Abstract
Background/objectives
In 2004, a survey conducted in Scandinavia documented insufficient knowledge in nutrition care among doctors and nurses. The survey also revealed a significant discrepancy in nutritional practice, where Norway ranked lowest, thus leading to several actions including elaboration of national guidelines. The aim of this study was to evaluate potential changes in nutritional practice, as well as assessing barriers to nutrition therapy, 10 years after the former study.
Subjects/methods
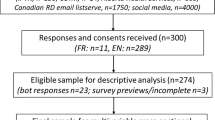
In the first half of 2014, a total of 4000 doctors and nurses received a questionnaire, similar to the one used in 2004. The questions dealt with nutritional practice, routines, knowledge, barriers, and use of clinical dietitians (CDs) in the hospitals.
Results
The response rate was 22%. Routines in nutritional practice were significantly improved. The level of knowledge among respondents were increased, but lack of knowledge and lack of assignment of responsibility were still important barriers. The patients’ contradiction could be a barrier to the use of enteral nutrition. CDs are used in a small amount of patients, and wards with good nutritional routines have a better cooperation with CDs than wards with insufficient routines.
Conclusions
Routines in clinical nutrition have improved from 2004 to 2014. Barriers in the daily practice among health care workers like lack of knowledge and lack of assignment of responsibility are still important, and health care professionals seem to let the patient himself or herself be a barrier to the use of enteral nutrition.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
McWhirter JP, Pennington CR. Incidence and recognition of malnutrition in hospital. BMJ (Clin Res Ed). 1994;308:945–8.
Tangvik RJ, Tell GS, Guttormsen AB, Eisman JA, Henriksen A, Nilsen RM, et al. Nutritional risk profile in a university hospital population. Clin Nutr. 2015;34:705–11.
Rasmussen HH, Kondrup J, Staun M, Ladefoged K, Kristensen H, Wengler A. Prevalence of patients at nutritional risk in Danish hospitals. Clin Nutr. 2004;23:1009–15.
Thoresen L, Frykholm G, Lydersen S, Ulveland H, Baracos V, Prado CM, et al. Nutritional status, cachexia and survival in patients with advanced colorectal carcinoma. Different assessment criteria for nutritional status provide unequal results. Clin Nutr. 2013;32:65–72.
Tangvik RJ, Guttormsen AB, Tell GS, Ranhoff AH. Implementation of nutritional guidelines in a university hospital monitored by repeated point prevalence surveys. Eur J Clin Nutr. 2012;66:388–93.
Kondrup J, Johansen N, Plum LM, Bak L, Larsen IH, Martinsen A, et al. Incidence of nutritional risk and causes of inadequate nutritional care in hospitals. Clin Nutr. 2002;21:461–8.
Correia MI, Waitzberg DL. The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr. 2003;22:235–9.
Laur C, Keller HH. Implementing best practice in hospital multidisciplinary nutritional care: an example of using the knowledge-to-action process for a research program. J Multidiscip Healthc. 2015;8:463–72.
Rasmussen HH, Kondrup J, Ladefoged K, Staun M. Clinical nutrition in danish hospitals: a questionnaire-based investigation among doctors and nurses. Clin Nutr. 1999;18:153–8.
Lindorff-Larsen K, Hojgaard Rasmussen H, Kondrup J, Staun M, Ladefoged K. Management and perception of hospital undernutrition-a positive change among Danish doctors and nurses. Clin Nutr. 2007;26:371–8.
Mowe M, Bosaeus I, Rasmussen HH, Kondrup J, Unosson M, Irtun O. Nutritional routines and attitudes among doctors and nurses in Scandinavia: a questionnaire based survey. Clin Nutr. 2006;25:524–32.
Thoresen L, Rothenberg E, Beck AM, Irtun O Doctors and nurses on wards with greater access to clinical dietitians have better focus on clinical nutrition. J Human Nutr Diet. 2008;21:239–47.
Mowe M, Bosaeus I, Rasmussen HH, Kondrup J, Unosson M, Rothenberg E, et al. Insufficient nutritional knowledge among health care workers? Clin Nutr. 2008;27:196–202.
Holst M, Staun M, Kondrup J, Bach-Dahl C, Rasmussen HH. Good nutritional practice in hospitals during an 8-year period: the impact of accreditation. e-SPEN J. 2014;9:e155–e60.
Cull WL, O’Connor KG, Sharp S, Tang SF. Response rates and response bias for 50 surveys of pediatricians. Health Serv Res. 2005;40:213–26.
Boynton PM. Administering, analysing and reporting your questionnaire. Br Med J. 2004;328:1372–5.
The Norwegian Ministry of Health and Care Services. Report No. 47 to the Storting (2008-2009) the coordination reform—proper treatment—at the right place and right time. 2009. https://www.regjeringen.no/contentassets/d4f0e16ad32e4bbd8d8ab5c21445a5dc/en-gb/pdfs/stm200820090047000en_pdfs.pdf.
The Norwegian Directorate of Health. National guidelines on preventing and treatment of malnutrition. 2009. https://helsedirektoratet.no/Lists/Publikasjoner/Attachments/916/Nasjonal-faglig-retningslinje-for-forebygging-og-behandling-av-underernering-IS-1580.pdf.
The Norwegian Directorate of Health. Nutritional competence in the health and care services. 2012. https://helsedirektoratet.no/Lists/Publikasjoner/Attachments/41/Erneringskompetanse-i-helse-og-omsorgstjenesten-oppdrag-fra-helse-og-omsorgsdepartementet-2009-2012-IS-2032.pdf.
The Norwegian Directorate of Health. National nutritional handbook. 2012. https://helsedirektoratet.no/Lists/Publikasjoner/Attachments/51/Kosthaandboken-IS-1972.pdf.
Juul H, Frich J. Screening for undernutrition in hospitals. What hinders and promotes nurses’ use of a screening tool for nutritional risk? Nord Nurse. 2013;3:77–89.
Eide HD, Halvorsen K, Almendingen K. Barriers to nutritional care for the undernourished hospitalised elderly: perspectives of nurses. J Clin Nurs. 2015;24:696–706.
Bailey N, Clark M, Nordlund M, Shelton M, Farver K. New paradigm in nutrition support: using evidence to drive practice. Crit Care Nurs Q. 2012;35:255–67.
Rufenacht U, Ruhlin M, Wegmann M, Imoberdorf R, Ballmer PE. Nutritional counseling improves quality of life and nutrient intake in hospitalized undernourished patients. Nutrition. 2010;26:53–60.
Braga JM, Hunt A, Pope J, Molaison E. Implementation of dietitian recommendations for enteral nutrition results in improved outcomes. J Am Diet Assoc. 2006;106:281–4.
Keller H, Allard JP, Laporte M, Davidson B, Payette H, Bernier P, et al. Predictors of dietitian consult on medical and surgical wards. Clin Nutr. 2015;34:1141–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Fjeldstad, S.H., Thoresen, L., Mowé, M. et al. Changes in nutritional care after implementing national guidelines—a 10-year follow-up study. Eur J Clin Nutr 72, 1000–1006 (2018). https://doi.org/10.1038/s41430-017-0050-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-017-0050-5
This article is cited by
-
Intervention-related, contextual and personal factors affecting the implementation of an evidence-based digital system for prevention and treatment of malnutrition in elderly institutionalized patients: a qualitative study
BMC Health Services Research (2023)
-
Comparison of nutritional risk screening with NRS2002 and the GLIM diagnostic criteria for malnutrition in hospitalized patients
Scientific Reports (2022)
-
Advancing European nutrition – are pharmacists eligible partners in the process?
European Journal of Clinical Nutrition (2021)