Abstract
Protein acetylation has emerged to play pivotal roles in alcoholic liver disease (ALD). Sirutin 2 (SIRT2) is a nicotinamide adenine dinucleotide (NAD+)-dependent deacetylase involved in the regulation of aging, metabolism, and stress. However, the role of SIRT2 in ALD remains unclear. Here, we report that the SIRT2-mediated deacetylation–deubiquitination switch of CCAAT/enhancer-binding protein beta (C/EBPβ) prevents ALD. Our results showed that hepatic SIRT2 protein expression was negatively correlated with the severity of alcoholic liver injury in ALD patients. Liver-specific SIRT2 deficiency sensitized mice to ALD, whereas transgenic SIRT2 overexpression in hepatocytes significantly prevented ethanol-induced liver injury via normalization of hepatic steatosis, lipid peroxidation, and hepatocyte apoptosis. Mechanistically, we identified C/EBPβ as a critical substrate of SIRT2 implicated in ALD. SIRT2-mediated deacetylation at lysines 102 and 211 decreased C/EBPβ ubiquitination, resulting in enhanced protein stability and subsequently increased transcription of C/EBPβ-target gene LCN2. Importantly, hepatic deacetylated C/EBPβ and LCN2 compensation reversed SIRT2 deletion-induced ALD aggravation in mice. Furthermore, C/EBPβ protein expression was positively correlated with SIRT2 and LCN2 expression in the livers of ALD patients and was inversely correlated with ALD development. Therefore, activating SIRT2-C/EBPβ-LCN2 signaling pathway is a potential therapy for ALD.
Similar content being viewed by others
Introduction
Alcoholic liver disease (ALD) is a major category of liver diseases, and the mortality from ALD continues to increase worldwide1,2. ALD encompasses several histopathologic changes, from simple steatosis to alcoholic steatohepatitis, progressive liver fibrosis, cirrhosis, and liver cancer2,3. Chronic alcohol intake promotes the accumulation of acetaldehyde and other reactive oxygen moieties in the liver, which leads to impaired hepatocyte metabolism, chronic oxidative stress, lipid peroxidation, hepatocytes damage, and death2,4. Although much research has investigated the pathogenesis and development of ALD, the underlying molecular mechanisms that defend against the detrimental effects of alcohol use remain elusive and current pharmacotherapy options are limited3,5,6. Therefore, the identification of novel therapeutic targets is an urgent clinical need in ALD.
Protein acetylation has emerged as a key posttranslational modification in alcohol metabolism6; yet, the regulation and mechanisms of the protein acetylation have not been completely understood in ALD. Sirtuins (SIRT) are a highly evolutionarily conserved family of nicotinamide adenine dinucleotide (NAD+)-dependent protein deacetylases. The seven homologs in the mammalian SIRT family (SIRT1–7) display diversity in tissue specificity, subcellular localization, enzymatic activity, and target selection7. SIRT1, SIRT6, and SIRT7 are mainly localized in the nucleus, where they deacetylate histones. SIRT3, SIRT4, and SIRT5 mainly localize in mitochondria7,8.
SIRT2 is the only sirtuin mainly located in the cytoplasm and abundantly expressed in the liver7. SIRT2 also may shuttle between the cytoplasm and nucleus during stress9. Growing evidence has suggested that SIRT2 plays an important role in the regulation of aging, glucose and lipid metabolism, cell differentiation, cell cycle, and tumorgenesis7,8. The previous work has demonstrated that SIRT2 maintains hepatic insulin sensitivity during physiological aging through deacetylation of NLRP310. However, the role of SIRT2 in ethanol-induced liver injury has not been described.
CCAAT/enhancer-binding protein beta (C/EBPβ) is an important transcription factor involved in numerous biological processes by regulating the expression of target genes, including adipogenesis, gluconeogenic pathway, liver regeneration, hematopoiesis, and apoptosis11. Moreover, the activity and stability of C/EBPβ may be post-translationally regulated by various modifications including acetylation12. Although elevation of C/EBPβ protein in ethanol-induced hepatosteatosis in mice has been observed13, the role and mechanism of the dysregulation and acetylation switch of C/EBPβ in ALD are still elusive. In this study, we identify SIRT2 as a novel deacetylase of C/EBPβ and uncover a critical protective function of SIRT2-mediated deacetylation–deubiquitination switch of C/EBPβ in ethanol-induced liver injury. Our in vivo findings suggest that SIRT2-C/EBPβ signaling pathway can be potentially targeted for ALD treatment.
Results
SIRT2 inversely correlates with ethanol-induced liver injury in patients
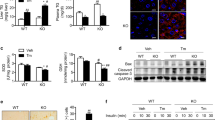
To assess the relevance of hepatic SIRT2 expression to alcoholic liver injury, we analyzed SIRT2 protein expression in liver samples from normal controls (n = 12) and patients with ALD (n = 102) (Supplementary Tables S1 and S2) by immunohistochemical (IHC) staining. The hepatic tissues presented different degrees of immunoreactive scores (IRS) of SIRT2, steatosis, and liver damage (Fig. 1a). The data revealed that SIRT2 protein level was significantly increased in the livers from ALD patients when compared to the normal controls through comparing the IRS of samples (Supplementary Fig. S1a). For the specimens from 102 patients, 54% of liver tissues showed higher SIRT2 expression (IRS > 5, SIRT2high), while 46% showed lower SIRT2 expression (IRS ≤ 5, SIRT2low) (Supplementary Fig. S1b). Then, we comprehensively evaluated the serum levels of alanine transaminase (ALT), aspartate transaminase (AST), and IRS of hepatic cleaved Caspase-3 (cl.Caspase-3), degree of necrosis, and fibrosis in the liver tissues of ALD patients. We found that the levels of serum ALT, AST, and hepatic cl.Caspase-3 expressions were much lower in the SIRT2high group than those of the SIRT2low group (Fig. 1b–d). The severity and stages of ALD may be identified by histopathologic changes. The alcoholic hepatitis histologic score (AHHS) model14 analysis results showed the reverse association between the expression of hepatic SIRT2 and the AHHS stage of ALD (Supplementary Fig. S1c). In addition, the liver injury score (LIS) model was used to focus on hepatic necrosis and fibrosis for making up the limitations of the AHHS model. SIRT2 protein expression was inversely correlated with ethanol-induced hepatic necrosis (Fig. 1e; Supplementary Fig. S1d) and fibrosis (Fig. 1f; Supplementary Fig. S1e). Collectively, our results showed that hepatic SIRT2 expression was negatively correlated to clinical ethanol-induced liver injury and the development of ALD.
a Representative IHC images of liver tissues from ALD patients for the lower (SIRT2low, IRS ≤ 5, n = 47) and higher (SIRT2high, IRS > 5, n = 55) expressions of SIRT2. The scale bar represents 50 μm. b–f Plots of serum ALT (b) and AST (c), cl.Caspase-3 IRS scores (d), and the percentages of liver tissues with high and low necrosis (e) or fibrosis (f) in SIRT2low and SIRT2high groups. Statistical significance was determined by two-tailed Student’s t-test (b–d), Pearson’s χ2 test (e, f). Data are shown as means ± SD and were considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001.
Liver-specific SIRT2 deficiency sensitizes mice to alcoholic liver injury
To further investigate the role of hepatic SIRT2 in ALD, we generated a liver-specific SIRT2-deficient mice using a floxed SIRT2 mouse strain and an Alb-Cre line (Supplementary Fig. S2a). Control SIRT2f/fAlb-Cre– (LoxP) and SIRT2f/fAlb-Cre+ (SIRT2-knockout (KO)) mice were genotyped by PCR and SIRT2 gene was efficiently deleted in the livers of SIRT2-KO mice (Supplementary Fig. S2b). The LoxP and SIRT2-KO mice were subjected to chronic-plus-binge ethanol feeding protocols (National Institute on Alcohol Abuse and Alcoholism (NIAAA) model) modified from the report by Bin Gao’s laboratory15. The pair-fed SIRT2-KO mice were phenotypically unremarkable (Fig. 2). Over the course of alcohol feeding, SIRT2-KO mice showed similar food intake, body weight, and organ to body weight ratios as LoxP mice (Supplementary Fig. S2c–g). However, the ethanol-fed SIRT2-KO mice displayed paler livers compared with the LoxP mice (Fig. 2a). Moreover, the hematoxylin–eosin (H&E) staining showed that the SIRT2-null livers on the ethanol diet had an increased number of vacuoles compared with those from LoxP mice (Fig. 2a), indicating more lipid accumulation. Similarly, liver triglyceride (TG) levels were significantly increased in the ethanol-fed SIRT2-KO mice (Fig. 2d). Meanwhile, ethanol-fed SIRT2-KO mice exhibited stronger lipid peroxidation in the livers as compared with ethanol-fed LoxP mice, indicated by the elevation of 4-hydroxynonenal (4-HNE) (Fig. 2a), malondialdehyde (MDA), and prostaglandin-endoperoxide synthase 2 (PTGS2) messenger RNA (mRNA) (Fig. 2e, f). Moreover, serum ALT and AST (Fig. 2b, c) levels, the number of terminal deoxynucleotidyl transferase dUTP nick end labeling (TUNEL)-positive hepatocytes (Fig. 2a, g), and cl.Caspase-3 expression (Fig. 2h) was markedly increased in the ethanol-fed SIRT2-KO mice, suggesting aggravated liver injury and apoptosis of hepatocytes. These results provide compelling evidence that liver-specific SIRT2 deficiency exacerbates ethanol-induced TG accumulation, lipid peroxidation, and hepatocyte apoptosis.
SIRT2f/fAlb-Cre– (LoxP) and SIRT2f/fAlb-Cre+ (SIRT2-KO) male mice were treated with pair (Pair) and ethanol diet (EtOH) according to NIAAA model (n = 8–10/group). a–h Liver injury, steatosis, lipid peroxidation, and cell apoptosis were assessed by images of the indicated livers (scale bar, 1 cm), mouse hepatic H&E staining (scale bar, 100 μm), IHC detection of 4-HNE and TUNEL (scale bar, 100 μm) (a), serum ALT (b) and AST (c), liver triglyceride (TG) (d), hepatic MDA content (e), and PTGS2 mRNA (f), quantitative analysis of TUNEL-positive hepatocytes (magnification, ×200) (g), Western blot analysis of cl.Caspase-3 in murine liver tissues (h). Student’s t-test was used for statistical evaluation. Data are shown as means ± SD and are considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001.
SIRT2 knockdown in a hepatocyte model of ALD leads to more apoptosis and lipid peroxidation
To verify the role of SIRT2 in a cell model, we created SIRT2 knockdown AML12 hepatocytes and assessed their response to ethanol exposure. Mouse AML12 hepatocytes efficiently metabolize ethanol and provide an adequate system to study how ethanol causes hepatocyte injury16. The cell count (Supplementary Fig. S3a, b), western blot analyses of Caspase-3 and PARP-1 cleavage (Supplementary Fig. S3c), and TUNEL assays (Supplementary Fig. S3d, e) demonstrated that SIRT2 knockdown caused more ethanol-induced hepatocyte apoptosis. Meanwhile, histological analysis revealed that SIRT2 knockdown caused an obvious elevation of ethanol-induced lipid ROS shown by C11-BODIPY and PTGS2 mRNA expression (Supplementary Fig. S3f, g). Together, these data indicate that SIRT2 knockdown results in increased ethanol-induced hepatocyte apoptosis with higher lipid peroxidation.
Hepatocyte-specific AAV8-mediated SIRT2 overexpression completely prevents ALD in mice
To assess the potential of SIRT2 to reverse alcoholic liver injury, we developed a recombinant adeno-associated viral vector serotype 8 (AAV8) expressing SIRT2 or its catalytic inactive SIRT2-H187A (H187A) mutant17,18 under the control of the hepatocyte-specific thyroxin-binding globulin (TBG) promoter (AAV8-SIRT2 and AAV8-H187A) (Supplementary Fig. S4a). The AAV8 vector contains a luciferase reporter gene for real-time observation of gene expression by bioluminescence imaging (BLI). We determined that the AAV8 constructs require 2 weeks for full and specific expression in the murine livers (Supplementary Fig. S4b). Therefore, we treated mice with 2 × 1011 viral particles containing AAV8-luciferase (Ctrl), AAV8-SIRT2, or AAV8-H187A construct via tail-vein injection 14 days before alcohol feeding (Supplementary Fig. S4c). In accordance with the BLI results (Supplementary Fig. S4d), PCR (Supplementary Fig. S4e) and western blot analysis (Fig. 3h) confirmed the hepatic SIRT2 and H187A overexpression in the AAV8-SIRT2 and AAV8-H187A groups. Hepatocyte-specific SIRT2 overexpression totally prevented ethanol-induced increases in 4-HNE staining (Fig. 3a), serum ALT and AST (Fig. 3b, c), liver TG content (Fig. 3d), MDA content (Fig. 3e), PTGS2 mRNA level (Fig. 3f), TUNEL-positive hepatocytes (Fig. 3a, g), and Caspase-3 cleavage (Fig. 3h), whereas H187A overexpression had no significant effects. Consistent with in vivo results, SIRT2 overexpression, but not H187A, led to less apoptosis in AML12 hepatocytes under ethanol exposure (Supplementary Fig. S5). Together, these data suggest that overexpression of SIRT2 in hepatocytes is sufficient to prevent ethanol-induced liver injury, connecting the protective role directly to SIRT2 catalytic activity.
Male C57BL/6 mice tail injected with AAV8-Ctrl (Ctrl), AAV8-SIRT2 (SIRT2), or AAV8-SIRT2-H187A (H187A) were treated with pair (Pair) and ethanol diet (EtOH) according to NIAAA model (n = 7/group). a Images of the indicated livers (scale bar, 1 cm), murine liver staining by H&E (scale bar, 50 μm), IHC detection of 4-HNE and TUNEL assay (scale bar, 100 μm). b–d Serum ALT (b) and AST (c) measurements and TG content (d). e–f Hepatic MDA measurements (e) and PTGS2 mRNA analysis by qRT-PCR (f). g Quantitative analysis of TUNEL-positive hepatocytes (magnification, ×200) in murine livers. h Western blot analysis of cl.Caspase-3 and SIRT2 expression in murine liver tissues. Student’s t-test was used for statistical evaluation. Data are shown as means ± SD and are considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001.
SIRT2 upregulates LCN2 expression
To explore how SIRT2 prevents ALD, we examined mRNA expression profiles in ALD mice livers by RNA-sequencing (RNA-seq) analysis. Altogether, 287 genes showed altered expression in 3/3 samples between livers from LoxP and SIRT2-KO mice with chronic-plus-binge feeding (> 2 fold, P < 0.05) (Supplementary Fig. S6a). Furthermore, when we subjected the RNA-seq data to gene set enrichment analysis, the top-ranked pathway affected by the SIRT2-KO was the acute-phase response (Supplementary Fig. S6b). Acute-phase proteins (APPs), mainly produced by hepatocytes, are the published acute-phase response signatures. Of note, RNA-seq and real-time reverse transcription-PCR (qRT-PCR) results showed the same direction of change of mRNA expression for most APPs (Fga, Fgg, Fgb, Orm1, lipocaline-2 (LCN2), Saa2, Saa1, Hp, Hpx, Orm2, and Saa3), in which SIRT2 deletion significantly suppressed ethanol-induced upregulation of APPs, even to the levels of pair-fed groups (Fig. 4a; Supplementary Fig. S6c). Among the most significantly regulated APPs, the previous studies reported that LCN2 functions as an antioxidant and plays an important role in protecting against liver injury19,20,21,22; therefore, we focused on whether LCN2 was regulated by SIRT2 in ALD. Consistent with in vivo results (Fig. 4b, c), SIRT2 knockdown significantly inhibited ethanol-induced elevation of LCN2 expression in AML12 hepatocytes (Fig. 4d, e). Meanwhile, wild-type SIRT2, but not its catalytically inactive H187A mutant, upregulated LCN2 mRNA and protein (Fig. 4f, g), connecting LCN2 expression directly to SIRT2 catalytic activity.
a Heatmap of differentially expressed genes associated with acute-phase response (Gene Ontology: 0006953) identified by RNA-seq using liver tissues from pair- or EtOH-fed LoxP or SIRT2-KO mice (n = 3). b, c qRT-PCR (b) and Western blot (c) analyses of LCN2 mRNA and protein expression in murine livers. d, e qRT-PCR (d) and Western blot analysis (e) of LCN2 expression in SIRT2 knockdown (SIRT2 KD) or control AML12 hepatocytes. f, g qRT-PCR (f) and Western blot analysis (g) of LCN2 in SIRT2 overexpression hepatocytes. h–o LoxP and SIRT2-KO male mice tail-vein injected with AAV8-Ctrl (Ctrl) or AAV8-LCN2 (LCN2) were treated with pair (Pair) or ethanol diet (EtOH) according to NIAAA model construction (n = 3–5/group). h Images of the indicated livers (scale bar, 1 cm), H&E staining of murine livers (scale bar, 50 μm), IHC detection of 4-HNE and TUNEL (scale bar, 100 μm). i, j Liver TG and MDA content of indicated mice. k Hepatic PTGS2 mRNA by qRT-PCR analysis of indicated mice. l, m Serum ALT and AST of indicated mice. n Quantitative analysis of TUNEL-positive hepatocytes (magnification, ×200). o Western blot analysis of cl.Caspase-3 protein in murine liver tissues. Student’s t-test was used for statistical evaluation. Data are shown as means ± SD and are considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001.
Hepatocyte-specific LCN2 overexpression completely prevents ALD in mice
To clarify the role of hepatocyte-expressing LCN2 in ALD, LoxP mice were given injections of either hepatocyte-specific expressed TBG-AAV8-LCN2 (LCN2) or AAV8-luciferase (Ctrl) prior to NIAAA alcohol construction. As shown in Supplementary Fig. S7, hepatocyte-specific LCN2 overexpression completely reversed ethanol-induced increases in the liver to body weight ratio (Supplementary Fig. S7b), TG accumulation (Supplementary Fig. S7c), lipid peroxidation (Supplementary Fig. S7a, d, e), serum ALT and AST (Supplementary Fig. S7f, g), and hepatocytes apoptosis (Supplementary Fig. S7a, h). Together, hepatic LCN2 plays a protective role in alcoholic liver injury.
SIRT2 protects against alcoholic liver injury by upregulating LCN2
To determine whether the protective effect of SIRT2 on ALD is mediated by upregulation of LCN2, LoxP and SIRT2-KO mice were given injections of either AAV8-luciferase (Ctrl) or AAV8-LCN2 (LCN2) prior to chronic-plus-binge feeding. The reverse of LCN2 expression was verified to be comparable to endogenous levels by western blot (Fig. 4o). Restoration of LCN2 expression in hepatocytes completely rescued the SIRT2 deletion-induced ALD aggravation, including liver TG accumulation (Fig. 4i), serum ALT and AST levels (Fig. 4l, m), lipid peroxidation (Fig. 4h, j, k), and hepatocyte apoptosis (Fig. 4h, n, o). Together, these results suggest that the aggravated alcoholic liver injury in SIRT2-KO mice is, to a large extent, a consequence of downregulated LCN2 expression in hepatocytes.
SIRT2 upregulates LCN2 through C/EBPβ under ethanol stress
Next, we addressed the mechanism by which LCN2 transcription is upregulated by SIRT2. Previous reports have shown that SIRT2 may deacetylate various transcription factors7,8. Therefore, we hypothesize that SIRT2 may regulate LCN2 transcription by affecting the expression or activity of certain transcription factors. Using the Match program (version 1.0), C/EBPβ was predicted as the only shared transcription factor on the six most significant SIRT2-regulated APPs (Fig. 5a). C/EBPβ protein was significantly upregulated in the livers of ethanol-fed mice, which paralleled the increased expression of LCN2 and SIRT2 (Fig. 5b). Furthermore, C/EBPβ positively regulated LCN2 mRNA expression in AML12 hepatocytes (Fig. 5c, d). To further validate the direct regulation of C/EBPβ on LCN2 transcription, we performed dual-luciferase reporter assay in HK293T and AML12 cells. C/EBPβ overexpression significantly increased the relative luciferase activity of the LCN2 promoter and rescued SIRT2 knockdown-caused suppression of luciferase activity both in HEK293T (Fig. 5e) and AML12 cells (Supplementary Fig. S8a). Then, according to previously reported chromatin immunoprecipitation-seq (ChIP-seq) data23 and via PROMO analysis (Fig. 5f, top), we predicted eight C/EBPβ binding sites at the LCN2 proximal promoter and designed six primers encompassing all binding sites (Fig. 5f, middle). ChIP assays showed that the fragments containing the sixth to eighth predicted C/EBPβ binding sites were mainly immunoprecipitated by anti-C/EBPβ antibodies and ethanol promoted the recruitment, indicating that −150 to ~−50 bp is the main binding region for C/EBPβ and mediated the upregulation of LCN2 by ethanol (Fig. 5f, bottom; Supplementary Fig. S8b). Furthermore, C/EBPβ or SIRT2 overexpression cannot increase the relative luciferase activity of LCN2 T-150 promoter truncation, in which −150 to −1 bp was deleted from the 3-kb LCN2 promoter (Supplementary Fig. S8c). The exogenous C/EBPβ overexpression reversed the suppression of LCN2 mRNA expression caused by SIRT2 knockdown under the ethanol exposure (Fig. 5g; Supplementary Fig. S8d). These results identified C/EBPβ as a novel transcription factor regulating LCN2 by directly binding to specific motifs in its promoter, which mediates the upregulation of LCN2 by SIRT2 under ethanol stress.
a Venn diagram shows common transcription factors predicted as the putative shared regulators on LCN2, Hp, Saa3, Saa1, Hpx, and Orm2. b Western blot analysis of hepatic LCN2, C/EBPβ, and SIRT2 expression in pair and EtOH-fed mice. c, d LCN2 mRNA expression after C/EBPβ knockdown (KD) or overexpression (C/EBPβ) in AML12 cells by qRT-PCR analysis. #P < 0.05 and ###P < 0.001 are used to indicate statistical significance compared between the group with EtOH treatment and the corresponding group without EtOH treatment. e Dual-luciferase reporter assay was performed in HK293T cells. Western blot analysis of C/EBPβ expression (top) and luciferase activities of the LCN2 promoter-reporter system (bottom) are shown. f UCSC Epigenome Browser tracks of the C/EBPβ ChIP-seq signal −3 kb before TSS of LCN2 from Cistrome DB ToolKit (top); information about predicted C/EBPβ binding sites and the primers targeting different sites on LCN2 promoter (middle); ChIP analysis showing C/EBPβ occupancy at the LCN2 proximal promoter in AML12 cells treated with EtOH and control (bottom). PPARγ and distant region primers were, respectively, used as a positive and negative control. g qRT-PCR analysis of LCN2 mRNA expression in SIRT2 knockdown AML12 cells transfected with C/EBPβ. Student’s t-test was used for statistical evaluation. Data are shown as means ± SD and are considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001.
SIRT2 deacetylates C/EBPβ
Since LCN2 mediates the protective role of SIRT2 and SIRT2 upregulates LCN2 through C/EBPβ in ALD, we investigated the mechanism by which SIRT2 regulates C/EBPβ. Immunofluorescence staining and western blot results showed that ethanol significantly increased the protein expression and nuclear colocalization of SIRT2 and C/EBPβ (Fig. 6a; Supplementary Fig. S9a). Meanwhile, the immunoprecipitation assay further validated that ethanol significantly enhanced endogenous interaction of C/EBPβ with SIRT2 (Fig. 6b) and suppressed endogenous C/EBPβ acetylation in AML12 hepatocytes (Fig. 6c). Moreover, coexpressing wild-type SIRT2, but not its catalytically inactive H187A mutant, with C/EBPβ caused a decrease of C/EBPβ acetylation level (Fig. 6d), connecting C/EBPβ deacetylation directly to SIRT2 catalytic activity. In contrast, Flag-C/EBPβ acetylation level was increased after endogenous SIRT2 was knocked down in AML12 cells (Fig. 6e). Of note, consistent with in vitro results, SIRT2, but not H187A mutant, inhibited the endogenous acetylation level of C/EBPβ in the livers of ALD mice (Supplementary Fig. S11a, b). Collectively, these data suggest that SIRT2 is a deacetylase of C/EBPβ.
a Immunofluorescence analysis of SIRT2 and C/EBPβ in AML12 cells treated with EtOH (scale bar, 50 μm). b Endogenous SIRT2–C/EBPβ interaction was analyzed by the amount of C/EBPβ coimmunoprecipitated with the same loading amount of SIRT2 in AML12 cells. c Acetylation levels of the same loading amount of endogenous C/EBPβ purified by IP in ethanol-treated AML12 cells detected by pan-acetyllysine antibody are shown, which indicates SIRT2 deacetylates C/EBPβ. d, e Acetylation levels of IP-purified Flag-C/EBPβ in HEK293T cells coexpressing SIRT2, SIRT2-H187A (d) or with SIRT2 knockdown (e). f, g qRT-PCR (f) and Western blot analysis (g) of C/EBPβ expression in SIRT2 knockdown or control AML12 cells treated with or without ethanol. h, i HEK293T cells co-transfected Flag-tagged C/EBPβ with the indicated plasmids or siRNA were treated with 10 μM MG132 or DMSO for 6 h. Ubiquitination level of C/EBPβ was probed by anti-HA antibody. j Ubiquitination levels of the same loading amount endogenous C/EBPβ purified by IP were probed by pan-ubiquitin antibody. k Acetylation levels of IP-purified C/EBPβ and its mutants in HEK293T cells with SIRT2 knockdown. K98R is used as a negative control. l Acetylation levels of IP-purified Flag-C/EBPβ and its mutants in HEK293T cells. m Ubiquitination levels of IP-purified Flag-C/EBPβ and its mutants in HEK293T cells with SIRT2 knockdown. n Ubiquitination levels of IP-purified Flag-C/EBPβ and its mutants in HEK293T cells. The experiments were repeated at least for three times with the same results, and the results of one representative experiment are shown.
SIRT2 decreases C/EBPβ ubiquitination and stabilizes C/EBPβ protein under ethanol stress
Acetylation has been identified as an evolutionarily conserved modification in proteins and plays important roles in protein stability24. Notably, SIRT2 knockdown had no effect on C/EBPβ transcription, but significantly decreased the C/EBPβ protein level in ethanol-treated AML12 cells and liver tissues (Fig. 6f, g; Supplementary Fig. S9b, c), suggesting that SIRT2 regulates C/EBPβ at posttranscriptional level. Both SIRT2 small interfering RNA (siRNA) and its inhibitor thiomyristoyl remarkably promoted C/EBPβ degradation upon cycloheximide treatment (Supplementary Fig. S10a, b). Furthermore, proteasome inhibitor MG132 treatment, but not the lysosome inhibitor chloroquine, completely reversed the downregulation of C/EBPβ protein by SIRT2 knockdown or inhibition (Supplementary Fig. S10c–f), suggesting that SIRT2 might stabilize C/EBPβ protein through inhibiting proteasome-mediated degradation. Consistent with this notion, wild-type SIRT2, but not H187A mutant, significantly decreased C/EBPβ ubiquitination (Fig. 6h), whereas SIRT2 knockdown or deficiency significantly enhanced C/EBPβ ubiquitination levels in vitro (Fig. 6i) and in vivo (Supplementary Fig. S11c, d). Importantly, SIRT2 deletion significantly rescued the ethanol-suppressed endogenous C/EBPβ ubiquitination level (Fig. 6j). These observations indicate that SIRT2-mediated deacetylation decreases C/EBPβ ubiquitination and enhances its protein stability under ethanol stress.
SIRT2 inhibits C/EBPβ ubiquitination by deacetylating lysines 102 and 211
To identify the C/EBPβ acetylation sites regulated by SIRT2, we transfected Flag-C/EBPβ with SIRT2 siRNA in HEK293T cells and then performed mass spectrometry (MS) analysis. MS analysis on purified C/EBPβ revealed that two lysine residues (K102/K211) were highly acetylated after SIRT2 knockdown (Supplementary Fig. S12a, b). A genomic analysis demonstrated that K102 and K211 are highly conserved among different species throughout evolution (Supplementary Fig. S12c). We further generated four single mutations by replacing K102 or K211 of C/EBPβ with an arginine (R) or a glutamine (Q), respectively, and analyzed the acetylation of these C/EBPβ mutants by SIRT2. The K to R mutation mimics the deacetylated state, whereas the K to Q mutation abolishes the positive charge and may act as a surrogate of acetylation25. Our results showed that either the K102R or K211R mutation completely reversed the enhancement of C/EBPβ acetylation and ubiquitination level caused by SIRT2 knockdown (Fig. 6k, m). Moreover, K102Q and K211Q mutants showed enhanced acetylation as compared with wild-type C/EBPβ in the presence of endogenous SIRT2 (Fig. 6l, n). These results indicate that acetylation of K102 and K211 mediates the regulation of SIRT2 on C/EBPβ protein stability.
C/EBPβ deacetylation reverses SIRT2 deletion-induced ALD aggravation
To determine whether the C/EBPβ acetylation switch in hepatocytes contributes to the protective role of SIRT2 against ALD in vivo, we treated ethanol-fed LoxP and SIRT2-KO mice with AAV8-C/EBPβ (C/EBPβ), AAV8-C/EBPβ K102R (K102R), and AAV8-C/EBPβ K211R (K211R) or AAV8-luciferase (Ctrl) viral particles via tail-vein injection. The five ethanol-fed groups showed similar food intake and body weight. Notably, K102R and K211R mutants reversed SIRT2 deficiency-aggravated alcoholic liver injury, including elevated liver to body weight ratio (Fig. 7b), TG accumulation (Fig. 7c), lipid peroxidation (Fig. 7a, d, e), serum ALT and AST level (Fig. 7f, g), and hepatocyte apoptosis (Fig. 7a, h, j). However, wild-type C/EBPβ had no effect on the enhancement of the lipid peroxidation (Fig. 7a, d, e) and hepatocyte apoptosis (Fig. 7a, h, j) caused by SIRT2 deletion. Consistent with the results in AML12 cells, K102R or K211R mutant protein level was significantly higher than that of wild-type C/EBPβ in SIRT2-KO murine livers (Fig. 7j), whereas the viral infection and transcription level were similarly indicated by BLI and qRT-PCR (data not shown). Importantly, this reversal of alcoholic liver injury was not due to non-physiological levels of C/EBPβ overexpression, because the reconstituted expression of K102R or K211R was comparable to endogenous C/EBPβ levels in ethanol-fed LoxP group (Fig. 7j). Moreover, both mRNA and protein level of target gene LCN2 paralleled the protein expression of C/EBPβ and mutants (Fig. 7i, j), which partially explained the different protective roles in ALD between wild-type C/EBPβ and K102R/K211R. Together, these data suggest that SIRT2-mediated C/EBPβ deacetylation and protein stability is directly linked to ethanol-induced liver injury in vivo.
LoxP and SIRT2-KO mice tail injected with AAV8-Ctrl (Ctrl) or AAV8-C/EBPβ (C/EBPβ) or AAV8-C/EBPβ K102R (K102R) or AAV8-C/EBPβ K211R (K211R) were treated with NIAAA model (n = 7/group). a–h The effects of wild-type C/EBPβ or constitutively deacetylated C/EBPβ mutants on steatosis, lipid peroxidation, and cell apoptosis were assessed by images of the indicated livers (scale bar, 1 cm), hepatic H&E staining (scale bar, 50 μm), IHC detection of 4-HNE and TUNEL (scale bar, 100 μm) (a), liver/body weight ratios (b), liver TG (c), hepatic MDA content (d), and PTGS2 mRNA (e), serum ALT (f), and AST (g), quantitative analysis of TUNEL-positive hepatocytes (magnification, ×200) (h). i Hepatic LCN2 mRNA analysis by qRT-PCR. j Western blot analysis of cl.Caspase-3, LCN2, C/EBPβ, and SIRT2 protein expression in the indicated livers. Student’s t-test was used for statistical evaluation. Data are shown as means ± SD and are considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001.
C/EBPβ inversely correlates with ALD and positively correlates with SIRT2 and LCN2 expression in patients
To further validate the relevance of hepatic C/EBPβ protein expression to ALD, we assessed C/EBPβ levels in liver tissues from 102 patients with ALD by IHC. The results showed that serum levels of ALT, AST, and hepatic cl.Caspase-3 expression were much lower in the C/EBPβhigh group than those in the C/EBPβlow group (Fig. 8a–c). Moreover, C/EBPβ protein expression was inversely correlated with ethanol-induced hepatic necrosis and fibrosis (Fig. 8d, e; Supplementary Fig. S13a, b), while being positively correlated with hepatic proliferation (Fig. 8f; Supplementary Fig. S13c). Furthermore, consistent with the results from mice and AML12 hepatocytes, SIRT2, C/EBPβ, and LCN2 protein expressions were positively correlated with each other in the livers of ALD patients (Fig. 8g–j). Collectively, our results suggest that SIRT2-C/EBPβ-LCN2 axis suppresses clinical alcoholic liver injury.
a–f Plots of serum ALT (a) and AST (b), cl.Caspase-3 IRS scores (c), the percentages of liver tissues with different degrees of necrosis (d), fibrosis (e), and proliferation (f) in ALD patients with high (C/EBPβhigh, n = 48) and low (C/EBPβlow, n = 54) C/EBPβ expressions. g Representative IHC images of patient liver samples for the low and high expressions of indicated proteins (scale bar, 100 μm). h–j Correlation analysis of relative protein expression of SIRT2, C/EBPβ, and LCN2 in liver tissues from ALD patients (n = 102). Statistical significance was determined by two-tailed Student’s t test (a–c), Pearson’s χ2 test (d–f), and linear correlation and regression (h–j). Data are shown as means ± SD and are considered statistically significant at **P < 0.01.
Discussion
The current study uncovers a critical protective role of SIRT2-mediated deacetylation of C/EBPβ against the ethanol-induced liver injury using patient specimens, along with animal and cell models. Mechanistically, we revealed for the first time that SIRT2 inhibits ubiquitination and degradation of C/EBPβ by deacetylation, and subsequently promotes the transcription of LCN2 under the ethanol stress. Importantly, this regulatory mechanism can be targeted to reverse the ethanol-induced liver injury. These findings establish SIRT2-C/EBPβ-LCN2 as a crucial axis protecting against ethanol-induced liver injury.
The liver is the major organ involved in alcohol degradation, oxidizing alcohol to acetaldehyde via alcohol dehydrogenase, and cytochrome P450 2E1 (CYP 2E1). In addition to the direct toxic effects of acetaldehyde production, chronic heavy alcohol consumption substantially upregulates and activates CYP2E1, which is associated with high production of reactive oxygen species (ROS). ROS attacks various subcellular organelles by initiating lipid peroxidation, with the generation of the products such as 4-HNE and MDA6. These lipid peroxidation products then lead to a chain reaction and liver injury. The role of SIRT2 in the modulation of oxidative stress through its different deacetylation targets is controversial. On the one hand, SIRT2 suppresses oxidative stress or increases antioxidant production and protects against cell apoptosis through deacetylating FOXO3a, PGC-1α, G6PD, NRF2, c-MYC, PGAM2, or regulating Mfn2, Drp1, and TFAM in mitochondria26,27. On the other hand, SIRT2 promotes oxidative stress-induced cell death through deacetylating PRDX-1, JNK, and S6K127,28,29. The methodologies in these previous studies did not allow for consideration of the differences caused by various stimulations and potential interaction among different organs in SIRT2-KO mice. In the present study, we used liver-specific KO mice and AAV8 viral expression system with hepatocyte-specific TBG promoter to investigate the role of hepatic SIRT2 in ALD. The current measurements of 4-HNE, MDA, and PTGS2 strongly suggest the protective roles of hepatic SIRT2-C/EBPβ-LCN2 axis against ethanol-induced oxidative stress and lipid peroxidation. Meanwhile, data were presented to show that SIRT2 mRNA and protein expression were elevated by ethanol. A previous study has reported that H2O2 or menadione does not change the transcriptional expression of SIRT225. Therefore, whether ethanol upregulates the SIRT2 transcription-independent of oxidative stress remains to be explored.
Accumulating previous studies reported that SIRT2 plays different roles in the fibrosis of various organs, including cardiac fibrosis, liver fibrosis, pancreatic fibrosis, pulmonary fibrosis, and renal fibrosis. On the one hand, SIRT2 acts as a protective deacetylase in cardiac fibrosis and SIRT2 deficiency exacerbates aging-related and angiotensin II (Ang II)-induced cardiac fibrosis through AMPK-LKB1 and NFAT signaling30,31. Moreover, the decreased expression of SIRT2 is associated with lipopolysaccharide or doxorubicin-induced cardiac fibrosis32,33. For the pancreas, SIRT2-KO induces extensive pancreatic fibrosis in the caerulein-induced pancreatitis mouse model34. On the other hand, a pro-fibrotic action of SIRT2 has been documented in renal and pulmonary fibrosis. Inhibition of SIRT2 alleviates renal tubulointerstitial fibrosis in the mouse model of obstructive nephropathy35,36 and pulmonary fibrosis in the ovalbumin-induced allergic airway inflammation murine model37. However, there are conflicting reports on the roles of SIRT2 in liver fibrosis. Li et al. reported that SIRT2 mediates the protective role of NAD+-boosting therapy in high-fat diet-induced fibrosis by deacetylation of Fndc538. On the contrary, in carbon tetrachloride- and thioacetamide-induced fibrosis mouse models, SIRT2 inhibition represses fibrogenic gene expression in hepatic stellate cells and prevents the development of hepatic fibrosis39. Therefore, the role of SIRT2 in fibrosis not only relates to the tissue specialty but also relates to the properties of the stimuli. In this study, the results from liver tissues of ALD patients display that hepatic SIRT2 was negatively associated with alcoholic liver fibrosis. Because NIAAA mice do not develop liver fibrosis, the more ideal mouse model may be helpful to further identify the roles of SIRT2 in alcoholic liver fibrosis.
In addition, there are various types of liver-resident immune cells40 and the pathogenesis and development of ALD are closely related to inflammation41. Our previous work demonstrated that SIRT2 in macrophages maintains hepatic insulin sensitivity through deacetylating NLRP310. However, the RNA-seq results showed that hepatocyte-specific SIRT2-KO had no impact on the alcohol-induced inflammation (Supplementary Fig. S6), which is further verified by similar infiltration of neutrophils and macrophages, phosphorylation of NF-κB-p65, and expression of IL-1β and MCP1 in the EtOH-fed livers of SIRT2-KO and LoxP mice (Supplementary Fig. S14).
Protein acetylation plays important roles in protein stability and has been reported to be involved in alcohol metabolism and ALD6. Here, using MS analysis and site-directed mutagenesis, we identified C/EBPβ as a novel and critical target of SIRT2 implicated in ALD. Moreover, unlike the regulation of transcriptional activity by acetylation42, the current data have revealed for the first time that acetylation switch may regulate C/EBPβ protein ubiquitination and stability. Our present work does not preclude the role of SIRT2 in the regulation of C/EBPβ transcriptional activation, but suggests a novel mechanism of regulating C/EBPβ protein stability at the posttranslation level. Moreover, K102R/K211R mutants, not wild-type C/EBPβ, may completely reverse the SIRT2 deletion-aggravated alcoholic liver injury by stabilizing C/EBPβ, supporting that SIRT2-mediated deacetylation-deubiquitination ‘switch’ is crucial for C/EBPβ to prevent ALD.
Our results showed that the polyubiquitination level of the K102R mutant was decreased compared with the WT C/EBPβ (Fig. 6m), suggesting the possibility that K102 is one of the ubiquitination sites. To further preclude that possibility, we mutated K to Q and found that K102Q mutation does not eliminate the polyubiquitination level, but elevates both ubiquitination and acetylation of C/EBPβ, suggesting that K102 is not the direct polyubiquitination site (Fig. 6l, n). C/EBPβ is a labile protein and is tightly controlled by polyubiquitination mediated by the E3 ubiquitin ligases Mdm2 and Nrdp1, and the ubiquitin-modifying enzyme A2011. The mechanisms by which SIRT2-mediated deacetylation regulates C/EBPβ polyubiquitination, including the identification of the ubiquitination sites of C/EBPβ, need further study.
LCN2 is an APP and a stress-responsive molecule that protects against various stresses. Accumulating previous studies reported that LCN2 functions as an antioxidant and plays an important role in protecting against liver injury19,20,21,22. On the other hand, Cai et al. reported that LCN2-KO mice were protected from ALD by reducing hepatic steatosis, liver injury, and neutrophil infiltration compared to WT controls43. However, in the same report, the authors indicated paradoxically that the protective phenotype observed in LCN2-KO mice was not seen in hepatocyte-specific LCN2-KO mice after ethanol administration. Given that LCN2 is secreted by a number of cell types, such as hepatocytes, neutrophils, adipocytes, and endothelia, the previous reports did not allow for consideration of the potential interaction among different organs in LCN2-KO mice44,45. In the current work, we have revealed for the first time the regulatory mechanism and protective roles of hepatocyte LCN2 in ALD using TBG-promoter AAV8 virus (Fig. 4; Supplementary Fig. S7). Meanwhile, we note that WT C/EBPβ did not promote the expression of LCN2 in alcoholic SIRT2-KO liver, but it was still able to reduce liver TG and serum ALT level (Fig. 7). This indicates that LCN2 is partially responsible for C/EBPβ acetylation-mediated phenotypes. The other targets of C/EBPβ in ALD need to be further studied in the future.
In the current study, we used the AHHS and LIS system to identify the correlation between hepatic SIRT2 and the severity of ALD. Although the results of the two analyses demonstrate an obvious reverse association between the expression of hepatic SIRT2 and liver injury/stage of ALD, the other scoring systems (e.g., MELD46) did not show the correlation. This may be because of the small sample size and selective bias from the hospital-based recruitment of only patients with the pathological test. Therefore, the patient sample size needs to be expanded in the future to comprehensively analyze the correlation between hepatic SIRT2-C/EBPβ-LCN2 axis and the liver injury in different types of ALD patients.
In conclusion, we have provided comprehensive evidence showing that hepatic SIRT2 stabilizes C/EBPβ protein via direct deacetylation at K102/K211, thereby promoting the expression of LCN2. This in turn prevents hepatic steatosis, lipid peroxidation, and hepatocyte apoptosis caused by ethanol consumption, and subsequently protects the mice against ethanol-induced liver injury. Conversely, deficiency in SIRT2 promotes the ubiquitination and degradation of C/EBPβ protein and aggravates ALD (shown in Model in Fig. 9). The inverse correlation between SIRT2-C/EBPβ-LCN2 axis expression and alcoholic liver injury in clinical samples further strengthen this novel mechanism. Remarkably, hepatocyte-specific reconstitution of LCN2 or deacetylated C/EBPβ mutants with AAV8 may completely reverse the SIRT2-KO mice phenotype with ethanol-fed mice. Moreover, hepatocyte-specific overexpression of LCN2 or SIRT2 with AAV8 may effectively protect mice against alcoholic liver injury. Therefore, future therapeutic interventions targeting the SIRT2-C/EBPβ-LCN2 signaling pathway may serve as a potential therapy for ALD.
Ethanol upregulated SIRT2 in hepatocytes, which directly deacetylates C/EBPβ on lysines 102 and 211 and inhibits ubiquitination of C/EBPβ, and subsequently promotes the transcription of LCN2. This in turn prevents oxidative stress and lipid peroxidation induced by ethanol. SIRT2 KO increases ubiquitination and degradation of C/EBPβ and aggravates ethanol-induced liver injury.
Materials and methods
Human study
Study subjects, including 102 patients with ALD and 12 controls without any evidence of liver diseases with paraffin-embedded hepatic biopsy tissues, were collected from the affiliated hospitals of Youjiang Medical University for Nationalities between January 2006 and December 2015. ALD was diagnosed based on the history of alcohol drinking and biopsy-diagnosed hepatic injury. Before samples were collected, we obtained Institutional Review Board approval. Demographic and clinicopathological information for all subjects, including gender, age, race, drinking and smoking information, and hepatic function, were obtained through the patients’ medical records, and detailed information is described in Supplementary Tables S1 and S2. This study was approved by the ethics committees of the participating hospitals and was carried out in accordance with the approved guidelines.
Animal models
The liver-specific SIRT2-KO mice were produced by crossing SIRT2flox/flox mice obtained from Johan Auwerxd Laboratory (Switzerland)47 and Alb-Cre mice purchased from Jackson Laboratory (USA) in a C57BL/6 background. Recombinant AAV8 constructs expressing targeted mouse SIRT2, SIRT2-H187A, LCN2, C/EBPβ, or mutated C/EBPβ (K101R and K102R) under the control of TBG promoter were generated by Sunbio Techservice Inc. (Shanghai, China). A noncoding plasmid carrying only the TBG promoter was used to produce control vector particles. All animals received care in compliance with protocols approved by the Institutional Animal Use and Care Committee of Shanghai Jiaotong University School of Medicine.
Statistical analysis
All the statistical analyses were performed by GraphPad Prism 7.02 (GraphPad Software Inc. La Jolla, CA). The Pearson’s χ2 test was used to evaluate the correlation between SIRT2 or C/EBPβ expression and hepatic necrosis, fibrosis, or proliferation degree. The correlations of relative protein expression of SIRT2, C/EBPβ, and LCN2 were analyzed using linear correlation and regression. Comparisons of the two groups were analyzed using the unpaired two-tailed Student’s t-test. For data with more than two groups, a one-way analysis of variance with Tukey’s multiple-comparison test was used. Data are shown as means ± standard deviation (SD) and are considered statistically significant at *P < 0.05, **P < 0.01, and ***P < 0.001. All experiments were repeated at least three times with the same results, and the results of one representative experiment are shown.
Additional methods can be found in Supplementary Data S1.
Change history
03 November 2023
A Correction to this paper has been published: https://doi.org/10.1038/s41421-023-00618-z
References
Kim, D. et al. Trends in mortality from extrahepatic complications in patients with chronic liver disease, from 2007 through 2017. Gastroenterology 157, 1055–1066.e1011 (2019).
Fuster, D. & Samet, J. H. Alcohol use in patients with chronic liver disease. N. Engl. J. Med. 379, 2579 (2018).
Satishchandran, A. et al. MicroRNA 122, regulated by GRLH2, protects livers of mice and patients from ethanol-induced liver disease. Gastroenterology 154, 238–252.e237 (2018).
Kim, H. G. et al. The epigenetic regulator SIRT6 protects the liver from alcohol-induced tissue injury by reducing oxidative stress in mice. J. Hepatol. 71, 960–969 (2019).
You, Y. et al. SNX10 mediates alcohol-induced liver injury and steatosis by regulating the activation of chaperone-mediated autophagy. J. Hepatol. 69, 129–141 (2018).
Teschke, R. Alcoholic liver disease: alcohol metabolism, cascade of molecular mechanisms, cellular targets, and clinical aspects. Biomedicines 6, 106 (2018).
Lin, S. et al. Sirtuins in mitochondrial stress: Indispensable helpers behind the scenes. Ageing Res. Rev. 44, 22–32 (2018).
Wang, Y., Yang, J., Hong, T., Chen, X. & Cui, L. SIRT2: Controversy and multiple roles in disease and physiology. Ageing Res. Rev. 55, 100961 (2019).
Inoue, T. et al. SIRT2, a tubulin deacetylase, acts to block the entry to chromosome condensation in response to mitotic stress. Oncogene 26, 945–957 (2007).
He, M. et al. An acetylation switch of the NLRP3 inflammasome regulates aging-associated chronic inflammation and insulin resistance. Cell Metab. 31, 580–591.e585 (2020).
Liu, S. S. et al. Targeting degradation of the transcription factor C/EBPbeta reduces lung fibrosis by restoring activity of the ubiquitin-editing enzyme A20 in macrophages. Immunity 51, 522–534.e527 (2019).
Liu, Y. et al. Protein inhibitor of activated STAT 1 (PIAS1) is identified as the SUMO E3 ligase of CCAAT/enhancer-binding protein beta (C/EBPbeta) during adipogenesis. Mol. Cell Biol. 33, 4606–4617 (2013).
Chen, Y. H., Yang, C. M., Chang, S. P. & Hu, M. L. C/EBP beta and C/EBP delta expression is elevated in the early phase of ethanol-induced hepatosteatosis in mice. Acta Pharm. Sin. 30, 1138–1143 (2009).
Altamirano, J. et al. A histologic scoring system for prognosis of patients with alcoholic hepatitis. Gastroenterology 146, 1231–1239.e1–6 (2014).
Bertola, A., Mathews, S., Ki, S. H., Wang, H. & Gao, B. Mouse model of chronic and binge ethanol feeding (the NIAAA model). Nat. Protoc. 8, 627–637 (2013).
Yin, H. et al. MicroRNA-217 promotes ethanol-induced fat accumulation in hepatocytes by down-regulating SIRT1. J. Biol. Chem. 287, 9817–9826 (2012).
Finnin, M. S., Donigian, J. R. & Pavletich, N. P. Structure of the histone deacetylase SIRT2. Nat. Struct. Biol. 8, 621–625 (2001).
Wang, F., Nguyen, M., Qin, F. X. & Tong, Q. SIRT2 deacetylates FOXO3a in response to oxidative stress and caloric restriction. Aging Cell 6, 505–514 (2007).
Xu, M. J. et al. Liver is the major source of elevated serum lipocalin-2 levels after bacterial infection or partial hepatectomy: a critical role for IL-6/STAT3. Hepatology 61, 692–702 (2015).
Li, H. et al. Hepatocytes and neutrophils cooperatively suppress bacterial infection by differentially regulating lipocalin-2 and neutrophil extracellular traps. Hepatology 68, 1604–1620 (2018).
Borkham-Kamphorst, E. et al. Protective effects of lipocalin-2 (LCN2) in acute liver injury suggest a novel function in liver homeostasis. Biochim. Biophys. Acta 1832, 660–673 (2013).
Yamada, Y. et al. Lipocalin 2 attenuates iron-related oxidative stress and prolongs the survival of ovarian clear cell carcinoma cells by up-regulating the CD44 variant. Free Radic. Res. 50, 414–425 (2016).
Zheng, R. et al. Cistrome Data Browser: expanded datasets and new tools for gene regulatory analysis. Nucleic Acids Res. 47, D729–D735 (2019).
Jiang, W. et al. Acetylation regulates gluconeogenesis by promoting PEPCK1 degradation via recruiting the UBR5 ubiquitin ligase. Mol. Cell 43, 33–44 (2011).
Wang, Y. P. et al. Regulation of G6PD acetylation by SIRT2 and KAT9 modulates NADPH homeostasis and cell survival during oxidative stress. EMBO J. 33, 1304–1320 (2014).
Lemos, V. et al. The NAD+-dependent deacetylase SIRT2 attenuates oxidative stress and mitochondrial dysfunction and improves insulin sensitivity in hepatocytes. Hum. Mol. Genet. 26, 4105–4117 (2017).
Singh, C. K. et al. The role of Sirtuins in antioxidant and redox signaling. Antioxid. Redox Signal. 28, 643–661 (2018).
Sarikhani, M. et al. SIRT2 regulates oxidative stress-induced cell death through deacetylation of c-Jun NH2-terminal kinase. Cell Death Differ. 25, 1638–1656 (2018).
Lee, D. H. et al. Inactivation of Sirtuin2 protects mice from acetaminophen-induced liver injury: possible involvement of ER stress and S6K1 activation. BMB Rep. 52, 190–195 (2019).
Tang, X. et al. SIRT2 acts as a cardioprotective deacetylase in pathological cardiac hypertrophy. Circulation 136, 2051–2067 (2017).
Sarikhani, M. et al. SIRT2 deacetylase represses NFAT transcription factor to maintain cardiac homeostasis. J. Biol. Chem. 293, 5281–5294 (2018).
Katare, P. B., Nizami, H. L., Paramesha, B., Dinda, A. K. & Banerjee, S. K. Activation of toll like receptor 4 (TLR4) promotes cardiomyocyte apoptosis through SIRT2 dependent p53 deacetylation. Sci. Rep. 10, 19232 (2020).
Zhao, D. et al. Adiponectin agonist ADP355 ameliorates doxorubicin-induced cardiotoxicity by decreasing cardiomyocyte apoptosis and oxidative stress. Biochem. Biophys. Res. Commun. 533, 304–312 (2020).
Quan, S. et al. Loss of Sirt2 increases and prolongs a caerulein-induced pancreatitis permissive phenotype and induces spontaneous oncogenic Kras mutations in mice. Sci. Rep. 8, 16501 (2018).
Ponnusamy, M. et al. Blocking sirtuin 1 and 2 inhibits renal interstitial fibroblast activation and attenuates renal interstitial fibrosis in obstructive nephropathy. J. Pharm. Exp. Ther. 350, 243–256 (2014).
He, F. F. et al. Inhibition of SIRT2 alleviates fibroblast activation and renal tubulointerstitial fibrosis via MDM2. Cell Physiol. Biochem. 46, 451–460 (2018).
Kim, Y. Y. et al. AGK2 ameliorates mast cell-mediated allergic airway inflammation and fibrosis by inhibiting FcepsilonRI/TGF-beta signaling pathway. Pharm. Res 159, 105027 (2020).
Li, D. J. et al. NAD(+)-boosting therapy alleviates nonalcoholic fatty liver disease via stimulating a novel exerkine Fndc5/irisin. Theranostics 11, 4381–4402 (2021).
Arteaga, M. et al. Inhibition of SIRT2 suppresses hepatic fibrosis. Am. J. Physiol. Gastrointest. Liver Physiol. 310, G1155–1168 (2016).
Zhao, J. et al. Single-cell RNA sequencing reveals the heterogeneity of liver-resident immune cells in human. Cell Discov. 6, 22 (2020).
Gao, B. & Tsukamoto, H. Inflammation in alcoholic and nonalcoholic fatty liver disease: friend or foe? Gastroenterology 150, 1704–1709 (2016).
Wiper-Bergeron, N., Salem, H. A., Tomlinson, J. J., Wu, D. & Hache, R. J. Glucocorticoid-stimulated preadipocyte differentiation is mediated through acetylation of C/EBPbeta by GCN5. Proc. Natl. Acad. Sci. USA 104, 2703–2708 (2007).
Cai, Y. et al. The detrimental role played by lipocalin-2 in alcoholic fatty liver in mice. Am. J. Pathol. 186, 2417–2428 (2016).
Wieser, V. et al. Lipocalin 2 drives neutrophilic inflammation in alcoholic liver disease. J. Hepatol. 64, 872–880 (2016).
Chen, J. et al. Hepatic lipocalin 2 promotes liver fibrosis and portal hypertension. Sci. Rep. 10, 15558 (2020).
Kamath, P. S. & Kim, W. R., Advanced Liver Disease Study, G. The model for end-stage liver disease (MELD). Hepatology 45, 797–805 (2007).
Lo Sasso, G. et al. SIRT2 deficiency modulates macrophage polarization and susceptibility to experimental colitis. PLoS ONE 9, e103573 (2014).
Acknowledgements
This study was funded by the National Natural Science Foundation of China (82070603, 92057118, 81470841, and 81772831, 81860489); Shanghai Natural Science Foundation (19ZR1428400 and 19ZR1440700); Shanghai Pujiang Program by Science and Technology Commission of Shanghai Municipality (16PJ1405400); Innovative research team of high-level local universities in Shanghai (SSMU-ZDCX20180800); Youth Science and Technology Innovation Studio of Shanghai Jiao Tong University School of Medicine (JYKCGZS15); Guangxi Natural Science Foundation (Nos. 2017GXNSFGA198002 and 2019AC19002). We thank Johan Auwerxd (Laboratory of Integrative Systems Physiology, NCEM, Ecole Polytechnique de Lausanne, Switzerland) for kindly providing the SIRT2flox/flox mice; Guoqiang Chen, Qing Zhong, Shaoming Shen, Xuyun Zhao (Shanghai Jiao Tong University School of Medicine), and Xiaoni Kong (Shanghai University of Traditional Chinese Medicine) for discussion; Core Facility of Basic Medical Sciences, Shanghai Jiao Tong University School of Medicine for the protein LC-MS analyses.
Author information
Authors and Affiliations
Contributions
M.H. conceived the project, designed and performed experiments, and analyzed data. Y.Z., X.L., X.R., Q.W., L.Z., L.W., D.H., L.L., D.W., and L.X. contributed to the acquisition and analysis of data as well as to the critical interpretation of the results. Y.Z., X.L., and X.R. performed most experiments. X.L. and Y.Z. collected and analyzed patient samples. Q.W., L.Z., L.W., D.H., L.L., D.W., and L.X. conducted partial experiments. Q.Z. and J.L. provided valuable suggestions. Q.Z. designed partial experiments and prepared the paper. M.H. wrote the manuscript with contributions from all authors.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, Y., Long, X., Ruan, X. et al. SIRT2-mediated deacetylation and deubiquitination of C/EBPβ prevents ethanol-induced liver injury. Cell Discov 7, 93 (2021). https://doi.org/10.1038/s41421-021-00326-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41421-021-00326-6
This article is cited by
-
Crosstalk of HDAC4, PP1, and GSDMD in controlling pyroptosis
Cell Death & Disease (2024)
-
Emerging role and therapeutic implications of p53 in intervertebral disc degeneration
Cell Death Discovery (2023)
-
Angiotensin-converting enzyme inhibitor promotes angiogenesis through Sp1/Sp3-mediated inhibition of notch signaling in male mice
Nature Communications (2023)
-
SIRT2 regulates extracellular vesicle-mediated liver–bone communication
Nature Metabolism (2023)
-
Protein acylation: mechanisms, biological functions and therapeutic targets
Signal Transduction and Targeted Therapy (2022)