Akhtar U, Keller HH, Tate RB, Lengyel CO. Construct validation of three nutrition questions using health and diet ratings in older Canadian males living in the community. Can J Diet Pract Res. 2015;76:194–9.
Raina PS, Wolfson C, Kirkland SA, Griffith LE, Oremus M, Patterson C, et al. The Canadian longitudinal study on aging (CLSA). Can J Aging. 2009;28:221–9.
Diener EF, Emmons RA, Larsen R, Griffin SJ. The satisfaction with life scale. J Pers Assess. 1985;49:71–75.
Cederholm T, Bosaeus I, Barazzoni R, Bauer J, Van Gossum A, Klek S, et al. Diagnostic criteria for malnutrition—an ESPEN consensus statement. Clin Nutr. 2015;34:335–40.
George LK, Fillenbaum GG. OARS methodology: a decade of experience in geriatric assessment. J Am Geriatr Soc. 1985;33:607–15.
Irwin A, Artin KH, Oxman MN. Screening for depression in the older adult: criterion validity of the 10-item Center for Epidemiological Studies Depression Scale (CES-D). Arch Intern Med. 1999;159:1701–4.
Sullivan GM, Feinn R. Using effect size–or why the P value is not enough. J Grad Med Educ. 2012;4:279–82.
Jones JM. Development of a nutritional screening or assessment tool using a multivariate technique. Nutrition. 2004;20:298–306.
Public Health England. England: Crown. 2015. https://www.gov.uk/government/publications/evidence-review-criteria-national-screening-programmes/criteria-for-appraising-the-viability-effectiveness-and-appropriateness-of-a-screening-programme. Accessed July 2018.
Hengeveld LM, Wijnhoven HA, Olthof MR, Brouwer IA, Harris TB, Kritchevsky B, et al. Prospective associations of poor diet quality with long-term incidence of protein-energy malnutrition in community-dwelling older adults: the Health, Aging, and Body Composition (Health ABC) study. Am J Clin Nutr. 2018;107:155–64.
Rosa CB, Garces SB, Hansen D, Brunelli AV, Bianchi PD, Coser J, et al. Malnutrition risk and hospitalization in elderly assisted in. Prim Care. 2017;22:575–82.
Chien MH, Guo HR. Nutritional status and falls in community-dwelling older people: a longitudinal study of a population-based random sample. PLoS ONE. 2014;9:e91044.
van der Pols-Vijlbrief R, Wijnhoven HA, Schaap LA, Terwee CB, Visser M. Determinants of protein-energy malnutrition in community-dwelling older adults: a systematic review of observational studies. Ageing Res. 2014;18:112–31.
Acknowledgements
This research was made possible using the data/biospecimens collected by the Canadian Longitudinal Study on Aging (CLSA). Funding for the Canadian Longitudinal Study on Aging (CLSA) is provided by the Government of Canada through the Canadian Institutes of Health Research (CIHR) under grant reference: LSA 9447 and the Canada Foundation for Innovation. This research has been conducted using the CLSA dataset Baseline Tracking Dataset version 3.3, Baseline Comprehensive Dataset version 3.2, under Application Number 170602. The CLSA is led by Drs. Parminder Raina, Christina Wolfson, and Susan Kirkland
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Morrison, J.M., Laur, C.V. & Keller, H.H. SCREEN III: working towards a condensed screening tool to detect nutrition risk in community-dwelling older adults using CLSA data. Eur J Clin Nutr 73, 1260–1269 (2019). https://doi.org/10.1038/s41430-019-0411-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-019-0411-3
This article is cited by
-
Social Network Factors Affect Nutrition Risk in Middle-Aged and Older Adults: Results from the Canadian Longitudinal Study on Aging
The Journal of nutrition, health and aging (2023)