Abstract
Background
Peptide-vaccination therapy targeting tumour-associated antigens can elicit immune responses, but cannot be used to eliminate large tumour burden. In this study, we developed a therapeutic single-chain variable-fragment (scFv) antibody that recognises the cancer stem-like cell/cancer-initiating cell (CSC/CIC) antigen, DNAJB8.
Methods
We screened scFv clones reacting with HLA-A24:20/DNAJB8-derived peptide (DNAJB8_143) complex using naive scFv phage-display libraries. Reactivity and affinity of scFv clones against the cognate antigen were quantified using FACS and surface plasmon resonance. Candidate scFv clones were engineered to human IgG1 (hIgG1) and T-cell-engaging bispecific antibody (CD3xJB8). Complement-dependent cytotoxicity (CDC) and bispecific antibody-dependent cellular cytotoxicity (BADCC) were assessed.
Results
scFv clones A10 and B10 were isolated after bio-panning. Both A10-hIgG1 and B10-hIgG1 reacted with DNAJB8-143 peptide-pulsed antigen-presenting cells and HLA-A24(+)/DNAJB8(+) renal cell carcinoma and osteosarcoma cell lines. A10-hIgG1 and B10-hIgG1 showed strong affinity with the cognate HLA/peptide complex (KD = 2.96 × 10−9 M and 5.04 × 10−9 M, respectively). A10-hIgG1 and B10-hIgG1 showed CDC against HLA-A24(+)/DNAJB8(+) cell lines. B10-(CD3xJB8) showed superior BADCC to A10-(CD3xJB8).
Conclusion
We isolated artificial scFv antibodies reactive to CSC/CIC antigen DNAJB8-derived peptide naturally present on renal cell carcinoma and sarcoma. Immunotherapy using these engineered antibodies could be promising.
Similar content being viewed by others
Background
The first immunotherapy against cancer was performed using Coley’s Toxins developed by William B. Coley in the nineteenth century.1 He vaccinated sarcoma patients with live or inactivated bacteria. Various vaccination therapies using tumour-associated antigen (TAA)-derived peptides, autologous tumour lysates and tumour lysate-loaded dendritic cells have been developed to date.2 We conducted peptide-vaccination trials using TAA-derived peptides of SYT–SSX junctional peptides derived from specific chromosomal translocation for synovial sarcoma, papillomavirus-binding factor (PBF) for osteosarcoma and survivin for various carcinomas.3,4 Although immune responses against the vaccinated peptides were frequently observed, the objective clinical response rates were low.
In contrast, cell-based immunotherapy using T cells exogenously expressing T-cell receptor (TCR) directed to TAA (TCR-T), especially for NY-ESO-I, showed clinical responses against melanoma and synovial sarcoma.5 Anti-CD19 chimeric antigen receptor-expressing T cells (CAR-T) also showed dramatic responses in B-cell haematological malignancies.6 However, CD19 CAR-T cells can destroy not only neoplastic B cells but also normal B cells. Target antigens are still restricted, and new antigens might be required for the development of immunotherapy for various cancers.
Considering the current status, we focused on (i) the identification of new TAAs that were expressed in cancer stem-like cells/cancer-initiating cells (CSCs/CICs) but not in normal organs that also regulate tumour-initiating ability, and (ii) the development of antibodies directed to CSC/CIC antigen using antibody engineering.3,7 Recently, various therapeutic antibodies targeting tumour antigens expressed on tumour cell surfaces have been developed. In particular, anti-CD20 monoclonal antibody rituximab and anti-CD19 T-cell-engaging bispecific antibody blinatumomab showed objective responses in B-cell haematological neoplasia.8,9
In this study, we developed a therapeutic single-chain variable-fragment (scFv) antibody recognising the HLA-A24/peptide derived from DNAJB8 complex as a prototype of CSC/CIC antigen.10,11 Then, we engineered the scFv to bivalent and bispecific formats to assess its in vitro cytotoxic capacity in renal cell carcinoma and sarcoma.
Methods
This study was performed in accordance with the guidelines established by the Declaration of Helsinki, and was approved by the Ethics Committee of Sapporo Medical University. The healthy donors provided informed consent for the use of blood samples in our research.
Cell lines and culture
Human renal cell carcinoma cell lines (CAKI-1 and ACHN), 1 human colorectal adenocarcinoma cell line (HT29), human osteosarcoma cell lines (OS2000, KIKU, OS13, HOS, U2OS and HuO9) and 1 human bone malignant fibrous histiocytoma cell line (MFH03) were used. OS2000, KIKU, OS13 and MFH03 were established in our laboratory.12,13,14,15 The other cell lines were purchased from the Japanese Collection of Research Bioresources Cell Bank (Tokyo, Japan) and from the American Type Culture Collection (Manassas, VA). OS2000, OS13 and MFH03 cells were cultured in Iscove modified Dulbecco’s medium containing 10% FBS, and the others were cultured in Dulbecco’s modified Eagle medium (DMEM) (Sigma-Aldrich, St Louis, MO) containing 10% FBS in a 5% CO2 incubator. HT29 transfected with DNAJB8 (HT29-DNAJB8) and HOS transfected with HLA-A*2402 (HOS-A24) were also used.10,16 T2-A24 cells lacked the peptide transporter and exogenously expressed HLA-A*24:02.17 T2-A24 cells were cultured in RPMI1640 supplemented with G418 used as antigen-presenting cells for exogenously pulsed peptides.
Biotinylated antigens and peptides
Biotinylated HLA-A*24:02/peptide complex monomers were constructed by Medical & Biological Laboratories, Co., Ltd. (Nagoya, Japan). HLA-A24-restricted peptides DANJB8_143 (AFMEAFSSF), HIV (RYLRDQQLLGI), CMV (QYDPVAALF) and EBV LMP2 (TYGPVFMSL) were used in this study.
Bio-panning with biotinylated antigen
Bio-panning was performed according to our previous report with some modifications.18 Biotinylated HLA–-A24:02/DNAJB8_143 peptide and HLA-A24:02/HIV peptide complexes were used as antigens. The scFv phage-display libraries constructed by our laboratory (Library #1) and provided by Daiichi-Sankyo Co., Ltd. (Library #2) were used for Experiment #1 and Experiment #2, respectively. The phage library (0.25 mL) was mixed with PBS (0.25 mL) containing 4% (w/v) milk in a 1.5-mL tube and incubated with 100 μL of magnetic beads (Dynabeads M-280 Streptavidin, Life Technologies, Carlsbad, CA), which were prewashed with PBS with 0.1% Tween 20 (PBST). The magnetic beads (100 μL) were prewashed and blocked with 2% PBS-M for 1–2 h at room temperature. The phage supernatant was mixed with 0.5 mL of biotinylated HLA-A24:02/HIV peptide complex (1000 nM) and incubated for 60 min (negative panning). After incubation, the phage–antigen mixture was mixed with the magnetic beads for 15 min. The resultant phage supernatant (500 μL) was mixed with 0.5 mL of biotinylated HLA-A24:02/DNAJB8_143 peptide complex (500 nM in the first round and 100 nM in the second and subsequent rounds) and mixed for 60 min (positive panning). After incubation, the phage–antigen mixture was mixed with the magnetic beads, followed by additional incubation for 15 min. Specific phage binders were eluted from the magnetic beads by incubation with 1 mL of 100 mM triethylamine for 7 min. The eluted phage aliquot was immediately neutralised with 100 μL of 1 M Tris-HCl, pH 7.4. The resultant phage aliquot was used for phage rescue.
Phage rescue was performed as follows. Half of the phage aliquot after bio-panning was added to 10 mL of log-phage TG1 or XL1 blue and incubated at 37 °C for 1 h with slow shaking. After incubation, ampicillin (final concentration 100 µg/mL), glucose and helper phage (M13K07 or VCM13) were added and incubated for 60 min. Then, 15 mL of fresh 2xYT containing ampicillin (100 μg/mL) and kanamycin (25 μg/mL) and 1% glucose was added to cultured E. coli infected with the phage and helper phage, followed by incubation at 26 °C overnight. Overnight culture of bacteria, including the proliferated phage, was isolated using polyethylene glycol precipitation and used for the next round of bio-panning.
After bio-panning, soluble scFv expression of E. coli infected with the phage was induced in a microplate. The phage aliquot after bio-panning (400 μL) was added to 10 mL of log-phage E. coli and incubated at 37 °C for 1 h with slow shaking. Following incubation, the E. coli aliquot was seeded on a 2xYTAG agar plate and incubated at 37 °C overnight. The next day, 94 clones were picked up and inoculated independently into wells containing 100 μL of 2xYTAG in a 96-well microculture plate. The plate was incubated at 37 °C with shaking for 5 h. After incubation, 20 μL of 2xYTAG with 3 mM isopropyl-β-d(−)-thiogalactopyranoside (IPTG) was added and incubated at 28 °C overnight. Then, 50 μL of the supernatant was harvested and immediately used for ELISA screening according to the previous report.18
Generation of scFv–hIgG and bispecific antibody
scFv cDNA in phagemid vector was subcloned into pFX-hIgG1 for scFv-hIgG1 expression previously constructed by our laboratory.18 For soluble expression of scFv-hIgG1, 4 μg of the plasmid was transfected using Lipofectamine 2000 (Life Technologies) into 293 T cells precultured on a 10-cm culture dish in DMEM supplemented with 10% FBS. After 4–5 h, the culture medium was replaced with fresh AIM-V (Life Technologies) without serum. The supernatant was harvested and replaced with fresh AIM-V at 24, 48 and 72 h after transfection. The collected supernatant was passed through a chromatography column with Protein G. The column was washed with 20 mM sodium phosphate (pH 7.0) and eluted by fraction (1 mL per fraction) with a total of 5 mL of 0.1 M glycine (pH 2.7), followed by immediate neutralisation with 1/10 volume of Tris-HCl (pH 9.0). Fractions containing antibodies were assessed by SDS-PAGE with or without DDT to confirm that oxidised scFv–hIgG formed a dimer protein.
The bispecific antibody was constructed as follows: CD3 scFv19 linked with a short peptide linker (SGGGGS) and multicloning site (5′-AGTGGCGGCGGAGGATCCAAGAATTCCGCCATGGCAGGTGGCGCGCCAGCGGCCGC-3′) was created by gene synthesis (Integrated DNA Technologies, KK, Tokyo, Japan) and subcloned into pFX-His (CD3-pFX-His). pFx-His was a derivative of pFX-hIgG1 where the hIgG1 constant region was replaced with His tag by our laboratory. scFv cDNA of A10 and B10 was subcloned into CD3 scFv-pFX-His [A10-(CD3×JB8) and B10-(CD3×JB8)]. Soluble expression was performed similar to scFv-hIgG1, followed by Ni-NTA purification using Ni Sepharose 6 Fast Flow (GE Healthcare Japan, Tokyo, Japan).
Surface plasmon resonance analysis
Surface plasmon resonance analysis was performed using a ProteOn XPR36 (Bio-Rad Laboratories, Inc., Tokyo, Japan) according to the protocol described by Nahshol et al.20 Briefly, 1 μg/mL biotinylated monomer (HLA-A*24:02/DNAJB8_143 peptide) in PBS supplemented with 0.005% Tween 20 (PBST) was injected at 30 μL/min at 25 °C and captured on a neutravidin-immobilised NLC sensor tip. Subsequently, serially diluted A10 scFv-hIgG1 and B10 scFv-hIgG1 in PBST was injected at 50 μL/min at 25 °C. All binding sensorgrams were collected and analysed using ProteOn Manager software (Bio-Rad Laboratories, Inc.).
Immunostaining, flow cytometry and fluorescence microscopy
Before immunostaining, T2-A24 cells (5–10 × 105) were incubated in 200 μL of AIM-V with each peptide at 50 μg/mL (DNAJB8_143, HIV, EBV LMP2 and CMV) on a 96-well round-bottom microculture plate at 26 °C overnight, followed by 2-h incubation at 37 °C. For immunostaining, 5–10 × 106 target cells were seeded in a 96-well microculture plate and incubated with 50–100 μL of 10 μg/mL scFv–hIgG or the supernatant of a hybridoma (C7709A2.6, anti-HLA-A24 mAb)21 on ice for 60 min. After two washes, the cells were incubated with 100 μL of anti-human IgG conjugated with PE (1:60 dilution, BioLegend, San Diego, CA) or FITC-conjugated rat anti-mouse IgG antibody (1:200 dilution, KPL, Gaithersburg, MD) for 40 min. The cells were also stained with 50 μL of the bispecific antibody (10 μg/mL) on ice for 60 min followed by anti-His-tag PE (clone AD1.1.10, Abcam). After immunostaining, cells were washed and then fixed with 200 μL of PBS with 0.5% formaldehyde and analysed using FACS Caliber and FACS AriaII (BD Bioscience, San Diego, CA). Fluorescence microscopy assay was performed using BZ-X700 (Keyence Corporation, Osaka, Japan) and Axio Observer.Z1 (Carl-Zeiss, Oberkochen, Germany). T cells and NK cells isolated from PBMC using Pan T Cell Isolation Kit and NK Cell Isolation Kit (Miltenyi Biotec, Gladbach, Germany) were also used.
Complement-dependent cytotoxicity
Target cells were seeded at 2 × 106 per 100 μL in a 96-well V-bottom plate. Aliquots of 50 μL of antibody (10 μg/mL) were added and incubated for 1 h on ice. After three washes with 0.5% BSA–PBS, cells were incubated with anti-C3b-PE (Clone 3E7/C3b, BioLegend, premixed with human serum) and DAPI (Vector Laboratories Inc., Burlingame, CA), immediately followed by fluorescence microscopy analysis.
Antibody-dependent cellular cytotoxicity
Target cells were seeded at 1 × 105 per 100 μL in a 96-well V-bottom plate. Aliquots of 50 μL of antibody (10 μg/mL) were added and incubated for 1 h on ice. Isolated T cells were then added (effector:target ratio of 3:1) and co-cultured for 6 h. The frequency of apoptosis of the target cells was assessed by MEBCYTO Apoptosis Kit (Annexin-V-FITC and propidium iodide, MBL International, Woburn, MA) and flow cytometry. In addition, cytotoxicity was assessed using the IMMUNOCYTO Cytotoxicity Detection Kit (MBL International) with carboxyfluorescein succinimidyl ester according to the manufacturer’s protocol.
Intracellular cytokine staining
Intracellular cytokine staining was performed according to the manufacturer’s protocol. Briefly, T cells were co-cultured with target cells at an effector:target ratio of 3:1. Brefeldin A (BioLegend) was added to the culture after 2 h, followed by further culture for 4 h. Cells were stained with anti-CD45-APC (BioLegend), fixed, permeabilised using the Cytofix/Cytoperm Kit (BD Biosciences) and then stained with anti-IL-2-FITC (clone 5344.111, BD Biosciences), anti-TNFα-PE (clone MAb11, BioLegend) and anti-IFNg-PE-Cy7 (clone 4S.B3, BioLegend). The frequency of cytokine-producing T cells was assessed using flow cytometry.
Statistical analysis
For comparisons, we used the unpaired t test in JMP software (SAS Institute Inc., Tokyo, Japan). Where relevant, figures indicate statistical parameters, including the value of n, means ± SD and statistical significance.
Results
Isolation of scFv specifically recognising HLA-A24/DNAJB8-derived peptide complex
First, we isolated specific scFv clones that recognise the HLA-A24:02/DNAJB8-derived peptide (DNAJB8_143) using naive scFv phage-display libraries. After two independent experiments of three-round bio-panning with biotinylated HLA-A24:02/DNAJB8_143 peptide complex, we isolated several scFv clones that strongly and specifically reacted with the complex (Fig. 1). For further characterisation, we selected A10 scFv and B10 scFv clones, which showed high reactivity with HLA-A24:02/DNAJB8-143 peptide and minimal reactivity with HLA-A24:02/HIV peptide from Experiment #1 and Experiment #2, respectively.
ELISA screening of the specific binders of 94 scFv clones reacting with biotinylated HLA-A*24:02/DNAJB8_143 peptide complex. Experiment #1 and Experiment #2 were performed using Library #1 and Library #2, respectively. The colours indicate highly reactive clones (optical density [A450(DNAJB8_143)-A450(HIV)] > 1.0 and A450(HIV) < 0.1). Colours represent identical CDR3 sequences.
A10 scFv-hIgG1 and B10 scFv-hIgG1 showed high affinity against the cognate antigen
We constructed A10 and B10 scFv-hIgG1 clones consisting of bivalent scFv and human IgG1 constant region. A10 and B10 scFv-hIgG1 recognised T2-A24 cells pulsed with DNAJB8_143 peptide but not with viral peptides (Figs. 2a, S1). A peptide titration assay using serial dilution of peptides showed that A10-scFv-hIgG1 and B10 scFv-hIgG1 reacted to T2-A24 cells pulsed with the peptide at minimal concentrations of 50 ng/mL and 5 ng/mL, respectively (Fig. 2b). The binding capacity of scFv-hIgG1 clones to DNAJB8_143 peptide presented by HLA-A24 on peptide-pulsed T2-A24 and HLA-A24(+) colorectal carcinoma cell line HT29-DNAJB8 on cell surfaces was also confirmed using fluorescence microscopy (Fig. 2c, d).
a Reactivity of scFv-hIgG1 to DNAJB8_143 and viral peptides. Each peptide was pulsed at 50 µg/mL. A10-hIgG1 and B10-hIgG1 were used at concentrations of 10 µg/mL. Mean fluorescence intensity (MFI) is indicated. b FACS analysis of scFv-hIgG1. T2-A24 cells were pulsed with the indicated peptides and stained with each scFv-hIgG1 at a concentration of 10 µg/mL. Anti-HLA-A24 mAb was used to detect the expression of HLA-A24 molecules. c, d Fluorescence microscopy of scFv-hIgG1. T2-A24 cells pulsed with the indicated peptides (c) and renal cancer cell lines (d) were used as targets. Anti-human IgG-PE was used as the second antibody for visualisation. HT29; HLA-A24(+)/DNAJB8(+), HT29/DNAJB8; HLA-A24(+)/DNAJB8(++), ACHN; HLA-A24(−)/DNAJB8(+). Each peptide was pulsed at 50 µg/mL. A10-hIgG1 and B10-hIgG1 were used at concentrations of 10 µg/mL. All experiments were repeated three times.
Next, the specificity of A10 scFv-hIgG1 and B10 scFv-hIgG1 was assessed using amino acid substitution peptides. The reactivities of the antibodies to amino acid substitution peptide-pulsed T2-A24 cells were determined using flow cytometry. The results showed that position 3 (P3) amino acid, P6 and P7 were critical for recognition (Fig. S2). P2 and P9 might be critical for binding HLA-A24 molecules as anchor amino acids. Considering the importance of the middle part of DNAJB8_143 peptide for specific recognition, A10 scFv and B10 scFv might react specifically with the cognate HLA/peptide complex similar to TCR.
Kinetics analysis of protein interactions between the antibodies and HLA-A24:02/DNAJB8_143 peptide complex was determined by surface plasmon resonance analysis. As shown in Fig. S3, A10 scFv-hIgG1 and B10 scFv-hIgG1 showed strong affinity with the cognate HLA/peptide complex (KD = 2.96 × 10−9 M and 5.04 × 10−9 M, respectively).
A10 scFv-hIgG1 and B10 scFv-hIgG1 induced complement-dependent cytotoxicity
Next, we investigated the capacity of the scFv-hIgG1 clones to induce complement-dependent cytotoxicity (CDC). CDC-induced cells were detected by complement C3b positivity on cell membranes and DAPI positivity in nuclei, which was the result of membrane permeability induced by the classical pathway of CDC. We observed that each of the scFv-hIgG1 clones induced CDC in HLA-A24(+)/DNAJB8(+) renal cell carcinoma cell line CAKI-1 and osteosarcoma cell line HOS-A24 (Fig. 3a, b). The proportion of CDC-induced cells was determined using flow cytometry. Similar to the observation by fluorescence microscopy, we also noted that each scFv-hIgG1 mediated CDC activity on CAKI-1 (5.72% and 29.12%, respectively) and HOS-A24 (20.89% and 18.11%, respectively) by A10 scFv-hIgG1 and B10 scFv-hIgG1 (Fig. 3c).
a The CDC of scFv-hIgG1 in renal cancer cell line (a) and osteosarcoma cell line assessed by fluorescence microscopy. C3b(+)/DAPI(+) cells were indicated as dead cells via CDC. b A10-hIgG1 and B10-hIgG1 was used at concentrations of 10 µg/mL. Anti-C3b antibody was used at a concentration of 20 µg/mL. c The CDC of scFv-hIgG1 assessed by FACS. The proportion of C3b(+)/DAPI(+) cells is indicated. Data represent the means ± standard error. *p < 0.05, **p < 0.01, ***p < 0.001.
Development of bispecific antibody possessing anti-CD3 scFv and anti-HLA-A24/DNAJB8_143 peptide complex scFv
We constructed a bispecific antibody, a combination of anti-CD3 scFv and A10 scFv/B10 scFv with a short GGGS linker (Fig. 4a), which we designated as A10-(CD3xJB8) and B10-(CD3xJB8). We hypothesised that these bispecific antibodies could engage non-specific T cells and HLA-A24(+)/DNAJB8(+) tumour cells and induce cytotoxicity like antibody-dependent cellular cytotoxicity (ADCC). These bispecific antibodies could react with DNAJB8_143 peptide presented by HLA-A24 on cell surfaces and T cells but not NK cells (Figs. 4b, c and S4). However, freshly isolated T-cell-mediated bispecific antibody-dependent cellular cytotoxicity (BADCC) was induced by B10-(CD3xJB8) but barely by A10-(CD3xJB8) (Fig. 4d, e). Therefore, B10-(CD3xJB8) might be suitable for further analysis. We assessed the BADCC capacity of B10-(CD3xJB8) against various cell lines of carcinoma and sarcoma. The results showed that B10-(CD3xJB8) induced BADCC to HLA-A24(+)/DNAJB8(+) cell lines (Figs. 4f and S5). In addition, BADCC capacity was greater when activated T cells were used as the effector cells compared with resting T cells (Fig. S6). Activated T cells via B10-(CD3xJB8) and HLA-A24(+)/DNAJB8(+) target cells produced TNFα predominantly, and IL-2 and IFNγ only slightly (Figs. S7 and S8).
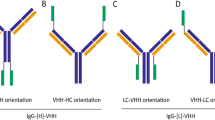
a Schematic of the bispecific antibodies, A10-(CD3xJB8) and B10-(CD3xJB8). His tag is located in the C terminus of A10 and B10 scFv. b Reactivity of A10-(CD3xJB8) and B10-(CD3xJB8) to peptide-pulsed T2-A24 cells. c Reactivity of A10-(CD3xJB8) and B10-(CD3xJB8) to isolated T cells and NK cells. d, e Antibody-dependent cellular cytotoxicity of A10-(CD3xJB8) and B10-(CD3xJB8) against peptide-pulsed T2-A24 and K562 cells. Annexin-V(+)/propidium iodide (PI)(−) cells indicated early apoptosis, and Annexin-V(+)PI(+) cells indicated late apoptosis. f Bispecific antibody-dependent cellular cytotoxicity (BADCC) against renal carcinoma and sarcoma cell lines.
Discussion
In this study, we (i) isolated specific scFv clones reacting to the HLA-A24-restricted CSC/CIC antigen DNAJB8-derived peptide, and found that (ii) A10 scFv and B10 scFv showed high specificity and strong affinity for the cognate antigen, (iii) bivalent A10 scFv-hIgG1 and B10 scFv-hIgG1 could induce CDC to HLA-24(+)/DNAJB8(+) carcinoma and sarcoma cell lines and (iv) T- cell-engaging bispecific antibody B10-(CD3xJB8) induced T-cell-mediated cellular cytotoxicity against HLA-A24(+)/DNAKB8(+) carcinoma and sarcoma cell lines. These results suggested that such artificial antibodies might be of benefit for antibody-based therapy in patients with carcinoma and sarcoma.
To date, many monoclonal antibodies have been approved and yielded clinical response in haematological malignancies and some solid tumours. However, acquired resistance of tumour cells can occur in monoclonal antibody therapy.22 In addition, loss of target antigens has also occurred.23 Therefore, new targets and formats of antibodies might be promising for clinical applications. DNAJB8 was previously reported as a CSC/CIC antigen expressed in RCC. Transduction of DNAJB8 increased tumorigenicity, while knockdown of DNAJB8 decreased tumorigenicity in ACHN in vitro and in vivo.10 Therefore, the antibody targeting DNAJB8-positive tumour cells might be an attractive candidate.
Recently, T-cell-engaging bispecific antibodies have been used particularly in haematological B-cell malignancies.24 Blinatumomab (CD3xCD19) showed 43% complete response (CR) and CR with partial haematological recovery (CRh) in patients with Philadelphia-chromosome-negative, primary refractory or relapsed leukaemia.25 T cells were activated by CD3 scFv only when they were engaged with CD19-expressing cells via blinatumomab.24 Clinical trials of various T-cell-engaging bispecific antibodies, including carcinoembryonic antigen (CEA) × CD3 for gastric cancer, epithelial cell adhesion molecule (EpCAM) × CD3 for epithelial cancer, B-cell maturation antigen (BCMA) × CD3 for multiple myeloma and prostate-specific membrane antigen (PSMA) × CD3 for prostate cancer, are currently being conducted. Most bispecific antibodies target cell surface proteins overexpressed on tumour cells; however, the challenge to develop bispecific antibodies directed to intracellular antigen-derived peptides presented by HLA class I remains. Dao et al. reported the potential efficacy of bispecific antibody directed to WT1-derived peptide in the context of HLA-A2.26 Ahmed et al. reported the TCR-like bispecific antibody targeting EBV LMP2A-derived peptide in the context of HLA-A2.27 Such bispecific antibodies with TCR specificity might be promising for targeting various tumour-specific intracellular proteins with oncogenic functions. DNAJB8 is a cancer stem-cell/cancer-initiating antigen and not expressed in normal organs, except for testis lacking HLA expression like cancer–testis antigen. Hence, the bispecific antibody targeting DNAJB8, B10-(CD3xJB8), might have therapeutic potential without adverse effects on normal organs.
B10-(CD3xJB8) showed cytotoxicity against HLA-A24(+)/DNAJB8(+) tumour cells; however, the frequencies of IL-2 and IFNγ-secreting cells were lower than those of TNFα. We previously observed that the mRNA expression of TNFα was detectable but not that of IL-2 and IFNγ in naive and stem-cell memory T cells.28 Therefore, these observations suggested that B10-(CD3xJB8) might activate T cells close to naive subsets. Further studies using in vivo experiments might be required to prove the efficacy of B10-(CD3xJB8) in the preclinical setting.
In conclusion, we developed scFv clones specific for HLA-A24/cancer stem-like antigen DNAJB8-derived peptide with high specificity and strong affinity. The T-cell-engaging bispecific antibody targeting DNAJB8, B10-(CD3xJB8), might hold promise for antibody-based therapy in patients with carcinoma and bone sarcoma.
References
MaCarthy, E. The toxins of William B. Coley and the treatment of bone and soft-tissue sarcomas. Iowa Orthop. J. 26, 154–158 (2006).
Tsukahara, T., Emori, M., Murata, K., Mizushima, E., Shibayama, Y., Kubo, T. et al. The future of immunotherapy for sarcoma. Expert Opin. Biol. Ther. 16, 1049–1057 (2016).
Tsukahara, T., Hirohashi, Y., Kanaseki, T., Nakatsugawa, M., Kubo, T., Sato, N. et al. Peptide vaccination therapy: towards the next generation. Pathol. Int 66, 547–553 (2016).
Shima, H., Tsurita, G., Wada, S., Hirohashi, Y., Yasui, H., Hayashi, H. et al. Randomized phase II trial of survivin 2B peptide vaccination for patients with HLA-A24-positive pancreatic adenocarcinoma. Cancer Sci. 110, 2378–2385 (2019).
Robbins, P. F., Kassim, S. H., Tran, T. L., Crystal, J. S., Morgan, R. A., Feldman, S. A. et al. A pilot trial using lymphocytes genetically engineered with an NY-ESO-1-reactive T-cell receptor: long-term follow-up and correlates with response. Clin. Cancer Res 21, 1019–1027 (2015).
Lim, W. A. & June, C. H. The principles of engineering immune cells to treat. Cancer Cell 168, 724–740 (2017).
Hirohashi, Y., Torigoe, T., Tsukahara, T., Kanaseki, T., Kochin, V. & Sato, N. Immune responses to human cancer stem-like cells/cancer-initiating cells. Cancer Sci. 107, 12–17 (2016).
Weiner, L. M., Murray, J. C. & Shuptrine, C. W. Antibody-based immunotherapy of cancer. Cell 148, 1081–1084 (2012).
Benjamin, J. E. & Stein, A. S. The role of blinatumomab in patients with relapsed/refractory acute lymphoblastic leukemia. Ther. Adv. Hematol. 7, 142–156 (2016).
Nishizawa, S., Hirohashi, Y., Torigoe, T., Takahashi, A., Tamura, Y., Mori, T. et al. HSP DNAJB8 controls tumor-initiating ability in renal cancer stem-like cells. Cancer Res 72, 2844–2854 (2012).
Morita, R., Nishizawa, S., Torigoe, T., Takahashi, A., Tamura, Y., Tsukahara, T. et al. Heat shock protein DNAJB8 is a novel target for immunotherapy of colon cancer-initiating cells. Cancer Sci. 105, 389–395 (2014).
Nabeta, Y., Kawaguchi, S., Sahara, H., Ikeda, H., Hirohashi, Y., Goroku, T. et al. Recognition by cellular and humoral autologous immunity in a human osteosarcoma cell line. J. Orthop. Sci. 8, 554–559 (2003).
Wada, T., Uede, T., Ishii, S., Matsuyama, K., Yamawaki, S. & Kikuchi, K. Monoclonal antibodies that detect different antigenic determinants of the same human osteosarcoma-associated antigen. Cancer Res 48, 2273–2279 (1988).
Mizushima, E., Tsukahara, T., Emori, M., Murata, K., Akamatsu, A., Shibayama, Y. et al. Osteosarcoma-initiating cells have metabolic features of high aerobic glycolysis and attenuation of OXPHOS mediated by LIN28B. Cancer Sci. 111, 36–46 (2019).
Tsukahara, T., Kawaguchi, S., Ida, K., Kimura, S., Tamura, Y., Ikeda, T. et al. HLA-restricted specific tumor cytolysis by autologous T-lymphocytes infiltrating metastatic bone malignant fibrous histiocytoma of lymph node. J. Orthop. Res 24, 94–101 (2006).
Tsukahara, T., Nabeta, Y., Kawaguchi, S., Ikeda, H., Sato, Y., Shimozawa, K. et al. Identification of human autologous cytotoxic T-lymphocyte-defined osteosarcoma gene that encodes a transcriptional regulator, papillomavirus binding factor. Cancer Res 64, 5442–5448 (2004).
Kuzushima, K., Hayashi, N., Kimura, H. & Tsurumi, T. Efficient identification of HLA-A*2402-restricted cytomegalovirus-specific CD8(+) T-cell epitopes by a computer algorithm and an enzyme-linked immunospot assay. Blood 98, 1872–1881 (2001).
Tsukahara, T., Emori, M., Murata, K., Hirano, T., Muroi, N., Kyono, M. et al. Specific targeting of a naturally presented osteosarcoma antigen PBF peptide using an artificial monoclonal antibody. J. Biol. Chem. 289, 22035–22047 (2014).
Stadler, C. R., Bahr-Mahmud, H., Celik, L., Hebich, B., Roth, A. S., Roth, R. P. et al. Elimination of large tumors in mice by mRNA-encoded bispecific antibodies. Nat. Med. 23, 815–817 (2017).
Nahshol, O., Bronner, V., Notcovich, A., Rubrecht, L., Laune, D. & Bravman, T. Parallel kinetic analysis and affinity determination of hundreds of monoclonal antibodies using the ProteOn XPR36. Anal. Biochem. 383, 52–60 (2008).
Ikeda, H., Lethe, B., Lehmann, F., van Baren, N., Baurain, J. F., de Smet, C. et al. Characterization of an antigen that is recognized on a melanoma showing partial HLA loss by CTL expressing an NK inhibitory receptor. Immunity 6, 199–208 (1997).
Cruz, E. & Kayser, V. Monoclonal antibody therapy of solid tumors: clinical limitations and novel strategies to enhance treatment efficacy. Biologics 13, 33–51 (2019).
Duman, B. B., Sahin, B., Ergin, M. & Guvenc, B. Loss of CD20 antigen expression after rituximab therapy of CD20 positive B cell lymphoma (diffuse large B cell extranodal marginal zone lymphoma combination): a case report and review of the literature. Med. Oncol. 29, 1223–1226 (2012).
Stieglmaier, J., Benjamin, J. & Nagorsen, D. Utilizing the BiTE (bispecific T-cell engager) platform for immunotherapy of cancer. Expert Opin. Biol. Ther. 15, 1093–1099 (2015).
Topp, M. S., Gökbuget, N., Stein, A. S., Zugmaier, G., O’Brien, S., Bargou, R. C. et al. Safety and activity of blinatumomab for adult patients with relapsed or refractory B-precursor acute lymphoblastic leukaemia: a multicentre, single-arm, phase 2 study. Lancet Oncol. 16, 57–66 (2015).
Dao, T., Pankov, D., Scott, A., Korontsvit, T., Zakhaleva, V., Xu, Y. et al. Therapeutic bispecific T-cell engager antibody targeting the intracellular oncoprotein WT1. Nat. Biotechnol. 33, 1079–1086 (2015).
Ahmed, M., Lopez-Albaitero, A., Pankov, D., Santich, B. H., Liu, H., Yan, S. et al. TCR-mimic bispecific antibodies targeting LMP2A show potent activity against EBV malignancies. JCI Insight 3, e97805 (2018).
Murata, K., Tsukahara, T., Emori, M., Shibayama, Y., Mizushima, E., Matsumiya, H. et al. Identification of a novel human memory T-cell population with the characteristics of stem-like chemo-resistance. Oncoimmunology 5, e1165376 (2016).
Acknowledgements
The authors thank the staff of Japanese Red Cross Hokkaido Block Blood Center for the kind donation of human sera.
Author information
Authors and Affiliations
Contributions
H.T. and T.T. designed the study. H.T., T.T., A.A. and I.N. performed the experiments. H.T., T.T., E.M., K.W., T.K., T.K. and Y.H. analysed the data. H.T. and T.T. drafted the paper. N.S. and T.T. supervised the study.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All studies were approved by the Institutional Review Board of Sapporo Medical University. Written informed consent was obtained from all blood donors according to the guidelines of the Declaration of Helsinki.
Consent to publish
Not applicable.
Data availability
The datasets used and analysed during this study are available from the corresponding author.
Competing interests
T. Torigoe received financial support through collaboration with Daiichi-Sankyo Co., Ltd. and Oho Pharmaceutical Co., Ltd. The remaining authors declare no commercial or financial competing interests.
Funding information
This work was supported by JSPS KAKENHI Grants-in-Aid (25462344 to T. Tsukahara, 17H01540 to T. Torigoe), and grants from AMED (19cm0106309h004 to T. Torigoe), the Takeda Science Foundation (2018-Kenkyu-Shorei Keizoku to T. Tsukahara) and the Suhara Memorial Foundation (H30 to T. Tsukahara).
Additional information
Note This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution 4.0 International (CC BY 4.0).
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tadano, H., Tsukahara, T., Mizushima, E. et al. Development of an artificial antibody specific for HLA/peptide complex derived from cancer stem-like cell/cancer-initiating cell antigen DNAJB8. Br J Cancer 123, 1387–1394 (2020). https://doi.org/10.1038/s41416-020-1017-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-020-1017-1
This article is cited by
-
Development of CAR-T cells specifically targeting cancer stem cell antigen DNAJB8 against solid tumours
British Journal of Cancer (2023)