Abstract
Raptor plays a critical role in mTORC1 signaling. High expression of Raptor is associated with resistance of cancer cells to PI3K/mTOR inhibitors. Here, we found that OTUB1-stabilized Raptor in a non-canonical manner. Using biochemical assays, we found that the tyrosine 26 residue (Y26) of OTUB1 played a critical role in the interaction between OTUB1 and Raptor. Furthermore, non-receptor tyrosine kinases (Src and SRMS kinases) induced phosphorylation of OTUB1 at Y26, which stabilized Raptor. Interestingly, phosphorylation of OTUB1 at Y26 did not affect the stability of other OTUB1-targeted substrates. However, dephosphorylation of OTUB1 destabilized Raptor and sensitized cancer cells to anti-cancer drugs via mitochondrial reactive oxygen species-mediated mitochondrial dysfunction. Furthermore, we detected high levels of phospho-OTUB1 and Raptor in samples of patients with renal clear carcinoma. Our results suggested that regulation of OTUB1 phosphorylation may be an effective and selective therapeutic target for treating cancers via down-regulation of Raptor.
Similar content being viewed by others
Introduction
Clear cell renal cell carcinoma (ccRCC) is the most common type of kidney cancer. Overexpression of hypoxia-inducible factor (HIF)-2α by the inactivated von Hippel Lindau (VHL) tumor suppressor gene is frequently detected in ccRCC, resulting in up-regulation of vascular endothelial growth factor (VEGF). Hence, inhibitors of the VEGF receptor (VEGFR) or the tyrosine kinase activity of the intracellular domain of VEGFR are used for treating ccRCC. However, side effects on VEGFR inhibitors have been reported, which limit their use [1]. In addition, the mammalian target of rapamycin (mTOR) pathway has been known to be frequently activated in the ccRCC [2, 3]. Inhibitors of mTORC1, such as everolimus and temsirolimus, have shown effective outcomes in clinical studies, albeit with certain limitations [4]. Therefore, various inhibitors, including inhibitors of mTORC1/2 and PI3K/mTORC1/2, have been developed and are being tested [5, 6].
The mTOR signaling pathway functions via mTORC1 and mTORC2 complexes. mTOR kinase, mLST8, DEPTOR, and Tti1/Tel2 are the proteins overlapping between these two complexes, while mTORC1 specifically contains Raptor and PRAS40 and mTORC2 contains Rictor and mSin1. Among these, Raptor and Rictor play critical roles in complex assembly, stability, localization, and regulation of mTOR signaling [7], and knockout of Raptor and Rictor disrupt functions of mTORC1 and mTORC2, respectively [8]. mTOR signaling is frequently activated by the activating mutation of the upstream kinase, PIK3CA, amplification or overexpression of mTORC complexes, and loss or mutation of negative regulators. In particular, patients with ccRCC harbor activating mTOR missense mutations, resulting in activation of mTORC1 rather than mTORC2 signaling [9]. Aberrant mTORC1 is known to contribute to tumorigenesis [10], because of which mTORC1 has been recognized as a therapeutic target for treating cancer [11]. Furthermore, up-regulation of Raptor correlates with resistance of renal cancer cells to PI3K-mTOR inhibitor [12], and up-regulation of Akt/Raptor is also associated with rapamycin resistance in breast cancer [13]. In contrast, down-regulation of Raptor sensitizes cancer cells to anti-cancer drug-induced cell death [14]. Therefore, inhibition of mTORC1 signaling via modulation of Raptor can constitute a novel strategy for treating cancers and reducing drug resistance.
Ubiquitination is a post-translational modification of proteins that determines their stability. The expression and function of proteins depend on the degree and linkage types of ubiquitination catalyzed by E3 ligases and deubiquitinases (DUBs). Perturbation of the balance between E3 ligase and DUB is closely related to tumorigenesis and the development of cancer [15]. Recently, DUBs have also been actively studied in cancer cells. Overexpression of ovarian tumor domain protease domain-containing ubiquitin aldehyde-binding proteins (OTUB1), a DUB, is related to poor prognosis of patients with colorectal cancer [16]. In addition, OTUB1 modulates tumorigenesis, invasion, and metastasis in multiple cancers [16, 17]. OTUB1 substrates vary with cancer cells, with some of the substrates being cIAP1 [18], p53 [19], Snail [20], FOXM1 (Forkhead box M1) [21], SLC7A11 [22], MSH [23], cyclin E1 [24], p100 [25], and DEPTOR [26]. However, studies regarding the mechanisms via which OTUB1 determines the regulation of specific substrates are lacking. In this study, we investigated the molecular mechanisms via which OTUB1 destabilizes Raptor. We have identified novel and important mechanisms via which OTUB1 selects its target. This will help researchers understand how the DUB recognizes the target.
Results
OTUB1 is a deubiquitinase that stabilized Raptor
Expression of Raptor is related to mTORC1 activation and anti-cancer drug resistance [8, 13]. However, the mechanism via which the stability of Raptor protein is regulated is largely unknown. To identify the DUB that stabilizes Raptor proteins, we first screened a siRNA library against 49 different DUBs and found that knockdown of OTUB1, USP53, and STAMBP significantly reduced Raptor protein expression (Fig. 1A and Fig. S1). To further identify the DUB that modulates the Raptor ubiquitination, we examined the binding between DUB and Raptor using ectopically expressed proteins. OTUB1, STAMBP, and USP53 interacted with Raptor (Fig. 1B); however, deubiquitination assays revealed that only OTUB1 was responsible for the deubiquitination of Raptor (Fig. 1C). OTUB1 knockdown increased ubiquitination of endogenous Raptor and decreased the expression of Raptor at the protein level, but not at the mRNA level (Fig. 1D–F). Furthermore, down-regulation of Raptor by OTUB1 knockdown was rescued by treatment with the proteasome inhibitor, MG132 (Fig. 1G), and OTUB1 overexpression increased Raptor expression (Fig. 1H). In addition, we observed that OTUB1 silencing decreased the stability of Raptor (Fig. 1I), whereas OTUB1 overexpression showed the opposite effect (Fig. 1J). In contrast, knockdown of STAMBP and USP53 decreased Raptor mRNA expression, and MG132 did not alter Raptor protein expression (Fig. S2). These data suggested that OTUB1 is the DUB that can modulate the stability of Raptor.
A Caki cells transfected with the GFP siRNA or 49 types of deubiquitinase siRNA were examined using western blotting for the Raptor proteins. The band intensity of Raptor was analyzed using ImageJ. B Caki cells were co-transfected with Flag-HA-DUB (OTUB1, USP53, and STAMBP) and pRK5-Myc-Raptor plasmids. The interaction was demonstrated using immunoprecipitation (IP). C HEK293T cells were co-transfected with Flag-HA-DUB and pRK5-Myc-Raptor plasmids in the presence of HA-Ub and treated with 0.5 µM MG132 for 6 h. Raptor ubiquitination was detected using an in vitro ubiquitination assay. D To analyze the ubiquitination of endogenous Raptor, Caki cells were co-transfected with HA-Ub and OTUB1 siRNA (siOTUB1) for the indicated time points. E–G Caki cells were transiently transfected with control siRNA (siCont) and siOTUB1 (E, F), and then incubated with 0.5 µM MG132 for 6 h (G). H Caki cells were transfected with different concentrations of the Flag-HA-OTUB1 plasmid. I, J Caki cells were transfected with siCont, two different sets of siOTUB1 (I) or pcDNA3.1(+), and Flag-HA-OTUB1 plasmid (J) and then treated with 20 µg/mL cycloheximide (CHX) for the indicated time points. The band intensity of Raptor was analyzed using ImageJ. The protein and mRNA expression levels were measured using western blotting and RT-PCR/qPCR, respectively. The band intensity of all proteins was analyzed using ImageJ. The values in graphs represent the mean ± SD of three independent experiments. *P < 0.01 compared to the Cont siRNA-transfected cells. #P < 0.05 compared to the MG132 in treatment OTUB1 siRNA-transfected cells. **P < 0.01 compared to the compared to vector-transfected cells. &P < 0.01 compared to the CHX treatment siCont-transfected cells. †P < 0.01 compared to the CHX treatment vector-transfected cells.
Tyrosine 26 residue of OTUB1 plays a critical role in inhibition of Raptor ubiquitination
Although OTUB1 is a DUB that removes ubiquitin chains [27], modulation of protein stability by OTUB1 is sometimes independent of its catalytic activity [28, 29]. Therefore, we investigated whether the catalytic activity of OTUB1 is necessary for modulation of Raptor stability. The catalytic C91 in the OTU domain of OTUB1 forms a catalytic triad with D88 and H265 when it comes in their proximity due to protein folding [28, 30, 31]. The OTUB1 C91S and D88A/C91S/H265A (ASA) mutants still suppressed the ubiquitination of Raptor (Fig. 2A). We also confirmed that the mutant forms of OTUB1, C91S, and ASA did not abolish the ability of OTUB1 to deubiquitinate endogenous Raptor (Fig. 2B). These data indicated that the catalytic activity of OTUB1 is not essential for modulation of Raptor stability.
A–D HEK293 cells (A, C) and Caki cells (B, D) were co-transfected with Flag-OTUB1 WT, mutant (OTUB1 C91S and ASA) (A, B) or Flag-OTUB1/Δ1-45 (C, D) plasmids in the presence of HA-Ub plasmid, following which the cells were treated with 0.5 µM MG132 for 6 h. The ubiquitination of Raptor was detected using in vitro (A, C) /endogenous (B, D) ubiquitination assay. E Caki cells were transfected with Flag-OTUB1 WT and four different sets of OTUB1 domain deletions (Δ1-10, Δ1-20, Δ1-30 and Δ1-45) in the presence of HA-Ub. Then, the cells were treated with 0.5 µM MG132 for 6 h. The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. F Caki cells were transfected with Flag-OTUB1 WT, Flag-OTUB1 2 mutants (N22A/C23A), and 3 mutants (Y26A/D27A/E28A) in the presence of HA-Ub, following which the cells were treated with MG132 for 6 h. The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. G, H Caki cells were transfected with plasmids harboring Flag-OTUB1 WT and each single mutant of Flag-OTUB1 (Y26A, D27A and E28A) (G) or Flag-OTUB1 (Y26A and Y26F) (H) in the presence of HA-Ub. The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. The band intensity of all proteins was analyzed using ImageJ. The values in graphs represent the mean ± SD of three independent experiments. *P < 0.05 compared to the vector-transfected cells. #P < 0.05 compared to the OTUB1 WT-transfected cells.
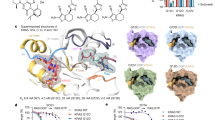
Next, we investigated the effect of OTUB1 ∆1-45, a mutant lacking the N-terminal part of OTUB1 containing a ubiquitin-binding site [31] on Raptor stability. As shown in Fig. 2C, D, OTUB1 ∆1-45 did not suppress the ubiquitination of Myc-Raptor or endogenous Raptor. To identify the critical site of OTUB1 responsible for the modulation of Raptor stability, we generated serial deletion mutant forms of OTUB1 (Fig. 2E). OTUB1 ∆1-20 induced deubiquitination of Raptor, while OTUB1 ∆1-30 did not, indicating that the 21−30 amino acids in N-terminus of OTUB1 are necessary for the deubiquitination of Raptor (Fig. 2E). Next, to identify the critical residue required for suppressing ubiquitination of Raptor, we changed five charged residues among amino acids 21−30 of OTUB1 to alanine (Fig. 2F). Interestingly, OTUB1 mutant 3 (Y26A/D27A/E28A) lost its deubiquitinase activity, while the effect of OTUB1 mutant 2 (N21A/C22A) was similar to that of OTUB1 wild type (WT) (Fig. 2F). We then compared the deubiquitinating activity of OTUB1 WT with that of OTUB1 Y26A, D27A, and E28A mutants. Among these three mutants, only the OTUB1 Y26A mutant did not deubiquitinate Raptor (Fig. 2G). We confirmed this using the OTUB1 Y26F mutant, in which phenylalanine did not induce any structural change in OTUB1, but did not deubiquitinate Raptor (Fig. 2H). Therefore, these data indicated that the Y26 residue of OTUB1 plays a critical role in stabilization of Raptor.
OTUB1 Y26A mutant increases mitochondrial dysfunction via down-regulation of Raptor
Previous studies have reported that Raptor plays a critical role in mitochondrial dynamics via Drp1 phosphorylation [14]. Therefore, we investigated whether OTUB1 modulated mitochondrial function via regulation of Raptor. We found that mitochondrial fusion increased dramatically in the OTUB1 Y26A mutant-transfected cells, which was reversed by the ectopic expression of Raptor (Fig. 3A). This phenomenon was consistent with the phosphorylation levels of Drp1 at serine 616, but total of Drp1 expression did not alter (Fig. 3B). Increase in mitochondrial fusion induced mitochondrial dysfunction and mitochondrial reactive oxygen species (ROS) production, which were also blocked by Raptor overexpression (Fig. 3C, D). In addition, we obtained similar results after OTUB1 knockdown (Fig. S3). Furthermore, we found that reconstitution of OTUB1 WT and Y26E (phospho-mimetic mutant form) in OTUB1 knockout (KO) cells restored phosphorylation of Drp1 at serine 616 and Raptor expression, but reconstitution of OTUB1 Y26A had no effect (Fig. 3E). OTUB1 KO also increased mitochondrial fusion, and reconstitution of OTUB1 WT reversed (Fig. 3F). We examined the effect of OTUB1 knockdown on expression of Opa1 and Mfns, which are related with mitochondrial dynamics. OTUB1 knockdown induced downregulation of Fis1 expression, and ectopic expression of Raptor reversed Fis1 expression (Fig. S3D). However, the expression levels of Opa1 and Mfns were not changed by OTUB1 knockdown (Fig. S3D). These data indicated that down-regulation of Raptor by OTUB1 Y26A or OTUB1 knockdown increases mitochondrial dysfunction.
A Representative confocal images of Caki/pDsRed2-mito cells co-transfected with Flag-OTUB1 WT, Flag-OTUB1 Y26A and Myc-Raptor. The nuclei were stained with DAPI, and the length of the mitochondria was measured using ZEN3.4. B–D Caki cells were transiently co-transfected with Flag-OTUB1 WT, Flag-OTUB1 Y26A and Myc-Raptor plasmids. Protein expression was detected using western blotting (B). Flow cytometry was used to detect the fluorescence intensity after mitochondrial damage (C). Mitochondrial ROS production was assessed after MitoSOX Red staining using microscopy and flow cytometry (D). E, F Representative confocal images of Caki/OTUB1 knockout (KO) cells were transiently co-transfected with plasmids harboring Flag-OTUB1 WT and each single mutant of Flag-OTUB1 (Y26A and Y26E) in the presence of pDsRed2-mito (F). Protein expression was detected using western blotting (E). The nuclei were stained with DAPI, and the length of the mitochondria was measured using ZEN3.4 (F). The band intensity of all proteins was analyzed using ImageJ. The values in graph A–F represent the mean ± SEM (A, F) or mean ± SD (B–E) of three independent experiments. *P < 0.001 compared to the vector-transfected cells. #P < 0.001 compared to the Flag-OTUB1 Y26A-transfected cells. †P < 0.05 compared to the compared to the vector-transfected cells. &P < 0.05 compared to the Flag-OTUB1 Y26A-transfected cells. **P < 0.01 compared to the vector-transfected OTUB1 KO cells. ##P < 0.001 compared to the vector-transfected OTUB1 KO cells.
Src and SRMS kinase plays a critical role in stabilizing Raptor
To identify the important role of the Y26 residue of OTUB1 on stabilization of well-known substrates, we examined the expression levels of target proteins after transfection with WT and Y26A mutant of OTUB1. Both the WT and Y26A mutant up-regulated most OTUB1 substrates, including cIAP1, p100 (NF-κB), MDMX, p53, Snail, SLC7A11, and Deptor. Interestingly, only Raptor was not up-regulated in OTUB1 Y26A-transfected cells (Fig. 4A). These results suggested that the Y26 residue of OTUB1 determines substrate specificity, at least partially, for Raptor.
A Caki cells were transiently transfected with vector, Flag-OTUB1 WT, and Flag-OTUB1 Y26A plasmids. B Phosphorylation of OTUB1 was detected using immunoprecipitation (IP) with anti-phospho-tyrosine antibody (4G10). C Caki cells were transiently transfected with vector, Flag-OTUB1 WT, Flag-OTUB1 Y26A, and Flag-OTUB1 Y26F plasmids. Phosphorylation of OTUB1 at Y26 was detected using western blotting with productive phospho-tyrosine 26 OTUB1 antibody. D Caki cells were transiently transfected with GFP siRNA or 85 types of tyrosine kinases siRNA. The band intensity of Raptor was analyzed using ImageJ. E Caki cells were treated with Src inhibitors or transiently transfected with Cont siRNA and Src siRNA in the presence of HA-Ub. The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. F Caki cell were transiently transfected with Cont siRNA, Src siRNA, or SRMS siRNA. G Caki cells were treated with 2 µM Src inhibitor (LCB03-0100 and KB SRC 4) for the indicated time points. H Caki cells were treated with Src inhibitors or transiently transfected with Cont siRNA and Src siRNA. The interaction was demonstrated using immunoprecipitation. I Caki cells were transiently transfected with vector, Flag-OTUB1 WT, Flag-OTUB1 Y26A and Flag-OTUB1 Y26F plasmids. Protein expression was detected using western blotting. The band intensity of all proteins was analyzed using ImageJ. The values in graphs represent the mean ± SD of three independent experiments. *P < 0.01 compared to control. #P < 0.01 compared to the Flag-OTUB1 WT-transfected cells.
To investigate how the Y26 residue of OTUB1 determines substrate specificity, we hypothesized that this residue may be phosphorylated. To prove this hypothesis, we transfected a Flag-OTUB1 plasmid, and performed immunoprecipitation with Flag-antibody and anti-phosphotyrosine antibody (clone 4G10), followed by western blotting with reciprocal antibodies, and detected OTUB1 phosphorylation (Fig. 4B). To further study the roles of Y26 phosphorylation, we generated phospho-Y26 specific antibodies (Fig. 4C). Next, to identify the tyrosine kinase responsible for the phosphorylation of OTUB1, we used siRNAs specific for tyrosine kinases. Among of them, knockdown of two non-receptor tyrosine kinases [Src and Src-related kinase lacking C-terminal regulatory tyrosine and N-terminal myristoylation sites (SRMS)] and two receptor tyrosine kinases (RET and RYK) dramatically decreased Raptor protein expression (Fig. 4D and Fig. S4A). Next, we investigated whether down-regulation of Raptor by Src kinase inhibition was related to increase in Raptor ubiquitination. As shown in Fig. 4E and Fig. S5, both Src inhibitors and Src knockdown increased Raptor ubiquitination, followed by increase in mitochondrial damage and ROS production. Interestingly, knockdown of Src or SRMS, but not that of RET and RYK kinase, dramatically decreased phosphorylation of OTUB1 on Y26 (Fig. 4F and Fig. S4B). To confirm these observations, we used two SRC inhibitors (LCB 03-0100 and KB SRC 4). Both inhibitors significantly decreased the phosphorylation of OTUB1 within 3 h, although OTUB1 level was not altered, and decreased the level of Raptor (Fig. 4G). Furthermore, we observed that the use of Src kinase inhibitors, Src knockdown, and OTUB1 mutations (Y26A and Y26F) inhibited the interaction between OTUB1 and Raptor (Fig. 4H, I). These data suggested that Src and SRMS kinases plays a critical role in interaction between OTUB1 and Raptor via phosphorylation of OTUB1 at Y26.
Phosphorylation of OTUB1 at tyrosine 26 by Src kinase plays a critical role in stabilizing Raptor
Next, we investigated the role of OTUB1 in modulation of Raptor expression by Src kinase. As mentioned above, it is confirmed that ubiquitination of Raptor was increased by Src knockdown and suppressed by OTUB1WT and Y26E overexpression (Fig. 5A). However, we did not detect increase of Raptor ubiquitination by Src knockdown when cells were overexpressed with OTUB1 Y26A (Fig. 5A). Furthermore, Src inhibitors did not induce mitochondrial fusion, mitochondrial dysfunction and mitochondrial ROS in OTUB1 Y26E (phospho-mimetic mutant form) transfected cells (Fig. 5B–D). We also found that phosphorylation of Drp1 was not altered by Src inhibitors in OTUB1 Y26E-transfected cells (Fig. 5E). In addition, we obtained similar results after Src knockdown (Fig. S6). These data suggested that Src-mediated Y26 phosphorylation of OTUB1 plays a critical role in stabilization of Raptor.
A Caki cells were co-transfected with plasmids harboring Flag-OTUB1 WT and each single mutant of Flag-OTUB1 (Y26A and Y26E) with Cont or Src siRNA in the presence of HA-Ub. The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. B Representative confocal images of Caki/pDsRed2-mito cells transfected with Flag-OTUB1 Y26E plasmid and then treated with 2 µM Src inhibitor (LCB03-0100 and KB SRC 4) for 24 h. The nuclei were stained with DAPI, and the length of the mitochondria was measured using ZEN3.4. C–E Caki cells were transiently transfected with Flag-OTUB1 Y26E plasmid and then treated with 2 µM Src inhibitor (LCB03-0100 and KB SRC 4) for 24 h. Flow cytometry was used to detect the fluorescence intensity after mitochondrial damage (C). Mitochondrial ROS production was assessed after MitoSOX Red staining using microscopy and flow cytometry (D). Protein expression was detected using western blotting (E). The band intensity of all proteins was analyzed using ImageJ. The values in graphs A–E represent the mean ± SEM (B) or mean ± SD (A, C–E) of three independent experiments. *P < 0.05 compared to control. #P < 0.05 compared to the Flage-OTUB1 WT-transfected cells. **P < 0.001 compared to vector-transfected cells. &P < 0.001 compared to the Src inhibitors treatment in vector-transfected cells.
UBC16, UBCH5A, and UBC13 E2 ligases are involved in the non-canonical DUB function of OTUB1
Previous studies have reported that the non-canonical activity of OTUB1 is mediated by inhibition of ubiquitin transfer from ubiquitin-charged E2 to substrate proteins [31], and that the N-terminal of OTUB1 interacts with several E2 enzymes [28]. Therefore, we investigated whether E2 ligase activity was involved in the deubiquitination of Raptor by OTUB1. Cells were transfected with WT, OTUB1 ∆1-45, and Y26 A mutant OTUB1, performed Flag-antibody immunoprecipitation, and we identified the E2 ligase (Fig. 6A). The OTUB1 ∆1-45 mutant did not interact with any of the tested E2 ligases, while UBC16, UBCH5A, and UBC13 did not complex with the OTUB1 Y26A mutant, confirming that they possibly inhibited the ubiquitination of OTUB1-mediated Raptor. As shown in Fig. 6B, OTUB1 knockdown decreased Raptor expression. However, knockdown of UBC16, UBCH5A, and UBC13 blocked the down-regulation of Raptor in OTUB1 siRNA-treated cells. Furthermore, knockdown of UBC16, UBCH5A, and UBC13 increased the expression of Raptor more than knockdown of other E2 ligases in cells ectopically expressing OTUB1 (Fig. 6C). Therefore, OTUB1-mediated stabilization of Raptor required UBC16, USCH5A, and UBC13.
A Caki cells were transiently transfected with vector, Flag-OTUB1 WT, and Flag-OTUB1 Y26A plasmids. The interaction was demonstrated using immunoprecipitation. B, C Caki cells were transiently co-transfected with OTUB1 siRNA (B) or Flag-OTUB1 plasmid (C) and six types of E2 siRNA. D Caki cells were transiently transfected with Raptor and Raptor mutants (K579R, K736R, K774R, and K789R). The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. E Caki cells were transiently co-transfected with OTUB1 siRNA and Raptor WT or Raptor mutants (K774R and K789R). The ubiquitination of endogenous Raptor was detected using the ubiquitination assay. F Caki cells were transiently transfected with Cont siRNA and Raptor siRNA. After 1 day, the cells were transfected with OTUB1 siRNA and Raptor or Raptor mutants (K579R, K736R, K774R, and K789R). Protein expression was detected using western blotting. The band intensity of all proteins was analyzed using ImageJ. The values in graphs represent the mean ± SD of three independent experiments. *P < 0.001 compared to control. #P < 0.05 compared to the Flag-OTUB1 Y26A-transfected cells. †P < 0.001 compared to the compared to the OTUB1 siRNA-transfected cells. &P < 0.001 compared to the Flag-OTUB1 WT plus Cont siRNA-transfected cells. **P < 0.01 compared to the Flag-OTUB1 WT-transfected cells. ##P < 0.001 compared to the Flag-OTUB1 WT plus OTUB1 siRNA-transfected cells.
Next, to identify the Raptor residues required for ubiquitination, we generated various Raptor mutants (K579R, K736R, K774R, and K789R). The K774R and K789R mutants dramatically blocked ubiquitination (Fig. 6D). The OTUB1 siRNA induced ubiquitination in Raptor WT, but not in K774R and K789R mutants (Fig. 6E). In addition, when cells were transfected with Raptor siRNA to remove the levels of endogenous Raptor, the K774R and K789R mutants were not degraded after treatment with the OTUB1 siRNA (Fig. 6F). These results suggested that the ubiquitination sites of K774 and K789 on Raptor are involved in OTUB1-mediated stabilization of Raptor.
Destabilization of Raptor by the OTUB1 Y26A mutant reduces tumor cell growth and sensitizes cancer cells to anti-cancer drugs
A previous study reported that Raptor silencing suppressed proliferation and colony formation in colon cancer cells [32]. Therefore, cancer cell proliferation and colony formation were studied to determine the physiological importance of OTUB1-mediated reduction in Raptor expression. First, we tested the effect of Raptor knockdown on colony formation and proliferation. shRNA-mediated Raptor knockdown inhibited colony formation and tumor cell growth (Fig. 7A). OTUB1 knockdown and the OTUB1 Y26A mutant also dramatically inhibited colony formation and tumor cell proliferation, which was rescued by ectopic expression of Raptor (Fig. 7B, C). In addition, as down-regulation of Raptor increased the sensitivity against anti-cancer drugs [14], we examined the effect of OTUB1-mediated Raptor modulation on cell death. Destabilization of Raptor by OTUB1 knockdown or in the OTUB1 Y26A mutant renal carcinoma Caki cells and lung carcinoma A549 cells sensitized these cancer cells to doxorubicin or oxaliplatin (Fig. 7D, E). Src knockdown and the use of Src inhibitors also sensitized the cancer cells to anti-cancer drugs (Fig. S7). Therefore, these data suggested that modulation of Raptor stabilization by OTUB1 may regulate tumor cell growth and death.
A Caki cells were transduced with lentivirus containing either a non-target (NT) or Raptor shRNA sequence. Colony formation was measured using crystal violet staining. Cell growth was determined using cell counting. B, C Caki cells were transiently co-transfected with Raptor and Cont siRNA (B), OTUB1 siRNA (B), Flag-OTUB1WT (C), or Flag-OTUB1 Y26A (C). Colony formation was measured using crystal violet staining. Cell growth was determined using cell counting. D, E Caki (D) and A549 (E) cells were transiently transfected with vector, Flag-OTUB1 WT, and Flag-OTUB1 Y26A plasmids, and then treated with 1 µM doxorubicin and 25 µM oxaliplatin for 24 h. Apoptosis and protein expression were measured using flow cytometry and western blotting. The values in graphs A–E represent the mean ± SD of three independent experiments. *P < 0.01 compared to the shNT-infected cells. #P < 0.01 compared to the vector and Cont siRNA-transfected cells. †P < 0.01 compared to the vector and OTUB1 siRNA-transfected cells. &P < 0.01 compared to the vector-transfected cells. $P < 0.01 compared to the Flag-OTUB1 Y26A-transfected cells. **P < 0.001 compared to the doxorubicin or oxaliplatin treatment in vector-transfected cells. ##P < 0.01 compared to doxorubicin or oxaliplatin treatment in Flag-OTUB1 Y26A-transfected cells.
Phosphorylation of tyrosine 26 OTUB1 correlates with Raptor and phospho-Drp1 (S616) in RCC patient tissues
To understand the role of Raptor in RCC, we assessed its level in RCC tissues from patients. The Yusenko Renal datasets were obtained from the Oncomine database (https://www.onco-mine.org/). Microarray analysis using this dataset demonstrated that Raptor mRNA expression in RCC cancer tissue was higher than that in normal kidneys (Fig. 8A) [33]. Kaplan–Meier curves generated using the data in Oncolnc (http://www.oncolnc.org/) showed that high expression of Raptor was related to poor prognosis in RCC patients (Fig. 8B). Next, we collected 40 specimens of human RCC tissues and analyzed the expression of Raptor, OTUB1, phospho-OTUB1 and -Drp1. The results revealed that phospho-OTUB1 (Y26), Raptor, and phospho-Drp1 (S616) were up-regulated in RCC tissues (Fig. 8C, D). The expression levels of these three proteins were quantified in all samples; results showed that 92.5% tumor samples (37/40) harbored phosphor-OTUB1 (Y26), 90.0% (36/40) expressed Raptor, and 90.0% (36/40) harbored phospho-Drp1 (S616), which were significantly higher than those in adjacent normal tissue (Fig. 8D). Moreover, Y26 phosphorylation of OTUB1 showed positive relationship with Raptor and phospho-Drp1(S616) (Fig. 8E). Overall, our results indicated that Tyr26 phosphorylation of OTUB1 modulates Raptor expression in a non-canonical manner, and that dephosphorylation of OTUB1 Tyr26 may be a novel therapeutic target for sensitizing cancer cell to anti-cancer drugs via down-regulation of Raptor expression. Collectively, our findings indicated that the Src/pOTUB1(Y26)/Raptor/pDRP1(S616) axis plays a critical role in sensitivity to anti-cancer drugs.
A Raptor mRNA expression in RCC cancer tissue and normal kidney using the Yusenko et al. renal cancer dataset from the Oncomine database (https://www.onco-mine.org/). B Survival analysis of the TCGA patient cohort in Oncolnc. n = 208. Patients from the TCGA cohort were divided into high and low Raptor-expressing groups based on the average Raptor expression level. C, D Investigation of protein expression in 40 paired primary renal tumor tissues and the corresponding normal adjacent tissues. E Correlation analysis of p-OTUB1/Raptor, p-Drp1/Raptor and p-OTUB1/p-Drp1 protein levels. F Scheme showing the mechanisms of OTUB1-mediated Raptor stabilization. The values in graphs A, B, D, E represent the mean ± SD of three independent experiments.
Discussion
Here, we aimed to investigate the mechanisms via which OTUB1 regulates the stability of Raptor and its relevance in the context of cancer prognosis. We identified a critical residue of OTUB1 that determines substrate specificity. Src or SRMS non-receptor tyrosine kinases phosphorylated the Y26 residue of OTUB1, and phosphorylated OTUB1Y26 bound only to Raptor, but not to other well-known substrates (p53, Snail, cIAP1, p100, and SLC7A11). The inability of the OTUB1 Y26A mutant to bind to Raptor resulted in down-regulation of the latter. Furthermore, we clearly demonstrated that OTUB1-mediated Raptor stabilization is associated with inhibition of the E2 ligase activity, but not the catalytic activity of OTUB1 (Fig. 8F). As a result, perturbation of mitochondrial function due to dephosphorylation of Y26 of OTUB1 sensitized cancer cells to anti-cancer drugs via down-regulation of Raptor.
The modulation of deubiquitination by OTUB1 might depend on its catalytic activity. The C91 residue in OTUB1 is critical for catalytic activity, and D88, C91, and H265 form a catalytic triad [28, 30, 31]. In this study, the OTUB1 C91S and ASA mutants were able to deubiquitinate Raptor (Fig. 2A, B); however, depletion of residues 1−45 in the N-terminus of OTUB1 abolished the deubiquitination of Raptor (Fig. 2C, D). OTUB1 commonly inhibits E2 ligase activity when it non-canonically modulates stabilization of its substrate, resulting in inhibition of ubiquitination. For example, OTUB1 inhibits ubiquitination of DNA-double strand break-induced chromatin and phospho-SMAD2/3 by inhibiting UBC13 [28] and UBE2D1 [30], respectively. Furthermore, OTUB1 suppresses MDM2-mediated p53 ubiquitination by inhibiting UBCH5 activity, and OTUB1 D88A impaired p53 stabilization [19]. However, the E2 binding site in OTUB1 is unclear. Nakada et al. have reported that OTUB1 C91S binds to UBC13, whereas OTUB1 ASA or ∆1-45 does not [28]. Binding of free ubiquitin to OTUB1 induced conformational changes to promote binding of UBC13 to OTUB1, and the N-terminal 16−45 residues in OTUB1 were critical for inhibition of ubiquitination by UBC13 [34]. In this study, the OTUB1 Y26 A mutant released UBC13, increasing ubiquitination of Raptor (Fig. 6A). Therefore, our results corroborated those of previous studies and further highlighted the importance of the Y26 residue of OTUB1. OTUB1 is known to regulate other E2 ligases, such as UBE2D1-3 and UBCH5A-C [28]; in addition, UBC16 and UBCH5A were also associated with destabilization of Raptor via its binding to OTUB1 (Fig. 6A–C). However, further studies are required to identify the detailed mechanisms via which each of these E2 ligases function.
OTUB1 stabilizes multiple proteins. However, how OTUB1 determines substrate specificity remains unknown. Here, we found that OTUB1 phosphorylated at Y26 specifically binds to Raptor and decreases its ubiquitination, resulting in up-regulation of Raptor. In contrast, the expression of other OTUB1 target proteins (cIAP1, p100, MDMX, p53, Snail, SLC7A11, and Deptor) was not affected by OTUB1 Y26 phosphorylation. A recent study showed that casein kinase 2 induces phosphorylation of OTUB1 at S16, which was critical for repair after ionizing radiation-induced DNA damage. However, phosphorylation of OTUB1 at S16 is independent of its deubiquitinase activity [35]. In contrast, Edelmann et al. reported that phosphorylation of OTUB1 at S16, S18, and Y26 modulates susceptibility to Yersinia invasion by stabilizing the active RhoA protein in a catalytic activity-dependent manner [36]. This indicated that phosphorylation of OTUB1 at Y26 reduces canonical OTUB1 function by interfering with its enzymatic activity, ubiquitin binding, or substrate recognition [36]. Here, we identified for the first time that phosphorylation of OTUB1 at Y26 specifically stabilizes Raptor by regulating their mutual binding.
Src kinase of the Src family tyrosine kinases (SFKs), a large class of non-receptor kinases, plays multiple roles in oncogenic processes such as cell proliferation, angiogenesis, migration, and invasion of cancer cells [37]. Activation of Src kinase and mTORC1 signaling are easily detected in cancers, although studies on the relationship between the two kinases is scarce. Here, we showed that Src and SRMS kinase are key tyrosine kinases that regulate Raptor expression via phosphorylation of OTUB1. Rituraj et al. has reported that amino acid-induced Src kinase recruits mTORC1 from the cytosol to the lysosome membrane by disrupting its interaction with GATOR1 and Rag GTPase, resulting in activation of mTORC1 signaling [38]. They suggested that activation of Src kinase is necessary and sufficient to activate mTORC1 signaling. Ondrušová et al. also reported that Src kinase binds to Raptor, and that a Src kinase inhibitor decreases phosphorylation of mTOR at S2448 and S6K [39]. Interestingly, as mTORC1 mediates negative feedback of Akt activation, mTORC1 inhibitor activates Akt signaling to promote drug resistance. However, Src kinase-mediated mTORC1 activation is independent of Akt/TSC2 signaling, as Akt activation is not induced, unlike that of rapamycin [38, 40]. We also found that OTUB1 knockdown only inhibits mTORC1 signaling [phospho-mTOR (S2448), p-4EBP1, and p-S6K], but not mTORC2 signaling [phospho-mTOR(S2481) and p-Akt] (Fig. S8). Therefore, we speculated that inhibition of mTORC1 by the Src kinase-OTUB1-Raptor axis may be an effective and selective therapeutic target for treating cancers. Indeed, results of our and previous studies have revealed a close link between Src kinase and mTORC1 signaling.
SRMS is also non-receptor tyrosine kinase composed of 488 amino acids [41]. SRMS mutant mice generated via gene targeting in embryonic stem cells displayed no apparent phenotype [42], suggesting that the functions of SRMS are redundant. However, SRMS promotes tumor growth and inhibits autophagy in cancer cells [43]. In addition, siRNA-mediated SRMS knockdown increases LC3 puncta in an mTORC1-independent manner [44]. Docking protein 1 (Dok1) [45], vimentin, and Sam68 [46] was found to be substrates of SRMS. In our study, SRMS knockdown dramatically decreased the phosphorylation of OTUB1, resulting in down-regulation of Raptor, indicating that OTUB1 could be a substrate of SRMS.
Few studies have investigated regulation of Raptor expression at the post-translational level. Bridges et al. reported that USP9X directly binds to Raptor and inhibits its proteasomal degradation, resulting in activation of the mTORC1 signaling in neural progenitor cells [47]. In addition, UCHL1 also inhibits the ubiquitination of Raptor in mTORC1, thereby destabilizing mTORC1 via a non-degradative mechanism [48]. In our study, knockdown of USP53, STAMBP, and OTUB1 down-regulated Raptor (Fig. 1A); among these DUBs, only OTUB1 reduced Raptor ubiquitination (Fig. 1C). USP9X knockdown decreased Raptor expression slightly, albeit not significantly (Fig. S1). The different effects of USP9X on stabilization of Raptor may be because of the differences between normal and cancer cells.
In conclusion, this study clearly demonstrated that phosphorylation of OTUB1 at Y26 by Src or SRMS kinase determines substrate specificity, and that phosphorylation of OTUB1 at Y26 stabilizes Raptor protein via inhibition of ubiquitin transfer by UBC16, UBCH5A, and UBC13 E2 ligase. Therefore, dephosphorylation of OTUB1 resulted in Raptor down-regulation, which increased the sensitivity against anti-cancer drugs. This suggested that targeting of OTUB1 phosphorylation may be an effective and selective therapeutic target for treating cancers.
Materials and methods
Cells and materials
Caki, HEK293T, and A549 cells were cultured in appropriate medium containing 10% fetal bovine serum (FBS; Welgene, Gyeongsan, Korea), 1% penicillin-streptomycin, and 100 µg/mL gentamycin (Thermo Fisher Scientific, Waltham, MA, USA). All cell lines tested negative for Mycoplasma contamination. The authenticity of the cell lines was verified using standard morphological examination with a microscope. More detailed information about the materials is described in Table S1.
Knockdown using siRNA and shRNA
Raptor siRNA was purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA), and siRNAs targeting GFP (control), various DUBs, and tyrosine kinase were obtained from Bioneer (Daejeon, Korea). Information regarding the siRNAs used in this study are listed in Table S3. The siRNAs were transfected into Caki cells using Lipofectamine RNAiMAX (Thermo Fisher Scientific, Waltham, MA, USA). HEK293TN cells were transfected with the non-target shRNA or Raptor shRNA in the presence of pMD2.G/psPAX2.0 plasmids using TransIT-2020 reagents (Mirus Bio, Madison, WI, USA). After transfection, the supernatants were filtered and infected into Caki cells using 8 µg/mL polybrene. Information regarding used siRNAs is described in Table S2.
Western blotting
Western blotting was performed according to methods described in our previous study [49]. In brief, cells were washed with cold PBS and lysed on ice in 50 μL of lysis buffer (50 mM Tris-HCl, 1 mM EGTA, 1% Triton X-100, 1 mM phenylmethylsulfonyl fluoride, pH 7.5). Lysates were centrifuged at 10,000 × g for 15 min at 4 °C, and the supernatant fractions were collected, boiled with 5× sample buffer, and separated using sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE). Then, the proteins were transferred to a nitrocellulose membrane and probed with specific antibodies, which were detected using enhanced chemiluminescence (ECL) solution (EMD Millipore, Darmstadt, Germany). Information regarding used antibodies in this study is described in Table S3. Full-length original western blots in this article are provided in Supplementary File.
Immunoprecipitation
To analyze protein-protein interactions, immunoprecipitation was performed according to the methods described in our previous study [50]. Briefly, cells were lysed in CHAPS lysis buffer and incubated overnight with primary antibodies (Table S3). Then, the lysates were treated with protein G agarose beads (Santa Cruz Biotechnology (Santa Cruz, CA, USA) for 2 h. After centrifugation, the supernatants were removed and the pellets were boiled using 2× sample buffer. Protein interaction was detected using western blotting.
Ubiquitination assay
This assay was performed using a tagged-ubiquitin plasmid and after pretreatment with MG132 as reported previously [51]. Briefly, the cells were harvested, washed with phosphate buffered saline (PBS) containing 10 mM N-ethylmaleimide (NEM) (EMD Millipore, Darmstadt, Germany), resuspended in 90 µL PBS/NEM containing 1% SDS, and boiled for 10 min at 95 °C. The lysates were added to lysis buffer containing 1 mM phenylmethylsulfonyl fluoride (PMSF) and 5 mM NEM, resuspended 3−4 times using an l mL syringe and centrifuged at 13,000 × g for 10 min at 4 °C. The supernatants were incubated overnight with primary antibody against target proteins and reacted by adding protein G agarose bead for 2 h. After centrifugation, the supernatants were removed, washed twice with lysis buffer containing 1 mM PMSF and 5 mM NEM, and boiled using 2× sample buffer for 10 min. Ubiquitinated Raptor was detected using horse radish peroxidase (HRP)-conjugated anti-Ub.
Reverse transcription-polymerase chain reaction (RT-PCR)
Total RNA was isolated using the TriZol reagent (Life Technologies; Gaithersburg, MD, USA) and the cDNA was obtained using M-MLV reverse transcriptase (Gibco-BRL; Gaithersburg, MD, USA). Blend Taq DNA polymerase (Toyobo, Osaka, Japan) and primers targeting Raptor and actin were used for PCR. The following primers were used to amplify the target genes: Raptor (forward) 5′-ATT CTC GCC GTG ATC GTC AA-3′ and (reverse) 5′-GGA GAA GGC AAG GCG TAG TT-3′ and actin (forward) 5′-GGC ATC GTC ACC AAC TGG GAC-3′ and (reverse) 5′-CGA TTT CCC GCT CGG CCG TGG-3′. To perform qPCR, SYBR Fast qPCR Mix (Takara Bio Inc., Shiga, Japan) was used, and reactions were performed on a Thermal Cycler Dice® Real Time System III (Takara Bio Inc). We calculated the threshold cycle number (Ct) of each gene using actin as the reference gene, and we reported the delta-delta Ct values of the genes. The following primers were used to amplify the target genes: Raptor (forward) 5′-ACT GAT GGA GTC CGA AAT GC-3′ and (reverse) 5′-TCA TCC ATC CTT CAT CCT C-3′, OTUB1 (forward) 5′-AGA GCG ACC ACA TCC ACA TC-3′ and (reverse) 5′- ATC GTA GTG TCC AGG CCG GT-3′, and actin (forward) 5′- CTA CAA TGA GCT GCG TGT G -3′ and (reverse) 5′- TGG GGT GTT GAA GGT CTC-3′.
Measurement of mitochondrial lengths
Caki/pDsRed2-Mito cells were transfected with plasmids (vector, OTUB1 wild type (WT), OTUB1 Y26A and Raptor). Fluorescence images of mitochondrial morphology was analyzed using a fluorescence microscope (Carl Zeiss, Jena, Germany). Mitochondrial lengths were measured using ZEN3.4. In three independent experiments, the average lengths of at least twenty mitochondria were analyzed from randomly selected five areas for each data.
Detection of mitochondrial damage
For assessing mitochondrial damage, Caki cells were stained with 1 μM MitoTracker Deep Red and 1 μM MitoTracker Green dye (Molecular Probes Inc., Eugene, OR, USA) for 15 min at 37 °C. MitoTracker Deep Red stains active mitochondria to show mitochondrial respiring, whereas MitoTracker Green dye stains all mitochondria to represent the mitochondrial mass [52]. The stained cells were trypsinized and resuspended in 300 µL PBS. Mitochondrial damage was assessed using the FACSCantoTM flow cytometer (BD Biosciences, San Jose, CA, USA).
Measurement of mitochondrial ROS
To assess mitochondrial ROS production, the cells were treated with the 2 μM MitoSOX Red mitochondrial superoxide indicator (Thermo Fisher scientific, Waltham, MA, USA). Before harvesting the lysate, the cells were stained with the 2 μM MitoSOX Red dye for 10 min, following which the cells were trypsinized and resuspended in PBS, and mitochondrial ROS production was measured on the basis of red fluorescence using the BD AccuriTM C6 cytometer (BD Biosciences, San Jose, CA, USA) and a fluorescence microscope (Carl Zeiss, Jena, Germany).
Generation of OTUB1 KO cells
Two CRISPR sgRNAs were designed using the CRISPR designing tool, their sequences being: oligomer, 5′- CAC CGG ACC TCT GTC GCC GAC CTG C-3′. The OTUB1 KO cell lines were established by transfecting these sgRNAs into Caki cells using the Lipofactor-pMAX reagent; cells were selected on 0.2 μg/ml puromycin, and OTUB1 KO efficiency was checked using western blot analysis.
Colony formation assay
Colony formation assay was performed according to methods described in our previous study [49]. Briefly, cells (0.5 × 105) were seeded in a 12-well culture plates, and then transduced with lentivirus containing either a non-target (NT) or Raptor shRNA sequence, or transiently co-transfected with Raptor and Cont siRNA, OTUB1 siRNA, Flag-OTUB1WT, or Flag-OTUB1 Y26A. After 5 days, the cells were fixed, stained with 0.5% crystal violet solution, and visualized by a digital camera.
Analysis of cell cycle and apoptosis using flow cytometry
The cancer and normal cell lines were fixed with 100% ethanol for 2 h and incubated in 1.12% sodium citrate buffer containing 50 µg/mL RNase for 30 min at 37 °C, followed by the addition of 50 µg/mL propidium iodide and measurement using the BD AccuriTM C6 cytometer (BD Biosciences, San Jose, CA, USA).
Patient specimens
In total, 40 renal cell carcinoma specimens and adjacent normal tissues were collected from the Keimyung University Dongsan Hospital Biobank (IRB-2019-11-040).
Survival rate of patients with kidney clear carcinoma
The overall survival according to Raptor expression was obtained from Oncolnc (http://www.oncolnc.org/) by analyzing the data of 208 patients from The Cancer Gene Atlas (TCGA) cohort with high versus low expression.
Statistical analysis
Experiments were repeated at least thrice, and all data are represented as means. Statistical analysis was performed using one-way analysis of variance (ANOVA) and post hoc comparisons (Student-Newman–Keuls) using the SPSS (Statistical Package for the Social Sciences, version 22.0) (SPSS Inc.; Chicago, IL). Sample size was decided on the basis of the minimum effects measured, and all of experiments are performed more than three times. P-values < 0.05 were considered significant.
Data availability
All data generated or analyzed during this study are included in this article and its supplementary data files and all original data are available from the corresponding authors upon request.
References
Kamba T, McDonald DM. Mechanisms of adverse effects of anti-VEGF therapy for cancer. Br J Cancer. 2007;96:1788–95.
Pantuck AJ, Seligson DB, Klatte T, Yu H, Leppert JT, Moore L, et al. Prognostic relevance of the mTOR pathway in renal cell carcinoma: implications for molecular patient selection for targeted therapy. Cancer. 2007;109:2257–67.
Robb VA, Karbowniczek M, Klein-Szanto AJ, Henske EP. Activation of the mTOR signaling pathway in renal clear cell carcinoma. J Urol. 2007;177:346–52.
Battelli C, Cho DC. mTOR inhibitors in renal cell carcinoma. Therapy. 2011;8:359–67.
Cho DC, Cohen MB, Panka DJ, Collins M, Ghebremichael M, Atkins MB, et al. The efficacy of the novel dual PI3-kinase/mTOR inhibitor NVP-BEZ235 compared with rapamycin in renal cell carcinoma. Clin Cancer Res. 2010;16:3628–38.
Pal SK, Quinn DI. Differentiating mTOR inhibitors in renal cell carcinoma. Cancer Treat Rev. 2013;39:709–19.
Kim LC, Cook RS, Chen J. mTORC1 and mTORC2 in cancer and the tumor microenvironment. Oncogene. 2017;36:2191–201.
Guertin DA, Stevens DM, Thoreen CC, Burds AA, Kalaany NY, Moffat J, et al. Ablation in mice of the mTORC components raptor, rictor, or mLST8 reveals that mTORC2 is required for signaling to Akt-FOXO and PKCalpha, but not S6K1. Dev Cell. 2006;11:859–71.
Xu J, Pham CG, Albanese SK, Dong Y, Oyama T, Lee CH, et al. Mechanistically distinct cancer-associated mTOR activation clusters predict sensitivity to rapamycin. J Clin Invest. 2016;126:3526–40.
Populo H, Lopes JM, Soares P. The mTOR signalling pathway in human cancer. Int J Mol Sci. 2012;13:1886–918.
Guertin DA, Sabatini DM. Defining the role of mTOR in cancer. Cancer Cell. 2007;12:9–22.
Earwaker P, Anderson C, Willenbrock F, Harris AL, Protheroe AS, Macaulay VM. RAPTOR up-regulation contributes to resistance of renal cancer cells to PI3K-mTOR inhibition. PLoS One. 2018;13:e0191890.
Shchegolev Y, Sorokin D, Scherbakov A, Shunaev A, Andreeva O, Mikhaevich E, et al. Upregulation of Akt/Raptor signaling is associated with rapamycin resistance of breast cancer cells. Chem Biol Interact. 2020;330:109243.
Seo SU, Woo SM, Kim MW, Lee HS, Kim SH, Kang SC, et al. Cathepsin K inhibition-induced mitochondrial ROS enhances sensitivity of cancer cells to anti-cancer drugs through USP27x-mediated Bim protein stabilization. Redox Biol. 2020;30:101422.
Yuan T, Yan F, Ying M, Cao J, He Q, Zhu H, et al. Inhibition of Ubiquitin-specific proteases as a novel anticancer therapeutic strategy. Front Pharm. 2018;9:1080.
Zhou Y, Wu J, Fu X, Du W, Zhou L, Meng X, et al. OTUB1 promotes metastasis and serves as a marker of poor prognosis in colorectal cancer. Mol Cancer. 2014;13:258.
Iglesias-Gato D, Chuan YC, Jiang N, Svensson C, Bao J, Paul I, et al. OTUB1 de-ubiquitinating enzyme promotes prostate cancer cell invasion in vitro and tumorigenesis in vivo. Mol Cancer. 2015;14:8.
Goncharov T, Niessen K, de Almagro MC, Izrael-Tomasevic A, Fedorova AV, Varfolomeev E, et al. OTUB1 modulates c-IAP1 stability to regulate signalling pathways. EMBO J. 2013;32:1103–14.
Sun XX, Challagundla KB, Dai MS. Positive regulation of p53 stability and activity by the deubiquitinating enzyme Otubain 1. EMBO J. 2012;31:576–92.
Zhou H, Liu Y, Zhu R, Ding F, Cao X, Lin D, et al. OTUB1 promotes esophageal squamous cell carcinoma metastasis through modulating Snail stability. Oncogene. 2018;37:3356–68.
Karunarathna U, Kongsema M, Zona S, Gong C, Cabrera E, Gomes AR, et al. OTUB1 inhibits the ubiquitination and degradation of FOXM1 in breast cancer and epirubicin resistance. Oncogene. 2016;35:1433–44.
Liu T, Jiang L, Tavana O, Gu W. The Deubiquitylase OTUB1 mediates Ferroptosis via stabilization of SLC7A11. Cancer Res. 2019;79:1913–24.
Wu Q, Huang Y, Gu L, Chang Z, Li GM. OTUB1 stabilizes mismatch repair protein MSH2 by blocking ubiquitination. J Biol Chem. 2021;296:100466.
Liao Y, Wu N, Wang K, Wang M, Wang Y, Gao J, et al. OTUB1 promotes progression and proliferation of prostate cancer via Deubiquitinating and Stabling Cyclin E1. Front Cell Dev Biol. 2020;8:617758.
Li Y, Yang JY, Xie X, Jie Z, Zhang L, Shi J, et al. Preventing abnormal NF-kappaB activation and autoimmunity by Otub1-mediated p100 stabilization. Cell Res. 2019;29:474–85.
Zhao L, Wang X, Yu Y, Deng L, Chen L, Peng X, et al. OTUB1 protein suppresses mTOR complex 1 (mTORC1) activity by deubiquitinating the mTORC1 inhibitor DEPTOR. J Biol Chem. 2018;293:4883–92.
Wang T, Yin L, Cooper EM, Lai MY, Dickey S, Pickart CM, et al. Evidence for bidentate substrate binding as the basis for the K48 linkage specificity of otubain 1. J Mol Biol. 2009;386:1011–23.
Nakada S, Tai I, Panier S, Al-Hakim A, Iemura S, Juang YC, et al. Non-canonical inhibition of DNA damage-dependent ubiquitination by OTUB1. Nature. 2010;466:941–6.
Pasupala N, Morrow ME, Que LT, Malynn BA, Ma A, Wolberger C. OTUB1 non-catalytically stabilizes the E2 ubiquitin-conjugating enzyme UBE2E1 by preventing its autoubiquitination. J Biol Chem. 2018;293:18285–95.
Herhaus L, Al-Salihi M, Macartney T, Weidlich S, Sapkota GP. OTUB1 enhances TGFbeta signalling by inhibiting the ubiquitylation and degradation of active SMAD2/3. Nat Commun. 2013;4:2519.
Saldana M, VanderVorst K, Berg AL, Lee H, Carraway KL. Otubain 1: a non-canonical deubiquitinase with an emerging role in cancer. Endocr Relat Cancer. 2019;26:R1–14.
Wang T, Zhang WS, Wang ZX, Wu ZW, Du BB, Li LY, et al. RAPTOR promotes colorectal cancer proliferation by inducing mTORC1 and upregulating ribosome assembly factor URB1. Cancer Med. 2020;9:1529–43.
Yusenko MV, Kuiper RP, Boethe T, Ljungberg B, van Kessel AG, Kovacs G. High-resolution DNA copy number and gene expression analyses distinguish chromophobe renal cell carcinomas and renal oncocytomas. BMC Cancer. 2009;9:152.
Wiener R, Zhang X, Wang T, Wolberger C. The mechanism of OTUB1-mediated inhibition of ubiquitination. Nature. 2012;483:618–22.
Herhaus L, Perez-Oliva AB, Cozza G, Gourlay R, Weidlich S, Campbell DG, et al. Casein kinase 2 (CK2) phosphorylates the deubiquitylase OTUB1 at Ser16 to trigger its nuclear localization. Sci Signal. 2015;8:ra35.
Edelmann MJ, Kramer HB, Altun M, Kessler BM. Post-translational modification of the deubiquitinating enzyme otubain 1 modulates active RhoA levels and susceptibility to Yersinia invasion. FEBS J. 2010;277:2515–30.
Qayyum T, McArdle PA, Lamb GW, Jordan F, Orange C, Seywright M, et al. Expression and prognostic significance of Src family members in renal clear cell carcinoma. Br J Cancer. 2012;107:856–63.
Pal R, Palmieri M, Chaudhury A, Klisch TJ, di Ronza A, Neilson JR, et al. Src regulates amino acid-mediated mTORC1 activation by disrupting GATOR1-Rag GTPase interaction. Nat Commun. 2018;9:4351.
Ondrusova L, Reda J, Zakova P, Tuhackova Z. Inhibition of mTORC1 by SU6656, the selective Src kinase inhibitor, is not accompanied by activation of Akt/PKB signalling in melanoma cells. Folia Biol (Praha). 2013;59:162–7.
Vojtechova M, Tureckova J, Kucerova D, Sloncova E, Vachtenheim J, Tuhackova Z. Regulation of mTORC1 signaling by Src kinase activity is Akt1-independent in RSV-transformed cells. Neoplasia. 2008;10:99–107.
McClendon CJ, Miller WT. Structure, function, and regulation of the SRMS Tyrosine Kinase. Int J Mol Sci. 2020;21:4233–47.
Kohmura N, Yagi T, Tomooka Y, Oyanagi M, Kominami R, Takeda N, et al. A novel nonreceptor tyrosine kinase, Srm: cloning and targeted disruption. Mol Cell Biol. 1994;14:6915–25.
Park JM, Yang SW, Zhuang W, Bera AK, Liu Y, Gurbani D, et al. The nonreceptor tyrosine kinase SRMS inhibits autophagy and promotes tumor growth by phosphorylating the scaffolding protein FKBP51. PLoS Biol. 2021;19:e3001281.
Potts MB, Kim HS, Fisher KW, Hu Y, Carrasco YP, Bulut GB, et al. Using functional signature ontology (FUSION) to identify mechanisms of action for natural products. Sci Signal. 2013;6:ra90.
Goel RK, Miah S, Black K, Kalra N, Dai C, Lukong KE. The unique N-terminal region of SRMS regulates enzymatic activity and phosphorylation of its novel substrate docking protein 1. FEBS J. 2013;280:4539–59.
Goel RK, Paczkowska M, Reimand J, Napper S, Lukong KE. Phosphoproteomics analysis identifies novel candidate substrates of the nonreceptor Tyrosine Kinase, Src-related Kinase Lacking C-terminal regulatory Tyrosine and N-terminal Myristoylation Sites (SRMS). Mol Cell Proteom: MCP. 2018;17:925–47.
Bridges CR, Tan M-C, Premarathne S, Nanayakkara D, Bellette B, Zencak D, et al. USP9X deubiquitylating enzyme maintains RAPTOR protein levels, mTORC1 signalling and proliferation in neural progenitors. Sci Rep. 2017;7:391.
Hussain S, Feldman AL, Das C, Ziesmer SC, Ansell SM, Galardy PJ. Ubiquitin hydrolase UCH-L1 destabilizes mTOR complex 1 by antagonizing DDB1-CUL4-mediated ubiquitination of raptor. Mol Cell Biol. 2013;33:1188–97.
Woo SM, Min KJ, Seo BR, Kwon TK. YM155 sensitizes TRAIL-induced apoptosis through cathepsin S-dependent down-regulation of Mcl-1 and NF-kappaB-mediated down-regulation of c-FLIP expression in human renal carcinoma Caki cells. Oncotarget. 2016;7:61520–32.
Woo SM, Min KJ, Seo BR, Seo YH, Jeong YJ, Kwon TK. YM155 enhances ABT-737-mediated apoptosis through Mcl-1 downregulation in Mcl-1-overexpressed cancer cells. Mol Cell Biochem. 2017;429:91–102.
Seo J, Lee EW, Shin J, Seong D, Nam YW, Jeong M, et al. K6 linked polyubiquitylation of FADD by CHIP prevents death inducing signaling complex formation suppressing cell death. Oncogene. 2018;37:4994–5006.
Zhou R, Yazdi AS, Menu P Tschopp J. A role for mitochondria in NLRP3 inflammasome activation. Nature. 2007;469:221v5.
Acknowledgements
The biospecimens and data used for the present study were provided by the Biobank of Keimyung University Dongsan Hospital Biobank, a member of the Korea Biobank Network.
Funding
This work was supported by an NRF grant funded by the Korea Government (MSIP) [NRF-2021R1A4A1029238, NRF-2019R1A2C2005921 and NRF-2020R1C1C1009889]. This work was supported by a grant from the KRIBB Research Initiative Program.
Author information
Authors and Affiliations
Contributions
KM, EL and TKK conceived and designed the project; SUS, SMW, and MWK performed experiments and analyses, and acquired data; EL and TKK contributed technical/reagents materials, analytical tools, and/or grant support; KM, and TKK prepared, wrote the manuscript; SMW, KM, EL and TKK reviewed, and/or revised the manuscript. All authors discussed the results and commented on the manuscript. The author(s) read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The present study was approved by the Ethics Committee of Keimyung Medical University.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Edited by L. Scorrano
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Seo, S.U., Woo, S.M., Kim, M.W. et al. Phosphorylation of OTUB1 at Tyr 26 stabilizes the mTORC1 component, Raptor. Cell Death Differ 30, 82–93 (2023). https://doi.org/10.1038/s41418-022-01047-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41418-022-01047-3
This article is cited by
-
OTUB1 accelerates hepatocellular carcinoma by stabilizing RACK1 via its non-canonical ubiquitination
Cellular Oncology (2024)
-
Cathepsin K inhibition induces Raptor destabilization and mitochondrial dysfunction via Syk/SHP2/Src/OTUB1 axis-mediated signaling
Cell Death & Disease (2023)
-
Phosphorylation of USP27X by GSK3β maintains the stability and oncogenic functions of CBX2
Cell Death & Disease (2023)