Abstract
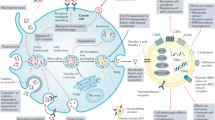
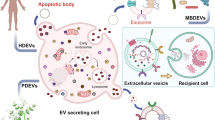
Extracellular vesicles (EVs) are released by all cells and produced at particularly high levels by many cancer cells, often inducing pro-tumorigenic effects. Since these cancer EVs carry tumour proteins and RNAs, they can potentially be used at biomarkers. The heterogeneity of surface markers and cargos carried by EVs, however, presents some challenges to developing such approaches. Nanou et al. [1] found that automated counting of large tumour-derived EVs (tdEVs) performed at least as effectively as counting circulating tumour-derived cells (CTCs) and with higher sensitivity, in distinguishing the survival of patients with castration-resistant prostate cancer (CRPC), metastatic colorectal cancer (mCRC) and metastatic breast cancer (MBC), but not for non-small cell lung cancer (NSCLC). Subsequent work has suggested that these tdEVs may also be used to assess tumour subtype and that the number of large EVs produced by endothelial cells can also be increased in cancer patients. While by itself, the tdEV imaging approach used by Nanou et al. [1] is not specific enough to predict the survival of individual patients, in combination with other EV-associated assays, this test, perhaps enhanced through the inclusion of other tumour antigens, could prove invaluable in predicting cancer survival and other outcomes in the clinic.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Nanou A, Miller MC, Zeune LL, de Wit S, Punt CJA, Groen HJM, et al. Tumour-derived extracellular vesicles in blood of metastatic cancer patients associate with overall survival. Br J Cancer. 2020;122:801–11.
van Niel G, Carter DRF, Clayton A, Lambert DW, Raposo G, Vader P. Challenges and directions in studying cell-cell communication by extracellular vesicles. Nat Rev Mol Cell Biol. 2022;23:369–82.
Meehan B, Rak J, Di Vizio D. Oncosomes—large and small: what are they, where they came from? J Extracell Vesicles. 2016;5:33109.
Cheng L, Hill AF. Therapeutically harnessing extracellular vesicles. Nat Rev Drug Discov. 2022;21:379–99.
Chen G, Huang AC, Zhang W, Zhang G, Wu M, Xu W, et al. Exosomal PD-L1 contributes to immunosuppression and is associated with anti-PD-1 response. Nature. 2018;560:382–6.
Poggio M, Hu T, Pai CC, Chu B, Belair CD, Chang A, et al. Suppression of exosomal PD-L1 induces systemic anti-tumor immunity and memory. Cell. 2019;177:414–27.
Wortzel I, Dror S, Kenific CM, Lyden D. Exosome-mediated metastasis: communication from a distance. Dev Cell. 2019;49:347–60.
Al-Nedawi K, Meehan B, Micallef J, Lhotak V, May L, Guha A, et al. Intercellular transfer of the oncogenic receptor EGFRvIII by microvesicles derived from tumour cells. Nat Cell Biol. 2008;10:619–24.
Ciardiello C, Leone A, Lanuti P, Roca MS, Moccia T, Minciacchi VR, et al. Large oncosomes overexpressing integrin alpha-V promote prostate cancer adhesion and invasion via AKT activation. J Exp Clin Cancer Res. 2019;38:317.
Weng J, Xiang X, Ding L, Wong AL, Zeng Q, Sethi G, et al. Extracellular vesicles, the cornerstone of next-generation cancer diagnosis? Semin Cancer Biol. 2021;74:105–120.
Jiang C, Fu Y, Liu G, Shu B, Davis J, Tofaris GK. Multiplexed profiling of extracellular vesicles for biomarker development. Nanomicro Lett 2021;14:3.
Hoshino A, Kim HS, Bojmar L, Gyan KE, Cioffi M, Hernandez J, et al. Extracellular vesicle and particle biomarkers define multiple human cancers. Cell. 2020;182:1044–1061.e18.
Tian Y, Gong M, Hu Y, Liu H, Zhang W, Zhang M, et al. Quality and efficiency assessment of six extracellular vesicle isolation methods by nano-flow cytometry. J Extracell Vesicles. 2020;9:1697028.
Crescitelli R, Lässer C, Lötvall J. Isolation and characterization of extracellular vesicle subpopulations from tissues. Nat Protoc 2021;16:1548–80.
Hilton SH, White IM. Advances in the analysis of single extracellular vesicles: A critical review. Sens Actuators Rep. 2021;3:100052.
Larson CJ, Moreno JG, Pienta KJ, Gross S, Repollet M, O’hara SM, et al. Apoptosis of circulating tumor cells in prostate cancer patients. Cytom A. 2004;62:46–53.
Coumans FAW, Doggen CJM, Attard G, de Bono JS, Terstappen LWMM. All circulating EpCAM+CK+CD45- objects predict overall survival in castration-resistant prostate cancer. Ann Oncol. 2010;21:1851–7.
Nanou A, Coumans FAW, van Dalum G, Zeune LL, Dolling D, Onstenk W, et al. Circulating tumor cells, tumor-derived extracellular vesicles and plasma cytokeratins in castration-resistant prostate cancer patients. Oncotarget. 2018;9:19283–93.
Dathathri E, Isebia KT, Abali F, Lolkema MP, Martens JWM, Terstappen LWMM, et al. Liquid biopsy based circulating biomarkers in metastatic prostate cancer. Front Oncol. 2022;12:863472.
Nanou A, Zeune LL, Bidard FC, Pierga JY, Terstappen LWMM. HER2 expression on tumor-derived extracellular vesicles and circulating tumor cells in metastatic breast cancer. Breast Cancer Res. 2020b;22:86.
Nanou A, Mol L, Coumans FAW, Koopman M, Punt CJA, Terstappen LWMM. Endothelium-derived extracellular vesicles associate with poor prognosis in metastatic colorectal cancer. Cells. 2020c;9:2688.
Yoh KE, Lowe CJ, Mahajan S, Suttmann R, Nguy T, Reichelt M, et al. Enrichment of circulating tumor-derived extracellular vesicles from human plasma. J Immunol Methods. 2021;490:112936.
Shiromizu T, Kume H, Ishida M, Adachi J, Kano M, Matsubara H, et al. Quantitation of putative colorectal cancer biomarker candidates in serum extracellular vesicles by targeted proteomics. Sci Rep. 2017;7:12782.
Lin AA, Nimgaonkar V, Issadore D, Carpenter EL. Extracellular vesicle-based multianalyte liquid biopsy as a diagnostic for cancer. Annu Rev Biomed Data Sci. 2022;5:269–92.
Théry C, Witwer KW, Aikawa E, Alcaraz MJ, Anderson JD, Andriantsitohaina R, et al. Minimal information for studies of extracellular vesicles 2018 (MISEV2018): a position statement of the International Society for Extracellular Vesicles and update of the MISEV2014 guidelines. J Extracell Vesicles. 2018;7:1535750.
Witwer KW, Goberdhan DC, O’Driscoll L, Théry C, Welsh JA, Blenkiron C, et al. Updating MISEV: Evolving the minimal requirements for studies of extracellular vesicles. J Extracell Vesicles. 2021;10:e12182.
Kowal J, Arras G, Colombo M, Jouve M, Morath JP, Primdal-Bengtson B, et al. Proteomic comparison defines novel markers to characterize heterogeneous populations of extracellular vesicle subtypes. Proc Natl Acad Sci. 2016;113:E968–77.
Fan SJ, Kroeger B, Marie PP, Bridges EM, Mason JD, McCormick K, et al. Glutamine deprivation alters the origin and function of cancer cell exosomes. EMBO J. 2020;39:e103009.
Acknowledgements
DCIG acknowledges Prof. Clive Wilson for helpful discussions. This work was supported by a Cancer Research UK Programme Award (C19591/A19076), Cancer Research UK Primer Award (C19591/A28123) and a BBSRC Project Award (BB/R004862/1).
Author information
Authors and Affiliations
Contributions
DCIG designed the work leading to the submission, drafted and revised the manuscript, approved the final version and agrees to be accountable for all aspects of this work.
Corresponding author
Ethics declarations
Conflict of interest
The author declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Goberdhan, D.C.I. Large tumour-derived extracellular vesicles as prognostic indicators of metastatic cancer patient survival. Br J Cancer 128, 471–473 (2023). https://doi.org/10.1038/s41416-022-02055-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-022-02055-3