Abstract
Background/objectives
To determine the association between cord blood 25-hydroxyvitamin D (25(OH)D) concentration with growth, adiposity and neurodevelopment during infancy.
Subjects/methods
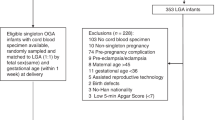
Serum 25(OH)D was measured in cord blood by the liquid chromatography tandem mass spectrometry (LC-MS/MS) from the Shanghai’s “Allergy and Obesity Cohort study” (n = 1244). Weight, length, head circumference, and body mass index (BMI) z-scores for age were calculated based on World Health Organization Standard (at 6 months, 1 years, and 2 years). Neurodevelopment was measured at 2 years using Ages and Stages Questionnaire. Generalized estimating equation and multivariable logistic regression model were exploited to examine associations between fetal 25(OH)D concentration and offspring outcomes.
Results
The median of the 25(OH)D concentration in cord blood was 22.4 ng/ml (interquartile range, 27.3–8.6). Infants born in winter had lower 25(OH)D concentration. 25(OH)D deficiency was not associated with weight z-score (mean difference, 0.07; 95% confidence internal (CI), −0.09 to 0.23), length z-score (mean difference, 0.01; 95% CI, −0.19 to 0.21), head circumference z-score (mean difference, −0.06; 95% CI, −0.27 to 0.15) and BMI z-score (mean difference, 0.09; 95% CI, −0.07 to 0.25) or neurodevelopment during infancy, adjusting for sex, socio-economic position, pre-pregnancy maternal BMI, and maternal and neonatal characteristics. The associations did not vary by gender. A sensitivity analysis of available case analysis showed virtually the same results.
Conclusions
Fetal vitamin D concentration was not associated with growth, adiposity or neurodevelopment during infancy. The role of vitamin D concentration and its mechanistic pathway in the early origins of adiposity needs to be clarified.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Holmes VA, Barnes MS, Alexander HD, McFaul P, Wallace JM. Vitamin D deficiency and insufficiency in pregnant women: a longitudinal study. Br J Nutr. 2009;102:876–81.
Salle BL, Delvin EE, Lapillonne A, Bishop NJ, Glorieux FH. Perinatal metabolism of vitamin D. Am J Clin Nutr. 2000;71:1317s–24s.
Barker DJ. The origins of the developmental origins theory. J Intern Med. 2007;261:412–17.
Young KA, Engelman CD, Langefeld CD, Hairston KG, Haffner SM, Bryer-Ash M, et al. Association of plasma vitamin D levels with adiposity in Hispanic and African Americans. J Clin Endocrinol Metab. 2009;94:3306–13.
Turer CB, Lin H, Flores G. Prevalence of vitamin D deficiency among overweight and obese US children. Pediatrics. 2013;131:e152–e161.
Olson ML, Maalouf NM, Oden JD, White PC, Hutchison MR. Vitamin D deficiency in obese children and its relationship to glucose homeostasis. J Clin Endocrinol Metab. 2012;97:279–85.
Morales E, Guxens M, Llop S, Rodriguez-Bernal CL, Tardon A, Riano I, et al. Circulating 25-hydroxyvitamin D3 in pregnancy and infant neuropsychological development. Pediatrics. 2012;130:e913–e920.
Gale CR, Robinson SM, Harvey NC, Javaid MK, Jiang B, Martyn CN, et al. Maternal vitamin D status during pregnancy and child outcomes. Eur J Clin Nutr. 2008;62:68–77.
Strøm M, Halldorsson TI, Hansen S, Granström C, Maslova E, Petersen SB, et al. Vitamin D measured in maternal serum and offspring neurodevelopmental outcomes: a prospective study with long-term follow-up. Ann Nutr Metab. 2014;64:254–61.
O’Loan J, Eyles DW, Kesby J, Ko P, McGrath JJ, Burne TH. Vitamin D deficiency during various stages of pregnancy in the rat; its impact on development and behaviour in adult offspring. Psychoneuroendocrinology. 2007;32:227–34.
Garcion E, Wion-Barbot N, Montero-Menei CN, Berger F, Wion D. New clues about vitamin D functions in the nervous system. Trends Endocrinol Metab. 2002;13:100–5.
Whitehouse AJ, Holt BJ, Serralha M, Holt PG, Kusel MM, Hart PH. Maternal serum vitamin D levels during pregnancy and offspring neurocognitive development. Pediatrics. 2012;129:485–93.
Baird J, Fisher D, Lucas P, Kleijnen J, Roberts H, Law C. Being big or growing fast: systematic review of size and growth in infancy and later obesity. BMJ. 2005;331:929.
Morales E, Rodriguez A, Valvi D, Iñiguez C, Esplugues A, Vioque J, et al. Deficit of vitamin D in pregnancy and growth and overweight in the offspring. Int J Obes. 2015;39:61–68.
Rice D, Barone S Jr. Critical periods of vulnerability for the developing nervous system: evidence from humans and animal models. Environ Health Perspect. 2000;108:511.
Yu X, Wang W, Wei Z, Ouyang F, Huang L, Wang X, et al. Vitamin D status and related factors in newborns in Shanghai, China. Nutrients. 2014;6:5600–10.
Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, et al. The2011 report on dietary reference intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know. J Clin Endocrinol Metab. 2011;96:53–58.
Zhao L, Wang W. Determinants of serum 25-hydroxyvitamin D2 and 25-hydroxyvitamin D3 concentrations in cord blood by liquid chromatography tandem-mass spectrometry. Lab Med. 2015;30:825–9.
Onis M. WHO child growth standards based on length/height, weight and age. Acta Paediatr. 2006;95(S450):76–85.
Squires J, Bricker D, Potter L. Revision of a parent-completed developmental screening tool: Ages and Stages Questionnaires. J Pediatr Psychol. 1997;22:313–28.
Limbos MM, Joyce DP. Comparison of the ASQ and PEDS in screening for developmental delay in children presenting for primary care. J Dev Behav Pediatr. 2011;32:499–511.
Kerstjens JM, Bos AF, ten Vergert EM, de Meer G, Butcher PR, Reijneveld SA. Support for the global feasibility of the Ages and Stages Questionnaire as developmental screener. Early Human Dev. 2009;85:443–7.
Schafer JL. Multiple imputation: a primer. Stat Methods Med Res. 1999;8:3–15.
Moons KG, Donders RA, Stijnen T, Harrell FE. Using the outcome for imputation of missing predictor values was preferred. J Clin Epidemiol. 2006;59:1092–101.
Graham JW, Olchowski AE, Gilreath TD. How many imputations are really needed? Some practical clarifications of multiple imputation theory. Prev Sci. 2007;8:206–13.
Mithal A, Wahl DA, Bonjour J-P, Burckhardt P, Dawson-Hughes B, Eisman JA, et al. Global vitamin D status and determinants of hypovitaminosis D. Osteoporos Int. 2009;20:1807–20.
Rockell JE, Green TJ, Skeaff CM, Whiting SJ, Taylor RW, Williams SM, et al. Season and ethnicity are determinants of serum 25-hydroxyvitamin D concentrations in New Zealand children aged 5–14 y. J Nutr. 2005;135:2602–8.
Chandler PD, Wang L, Zhang X, et al. Effect of vitamin D supplementation alone or with calcium on adiposity measures: a systematic review and meta-analysis of randomized controlled trials. Nutr Rev. 2015;73(9):577–593.
Krishnaveni GV, Veena SR, Winder NR, et al. Maternal vitamin D status during pregnancy and body composition and cardiovascular risk markers in Indian children: the Mysore Parthenon Study. Am J Clin Nutr. 2011;93(3):628–635.
Parikh SJ, Edelman M, Uwaifo GI, Freedman RJ, Semega-Janneh M, Reynolds J, et al. The relationship between obesity and serum 1, 25-dihydroxy vitamin D concentrations in healthy adults. J Clin Endocrinol Metab. 2004;89:1196–9.
Drincic AT, Armas LA, Diest EE, Heaney RP. Volumetric dilution, rather than sequestration best explains the low vitamin D status of obesity. Obesity. 2012;20:1444–8.
Van Eijsden M, Snijder M, Brouwer I, Vrijkotte T. Maternal early-pregnancy vitamin D status in relation to linear growth at the age of 5–6 years: results of the ABCD cohort. Eur J Clin Nutr. 2013;67:972–7.
Ong YL, Quah PL, Tint MT, Aris IM, Chen LW, van Dam RM, et al. The association of maternal vitamin D status with infant birth outcomes, postnatal growth and adiposity in the first 2 years of life in a multi-ethnic Asian population: the Growing Up in Singapore Towards healthy Outcomes (GUSTO) cohort study. Br J Nutr. 2016;116:621–31.
Gould JF, Anderson AJ, Yelland LN, Smithers LG, Skeaff CM, Zhou SJ, et al. Association of cord blood vitamin D with early childhood growth and neurodevelopment. J Paediatr Child Health. 2017;53:75–83.
Leffelaar ER, Vrijkotte TG, van Eijsden M. Maternal early pregnancy vitamin D status in relation to fetal and neonatal growth: results of the multi-ethnic Amsterdam Born Children and their Development cohort. Br J Nutr. 2010;104:108–17.
Eckhardt CL, Gernand AD, Roth DE, Bodnar LM. Maternal vitamin D status and infant anthropometry in a US multi-centre cohort study. Ann Human Biol. 2015;42:217–24.
Keim SA, Bodnar LM, Klebanoff MA. Maternal and cord blood 25 (OH)‐vitamin D concentrations in relation to child development and behaviour. Paediatr Perinat Epidemiol. 2014;28:434–44.
Wahl D, Cooper C, Ebeling P, Eggersdorfer M, Hilger J, Hoffmann K, et al. A global representation of vitamin D status in healthy populations. Arch Osteoporos. 2012;7:155–72.
Zhu P, Tong S-L, Hao J-H, Tao R-X, Huang K, Hu W-B, et al. Cord blood vitamin D and neurocognitive development are nonlinearly related in toddlers. J Nutr. 2015;145:1232–8.
Zhu P, Tong SL, Hu WB, et al. Cord Blood 25-hydroxyvitamin D and Fetal Growth in the China-Anhui Birth Cohort Study. Sci Rep. 2015;5:14930.
Acknowledgements
We thank our colleagues at Xinhua Hospital and the International Peace Maternal and Child health Hospital for their assistance and collaboration. Funding sources: This work was supported by the Chinese National Natural Science Foundation (No.81373004; No. 81372954; No. 81673178) and the Shanghai Science and Technology Commission (14XD1403300).
Author information
Authors and Affiliations
Contributions
HW and XDY preformed the literature review, accomplished the statistical analysis and wrote the drafted of the manuscript. LSH, QC, FXO, and XW contributed to analysis of the data, revise the paper critically. Zhang is the guarantor. He developed the hypothesis in the study, guided the strategy in the analysis procedure and supervised the draft of the paper. All authors have approved the final version of the manuscript.
Funding
The authors have no financial relationships relevant to this article to disclose.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
H Wang and X.D Yu contributed equally to this work.
Electronic supplementary material
41430_2017_75_MOESM2_ESM.docx
Appendix table 2 Association between umbilical cord blood 25(OH)D concentration and growth during infancy using complete analysis
41430_2017_75_MOESM3_ESM.docx
Appendix Table 3 Association between umbilical cord blood 25(OH)D concentration and neurodevelopment infants at 2 years using complete data
Rights and permissions
About this article
Cite this article
Wang, H., Yu, X.D., Huang, L.S. et al. Fetal vitamin D concentration and growth, adiposity and neurodevelopment during infancy. Eur J Clin Nutr 72, 1396–1403 (2018). https://doi.org/10.1038/s41430-017-0075-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-017-0075-9
This article is cited by
-
“You are my sunshine, my only sunshine”: maternal vitamin D status and supplementation in pregnancy and their effect on neonatal and childhood outcomes
Hormones (2023)
-
Maternal and neonatal blood vitamin D status and neurodevelopment at 24 months of age: a prospective birth cohort study
World Journal of Pediatrics (2023)
-
Neurodevelopmental effects of prenatal vitamin D in humans: systematic review and meta-analysis
Molecular Psychiatry (2020)