Abstract
Background/objectives
Dietary carbohydrate quality and quantity fluctuate but it is unknown which attribute takes precedence in vascular health preservation. We investigated all four permutations of glycemic index (GI) and glycemic load (GL) on acute vascular and glycemic responses.
Subjects/methods
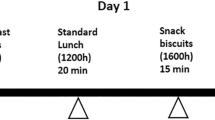
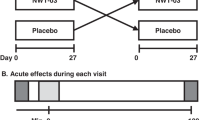
Twenty-one healthy adults were screened for this crossover trial. Seventeen (8 M:9 F; 26.7 ± 12.3 y; BMI 22.2 ± 2.8 kg/m2) entered randomization and completed the study, receiving four isocaloric meals, varying in GI and GL, in random order at least 3 days apart. The four meals included either chickpeas (GI = 28, GL = 14, 50 g available carbohydrates (CHO)), a small potato portion (GI = 85, GL = 14, CHO = 17 g), pasta (GI = 45, GL = 42, CHO = 94 g) or a large potato portion (GI = 85, GL = 42, CHO = 50 g) as the source of carbohydrate. Augmentation index (AIx) and central and peripheral blood pressure were measured fasting, 1, 2, 3, and 4 h post-consumption. Capillary blood glucose was analyzed fasting, 15, 30, 45, 60, 90, 120, 180, and 240 min.
Results
A reduction in AIx from baseline was observed 4 h following the chickpeas (low GI–low GL) (p = 0.046). The incremental area under blood glucose curves were significantly higher 2 h post-consumption following high compared with low GL meals (p < 0.001). Despite doubling carbohydrates, there was no difference in glycemic response between the large potato (high GI–high GL) and the pasta (low GI–high GL) meals. No significant differences in AIx or blood pressure were seen between meals.
Conclusions
Low GI, low-carbohydrate meals may support a healthy vascular tone. Varying meal GI and GL results in different glycemic profiles, which are not necessarily predicted by carbohydrate content. Further investigations on cardiometabolic profiles to meals varying in GI and GL are warranted.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Jenkins DJ, Wolever TM, Taylor RH, Barker H, Fielden H, Baldwin JM, et al. Glycemic index of foods: a physiological basis for carbohydrate exchange. Am J Clin Nutr. 1981;34:362–6.
Levitan EB, Song Y, Ford ES, Liu S. Is nondiabetic hyperglycemia a risk factor for cardiovascular disease? A meta-analysis of prospective studies. Arch Intern Med. 2004;164:2147–55.
Glucose tolerance and mortality: comparison of WHO and American Diabetes Association diagnostic criteria. The DECODE study group. European Diabetes Epidemiology Group. Diabetes epidemiology: collaborative analysis Of Diagnostic criteria in Europe. Lancet. 1999;354:617–21.
El-Osta A, Brasacchio D, Yao D, Pocai A, Jones PL, Roeder RG, et al. Transient high glucose causes persistent epigenetic changes and altered gene expression during subsequent normoglycemia. J Exp Med. 2008;205:2409–17.
Roberts AC, Porter KE. Cellular and molecular mechanisms of endothelial dysfunction in diabetes. Diabetes Vasc Dis Res. 2013;10:472–82.
Thijssen DH, Black MA, Pyke KE, Padilla J, Atkinson G, Harris RA, et al. Assessment of flow-mediated dilation in humans: a methodological and physiological guideline. Am J Physiol Heart Circ Physiol. 2011;300:H2–12.
Das Evcimen N, King GL. The role of protein kinase C activation and the vascular complications of diabetes. Pharmacol Res. 2007;55:498–510.
Vistoli G, De Maddis D, Cipak A, Zarkovic N, Carini M, Aldini G. Advanced glycoxidation and lipoxidation end products (AGEs and ALEs): an overview of their mechanisms of formation. Free Radic Res. 2013;47(Suppl 1):3–27.
Ahuja KD, Robertson IK, Ball MJ. Acute effects of food on postprandial blood pressure and measures of arterial stiffness in healthy humans. Am J Clin Nutr. 2009;90:298–303.
Greenfield JR, Samaras K, Chisholm DJ, Campbell LV. Effect of postprandial insulinemia and insulin resistance on measurement of arterial stiffness (augmentation index). Int J Cardiol. 2007;114:50–6.
Cai X, Wang C, Wang S, Cao G, Jin C, Yu J, et al. Carbohydrate intake, glycemic index, glycemic load, and stroke: a meta-analysis of prospective cohort studies. Asia-Pacific J Public Health/Asia-Pacific Academic Consortium for Public Health. 2015;27:486–96.
Dong JY, Zhang YH, Wang P, Qin LQ. Meta-analysis of dietary glycemic load and glycemic index in relation to risk of coronary heart disease. Am J Cardiol. 2012;109:1608–13.
Fan J, Song Y, Wang Y, Hui R, Zhang W. Dietary glycemic index, glycemic load, and risk of coronary heart disease, stroke, and stroke mortality: a systematic review with meta-analysis. PLoS ONE. 2012;7:e52182.
Mirrahimi A, de Souza RJ, Chiavaroli L, Sievenpiper JL, Beyene J, Hanley AJ, et al. Associations of glycemic index and load with coronary heart disease events: a systematic review and meta-analysis of prospective cohorts. J Am Heart Assoc. 2012;1:e000752.
Jovanovski E, Zurbau A, Vuksan V. Carbohydrates and endothelial function: is a low-carbohydrate diet or a low-glycemic index diet favourable for vascular health? Clin Nutr Res. 2015;4:69–75.
Recio-Rodriguez JI, Gomez-Marcos MA, Patino-Alonso MC, Rodrigo-De Pablo E, Cabrejas-Sanchez A, Arietaleanizbeaskoa MS, et al. Glycemic index, glycemic load, and pulse wave reflection in adults. Nutr Metab Cardiovasc Dis. 2015;25:68–74.
Lavi T, Karasik A, Koren-Morag N, Kanety H, Feinberg MS, Shechter M. The acute effect of various glycemic index dietary carbohydrates on endothelial function in nondiabetic overweight and obese subjects. J Am Coll Cardiol. 2009;53:2283–7.
Buscemi S, Cosentino L, Rosafio G, Morgana M, Mattina A, Sprini D, et al. Effects of hypocaloric diets with different glycemic indexes on endothelial function and glycemic variability in overweight and in obese adult patients at increased cardiovascular risk. Clin Nutr. 2013;32:346–52.
Philippou E, Bovill-Taylor C, Rajkumar C, Vampa ML, Ntatsaki E, Brynes AE, et al. Preliminary report: the effect of a 6-month dietary glycemic index manipulation in addition to healthy eating advice and weight loss on arterial compliance and 24-hour ambulatory blood pressure in men: a pilot study. Metabolism. 2009;58:1703–8.
Wolever TM, Jenkins DJ, Jenkins AL, Josse RG. The glycemic index: methodology and clinical implications. Am J Clin Nutr. 1991;54:846–54.
Arcaro G, Cretti A, Balzano S, Lechi A, Muggeo M, Bonora E, et al. Insulin causes endothelial dysfunction in humans: sites and mechanisms. Circulation. 2002;105:576–82.
Wolever TM. The glycaemic index: a physiological classification of dietary carbohydrates.. United Kingdom: CAB International; 2006.
Bao J, Atkinson F, Petocz P, Willett WC, Brand-Miller JC. Prediction of postprandial glycemia and insulinemia in lean, young, healthy adults: glycemic load compared with carbohydrate content alone. Am J Clin Nutr. 2011;93:984–96.
Wolever TM, Bolognesi C. Source and amount of carbohydrate affect postprandial glucose and insulin in normal subjects. J Nutr. 1996;126:2798–806.
de Graaf C, Blom WA, Smeets PA, Stafleu A, Hendriks HF. Biomarkers of satiation and satiety. Am J Clin Nutr. 2004;79:946–61.
Kissileff HR, Gruss LP, Thornton J, Jordan HA. The satiating efficiency of foods. Physiol Behav. 1984;32:319–32.
Schwingshackl L, Hoffmann G. Long-term effects of low-glycemic index/load vs. high glycemic index/load diets on parameters of obesity and obesity-associated risks: a systematic review and meta-analysis. Nutr Metab Cardiovasc Dis. 2013;23:699–706.
Fleming P, Godwin M. Low-glycaemic index diets in the management of blood lipids: a systematic review and meta-analysis. Fam Pract. 2013;30:485–91.
Ellison JM, Stegmann JM, Colner SL, Michael RH, Sharma MK, Ervin KR, et al. Rapid changes in postprandial blood glucose produce concentration differences at finger, forearm, and thigh sampling sites. Diabetes Care. 2002;25:961–4.
Spiller GA, Jensen CD, Pattison TS, Chuck CS, Whittam JH, Scala J. Effect of protein dose on serum glucose and insulin response to sugars. Am J Clin Nutr. 1987;46:474–80.
Wolever TM, Katzman-Relle L, Jenkins AL, Vuksan V, Josse RG, Jenkins DJA. Glycaemic index of 102 complex carbohydrate foods in patients with diabetes. Nutr Res. 1994;14:651–69.
Sawaya AL, Fuss PJ, Dallal GE, Tsay R, McCrory MA, Young V, et al. Meal palatability, substrate oxidation and blood glucose in young and older men. Physiol Behav. 2001;72:5–12.
Acknowledgements
This study was funded internally.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
ALJ is part owner and vice-president of Glycemic Index laboratories, Inc., (GI Labs) a contract research organization. AZ and FA-Y are contract research assistants for GI labs. TMSW and his wife receive payment as Officers and part owners of GI Lab. However, neither they, nor GI Labs, have any financial interest in any intellectual property developed as a result of research done at GI Labs, and have no equity in companies which produce or sell food products. VV was vice-president and partial owner of GI Labs from 2004 until 2015. He acted as a consultant to Salba Corporation, Buena Aires, Argentina (2003-2006), Core Naturals, FL, USA (2007–2008) and received conference travel grants from Salba Smart Natural Products (2008 and 2010), LLC, Centennial, CO, USA, and Source Salba Inc, Toronto, Canada (2008). VV holds an American (no. 7,326,404 B2) and Canadian (no. 2,410,556) patent for use of viscous fiber blend in diabetes, metabolic syndrome and cholesterol lowering; received a honorarium for a scientific advice from InovoBiologic (Calgary, AB., Canada) the producer of viscous fiber blend PGX® that is developed based on his patent. The remaining authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zurbau, A., Jenkins, A.L., Jovanovski, E. et al. Acute effect of equicaloric meals varying in glycemic index and glycemic load on arterial stiffness and glycemia in healthy adults: a randomized crossover trial. Eur J Clin Nutr 73, 79–85 (2019). https://doi.org/10.1038/s41430-018-0182-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-018-0182-2